Abstract
Scaphoid fractures represent the most common carpal injury, particularly prevalent among younger populations. 1 The unique vascular anatomy of the scaphoid predisposes proximal fractures to elevated risks of avascular necrosis and nonunion.2,3 These complications significantly hinder functional recovery and diminish patients’ quality of life.4,5 Conventional therapeutic approaches, including open bone grafting or vascularized bone flap grafting, demonstrate limited efficacy with union rates ranging from 40% to 80%. 6 This is primarily attributed to the fact that open surgery may further disrupt the scaphoid’s blood supply, thus increasing the risk of nonunion and leading to scarring and adhesions in the joint capsule. 6 These limitations highlight the need for more precise and minimally invasive treatment approaches.
Since its inaugural application in scaphoid nonunion management in 2003, arthroscopic techniques have demonstrated satisfactory therapeutic outcomes. 7 Arthroscopy-assisted bone grafting combined with screw fixation minimizes iatrogenic soft tissue trauma and vascular compromise, thereby reducing postoperative complication rates.8–10However, traditional arthroscopic surgery requires extensive fluid irrigation to maintain the surgical field, and prolonged irrigation can result in soft tissue swelling or even compartment syndrome. Additionally, fluid leakage may cause a loss of visibility and complicate the bone grafting process. 11 Therefore, it is of vital importance to seek a technology that can effectively improve the surgical field of view and reduce complications.
Drawing inspiration from laparoscopic and thoracoscopic procedures, this study pioneered the implementation of pulsed carbon dioxide (CO2) gas insufflation technology in wrist arthroscopic surgery. The pulsatile CO2 delivery system effectively resolves the dual challenges of visual obscuration and graft displacement associated with liquid irrigation. 12 The pulsed CO2 gas arthroscopy not only enhances the clarity of the surgical field, particularly in cases of synovial hyperplasia or multiple fracture fragments, but also mitigates the adverse effects of fluid irrigation on visualization.
Accurate reduction of the scaphoid is essential for successful postoperative healing. However, the unique morphology and anatomical location of the scaphoid present significant technical challenges for screw implantation. 13 The advent of robot-navigated technology has considerably enhanced the precision and safety of orthopedic surgical procedures, especially in the reduction and fixation of complex fractures. 14 Utilizing robot-navigated technology enables precise screw placement, thereby minimizing human error and enhancing surgical stability.
In light of the aforementioned background, this study endeavored to evaluate the effectiveness and safety of pulsed CO2 gas arthroscopy in conjunction with autologous iliac bone grafting and robot - navigated screw fixation for the treatment of scaphoid nonunion. It was anticipated that the application of this innovative technology will provide a more precise, low - risk, and efficient treatment modality for scaphoid nonunion, ultimately improving functional outcomes and enhancing the quality of life for patients.
Methods
Inclusion Criteria:(1) radiologically confirmed scaphoid nonunion persisting for >6 months, (2) failure of conservative management, and (3) willingness to undergo surgical intervention with signed informed consent.Exclusion criteria: (1) severe cardiopulmonary/hepatic/renal dysfunction, (2) psychiatric disorders impairing treatment compliance, and (3) active local or systemic infections.
The cohort comprised 18 patients (11 males, 7 females) aged 20-55 years (mean 34 ± 5 years) with injury durations of 19 ± 7 months. Fracture distribution included 12 waist fractures, 2 distal pole fractures, and 4 proximal pole fractures, with two cases exhibiting scaphoid humpback deformity.
Surgical methods
All patients were treated in accordance with the Declaration of Helsinki. All patients had signed the surgical consent form.
