Abstract
Introduction:
Transverse myelitis (TM) is a rare inflammatory disorder involving single or multiple spinal segments. There are various Infectious and parainfectious causes.
Case presentation:
We report the case of 29-year-old female who presented to an emergency department with acute urinary retention, progressive headache and sensory and motor deficits with a genital infection. Cerebrospinal fluid (CSF) analysis revealed WBC 75/μL, protein 96 (15-40 mg/dL), and VZV IgG positive. The magnetic resonance image (MRI) of the spine revealed acute transverse myelitis of C4, C6/C7 and T2-T3, T4-T7. She was treated with steroid pulse therapy, intravenous antiviral therapy, antibiotics, and rehabilitation. Urinary symptoms resolved in six days and her motor deficit resolved. She had mild numbness in the thigh area 2 months later.
Discussion:
Identification of the causes and diagnosis of TM are challenging because there are variable clinical signs and numerous potential pathogens.
Conclusion:
It is essential to diagnosis TM in the early and timely phase, careful, detailed history and thorough physical examination by emergency physicians.
Introduction
Transverse myelitis (TM) is a rare inflammatory disorder involving single or multiple spinal segments. TM is a pathobiologically heterogeneous syndrome characterized by acute or subacute spinal cord dysfunction resulting in paresis, sensory-level deficits, and autonomic (bladder, bowel, and sexual) impairments below the level of the lesion. 1
Magnetic resonance image (MRI) is one of the most important examination tools of the entire spinal axis and brain. The location and length of the lesion caused by inflammation are important discriminators with etiologic and prognostic significance. TM can have various causes, such as infectious or post-infectious causes. 2
We report a case of a young woman who repeatedly presented to the emergency department (ED) with progressive symptoms of TM.
Case presentation
A 29-year-old female was admitted to the ED for an acute urinary retention problem. She had not been able to void urine for over 24 h. We examined her vital signs, which were as follows: 129/85 mm Hg, pulse rate 91 beats/min, respiratory rate 20 breaths/min, and body temperature 37.1°C. The patient did not have any fever throughout her stay in the ED. As she again failed to urinate in the ED, we performed urinary catheterization, and the residual urine volume was 550 mL. Her laboratory data revealed no other specific problems. There was no tender point on abdomen. She had myalgia and genitalia pain and lymph node enlargement on the inguinal area. The gynecological examination showed white vesicle on the labium minora and whitish discharge from the vagina. She had a herpetic infection of the genitalia and was treated with an antiviral (famciclovir, Famvir®) at a private gynecologic department 4 days before presenting herself to the ED. We consulted the gynecologic department, and antibiotics were added to antiviral medication for vaginitis. She was discharged from the ED with a Foley catheter and was scheduled for an outpatient department.
After 12 h, the patient revisited the ED for new-onset headache and nausea. Her vital signs revealed as follows: 119/65 mmHg, pulse rate 83 beats/min, respiratory rate 20 breaths/min, and body temperature 37.6°C At this time, she complained that there was mild numbness on her buttock and posterior thigh area for 1 day, saying that the symptoms had aggravated after previous discharge from the ED. Physical examination showed a lowest upper limb motor grade in wrist flexion (GIII/GIII); extension (GII/GII). Lower limb strength was also the lowest on knee flexion (GIII/GIII); extension (GII/GII). Light touch and pinprick sensory decreased below T5. Deep tendon reflex was decreased in biceps and also in triceps. Kernig and Brudzinski signs were negative. She was, thus, referred to a neurologist to rule out viral meningitis. Cerebrospinal fluid (CSF) analysis revealed opening pressure 160 mmH2O, white blood cells (WBCs) 75/µL, lymphocytes (80%), red blood cells (RBCs) 10/µL, protein 96 (15–40 mg/dL), glucose 126 (40–70 mg/dL), and albumin 59.4 (17.7–25.1 mg/dL). Varicella zoster virus (VZV) IgM, herpes simplex virus (HSV) type I IgG, HSV type II, HSV IgM, and venereal disease research laboratory (VDRL) test of CSF were negative. VZV IgG was positive. Chlamydia trachomatis in vaginal swap was also positive. Finally, the spine MRI revealed acute TM at multiple segments of the cervical and thoracic spine. The T2-weighted MRI showed multifocal patchy with high signal intensity of the cervical and thoracic spinal cord. The lesion involved gray matter of the central portion and both anterior and anterolateral of white matter in some part. Signal changes on C4, C6/C7 and T2–T3, T4–T7 were severe (Figure 1). Bacterial and fungal cultures were also negative.
