Abstract
Introduction:
Angina bullosa hemorrhagica is a disease without a concomitant hematological or vesiculobullous disorder characterized by painless hemorrhagic bullae in the oral mucosa; it is rarely seen and has a good course.
Case presentation:
A 45-year-old female patient was admitted to the emergency department with a painless hemorrhagic bulla that suddenly appeared on the soft palate. A blister, 2 cm in diameter and dark red in color, was seen extending from the hard palate’s posterior to the soft palate. Nasolaryngoscopic evaluation was performed, and no additional hemorrhagic bulla was detected. She was discharged with the recommendation of oral mouthwash.
Discussion:
Solitary hemorrhagic bulla, suddenly occurring on the soft palate, is diagnostic for angina bullosa hemorrhagica. Some authors have reported that blisters in the posterior pharynx may progress to acute upper airway obstruction.
Conclusion:
Early nasolaryngoscopic evaluation in angina bullosa hemorrhagica is an excellent option to be considered by the emergency physician to prevent life-threatening situations.
Introduction
Angina bullosa hemorrhagica (ABH) is a benign condition characterized by a sudden, rare, red-violet colored hemorrhagic bulla or bullae that can be associated with neither a systemic disease nor a dermatological disease or a hemostatic disorder. 1 It predominantly appears on the soft palate and heals without a trace.1,2 Recurrence may occur in 30% of patients. 3 In more than 35% of cases, a traumatic factor related to hot or solid food plays a role.1,4–6 Besides, hypertension, 4 diabetes mellitus (DM), 3 and long-term steroid use 7 are among the etiological risk factors. The diagnosis is made clinically and has a good prognosis. 8 Here, we present an ABH case to benefit the emergency doctor in diagnosis and treatment since it is not very encountered in emergency medicine practice, and it has a tiny place in the literature.
Case presentation
