Abstract
Objectives:
To examine willingness to adopt protective behaviours, and perceived barriers, during a pandemic influenza, in people with schizophrenia.
Methods:
A cross-sectional study using a questionnaire was conducted exploring the responses of 71 adults with schizophrenia and 238 adults without schizophrenia attending a general practice setting, regarding willingness and perceived barriers to adopting protective measures against the 2009 swine influenza pandemic in Australia.
Results:
The majority of participants with schizophrenia reported that they would be at least moderately willing to be vaccinated (74.2%), isolate themselves (73.2%), wear a face mask (54.9%) and increase hand washing (88.6%). However, 71.8% were concerned about “catching” flu from vaccination. Predictors of willingness to adopt protective actions included self-efficacy (vaccination, face mask, isolation), perceived likelihood of contracting swine flu (vaccination), educational status (face mask) and perceived overall risk from swine flu (face mask). Key modifiable perceived barriers to adopting protective measures were identified, including cost and need for transport assistance for vaccination.
Conclusions:
People with schizophrenia report being generally willing to adopt protective measures, especially increased hand washing, during a pandemic influenza. Understanding perceived barriers may enable development of effective interventions to increase uptake of protective measures.
Pandemic influenza continues to pose a major public health threat in the 21st century. Therefore, it is essential that health services are maximally prepared with a well-considered response plan. Health outcomes of a significant influenza outbreak are influenced by the behavioural response of the community. The adoption of protective measures by the public attenuates the spread of the virus, especially in the early stages of a pandemic. In particular, vaccination can significantly reduce the number of people infected, as well as hospitalization and mortality rates. 1 However, because there are likely to be limitations in the supply and effectiveness of vaccines (and antiviral medication) in a pandemic influenza, non-pharmacological (infection control) measures also have an important role to play. 2 Increased hand hygiene, isolation and wearing a face mask have been demonstrated to be effective in reducing transmission of respiratory viruses 3 and their use during a pandemic influenza has been endorsed by expert opinion.2,4,5 Protective behaviour is linked to a person’s risk perceptions of the health threat as well as their evaluation of the potential benefits and risks associated with a given preventative action. 6
People with a mental illness, including those with schizophrenia, have been shown to have significantly higher mortality rates from influenza and pneumonia compared with the general population, as well as a 50% excess hospitalization for influenza. 7 However, there is a paucity of research investigating: what people with mental illness believe about protective measures; how willing they would be to adopt them; and what they perceive as barriers to their uptake, in the event of a significant outbreak of influenza.
This study was conducted in 2009 during the H1N109 (“swine flu”) outbreak in Australia, which the World Health Organization declared a global pandemic on 11 June 2009. The key aims of this study were to explore the willingness of people with schizophrenia to undertake protective measures against the 2009 swine influenza, as well as perceived barriers to adopting these measures.
Methods
The following is a summary of the methods used in this study, which have been described elsewhere. 8
Participants
The sample has been described previously
8
but can be summarized as follows. Within the Australian Capital Territory, a purposive stratified sample of 309 patients aged 18–65 (inclusive) was recruited from healthcare settings. This included 71 patients with schizophrenia (SCZ) from mental health care settings, as well as 238 adults from 13 general practice (GP) settings, none of whom had a diagnosis of schizophrenia. Participants with schizophrenia (excluding schizoaffective disorder) were recruited from both hospital (
Measures
Participants were invited to complete a questionnaire that included items examining their willingness to undergo protective measures during a pandemic influenza in Australia, and perceived barriers to adopting these measures (Table 1).
Questionnaire items

Statistical analyses
All analyses were carried out using SPSS version 22. Within-group analyses using logistic regression were performed to examine for significant predictors of willingness to take protective actions. Odds ratios were obtained after responses were dichotomized into:
Results
Demographics
The mean age in the SCZ group was 36.1 years (SD 9.7) and 36.6 years (SD 14.1) in the GP group (Table 2). There was no statistically significant difference between the SCZ and GP groups for age. However, significant differences were present for gender, employment status, living alone, children in the household, and highest level of education.