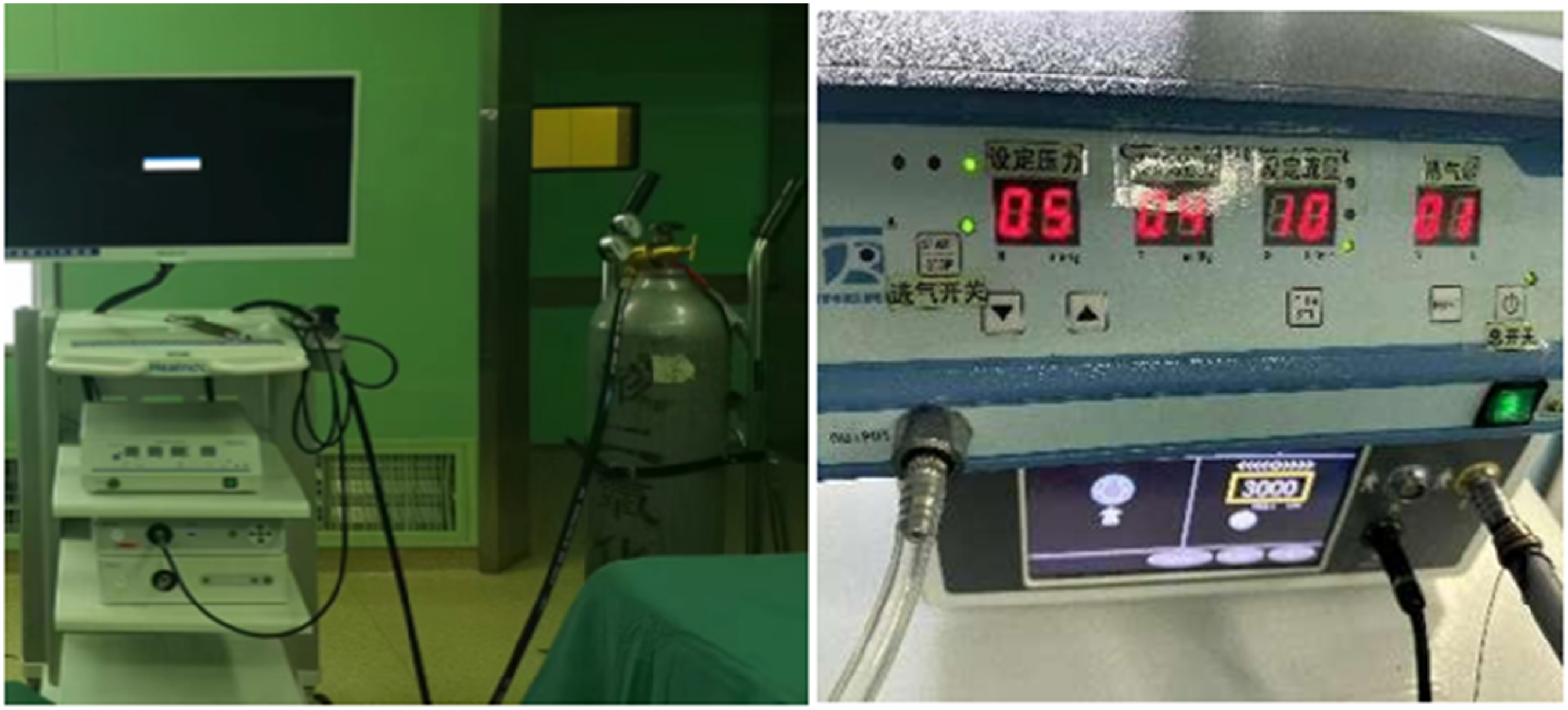
The surgery was conducted under general anesthesia with the patient positioned supine. A pneumatic tourniquet was routinely applied to the upper arm. (1) Wrist arthroscopic approach: The wrist arthroscopic tower maintained a traction force of 5 - 7 kg. The scope was routinely inserted through the dorsal 3/4 and 4/5 portals of the wrist to examine for any combined cartilage, ligament, and triangular fibrocartilage complex injuries in the radiocarpal joint. The wrist joint scope and operating instruments were inserted through the ulnar and radial portals of the midcarpal joint, respectively, to examine the midcarpal joint. (2) Examination content: The scaphoid fracture line was observed with a focus on identifying any obvious steps or displacement at the fracture line and whether fibrous hyperplasia had connected the proximal and distal fracture fragments. The presence of synovial hyperplasia in the midcarpal joint was also examined. The hyperplastic synovium was debrided using a bur head and radiofrequency head, followed by grinding the scaphoid fracture gap surface with a grinding drill to remove sclerotic bone while protecting the cortical bone shell (Figures 1 and 2). (3) Fracture reduction and fixation: The scaphoid was reduced under continuous fluoroscopy using a C - arm machine. If the fracture displacement or hump deformity was significant and manual closed reduction was difficult, 1.0 - 1.2 mm Kirschner wires were inserted percutaneously into the proximal and distal fracture fragments as manipulators. After reduction under the arthroscope, fixation was achieved by prying and fixing. For waist fractures or distal fractures, fixation was performed with Kirschner wires from the scaphoid tubercle; for proximal or proximal 1/3 fractures, percutaneous fixation via the dorsal approach was used to ensure stability of the proximal fracture fragment. (4) Pulsed CO2 gas arthroscopy for iliac bone grafting: A cortical window was routinely opened at the iliac crest. Fine cancellous bone was dug out using a spoon, wrapped with gauze, and then crushed into a bone paste with a bone hammer. The cortical flap at the iliac crest was repaired in situ. Under the MCR or MCU pathway, the irrigation fluid pipeline was replaced with CO2 gas used in laparoscopy. The CO2 gas pipeline was connected to the arthroscopic sheath through a three - way tube, with the injector needle head at the 6U pathway retained to facilitate CO2 gas escape.
