Abstract
Objective:
The aim of this study was to identify the factors associated with tic severity in Vietnamese children with Tourette syndrome (TS).
Methods:
A total of 77 children with TS who underwent outpatient care at the Psychiatric Clinic, Vietnam National Children’s Hospital, were enrolled in this study. The International Classification of Diseases, Tenth Revision (ICD-10) was employed to diagnose TS. The severity of tic symptoms was evaluated using the Yale Global Tic Severity Scale (YGTSS). The effect of associated factors on YGTSS was evaluated using generalized multiple linear regression.
Results:
In total, the motor tic score had a positive association with parents’ history of psychiatric disorders (
Conclusions:
This study suggested that a parent’s history of psychiatric disorders, maternal pregnancy complications, and maternal smoking during pregnancy were associated with increased scores in the severity of tic symptoms in TS patients in Vietnam.
Introduction
Gilles de la Tourette syndrome (TS) is an inherited neuropsychiatric disorder that typically manifests during childhood, characterized by a heterogeneous array of motor and vocal tics whose severity fluctuates over time. 1 The factors contributing to the risk of developing TS and other chronic tic (CT) disorders are not yet fully understood. Although susceptibility to both TS and CT is genetically mediated, heritability studies indicate that environmental factors may also contribute to an elevated risk for CT.2,3 However, it remains uncertain which non-genetic factors contribute to TS/CT and at what point during the life course these factors may influence risk. In recent years, epidemiologists focused on chronic diseases have increasingly embraced a life-course approach, 4 which offers a strong conceptual foundation for understanding how timing and environmental exposures affect disease risk.
Prior research has suggested a possible link between maternal psychological disorders during pregnancy and heightened risk of neurological and mental health issues in children. Specifically, findings from the Avon Longitudinal Study of Parents and Children (ALSPAC) indicated that prenatal maternal anxiety—but notably not prenatal depression—was significantly related to emotional and behavioral problems in children at age four. 5 Three studies examined the relationship between CT disorders and maternal psychological morbidity during pregnancy. A small-scale study found that the severity of tics in patients with TS was linked to the intensity of stressful life events experienced by their mothers during pregnancy. 6 Another study demonstrated a propensity toward an increase in severe maternal psychological stress throughout pregnancy in correlation with TS. 7 The third study showed that prenatal depression and chronic maternal anxiety were likely to be associated with a subsequent risk of CT and TS, with the latter perhaps associated with a history of depression during pregnancy. 8 However, a systematic review and qualitative analysis were conducted to comprehensively examine the association between pre- and perinatal factors and TS. The findings indicated that most parental demographic factors—including age, education, socioeconomic status, and marital status—were not significantly associated with TS onset or the presence of comorbidities. However, several factors were identified as significantly related to TS onset, comorbidity, and symptom severity, with maternal smoking and low birth weight emerging as the most consistently reported risk factors. Nonetheless, the methodological quality of the included studies was limited, as most samples were derived from specialty clinics, and exposures were predominantly assessed retrospectively. 9
In particular, understanding whether environmental factors influence the severity of tics might significantly improve therapeutic approaches for patients with TS. 10 To our knowledge, there is no study research examining the severity of tic symptoms in Vietnamese children with TS. This is the first research exploring the relationship between tic disorders and parental psychological morbidity in Vietnam. We hypothesized that parental psychological morbidity is a risk factor for TS/CT, with a stronger association observed for prenatal exposure compared to postnatal exposure, given the increased vulnerability of the fetal brain to adverse influences. Furthermore, we evaluated this association while adjusting for various perinatal confounders and sociodemographic factors.
Methods and Materials
Study Design and Participants
This cross-sectional study included 77 patients with TS, aged 3-14, who received outpatient treatment at the Psychiatric Clinic, National Children’s Hospital, Hanoi, Vietnam, between August 2020 and August 2021. Parents filled out self-administered questions regarding their own and their child’s growth, exposure to the environment, and health outcomes. The study was approved by the Institutional Review Board of National Children’s Hospital (approval number: 1661/BVNTW-VNCSKTE).