Socio-demographic characteristics
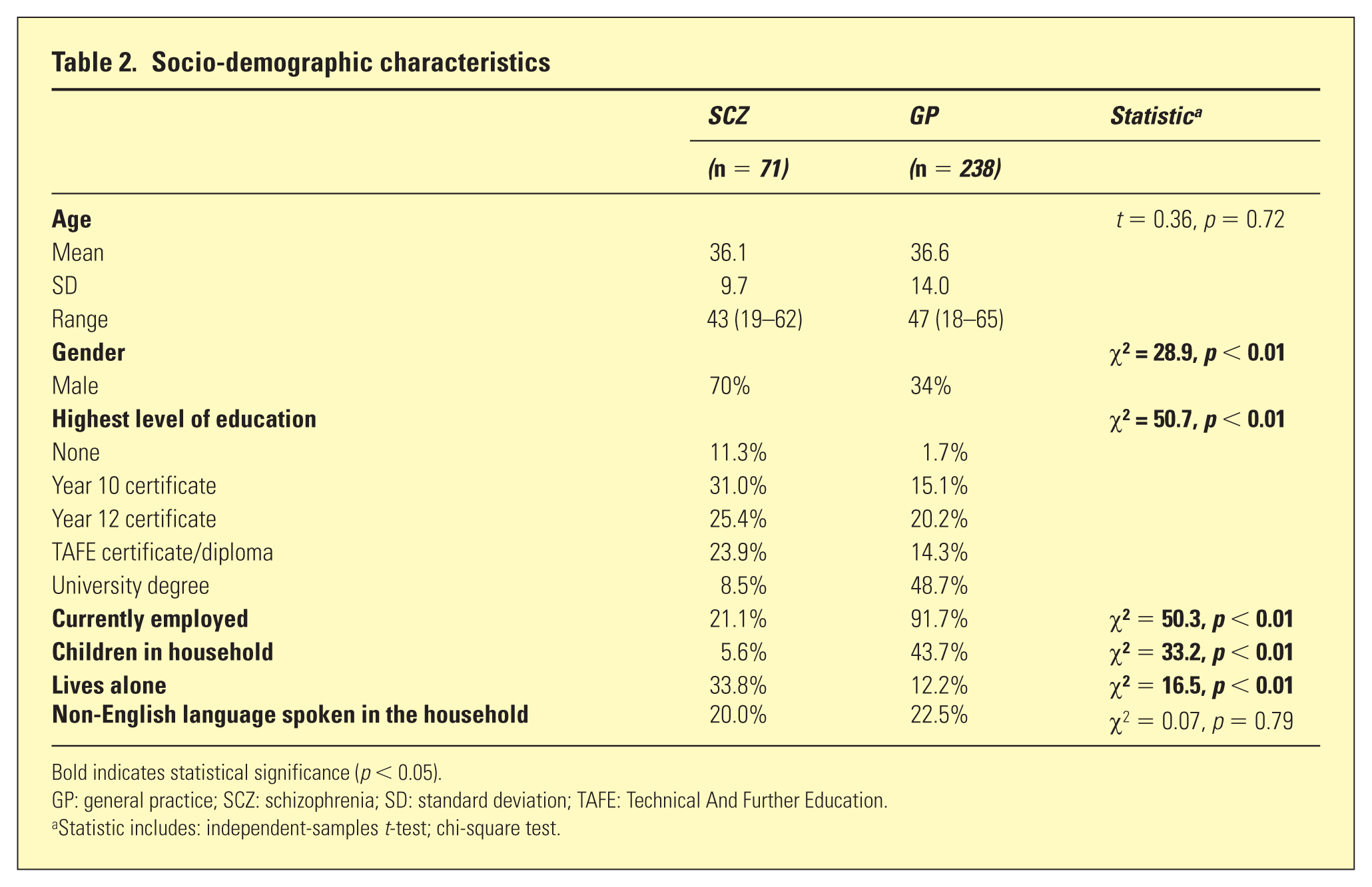
Bold indicates statistical significance (
GP: general practice; SCZ: schizophrenia; SD: standard deviation; TAFE: Technical And Further Education.
Statistic includes: independent-samples
Willingness
Vaccination
In the SCZ group, 74.2% of participants were moderately, very or extremely willing to receive a vaccination compared with 80.1% in the GP group (Table 3). Within-group analysis (Table 4) revealed that, for participants in the SCZ group, predictors of increased willingness to receive a flu vaccination included self-efficacy and perceived own likelihood of contracting swine influenza. In the GP group, predictors of increased willingness to be vaccinated included perceived effectiveness of vaccination and self-efficacy. Those in the GP group who perceived a substantive risk of adverse reaction were less likely to be willing to receive a vaccination.
