Abstract
Background
Central lines are frequently used in the Neonatal Intensive Care Unit (NICU). Incorrectly positioned central lines are associated with increased complications. Central line malposition has been related to prematurity, catheter size, and small-for-gestation-age status. The impact of provider experience on proper central line positioning has not been established.
Methods
In this retrospective cohort study, neonates had central lines placed within the first 10 days of life. Central lines included umbilical artery catheters (UAC), umbilical vein catheters (UVC), and peripherally inserted central catheters (PICC). Central line malposition was confirmed with thoracoabdominal radiography. Different providers with various months/years of experience were coded. Logistic regression models were fit to adjust for potential confounders of the association of years of experience with line malposition.
Results
Between 2019 and 2021, 301 neonates had 616 central lines. 66% (405/616) of all central lines were malpositioned. The median years of providers’ experience who placed malpositioned and properly positioned lines were 1.93 (interquartile range [IQR]: 1.03–5.48) years and 2.17 (IQR: 1.38–4.85) years, respectively (P = .78). The distribution of malposition lines was UVC 49% (199/405), UAC 20.5% (83/405), and PICC 30.5% (123/405). Only UVC was significantly associated with malposition (P = .002).
Conclusions
Malposition of central lines frequently occurred in the NICU and was associated with UVC placement, irrespective of the provider’s experience who accessed it. Anatomical variations in neonates with different gestational ages and birth weights may mean that current methods to estimate insertion depth can be misleading. Future interventions should involve novel techniques of confirming real-time positioning during insertion rather than focusing on placement calculations.
Introduction and Background
Central lines are common in the Neonatal Intensive Care Unit (NICU); they are placed in as many as 22% of NICU admissions. 1 Central lines are used to administer medications, assess hemodynamic status, infuse fluids, and provide parenteral nutrition.1–3 Commonly used central lines in the NICU include umbilical artery catheters (UAC), umbilical vein catheters (UVC), and peripherally inserted central catheters (PICC). Central line complications such as perforation and hemorrhage, cardiac tamponade, and pseudoaneurysm, among others, are rare but may be life-threatening.1, 4, 5 Multiple UVC placement attempts may result in hepatic infarction, hematoma, or portal venous gas. 1 Complications are more common in malpositioned central lines, including non-centrally positioned PICC tips and those lines that migrate from their correct position.6–14
The depth of central line catheters is estimated with formulas using neonatal measurements. For example, UAC and UVC placement formulas are based on the patient’s length and weight.12, 15, 16 PICC insertion formula depends on external measurements or equations using body weight or length. 13 However, the accuracy of these methods is limited, particularly in premature, large for gestational age (LGA) and small for gestational age (SGA) neonates. 15 Routinely, central line position is confirmed with thoracoabdominal radiography after placement.
There are known clinical and demographic risk factors associated with malpositioned central lines. Prematurity and very low birth weight (VLBW) neonates are at increased risk of malpositioned UACs and UVCs.7, 9, 12 Specifically, extremely low birth weight (ELBW) neonates are likelier to have UVC positioned in the heart—right atrium, foramen ovale, and left atrium.11, 17 Larger catheters and escalation of respiratory support required by the neonate are also risk factors for malpositioning, 9 in contrast to sex and central line indication.3, 9
It is unclear how provider experience impacts central line malpositioning. In the adult literature, the complication rate for subclavian catheters ranges from increased to unchanged based on resident experience.18, 19 While experienced clinicians are assumed to be more likely to place catheters appropriately among neonates, 9 there is no evidence that more experienced neonatologists have lower malposition rates. 7 In our institution, NICU providers have variable expertise and include pediatric residents, Neonatal-Perinatal Medicine fellows, nurse practitioners (NPs), physician assistants (PAs), and neonatology attending physicians. We hypothesized that central line malposition would be lower among providers with more experience working in the NICU. This study aimed to find the association between malpositioned central lines and provider experience.
Materials and Methods
Design, Setting, and Timeframe
This retrospective analysis was conducted in an urban, academic, quaternary referral center level-IV NICU from February 2019 to January 2021. This hospital had an average of 3,400 deliveries per year in the above specified time period.
We included all neonates admitted to the NICU who required central line placement within the first 10 days of life. The study cohort consisted of infants who had central lines (UVC, UAC, and PICC) placed within the first postnatal days. Patients transferred from another facility with a central line already in place were excluded. A central line was defined as a UAC, a UVC, or a PICC. The data were curated from our electronic health records (EPIC) by one author (ML). Removal of all patient identifiers occurred before analysis. There was no direct patient or public involvement. The Institutional Review Board and the Ethics Committee approved the study design. Informed written parental consent was waived as this was a retrospective study.
