Abstract
A 2-year-old, female goat from Connecticut was submitted for necropsy with a 5-day history of pyrexia and intermittent neurologic signs, including nystagmus, seizures, and circling. Postmortem examination revealed suppurative meningitis. Histologic examination of the brain revealed that the meninges were diffusely infiltrated by moderate numbers of lymphocytes, macrophages, and fibrin, with scattered foci of dense neutrophilic infiltrate. Culture of pus and brainstem yielded typical mycoplasma colonies. DNA sequencing of the 16S ribosomal RNA gene revealed 99% sequence homology with Mycoplasma mycoides subspecies capri and Mycoplasma mycoides subspecies mycoides Large Colony biotype, which are genetically indistinguishable and likely to be combined as a single subspecies labeled M. mycoides subsp. capri. The present case is unusual in that not only are mycoplasma an uncommon cause of meningitis in animals, but additionally, in that all other reported cases of mycoplasma meningitis in goats, systemic lesions were also present. In the present case, meningitis was the only lesion, thus illustrating the need to consider mycoplasma as a differential diagnosis for meningitis in goats.
Keywords
Mycoplasmas are the cause of serious diseases in human beings and animals (e.g., walking pneumonia in human beings; contagious bovine pleuropneumonia, arthritis, and mastitis in cattle; enzootic pneumonia in pigs; and infectious anemia in cats). In goats, mycoplasmosis can manifest in many different ways, ranging from pneumonia and joint pain, to agalactia, pleuropneumonia, or death. Meningitis or central nervous system (CNS) involvement is an uncommon manifestation of mycoplasmosis, reported occasionally in human beings and other animals. Most notably, Mycoplasma pneumoniae infection has been associated with encephalitis, aseptic meningitis, acute transverse myelitis, stroke, and polyradiculopathy.21 In goats, CNS involvement appears to be even less common, with only 4 naturally occurring cases reported in the literature, all occurring in goat kids. These cases occurred in goat herds in Hungary, Canada, and California, where goats exhibited the more usual systemic lesions such as polyarthritis, pneumonia, and mastitis, in addition to meningitis. 2,14,18 The present paper describes a naturally occurring case of meningitis in an adult Toggenburg goat from which only Mycoplasma mycoides subspecies capri was recovered, and in which there was no evidence of pneumonia or other systemic lesions.
A 2-year-old, 3-month-pregnant, female Toggenburg goat was submitted to the Connecticut Veterinary Medical Diagnostic Laboratory (Storrs, Connecticut) for postmortem examination. This goat was a member of a herd of 19 adults and 11 kids used for milking and show. At different time points throughout the past year, the herd had 4 adult goats with neurologic disease including facial paralysis and circling. One of the 4 neurologic goats had a history of a lump at the base of the ear. Two goats recovered after treatment with antibiotics and palliative care; another was euthanized but a necropsy was not performed. The goat in the current report had a 5-day history of pyrexia and intermittent neurologic signs, including nystagmus, seizures, and circling, followed by death.
At necropsy, the goat was in good body condition. The subarachnoid space contained diffusely distributed liquid and cream-colored pus; the lungs were diffusely, mildly congested; and a fibrous tag was present on the surface of the heart. No other gross lesions were present. In particular, no lesions were present in the ear canals or tympanic bullae. Tissue samples of brain, spinal cord, trachea, lung, liver, kidney, urinary bladder, heart, rumen, reticulum, omasum, abomasum, small intestine, and large intestine were fixed in 10% neutral buffered formalin, processed routinely, and embedded in paraffin. Sections were cut at 4-µm thickness and stained with hematoxylin and eosin, Brown and Brenn Gram stain, and Wolbach–Giemsa stains.