Comparison between SCZ and GP groups for protective measures against pandemic influenza
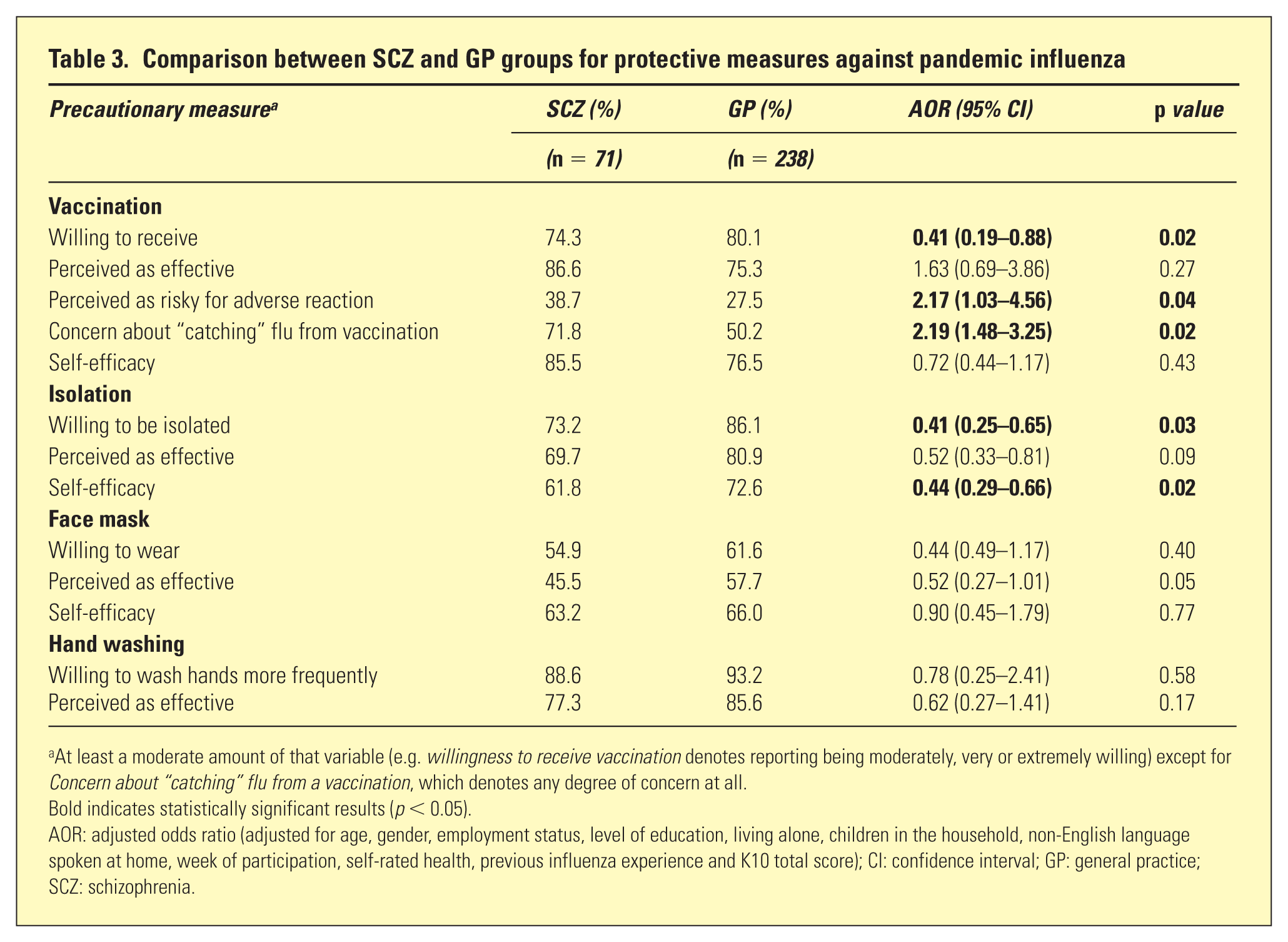
At least a moderate amount of that variable (e.g.
Bold indicates statistically significant results (
AOR: adjusted odds ratio (adjusted for age, gender, employment status, level of education, living alone, children in the household, non-English language spoken at home, week of participation, self-rated health, previous influenza experience and K10 total score); CI: confidence interval; GP: general practice; SCZ: schizophrenia.
