Abstract
Chlamydiae are reported to cause abortion in several species, however the association between Chlamydia sp. and equine abortions is poorly understood. A zoonotic transfer event of C. psittaci from aborted equine tissues in Australia has emphasized the need to better understand the prevalence of this pathogen in equine populations. The prevalence of chlamydia in equine abortions in North America has not been investigated thoroughly. We examined 99 formalin-fixed, paraffin-embedded placental samples submitted between 2009 and 2020 from equine abortions in Western Canada using chlamydia-specific 16S rRNA conventional PCR testing; 26 of 99 submissions tested positive for chlamydial DNA. Most of these submissions (n = 17) had no final diagnosis noted on their original pathology reports. DNA sequencing identified 22 of the 26 cases as C. abortus; 21 of the 22 C. abortus–positive samples were positive on chlamydial immunohistochemistry. These findings contrast with studies in Europe that found a low prevalence of chlamydiae using similar methodology. The high prevalence of the potentially zoonotic C. abortus identified in our study suggests that more substantial biosecurity protocols may be warranted for equine foaling, abortion, and stillbirth in Western Canada to prevent zoonotic transfer of the pathogen.
Chlamydiales is an order of obligate intracellular, gram-negative bacteria with a diverse host range. 9 Chlamydia abortus, the causative agent of enzootic abortion, has been associated frequently with abortions in sheep, cattle, goats, and swine, causing significant economic losses.9,17 Interestingly, most previously reported chlamydial abortions in horses have been attributed to C. psittaci, with only occasional reports of C. abortus.5,6,14,24 C. psittaci is the causative agent of psittacosis in birds, primarily causing pneumonia, hepatitis, and enteritis. 9 The pathogenesis of these equine abortions is unknown, but transmission is presumed to be through contact with bird feces. 9 Other potentially zoonotic organisms detected in equine abortions include Neospora sp., Coxiella burnetii, and Leptospira sp. 3 Toxoplasma gondii has also been reported in aborted equine fetuses under experimental conditions. 18
Interest in chlamydiae as abortigenic pathogens has increased following cases of zoonotic transfer of C. psittaci from aborted fetal membranes to students and staff at a veterinary school in New South Wales, Australia in 2014. 11 In this event, 5 of the 9 individuals exposed to contaminated fetal membranes developed symptoms of psittacosis, indicating a potential association between fetal membrane exposure and C. psittaci infection. 11 The most likely routes of transmission were identified as either airborne or direct exposure of the pathogen to the eyes or nose. 11 Precise identification of the pathogen using serology was unsuccessful, leading investigators to suggest that psittacosis may be under-diagnosed, either because of mild symptoms not warranting medical care, inadequate sampling, or samples not being taken as a result of a low suspicion for psittacosis. 11 These factors suggest that cases of psittacosis associated with equine abortions may have gone unreported. 11
Further investigation into equine abortions in Australia revealed that 6.5% of submissions analyzed between 1994 and 2019 were C. psittaci–positive, and that cases occurred in other Australian states.2,16 Through sequence typing, researchers identified that the strain of C. psittaci implicated in several equine abortions clustered with the avian 6BC clade, and were closely related to strains found in pigeons. 16 Pigeon-like strains are considered highly transmissible to humans, which may have contributed to the large number of individuals affected in the event described above. 16 Based on these results, the researchers encouraged more specific testing for this pathogen, given that it is not typically included in routine testing of equine abortion submissions. 2
Historically, the role of chlamydiae as abortigenic pathogens in horses has been controversial. 28 Investigators in the United States and Germany found a high prevalence of chlamydiae in aborted equine tissues, 55% and 27%, respectively.7,12 Studies in Hungary found 83% of tested equine aborted tissues positive for chlamydiae. 24 In contrast, other studies in Germany, Switzerland, and Denmark have identified few or no cases of chlamydial infection.1,5,14,21
Given the contrary findings in Europe, and identification in Australia, further investigation into the situation in North America is warranted. Our search of PubMed, Google Scholar, ScienceDirect, SAGE Journals, Scopus, Wiley Online, and Web of Science revealed one North American study identifying chlamydiae as abortigenic agents in horses. 12 To our knowledge, chlamydiae have not been reported as equine abortigenic agents in North America since 1985. 12 Because both C. abortus and C. psittaci are zoonotic agents, understanding the risk of exposure when handling equine aborted tissues is of utmost importance. We investigated the presence of chlamydiae in equine aborted tissues submitted from British Columbia, Alberta, Saskatchewan, and Manitoba. We expected to find only occasional cases, similar to studies in Germany, Switzerland, and Denmark.
