Abstract
Objective
This study aimed to analyse the differences in Emergency Departments (EDs) length of stay (LOS) for mental health (MH) presentations between older patients (aged 65 and above) and younger adults, identifying factors contributing to longer stays.
Methods
A retrospective data analysis of MH patients presenting to MHEDs in three Brisbane hospitals between May 2018 and May 2019 was conducted. We dichotomised LOS around the 75th quartile (20 h), given the skewness of the data. Patients remaining in MHED for longer than 20 h were considered as a prolonged length of stay (PLOS).
Results
Older patients constituted 4.5% (n = 423) of the 9452 MH presentations. They were significantly more likely to experience PLOS (p < .0001). Awaiting admission had an 11-fold increased risk of PLOS (Adjusted OR 9.69–12.48, 95% CI). Additionally, alcohol and drug-related cases were prone to PLOS (p < .0001), though these factors did not explain the extended stays in the elderly.
Conclusion
Older MH patients had a significantly longer LOS in MHED compared to younger adults. Neither waiting for admission nor substance-related issues fully accounted for this discrepancy. Further research is needed to explore other potential contributing factors to PLOS, for example, medical comorbidities, psychosocial issues, and systemic-related delays in elderly MH care.
Keywords
In recent years, there has been an increase in mental health presentations to Emergency Departments (EDs). The rate of mental health ED (MHED) presentations per 10,000 population was 121.6, with 310,471 presentations to EDs of public hospitals between 2019 and 2020. The proportion of these patients who are aged 65 years and over has increased from 10.3% in 2015–2016 to 23.0% in 2020–21. In Queensland, the rate of older adult (65 years or older) presentations to MHED per 10,000 population increased from 58.2 (2399 presentations) between 2015 and 2016 to 66.8 (3152 presentations) between 2019 and 2020. 1
Nearly two-thirds of MHED presentations are discharged or referred to another hospital (58.1%), whilst one-third of presentations (34.0%) are admitted to the same hospital.1,2 MHED presentations spent more time in EDs (up to 14 h) than those for other presentations (up to 8 h). 3
Some studies found that a prolonged stay in a crowded ED environment could lead to deterioration in patient outcomes, including enhanced risk of self-harm and aggression. This can put patients and staff at risk of violence, delay patient care and impact staff morale.4–7
International evidence suggests that older patients with mental health presentations had a longer LOS than younger patients. Reasons offered in studies include presenting features such as suicidality, alcohol or substance-related presentations, physical comorbidity, dementia, neurocognitive disorders and psychosocial-related issues,3,8–11 as well as and more complicated departure dispositions.3,4,8,9,12 The current understanding of reasons for prolonged ED LOS for psychiatric presentations in older patients in Australia is limited. One reason might be that this population are more likely to require admission with one Australian study reporting that 63% of older patients presenting to ED were admitted to a hospital ward although there was no comparison with other age groups. 8 Another might be a high rate of comorbidity that may lengthen ED stays in this population through the need for extensive organic screening. This may be compounded by the presence of cognitive impairment, which was present in more than 40% of people aged 65 years and over in one study of Australia and New Zealand mental health services. 13 More research in this field would provide insight into possible contributing factors to older patients’ MHED LOS and a better understanding of ageing-related care needs during ED presentations. This could help to form comprehensive treatment plans and identify strategies for shortening LOS in EDs without compromising the quality of patient care.
Based on existing research, the research question was that older patients would stay in EDs longer than younger patients due to age-related complex health issues and psychosocial situations requiring more assessment and management planning time.
Method
The setting for this study was the Mental Health Emergency Department (MHED) in each of three Brisbane hospitals. Each MHED is staffed by a multidisciplinary team comprising psychiatric doctors, nurses, and mental health clinicians trained to address acute psychiatric presentations. The service provides consultation to the medical ED on patients (including general adults and patients aged 65 years and over) with mental health related presentations including mental health assessments and management planning. Patients with mental health presentations are triaged through the main ED of each hospital before being referred to MHED for assessments and management planning. Some patients were referred directly from the triage and some patients were secondary referrals after initial medical assessment and management by medical EDs. During the study period, patient data were sourced from a journey board (JB), an electronic patient presentation system where all mental health referrals to the MHEDs of three hospitals were recorded. The information captured on journey boards included gender, age, presenting complaints, referring times (not including the time that patients were receiving medical assessments and treatments prior to referral to MHEDs), discharge time, and departure destinations. The Length of Stay (LOS), regardless of direct triages or internal ED referrals is captured in the system by the time of referral and the time of departure. Given how the EDs functioned, patients with repeat mental health presentations could be recorded more than once on the JB over the study period but were not considered as duplicate presentations.