A 45-year-old female patient was admitted to the emergency department with a painless, blood-filled blister that suddenly appeared on the soft palate after a hard bread she had eaten 2 days ago. She said that her complaint started with a feeling of swelling on the soft palate, but when she saw it in the mirror today, she came to the emergency department with fear. After drinking a hot tea for 6 months ago, she stated that a 3-mm-sized blue spot had formed and passed in the same place. She had no difficulty swallowing and never smoked. She had never seen anything like it in her family. There was no steroid use or inhaler use, no DM, only hypertension. The patient had no medication other than the angiotensin-converting enzyme inhibitor, ramipril. She also had no history of allergies. Of the patient’s vital signs on arrival, only blood pressure was 170/90 mmHg, and other parameters were within normal limits. A painless blister, 2 cm in diameter and dark red in color, was seen extending from the posterior of the hard palate to the soft palate (Figure 1). No other lesions were found, neither on the skin nor in the oral cavity.
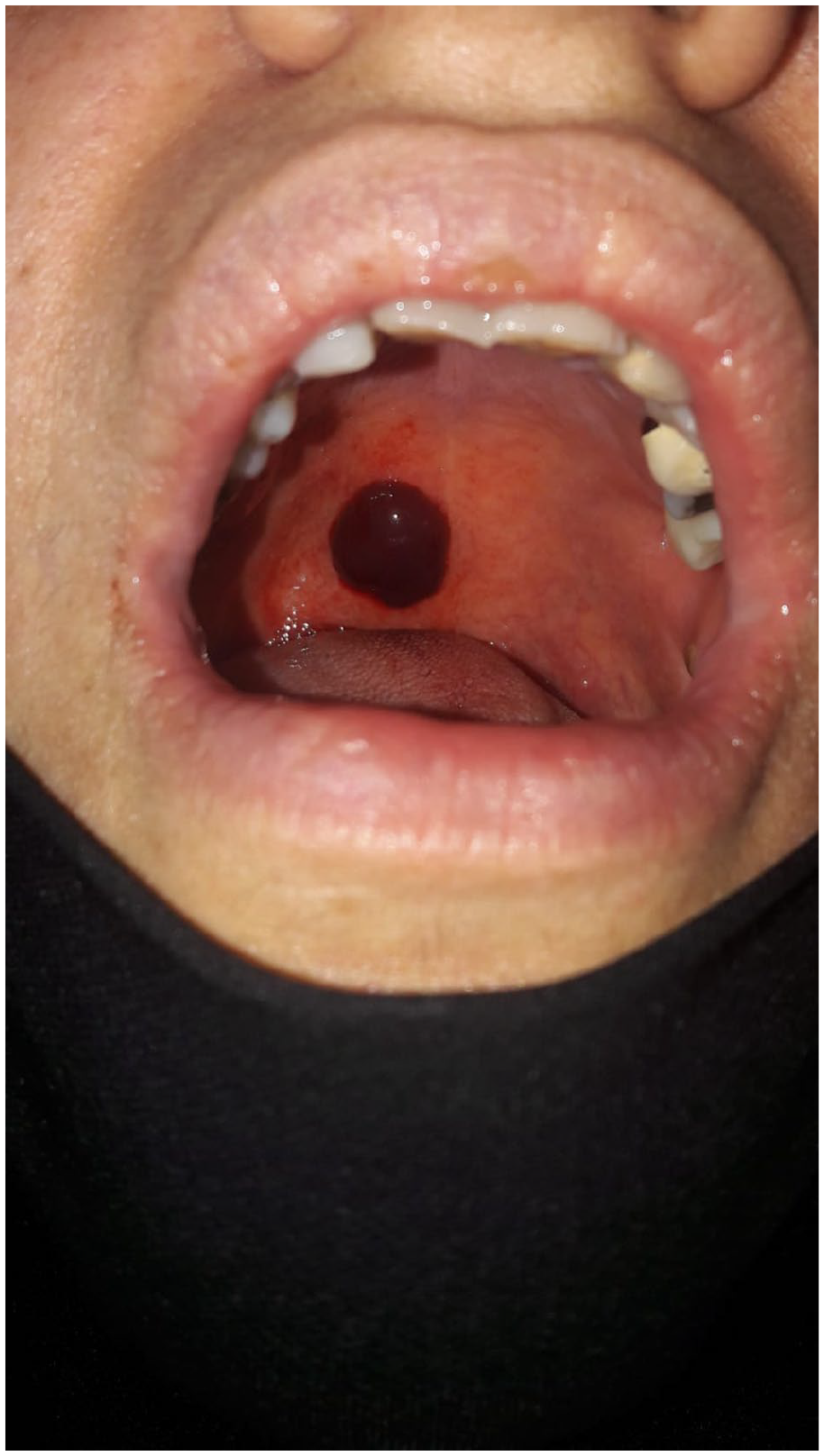
On the day of application, the blister extends from the hard palate’s back to the soft palate.
Complete blood count, erythrocyte sedimentation rate, biochemical values, blood glucose level, and coagulation tests were normal. An otorhinolaryngologist was consulted. Hypopharynx and larynx were checked for possible bleeding with a flexible fiberoptic nasolaryngoscope, and no additional hemorrhagic bulla was detected. After 6 h of follow-up, a combination of 0.15% benzydamine hydrochloride and 0.12% chlorhexidine gluconate was prescribed for use as a mouthwash 3–4 times a day for 5 days. The patient was discharged, emphasizing that she should not consume hard and hot food. In the patient who came for control on the 10th day, it was observed that the lesion passed without leaving a scar on the soft palate (Figure 2).