Materials and methods
We manually identified equine abortion cases submitted between 2009 and 2020 from the database of Prairie Diagnostic Services (PDS) in Saskatoon, Saskatchewan, Canada, and recovered 218 cases. We reviewed the autopsy reports for all submissions and removed those without placental tissue submitted from our study. We randomly selected 100 submissions using simple random sampling from the remaining pool of 186 submissions. Of the 100 submissions selected, 73 had no final diagnosis, 12 were attributed to noninfectious fetoplacental causes of abortion, such as umbilical cord torsion, 11 were attributed to equine herpesvirus 1 (Equid alphaherpesvirus 1), and 4 were attributed to bacterial infections. For each randomly selected submission, the full set of histologic slides was retrieved and examined by a veterinary pathology resident. Given that chlamydiae commonly cause lesions in the placenta in other species, the slides containing chorioallantoic placental tissues were identified, and those formalin-fixed, paraffin-embedded blocks from these submissions were retrieved. Given the nature of trimming samples, the slides with placental tissues occasionally contained other fetoplacental tissues, including amnion and fetal organs.
DNA retrieval was performed using a method described previously. 29 Briefly, five 20-µm shavings were sequentially removed from the blocks using a microtome and deparaffinized by 2 xylene washes. A 100 mM NaCl, 500 mM Tris, and 10% sodium dodecyl sulfate lysis buffer solution and 5 µL of proteinase K were added to the deparaffinized tissue for DNA extraction. The samples were incubated at 56°C overnight. Proteins were subsequently removed using phenol–chloroform–isoamyl alcohol. The remaining DNA was precipitated using 2 volumes of 100% ethanol and 0.1 volumes of 3 M sodium acetate. Each sample was resuspended in 50 µL of Tris-EDTA buffer before reading nucleic acid concentrations (NanoDrop 2000C spectrophotometer; Thermo Scientific). The presence of amplifiable DNA was confirmed for all samples by performing PCR with primers for the beta-actin reference gene, as described previously. 29
For detection of chlamydiae, PCR primers 16SIGF/16SIGR (16SIGF: 5′-GATGAGGCATGCAAGTCGAACG-3′; 16SIGR: 5′-CCAGTGTTGGCGGTCAATCTCTC-3′) were used. 8 The primers target a conserved region of the 16S rRNA gene, producing a 278-bp fragment. A 50-µL PCR reaction was performed using 2 µL of sample DNA with 3.5 µL of 3.5 mM MgCl2, 2 µL of 0.4 mM of deoxyribonucleotides (dNTP; Thermo Scientific), 5 µL of 1.0 µM of each forward (16SIGF) and reverse (16SIGR) primer (Sigma Life Science), 2 U of DNA polymerase (Quantabio), and distilled water to complete the 50-µL volume. PCR cycling was completed (Mastercycler; Eppendorf). The initial denaturation step was 15 min at 95°C, followed by 45 cycles of denaturation at 94°C for 30 s, primer annealing at 70°C for 30 s, and extension at 72°C for 45 s. A final extension step of 5 min at 72°C completed the reaction.
Each amplification product was electrophoresed on 1.2% Tris-EDTA agarose gel, with ethidium bromide staining. For each PCR batch, a blank wax negative control, blank extraction negative control, and no template controls were included; 2 samples from PCR-confirmed submissions of sheep abortions were used as positive controls. The gels were examined for bands under UV light. Test samples were considered positive for chlamydiae if a band was seen at ~278 bp, consistent with the positive controls. All of the positive test samples were purified (PCR purification kit; Qiagen) and quantified (NanoDrop 2000C spectrophotometer). The samples were sequenced (Macrogen) and compared with the bacterial sequences in GenBank through Blast analysis (https://blast.ncbi.nlm.nih.gov/Blast.cgi). For each submission, the Blast result with the smallest E-value was selected as the most likely bacterial species.
