Abstract
A heifer developed severe signs of acute gastrointestinal irritation 48 hr after ingesting fresh leaves of Colchicum autumnale growing on a damp meadow. Confirmation of the suspected toxicosis was obtained by detecting colchicine in serum and urine using liquid chromatography coupled with tandem mass spectrometry using atmospheric pressure chemical ionization. Although the serum colchicine concentration had declined to an apparently nontoxic level of 2.4 ng/ml, a more prominent concentration (640 ng/ml) indicative of colchicine poisoning was detected in the urine. This finding is consistent with the known toxicokinetic properties of colchicine, whereby a large volume of distribution results in low circulating blood concentrations and prolonged urinary excretion.
Plants of the genera Colchicum and Gloriosa, both members of the family Liliaceae, contain the natural alkaloid colchicine in toxic amounts. 6,14 The autumn crocus (Colchicum autumnale), also known as meadow saffron, is a perennial species widely encountered in Europe, where it may be mistaken with Crocus spp. or wild garlic (Allium ursinum). In other areas of the world, the autumn crocus is often grown as a house or garden ornamental plant, although it has become naturalized in parts of the United States. 8 The purple flowers, which develop from underground bulbs or corms in autumn, are usually the most visible feature of this plant. The young leaves appear in the spring and die back before flowering. 6 The overall alkaloid concentration of the autumn crocus fluctuates from 0.1% to 2% and, although the highest colchicine level is detected in flowers and seeds, all parts of the plant are toxic. The alkaloid content ranges from 0.5% to 1.2% in seeds, 1.2% to 2% in fresh flowers, 0.15% to 0.4% in fresh leaves, and 0.1% to 0.6% in the underground bulbs. Colchicine contributes 50–70% of the total alkaloid content along with minor amounts of colchicoside, demecolcine, and various related tropolone derivatives. These alkaloids withstand storage, drying, and heat treatment. 19