Predictor/Outcome Variables
Patient variables included demographic data such as gestational age (GA), sex, birth weight (BW), length, and BW percentiles based on Fenton growth charts. 20 Neonates were considered SGA if their BW was less than the 10th percentile for GA and sex and LGA if their BW was greater than the 90th percentile for GA and sex. Other variables collected were postmenstrual age (PMA), postnatal age, length, and weight at the time of catheter insertion.
Catheter-related characteristics included the number of lumens and catheter size. We recorded provider type (NPs, PAs, Neonatal-Perinatal Medicine fellows, and Pediatrics residents) and years of experience in the NICU. Residents’ experience was coded using months spent in the NICU during their Neonatology rotations. For fellows in Neonatal-Perinatal Medicine, the experience was the difference between the procedure date and the fellowship program starting date, plus the three months they spent in the NICU during their pediatric residency. Among NPs and PAs, provider experience was quantified in years by subtracting the procedure and hire dates. If multiple providers were involved in central line placement, the provider with the lowest experience level was coded.
The insertion depth for all UAC and UVC insertions was calculated using Shukla and Ferrara’s method. 15 For most PICC insertion depth calculations, external measurements such as the distance from the insertion site to the expected correctly positioned catheter tip were used. 13 The central line tip location was confirmed by plain radiography. Correctly placed UACs terminated between T6 and T9 vertebral bodies. The optimal placement of a UVC ended at the IVC-RA junction, roughly at the diaphragm level. PICC was defined as central and correctly positioned if visualized on the superior vena cava, preferably on the (SVC)-RA junction when placed in the upper limbs or on the IVC length when placed in the lower limbs. Neonates with multiple central lines were evaluated for the initial positioning of each central line. The radiologist’s official report was considered the standard for correct position determination. Infant outcome, death or discharge from the NICU, was also coded.
Statistical Analysis
The initial expected sample size was 500 observations. Assuming 50% had central lines placed by experienced providers 21 and the malposition rate in this group around 10%, the study would have 80% power with a two-sided Type 1 error rate of 5% in a logistic regression analysis to detect an increase in the malposition rate to 20.2% when less experienced providers placed lines, with an odds ratio (OR) of 2.3. 9 T-tests or Wilcoxon rank sum tests were used to compare continuous variables between central line malposition/no malposition groups, and chi-square tests were used to compare categorical variables. Logistic regression models were fit to adjust for potential confounders associated with years of NICU experience and central line malposition. The data were coded and analyzed using the statistical analysis software SAS version 9.4. A two-sided P < .05 was considered statistically significant.
Results
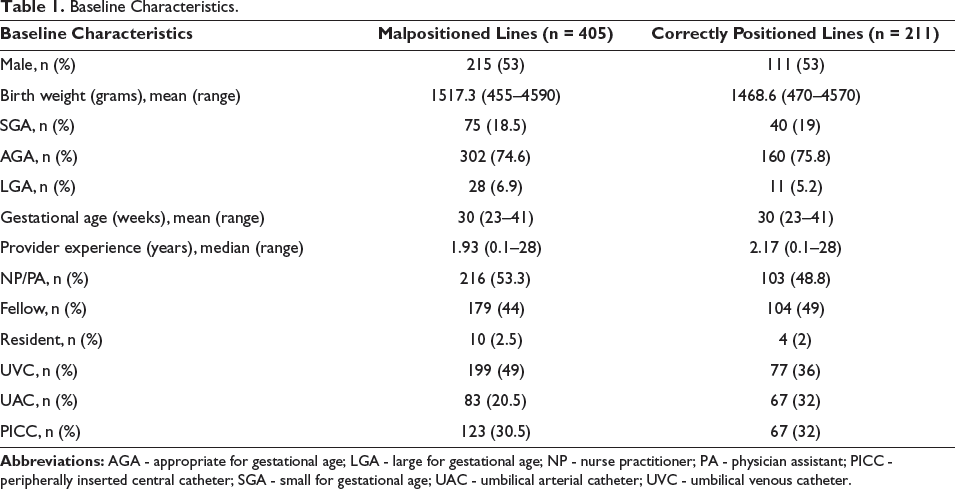
Between 2019 and 2021, 301 neonates had 616 central lines in the NICU. Most neonates were male, 53% (326/616), and the mean BW was 1504 gm. The GA ranged from 23 to 41 weeks, with a mean of 30 weeks. Provider experience was broad, with a median of two years, ranging from two months to 28 years. Baseline characteristics separated by position (malpositioned/correctly positioned) are shown in Table 1. Of all central lines, 66% (405/616) were malpositioned as per the first radiography. The median years of providers experience who placed malpositioned and properly positioned lines were 1.93 (interquartile range [IQR]: 1.03–5.48) years and 2.17 (IQR: 1.38–4.85) years, respectively (P = .78; Table 2).
