Abstract
Background:
Long-term quality of life is an important consideration of patients in deciding on disease management options for low-risk papillary thyroid cancer (PTC).
Methods:
We conducted a prospective cohort study of Canadian patients who were diagnosed with small (<2 cm in maximal diameter), low-risk papillary thyroid cancer (PTC) and were given the choice of active surveillance (AS) or immediate surgery. We report the results of a self-administered questionnaire on patient-reported outcomes (PROs) that was completed approximately three years after the initial disease management choice. PROs included overall and subscale scores from questionnaires, including those on quality of life (EORTC QLQ-C30, EORTC THY-34), the Assessment of Survivor Concerns, the Decision Regret Scale, and the Generalized Anxiety Disorder 7-item Scale. We compared the results according to the initial disease management choice and according to the disease management status at the time of questionnaire completion.
Results:
The participant response rate was 64% (120/188), including 98 individuals who chose AS and 22 who chose immediate surgery. The median duration of follow-up at the time of questionnaire completion was 42 months (interquartile range [IQR] = 39, 46). After statistical adjustment for multiple comparisons, there were no significant differences in the overall scores or subscales of any of the questionnaires between patients who chose AS and those who chose immediate surgery. However, in a secondary analysis, patients who crossed over from AS to surgery experienced greater cancer-related worry as well as overall worry (p = 0.021 for each) and decision regret (p = 0.031) as compared with patients who remained under AS and those who initially chose surgery.
Conclusions:
We observed that PROs do not significantly differ between patients who chose AS and those who chose immediate surgery a few years after the initial disease management choice. However, patients who crossover from AS to surgery may experience greater cancer-related worry and decision regret.
Introduction
In the United States1,2 and Canada,1,3 papillary thyroid cancer (PTC) is much more commonly diagnosed than in prior decades. The increase in the incidence rate over time has been particularly notable for small, low-risk PTC, 2 and this may be, in part, attributed to advances in diagnostic technology. 1
Given the high incidence and relatively low disease-related mortality risk of small, low-risk PTC, active surveillance (AS) has emerged as a viable alternative to surgery for PTC disease management, particularly for those tumors measuring 1 cm or less in diameter (papillary thyroid microcarcinoma).4–6 The longest follow-up of patients with low-risk papillary microcarcinoma managed with AS was reported from Kuma Hospital in Japan, where this approach was established >30 years ago. 7 Overall, patients with small, low-risk PTC who undergo AS have a very low risk of dying of thyroid cancer, which is similar to that of surgically treated patients. 8
One of the main reasons why patients may choose AS over surgery for the management of small, low-risk PTC is the preservation of quality of life. 9 Multiple observational studies from Asia examining patient-reported outcomes (PROs) in individuals with low-risk papillary thyroid microcarcinoma have suggested that quality of life at follow-up may be superior in patients who undergo AS as compared with surgically treated patients.10–13 However, the quality-of-life implications of the choice of surgery compared with AS are not known for patients with PTCs that are larger than microcarcinomas, nor in the North American clinical and cultural context.
In this study, we report the three-year follow-up PROs in Canadian patients with low-risk PTC <2 cm in maximal diameter who chose AS or immediate surgery. The outcomes examined include quantitative scores from the following questionnaires: quality of life (EORTC QLQ-C30, 14 EORTC THY-3415,16), Assessment of Survivor Concerns, 17 the Decision Regret Scale, 18 and the Generalized Anxiety Disorder 7-item Scale. 19
Methods
Study design and participants
We report on a single-center, prospective, cohort study of PTC patients enrolled at University Health Network (UHN) in Toronto, Canada, between May 2016 and February 2021. Eligible participants were 18 years of age or older and had untreated PTC <2 cm in maximal diameter, which was confined to the thyroid and in a location amenable to AS.20,21 Patients were offered the choice of either AS or surgery. The study protocol details were previously reported (NCT03271892).20,21 Patients under AS underwent routine clinical follow-up every six months for two years, followed by yearly (with additional assessments, if needed). The patients who had immediate surgery received usual care from their surgeons or other treating physicians. The patients in the AS group received a recommendation to crossover to surgery if prespecified study criteria were met (e.g., PTC progression), and they had the option to crossover to active treatment at any time as per their own choosing, in the absence of disease progression/study indications. In this report, crossover from AS refers to patients in the AS group who received an investigator recommendation for surgery due to disease progression or study-related concern or patients who chose to undergo surgery/definitive treatment in the absence of disease progression.
Our original protocol included PRO questionnaires at baseline and one year, and those results were reported.22,23 We secured additional research funding for the collection of long-term PRO data as a part of a prospective multicenter study (NCT04624477). 24 Patients from the original Toronto study were offered the opportunity to participate in the extended follow-up of PROs.
The UHN Research Ethics Board approved this study, with the extended follow-up protocol amendment (15-8942). The study patients provided informed consent for participation in the original study, and those who agreed also provided a second consent for participation in the extended follow-up study. Participants were free to decline the questionnaires in the extended follow-up study, without withdrawing formally from the main study clinical follow-up. We report herein the data from the participants of the original Toronto study who participated in the three-year PRO evaluation.
Questionnaires
Self-administered patient questionnaires included an update on thyroid cancer status/treatment as the following questionnaires: quality of life (EORTC QLQ-C30 14 for cancer patients and survivors, EORTC THY-3415,16 for thyroid cancer patients and survivors), the Assessment of Survivor Concerns (ASC 17 for cancer survivors, 5-item scale), the Decision Regret Scale 18 designed to measure remorse after a health care decision, and the Generalized Anxiety Disorder 7-item Scale (GAD-7) for anxiety disorder screening. 19 The questionnaire scores were calculated as per the developers’ guidance. Missing values were imputed with the subscale mean for the EORTC and ASC questionnaires. Listwise deletion was performed for missing values from other questionnaires.