Although the toxicity of colchicine is well documented, there are only a few reports in the veterinary literature where toxin concentrations have been determined in cases of spontaneous poisoning. In an instance of acute poisoning in cattle, high-performance liquid chromatography was used to determine a colchicine concentration of 1.7 μg/ml in the urine. 23 In another report, thin-layer chromatography was used to determine colchicine concentrations in samples obtained from 2 fatally poisoned nomadic sheep in Albania. The highest colchicine concentration (1.1 μg/ml) in sheep was detected in the milk. 15 More recently, colchicine concentrations have been monitored by liquid chromatography coupled to tandem mass spectrometry (LC-MS/MS) in a similar outbreak of autumn crocus poisoning in nomadic sheep. Concentrations of up to 0.91 μg/ml and 0.97 μg/ml were found in serum and milk, respectively. 7
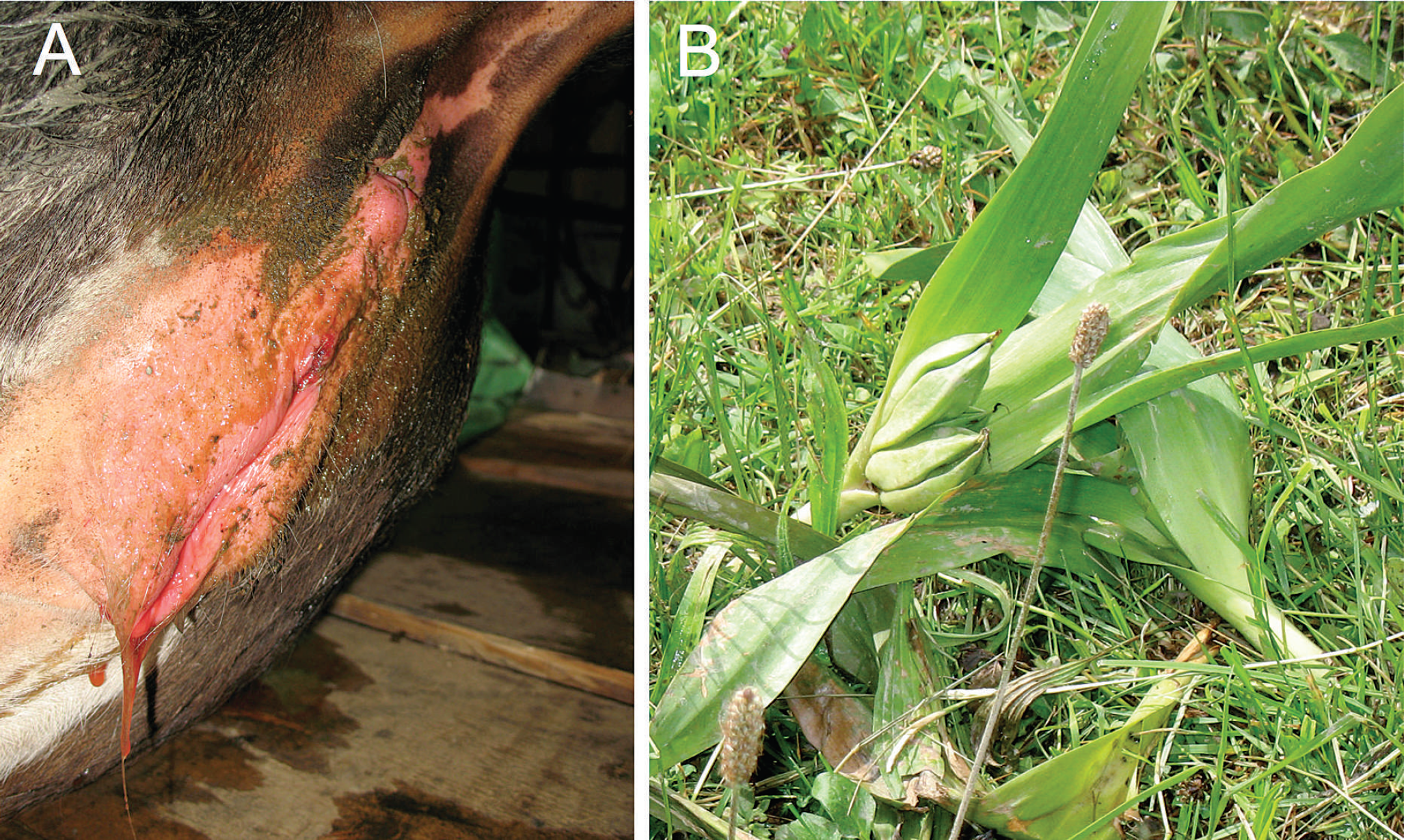
In the present case, a group of Randall heifers gained uncontrolled access to a damp meadow that was part of a local nature conservation area. Two days later, one heifer weighing 350 kg became listless and developed signs of acute intestinal irritation with anorexia, salivation, and abdominal pain accompanied by the passage of fetid feces. These signs culminated in severe serous diarrhea with bleeding and the appearance of mucus (Fig. 1A). Other clinical signs included tenesmus, rectal prolapse, incoordination, weakness, recumbency, tachyarrhythmia, hypothermia, and pale to muddy mucous membranes. The heifer was treated with activated charcoal and intravenous fluids. Examination of the urine disclosed hematuria and proteinuria. Death occurred 3 days later after a period of slight recovery. Inspection of the damp meadow revealed a high density of long, bright green, shiny leaves, many of which were partially bitten off, which suggested recent foraging activity. Based on the elongated shape and parallel veins of the leaves, as well as the accompanying fruit capsules (Fig. 1B), these abundantly growing plants were identified as Colchicum autumnale.
