Abstract
A hepatic mass was identified in a 5-year-old, female mixed-breed cat that died spontaneously after a clinical history of progressive emaciation, ptyalism, and persistent coryza. At necropsy, a 7-cm-diameter, yellow-brown, firm, multilobulated tumor was identified in the liver. Microscopically, the mass consisted of neoplastic cells arranged in small, closely packed nests within a thin fibrovascular stroma. These cells were of medium sized and polygonal, with fine argyrophilic cytoplasmic granules. Nuclei were predominantly round with finely stippled chromatin and indistinct nucleoli. Mitotic figures were numerous. Immunohistochemically, most of the neoplastic cells were immunoreactive for chromogranin A, neuron-specific enolase (NSE), and cytokeratin AE1/AE3 and weakly labeled for synaptophysin. The tumor was negative for glial fibrillary acidic protein (GFAP), vimentin, and cytokeratins 5, 6, 8, and 17. Vascular emboli and intrahepatic micrometastasis were also identified with chromogranin A. All these features were consistent with a hepatic neuroendocrine carcinoma and emphasized the importance of using a panel of antibodies to diagnose such rare tumors.
Neuroendocrine carcinomas are rare tumors of humans and animals arising from dispersed cells of the neuroendocrine system. 1,2,7 These tumors initially described in the small intestine of human beings were first named carcinoid. The term neuroendocrine carcinoma is now used for all neuroendocrine tumors, acknowledging that all neuroendocrine tumors are potentially malignant. 2
Neuroendocrine cells embryologically derive from the endoderm and belong to 1 of 2 functional groups: the amine precursor uptake and decarboxylation (APUD) cells that produce serotonin and catecholamine hormones, the cells capable of synthesizing low molecular weight polypeptide or protein hormones, such as chromogranin, cholecystokinin, and secretin. 7
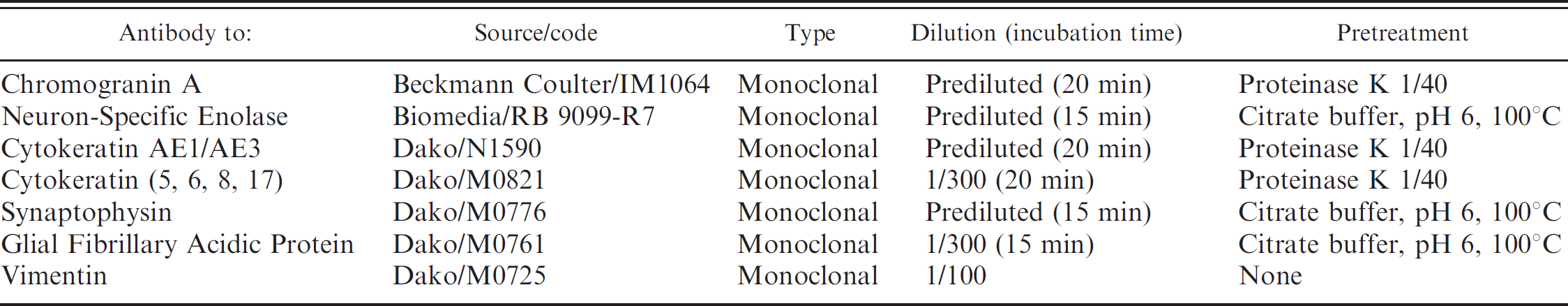
Antibodies, dilutions, and pretreatments used for the immunohistochemical study.
In humans, neuroendocrine tumors are most frequently encountered in the gastrointestinal tract and in the bronchopulmonary system. 6 In domestic animals, they have been described mainly in dogs, but also in cats, horses, and cows, and involve the nasal cavity, nasopharynx, lungs, esophagus, stomach, intestine, liver, bile ducts, and gallbladder. 1,7,8,11,14 Neuroendocrine carcinomas of the liver, extra hepatic bile ducts, and gallbladder are rare neoplasms in cats. 10 Therefore, the prevalence of these tumors is not established, and there are no defined age, breed, or sex predilections.
Hepatic neuroendocrine carcinomas are composed of uniform oval- to spindle-shaped cells, with hyperchromatic, round, or oval nuclei, and abundant granular eosinophilic cytoplasm 1 that form small aggregates separated by a fine fibrovascular stroma. Very few cases of feline hepatic neuroendocrine carcinomas with an immunohistochemical (IHC) profile have been published. An IHC study of 10 feline hepatic neuroendocrine carcinomas published in 2005 showed that chromogranin A, which is the most commonly used neuroendocrine marker in human medicine, was not detected in cats. 10 The present study describes the histopathologic and IHC features of a hepatic neuroendocrine carcinoma in a cat.
A 5-year-old, female mixed-breed cat was referred to the Veterinary School of Alfort with a clinical history of persistent coryza with mucous suppurative discharge, ptyalism, and progressive emaciation. Hematocrit, hemoglobin, and platelet counts were within the normal range: leukocytes and neutrophils were moderately increased (data not shown). The only serum biochemical abnormality was elevated alkaline phosphatase (175 IU/liter; reference range: 0–50 IU/liter) consistent with hepatocellular damage. Polymerase chain reaction (PCR) was performed for feline immunodeficiency virus (FIV) and feline leukemia virus (FeLV), and both were negative. The serological test for feline infectious peritonitis (FIP) by searching for anticoronavirus antibodies was also negative. An ultrasound exam revealed a hepatic mass suggesting a malignant neoplastic process. The owner declined surgery, and the cat died a few days later.