Domain scores were calculated for the respective EORTC questionnaire domains for the QLQ-C30 and EORTC THY-34 and transformed for a scale of 0 to 100. In the EORTC QLQ-C30, a higher symptom score represents worse distress, a higher functional scale reflects better functioning, and a higher overall score reflects better quality of life. In the EORTC THY-34, a higher symptom score reflects worse symptoms. The Decision Regret Scale scores were transformed and expressed on a scale of 0 to 100, where 100 reflects worse regret. In terms of score severity, most of the questionnaires did not have established cut-offs. However, for the Decision Regret Scale, a score of 25 has been reported in distinguishing low versus higher decision regret about health care decisions. 25 Furthermore, the GAD-7 scores of 5, 10, and 15 have been reported as cut-off points for distinguishing mild, moderate, and severe anxiety, respectively, and a cut-off point of 10 or greater has been reported as a screen for generalized anxiety disorder. 19
Statistical analysis
Cohort characteristics were summarized using descriptive statistics and stratified by the initial choice of AS or surgery. Descriptive data were summarized as numbers with percentages or means with standard deviations (SDs) or medians with interquartile ranges (IQRs). The differences in the demographic and clinical characteristic distribution were assessed using the Mann–Whitney U and Fisher’s exact tests for continuous and categorical characteristics, respectively.
The respective domain and the overall scores from all questionnaires were summarized using descriptive statistics for the entire study population, according to the initial treatment choice (AS or surgery) as well as according the disease treatment status as of the time of questionnaire completion (i.e., continuing AS in the absence of disease progression, crossover [defined by crossing over from AS to surgery/active treatment or meeting the criteria for crossover surgery due to the prespecified study criteria], or immediate surgery). The differences in the distribution of questionnaire scores for the AS versus surgery comparisons were examined using the Mann–Whitney U test, and the differences in the AS versus AS crossover versus surgery comparisons were examined using the Kruskal–Wallis test. The Benjamini-Hochberg correction was applied to the comparisons of all subscales within each questionnaire to adjust for multiplicity.
To check for the robustness of the findings, secondary linear regression sensitivity analyses adjusting for age (continuous) and sex were performed. The resulting β coefficients, confidence intervals (CIs), and associated p-values are presented. The Benjamini-Hochberg correction was applied to adjust for the multiplicity of all of the comparisons.
Post hoc secondary subgroup analyses were performed in response to peer review. Within each subgroup, the mean (SD) QoL score was summarized. To assess the differences between the subgroups, the mean difference and its CI (estimated using the paired t-test assuming unequal variances) were estimated. No formal hypothesis tests were conducted on the post hoc secondary subgroup analyses; thus, these should be considered hypothesis-generating.
All hypothesis tests were two-sided, and p-values <0.05 were considered statistically significant. Statistical analyses were conducted by experienced statisticians (K.L., W.X.) using R version 4.4.2.
Results
Study participants
We included data from 120 participants, including 98 who originally chose AS and 22 who chose immediate surgery (Fig. 1). The response rate for eligible patients who were sent the survey was 64% (120/188) (Fig. 1). The median follow-up period at the time of questionnaire completion was 42 months (IQR = 39, 46). In keeping with the epidemiology of low-risk PTC, females comprised 74% (89/120) of the respondent population. The median age of respondents was 53 years (IQR = 44, 66). The demographic and clinical details of participants according to their initial disease management choice (AS or immediate surgery) are shown in Table 1. The most notable difference between the groups was that patients who chose AS (median age = 55 years) were significantly older than those who chose immediate surgery (median age = 46 years) (p = 0.012) (Table 1).
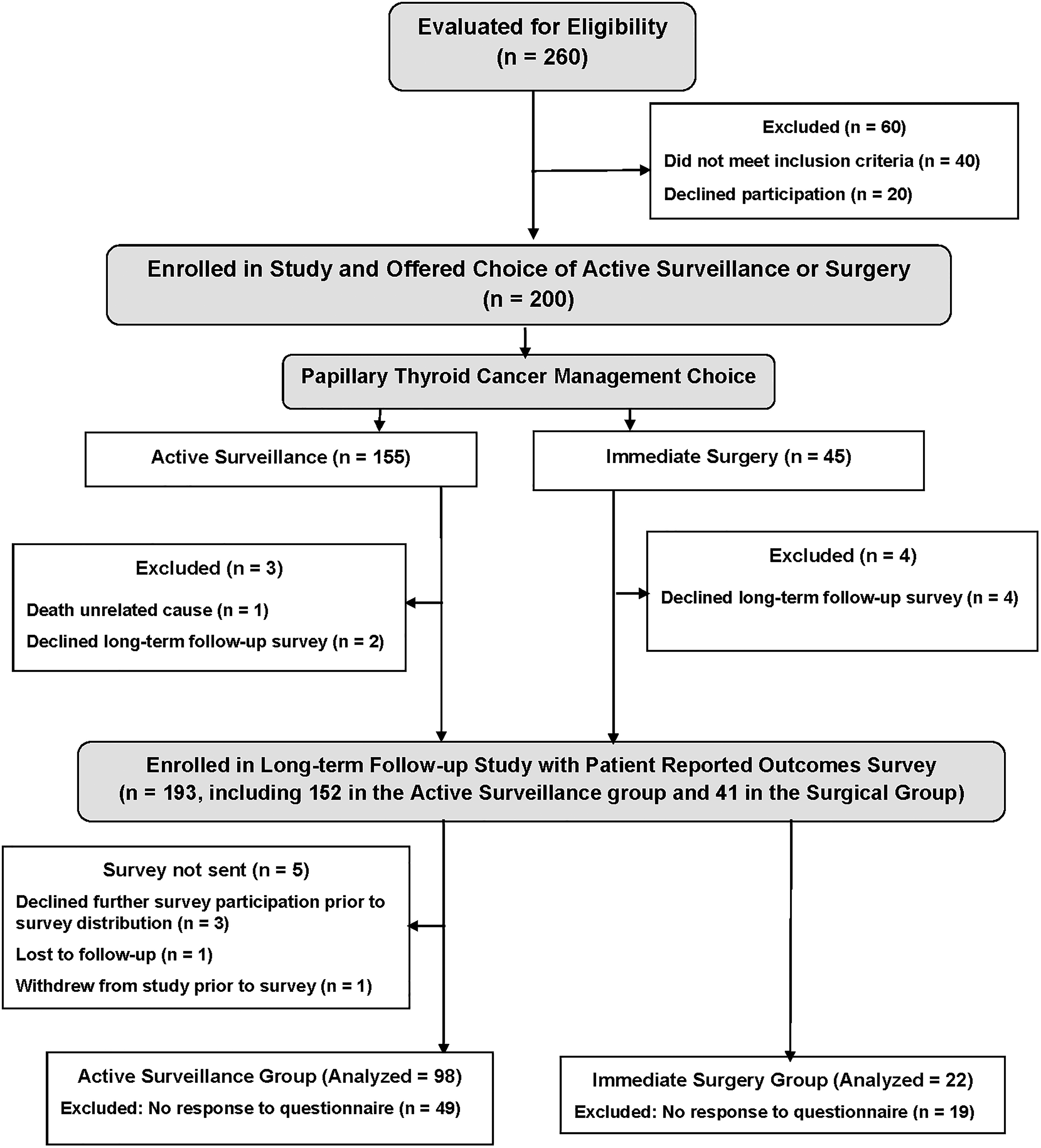
Participant flow diagram. The written questionnaire was distributed to 193 patients with small, low-risk papillary thyroid carcinoma, including 152 who had originally chosen active surveillance and 41 who originally chose surgery approximately three years after the original decision on disease management.