15
The gas pressure was set at 5mmHg, the flow rate at 10 mL/min, and it was injected in a pulsed manner to flush away bleeding at the fracture end and obtain a clear field of view.
15
Cancellous bone fragments were placed into the scaphoid fracture gap multiple times through a 3.5 mm cannula and pressed and filled with a tamper until full (Figures 3–5). (5) Orthopedic robot-navigated(Tianji Orthopedic Robot, China) screw internal fixation: The affected limb was fixed on the TPU bracket using a surgical membrane, with the wrist joint maintained in a dorsiflexed position to prevent movement during the operation and reduce the accuracy of screw placement. The robot positioning sensor was fixed on the TPU bracket. The scaphoid was positioned in the middle area using anteroposterior and lateral fluoroscopy of the C - arm X - ray machine. A ring scan was performed to collect three - dimensional images of the sagittal, coronal, and axial planes of the affected side scaphoid, and the data were transmitted to the robot workstation. The planning of the screw entry point, entry direction, and path was visualized on the three - dimensional image. The screw placement path was inspected through the three - dimensional reconstruction image, and fine - tune adjustments were made to the screw position to place it on the central axis of the scaphoid. The designed entry point and path were adjusted and confirmed to be in the optimal position of the scaphoid. The size of the screw and Kirschner wire was then adjusted. After planning, the robotic arm was controlled to the screw planning position until the control interface prompted an error of < 1 mm. After confirming the planning and design, the robot automatically adjusted the robotic arm according to the designed parameters and navigated to the designed entry point and entry direction. The cannula was inserted, and a 1.2 mm guide wire was driven into the scaphoid fracture through the cannula. After fluoroscopy confirmed that the path was consistent with the plan, a 2 - 3 mm skin incision was made at the entry point, a hole was drilled with a cannulated drill, and the Herbert compression screw with the planned diameter and length was screwed in. The fracture end alignment, screw length, and position were confirmed to be consistent with the navigation plan by fluoroscopy of the C - arm X - ray machine. The guide wire and robot sensor were then removed (Figure 6). Intraoperative nonunion of the scaphoid fracture was seen, Hyperplasia of fibrous and synovial tissue at the fracture site. The hyperplastic synovium was removed, and the scaphoid bone was ground with a grinding drill until the fracture block appeared to ooze blood in spots. Taken from the iliac bone of the body. Intraoperatively, a pulsed CO2 gas system was connected and the parameters of the device were adjusted, with the pressure set at 5 kPa and the flow rate at 10 mL/min. Under pulsed CO2 gas arthroscopy, cancellous bone fragments were placed into the scaphoid fracture gap multiple times through a 3.5 mm cannula and pressed and filled with a tamper until full. The orthopaedic robot was used to select the optimal screw entry point, direction of entry and path of travel, and the Herbert compression screw was screwed in.





Rehabilitation protocol
Immediate postoperative mobilization of the metacarpophalangeal and interphalangeal joints was initiated. At 1 week postoperatively, adjunctive electromagnetic therapy (HP400 Osteogenesis Stimulator) was administered to enhance fracture healing, complemented by physiotherapy to restore articular range of motion. A short-arm brace was applied at 6 weeks for wrist immobilization, which was discontinued upon radiographic and clinical confirmation of union. Patients subsequently commenced active wrist flexion-extension and pronation-supination exercises under supervised rehabilitation. Weight-bearing activities were strictly prohibited during the 6-month postoperative period.
Statistical methods
Statistical analysis was performed using SPSS 26.0 software. Normally distributed data (verified by the Shapiro - Wilk test) were presented as mean ± standard deviation. Intergroup comparisons were conducted using the independent - samples t - test or the Mann - Whitney U test, while pre - and postoperative data were compared using the paired t - test or the Wilcoxon signed - rank test. The significance level was set at p < .05.