Immunohistochemistry (IHC) using a mouse anti-chlamydial antibody (Pennsylvania State University) was completed on samples testing positive for chlamydiae on PCR and identified as C. abortus on sequencing. Staining was performed using an automated slide stainer (Agilent). Epitope retrieval was performed using a proteinase K (Agilent) treatment, followed by incubating the primary antibody at a 1:5,000 dilution at room temperature for 30 min. A biotinylated secondary antibody (Vector) and avidin-biotin immunoperoxidase complex reagent (Vector) were used to identify binding of the primary antibody. Stained slides were examined by a veterinary pathology resident to assess positive antibody staining. Three randomly selected samples that tested negative for chlamydiae on PCR were also stained to act as a negative control.
Aspects of the submission history, if provided in the autopsy report, were categorized for further analysis. Dam breed was classified into one of the following categories: donkey, baroque, light pleasure, draft, Miniature Horse, Standardbred, stock horse, Thoroughbred, Warmblood, pony, and other. The age of the dam was categorized into 4 age ranges: young mares < 8-y-old, mature mares ≥ 8–13-y-old, aging mares 14–18-y-old, and senior mares ≥ 19-y-old. Gestational length was categorized as early gestation at 2–5 mo, mid-gestation at 6–8 mo, and late gestation for all submissions aborting after 8 mo. Dam parity was categorized in maidens, with no previous pregnancies, and multiparous mares. Breeding method was categorized as natural breeding, artificial insemination, or embryo transfer.
Results
We found amplifiable DNA in 95 of the submissions on conventional PCR using primers for the beta-actin reference gene. We selected 5 additional submissions from the remaining pool to replace the 5 submissions without amplifiable DNA. Of these 5 additional submissions, only 4 had amplifiable DNA, making the final total 99 submissions; 26 of the submissions tested positive for Chlamydia sp. on conventional PCR (Fig. 1). Positive submissions were submitted from all 4 western Canadian provinces (Alberta, British Columbia, Manitoba, Saskatchewan), with positive cases in every year between 2009 and 2019; 2020 had no positive submissions within our random sample.
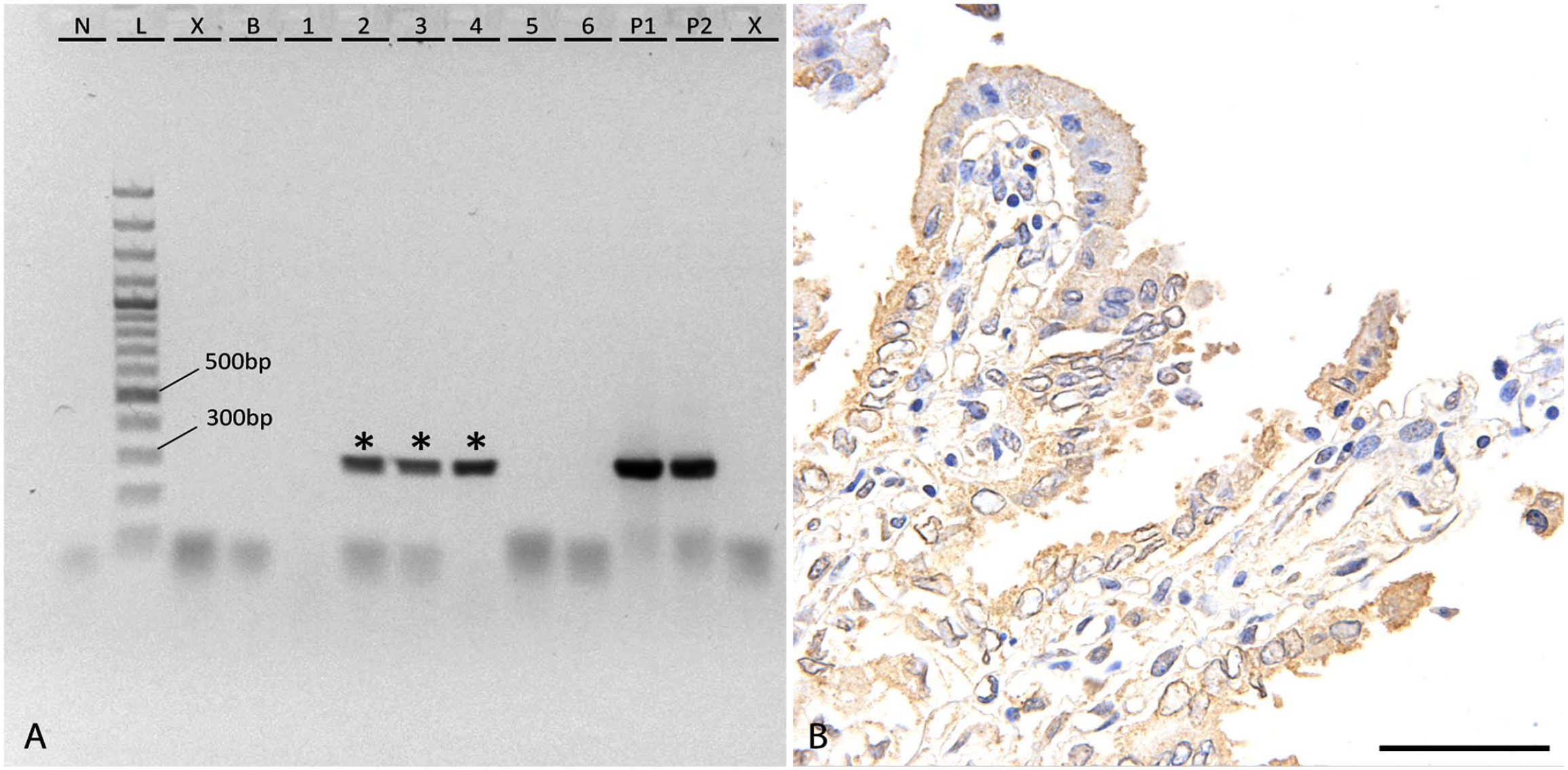
Detection of Chlamydia abortus in aborted chorioallantoises of horses from Western Canada.
Most of the positive submissions did not have a final diagnosis on their autopsy report (n = 17; Table 1). The proportion of undiagnosed, test-positive submissions versus diagnosed, test-positive submissions was not statistically different from the test-negative groups on a Fisher exact test (p = 0.451).