Demographic and Clinical Characteristics of the Respondents
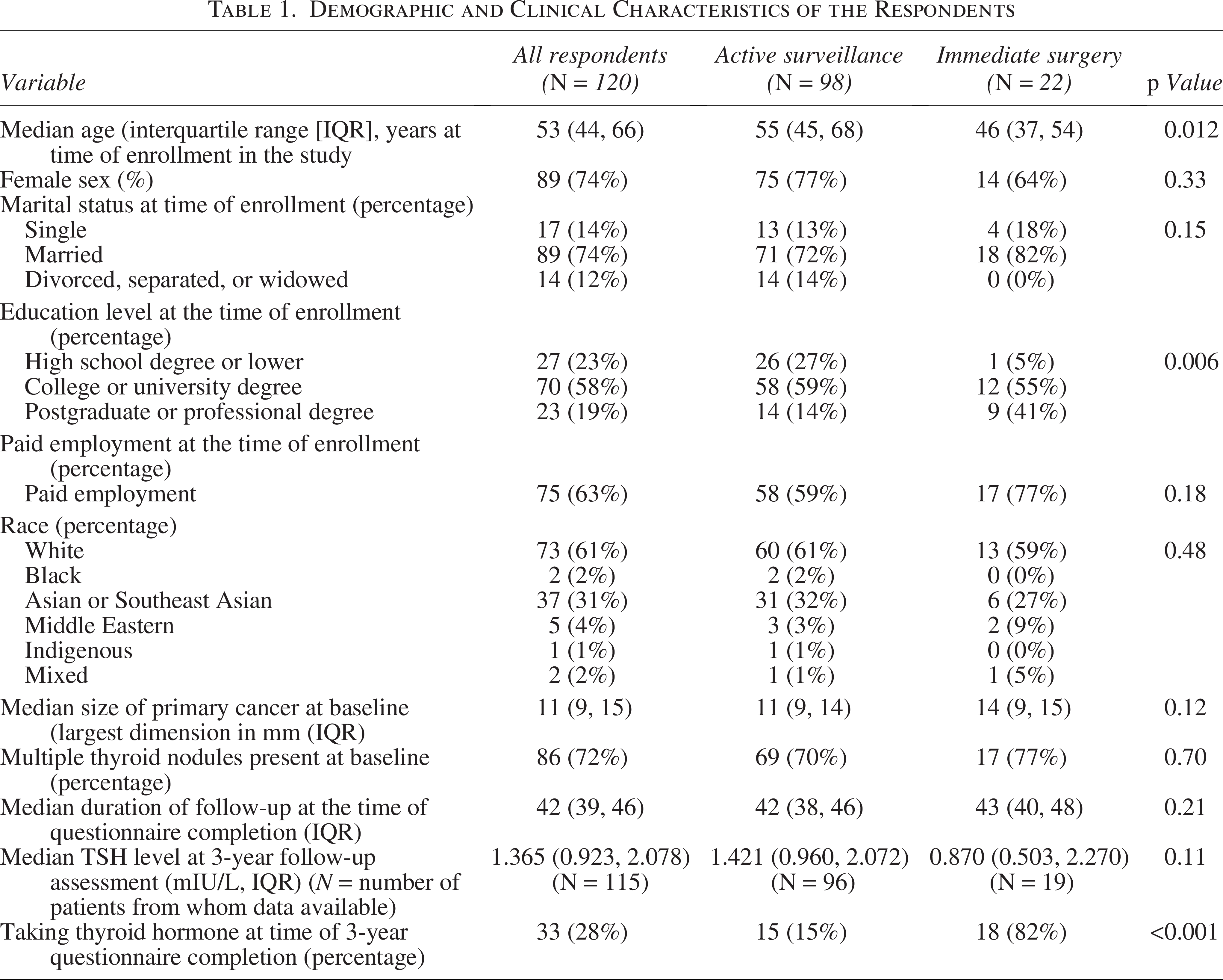
Of the 98 patients who had initially chosen AS, 16 (16%) crossed over to surgery/active treatment (i.e., underwent delayed surgery/active treatment [n = 13] or had received an investigator recommendation for surgery due to disease progression or other investigator concern but declined treatment [n = 3]) as of the time point of questionnaire completion. Of the 16 patients who crossed over, half had disease progression (50%, 8/16), 44% (7/16) chose to cross over to active treatment in the absence of disease progression, and 1 patient was advised to have surgery due to measurement uncertainty in the tumor, as the tumor margin and the surrounding tissue were obscured in the context of Hashimoto’s thyroiditis. Three of the patients with disease progression (tumor growth [and suspicion of possible extrathyroidal extension in one case]) declined surgery and continue to be followed up.
The most common initial surgical procedure/treatment performed in this study was a hemithyroidectomy, which was performed in 77% of both the AS crossover group (10/13) and the immediate surgical group (17/22). Of the patients who had an initial hemithyroidectomy, one patient in the immediate surgery group underwent completion thyroidectomy within a year of the first surgery. There were 2/13 (15%) patients in the AS group and 5/22 in the immediate surgical group (23%) whose first thyroid surgery was a total thyroidectomy. One patient in the AS group who crossed over to definitive treatment due to patient choice with no evidence of disease progression underwent radiofrequency ablation (RFA) outside of the study in another country (sought out by the patient). This patient continued to be followed up in the study, and the RFA was counted as a crossover to definitive treatment in the analyses.