Histologic examination of the brain revealed that the meninges were diffusely congested and infiltrated by moderate numbers of lymphocytes, macrophages, and fibrin, with lesser numbers of plasma cells and neutrophils (Fig. 1). Additionally, there were multiple foci where the infiltrate was almost exclusively neutrophilic. Aggregates of pleomorphic basophilic organisms less than 1 µm in length were present in these areas (Fig. 1, inset). The organisms did not stain with Brown and Brenn Gram stain but they were stained blue in Wolbach–Giemsa-stained sections, features which are consistent with Mycoplasma. 10 Histologic examination of the lung revealed diffuse alveolar edema, and a fibrous tag was present on the epicardial surface. Histologic lesions were not present in any other tissue.
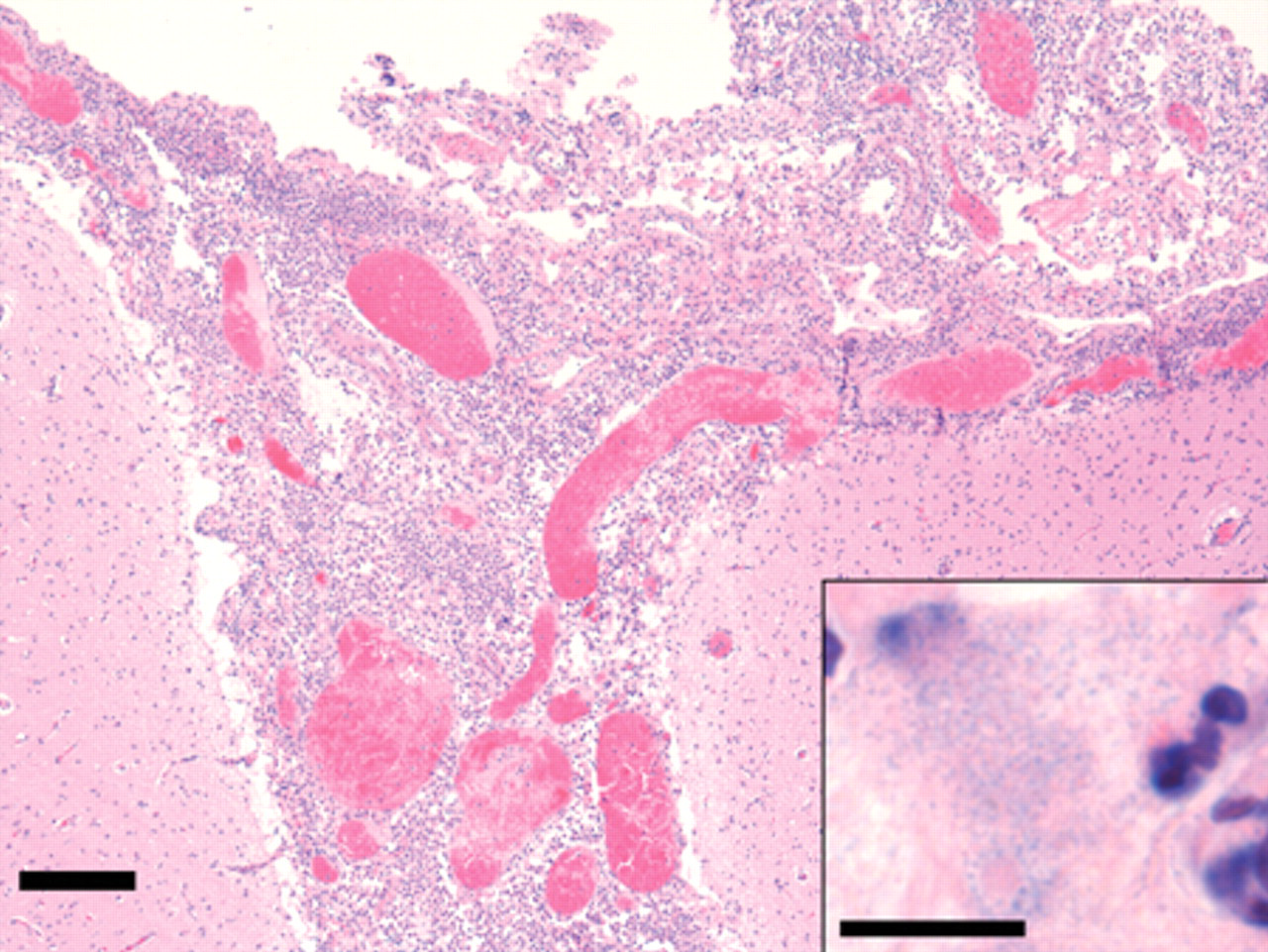
Cerebral cortex, meninges. Diffuse infiltration of the meninges by moderate numbers of lymphocytes, macrophages, and fibrin, with lesser numbers of plasma cells and neutrophils. Hematoxylin and eosin. Bar = 200 um. Inset: Meninges. Basophilic pleomorphic organisms less than 1 µm in length, surrounded by neutrophils, lymphocytes, and abundant fibrin. Hematoxylin and eosin. Bar = 100 µm.