Tourette Syndrome Diagnosis
The International Classification of Diseases, Tenth Revision (ICD-10) Diagnostic Criteria for Tourette Syndrome (F95.2) was used to diagnose TS including (a) multiple motor tics and one verbal tic have been present at some point during the duration of the disorder, although they need not be present simultaneously; (b) the frequency of the tics must be multiple times a day, occurring nearly every day, for more than one year. During that year, no period of recovery has lasted more than 2 months; and (c) onset before the age of 18years. 11
We employed the most popular Yale Global Tic Severity Scale (YGTSS) to evaluate the severity of tic symptoms in the study participants. 12 There are two sections in this tool, including a semi-structured clinical interview and an impairment scale. A questionnaire that includes the five domains of number, frequency, intensity, complexity, and interference following the first section. There are six items in the response choices for both the motor and phonic domains, ranging from 0 to 5 points, respectively. Total Motor Tic Score, Total Phonic Score, and Total Tic Score (Motor + Phonic) are obtained by the semi-structured interview section. The second section of YGTSS consists of an impairment scale, which is documented from 0 to 50 points. This section describes how the tic condition affects a person’s physical health, social acceptance, family life, self-esteem, and ability to function in school. 13 The overall impairment score is calculated from the impairment scale. Finally, the global severity score is the sum of total motor, phonic, and impairment scores. The higher total score was related to the more severe the tic.
Potential Factor Assessment
At the time of enrollment, mothers completed self-administered questionnaires designed to comprehensively evaluate potential risk factors. These questionnaires collected demographic data, parental education level and occupational status, dietary habits, lifestyle exposures, as well as detailed family and medical histories. Potential risk factors were categorized into prenatal, perinatal, and postnatal variables. Prenatal factors included level (binary, under 12 years and over 12 years), history of psychological disorders (binary, yes and no), medical history (binary, yes and no), and smoking during pregnancy (binary, yes and no). Perinatal factors encompassed birth trauma during labor (binary, yes and no), maternal pregnancy complications (binary, yes and no), gestational age (continuous, weeks), and birth weight (continuous, grams). Postnatal variables included patient age (continuous, years), age at tic onset (continuous, years), psychosocial stress exposure (binary, yes and no), presence of comorbid conditions such as attention-deficit hyperactivity disorder (ADHD), obsessive-compulsive disorder (OCD), and premonitory urges associated with tic symptoms.
Statistical Analyses
We examined basic descriptive statistics for age groups (under 10 vs. above 10 years old) and total cases. Student’s
The YGTSS mean values and 95% confidence intervals (95% CIs) were calculated using a general linear model analysis that controlled for the following variables: Model 1: adjusted for gender and age; Model 2: adjusted for Model 1 and gestational age (year, continuous); birth weight (gram, continuous); birth trauma during labor (binary, yes vs. no); comorbid psychological disorders (continuous, number of comorbidities); Model 3: adjusted for Model 2 and maternal age (year, continuous); parental history of psychiatric disorders (binary, yes vs. no); maternal pregnancy complications (binary, yes vs. no); and maternal stimulants during pregnancy (binary, yes vs. no).
The relationship between the variables is illustrated by the general linear model, which also enables us to forecast the value of the dependent variable given one or more new values of the independent variables. Population-based studies indicated that up to 80% of persons who have presented with a tic disorder before 10 years old and a significant decrease during adolescence
14
; therefore, in this study, subgroup stratification analysis by age ≤ 10 years and >10 years was performed. The impact of associated factors on YGTSS was evaluated using generalized multiple linear regression. Version 29.0.2 of SPSS (IBM Corporation, USA) for Mac was used for all statistical analyses. A
Results
Characteristics of Participants
Table 1 presents the descriptive statistics of unadjusted exposure and confounder variables in TS/CT patients. The results indicate that the prevalence of TS/CT was higher in boys than in girls and more common in urban areas compared to rural areas. The prevalence of comorbid psychological disorders included AHDH (24.7%) and OCD (5.2%). The average age of TS/ CT was 9.2 years old, while the age at tic onset was 6.9 years. The mean number of motor tics was 2.9 and 1.4, respectively. The corresponding YGTSS scores for motor tics, phonic tics, overall impairment, and global severity were 18.0, 15.7, 16.2, and 49.9, respectively. There were no differences in exposure and confounding variables of TS/CT between age groups except for the number of motor tics. Patients older than 10 years exhibited a higher number of motor tics than those aged ≤10 years.
Characteristic of Participants.