Primary analyses of PROs
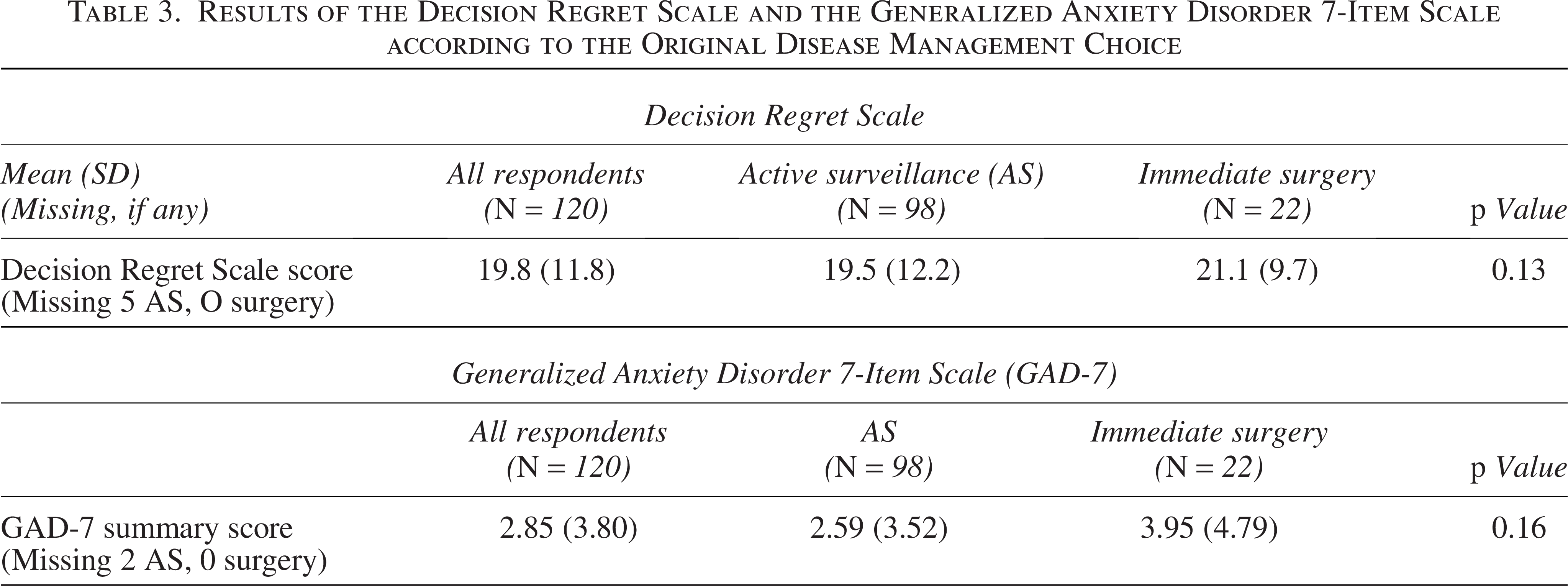
The PRO results according to the original disease management choice (AS or immediate surgery) are shown in Tables 2 and 3, whereas PROs according to the disease management status (AS, crossover from AS to surgery/active treatment [or meeting the progression criteria for crossover], or immediate surgery) are shown in Tables 4 and 5 (and Fig. 2). After statistical adjustment for multiple comparisons (where applicable), there was no significant difference in any of the subscales or overall PRO scores between the AS and immediate surgery groups (Tables 2 and 3). However, on stratifying the data