Retrospective data analysis was used to identify the difference in length of stay (LOS) between older and younger patients at each MHED between May 2018 and May 2019. We investigated the association between age, gender, diagnoses, LOS and departure destinations (hospital admission or discharge).
We dichotomised the duration of time in ED around the 75th quartile (20 h) to address the skewed distribution of the data. Patients who remained in MHED for longer than 20 h were considered to have a prolonged length of stay (PLOS).
Ethical clearance was obtained from the local District Health Service Ethics Committee.
Data were entered and analysed by SPSS (v26). We initially examined associations using descriptive and bivariate statistics. Multivariate analysis and logistic regression were then conducted to explore the differences in length of stay between older and younger patients.
Results
The initial recorded number of MH presentations was 19,575 including those with missing information (such as basic demographics, diagnoses, referring times, departure times, and discharge destinations), duplicated data entry of those being recorded twice on JB for the same presentation at the same time that could potentially impact on data analysis. Patients who re-presented to ED on subsequent occasions were not considered as duplicate presentations. After removing those patients with missing information and duplicated presentations, a total of 9452 mental health patients presented to MHED between May 2018 and May 2019. There were slightly more females (n = 4782; 50.6%) than males (n = 4670; 49.4%). Only a small proportion of patients were aged 65 or over (n = 423; 4.5%).
Time in emergency department (ED) by patient characteristics
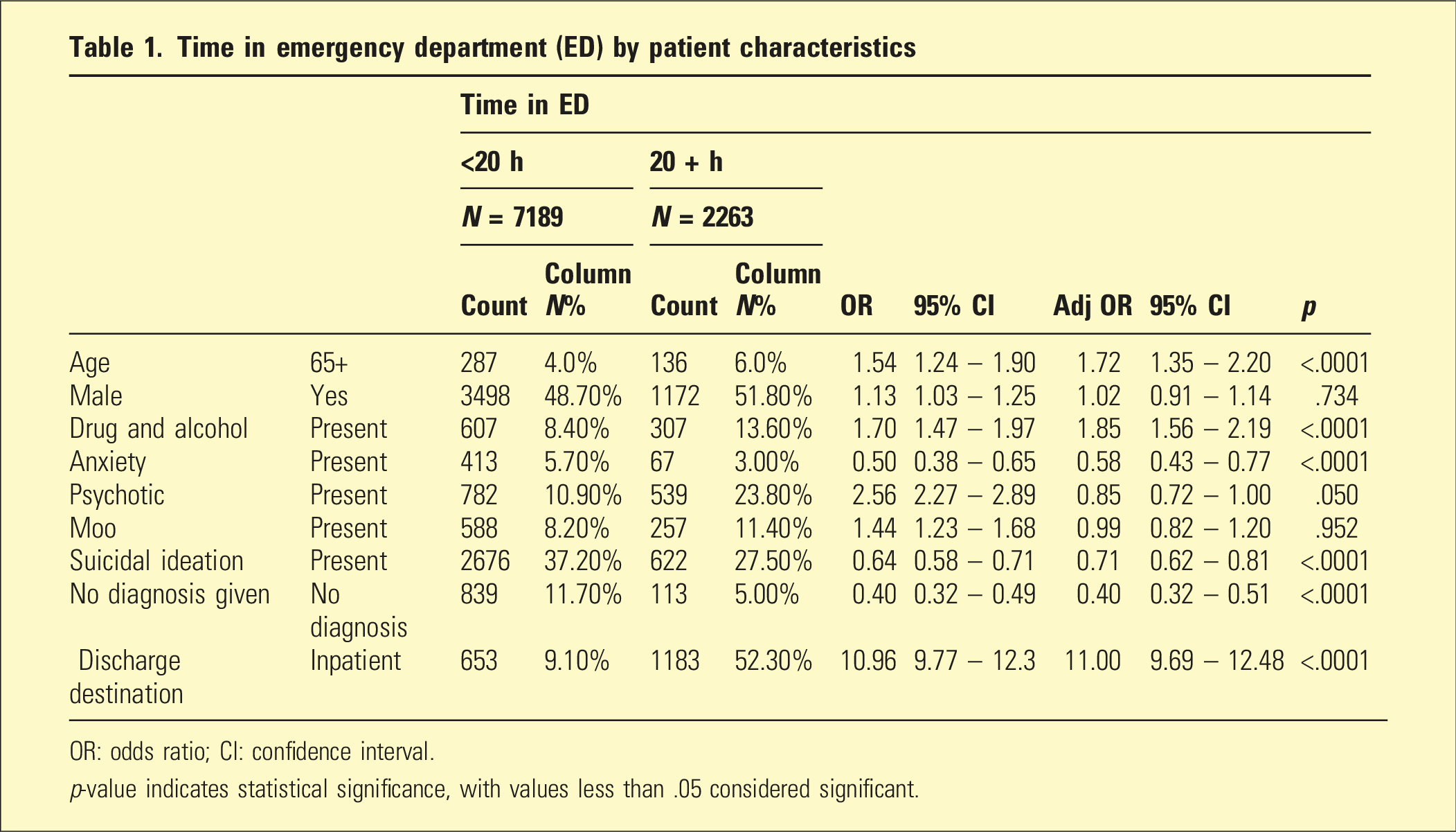
OR: odds ratio; CI: confidence interval.
p-value indicates statistical significance, with values less than .05 considered significant.
The associations between LOS, clinical diagnoses and discharge destinations, both unadjusted and adjusted, are described in Table 1.