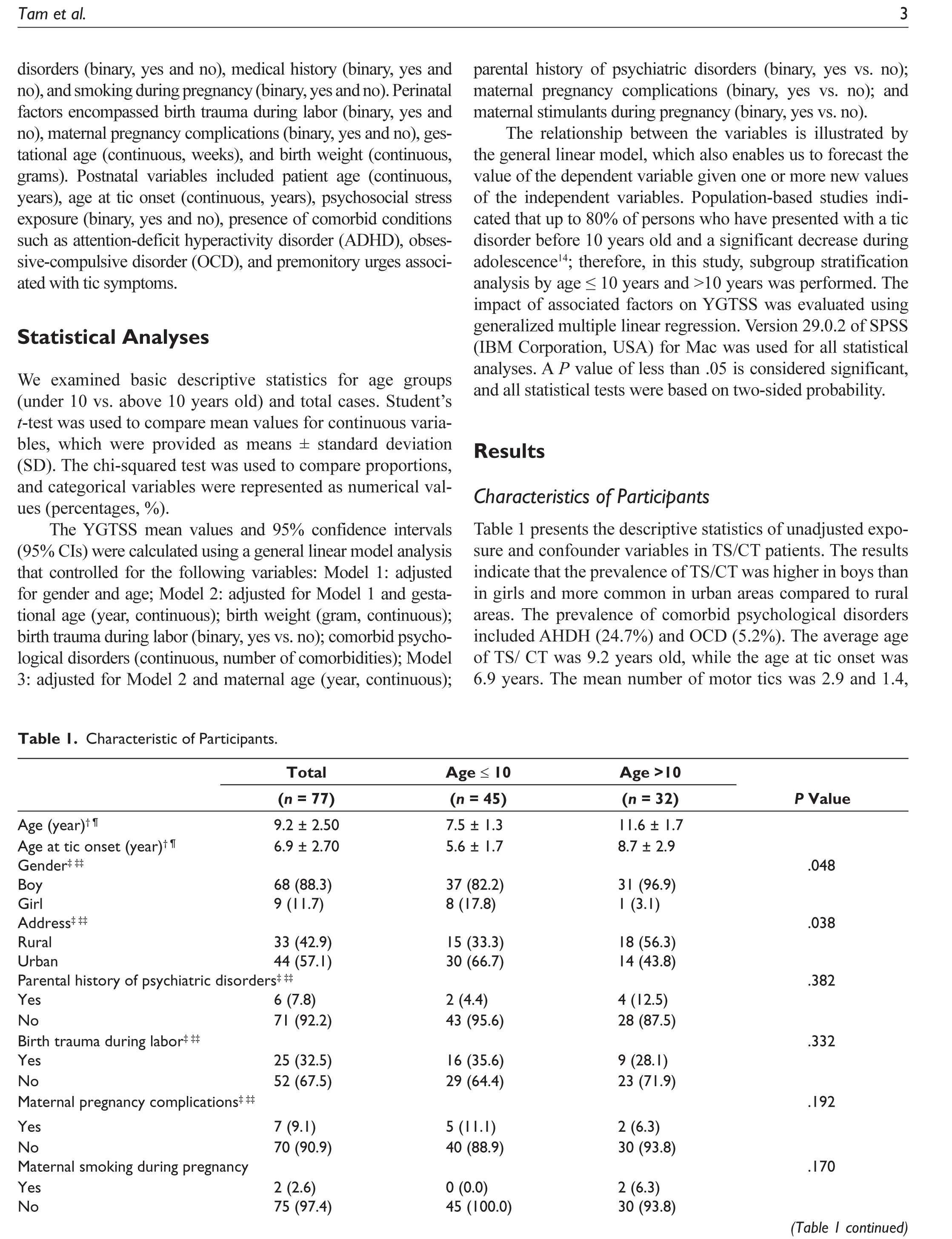
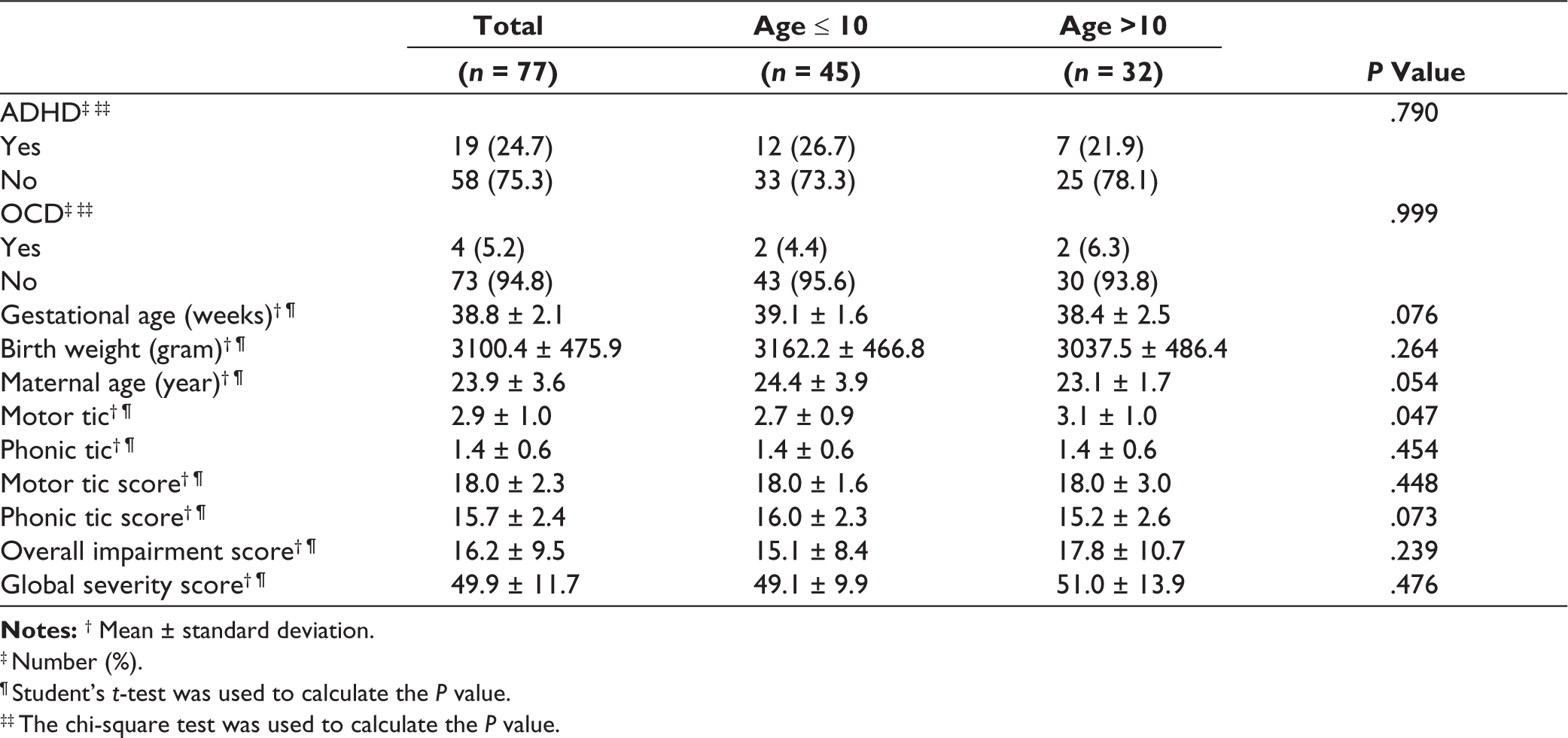
‡ Number (%).
¶ Student’s
‡‡ The chi-square test was used to calculate the
Association Between Factors and YGTSS in TS Patients
Table 2 performed the adjusted mean of YGTSS components (95% CI) by total participants and in stratified analysis by age group. There was no significant difference in YGTSS and components between age groups except for the phonics score, whereas age >10 years tended to be lower than age ≤10 years. The similar results showed no significant difference between the two age groups after controlling for confounding factors.
The YGTSS Adjusted Mean Value.†, ‡
