Abstract
Industrial hog operation (IHO) workers face a range of occupational hazards, including exposure to zoonotic pathogens such as livestock-associated antimicrobial-resistant Staphylococcus aureus and swine-origin influenza viruses with epidemic or pandemic potential. To better understand this population's occupational exposure to zoonotic pathogens, we conducted a community-driven qualitative research study in eastern North Carolina. We completed in-depth interviews with ten IHO workers and used thematic analysis to identify and analyze patterns of responses. Workers described direct and indirect occupational contact with hogs, with accompanying potential for dermal, ingestion, and inhalation exposures to zoonotic pathogens. Workers also described potential take-home pathways, wherein they could transfer livestock-associated pathogens and other contaminants from IHOs to their families and communities. Findings warrant future research, and suggest that more restrictive policies on antimicrobials, stronger health and safety regulations, and better policies and practices across all IHOs could afford greater protection against worker and take-home zoonotic pathogen exposures.
Keywords
Introduction
North Carolina is the second largest hog producer in the United States (U.S.) and most animals are raised in industrial hog operations (IHOs).1,2 IHOs are high animal density, confinement-based operations which vertically integrate the phases of hog production, including breeding, farrowing, nursing, and finishing.1,2 Workers at IHOs have higher rates of injury and illness compared to all U.S. workers, and IHO work is associated with infectious and respiratory diseases, cancers, and occupational injuries.3–8 This may be due to the types of workplace exposures and stressors (e.g., physical, chemical, biological, psychological) at IHOs as well as lower wages, temporary employment, lower levels of formal education, challenges related to documentation or citizenship status, and/or limited English proficiency, which can restrict workers’ abilities to access information, training, and protections.9–12
IHO workers are exposed to a variety of occupational hazards, including livestock-associated microbes and zoonotic pathogens.4,5,8 IHOs use antimicrobials to treat sick animals as well as to control or prevent the spread of disease in crowded conditions, which can lead to the development of pathogen antimicrobial resistance. 13 Through a series of guidance for industry documents, the U.S. Food and Drug Administration worked with producers of medically important antimicrobial drugs to achieve voluntary withdrawal of approvals for indicated uses that are not necessary for animal health (e.g., growth promotion). This process was completed in 2017.14–17 However, the same drugs can be used at low dosages and extended periods for disease prevention. 17 Antimicrobials for use in food animals continue to represent approximately 65 percent of all antimicrobials sold in the US. 18 Epidemiologic studies have identified livestock-associated methicillin-resistant S. aureus (MRSA) and multidrug-resistant S. aureus (MDRSA) among IHO workers.19–22 Further, frequent and direct contact with live swine has been associated with colonization of workers by antimicrobial-resistant S. aureus from IHOs. 19 Davis et al. identified livestock-associated MDRSA among swine, in IHO worker breathing zone air samples, and in ambient air at IHOs, suggesting that touching or working close to swine could facilitate transmission of livestock-associated pathogens between animals and workers. 23
Research indicates that livestock-associated microbes are risk factors for adverse health outcomes. IHO workers carrying livestock-associated strains of S. aureus were more likely to report recent skin and soft tissue infection (SSTI) symptoms compared to those not carrying livestock-associated strains. 24 There is also evidence that livestock-associated MRSA and MDRSA strains contracted by IHO workers are more pathogenic than community-associated strains. 25 Beyond S. aureus, IHO workers also are at risk of infection with other antimicrobial-resistant bacteria (e.g., Carbapenem-resistant Enterobacteriaceae [CRE], Streptococcus suis), swine-origin influenza viruses, and hepatitis E virus.26–34 Common IHO practices, including confining large numbers of swine and consistently introducing new animals, could increase risk of recombination, development, and spread of emerging and re-emerging zoonotic influenza strains.35,36
Contaminants unintentionally brought home from the workplace are termed “take-home” exposures. Take-home exposures to asbestos, lead, arsenic, solvents, hydrocarbons, pesticides, flour, influenza virus, and SARS-CoV-2 have all been associated with adverse health effects among workers and workers’ household members.37–39 Research suggests that workers infected with S. aureus, MRSA, MDRSA, or other livestock-associated microbes in the workplace can bring those pathogens home to household members.19–21 Workplace factors including antimicrobial use, higher swine stocking density, and bringing home personal protective equipment (PPE) have all been associated with increased prevalence of S. aureus, MRSA, and MDRSA in workers’ household members.21–24 However, there is limited understanding of the range and types of activities that could produce microbial take-home exposure from IHO operations.19,21
Here we undertook a qualitative study to address current knowledge gaps by investigating potential occupational microbial exposure pathways in IHOs, including circumstances of worker contact with swine and worker practices during transitions from work to home that could affect transfer of microbes from IHOs to workers’ families and communities. Qualitative research methods are well-suited for this investigation because of their strengths in understanding health behaviors, needs of vulnerable populations, personal experiences and contextual knowledge, and unexplained phenomena. 40 Below, we describe IHO workers’ accounts of potential occupational microbial exposure pathways and take-home practices.