On unadjusted analysis, older patients were 54% more likely to spend longer than 20 h in MHED. Other variables associated with PLOS included male gender (OR 1.13), drug and alcohol problems (OR 1.7), mood disorders (OR 1.44), and self-harm (OR 1.11). People with psychotic disorders were over two and a half times (OR 2.56) more likely to have a PLOS, and those subsequently admitted to the ward had an 11-fold risk of PLOS. By contrast, people presenting with suicidal ideation, anxiety disorders, personality disorders, or other diagnoses, including medical conditions, and given no diagnoses were less likely to have a PLOS (Table 1).
On adjusted odds ratio analysis, accounting for the influence of other co-variables, older patients were still more likely to have a PLOS (OR = 1.72), as well as those presenting with alcohol and drug problems or requiring admission (Table 1). Patients presenting with psychotic disorders, anxiety disorder, suicidal ideation, and those given no diagnoses were less likely to have PLOS. There was no significant difference in LOS between genders.
We further explored whether PLOS in older patients could be explained by a greater proportion of ED visits being due to alcohol and drug problems or resulting in admission. However, older patients were significantly less likely to present with the former (OR = 0.33; 95% CI 0.20–0.56) and were not admitted at a greater rate (OR = 1.19; 95% CI 0.94–1.51).
Discussion
This study corroborates international evidence indicating that older patients with MH presentations experience prolonged LOS in ED compared to younger adults.1,5,8–10,14 While this study confirms that older patients experience longer LOS in MHED, most factors discussed, such as substance use and admission rates, were not examined specifically for their impact on older adults and so the lack of age-specific analysis limited the ability to draw targeted conclusions. As the LOS calculations did not include patients’ medical ED time before MHED, the likelihood of LOS could be even longer for older patients due to the complexity of their presentations and needs for medical interventions prior to MHED input, as reported in previous studies. 11 Given the MHED model is designed for specialist mental health interventions, it is important to consider that contributing factors to prolonged LOS may originate in the general ED prior to MHED referral.