Predictors of willingness to adopt protective measures: within-group multiple logistic regression (Exp(B) with
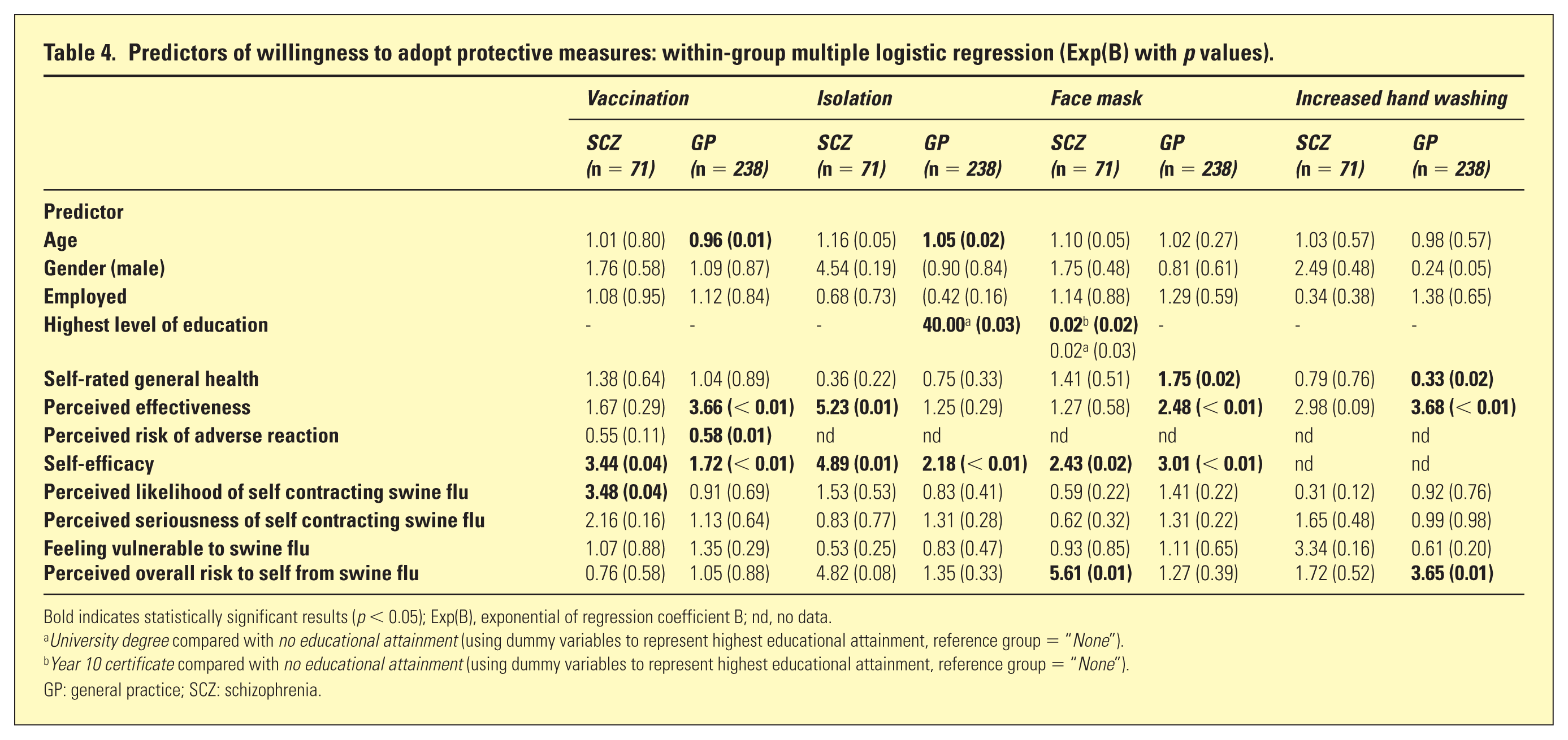
Bold indicates statistically significant results (
GP: general practice; SCZ: schizophrenia.
Social isolation
In the SCZ group, 73.2% of participants were at least moderately willing to isolate themselves from others compared with 86.1% in the GP group (Table 3). Within-group analysis (Table 4) showed that in the SCZ group, positive predictors for willingness to be isolated included perceived effectiveness of isolation and self-efficacy. In the GP group, educational attainment and self-efficacy were positive predictors.
Facial mask
In the SCZ group, 54.9% of participants were at least moderately willing to wear a face mask, compared with 61.6% in the GP group (Table 3). Of all the precautionary measures examined in both groups, wearing a face mask was the least likely to be adhered to and the most likely to be viewed as ineffective or minimally effective. Within-group analysis (Table 4) revealed that in the SCZ group, positive predictors of willingness to wear a face mask included self-efficacy and perceived overall risk from swine flu. Negative predictors included a university degree compared with no educational attainment, and a Year 10 Certificate compared with no educational attainment. In the GP group, self-efficacy, perceived effectiveness, and higher self-rated general health were positive predictors of willingness to wear a facial mask.