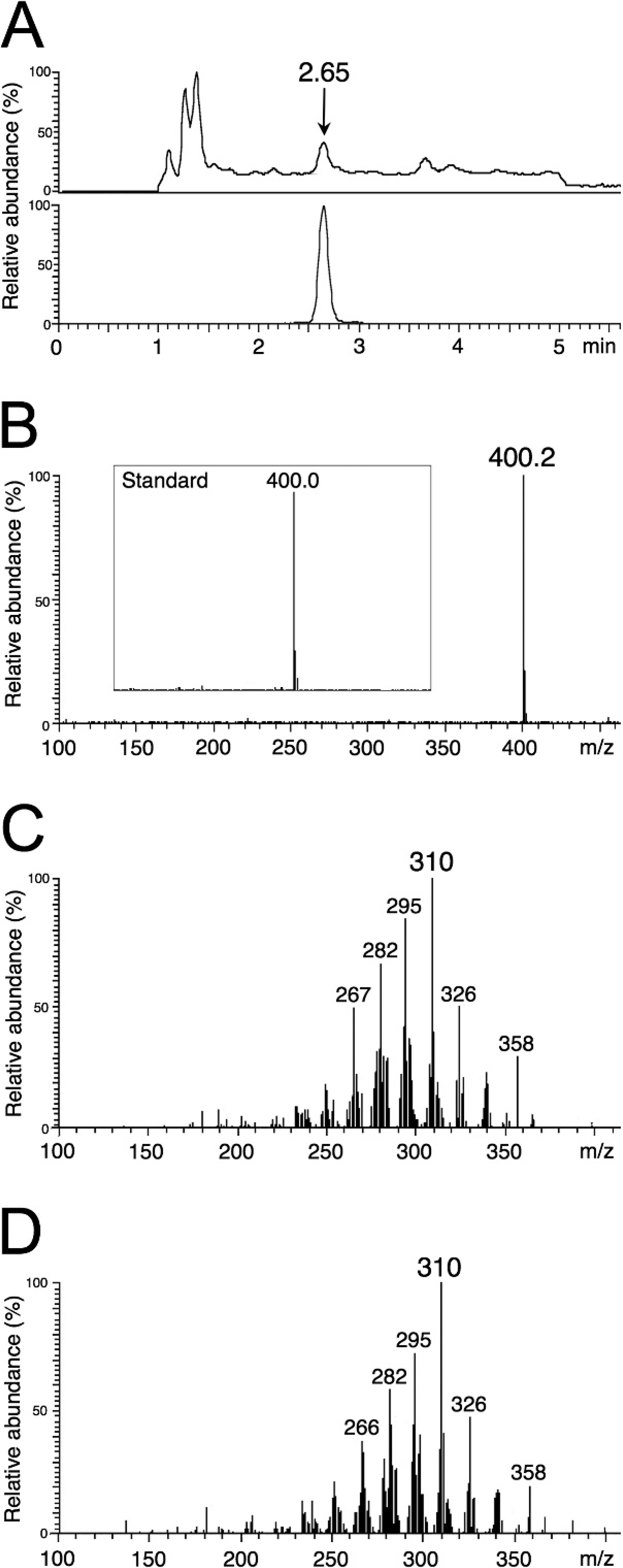
Confirmation of the suspected poisoning was obtained by detection of colchicine using a modified LC-MS/MS method. 5,20 Briefly, blood and urine were taken from the affected animal 2 days after ingestion of the toxic plant. The pH of each probe (1 ml) was adjusted by adding 1 ml of 1 mM ammonium phosphate buffer (pH 8.0), and the samples were extracted with 5 ml dichloromethane. After agitation for 10 min, the organic layer was removed, dried, and dissolved in 25 μl of acetonitrile and 75 μl of 50 mM ammonium formate buffer (pH 3.0). An aliquot (10 μl) of the extract was injected into a C18 column a with a mobile phase consisting of acetonitrile, methanol, and 5 mM ammonium formate buffer (pH 3.0). The separation was completed at a flow rate of 0.3 ml/min using acetonitrile, methanol, and ammonium formate in a ratio of 1.25:51.25:47.5 (vol/vol/vol). Under these conditions, colchicine eluted with a retention time of 2.65 min (Fig. 2A). The detection was performed with a triple-stage quadrupole b after atmospheric pressure chemical ionization in positive mode, thereby monitoring the diagnostic mass transition m/z 400 → 310 (Fig. 2B, 2C). The principal daughter ions obtained from serum and urine samples (Fig. 2C) were in conformity with those resulting from a pure colchicine standard c (Fig. 2D). For quantification, appropriately spiked serum and urine samples were prepared and extracted as described previously. The measured concentration of colchicine was 2.4 ng/ml in serum and 640 ng/ml in urine.