A sample of the meningeal pus was collected using a sterile swab, and a sample of brain stem was collected aseptically for bacteriological examination. Brainstem and pus were cultured separately, each onto a blood agar plate using a sterile swab. Samples were incubated for 48 hr at 37°C with 10% CO2. After initial incubation on blood agar, pinpoint colonies were observed on both plates. These organisms did not stain with the Gram stain. Attempts to subculture on blood agar proved unsuccessful. A 1 cm × 1 cm block of one of the blood agar plates bearing colonies was cut out with a sterile blade, and placed colony side down onto a Hayflick agar plate. The block of blood agar was moved across the plate with a sterile swab. The procedure was repeated for the second sample, and the new plates incubated for 48 hr at 37°C with 10% CO2. After 48-hr incubation at 37°C with 10% CO2 on Hayflick agar plates, typical mycoplasma colonies were observed on both sample plates.
Colonies were transferred to 15 ml of Hayflick 11 broth and incubated at 37°C overnight under aerobic conditions. A 1.5-ml sample of the overnight broth culture was centrifuged (10,000 × g for 10 min at 25°C), and the pellet was resuspended in 10 µl of phosphate buffered saline. One hundred µl of 10% (weight/volume in water) Chelex 100 resin a was added, and the sample was vortexed, centrifuged as before, heated at 95°C, vortexed, and centrifuged again for DNA isolation. 23 Polymerase chain reaction (PCR) was carried out on the supernatant of the clinical isolate and a positive control isolate (Mycoplasma gallisepticum), and also on a no template control, using universal 16S ribosomal RNA (rRNA) primers fD1 and rP1 24 from which the restriction site recognition sites had been omitted (i.e., the forward primer used was AGAGTTTGATCCTGGCTCAG and the reverse primer was ACGGTTACCTTGTTACGACTT). The reaction was run under the following conditions: 94°C for 2 min, followed by 35 cycles of 94°C for 1 min, 55°C for 1 min, and 72°C for 2 min. Samples were loaded into 0.8 % agarose gel and a discrete positive band approximately 1,500 bp was visualized with ultraviolet light after electrophoresis. The PCR product was cloned into a topoisomerase I Taq-amplified vector and transformed into 1 shot Escherichia coli TOP10 competent cells according to the manufacturer’s instructions. b DNA was extracted from these samples using a mini prep kit c according to the manufacturer’s instructions. Samples were digested with EcoRI and a clone with the insert, and were sent to the University of Connecticut Biotechnology Bioservices Center (Storrs, CT) for Sanger sequencing using M13 forward (GTAAAACGACGGCCAG) and M13 reverse (CAGGAAACAGCTATGAC) primers. Chromatograms were base-called, and sequences were assembled using Sequencher v.4.2. d The amplicon sequence was analyzed using BLAST 1 (http://blast.ncbi.nlm.nih.gov/), aligned with relevant sequence matches using ClustalW, 20 and subjected to phylogenetic analysis using the Phylo_Win package. 9
Based on the 16S rRNA gene sequence, the isolate could not be distinguished from M. mycoides subspecies capri and Mycoplasma mycoides subspecies mycoides Large Colony (LC) biotype, which are members of the M. mycoides cluster (Fig. 2). Other members of this cluster are M. mycoides subsp. mycoides Small Colony biotype, Mycoplasma capricolum subspecies capricolum, Mycoplasma capricolum subspecies capripneumoniae, and Mycoplasma sp. bovine group 7. 22 In the past, M. mycoides subsp. capri and M. mycoides subsp. mycoides LC biotype have been considered as different subspecies based on serology. 15,22 However, these subspecies are genetically indistinguishable, and likely represent different serovars rather than different subspecies. 22 It is likely that they will be placed into a single subspecies,M. mycoides capri. 22 For this reason, the isolate was designated as M. mycoides subsp. capri.