Final diagnoses listed on the autopsy reports of 26 equine abortion submissions that were positive for Chlamydia sp. on conventional PCR, and distribution of Chlamydia sp. identified for each final diagnosis.

Only one submission had bacterial culture performed; Streptococcus equisimilis was identified. The remaining 2 submissions were presumed cases of bacterial placentitis.
Approximately half (n = 14) of the chlamydia-positive submissions had a bacterial culture done as part of their initial diagnostic workup; 2 of the submissions had potential abortigenic bacteria identified: Streptococcus dysgalactiae subsp. equisimilis and alpha Streptococcus species. All of the bacterial cultures completed on positive submissions identified organisms, but the organisms were considered insignificant by the reviewing microbiologist and pathologist. Bacterial species identified included Escherichia, Enterobacter, Bacillus, Streptococcus, Acinetobacter, and Pseudomonas.
Of those submissions with a gestational length provided, 11 of the chlamydia-positive submissions were late-pregnancy abortions, although 1 submission was identified in early-gestation and 7 in mid-gestation. The proportion of chlamydia-positive submissions in early-, mid-, and late-gestation was not significantly different from the chlamydia-negative submissions on a Fisher exact test (p = 0.910). There were no statistically significant differences in proportions of chlamydia-negative and -positive submissions based on dam age group (p = 0.739), fetal sex (p = 0.685), dam parity (p = 1.000), breeding method (p = 0.325), or dam breed category (p = 0.262).
Sequencing of the 26 chlamydia-positive submissions identified 22 cases of C. abortus with over 95% identity (GenBank NZ_LS450958.2). The remaining 4 submissions were not successfully identified because of a low identity percentage (80–85%) and were considered chlamydia-like bacteria (Table 1).
Of the C. abortus submissions with an autopsy completed, 14 of 18 did not have any gross lesions. Of the 22 C. abortus–positive cases, 21 cases had completed histology reports; 7 of these reports identified no abnormal findings or listed no significant findings without further detail. The most common gross finding was thickening of the placenta (n = 3), with 1 submission of edematous placental tissue. The most common histologic placental findings were mineralization (n = 9), neutrophilic inflammation (n = 5), and hemorrhage (n = 4). In the cases with neutrophilic placentitis, the inflammation was frequently described as multifocal and widespread, with one report specifically indicating that the cervical star and the non-pregnant horn were affected.