Contributing factors to prolonged LOS in older patients
The extended LOS for older patients may stem from multifaceted challenges inherent to geriatric MH care. Firstly, the interplay of medical comorbidities, such as frailty, delirium, or neurocognitive disorders) likely required time-consuming evaluations (e.g. cognitive assessments, imaging, laboratory tests, and specialist consultations.12,15,16 Such assessments are critical for distinguishing psychiatric symptoms from organic aetiologies but may delay decision-making. 15 In addition, it can be challenging and time-consuming to recognise and differentiate between primary psychiatric presentations, delirium with behavioural disturbances or psychotic-like symptoms. Secondly, psychosocial complexities, such as inadequate community support, housing instability, or safeguarding concerns that usually require meticulous discharge planning, especially when patients did not meet the criteria for inpatient care.3,4,9 The third factor could be system barriers including shortage of geriatric MH beds or delays in interhospital transfers, which may exacerbate PLOS in EDMH.3–5,7,9,10,14,16,17 Such limitations in bed availability may be indicated by admissions to general adult psychiatry or medical wards, which in turn may obscure the true demand for geriatric MH care. These factors align with global studies attributing prolonged ED stays in older patients logistically, clinically and systematically.
The model of care of MHEDs in this study is a consultation-liaison model where the MH service of each hospital provides psychiatric care to people presenting to the ED, the emergency physicians retaining overall responsibility for individuals during their ED stay. This is different from dedicated short-stay psychiatric wards that provide 24/7 multidisciplinary care for people presenting to the ED in crisis.
Implications for clinical practice and future research
The implications for clinical practice must be interpreted in light of the MHED model and the data limitations. The following strategies should be considered: • Improving referral pathways to MHED by effective collaboration and communication between medical ED and MHED regarding older patients’ presenting complaints, associated complexity and their needs for mental health services’ input. • Implementing care pathways that streamline interdisciplinary assessments in ED and discharge for older adults. • Embedding geriatric MH specialists within ED/MHED teams to support rapid and focused assessments and care planning for those older mental health patients with comorbid medical issues. • Enhancing access to geriatric MH inpatient beds that would require improving accessibility to community services with adequate psychological, geriatric, and social supports to facilitate timely disposition, as being identified by Australian researchers.
18
• Advocating for better resources for service improvement with studies on MHED workflows and age-specific analyses and clarify the impact of referral pathways and discharge destinations on LOS for older adults.
Study limitations
This study has several limitations. The retrospective design, the delays in obtaining more recent data after the COVID-19 pandemic, and reliance on administrative data restricted the exploration of variables such as medical complexity, psychosocial circumstances, or care coordination processes.1,8 It is also possible that some over-65 year old who initially presented with medical symptoms may not have been recorded in the journey board (JB) by the time of being either directly discharged to home or to medical admissions irrespective of further MH input. Coding inconsistencies without the standardisation in coding practices may have influenced diagnostic categorisations, potentially skewing associations between diagnoses and LOS.8,12 Additionally, the small proportion of older patients (4.5%) and restriction to just three hospitals in one health district limit generalisability. Moreover, the unit of analysis was ED presentations, rather than individual patients so individuals may have been included more than once. Finally, there was no information on the presence of factors that might have affected LOS such as cognitive impairment and psychosocial circumstances. Future prospective studies should incorporate detailed clinical, social, and systemic data to better delineate drivers of PLOS in this population.10,14
Conclusion
Older patients with MH presentations experienced significantly longer ED stays than younger adults. The disparity was not fully explained by common risk factors like substance use or hospitalisation needs, which could suggest involvement of other unmeasured factors. Addressing this issue requires targeted interventions, including geriatric MH specialisation within EDs, staff training in ageing-related complexities, and systemic reforms to optimise care pathways.3,8,17 Such measures could enhance patient outcomes, reduce ED overcrowding, and align services with the evolving needs of an ageing population.
Footnotes
Author contributions
All authors contributed equally to the conceptualization and design of the study, data collection and analysis, interpretation of the results, and drafting and revising the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical considerations
All procedures involving human subjects were approved by the Metro South Human Research Ethics Committee (HREC/2022/QMS/78893). This included a waiver of consent given the use of anonymised data.
