Abstract
Background
The purpose of this study was to assess whether China-made robot-assisted medial UKA can improve prosthesis placement accuracy and yield superior short-term outcomes compared with conventional UKA.
Methods
50 patients who underwent initial medial UKA were included in this single-center, prospective, parallel, randomized, controlled trial. Preoperatively, patients were randomly categorized the robot-assisted UKA group and conventional UKA group. The operation time, intraoperative blood loss, postoperative pain scores (VAS scores at 24 h, 72 h, and 3 months post-surgery), KSS scores (clinical and functional scores), and knee range of motion (ROM) were compared between the two groups. The coronal deviation values of the femoral component, tibial component, and knee joint line height change were also compared between the two groups.
Results
The deviations in tibial component coronal plane alignment, femoral component coronal plane alignment, and joint line height change were significantly smaller in the robot-assisted group compared to those in the conventional group (p < 0.05). The operation time of the robot-assisted group was longer than that of the conventional group (p < 0.05). At 24 h and 72 h postoperatively, patients in the robot-assisted group reported lower VAS scores compared to those in the conventional group (p < 0.05). No significant differences were observed between the two groups regarding intraoperative bloodloss, the VAS scores at 3 months postoperatively, the KSS scores (clinical scores and functional scores) at 3 months postoperatively, and the Knee range of motion at 3 months postoperatively.
Conclusions
The China-made UKA robot can enhance the precision of prosthesis placement, yielding favorable short-term therapeutic outcomes.
Introduction
Knee osteoarthritis commonly accumulates in the medial compartment, 1 Medial Unicompartmental knee arthroplasty (UKA) is an effective treatment for medial compartment osteoarthritis. Compared to total knee arthroplasty (TKA), UKA offers advantages such as less trauma, faster recovery, and a minimal risk. With the continuous advancement of UKA technology, there has been a further increase in its utilization. 2 However, compared to TKA, medial UKA have higher rates of revision and prosthetic loosening, which partially negate the minimally invasive advantages of medial UKA. 3 Study have confirmed that prosthesis malalignment is one of the main reasons for UKA revision and prosthesis loosening. 4 In order to improve the accuracy of prosthesis placement during UKA and achieve more precise control over soft tissue balance, China-made assistant robot systems have emerged. Nevertheless, their application is still in its early stages with limited related reporting available. 5 The aim of this study is to compare the short-term efficacy differences between China-made Zhengtian robot-assisted medial UKA and conventional medial UKA through a prospective controlled trial. We hypothesize that China-made robot-assisted medial UKA can improve prosthesis placement accuracy and yield superior short-term outcomes.
Subjects and methods
Study subjects
50 patients scheduled for initial medial unicompartmental knee arthroplasty (UKA) at the Department of Arthropathy, Sixth Affiliated Hospital of Xinjiang Medical University from January 2023 to January 2024 were consecutively enrolled. After obtaining informed consent from patients and their families, they were assigned a treatment number in sequential order. Patients were then randomized in a 1:1 ratio using computer-generated randomization into either the robot-assisted UKA group or conventional UKA group. Patients will be blinded to the allocation until the first postoperative days. Surgeons and personnel involved in the clinical management of the patients will be unblinded to the allocation. All surgeries were performed by the same experienced surgeon, and postoperative rehabilitation was conducted under the guidance of a consistent professional team. (Figure 1). Flow diagram of the subjects.
Inclusion criteria
(1) Medial compartment osteoarthritis of the knee, Kellgren-Lawrence classificationⅢ and Ⅳ (Table 1), Conservative treatment does not work for at least 3 months, (2) Age between 55 to 75 years old for both sexes, (3) Body mass index (BMI) ≤30 kg/m2, (4) Intact anterior cruciate ligament, Knee varus deformity ≤15°,without significant flexion contracture deformity, (5) No systemic or local infection present. Kellgren Lawarence classification.

Exclusion criteria
(1) Previous history of knee surgery, (2) Severe knee varus or valgus deformity (>20°), accompanied by severe knee extension disorder, (3) Obvious cartilage destruction on weight-bearing surface of lateral compartment in affected knee joint, (4) Patients with severe medical or surgical conditions that make them unable to tolerate surgery,
General conditions of the patients
General conditions of the patients in the two groups.