according to the disease management status, we observed statistically significant group differences, such that patients who crossed over from AS to surgery had the greatest cancer worry and overall worry on the ASC questionnaire (p = 0.021 for group differences, Table 4, Fig. 2C) and the worst level of decision regret (p = 0.031 for group differences, Table 5 and Fig. 2D) as compared with patients who remained on AS without meeting the criteria for crossover or those who chose immediate surgery.
Results of Cancer-Related Patient-Reported Outcomes according to the Original Disease Management Choice
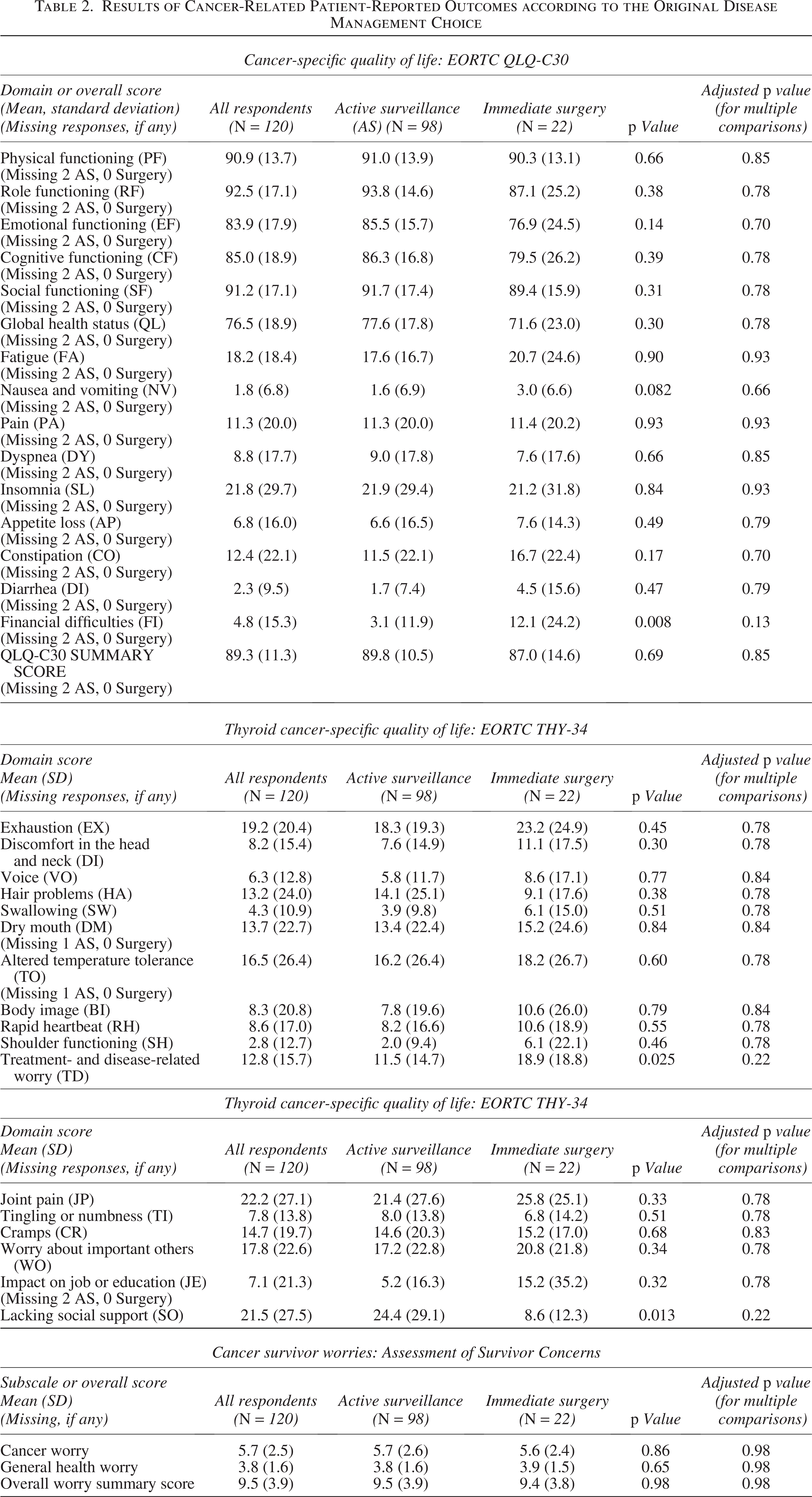