Methods
This study was part of an ongoing collaboration between the Johns Hopkins Bloomberg School of Public Health (JHSPH) and the Rural Empowerment Association for Community Help (REACH, https://www.ncruralempowerment.org/), a community-based 501(c)(3) organization in Duplin County, North Carolina. Participants were eligible for inclusion in this study if they were current or past IHO workers residing in one of the top 10 hog-producing counties in North Carolina, were 18 years of age or older, spoke English or Spanish, and agreed to participate in the study. REACH organizers purposely sampled individuals representing a range of worker characteristics, including age, gender, race, ethnicity, operation type, job activity, and duration of employment at an IHO. Participants received a $25 cash incentive. The sample size was based on feasibility in reaching respondents, which was challenging, partly due to workers’ concerns about employer retaliation for participating. Three of thirteen initially recruited IHO workers declined to participate in the interviews due to concerns that participation could jeopardize their employment.
A team of one REACH community organizer and one university researcher conducted the interviews at participants’ homes or private locations during spring 2014. A bilingual REACH organizer served as translator for interviews with Spanish-speaking individuals. Interviewers followed a semi-structured interview guide, which included the following topics: (1) IHO work conditions and livestock exposures, and (2) transitions from work to home and family (Supplementary File). In addition, we collected demographic information. Interviews were audio-recorded and lasted about an hour in length. A service transcribed the recorded interviews. One team member who was present at all interviews (A.L.) reviewed and corrected the transcripts for accuracy.
The research was approved by the Institutional Review Board of the Johns Hopkins Bloomberg School of Public Health (IRB#00005253). In addition to following the IRB-approved protocol for protecting study participants’ confidentiality, we obtained a certificate of confidentiality from the Centers for Disease Control and Prevention (CDC), which protects personally identifiable information from being released in any federal, state, or local legal proceedings, even under court order or subpoena.
Analysis
We used thematic analysis to explore participants’ experiences of workplace conditions and circumstances that may promote exposure to zoonotic pathogens and facilitate or limit transmission from work to home.40–42 As a team, we developed a codebook based on our interview guide and themes we identified. 40 A.L. used ATLAS.ti to code interview text segments and to assemble similarly coded passages across all interviews.40,43 A.L., C.C., and C.G. reviewed the codes and representative quotations, identified key themes to summarize our findings, and discussed the range of experiences and opinions related to each theme. 42 Throughout the analysis, we returned to interview transcripts to verify that our interpretations were consistent. We also met with our community partner to discuss themes and the representativeness of the results.
Results
Participants included 10 current or former IHO workers from two corporation-owned IHOs, one contract farm (i.e., owned by grower, but practices dictated by corporation), and one privately owned farm, representing all production phases from breeding to pre-slaughter (described in the note below Table 1) and located in three North Carolina counties. Participants ranged in age from twenty-one to sixty years old. Half identified as female and half as male. Half identified as Black with no Hispanic/Latino ethnicity and half as Hispanic/Latino only. Participants’ education ranged from less than a high school diploma to some college (Table 1).
Characteristics of IHO Worker Participants (N = 10), North Carolina, 2014.