Hand washing
There were no differences between the SCZ and GP groups in terms of being at least moderately willing to increase hand washing in the event of an Australian pandemic influenza (Table 3). Approximately 90% of participants in both groups were willing to engage in this simple but important protective measure. In addition, over three-quarters of people in each group evaluated increased hand washing as an effective preventative action. Perceived effectiveness and perceived substantive overall risk from swine flu increased the likelihood of people in the GP group being willing to increase hand washing, whereas higher self-rated general health reduced the likelihood (Table 4).
Between-group differences
Despite the majority of people in both groups being willing to adopt all four protective measures, logistic regression analysis revealed that people with schizophrenia were less willing to receive a vaccination and to isolate themselves compared with those in the GP group, had less self-efficacy for isolation, and were more likely to perceive vaccination as risky for an adverse reaction, including having concerns about “catching” flu from it (Table 3).
Perceived barriers
Perceived barriers for each protective measure are shown in Figures 1–4. For people with schizophrenia the main barriers are summarized in Table 5.
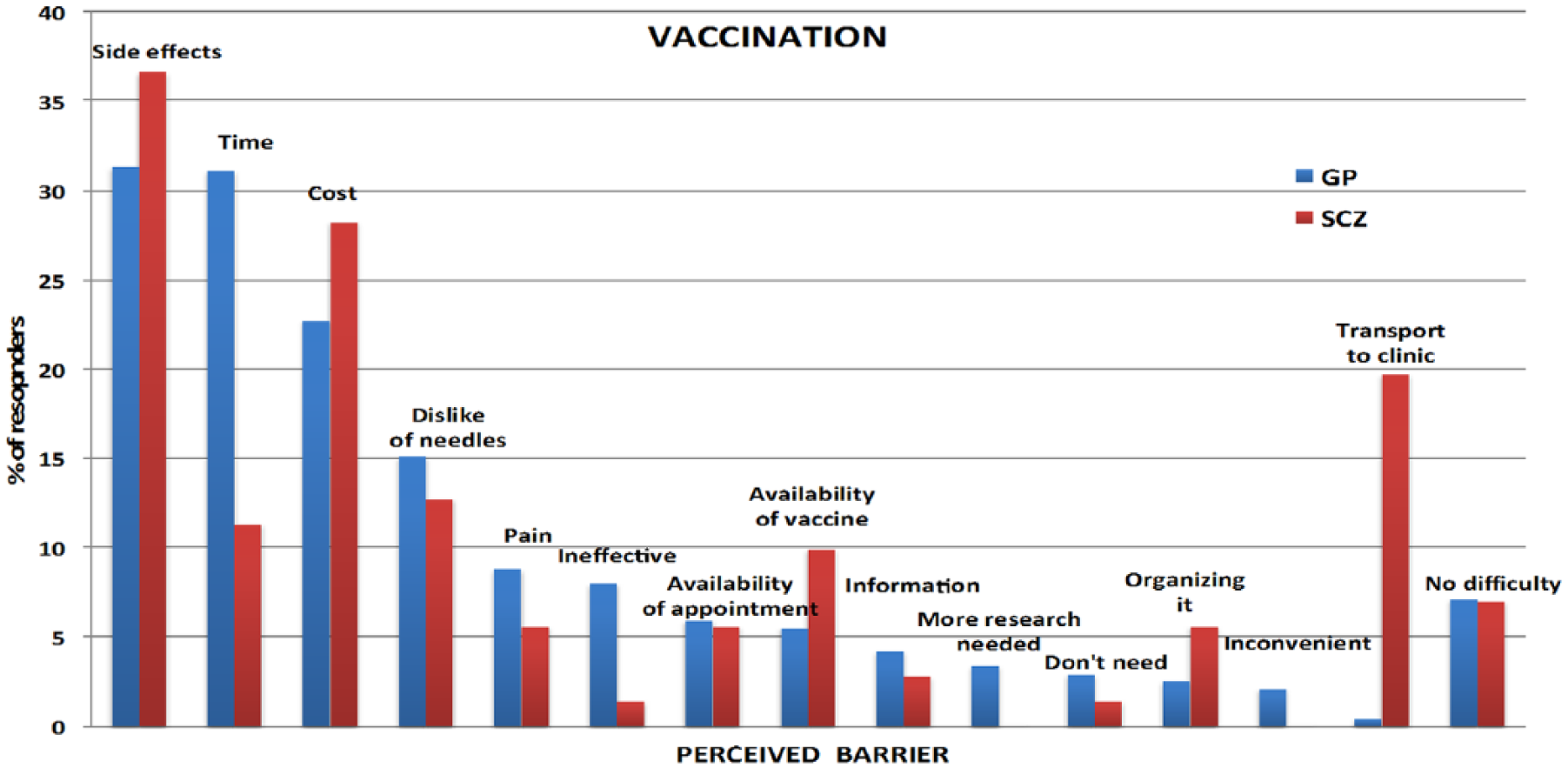
Perceived barriers to vaccination.