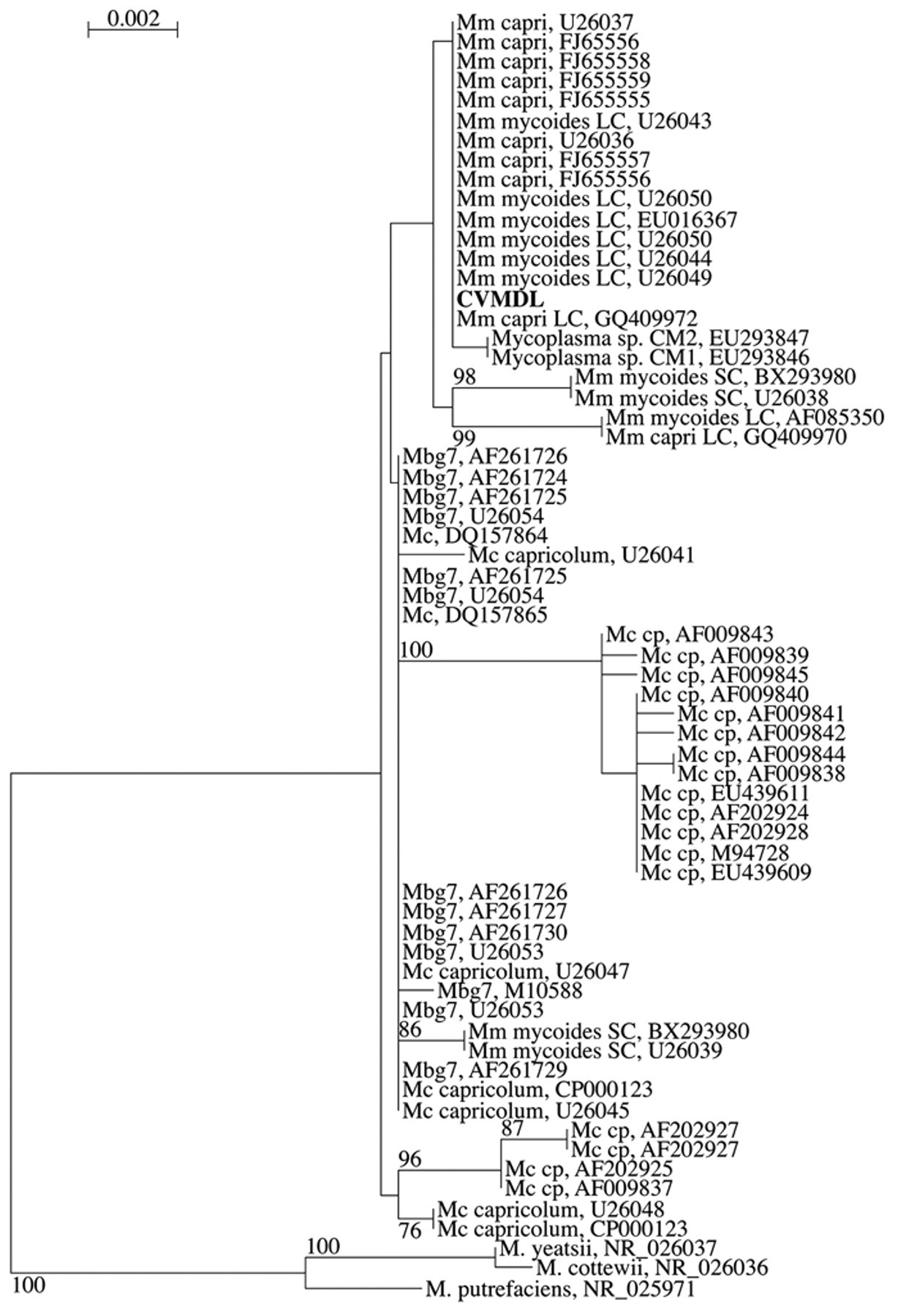
Phylogenetic analysis of Connecticut Veterinary Medical Diagnostic Laboratory isolate relative to other members of the Mycoplasma mycoides cluster. The 16S ribosomal RNA gene sequences were aligned, and a neighbor-joining tree was generated on 1,309 sites using a Jukes and Cantor model and 500 bootstrap replicates. Sequence taxa are referenced to GenBank accession numbers, and species names are abbreviated as follows: Mm: Mycoplasma mycoides; Mc: Mycoplasma capricolum; LC: Large Colony biotype; SC: Small Colony biotype; cp: capripneumoniae; Mbg7: Mycoplasma bovine group 7. Bootstrap values exceeding 70% are indicated, as are estimated genetic distances via the bar scale.