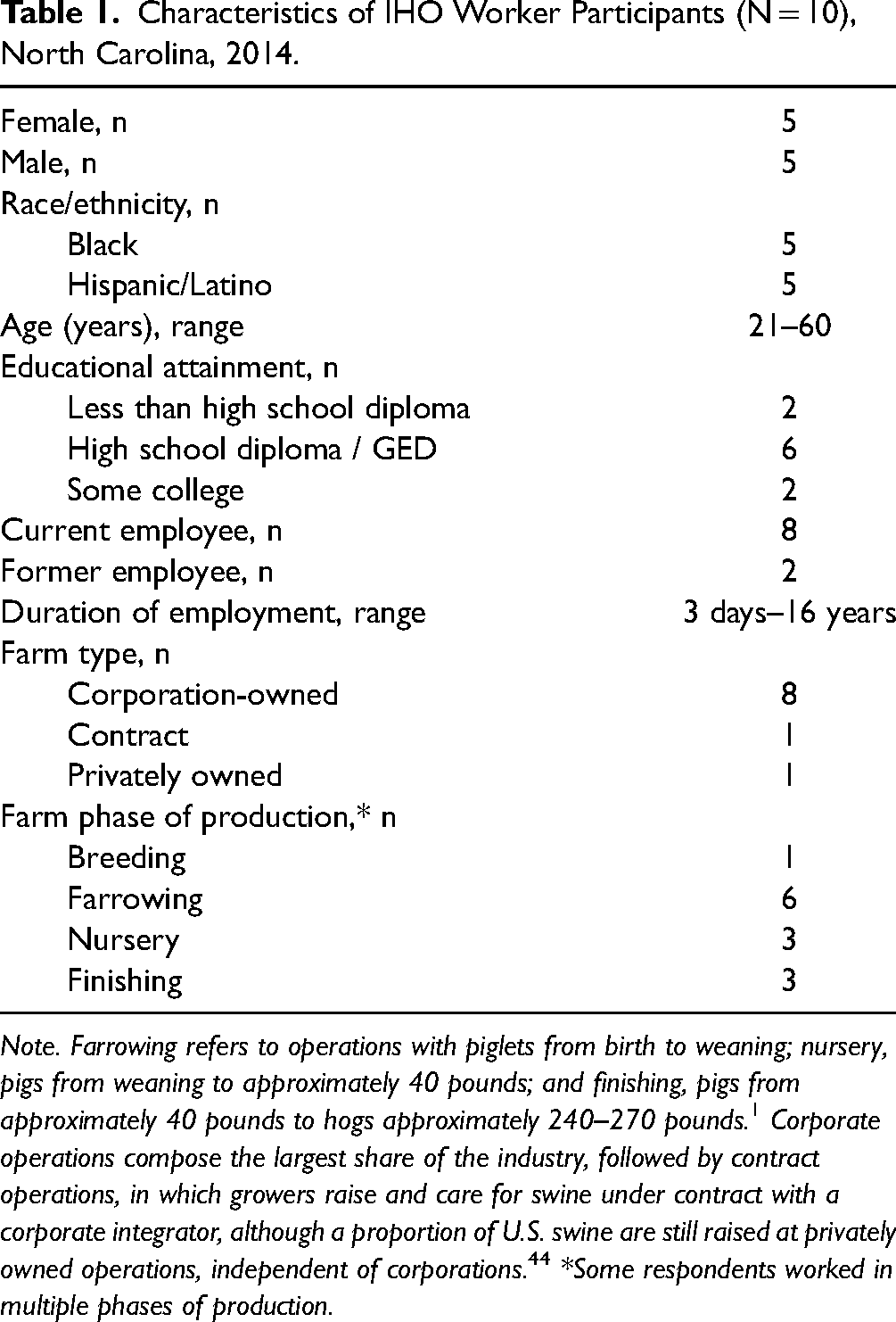

Note. Farrowing refers to operations with piglets from birth to weaning; nursery, pigs from weaning to approximately 40 pounds; and finishing, pigs from approximately 40 pounds to hogs approximately 240–270 pounds. 1 Corporate operations compose the largest share of the industry, followed by contract operations, in which growers raise and care for swine under contract with a corporate integrator, although a proportion of U.S. swine are still raised at privately owned operations, independent of corporations. 44 *Some respondents worked in multiple phases of production.
Potential occupational exposures to livestock-associated microbes in IHOs
Participants described a variety of opportunities for microbial exposure in the workplace, including inhalation exposure via malodor and dusty work conditions, ingestion exposure at lunch canteens near swine and swine waste, and dermal exposure via physical contact with swine while performing work tasks.
Nearly all participants commented on noxious smells associated with the swine or swine waste. One explained, “It just stinks really bad! I can’t really compare it to anything,” adding that she experienced decreased appetite and increased headaches since starting work at the IHO (Participant 1). A finishing worker associated malodor with nausea and headache: “I mean, you have the smell, what gets me in the morning, because if you go on an empty stomach, you’ll feel kind of nauseated, head will be hurting” (Participant 2). The same participant added that some other workers became sick “from the smell, like vomiting” when unloading swine at the operation. A third participant also described feeling sick from the smell and increased frequency of headache (Participant 8). A finishing worker associated IHO dust and hog urine odors with eye and throat irritation: I do get bothered by dust or the [hog] urine. I feel like [the urine] affects me the most … especially during summertime I guess because of the heat. Urine gets into me, and it irritates my eyes and makes my throat itchy, and I’ll start with the coughing. Bothers my chest also. I continue with the coughing like throughout the whole day and sometimes half of the next one. (Participant 5)
Three workers described the lunch canteen as being very close to the hogs and having bad smells. A finishing worker described the canteen location: Yeah, [the canteen] is not even about 5 to 6 steps from where the hogs, where the truck comes in, and the canteen room is about 7 or 8 steps across from that, so you can still smell it by you sitting down in there, eating. (Participant 2)
Participants also described opportunities for exposure to microbes through physical contact with swine, which we categorized as “direct contact,” i.e., physically touching the animals with or without protective gear, versus “indirect contact,” i.e., contact with things that have directly touched the animals (Table 2).
Circumstances of Direct and Indirect Worker Contact with Swine, North Carolina, 2014 (N = 10 Participants).

Circumstances of direct contact included when swine were sick. Participants reported contact while checking for fever and giving medication to swine by mouth or injection. One farrowing worker commented, “When they have scours [diarrhea], I put medicine for the mouth… when I [give shots] to the little pigs, sometimes the pigs move, and sometimes I accidentally poke myself” (Participant 6). While he had not done this task himself, a finishing worker described how skin infections on swine are handled: “the part that's abscessed, they cut it off. They cut that part–cut around that part, spray it off with a water hose” (Participant 8). Participants also reported direct contact with animals when killing sick swine and removing the dead swine from pens, as well as while assisting with births and newborns, and while moving swine (Table 2).