Results
The study cohort comprised 18 patients with follow-up durations of 12-16 months (mean 14.3 ± 1.8 months). Mean operative time was 103 ± 35 minutes, with CO2-assisted grafting requiring 23.3 ± 6.2 minutes. Intraoperative blood loss averaged 80 ± 25 mL, and hospitalization duration was 4.0 ± 1.5 days.
Radiographic parameters demonstrated significant improvement in scapholunate angle from preoperative 61.8 ± 11.6° to postoperative 52.9 ± 7.0° (t = 6.23, p < .001). Fracture union rates progressed as follows: 38.9% (7/18) at 2 months, 88.9% (16/18) at 3 months, and 100% (18/18) at 6 months postoperatively.
Wrist functional results at 6 months(‾x±s).

Typical case
The patient,a male, 26 years old, who suffered a nonunion of a right scaphoid fracture for 9 months as a result of a cycling fall. Arthroscopic removal of sclerotic bone and bone grafting of the posterior iliac bone for internal fixation at the wrist; the patient’s pain was relieved and wrist function was improved after the operation (Figures 7–10). Preoperative X-ray and CT examination of the patient, Suggests that the patient’s scaphoid fracture is not healing. Intraoperative X-rays showed the fracture to be well aligned and centrally fixed with Herbert compression screws. CT scan at 3months postoperatively, the scaphoid fracture was seen to have healed and the Herbert compression screws were fixed centrally in the axis of the scaphoid bone. After 6months postoperatively, the patient had good left wrist flexion and extension movements.Grip strength of 35 kg and pinch strength of 10 kg.



Discussion
Approximately 10% of scaphoid fractures result in nonunion.16,17 Scaphoid nonunion predominantly occurs in cases with >1 mm displacement, proximal pole fractures, and occult fractures that evade timely diagnosis. 18 The vascular anatomy of the scaphoid plays a critical role, with 70%-80% of the proximal region supplied by dorsal vessels, while the distal 20%-30% received vascularization from the tubercle branches. 4 Morsy et al. 19 classified scaphoid morphology into Type I (capitate fossa index [CFI] ≤0.5, waist index [WI] ≥0.4) and Type II (CFI >0.6, WI <0.4) through CT-based 3D reconstructions. Their findings revealed that Type I scaphoids possessed more extensive intraosseous vascular anastomoses, potentially explaining the heightened susceptibility of slender Type II variants to avascular necrosis.
Untreated or mismanaged scaphoid fractures may progress to nonunion, avascular necrosis, flexion deformities, and eventual scaphoid nonunion advanced collapse (SNAC) through progressive articular cartilage degeneration. 20 Current treatments for scaphoid nonunion are mostly based on the removal of unhealthy bone and fibrous tissue, correction of malalignment of the carpal bones, bone grafting, and rigid fixation. 21 In recent years, an increasing number of scholars have adopted arthroscopic - assisted bone grafting for the treatment of scaphoid nonunion. 22 Hsiung et al. 8 reported a series of 41 patients with unstable scaphoid nonunion treated with arthroscopy combined with bone grafting, achieved a healing rate of 92.6% (38/41).Compared with the contralateral wrist joint, patients regained almost the entire range of motion.A multicenter prospective study further demonstrated 93.5% success (72/77 cases) using arthroscopic cancellous grafting. 23 Cheng et al. 24 summarized the main advantages of arthroscopic surgery for scaphoid nonunion, which include: (1) Direct fracture characterization and debridement under magnification, (2) Concurrent management of concomitant injuries, (3) Percutaneous reduction via arthroscopic probes, (4) Real-time articular surface surveillance during screw placement, and (5) Minimized soft tissue trauma promoting early rehabilitation.