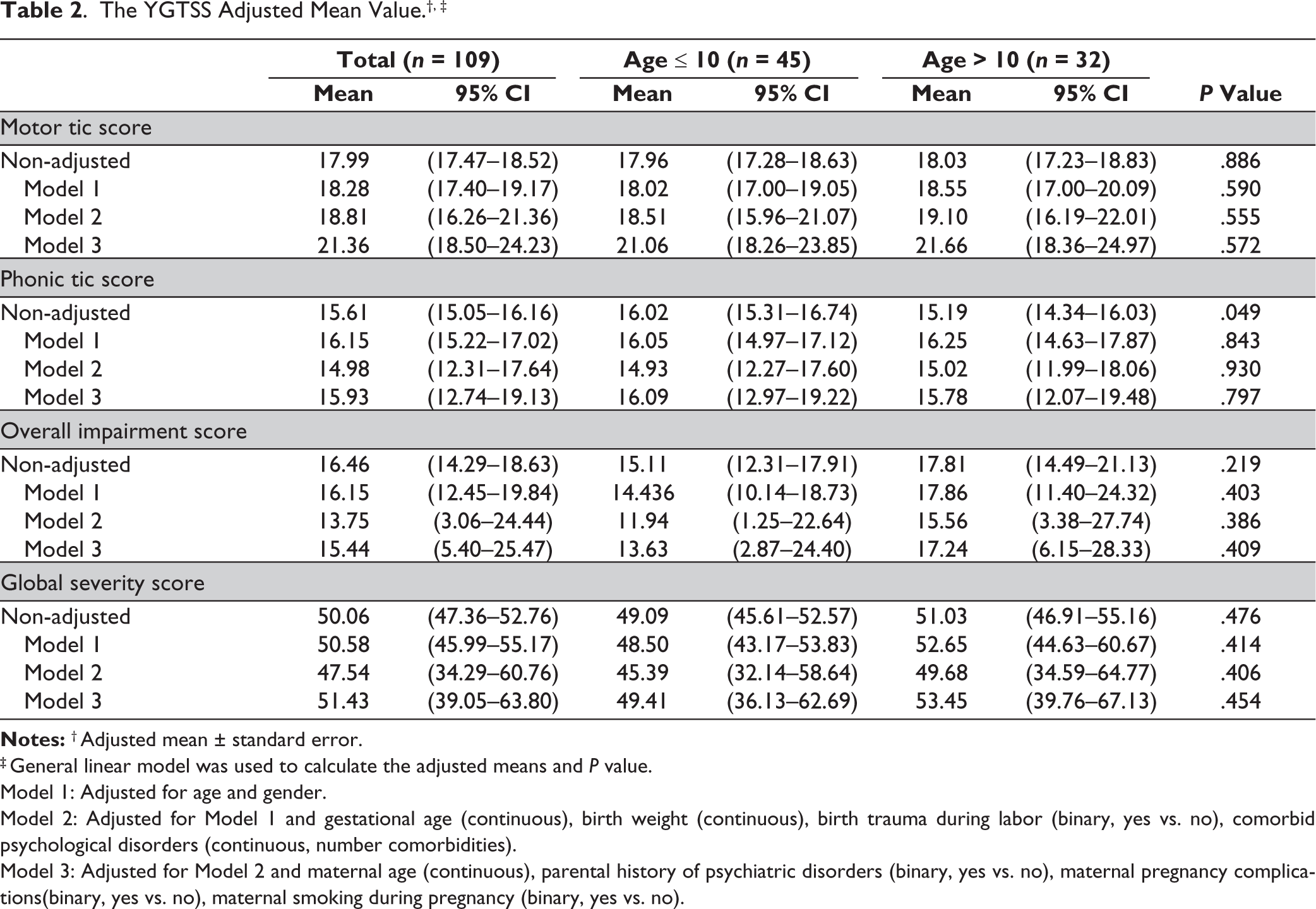
‡ General linear model was used to calculate the adjusted means and
Model 1: Adjusted for age and gender.
Model 2: Adjusted for Model 1 and gestational age (continuous), birth weight (continuous), birth trauma during labor (binary, yes vs. no), comorbid psychological disorders (continuous, number comorbidities).
Model 3: Adjusted for Model 2 and maternal age (continuous), parental history of psychiatric disorders (binary, yes vs. no), maternal pregnancy complications(binary, yes vs. no), maternal smoking during pregnancy (binary, yes vs. no).
Table 3 presents the correlations between various factors and the components of the Yale Global Tic Severity Scale (YGTSS). In the total groups, the motor tic score had a positive correlation with the parent’s history of psychiatric disorders (
Discussion
This is the first study in Vietnam that examines TS/CT patients and the relationship between YGTSS and TS/CT factors. We observed that higher scores of YGTSS and its components were correlated with the more severe tic in TS patients. These factors included the parent’s history of psychiatric disorders, maternal pregnancy complications, and maternal smoking during pregnancy. The maternal age had negative associations with scores of YGTSS in the age group over 10 years.