A few participants reported unintentional direct contact with hogs when the animals behaved in unexpected ways. A finishing worker described concerns around unintentional contact: Sometimes you might get in a jam, and sometimes your glove might go. Some of your skin might be showing, so you never know because you’re dealing from a small to a big animal; you might catch a cramp, anything … It's a lot of hogs that have abscess on them, and they spread. And I’m scared of it when the hogs get big because they cut up in those pens. I mean they run you over. Seem like they try to bite you sometimes. You got like a 400-pound animal in there. I’m like 170 pounds and you know that animal is big and you got two or three of them in a pen and they’ll try to box you in. (Participant 8)
A farrowing worker described unintentional direct contact on multiple occasions, including a condition requiring medical treatment: “a big momma [sow] hurt my leg…and the doctor said my ligament was broken” (Participant 4). On another occasion when she was taking a temperature, she said “a sow hit my wrist” (Participant 4).
Participants also described indirect contact through swine waste and while spraying swine or pens. A finishing worker noted infection as a risk related to indirect contact: I knew one girl, she was breaking out, she’d been there longer than I have, and she was telling me about the infection that she would catch from the hogs, and if they come in with red spots all over them, and if you touch them, you don’t have to actually touch them, you can be spraying them down, the water off them get on your skin, that would get in your skin, and it infects your skin also … Your ears don’t be covered. So the water can bounce off on your ears or your forehead. And your neck don’t be covered up neither. (Participant 2)
Another finishing worker also noted indirect contact while washing swine pens: “It [water] can hit your face and stuff and then you’ll probably break out” (Participant 8).
Take-home practices
Workers described a variety of practices during transitions from work to home that could affect transfer of microbes from IHOs to families and communities (Figure 1). “Take-home” refers to how respondents and coworkers manage their work clothes and hygiene practices before and after work. “Work clothes” include smocks or coveralls and PPE, such as gloves, boots, and face masks. It may also include personal clothes that get soiled or wet at work.
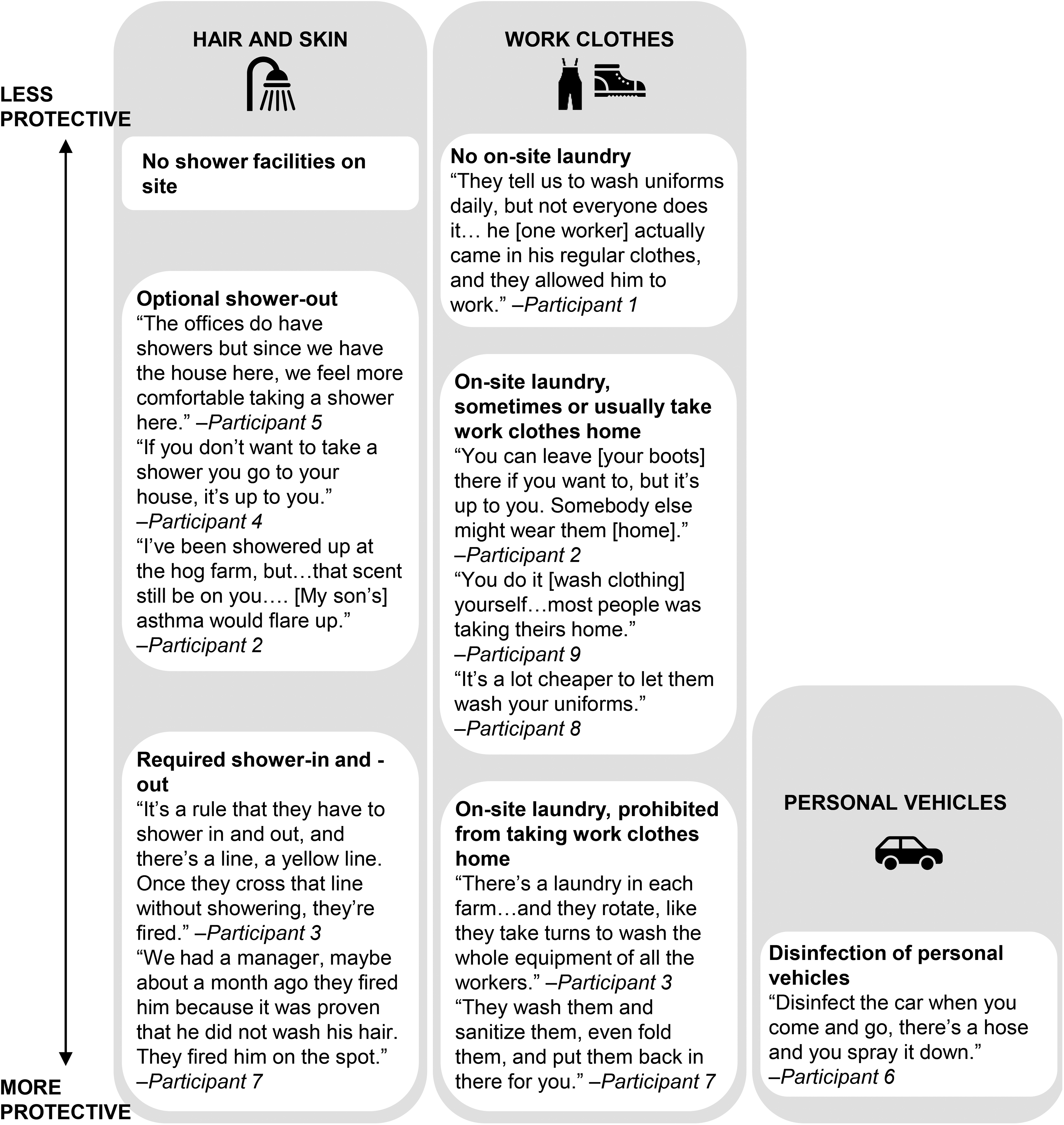
Take-home practices related to risk of transfer of livestock-associated microbes from work to home, grouped by potential exposure pathway (worker hair and skin, work clothes, worker personal vehicle) and arranged from less to more protective in terms of reducing risk of transfer of livestock-associated microbes from work to home, North Carolina, 2014 (N=10 participants). Note. Overalls icon from the Noun Project. 45