A complete necropsy was performed, and tumor samples were fixed in 10% buffered formalin, routinely processed, embedded in paraffin, and sectioned at 5 μm. Sections were stained with hematoxylin-eosin-saffron (HES) and Grime-lius methenamine-silver method.
The antibodies and pretreatments used for immunohis-tochemistry are indicated in Table 1. A streptavidin-biotin detection system a with diaminobenzidine b as chromagen was used to demonstrate the immune-reaction activity. Slides were counterstained with hematoxylin. For each IHC stain, a control slide was used in which the primary antibody was omitted or an irrelevant antibody was used. Normal cat tissues were used as positive controls for all antibodies.
At necropsy, the cat was emaciated and presented a severe bilateral mucopurulent sinusitis. Excluding the liver, all other organs were macroscopically normal. In particular, no tumor was observed in the gastrointestinal tract. The liver had a 7–cm-diameter, yellow-brown, firm, multilobulated mass involving both medial and lateral left lobes (Fig. 1). Extrahepatic bile ducts and gallbladder were not affected. On the cut section, the tumor was white with multiple hemorrhagic cavities and a few necrotic foci.
Microscopically, the hepatic lesion was an unencapsu-lated, well-demarcated, highly cellular neoplastic proliferation with few hemorrhagic foci. Neoplastic cells were arranged in small, closely packed nests supported by a fine fibrovascular stroma (Fig. 2). These cells were of medium sized (10–15 μm) and polygonal, with variably distinct cell borders and abundant lightly eosinophilic to clear cytoplasm. Nuclei were predominantly round with finely stippled chromatin and 1–2 indistinct nucleoli. Mitotic figures were frequent (32 mitotic figures per 10 × high power fields), and cellular atypia was minimal (Fig. 3). Grimelius stain, a technique used to identify cytoplasmic argyrophilic granules, was positive, with fine cytoplasmic granules in the majority of neoplastic cells. Microscopic and histochemical findings were consistent with hepatic neuroendocrine carcinoma. Mild lymphoplasmacytic and neutrophilic cholangitis associated with a minimal, diffuse interstitial hepatitis were also observed.
Immunohistochemistry stains were scored as follows: 3+ for a positive signal in more than 75% of the neoplastic cells, 2+ for a positive signal in 25%-75% of the neoplastic cells, 1+ for a positive signal in less than 25% of the neoplastic cells, and — for a negative staining.
Most of the neoplastic cells were intensely immunoreactive for chromogranin A (3+) (Fig. 4). With NSE (Fig. 5) and cytokeratin AE1/AE3 (Fig. 6), a positive signal (2+) was observed in many tumor cells, but with cytokeratin AE1/AE3, the pattern of immunolabeling was heterogeneous with variable intensity and distribution. Neoplastic emboli in lymphatic vessels of portal areas were immunolabeled with chromogranin A (Fig. 7), and hepatic intraparenchymatous micrometastasis, not identifiable with HES, was seen with this marker (Fig. 8). In addition, haphazardly distributed neoplastic cells were immunolabeled for synaptophysin (1+). Differences in the color of the immunohistochemical reaction were attributable to the intensity of the staining reaction of these neoplastic cells. Tumor cells were negative for GFAP, vimentin, and cytokeratins 5, 6, 8, and 17 (data not shown).