The Association Between Related Factors and YGTSS.‡
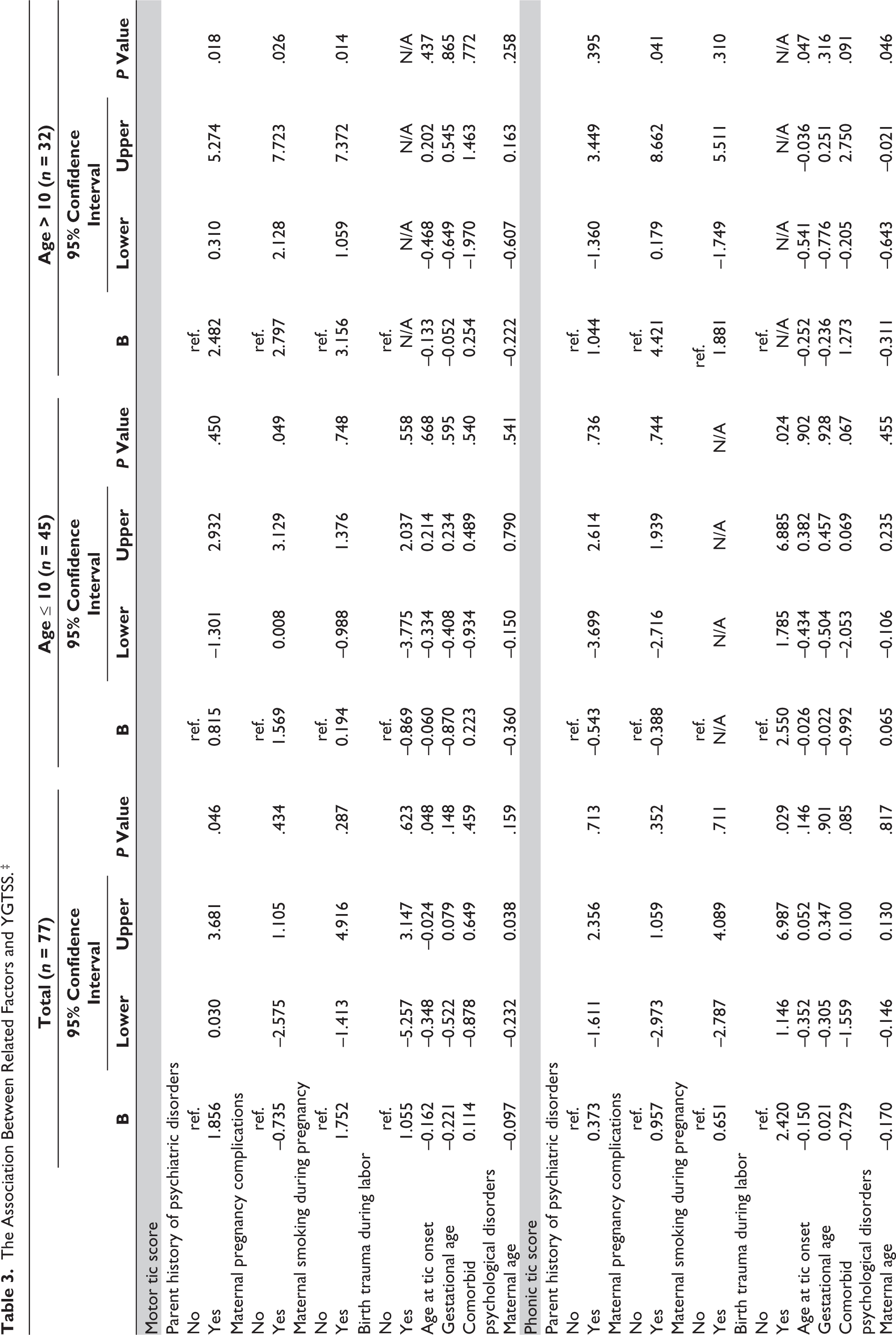
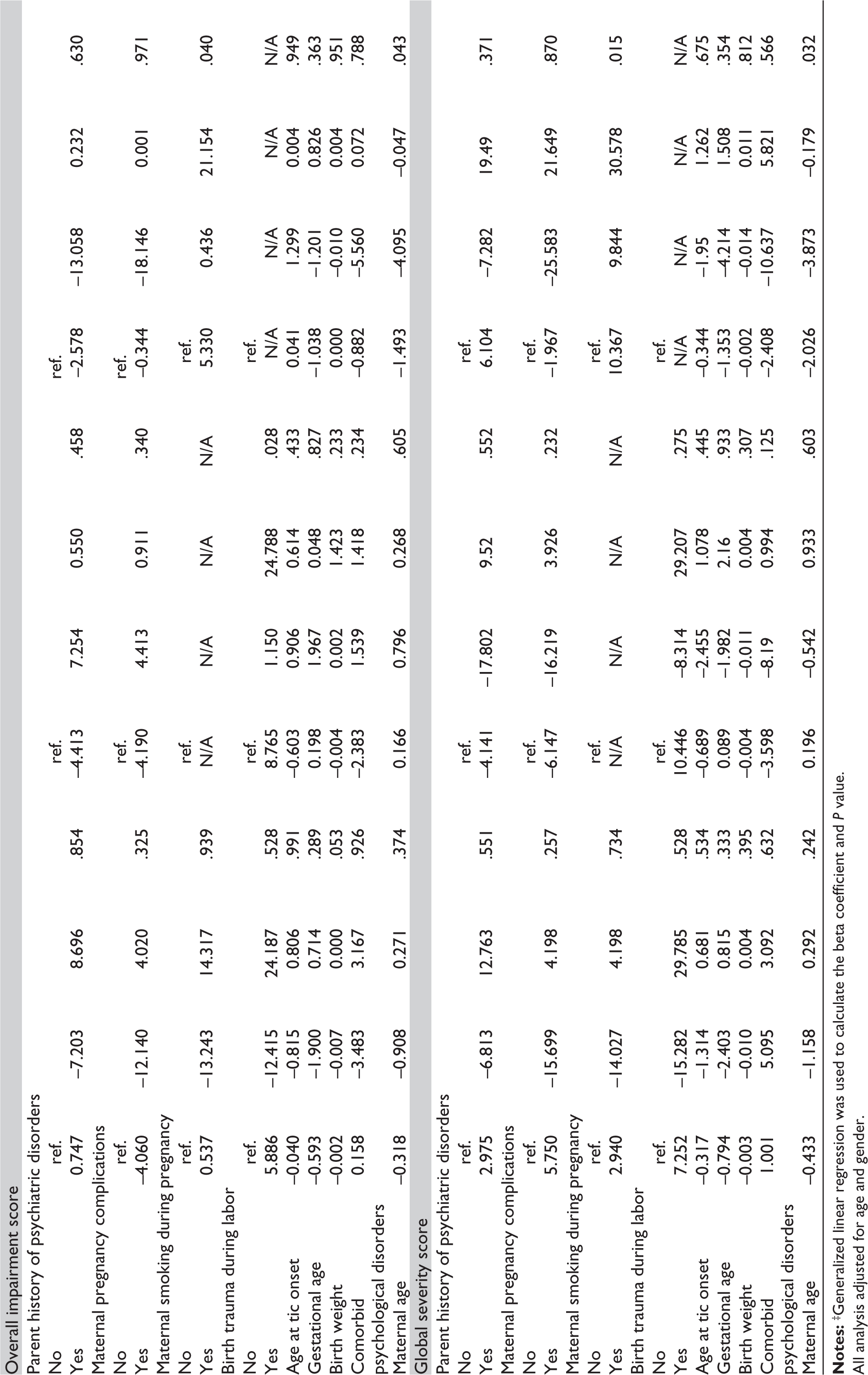
All analysis adjusted for age and gender.
These findings are in line with previous studies that evaluated the association between psychological disorders in children and parental psychiatric diseases.8,10,15 A UK-based longitudinal study investigating the relationship between parental anxiety and depression during the prenatal and postnatal periods and the risk of TS/CT followed 7152 children over 13 years. The results suggested that prenatal depression and chronic maternal anxiety were associated with an increased risk of CT and TS, though the association with TS may be influenced by a maternal history of psychiatric conditions. 8 Similarly, a study conducted in the Netherlands, involving two cohorts totaling 5722 children, suggested that residual confounding may contribute to the observed intrauterine effects of maternal anxiety and depression on behavioral disorders in offspring. This highlights the complexity of distinguishing direct biological effects from shared genetic and environmental influences. 16 Further supporting the role of environmental factors in tic disorders, increasing YGTSS global severity, total tic scores, and impairment ratings were found to be independently associated with stressors related to family, relationships, and education. Previous research has demonstrated that tic severity tends to escalate in response to increased exposure to stressful life events. 15 Several mechanisms might explain these associations. First, depressive symptoms during pregnancy may reflect a long-standing psychiatric disorder, suggesting an underlying genetic susceptibility that is exacerbated during pregnancy.8,17 Second, the association between maternal mood and anxiety disorders and tic disorders in offspring may be explained by confounding factors that contribute to increased psychosocial stress during pregnancy. 18 Notably, associations between parental psychiatric symptoms and tic disorders tend to weaken when socioeconomic factors are taken into account. 19 Lastly, maternal mood and anxiety symptoms could have a direct impact on fetal brain development, reinforcing the importance of investigating prenatal environmental influences on TS/CT risk and severity. 20
According to our research, maternal smoking during pregnancy and maternal age have been associated with higher YGTSS and its component scores, particularly in children older than ten (Table 3). These findings align with previous studies evaluating associations between severe psychosocial stress, maternal smoking during pregnancy, and the risk of TS and related disorders. The results showed that maternal smoking during pregnancy was statistically significant for the group of offspring with a TS diagnosis and independently associated with an ADHD diagnosis alone. 