Colchicine interferes with the assembly of tubulin filaments, thus disrupting spindle formation and arresting the cellular mitotic process during metaphase. Colchicine also displays beneficial anti-inflammatory effects in the prevention and treatment of acute gout, presumably by inhibiting the migration of granulocytes into inflamed areas and by suppressing their phagocytic activity. 16 The most frequent adverse effects of colchicine involve the digestive tract because of the sensitivity of dividing cells in the intestinal mucosa. 18 Histologic findings include karyopyknosis, karyorrhexis, and mitotic arrest of cells in the alimentary epithelium as well as in lymphoid and hemopoietic tissues. 22 Human studies indicate that colchicine is rapidly absorbed after oral uptake, and peak blood concentrations occur within 2 hr. 13 Oral bioavailability averages 44%, 1 and the therapeutic steady-state concentration in serum ranges from 0.3 ng/ml to 2.5 ng/ml. 18 In a study of acute human colchicines overdoses, the toxicokinetic profile of colchicine was characterized by a short distribution half-life of 30–90 min, a large volume of distribution of up to 21 l/kg body weight, and a terminal plasma half-life ranging from 10.6 hr to 31.7 hr. 17 These parameters indicate strong tissue binding with low circulating blood concentrations of the compound. An oral colchicine dose of 0.5 mg/kg body weight causes gastrointestinal symptoms in humans, whereas a dose exceeding 0.8 mg/kg leads to multiple organ failure. 3,11 In cattle, 8–10 g of fresh leaves per kilogram body weight has been reported to induce severe diarrhea. 12
Colchicine displays a slow systemic clearance. The main metabolic pathway for the compound involves biotrans-formation in the liver by CYP3A4 followed by conjugation with glucuronic acid, sulfate, or glutathione. 21 After secretion into the bile, these metabolites are subject to extensive enterohepatic cycling, although 10–30% of an oral dose of colchicine is excreted unchanged in the urine. 1,13 In human poisonings, blood colchicine concentrations have reached 62 ng/ml. 9 However, the colchicine concentration in the blood drops below the detection limit of the assay when analysis is performed 40 hr or later after drug ingestion. This probably explains a negative test result in at least 2 fatal cases of colchicines overdose. 4,10 In the heifer of the present report, a considerably elevated colchicine concentration was detected in urine even when the respective blood colchicine concentration had already returned to apparently nontoxic levels.
Management of colchicine poisoning is based on decontamination and aggressive supportive treatment. Activated charcoal is the adsorbent of choice to prevent intestinal absorption. Fluid therapy should be performed to counteract dehydration and electrolyte losses. Immunotherapy with infusion of colchicine-specific antibodies or neutralizing fragment antigen-binding fragments has been used successfully to treat human colchicine toxicoses. 2 Because the alkaloids are transferred through the mammary epithelium, it is advisable not to consume or use the milk from lactating animals exposed to Colchicum autumnale. 7,15 Periodic inspection of meadows and eradication of toxic plant infestations are necessary to prevent further cases of colchicines toxicosis in affected areas.
Footnotes
a.
Uptisphere 5 μ ODB, 125 × 2 mm; Interchim, Montluçon, France.
b.
TSQ 7000, Thermo Fisher Scientific (Schweiz) AG, Reinach, Switzerland.
c.
HPLC-grade, purity 98%; Sigma-Aldrich Chemie GmbH, Buchs, Switzerland.