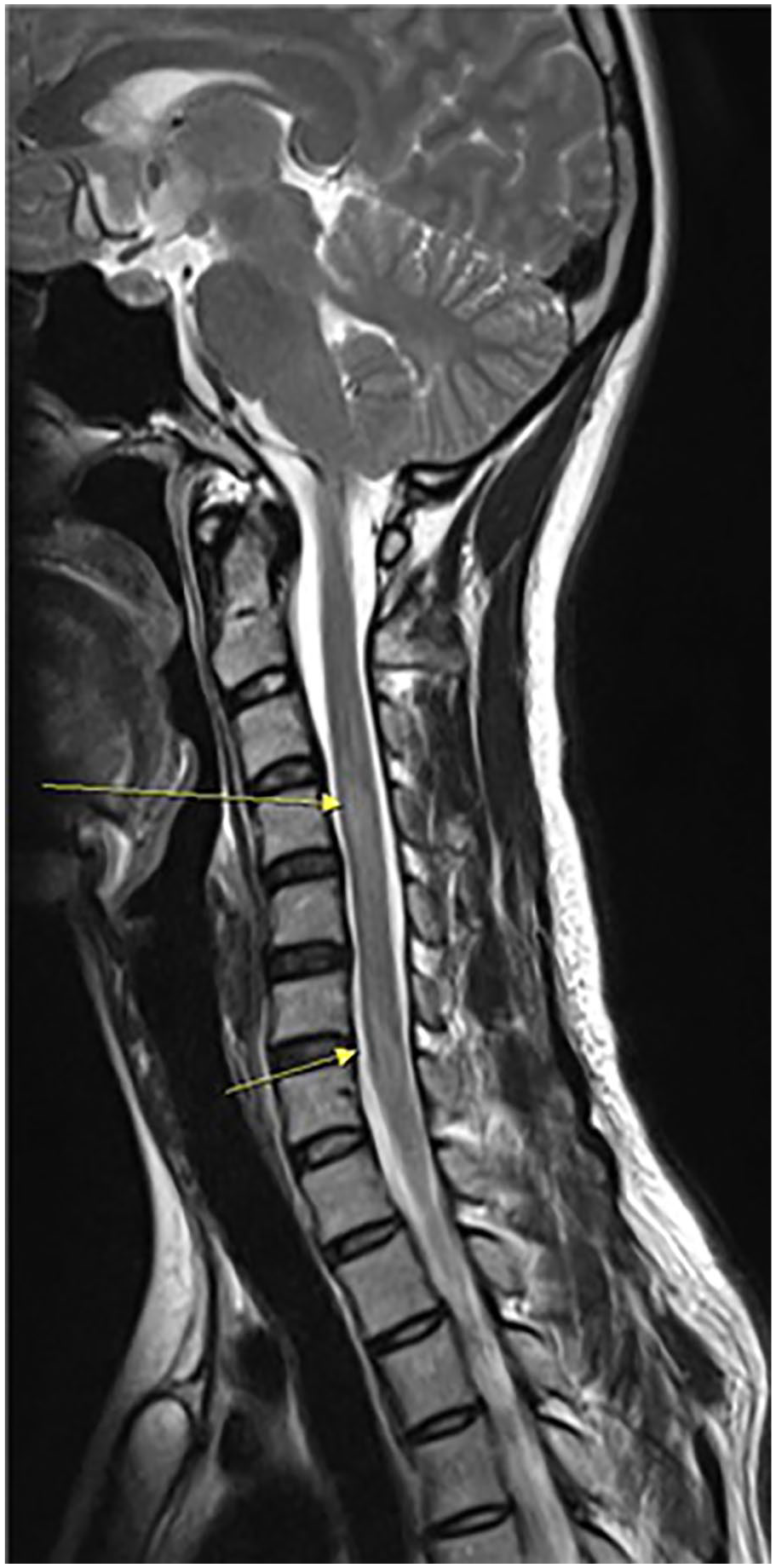
T2-weighted magnetic resonance image of the spinal cord.