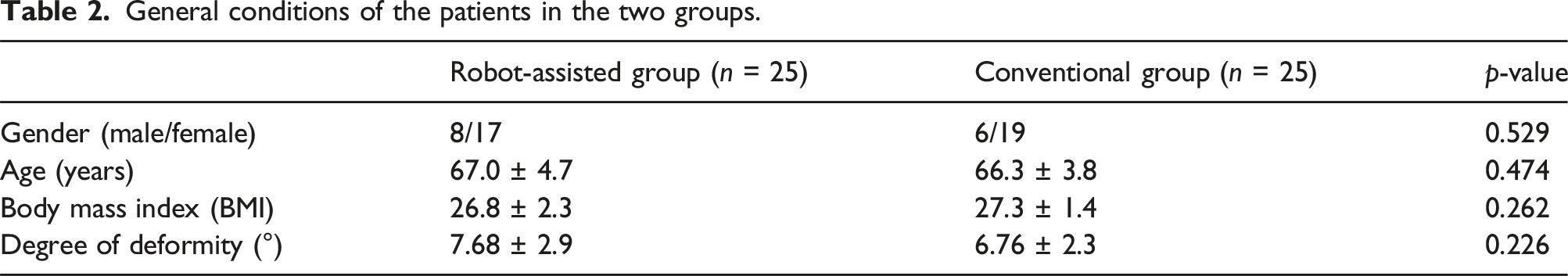
Methods
Preoperative planning
Individual preoperative CT scans of the lower limbs, including the hip, knee, and ankle joints, were performed to obtain DICOM format data for establishing three-dimensional bone models of the femur and tibia using robotic software. The surgeon conducted preoperative planning based on the three-dimensional model, taking into consideration optimal prosthesis coverage, minimal osteotomy , and achieving the best anatomical shape of the knee joint as reference standards for determining initial placement angle, position, and type of prosthesis (Figure 2(a)–(d)). Notes: (a): Preoperative planning for the tibial prosthesis; (b): Preoperative femoral prosthesis planning; (c, d), The position and size of the prosthesis were preliminarily determined; (e): Placement of tibial and femoral positioning tracers; (f-h): Completion of registration for hip rotation center, femoral condyle, medial and lateral malleolus; (i): Verification of the final surgical plan; (j-m): Robot-assisted osteotomy of the medial tibial plateau, posterior femoral condyle, and distal femur was performed.
Surgical methods
All surgeries were performed by a consistent surgical team using Zhengtian Company’s Unique UKA prosthesis. The robot-assisted group received subarachnoid block anesthesia combined with continuous epidural anesthesia while a pressure tourniquet was applied to the proximal thigh of the affected side at a pressure value of 50-55 kPa. Patients were positioned supine with a knee flexion and extension fixator installed below the affected limb. An approximately 8 cm long anteromedial incision was made along the medial edge of the patella to access the knee joint after confirming normal anterior cruciate ligament function and lateral condylar cartilage condition suitable for UKA. Metal detection needles were placed near both sides: one on the medial tibial plateau close to tuberosity and another on the medial edge of medial femoral condyle; two metal fixation needles were percutaneously fixed at four transverse fingers from each side: from medial tibia to its tuberosity and from medial femur to upper pole of patella in order to place positioning tracers (Figure 2(e)). Calibration was used to register landmarks such as hip rotation center, medial/lateral femoral condyles, and medial/lateral malleolus (Figure 1(f)–(h)). The osteophytes were excised, and the knee joint was subjected to appropriate valgus and varus stress. The robot system recorded the motion parameters of the knee joint at 30° intervals from 0° extension to obtain the initial flexion and extension gap of the knee. After adjusting the preoperative design of prosthesis placement and movement trajectory, the designed knee joint exhibited medial and lateral gaps in flexion and extension ranging between 1 and 2 mm. Following completion of intraoperative verification, the final surgical plan was determined (Figure 1(i)). The surgeon maneuvered the mechanical arm, employing a swinging saw to precisely incise the medial platform of the tibia and posterior condyle within the predetermined range. Subsequently, the anterior condyle cartilage of the femur was meticulously abraded using a high-speed drill (Figure 2(j)–(m)). Subsequently, thorough cleaning of bone cutting surfaces took place followed by installation testing of prostheses with subsequent clearance and pressure tests for knee flexion-extension within an ideal range. Once dried, Zhengtian Unique unicompartmental prosthesis (with a fixed-bearing polyethylene insert.) was implanted using bone cement. After hardening of bone cement, pulse gun rinsing was performed again on both joint cavity and prosthesis followed by injection of cocktail capsule for postoperative pain relief. Evaluation comparing knee joint space pressure and soft tissue balance with preoperative design was conducted once more before closing incisions layer by layer.
Conventional group: The anesthesia, incision selection, and surgical exposure were consistent with those of the robot-assisted group. In accordance with the UKA surgical procedure, a tibial osteotomy guide was positioned to perform the manual osteotomy, followed by measurement of the osteotomy surface size and selection of the tibial component. Subsequently, the intramedullary femoral osteotomy guide was utilized for the completion of both anterior and posterior femoral condyle osteotomies. The trial prosthesis were then installed followed by thorough clearance testing for flexion and extension movements. After achieving satisfactory balance, pulse washing gun was utilized to flush both articular cavity and bone cutting surface prior to drying of the latter. Finally, bone cement prosthesis installation was conducted following identical steps as those employed in the robot-assisted group.