Participants described a range of showering facilities and requirements. One worker reported no showering facilities, and several reported required shower-in upon arrival at the facility to prevent transmitting disease to livestock, but no required shower-out after work. A few reported showering at home after work for convenience or comfort. Even without a shower-out requirement, a few workers reported showering at work before they left, including a finishing worker who does so as well as showering a second time at home, because lingering malodor from the operation affected her school-age son's asthma: I’ve been showered up at the hog farm, but they don’t have, like, good soap and stuff like that. They just have…like a cheap spray on foam. But when you get home, you have to set your clothes out, I mean, you already have your clothes off, but just to have that scent still be on you…. [My son's] asthma would flare up…. He’d have to take two puffs. (Participant 2)
Several participants reported strictly enforced shower-in and shower-out policies with penalties for non-compliance. Similarly, participants reported a range of policies and practices regarding laundering and storing work clothes. The same participant who reported no shower facilities also reported no on-site laundry and said workers were advised to take their coveralls home or elsewhere to wash daily and bring them back, “but not everyone does” (Participant 1). This participant—a worker at an IHO with approximately 80 employees—noted “incidents where people came in missing parts of their uniform and still are able to work.” She described one worker arriving without coveralls and boots working in his regular clothes, rather than being provided with appropriate PPE. She also wondered why another employee reported to work without his uniform and “they told him to go home.”
Several participants described on-site laundry and storage facilities, but limited use. A farrowing worker explained that because employees were told to launder clothes on their own time, “most of them was taking theirs home” (Participant 9). In contrast, a finishing worker reported always keeping work clothes at work because “it's a lot cheaper to let them wash your uniforms” (Participant 8). Even though coveralls were washed at work, that participant reported personal clothes getting “soaked” several times a day from spraying down the swine. Another finishing worker explained why she typically took work boots home, “You can leave [your boots] there if you want to, but it's up to you. Somebody else might wear them [home]” (Participant 2). Several participants described requirements to use on-site laundry and storage facilities or prohibitions on bringing work clothes off the operation. After a porcine epidemic diarrhea (PED) outbreak, one farrowing worker also described a requirement to wash even personal vehicles before leaving the IHO property, “Disinfect the car when you come and go, there's a hose and you spray it down” (Participant 6).