The patient was then admitted to the emergency neurology department. She was treated with steroid pulse therapy, intravenous acyclovir of 10 mg/kg every 8 h, metronidazole, and rehabilitation. On the third hospital day, her nerve conduction velocity tests on her arm and leg and tibia and median nerve–evoked potential tests turned out to become normal. On the sixth hospital day, the Foley catheter was removed. On the 10th hospital day, there was no positive result in CSF viral polymerase chain reactions (PCRs), and we, thus, discontinued acyclovir. She was discharged on the 18th hospital day. Her motor neurologic deficits had been resolved. She has mild numbness on the thigh area 2 months later.
Discussion
Many etiologies cause TM, including acquired demyelinating disorders such as multiple sclerosis, systematic inflammatory autoimmune disorders such as systemic lupus erythematosus, and parainfectious of viral, bacterial, fungal, parasitic infections, as well as drugs reactions.1,3 This fact challenges emergency medicine (EM) doctors for finding out its causes. We were able to find out the major cause of our patient’s problem on her second visit to EM.
MRI evaluation of the entire spinal cord axis is mandatory in all patients with myelopathy. MRI excludes structural lesions and provides the location and length of the cord lesions to provide clues about the underlying disease. The most sensitive MRI sequence is the T2-weighted fast spin-echo sequence. 4 In this case, T2-weighted images showed severe signal changes in the cervical (C4, C6, C7) and the upper thoracic spine (T2–T3, T4–T7).
Our patient was treated with an antiviral agent for herpes genitalis. There are reports that HSV causes TM.5–7 There have been two reported TM cases with herpetic genital lesion. 6 We believed that HSV might be the cause of TM. However, CSF PCR for HSV type I and II were negative, whereas only VZV IgG in CSF was positive. It is possible that previous VZV infection or current HSV was the trigger to an abnormal neurotoxic immune response. Chern et al. in their study reported a young woman with TM who had acute urinary retention. Her serum VZV IgG was positive but CSF PCR for VZV was negative. 8 In the present case, we could not rule out other causes of viruses.
Bladder dysfunction is one of the most common and disabling consequences of TM. Generally, three forms of bladder dysfunction may be present: detrusor overactivity (failure to store), detrusor-sphincter dyssynergia, and detrusor hypocontractility (failure to empty). 9 Despite complete motor recovery following TM, bladder dysfunction often persists. 10 Our patient recovered urinary sensation and function in 6 days, while she still had motor deficits.
The management of TM depends on etiology. We administered antiviral agents for viral infection and steroid pulse therapy for inflammation. On the basis of our treatment, high-dose IV corticosteroids (IV methylprednisolone 1 g daily for 3–7 days) should be started as early as possible for all patients with TM. If there is no response to corticosteroids, plasmapheresis should be considered. 11
Voiding dysfunction in women remains a difficult condition to manage. Kavia et al. 12 reported the cause of voiding dysfunction were primary disorder of sphincter relaxation (57.5%), diagnosis unknown (32.0%), neurological (1.2%), pain/structural (1.6%), drugs (4.8%), and so on. Urinary retention and obstructed voiding can occur in women with no neurological or structural problem. Even specialists have difficulty in diagnosing cases of urinary retention in women. Even if a clear diagnosis is not always possible, emergency physician who may meet young women complaining urinary retention in the early stages should keep in mind various causes, including neurologic causes.
Conclusion
Identification of the causes and diagnosis of TM are challenging because there are various clinical signs and numerous potential pathogens. We reported a patient’s revisit to the ED complaining of acute urinary retention, headache, and progressive paraplegia with genital infection. To diagnose TM in the early phase, careful and detailed history and thorough physical examination are essential.
Supplemental Material
consent – Supplemental material for Acute urinary retention and progressive paraplegia with genital infection: A case report of transverse myelitis
Supplemental material, consent for Acute urinary retention and progressive paraplegia with genital infection: A case report of transverse myelitis by Eun Kim and Duk Hee Lee in Hong Kong Journal of Emergency Medicine
Footnotes
Authors’ contribution
D.H.L. and E.K. have made substantive contributions to the study, and all authors endorse the data and conclusions.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of data and materials
This case report has no restrictions on the availability of data and materials.
Ethical approval and human right
All authors adhered to the Helsinki Declaration; patient confidentiality and anonymity were preserved.
Informed consent
Written consent was obtained from the patient to publish and educate the case with anonymized data.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