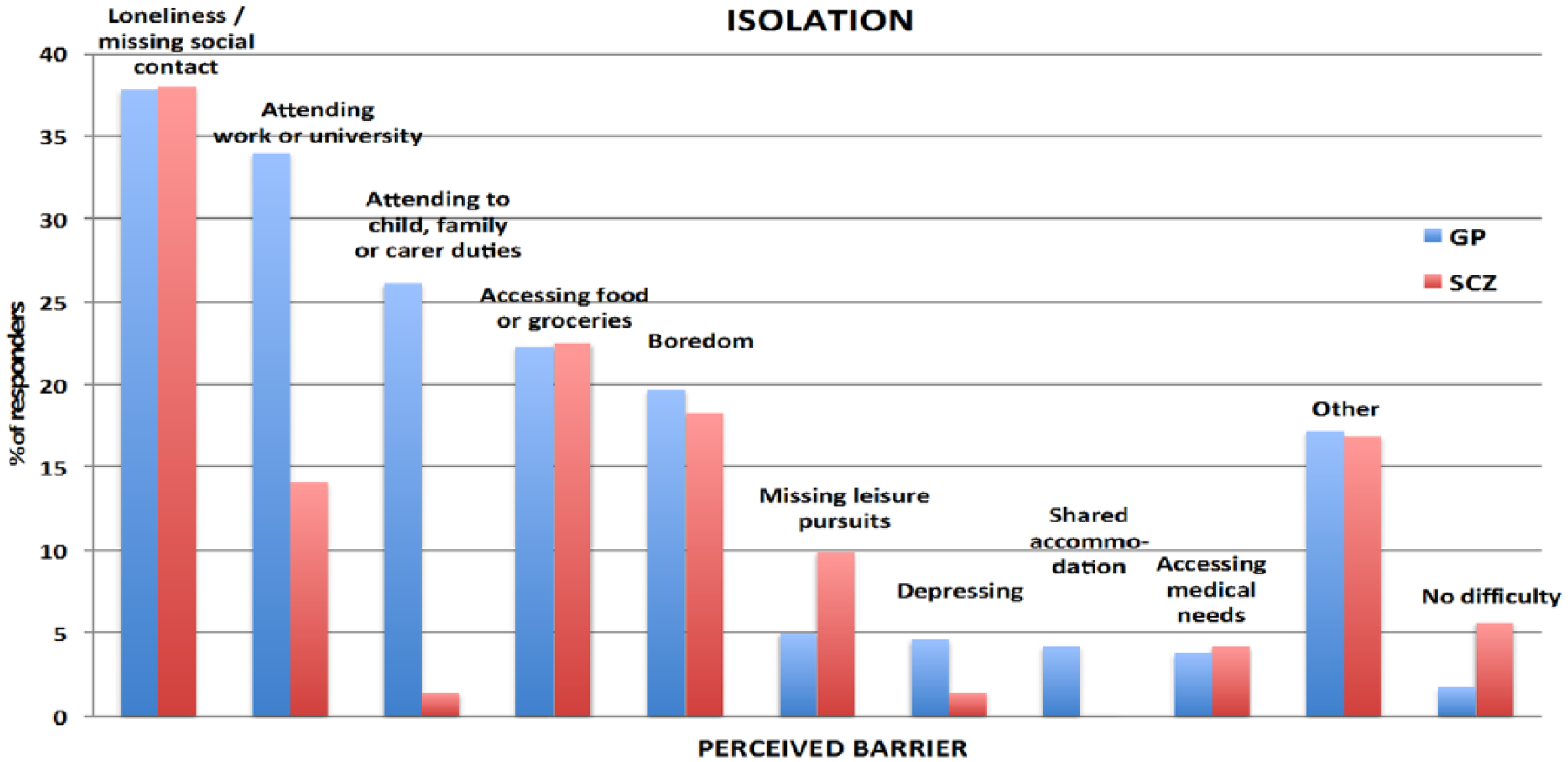
Perceived barriers to isolating oneself.