While arthroscopic surgery for scaphoid nonunion yielded satisfactory outcomes, it was associated with a significantly prolonged surgical duration compared to traditional open surgery. Wong et al. 4 documented mean operative times of 213 minutes (range: 90-420) for fluid-based arthroscopy, consistent with our initial experience. In summarizing our practical experience, we found that prolonged fluid irrigation may lead to fluid infiltration into tissues, causing swelling of the surrounding soft tissues. During bone grafting, fluid lavage may cause bone graft fragments to float and displace, or even enter other joint spaces, thereby increasing the time required to manage free - floating bone fragments.To address the impact of fluid irrigation on arthroscopic surgery, del Piña et al. 25 proposed the dry - wrist arthroscopic technique. Similar to traditional techniques, this dry - wrist arthroscopic technique eliminated fluid irrigation, but it also brings a series of new challenges. The main issue was that blood or soft - tissue debris may splash onto the lens, causing visual blurring and even the so - called “red sea” phenomenon. 12 Although the visual field can be cleared by removing the arthroscope and wiping the lens with a wet sponge, this procedure is time - consuming. Moreover, in surgeries for chronic scaphoid nonunion, it is necessary to use a bur head to debride the fracture ends, remove fibrous tissue or cystic changes, and use a grinding drill to smooth the scaphoid fracture gap and remove sclerotic bone. These operations necessitate timely irrigation to remove bone debris and fibrous tissue, ensuring the smooth progression of the surgery.
Drawing inspiration from laparoscopic surgery, we first proposed a surgical method of wrist arthroscopic pulsed CO2 gas arthroscopy, based on the principle of pneumoperitoneum. By connecting the pulsed CO2 gas outlet tube to the inlet of the wrist arthroscope, we found that the two can be closely integrated.CO2 gas arthroscopy had been widely used in surgical operations. Although there had been reports of complications such as gas embolism, CO2 entering the bloodstream, and CO2 accumulation due to excessive insufflation, its safety had long been confirmed in both adults and children. Complications associated with CO2insufflation primarily stem from direct puncture of blood vessels (or abdominal organs) by the Veress needle and excessively high pressure during pneumoperitoneum establishment. 29 Given the wrist joint’s location at the limb’s distal end, the risk of damaging major blood vessels during wrist arthroscopic approach establishment is minimal. CO2gas exhibits excellent diffusion and can bind to blood cells. When it enters the bloodstream through a ruptured vessel or is forced into surrounding veins under high pressure, the vast majority enters the pulmonary circulation and is expelled. Minor CO2 gas embolisms typically cause no significant symptoms and thus have little clinical significance. 30 Overall, CO2 gas embolism incidence is low, with severe cases being extremely rare and reported at less than 1% in the literature. 31 To mitigate potential CO2 - related risks, we implemented three key safeguards: (1) Low - pressure pulsed insufflation: Gas pressure was maintained at 5 mmHg with a flow rate of 10 mL/min, which is significantly lower than laparoscopic standards (typically 12 - 15 mmHg), thereby minimizing intravascular absorption risk. (2) Open - system design: The drainage needle at the 6U pathway was retained to allow the CO2 gas in the wrist joint to be discharged spontaneously, thereby preventing intra - articular pressure buildup. (3) Short exposure duration: Compared with traditional laparoscopic surgery, CO2 gas was used for a shorter duration during bone grafting in this study.During the surgical procedure, the patient’s vital signs were closely monitored to promptly detect and manage any potential complications.No discomfort or complications related to pulsed CO2 gas arthroscopy were observed in any patients during or after the operation.Similar to dry arthroscopy, pulsed CO2 gas arthroscopy helps preserve cellular growth factors and other progenitor cells within the bone graft, thereby promoting bone healing.In our cohort, the mean CO2-assisted grafting duration was 23.3 ± 6.2 minutes. While direct comparisons with historical controls (e.g., 167.5 minutes reported by Yi et al. 14 for traditional arthroscopy) should be interpreted cautiously due to potential confounding factors such as surgeon experience and case complexity, our observed total operative time (103 ± 35 minutes) suggests that pulsed CO2 insufflation may enhance procedural efficiency by reducing graft displacement and minimizing intraoperative interruptions for debris clearance.