Baseline Characteristics.
Bivariate Analysis of Central Line Malposition.
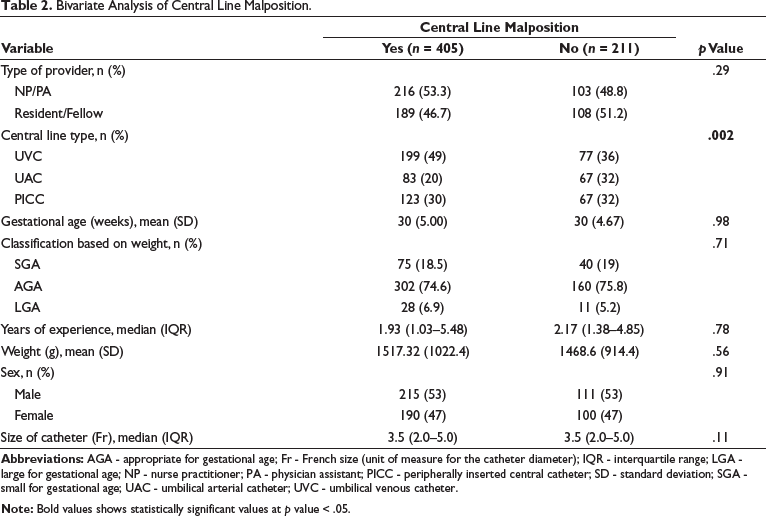
The distribution of malpositioned lines was UVC 49% (199/405), UAC 20.5% (83/405), and PICC 30.5% (123/405). Among the correctly positioned lines, UVC corresponded to 36% (77/211), followed by UAC 32% (67/211) and PICC 32% (67/211), with a total of 34% (211/616). When malpositioned were compared to correctly positioned central lines, only central line type was significantly associated with malposition (P = .002).
The initial position of the central line was adjusted to a correct position in 81% (327/405) of neonates, and the catheter was removed in 13% (52/405) of them. Some catheters were kept in the same position (6%–26/405), even if not centrally placed, due to the need for medications and fluids and no other intravenous access. On further analysis, evaluating lines by type, among all placed UVCs, 72% (199/276) were malpositioned on the first radiography, followed by PICCs with 65% (123/190) and UACs with 55% (83/150).
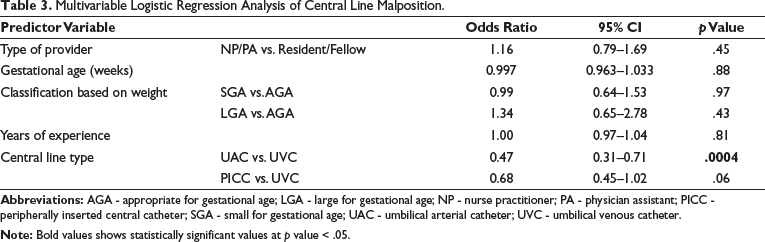
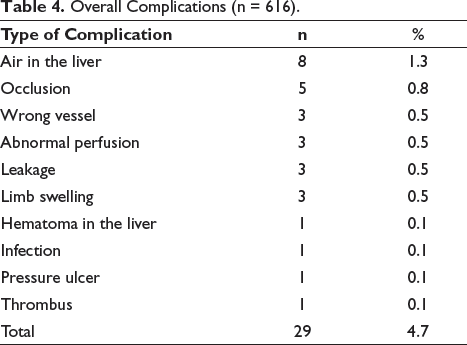
Sex, GA, catheter size, BW, length, provider type, and classification based on weight for GA (e.g., SGA, AGA, or LGA) were not associated with central line malposition. In addition, logistic regression analysis did not show an independent association of years of experience with central line malposition after adjustment for potential confounders (OR = 1.00; 95% CI: 0.97–1.04; P = .81; Table 3), whereas central line type remained a significant predictor of central line malposition (UAC vs. UVC: OR = 0.47; 95% CI: 0.31–0.71; P = .0004). Though severe central line complications were rare, complications were seen with 4.7% (29/616) of central lines (Table 4). Of the 301 neonates, 6% (19/301) died in the NICU. None of the deaths was related to catheter insertion or complications.