On IHC, 21 of the 22 C. abortus PCR-positive samples were positive for Chlamydia sp. (Fig. 1). The chlamydial antigen primarily appeared as small aggregates of stained proteins within the cytoplasm of trophoblasts. The proteins were frequently arranged along the apical border of the cell. Occasional cells had diffuse staining of the cytoplasm with few discernible aggregates. The trophoblasts at the tips of the chorionic villi were more strongly antigenic in most submissions, with occasional submissions having diffuse staining of all trophoblasts. The final submission that tested PCR-positive for C. abortus had no chorionic villi present in the submitted section; therefore, antigenic staining of the chorionic epithelial cells could not be confirmed. The 3 negative control samples had minimal stain uptake within the cytoplasm of trophoblasts.
Discussion
The finding of 26 chlamydia-positive submissions in a pool of 99 samples was unexpectedly high, particularly compared to reports from Germany, Switzerland, and Denmark.1,5,14 The high prevalence of C. abortus is particularly interesting, given that this pathogen has only been reported as an occasional cause of equine abortion.5,13,26 Having no detections of C. psittaci was expected, consistent with the low prevalence identified in European studies.1,5,14
Other than one previous report, 12 there has been little investigation into chlamydiae as equine abortigenic pathogens in North America. The authors 12 examined fresh or frozen tissues for the pathogen, using Gimenez stain, immunofluorescence, and inoculation of embryonated eggs, and reported a prevalence of 55%, which is much higher than the prevalence that we found. The formalin-fixation process used to preserve the tissues in our study can cause DNA fragmentation, which can prevent appropriate binding of PCR primers; without primer binding, false-negative results can occur. 5 Therefore, our study likely underestimates the overall prevalence of chlamydiae in aborted equine tissues, compared to the study on fresh tissue. 12
All of the cases in a 1985 study were identified as C. psittaci. 12 C. abortus was distinguished as a unique species in 1999, separating it from C. psittaci. 13 Without sequencing data from the 1985 study, it is difficult to know whether the pathogen identified was C. psittaci or C. abortus under the new classification. Similar to our study, 45.5% of the chlamydia-positive cases had no significant gross or microscopic lesions. 12 Comparing the overall prevalence and histologic findings between the 2 studies, it can be postulated that the cases of C. psittaci identified earlier 12 may have been cases of C. abortus. However, given the high similarity of the 16S rRNA gene between C. psittaci and C. abortus, it is also possible that the cases identified in our study are cases of C. psittaci if the relatively short length of the amplicon produced by our primers was insufficient to properly distinguish between the 2 species. Repeated investigation into the prevalence of chlamydiae in horses in North America would be prudent, based on these results.
The pathogenesis of C. abortus abortions in horses is unknown. It is presumed that horses acquire C. abortus through oronasal transmission from a contaminated environment, similar to enzootic ovine abortion in sheep. 26 An investigation into the prevalence of C. abortus antibodies in horses in Mexico identified that 75% of seropositive horses came from farms with seropositive sheep, supporting this postulate. 23 The elementary bodies of chlamydiae are highly resistant to environmental challenges, such as freezing. 26 In sheep, elementary bodies are thought to colonize the tonsils or nasopharyngeal lymphoid tissues before disseminating to the placenta via blood. 26 The bacteria infect trophoblasts, causing damage, as well as inducing placentitis, vasculitis, and thrombosis. 26 The combined effects of these outcomes reduce fetoplacental exchange and ultimately cause abortion. 26
Placentitis, vasculitis, and rare thrombosis, similar to ovine cases of C. abortus, were reported in cases of C. psittaci equine abortions in Australia 6 ; the authors identified a characteristic lymphohistiocytic placentitis. 6 Similar findings were reported in C. psittaci abortions in Hungary in 2005. 24 Both studies also reported PCR-positive cases with suppurative placentitis.6,24 We identified 6 cases of placentitis in the PCR-positive group; 5 cases were identified as suppurative placentitis, and 1 was identified as mild lymphoplasmacytic placentitis. Suppurative placentitis was more common in our cases than in the reported equine studies of C. psittaci; however, suppurative placentitis is common in sheep with C. abortus abortion. 10 Suppurative placentitis is also reported in goats with C. pecorum abortion. 15 The reason for a higher incidence of lymphohistiocytic placentitis with C. psittaci equine cases is unknown but may be related to differences between Chlamydia sp.