7 Moreover, a population-based cohort study reported a dose-response association between maternal smoking during pregnancy and the risk of tic disorders (TD/CTD) in offspring, indicating that higher cigarette consumption corresponds to increased risk. 21 In high-risk groups, efforts are needed to reduce the prevalence of these risk factors. Further research is needed to identify the causative pathways utilizing genetically sensitive designs. Global severity, overall impairment, and phonics scores were all negatively correlated with maternal age (Table 3). These findings are consistent with a Dutch study indicating a negative linear relationship between maternal age and externalizing behavioral difficulties in children aged 10-12. 22 Another review suggested older maternal age might confer protective effects on children’s behavioral, emotional, and social functioning, potentially due to increased maternal emotional maturity and preparedness. These protective factors associated with older motherhood could potentially mitigate or offset some of the biological risks linked to advanced maternal age. 23 Notwithstanding, a previous UK-based study using data from the Biobank indicated that women who give birth at an earlier and possibly later age may carry an elevated genetic risk for developing schizophrenia. 24 Another study reported a U-shaped association between parental age and offspring psychiatric risk, indicating that maternal age below 20 years (aOR: 1.44, 95% CI: 1.29-1.60) and paternal age above 50 years (adjusted odds ratio (aOR) 1.51, 95% CI: 1.23-1.86) were associated with the highest risk of psychiatric disorders in children, compared to parents aged 25-29 years. 25 Therefore, the age of the parents should be taken into consideration when assessing the risk of mental disorders in children. Although our primary hypothesis centered on prenatal parental psychological morbidity as a risk factor for increased tic severity in children with TS/CT, we also explored the influence of additional perinatal factors. Interestingly, maternal age showed a negative association with tic severity scores in older children. However, as age-related findings were exploratory and not part of our initial hypothesis, further studies are required to validate these results.
This study identified key factors associated with tic severity in TS/CT patients in Vietnam. Higher YGTSS scores were linked to greater tic severity, with significant contributing factors including parental psychiatric history, maternal pregnancy complications, and maternal smoking during pregnancy. A parental history of psychiatric disorders was associated with increased tic severity, suggesting both genetic and environmental influences. Maternal pregnancy complications and stimulant use, such as nicotine and caffeine, may contribute to neurodevelopmental disruptions affecting tic severity. Additionally, younger maternal age was negatively associated with tic severity in children over 10 years old, indicating that older maternal age