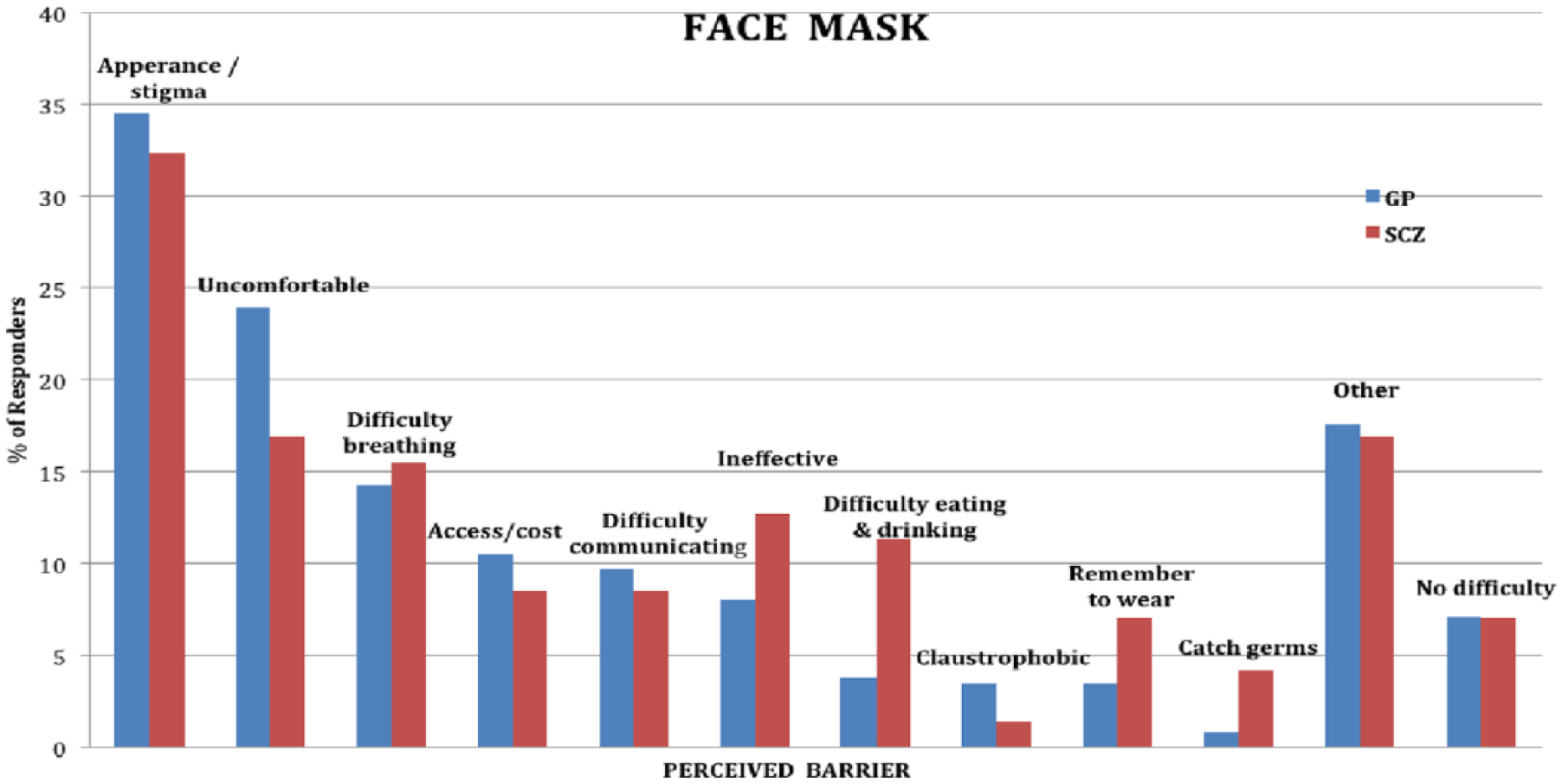
Perceived barriers to wearing a face mask.