In the management of scaphoid nonunion, autologous bone grafting was routinely employed and primarily classified into vascularized and nonvascularized bone grafting. Studies had shown that both vascularized and nonvascularized bone grafting yield comparable outcomes in terms of healing rate, healing time, and functional recovery. However, the vascularized group exhibits a higher graft failure rate. 26 Additionally, vascularized bone grafting is a more complex procedure, requiring a longer duration and the utilization of vascular microsurgery techniques. It may also lead to heterotopic ossification, which can restrict the mobility of the wrist joint. 27 In contrast, nonvascularized bone grafting provides osteoconductive properties and osteogenic precursor cells, and is commonly used to treat nonunion. The distal radius and iliac crest are frequently employed as donor sites for autologous bone. However, the structural integrity of the donor site at the distal radius is relatively poor, and its strength is compromised after bone harvesting. 13 To promote scaphoid fracture healing, it is essential to ensure good bone contact and stable graft fixation. Cancellous bone grafts should be impacted into the fracture defect area, with the graft volume being approximately 3 to 5 times the size of the defect. 25
Research had shown that aligning the screw insertion direction parallel to the long axis of the scaphoid enhances biomechanical strength while minimizing disruption to the scaphoid’s blood supply. 28 Robotic three - dimensional navigation technology provides an accurate, rapid, and safe method for internal fixation of non - displaced and displaced scaphoid fractures, enabling precise one - time localization of the optimal central axis. 14 The robot can performed real - time three - dimensional image reconstruction, accurately plan the screw placement points during surgery, measure screw length, and guide the position and direction of the screw, with an error margin of less than 1 mm.In contrast, the manual insertion of a guide wire under fluoroscopy is prone to instability, as even slight tremors can cause significant deviations in positioning, often necessitating multiple attempts and exposing the patient to additional radiation. Repeated guide wire insertions can also lead to increased soft - tissue injury, enlarged the wire tracts, and even fragmentation of bone fragments, making fracture fixation more difficult and less secure. 8 By contrast, the robot, guided by its manipulator arm, achieves much more precise positioning. The guide wire is inserted through a preset rigid tube, greatly enhancing stability and significantly reducing human - induced errors. In this study, both guide wire and screw placement were completed in one go during the operation. By combining three - dimensional reconstruction with precise navigation, we minimized iatrogenic damage and achieved optimal internal fixation.
The fundamental innovation of this study resides in the pioneering adaptation of laparoscopic CO2 insufflation technology to wrist arthroscopy, representing the first documented application of gas-based visualization in carpal surgery. This technological breakthrough, synergized with autologous grafting and robotic navigation, specifically addresses the cardinal challenge in scaphoid nonunion management: preservation of precarious vascular integrity. The combination of these technologies conferred significant advantages in enhancing surgical outcomes and reducing recovery time.This study aligns with the concept of precision medicine and possesses the following merits:(1)Guided by the robotic system, the appropriate - length screws can be precisely selected and accurately implanted, thereby reducing surgical trauma and promoting fracture healing.(2)The surgery employs minimally invasive techniques, minimizing iatrogenic injury and exerting a relatively minor impact on the blood supply surrounding the scaphoid.(3)The pulsed CO2 gas insufflation enhances the efficiency of bone grafting.However, this study also has the following limitations:(1)The high cost of orthopedic robots restricts the widespread application of this technology.(2)Robot-navigated technology demands that patients remain completely still during the procedure; any limb movement can compromise the accuracy of positioning.(3)Intraoperatively, it may be necessary to adjust the CO2 pressure and flow rate according to the actual situation.(4)Wrist arthroscopic techniques have a certain learning curve, and the bone grafting operations under the scope are somewhat challenging.
The integration of pulsed CO2 gas arthroscopy and robot-navigated screw fixation represents a significant advancement in the treatment of scaphoid nonunion. While not all institutions may have access to these technologies, our study suggests that the adoption of these techniques can lead to improved surgical outcomes, reduced recovery times, and enhanced functional prognosis. The use of pulsed CO2 gas arthroscopy addresses the challenges associated with traditional arthroscopic irrigation, providing clearer visualization and reducing the risk of complications. Additionally, robot-navigated screw fixation enhances the precision and accuracy of screw placement, minimizing human error and improving overall surgical stability.
However, it is important to note that the benefits of these technologies may not be universally applicable. Institutions without access to pulsed CO2 gas arthroscopy and robot-navigated may still achieve satisfactory outcomes using traditional arthroscopic or open surgical techniques. The key to successful treatment of scaphoid nonunion lies in the accurate reduction and stable fixation of the fracture, regardless of the specific technology employed. Therefore, while the combination of pulsed CO2 gas arthroscopy and robot-navigated screw fixation offers significant advantages, it is not a prerequisite for successful treatment. Future research should focus on comparing the outcomes of this novel approach with traditional methods in larger, multicenter studies to provide more robust evidence for clinical practice. Additionally, efforts should be made to develop more cost-effective and accessible technologies that can bring the benefits of precision medicine to a broader range of patients.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Jiangsu Province Xuzhou City Health Commission Youth Project for Medical Science and Technology Innovation (XWKYHT20240041).
Ethical Statement
Data Availability Statement
All authors had full access to the data, contributed to the study, approved the final version for publication, and take responsibility for its accuracy and integrity.