Discussion
This qualitative pilot study describes the experiences of IHO workers, illustrating varied circumstances of worker contact with swine and take-home practices. Most participants described direct contact with swine which could put them at risk of exposure to zoonotic pathogens and microbes, including during intensive direct contact tasks that can cut or lacerate workers’ skin and produce other skin injuries—e.g., providing oral or intravenous medications, restraining and shooting swine, handling dead swine, assisting with births, and conflict with swine when managing pens. Many activities involved interactions with sick swine, further increasing the potential risk of zoonotic pathogen transmission and infection. Participants also discussed take-home practices related to showering, work clothes and PPE, and personal vehicles that could contribute to the transfer of livestock-associated microbes, including zoonotic pathogens, from IHOs to families and communities. These IHO workers’ experiences could begin to explain others’ findings of elevated prevalence of S. aureus, MRSA, and MDRSA among children of IHO workers compared to children living in nearby households with no known occupational exposure to livestock.20,21
Policies to limit the use of antimicrobials in IHOs could reduce worker risk of MRSA, MDRSA, and other antimicrobial-resistant zoonotic pathogen exposures. Interventions to reduce antimicrobial use in food animals are associated with reduced antimicrobial-resistant bacteria in both animals and humans, especially humans in direct contact with the animals. 46 California banned both antimicrobial use for animal disease prevention and any antimicrobial use without a veterinarian's prescription in 2018. 18 An analysis by Casey et al. associated this legislation with a reduction in antimicrobial resistance of human urine sample E. coli strains. 18 Another policy tool is mandatory monitoring or reporting, which has had some success in the European Union (EU). 17 The EU has also established a process to withdraw certain antimicrobials from use in food animal production entirely. 17 Similar policies could also be beneficial in the U.S., particularly for medically important drugs with limited alternatives. Antimicrobials are important for treating livestock diseases. However, limiting use and requiring veterinary supervision could help prevent the development of antimicrobial resistance and transmission to workers. Other methods, such as vaccination, livestock production facility management, and biosecurity, could also be used to help control the spread of disease. 47 Vaccines can reduce the need for antimicrobial use by preventing infections. Reducing crowding, providing appropriate housing, and maintaining feed hygiene can also promote animal health and reduce the spread of pathogens. 47 Biosecurity measures and practices to keep disease away from livestock, including keeping visitors to a minimum and cleaning any tools or equipment transferred between operations, can reduce the risk of pathogens being introduced to and spreading among livestock. 47
Adequate information and training is necessary to protect IHO workers from hazards, including zoonotic pathogens. Our results suggest such training and information is lacking in some IHO environments. For example, some respondents described not expecting direct contact during certain high-risk work tasks (e.g., entering pens to feed swine, moving swine) which might reduce their likelihood of using adequate PPE. Further, some workers seemed to perceive high-risk tasks (e.g., touching dead swine) as routine or low-risk, and therefore could be minimizing associated zoonotic pathogen transmission risks and the need for precautions. This could result in employer violations of OSHA's PPE standard, which requires PPE provision, maintenance, and use “wherever it is necessary by reason of hazards of processes or environment.” 48 This finding also aligns with current literature, including a survey of Missouri hog workers which found that a majority of workers did not perceive their job as dangerous, despite 33 percent reporting an occupational injury and 28 percent reporting occupational health problems such as headache, coughing, congestion, and nausea. 9 This study, combined with consistently reported high rates of injury and illness, 3 suggests a need for improved safety training around both microbial and injury risks in IHOs.
Injury from animal handling is a major risk of IHO work, 9 and our results suggest that circumstances presenting injury risks might also present microbial risks for workers. For example, a worker expressed concern about contracting an infection from hogs with abscesses while she risked being pinned or trampled when entering hog pens. Hence, interventions to reduce the risk of physical injury could also reduce the risk of pathogen transmission from swine to workers.
Nearly all participants described challenges with malodor at the IHO. Some described the location of their lunch canteen as steps away from the swine and noted bad smells while eating. Air and fomites represent transmission routes for livestock-associated, antimicrobial-resistant S. aureus.49–53 These reported IHO workplace conditions represent another opportunity for transmission of livestock-associated microbes via aerosols or surfaces. Participants attributed symptoms of infection and respiratory disease to inhaling dust, smelling swine urine, and dermal contact with water from washing swine or pens. The circumstances of IHO workers’ contact with swine, especially those that workers connected with symptoms, could be avenues for future research to better understand and prevent livestock-associated microbial transmission and infection at IHOs and in surrounding communities. For example, workers’ concerns about infection while spraying swine suggest future research could monitor farm surface water or measure airborne microbes during that task.
In terms of take-home pathway mitigation, participants reported varied shower policies and practices. Mandatory shower-out after work has been associated with reduced risk of take-home exposures to pesticides related to farm work as well as toxic metals related to e-waste recycling work. 37 Yet, participants described shower-in policies as more common and more strictly enforced when compared to shower-out policies, suggesting IHO management could be more concerned with biosecurity and livestock disease control than workers’ individual and take-home exposures. Facility shower quality, conditions, and convenience also presented barriers to shower-out that could be remedied. One participant remarked on inadequate soap and lingering malodor after showering at the facility where she worked. This is consistent with the research of Leedom Larson et al. 54 which found that, across six swine production operations, MRSA-positive shower samples varied from 0 percent to 26 percent.
Participants also reported varied practices around taking home their work clothes, including PPE. Our findings are consistent with previous studies which found that prevalence of S. aureus, MRSA, and MDRSA was higher among children of IHO workers who reported taking home PPE than among the children of those who did not, suggesting take-home practices around work clothes modify the transfer of microbes from IHOs to homes.20,21 One participant reported a worker arriving without boots and coveralls and working in regular clothing rather than being provided the appropriate PPE. This could put the worker at risk and facilitate take-home exposures. While employers at that operation provided PPE, in accordance with OSHA general requirements, 48 they did not provide laundry facilities—workers were instructed to take home PPE, wash it, and bring it back the next workday. The situation she described may have been a violation of OSHA's PPE standard, which requires maintenance and use of appropriate PPE.48,55 To better ensure employees always work with adequate PPE, and limit take-home exposures, OSHA should add language to the standard requiring provision, cleaning, and maintenance of all PPE at the worksite. Even in the absence of a clearer standard, employers should make it possible for employees to work with appropriate PPE by providing clean PPE on site.