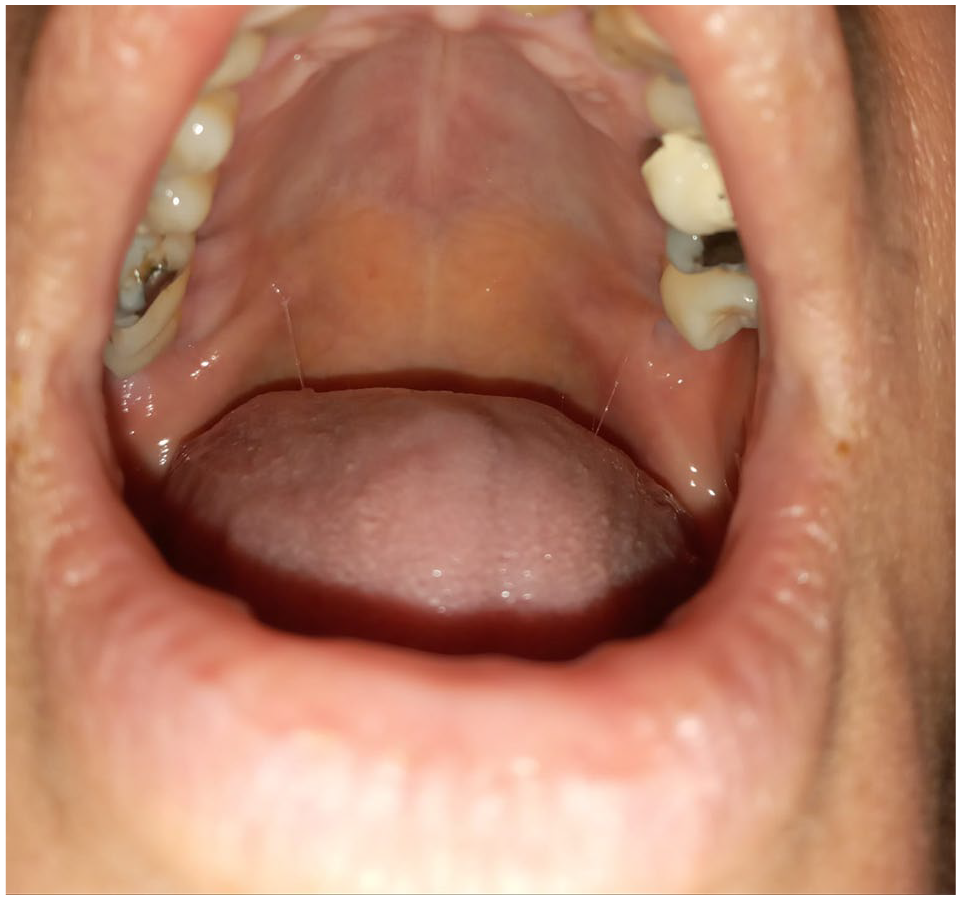
On the 10th day, the lesion healed on the soft palate without any traces.
Discussion
The disease, which was defined as “angina bullosa hemorrhagica” as a new term by Badham in 1967, is a rare, idiopathic condition in the oral mucosa characterized by a blood-filled blister or bulla, which cannot be attributed to a bleeding disorder or is not associated with a systemic disease.1,9 Since the lesions are generally painless, it is suggested that it would be more appropriate to call this disease “stomatopompholyx hemorrhagica,” but this term fell behind the first term. 10
The blister of ABH appears stretched, dark red-purple in color, and filled with blood surrounded by an ecchymotic halo. It has an average diameter of 1–3 cm. 2 The soft palate is the most commonly affected site in ABH. 6
The etiopathogenesis of this disease has not been fully elucidated yet. Loose attachment between the epithelium of the mucosa and corium caused by a genetic cause, or weak anchorage of the mucosal vessels, may cause subepithelial bleeding. 2 Bleeding in the superficial capillaries may occur due to traumatic damage to the epithelial-connective-tissue junction, resulting in subepithelial hemorrhagic bulla formation. 4 Also, vascular fragility in diabetic patients is thought to contribute to ABH. 2 The mechanism of action of corticosteroids in the formation of ABH works by the reduction of submucosal elastic fibers and mucous atrophy, which will easily make the capillaries prone to rupture. 4 It is thought in the etiology that it starts spontaneously or occurs with a traumatic factor mostly due to hot or hard food.1,4–6 Apart from this, it is mentioned that it is caused by anticoagulant 6 or inhaler steroid usage, 11 coughing, sneezing, or screaming.4,12 Hypertension is shown, although its exact relationship cannot be revealed as the underlying disease. 4 In almost half of the patients, the causing factor has not been demonstrated. 12 Women and men are not superior to each other in terms of being affected by this disease. 3 Although it starts to affect adults in the third decade of life, it is most common in the fifth decade.3,4 Our patient was a female in the fifth decade. She was a person with no systemic conditions other than hypertension, who regularly used an angiotensin-converting-enzyme inhibitor, ramipril. The piece of hard bread she ate had drawn her palate.