In the study from Hungary, 22% of the PCR-positive cases had no gross or histologic lesions.2,4 This is similar to our finding of 17 cases with no lesions noted in their autopsy and histology reports. It is possible that these PCR-positive cases were the result of environmental contamination at the time of birth, prior to submission for autopsy. However, positive IHC staining of the trophoblasts in these cases, as identified both in our study and the study from Hungary 24 would not be expected from environmental contamination. Therefore, these cases with the features of limited placentitis, vasculitis, and thrombosis may suggest that infection is latent, rather than fulminant. 24
The progesterone drop in the period before parturition is thought to be the trigger for chlamydial invasion of trophoblasts and development of disease in sheep. 4 Hence, only sheep affected in the 5–6 wk prior to lambing should be affected by the pathogen. However, this is not the case. 26 Sheep infected when not pregnant or in early- to mid-gestation develop a latent infection by C. abortus. 22 The location of the latent infection is unknown. 22 The latent pathogen is activated during a subsequent pregnancy, in the case of non-pregnant ewes, or during late pregnancy, in early- to mid-gestation ewes, resulting in abortion. 26 Latent infection by chlamydiae resulting in reproductive loss has been postulated to occur in horses; however, this has not been confirmed. 24 A study has identified latent C. abortus in the respiratory tract of clinically healthy horses, supporting this postulate. 25
C. abortus has been implicated as a cause of chronic endometritis in mares 19 ; 6 of 50 mares had C. abortus DNA detected on a uterine cytologic sample, but only 1 had a history of abortion. 19 Uterine biopsy samples from the mares had a low degree of fibrosis and focal lymphocytic infiltration, which was graded as mild endometritis. 19 These findings may correlate with the minimal lesions noted within the placenta histologically in our study; 4 of the mares had been treated with intrauterine oxytetracycline, and all 4 mares successfully conceived after testing chlamydia-negative on post-treatment cytology, suggesting a potential means of preventing C. abortus abortions. 19 The association between C. abortus chronic endometritis and C. abortus abortions has not been investigated to our knowledge, after searching PubMed, Google Scholar, ScienceDirect, SAGE Journals, Scopus, Wiley Online, and Web of Science.
C. abortus is a potentially zoonotic pathogen, although human infections are rare. 26 Infections are most commonly acquired through mishandling of placentas or exposure to vaginal secretions from infected ewes. 26 Fomites, including clothing, footwear, bedding, veterinary equipment, and other tools, may also carry the bacteria. 26 Individuals most at risk of exposure include veterinarians, meat processors, sheep farmers, and laboratory technicians. 26 Human infections may result in flu-like symptoms and atypical pneumonia; however, pregnant women are most at risk for serious disease.20,26 Similar to sheep, C. abortus colonizes the trophoblasts, resulting in placental dysfunction and fetal death. 26 In many cases, the infection can cause coagulopathies, septicemia, shock, and multi-organ failure in the mother, requiring hospitalization and intensive care. 27 It is recommended that pregnant women avoid contact with post-parturient ewes; a recommendation that may be advised when handling post-parturient horses based on the results of our study (Table 2).26,27 Search of PubMed, Google Scholar, ScienceDirect, SAGE Journals, Scopus, Wiley Online, and Web of Science returned no results suggesting zoonotic transfer of C. abortus from equine placental tissues to humans. Additionally, detection of C. abortus DNA on PCR does not indicate that the pathogen is present in sufficient numbers to cause zoonotic disease. Further research into whether C. abortus is truly abortigenic in horses is needed before adding chlamydiae to routine testing for equine abortion cases.
Suggested biosecurity recommendations for equine abortions, based on recommendations for enzootic ovine abortion. 26

Limiting the tested study samples to those submitted to a diagnostic laboratory introduces potential bias in sampling, as not all cases of equine abortion are submitted for autopsy evaluation. Using this sampling method may bias toward unexpected cases of abortion or outbreak situations, or toward owners who have the financial means to investigate abortion cases. There is also likely a sampling bias toward cases without obvious gross lesions, given that lesions may be easily identified by a veterinarian or knowledgeable breeder upon examination. The impact of these biases on the prevalence reported in our study is unknown. We used a short primer to maximize primer annealing; however, it is possible that some relevant DNA fragments were too small for appropriate annealing. Therefore, the overall prevalence of PCR positivity for chlamydiae may be under-reported in our cases.