All patients received standardized anticoagulant, anti-inflammatory, and analgesic therapy following surgery. Active and passive rehabilitation exercises were initiated 24-48 h post-surgery under the supervision of medical professionals.
Oservation indicators
The primary objective of this study was to evaluate the accuracy of medial UKA prosthesis positioning using full-length radiographs of the lower extremities with China-made robot-assisted. Full-length standing X-ray films were taken on day 5 after surgery in both groups to compare coronal deviation values for femoral component, coronal deviation values for tibial component, and knee joint line height change. The X-ray measurements were independently performed twice by two non-operative doctors using specialized software (Senyint PACS Workstation), with an average value used for analysis. The two doctors were not cognizant of the categorization.
The second objective aimed to compare the operation time, intraoperative blood loss, pain levels using VAS scores at 24 h, 72 h, and 3 months postoperatively, clinical outcomes at 3 months postoperatively through KSS clinical Score, KSS functional score, and knee range of motion measurements.
Statistical methods
The data were analyzed using SPSS 26.0 statistical software. Measurement data that followed a normal distribution were presented as mean ± standard deviation (
Outcomes
Radiological outcomes comparison between groups
Radiological outcomes.

Surgical outcomes and clinical outcomes comparison between groups
Surgical outcomes and Clinical outcomes.

Discussion
The most important finding of this study is that compared with Conventional medial UKA,China-made robot-assisted medial UKA can reduce the coronal deviation value of tibial, femur prostheses and postoperative joint line height change, that is, improve the accuracy of prosthesis placement. Since its inception in the 1960s, UKA has emerged as a pivotal knee preservation procedure.6,7 However, when compared to TKA, medial UKA has consistently grappled with the predicament of elevated revision rates.8,9 Factors contributing to UKA revision encompass aseptic loosening of the prosthesis, progression of contralateral compartment arthritis, unexplained pain occurrences, and infections; among these factors, aseptic loosening stands out as the primary cause. 10 Some scholars posit that prosthesis malalignment leading to abnormal changes in the internal stress of the knee joint responsible for aseptic loosening.4,11 Prosthesis malalignment can lead to increased load on articular surfaces, aseptic loosening of prosthesis, and accelerated wear of PE inserts. Particles generated from PE inserts wear can cause local osteolysis and further accelerate prosthesis loosening. 12 Ma and Kang et al.13,14 demonstrated that the positioning of the medial UKA femur prosthesis significantly influenced the stress on both the PE inserts and medial collateral ligament, with minimal stress observed in a neutral position, Stress on prostheses increased with valgus/varus positioning and positively correlated with angle increasing. Additionally, elevated stress on the medial collateral ligament is also a significant contributor to postoperative residual pain. The placement of the tibial prosthesis is equally critical as improper placement can lead to heightened stress within the lower and lateral intercompartment of the tibial prosthesis, increased tension on the medial collateral ligament, long-term stiffness, and pain in the medial knee joint; all factors that impact postoperative efficacy.15,16 The Navio and Mako Robot-assisted systems, manufactured in the United States, have demonstrated their ability to enhance the precision of prostheses.17,18 Similarly, this study reveals that China-made robot-assisted system has achieved comparable outcomes (Figure 3).
The alteration of joint line height following UKA also plays a crucial role in determining postoperative efficacy and prosthesis survival rate.
19
This study compared the changes in joint line height after surgery between the two groups and found that the robot-assisted group exhibited smaller changes than the conventional group, with statistically significant differences. Previous studies have indicated that excessive elevation or reduction of joint line height after UKA can lead to higher rates of surgical revision and anterior knee pain.
20
Kwon and Kang et al.21,22 discovered that compared to normal joint line height, post-UKA joint line height increased by 6 mm, resulting in a respective increase of 31.1% and 49.3% in contact stress on the upper surface of fixed-bearing and mobile-bearing prosthesis. Clinical studies have also confirmed that excessive elevation of the joint line, whether it involves fixed-bearing or mobile-bearing prosthesis, can result in limited postoperative knee joint movement and even flexion contracture deformity.23–25 The design concept UKA is to completely replace the cartilage surface with prostheses known as “prosthesis surfacing.” To achieve goals while minimizing prosthesis loosening risk, it is necessary to securely fix femoral prostheses onto solid subchondral bone. However, during actual procedures, complete removal of cartilage without involving real bone becomes challenging without osteotomy guides or robotic assistance, demanding surgeons with extensive experience.