Although ABH has a good prognosis, some authors have reported that acute upper airway obstruction may develop as a result of a rapidly expanding blister in the posterior pharynx and epiglottic region. 12 The risk of asphyxia is quite low in palatal or pharyngeal lesions. 2 A large bulla in the palatal area can also cause a feeling of suffocation. In such patients, tracheal intubation and surgical tracheostomy may rarely be required. In our patient, airway safety was checked via flexible nasolaryngoscopy, and it was confirmed that there was no additional hemorrhage. We think that evaluation with a video-assisted device is essential for early intervention in such patients.
Solitary hemorrhagic bulla, suddenly occurring on the soft palate, is diagnostic for ABH. Laboratory work can assist in differential diagnosis and treatment. In ABH, platelet count and coagulation tests remain within normal limits. Coagulation tests and platelet count are useful in eliminating blood dyscrasia. No biopsy is required for the vast majority of lesions. 13 The fact that the lesion nature is well limited, rare, rapid healing, and normal blood values makes it efficiently differentiated from thrombocytopenia, ecchymosis, nosebleeds, and various systemic diseases such as pemphigoid, epidermolysis bullosa, and dermatitis herpetiformis. 14 Nevertheless, the diagnostic criteria proposed by Ordioni et al., based on a systematic review of the literature, aimed at improving the care of patients presenting with ABH, are as follows: (1) a clinically noticeable hemorrhagic blister or erosion of the oral mucosa; (2) primarily oral or oropharyngeal localization; (3 palatal localization; (4) a factor that triggers the event (too hot or hard food intake); (5) recurrent lesions; (6) healing within a few days without scarring; (7) painless lesion; (8) no abnormality in platelet count and coagulation test; and (9) negative direct immunofluorescence results. The authors suggested that a combination of at least six of the nine diagnostic criteria (provided criteria I and II are present) should lead to ABH diagnosis. 15
The purpose of the treatment is to provide palliation. Benzydamine hydrochloride or chlorhexidine gluconate can be used as a mouthwash to reduce the damage of topical steroids and prevent infection.8,12 Ascorbic acid intake can contribute to reducing/preventing relapse. 3 Spontaneous healing occurs in 7–10 days.1,13
The information that the process will be benign should be explained to the patients. 10 An emergency doctor should know the risks and should not skip calling the patient again for control, even though it is a disease with a good course, and the probability of threatening airway safety is negligible.
Conclusion
ABH has a good prognosis, and the clinical examination is highly sufficient for diagnosis. Due to the bulla placement, eventual drainage may be required from the risk of airway obstruction and severe problems in eating and drinking. Flexible nasolaryngoscopic evaluation seems to be a useful intervention in the early period.
Footnotes
Acknowledgements
The authors would like to thank Dr Sercan Eroğlu for his assistance and guidance in this research.
Author contributions
M.C.D. and İ.A. researched literature and conceived the study; made a substantial contribution to acquisition, analysis, or interpretation of data; and revised the first draft of the manuscript critically for important intellectual content. M.C.D. wrote the first draft of the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of data and materials
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to their containing information that could compromise the privacy of the patient.
Informed consent
Since the report did not show any identification with the patient involved, there was no need for ethics committee approval. Nonetheless, all procedures on the reported patient were subjected to informed consent. The informed patient consent form was taken and sent as a separate document.
Ethical approval
This case report complies with hospital and journal regulations for publication.
Human rights
All procedures performed on the reported patients were conducted in accordance with good clinical practice respectful of any human rights, and we also carefully read the regulations of human right on submission guideline of Hong Kong Journal of Emergency Medicine.