may have a protective effect. These findings provide important insights into the potential risk factors influencing tic severity in TS/CT patients. Future research should prioritize longitudinal designs, genetic analysis, and objective parental health assessments while recruiting larger participants and more diverse populations. Employing robust methods to control for confounding will enhance the validity of findings and allow for a more comprehensive understanding of the factors influencing tic severity in TS/CT patients.
This study had several limitations. First, as the study is cross-sectional, the factors cannot be considered causally responsible. Second, this study did not adjust for socioeconomic status. According to previous studies, a less wealthy socioeconomic level is also associated with a higher risk of TS and CT. 19 Third, a small sample size consequently limits the association assessment. The patient was conducted only in National Children’s Hospital; therefore, findings in our study might not be generalizable to other populations. Fourth, the study did not collect information on the use of medications other than stimulants, particularly a more detailed description of the stimulants in maternal, therefore limited in describing their association between tic disorders and medication use in treatment psychology disorders. Finally, because our data are observational, we have made an effort to account for confounding, but we acknowledge that insufficient adjustment may still result in residual confounding. Despite these drawbacks, the findings of the study were useful because it was the first to evaluate the severity of tic symptoms with TS in Vietnam. Future studies should employ longitudinal designs with larger, representative samples and comprehensive data collection to better assess these associations.
Conclusion
This study suggested that the parent’s history of psychiatric disorders, maternal pregnancy complications, and maternal smoking during pregnancy were associated with higher scores in the severity of TS/ CT. It is necessary to focus on counseling, education, and guidance for both fathers and mothers during the prenatal, perinatal, and postpartum periods to reduce the severity of tic as well as have strategies to treat tic disorders in the early stages.
Footnotes
Acknowledgements
We are sincerely grateful to all the families who agreed to participate in this study and the whole team for their support in completing the study.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval and Informed Consent
The study was approved by the Institutional Review Board of Vietnam National Children’s Hospital (approval number: 1661/BVNTW-VNCSKTE dated 29 October 2020) and conducted according to the ethical standards of the Declaration of Helsinki. The consent form was written by parents. The participants could withdraw from the interview at any time, and this did not affect their continuation of healthcare services.