26
Consequently, femoral osteotomy often tends to reduce osteotomy amounts which may cause joints to fall below this reference line; such positioning increases stress on both PE inserts and subtibial cancellous bone. Research conducted by Chatellard et al
27
has demonstrated that an absolute change value in joint line height <3 mm leads to significantly higher implant survival rates and postoperative knee scores compared to values ≥3 mm. In this study, robot-assisted medial UKA resulted in less reduction of joint line height than observed in the control group—another advantage offered by China-made robot-assisted system (Figure 4). The coronal deviation values of femoral and tibial prosthesis. knee joint line height. Notes: Joint line height was determined using Herry’s method [5].

The second interesting finding of this study was that the robot-assisted group exhibited lower postoperative pain scores compared to the conventional group, as indicated by 24-h VAS score and a VAS score of 72-h post-operation. This suggests that robot-assisted during surgery may result in milder postoperative pain. The reasons for this observation could be attributed to the following factors: ① The Robot-assisted group underwent less soft tissue release and osteotomy. Robot-assisted technology aims to achieve minimal osteotomy range and limited soft tissue release for optimal gap balance during preoperative planning. The robotic arm’s tactile, visual feedback enables precise definition of the osteotomy range, minimizing unnecessary bone resection.② Robot-assisted technology provides better protection for the soft tissues surrounding the knee joint. Studies by Hampp 28 and Kayani et al 29 have demonstrated that robot-assisted TKA leads to reduced iatrogenic soft tissue injury, which subsequently results in decreased inflammatory exudation and pain. The reduced postoperative pain observed in the robot-assisted group in this study may be attributed to the enhanced protection of the soft tissues surrounding the knee joint by the UKA robot.
In this study, the group undergoing robot-assisted UKA had a longer Operation time compared to the control group. The reason for this can be attributed to the need for precise localization of the robot in the medial tibia and femur, as well as the requirement to register the hip rotation center, internal and external femoral condyles, and external ankle by using tracers. At the same time, the operation time may be prolonged due to factors such as repeated disinfection affecting the accuracy of positioning devices like tracers, as well as mechanical arm failures. Peter Savov et al 30 also demonstrated that conventional UKA is on average 13 min shorter than robot-assisted UKA; however, this difference gradually diminishes with increasing surgical proficiency.
The study found that the learning curve of the Zhengtian UKA robot was comparatively shorter. Among the 25 cases analyzed in this study, the surgeon possessed experience with other types of TKA robots but had not previously operated UKA robot. We observed that there exists a learning curve for the Operation time of this robot-assisted system. Initially, the Operation time is significantly longer than that of conventional UKA; however, after conducting 10 cases, the operation time is considerably reduced, suggesting that 10 cases may represent an inflection point in terms of time efficiency. Nevertheless, no discernible learning curve was identified regarding implant placement accuracy and size selection. It is postulated that for surgeons with limited experience in UKA procedures, this UKA robot can be beneficial; nevertheless, certain considerations must be taken into account during actual operations: 1) Full consideration should be given to the impact of posterior condyle osteophytes on soft tissue balance. The robot-assisted system cannot quantify how posterior condyle osteophytes influence joint capsule and ligament tension during preoperative design; however, soft tissue balance will inevitably change to some extent following osteophyte removal which can affect prosthetic size preoperative design accuracy. 2) This UKA robot has the capability to evaluate knee joint soft tissue tension through virtual stress simulations enabling balanced internal and external stresses at various flexion and extension angles. However, when assessing knee joint flexion-extension gap and stress during surgery, it is crucial for surgeons to apply consistent external forces matching those designed by machine-generated virtual stress in order to obtain accurate results - necessitating both experience and tactile sensitivity.
The research has several limitations. Firstly, the short follow-up period in this study prevents a comparison of the long-term efficacy of surgery and the survival rate of prosthesis. Secondly, the limited number of records necessitates further investigation with larger sample sizes and longer-term follow-ups to verify the long-term efficacy of China-made robot-assisted systems. Third, this study only compared the coronal position of the prosthesis through the full-length X-ray of the lower limb, without involving the sagittal position and the rotation of the prosthesis.
Currently,a significant shift is occurring towards personalized or kinematic lines in knee arthroplasty alignment, rather than relying on traditional mechanical lines. 31 In this context,the Chinese-made Zhengtian UKA robot has demonstrated precision and personalization advantages, yielding favorable short-term outcomes. However, proficiency in operating this system necessitates a learning process and experience accumulation, while long-term efficacy still requires further observation.
Footnotes
Acknowledgments
We appreciate the technical support provided by Sixth Affiliated Hospital of Xinjiang Medical University.
Authors’ contributions
RS and KJ contributed to the conception of the study; WY,AA,GC and ZZ contributed signifcantly to literature search, data extraction, quality assessment, data analyzes and manuscript preparation; LZ and JG contributed improving the article for language and style and protocol preparation; GZ helped perform the analysis with constructive discussions; MM,YR and KJ revised the manuscript and approved the final version; All authors have read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