Results of the Decision Regret Scale and the Generalized Anxiety Disorder 7-Item Scale according to the Original Disease Management Choice
Results of Cancer-Related Patient-Reported Outcomes according to the Disease Management Status
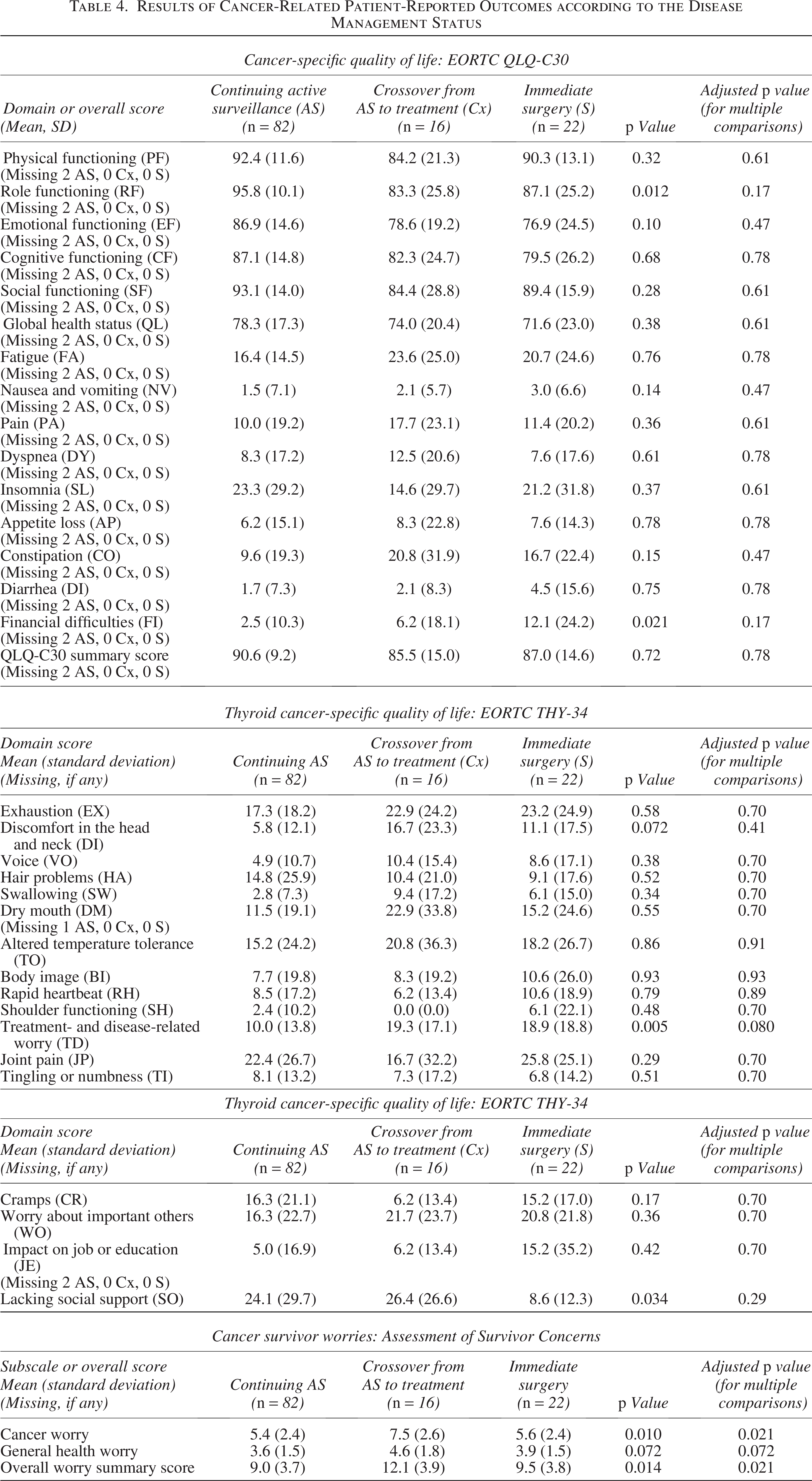
Results of the Decision Regret Scale and the Generalized Anxiety Disorder 7-Item Scale according to the Disease Management Status
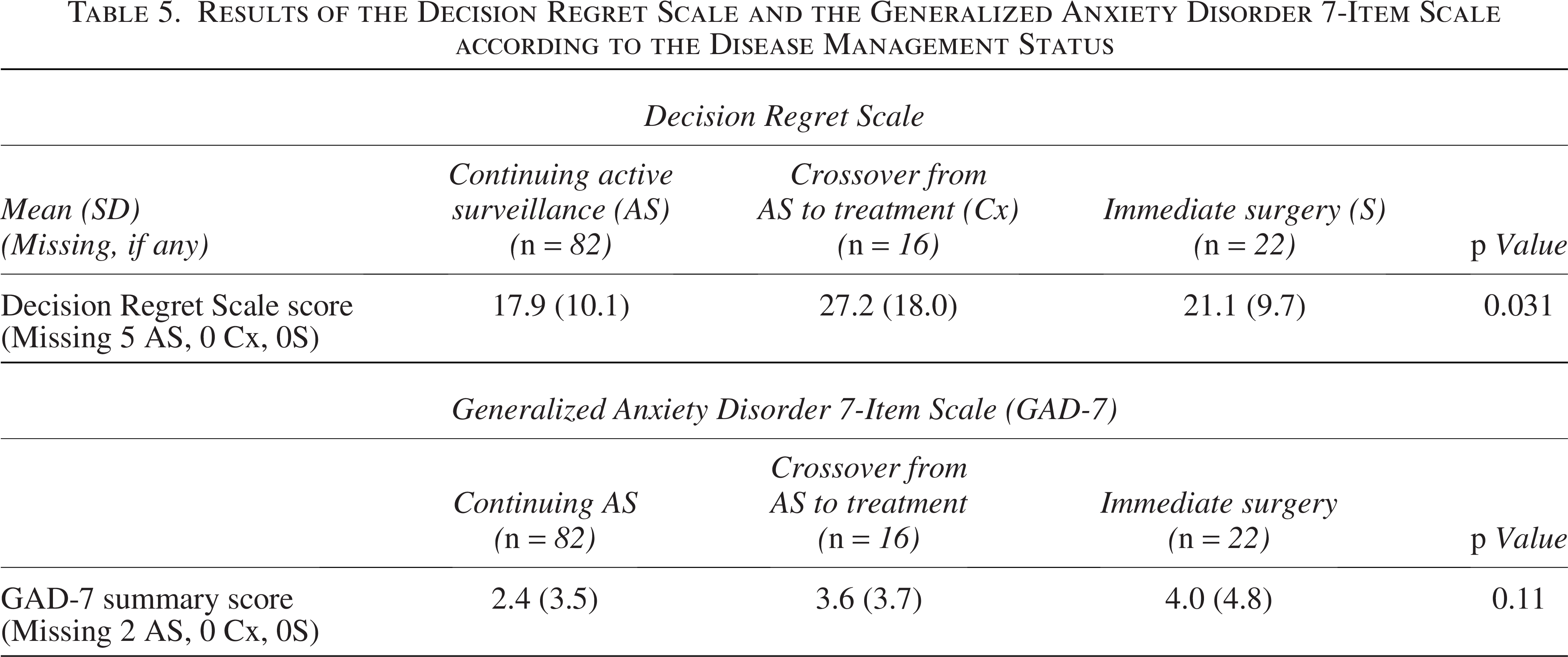
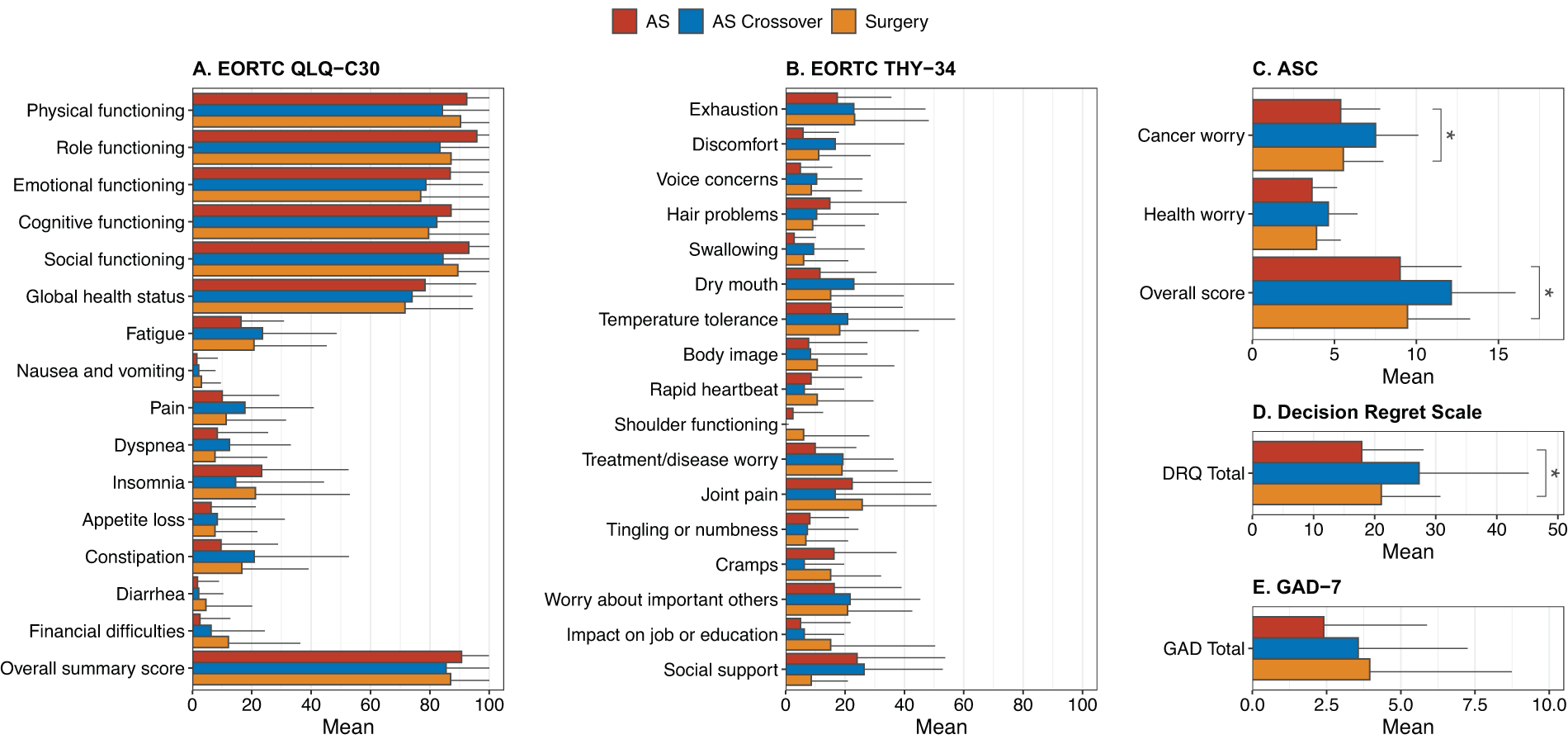
Patient-reported outcomes according to disease management status (continuing active surveillance [AS], crossover from AS to surgery [AS crossover], or initial choice of surgery [Surgery]).