A participant reported taking home work boots because of concerns about secure storage. If employees are required to wear protective clothing, OSHA requires employers to provide change rooms with storage facilities for street clothes separate from storage for work clothes and PPE. 55 OSHA could improve this standard by adding language requiring secure storage, rather than storage space alone, to promote storage facilities use and limit take-home exposures. In addition, OSHA should require shower facilities between work clothes storage and street clothes storage areas to engineer separation of potentially contaminated work clothes and street clothes. Reconfiguring facilities might be difficult and costly for smaller IHOs. In addition, there might be little OSHA monitoring and enforcement because operations with ten or fewer employees, not including immediate family members, are neither inspected by OSHA nor subject to recordkeeping requirements. 56 The exemption for workplaces with ten or fewer employees and exclusion of immediate family members from consideration as employees limits employer health and safety accountability at smaller IHOs. 57 This could be the case for the contract and privately owned operation workers in our interviews. Federal and North Carolina OSHA offer no-cost, confidential consultations, primarily for smaller businesses, to help identify and address hazards.58,59 OSHA consultations could be an opportunity for IHOs, especially smaller operations, to improve workplace safety.
One participant reported a requirement during the PED outbreak to wash boots and cars when entering and leaving the IHO property as a biosecurity and livestock disease control measure. Facilities and policies for livestock disease control can also benefit workers and families. Future research on biosecurity measures could also include investigation of livestock-associated and antimicrobial-resistant pathogens among workers and household members.
A strength of this study is our collaboration with our community research partner, REACH, facilitating recruitment of IHO workers representing a range of characteristics—age, gender, race, ethnicity, operation type, and job activity. A community-driven research framework can facilitate the participation of individuals who might otherwise decline to participate, enriching the data, and facilitating the identification of IHO worker experiences that represent deviations from best management practices and policies.60,61 We believe this was true in this study, in which participants described a range of possible workplace pathways of exposure for further study.
A limitation of the study is the relatively small number of interviews. It is customary for researchers engaged in qualitative interviewing to complete data collection when they determine they have reached saturation and nothing new or contradictory is emerging from the interviews. 62 While we believe more in-depth interviews with IHO workers may have produced additional information on the study topic, concerns about employer retaliation and limited resources prevented us from conducting additional interviews. Even so, our sample of 10 respondents represents a range of IHO worker characteristics, and their responses highlight potential pathways of exposure to zoonotic pathogens.
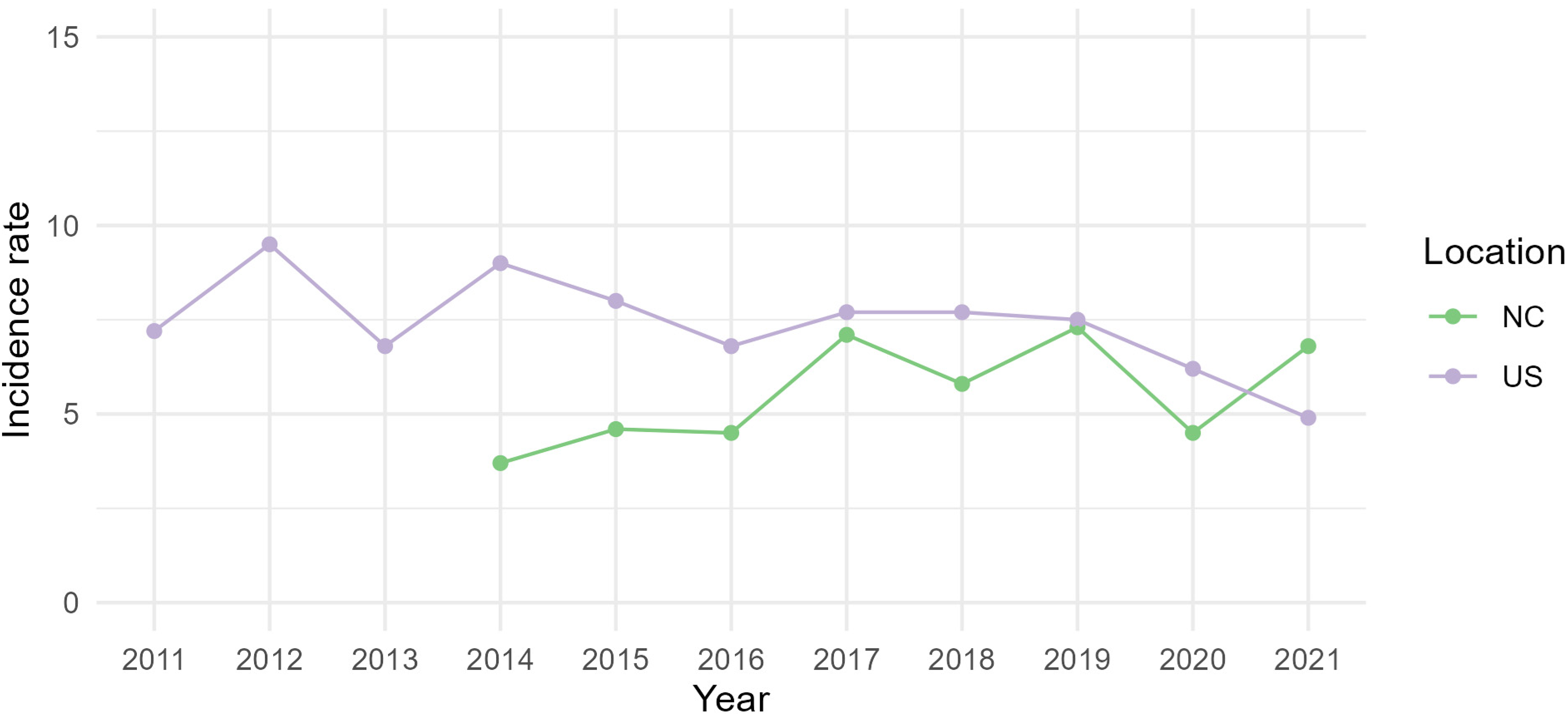
Another limitation of this study is the amount of time that has passed since the interviews were conducted in April 2014. However, the interviews are likely to reflect current reality because IHO workplace conditions may not have significantly changed or improved. There has been little improvement since 2014 in the high incidence of reported injuries and illnesses at work over time among North Carolina hog industry workers (Figure 2). Moreover, the occupational safety and health regulatory landscape has not changed appreciably since interviews were conducted. Only six of OSHA's more than 100 health and safety regulations affect agricultural workers specifically, and there is no occupational infectious disease standard.63,64 This slow pace of change is typical of OSHA. A review by the U.S. Government Accountability Office found that between 1981 and 2010, it took OSHA an average of more than 7 years to develop and issue safety and health standards. 65