Mycoplasma mycoides subsp. capri and M. mycoides subsp. mycoides LC biotype have been reported to cause caprine mastitis, pleuropneumonia, interstitial pneumonia, polyarthritis, and septicemia. 2,6,7,9,12,13,16–18 Meningitis has only rarely been reported in affected goats, and then it developed as part of multisystem disease.
Mycoplasmas are considered an important cause of meningitis in human beings, especially neonates. Most notably, M. pneumoniae infection has been associated with several different lesions of the CNS including encephalitis, aseptic meningitis, acute transverse myelitis, stroke, and polyradiculopathy. 21
Mycoplasmas are uncommonly reported as a cause of meningitis in animals. Two pigs inoculated with a Mycoplasma pleuropneumonia–like organism from goats exhibited leptomeningeal infiltration by neutrophils and mononuclear cells, along with other systemic lesions. 5 Meningitis has been seen in turkeys due to M. gallisepticum, in calves due to Mycoplasma bovis, and in American alligators due to Mycoplasma alligatoris. 3,4,19 Goat kids experimentally infected with M. mycoides subsp. mycoides LC biotype and M. mycoides subsp. capri developed mild meningitis in addition to many other severe systemic manifestations. 16,17 In an experimental infection of goat kids with M. mycoides subsp. mycoides LC biotype, brain lesions were limited to meningeal vascular fluid leakage and minimal perivascular accumulation of leukocytes. 6 In another experimental study of a goat inoculated into the conjunctival sac by M. mycoides subsp. capri, the organism was isolated from various tissues, including cerebrospinal fluid, but lesions in nervous tissue were not described. 13 In outbreaks in dairy goat herds, M. mycoides subsp. mycoides was isolated from goat kids with meningitis among other pathologic lesions. 2,8,12,18
It is of note that in previous instances of mycoplasmal meningitis in goats and other animals, lesions were invariably present in other organs. To the author’s knowledge, meningitis in an adult goat due to M. mycoides subsp. capri has not been reported. In the current case, fatal M. mycoides subsp. capri–associated meningitis was present in an adult goat, in the absence of systemic lesions. Entry through the ear canals cannot be excluded, as cultures of the ear canals were not performed. Diagnosis of mycoplasmal disease may be challenging due to the lack of pathognomonic disease characteristics and fastidious nature of the organism requiring specific culture conditions. The current case demonstrates the importance of considering mycoplasmosis as a differential in cases of meningitis in goats.
Footnotes
a.
Bio-Rad Laboratories, Hercules, CA.
b.
Invitrogen Corp., Carlsbad, CA.
c.
QIAprep® Spin Miniprep Kit, Qiagen Inc., Valencia, CA.
d.
Gene Codes Corp., Ann Arbor, MI.
The authors declared that they had no conflicts of interest with respect to their authorship or the publication of this article.
The authors declared that they received no financial support for their research and/or authorship of this article.