Age- and sex-adjusted PRO sensitivity analyses
Age- and sex-adjusted linear regression analyses of the questionnaire domain and overall scores are presented in Supplementary Tables S1 and S2. These findings were similar to the crude data comparisons, in that there were no significant group differences in age- and sex-adjusted questionnaire outcomes between patients who chose AS and those who chose surgery after accounting for the multiplicity of analyses (Supplementary Table S1). However, patients who crossed over from AS to surgery had significantly greater cancer worry (β coefficient = 2.01 [CI: 0.68, 3.34], p = 0.01), health worry (β = 0.99 [CI: 0.14, 1.84], p = 0.02), and overall worry (β = 3.00 [CI: 0.94, 5.06], p = 0.01) compared with patients who remained on AS without crossing over on the ASC questionnaire (after adjustment for age and sex and the multiplicity of comparisons) (Supplementary Table S2). Also, patients who crossed over from AS had significantly worse age- and sex-adjusted decision regret compared with patients who remained on AS without crossing over (β = 9.64 [CI: 3.45, 15.8], p = 0.003; adjusted for age, sex, and multiple comparisons) (Supplementary Table S2).
Exploratory post hoc subgroup analyses
In post hoc exploratory subgroup analyses, the mean level of decision regret in seven individuals who crossed over from AS to surgery/definitive treatment due to patient preference was 38.9 (SD = 18.0), whereas it was 19.0 (SD = 13.0) in eight individuals who had disease progression during AS, with a mean difference of 19.9 [CI: 1.8, 38.0] between the groups (Supplementary Table S3). However, other PROs did not appear to be significantly different between these groups (Supplementary Table S3). Of the eight patients whose disease progressed under AS, there was no significant mean difference in decision regret or cancer-related worry between the five patients who underwent surgery and the three patients who declined surgery (Supplementary Table S4).
In combining 22 patients from the immediate surgery group and 13 patients from the AS group who underwent surgery/definitive treatment, there was no significant difference in PROs according to whether patients took thyroid hormone treatment or not at the time of three-year questionnaire completion (Supplementary Table S5).
Discussion
In conclusion, in this prospective observational study examining PROs in patients with small, low-risk PTC, the overall quality of life did not significantly differ between patients who chose AS and those who chose immediate surgery. However, patients who crossed over from AS to active treatment or met the crossover criteria for surgery due to disease progression (the crossover group) had the greatest cancer worry and overall worry on the ASC questionnaire and the most decision regret on the Decision Regret Scale. Our findings were robust after adjusting for age, sex, and multiple comparisons.
In examining the prior literature, two respective published cross-sectional studies from Japan 11 and Korea 10 as well as two prospective studies from Korea with median follow-up periods of approximately two years12,13 have reported that some aspects of quality of life were superior in patients with papillary thyroid microcarcinoma choosing AS compared with those who had immediate surgery. We have also previously reported that at the one-year time point in our cohort, patients who chose immediate surgery had greater symptom interference with life (compared with those who chose AS), attributed to some impairments in general activity, mood, work, relationships, and enjoyment of life 23 (using the MD Anderson Symptom Inventory for Thyroid Cancer 26 ). However, the current assessment was performed at a much later time point in the follow-up trajectory (median = 42 months after enrollment/decision-making), and we utilized the more recently validated EORTC THY-34 questionnaire 16 (that was not available when our study began). There were some conflicting findings between the two Korean prospective studies on the outcome of overall quality of life in patients with papillary microcarcinoma who were offered surgery or AS, in that Kim et al. reported no significant group differences after 12 months, 13 but Moon et al. reported that physical QOL was better in patients under AS compared with those who chose surgery (and adjusted for the multiplicity of analyses). 12 Kim et al. reported that quality of life improved over time in surgically treated patients, and this was attributed to recovery from the temporary impact of surgery. 13 Our findings suggest that a few years after choosing AS or surgery, there do not appear to be clinically important differences in quality of life between patients with small, low-risk PTC choosing AS or surgery (when a relatively conservative surgical approach is used, i.e., mostly hemithyroidectomy).
Overall, the aggregate values for quality of life of our low-risk PTC study participants were fairly good. Our EORTC QLQ-C30 questionnaire data are relatively comparable to the recently reported normative data for a U.S. general population. 27 In the general population study, 27 some floor and ceiling effects related to low symptom severity and high functioning in some domains were observed, and we also observed such effects in the current study. In understanding the clinical importance of the EORTC QLQ-C30 differences, Snyder et al. reported that a difference of 10 points or greater on an EORTC QLQ-C30 score corresponded to clinically meaningful changes in the supportive care needs of cancer patients. 28 However, this magnitude of difference was not observed in any of the EORTC QLQ-C30 domains or the overall score in comparing patients who chose AS or surgery in this study. The EORTC THY-34 mean scores in our population are generally either comparable to or better than that of thyroid cancer survivors of mixed clinical and treatment characteristics, who were evaluated two or more years following their initial diagnosis by Singer et al. 16
We found that patients who crossed over from AS to active treatment (or met the disease progression criteria for crossover) had the greatest cancer worry, overall worry, and decision regret, although for the most part, quality of life scores were not significantly different from patients who remained under AS with no disease progression or those who chose immediate surgery. We have previously reported similar findings with respect to decision regret at the one-year follow-up time point in this cohort. 23 Kim et al. have previously reported that at 12 months, quality of life scores were worse in those who crossed over from AS to surgery than those of patients who remained under AS, 13 but the other outcomes were not specifically examined. Moon et al. reported on 101 patients who crossed over from AS to surgery as of a two-year time point in follow-up (which was 20% of the respondents who initially chose AS) and suggested that 35 patients who crossed over due to disease progression had better quality of life than 66 patients who crossed over but did not have disease progression. 12 In an exploratory analysis, we observed that the level of decision regret was greater in patients who crossed over due to patient choice as compared with those who crossed over due to disease progression. This finding requires confirmation in future research.