We also believe this research still provides valuable information because of limited literature on IHO worker health. Concern about industry retaliation or litigation makes studying IHO workplace and take-home hazards difficult.61,67 Many IHO workers are vulnerable socially, economically, and legally (due to challenges related to immigration status or employer-based sponsorship). 68 Thus, they face greater occupational risks and can be more difficult to reach for health research. Participants’ descriptions of the workplace environment, direct and indirect contact with animals, and take-home practices suggest a variety of exposure routes by which workers and their household members could encounter IHO-related and antimicrobial-resistant microbes.
Conclusions
This research provides insights into IHO workers’ experiences that could contribute to their own and their household contacts’ exposure to zoonotic pathogens. Our findings suggest a need for greater attention to workplace and take-home practices and policies that could prevent livestock-associated microbial exposures among IHO workers. Participants recognized the health hazards of interacting with sick animals and potentially bringing home dirt, dust, and zoonotic pathogens that might pose health risks to themselves and their family members, including skin infections and asthma exacerbations. Participants’ descriptions also represent a variety of plausible take-home microbial exposure pathways from their work at IHOs that could be investigated as points of intervention to reduce transmission and infection opportunities. More rigorous and consistent health and safety policies and practices across all IHOs could afford greater protection of IHO workers and their household and community contacts from zoonotic pathogen exposure and other hazards associated with swine contact.
Supplemental Material
sj-docx-1-new-10.1177_10482911231217055 - Supplemental material for Industrial Hog Operation Workers’ Perspectives on Occupational Exposure to Zoonotic Pathogens: A Qualitative Pilot Study in North Carolina, USA
Supplemental material, sj-docx-1-new-10.1177_10482911231217055 for Industrial Hog Operation Workers’ Perspectives on Occupational Exposure to Zoonotic Pathogens: A Qualitative Pilot Study in North Carolina, USA by Carolyn Gigot, Amy Lowman, Caitlin A. Ceryes, Devon J. Hall and Christopher D. Heaney in NEW SOLUTIONS: A Journal of Environmental and Occupational Health Policy
Footnotes
Acknowledgements
This research would not have been possible without a strong partnership between researchers and community-based organizations that have the trust of members of communities in areas where the density of industrial hog production is high. We thank the workers who participated in this study and all the REACH community organizers who worked on this project, especially Norma Mejia, Martha Paez, and Revenda Ross. We also acknowledge Dr. Meghan Davis for assistance with background information.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute for Occupational Safety and Health (NIOSH, grant number K01 OH010193-01A1), National Institute of Environmental Health Sciences (R01 ES026973 and P30 ES032756), Thrasher Research Fund (E.W. “Al” Thrasher Award 10287), National Institute of Allergy and Infectious Diseases (R21 AI139784), Johns Hopkins NIOSH Education and Research Center (T42 OH0008428), National Science Foundation (1316318), GRACE Communications Foundation, and Johns Hopkins Center for a Livable Future (CLF-Lerner Fellowship).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