Cat, liver. Firm, lobulated, 7-cm-diameter hepatic neoplasm with a few necrotic foci.

Cat, liver. Highly cellular neoplasm arranged in small, closely packed nests and packets supported by fine fibrovascular stroma. Hematoxylin and eosin stain. Bar = 50 μm.

Cat, liver. Neoplastic cells are polygonal with variably distinct cell borders and abundant, lightly eosinophilic to clear, occasionally granular, cytoplasm. Mitotic figures are frequent, and cellular atypia is minimal. Hematoxylin and eosin stain. Bar = 25 μm.
In cats, hepatic neoplasms, with the exception of lymphoid tumors, are uncommon, with an incidence varying between 1.5% and 2.3% of all feline neoplasms. 10 Anorexia, lethargy, vomiting, and hepatomegaly are the most common clinical signs associated with hepatic neoplasms in cats. 5,13 Icterus can be observed in tumors of the bile ducts and gallbladder. In this case, the cat did not show clinical signs of hepatic failure but did show elevated alkaline phosphatase. The only clinical sign consistent with neoplasia was emaciation and a hepatic mass. This cat was diagnosed with a liver tumor at a relatively young age. Nonlymphoid neoplasms occur in cats older than 10 years. 13 The most common hepatic tumor in cats is from the biliary system, which is different in humans and dogs. 1,9 Histological differentiation of hepatic neuroendocrine carcinoma from biliary adenocarcinoma and especially hepatocellular carcinoma is essential to evaluate the prognosis. 12 Neuroendocrine carcinomas in pets tend to be locally invasive and metastasize in local lymph nodes, lung, pleura, pancreas, and peritoneal cavities. 14,15
Confirmation of a histopathologic diagnosis requires special stains to reveal argyrophilic properties, but those reactions may be negative, especially in rectal neuroendocrine carcinomas. 8 Immunohistochemical stains can be useful in confirming the diagnosis. Morphologic, histochemical, and IHC features of this cat tumor were consistent with neuroendocrine carcinoma, although, to the authors' knowledge, this is the first report of a feline intrahepatic neuroendocrine carcinoma positive for chromogranin A, NSE, synaptophysin, and cytokeratin AE1/AE3. This emphasizes the importance of using a panel of antibodies (NSE, chromogranin A, and synaptophysin) when evaluating such tumors as has been stated in a previous study. 12
Chromogranin A is present in the secretory granules of endocrine cells, but its functions are still incompletely understood, with several proposed roles, including hormone packaging, stabilization of the granule against osmotic pressure, and excretion of intracellular calcium. 3 Traditionally, chromogranin A has been widely used to facilitate diagnosis of endocrine neoplasia. In a retrospective study, 10 3 of 10 cases of neuroendocrine carcinoma with IHC staining performed were located in the liver parenchyma, and all 3 were chromogranin A, cytokeratin, and synaptophysin negative. The authors discussed the fact that chromogranin A, which is the most commonly used neuroendocrine marker in human medicine, was not useful in their study, although they mentioned that in the extrahepatic neuroendocrine carcinomas tested in the same study (bile duct and gallbladder neuroendocrine carcinomas), chromogranin A and synaptophysin were positive.
Cytokeratin expression in hepatic neuroendocrine neoplastic cells has been demonstrated in a dog 15 and in a retrospective study of humans (4 of 31 were positive). 4 To the authors' knowledge, there have been no published studies of feline neuroendocrine carcinoma that are cytokeratin positive.
Several theories have been postulated concerning the cellular origin of the hepatic neuroendocrine neoplasia as a pluripotential cell, transformation of a liver stem cell, pancreatic rest tissue occurring in the liver, or a intrahepatic biliary neuroendocrine stem cell. 2 The different expression and immunolabeling patterns of chromogranin A and synaptophysin observed in this study could be explained by the presence of more differentiated neoplastic cells or by a different origin of the tumoral cells than the ones previously mentioned, 2 but these hypotheses would require further investigation. The positivity for cytokeratin and chromogranin A, never observed before in a hepatic neuroendocrine carcinoma in a cat, could also be due to the use of different pretreatments or antibodies in comparison to a previous study. 10
In conclusion, this case report demonstrates the existence of different IHC patterns in feline hepatic neuroendocrine carcinoma, therefore, emphasizing the importance of using a panel of antibodies (NSE, chromogranin A, and synaptophysin) to diagnose such tumors. It also reaffirms the importance of morphological features in the diagnosis of such tumors. In addition, IHC staining was useful for detection of vascular emboli and micrometastases.
Acknowledgements. The authors gratefully thank N. Towaco, A. Chapeaux, and P. Wittier for their excellent technical assistance.

Cat, liver. Most of the neoplastic cells react positively to chromogranin A. Immunoperoxidase staining, hematoxylin counterstain. Bar = 25 μm.

Cat, liver. Many neoplastic cells react positively to neuron-specific enolase, others have a weak expression. Immunoperoxidase staining, hematoxylin counterstain. Bar = 25 μm.

Cat, liver. A heterogeneous expression of cytokeratin AE1/AE3 in neoplastic cells is seen. Immunoperoxidase staining, hematoxylin counterstain. Bar = 50 μm.

Cat, liver. Vascular emboli of neoplastic cells are immunolabeled by chromogranin A. Immunoperoxidase staining, hematoxylin counterstain. Bar = 70 μm.

Cat, liver. Intrahepatic micrometastases, immunolabeled by chromogranin A. Immunoperoxidase staining, hematoxylin counterstain. Bar = 200 μm and 25 μm (inset).
Footnotes
a.
Ventana system, Ventana Medical Systems, Inc., Illkirch, France.
b.
Ventana DAB detection kit, Ventana Medical Systems, Inc., Illkirch, France.