Some strengths of this study include its prospective nature, the comprehensiveness of the PRO assessment, the relatively long duration of follow-up, and the execution of a statistical analysis plan attentive to accounting for the multiplicity of analyses and adjustment for confounders in sensitivity analyses. However, some limitations include a relatively limited sample size, a 64% response rate with potential nonresponder bias, and a single participating study center. Furthermore, we were unable to adjust for baseline questionnaire scores, as the questionnaires administered at baseline were different than those at long-term follow-up. For example, we did not collect data on the EORTC THY-34 questionnaire at baseline or the one-year time point, 23 as this questionnaire was not available at the time we began our study. Larger prospective studies are needed to confirm our findings and to explore if more subtle differences in the subscales of PRO instruments may be detectable.
In conclusion, we found that in general, PROs did not significantly differ between patients with small low-risk PTC who chose AS and those who chose immediate surgery a few years after making the initial disease management choice. This is important information for patients and clinicians to consider when deciding about the disease management of small, low-risk PTC, as long-term quality of life is prioritized by many patients. Our findings cannot be generalized to patients who have other histological types of thyroid cancer, more severe disease, undergo more extensive surgery or other treatments, or who are in a different health care setting. It is also important to acknowledge that quality-of-life scores are, by their inherent nature, subjective, and individual patients may experience greater symptoms or functional interference due to a variety of individual factors. Our findings need to be confirmed in larger prospective studies, including our multicenter Canadian study that is ongoing (including additional participants and participants in other Canadian cities). 24
Authors’ Contributions
A.M.S.: Conceptualization, data curation, formal analysis, funding acquisition, investigation, methodology, project administration, resources, supervision, writing—original draft, writing—reviewing and editing. S.G.: Conceptualization, data curation, funding acquisition, investigation, methodology, resources, supervision, writing—reviewing and editing. L.R.: Conceptualization, investigation, writing—reviewing and editing. J.C.I.: Conceptualization, investigation, writing—reviewing and editing. J.D.P.: Conceptualization, investigation, writing—reviewing and editing. K.L.: Formal analysis, methodology, software, visualization, writing—reviewing and editing. W.X.: Supervision, formal analysis, methodology, software, visualization, writing—reviewing and editing. J.M.J.: Conceptualization, methodology, funding acquisition, writing—reviewing and editing. A.G.: Conceptualization, methodology, funding acquisition, writing—reviewing and editing. N.N.B.: Conceptualization, methodology, funding acquisition, writing—reviewing and editing. D.P.G.: Conceptualization, data curation, funding acquisition, investigation, methodology, project administration, resources, supervision, writing—reviewing and editing. All of the authors reviewed and approved the article and are accountable for this work.
Footnotes
Acknowledgments
The authors would like to express our greatest appreciation to all of the study participants as well as our clinical collaborators. The authors would also like to thank our current and former research staff members: Alex O. Esemezie, BSc, Ogemdi Ihekire, Giselle Peralta, Ailya Salman, Jasmeen Sidhu, Sherome Vijayendran, and Tom Yoannidis.
Author Disclosure Statement
No competing financial interests exist. Anna M. Sawka is the Editor-in-Chief of the journal, Thyroid; she was blinded to the peer review process of this manuscript.
Funding Information
The original single-center study in Toronto was funded by the Ontario Academic Health Sciences Centres Alternate Funding Plan Innovation Grant (Ontario Ministry of Health) and the Canadian Cancer Society (Lotte and John Hecht Memorial Foundation Innovation Grant, #703948). Consenting patients from this cohort were included in an expanded pan-Canadian multicenter study, which is supported by the Canadian Institutes of Health Research (Project Grant, #PJT-162314) and the Canadian Cancer Society (Innovation to Impact Grant, # 706302). The funders had no role in the study design data collection, data analysis, data interpretation, or writing of the report.
Canadian Thyroid Cancer Active Surveillance Study Group
(Greater Toronto Area — sites listed in alphabetical order): Grand River Hospital (Kitchener) — Avik Banerjee, Vinita Bindlish, Maky Hafidh, Jose Prudencio, Vinod Bharadwaj; Guelph General Hospital — Denny Lin; Humber River Hospital — Laura Whiteacre; Lakeridge Health — Eric Arruda, Artur Gevorgyan; Independent Practice — Marshall Hay; Mackenzie Health Hospital — Philip Solomon; Mount Sinai Hospital — Eric Monteiro, Karen Gomez Hernandez, Allan Vescan, Ian Witterick; North York General Hospital — Everton Gooden, Manish Shah; Scarborough Health Network (Centenary Hospital) — Michael Chang; St. Joseph’s Health Centre — Andres Gantous; St. Michael’s Hospital — Jennifer Anderson; Scarborough Health Network (General Hospital) — Vinay Fernandes; Scarborough Health Network (Centenary Hospital, General Hospital, and Birchmount Hospital) — Sumeet Anand; Sunnybrook Health Sciences Centre — Danny Enepekides, Antoine Eskander, Ilana J. Halperin, Kevin Higgins; Trillium Health Partners — Janet Chung, Karim Nazarali, Lorne Segall (deceased); University Health Network — John De Almeida, Shereen Ezzat, Ralph Gilbert, Patrick J. Gullane, Amin Madani, Richard W. Tsang (retired); William Osler Health System — Mark Korman; Women’s College Hospital: Karen Devon, Afshan Zahedi.