Multivariable Logistic Regression Analysis of Central Line Malposition.
Overall Complications (n = 616).
Discussion
In this study, 66% of central lines were malpositioned on the first radiograph. The most common malpositioned central line was the UVC, accounting for 49% of the malpositioned central lines. Among all factors analyzed, only central line type was related to malposition. Provider experience was not associated with central line malpositioning.
Providers with a broad range of experience and levels of training comprise the NICU team. 18 This diverse group was analyzed into two categories: type of provider and duration of experience as a NICU clinician. Despite including a range of providers with an experience span, neither provider type nor years spent in the NICU impacted the proper catheter position, similar to prior data about malpositioned UVCs.9, 21 UVC catheter was the only factor associated with incorrect catheter placement. In practice, inserting a UVC is a blind procedure where the catheter follows the pathway of least resistance and could enter a collateral route into the portal system, an intrahepatic branch of the portal vein, or a hepatic vein or if not sufficiently advanced, may terminate in the umbilical vein, umbilical recess, or ductus venosus.22, 23
As previously published, central line malposition is common among neonates admitted to the NICU. In previous reports, up to 70% of central lines were malpositioned, and UACs were malpositioned 50% of the time.16, 24, 25 Another study showed that in over one-third of the UVC cohort, the line was not centrally placed on the first attempt. 9 A recent publication using Shukla and Ferrara’s method in most insertions demonstrated better-positioned lines with a 71% successful rate. 21 Shukla and Ferrara’s formulas 15 are routinely used at our NICU for UVC and UAC placement. Still, recently revised weight-based formulas 26 are available based on the provider’s preference. Surface anatomy measurements are used for most PICC insertions. New evidence suggests that successful PICC placement using formulas based on the neonate’s weight and/or length may be more accurate for PICCs. 13
In our cohort, GA and SGA or LGA status were not associated with malposition of the catheters. Soonsawad et al. did not find a difference in malposition for the more premature neonates either. In a multicenter observational study, GA and BW did not affect the procedure’s success.9, 21 In previous research, SGA, LGA, premature, VLBW, and ELBW neonates had increased rates of malpositioned UACs and UVCs, as formulas do not accurately calculate insertion depth for these smaller neonates.7, 9, 11, 17
We acknowledge the weaknesses of this retrospective single-center study that relied on provider charting and radiographic images. Our limitations included incomplete electronic health records review (e.g., the provider not describing multiple attempts or adjustments made before the first radiography). We understand that using years of experience could fail to represent the exact number of procedures a specific provider performs while working in the NICU. However, it gives a reasonable estimate of familiarity with catheter insertion. The findings represent the academic setting where the research was performed and may not be generalizable to other institutions. Our strengths are related to the sample size with a diverse patient and provider population. We analyzed malpositioned lines using a broad range of provider types and experiences. Finally, the results address a common clinical question: reasons for malpositioned catheters in the NICU.
Conclusions
Central line malposition frequently occurred in the NICU and was most often associated with UVC placement, irrespective of the provider’s experience who accessed it. Anatomical variations in neonates with different GAs and BWs may mean that current methods to estimate insertion depth can be misleading. Future interventions should involve novel techniques of confirming real-time positioning during insertion, such as point-of-care ultrasound (POCUS), rather than focusing on placement calculations.
Footnotes
Abbreviations
BW: Birth weight
ELBW: Extremely low birth weight
Fr: French size (unit of measure for the catheter diameter)
GA: Gestational age
IQR: interquartile range
IVC: Inferior vena cava
LGA: Large for gestational age
NICU: Neonatal intensive care unit
NP: Nurse practitioner
OR: Odds ratio
PA: Physician Assistant
PGY: Postgraduate year
PICC: Peripherally inserted central catheter
PMA: Postmenstrual age
POCUS: Point-of-care ultrasound
RA: Right atrium
SGA: Small for gestational age
SVC: Superior vena cava
UAC: Umbilical artery catheter
UVC: Umbilical vein catheter
VLBW: Very low birth weight
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The Albert Einstein School of Medicine Institutional Review Board approved the study design.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Informed written parental consent was waived as this was a retrospective study.