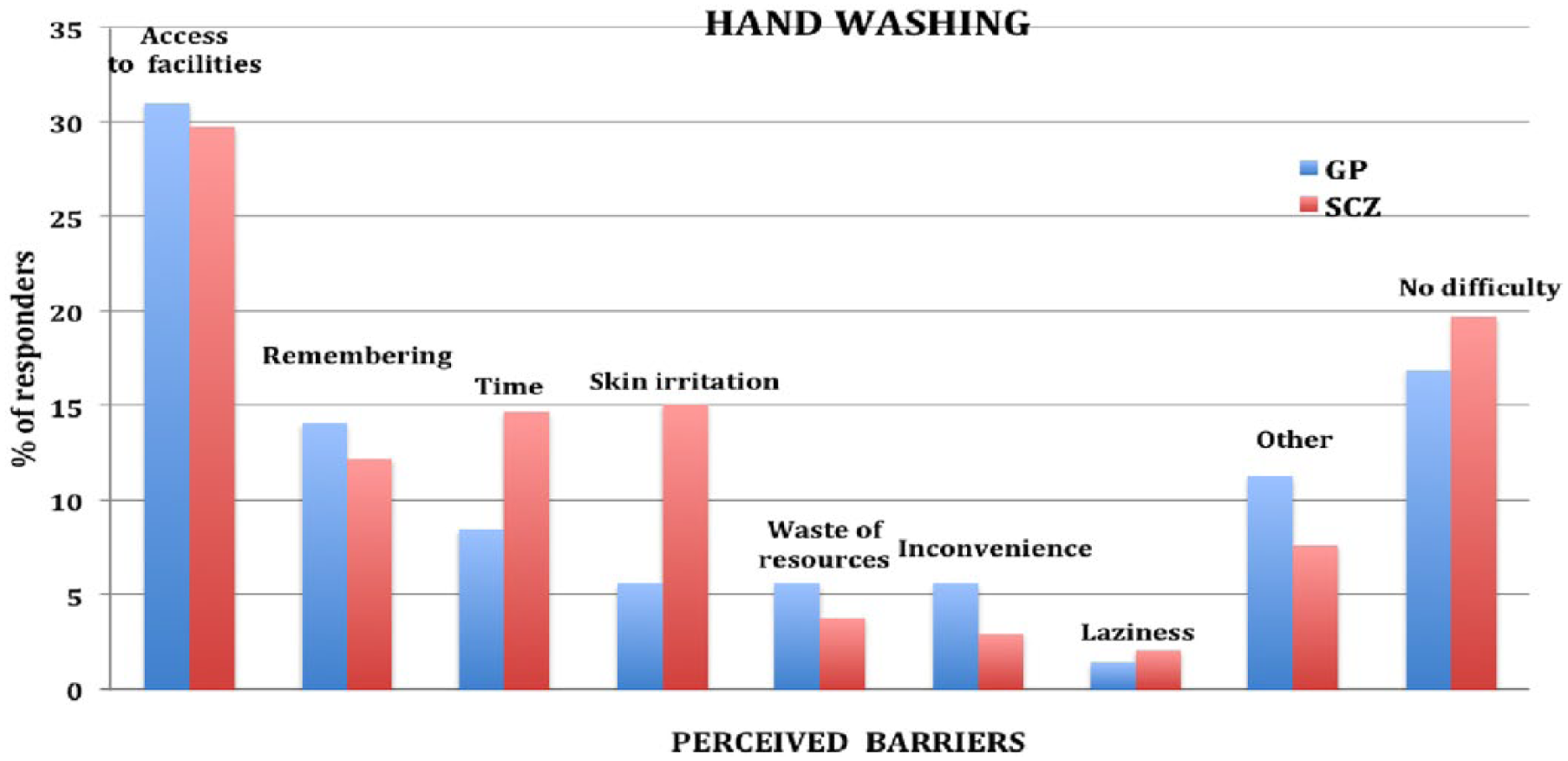
Perceived barriers to increased hand washing.
Summary of commonest perceived barriers for people with schizophrenia

Discussion
The results indicate that most people with schizophrenia attending public mental health services and GP attendees are willing to take protective action against pandemic influenza. In both groups, increased hand washing was the most accepted measure and wearing a face mask the least accepted. Hand washing as a simple, inexpensive and effective protective measure should be a core focus in public health messaging during a pandemic.
Significant perceived barriers exist for each of the protective measures for people with schizophrenia and in the general population. Although there are similarities between the two groups in how they perceive barriers, there are also substantive differences, which are likely to reflect
Limitations of this study include relatively small sample size, self-selection bias and clustering sampling, and the cross-sectional nature of the study.
Conclusion
People with schizophrenia report being generally willing to adopt protective measures, especially increased hand washing, during a pandemic influenza. Understanding and further investigating perceived barriers may enable development of effective interventions to increase uptake of protective measures.
Footnotes
Disclosure
The authors report no conflict of interest. The authors alone are responsible for the content and writing of the paper.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors gratefully acknowledge funding provided by the Private Practice Fund, Canberra Hospital.
