Abstract
Severe depression is the most common mental disorder, with a heavy economic burden and limited treatment. The lifetime prevalence of depression among adults in China is 6.8%, with depression accounting for 3.4%. Currently, there are 95 million people suffering from depression in China, with approximately 280,000 people committing suicide each year, of whom 40% suffer from depression. Oral antidepressants are commonly used treatment methods in modern medicine, but they have significant drawbacks. Acupuncture therapy has shown promising physiological and pharmacological research evidence and good clinical efficacy, with small side effects, lasting efficacy, and low cost in depression. Depression is classified as a “depression syndrome” in Traditional Chinese Medicine, and its disease progress is closely related to the damage of the five zang organs: heart, liver, spleen, lung, and kidney. Acupuncture and moxibustion have been proven to be effective in treating depression by intervening in the points related to the five viscera. This article summarizes the research progress of acupuncture and moxibustion treatment of depression from the perspective of the five viscera.
Introduction
In recent years, the incidence rate of depression has continued to rise, affecting an average of three out of every 100 people. It is predicted that by 2030, depression will become the leading disease burden worldwide (Martinotti et al., 2022). Currently, there are over 350 million depression patients worldwide, with China accounting for 95 million, or approximately 30% of the total. The risk of suicide for patients with depression is 30 times higher than that of normal individuals, with approximately 1 million people worldwide committing suicide each year due to depression (Yang et al., 2022). Effective treatment of this disease has become a pressing concern in various sectors of society.
Oral antidepressants are commonly used treatment methods in modern medicine, but the clinical effective rate of antidepressants is less than 50%, and the recurrence rate within 6 months exceeds 50%. The recurrence rate within 10 years is as high as 85%, and even 30% to 60% of patients are ineffective in drug treatment (Xie et al., 2022). In contrast, acupuncture therapy, a traditional Chinese medicine (TCM) treatment, has shown promising physiological and pharmacological research evidence and good clinical efficacy (Li et al., 2023). Acupuncture refers to the practice of inserting needles (usually filiform needles) into a patient’s body at a certain angle under the guidance of TCM theory, using techniques such as twisting and lifting to stimulate specific parts of the body and achieve the goal of treating diseases (Kapadia, 2020). Clinical evidence suggests that they have a positive effect on improving patients’ depression, with small side effects, lasting efficacy, and low cost (Yang et al., 2022). Acupuncture and moxibustion therapy aims to prevent diseases by clearing the meridians, regulating the organs, and balancing yin and yang (Liu, 2015). There are various methods of acupuncture and moxibustion used in the treatment of depression, including body acupuncture, electroacupuncture, acupoint injection, auricular acupuncture, scalp acupuncture, catgut embedding, iontophoresis, and moxibustion (Yang et al., 2022). Depression is mainly treated from the perspective of the five internal organs (liver, heart, spleen, lung, and kidney) (Chen et al., 2021). This article summarizes the research progress of acupuncture and moxibustion treatment of depression from the perspective of the five internal organs (Figure 1).
Summary of Acupuncture and Moxibustion Treating Depression Through Five Zang Organs Theory. The Progress of Depression is Closely Related to the Heart, Lung, Kidney, Liver, and Spleen, While Acupuncture and Moxibustion can Effectively Treat Depression through Different Acupoints and the Theory of the Five Zang Organs.
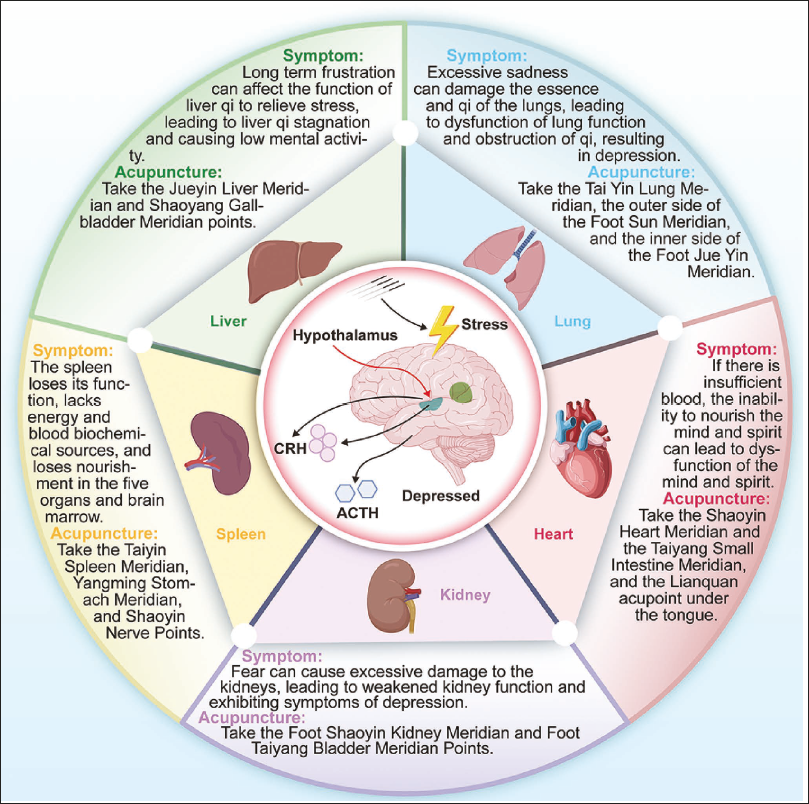
Depression from a Traditional Chinese Medicinal Point of View
TCM believes that the human body is a unified whole, centered around the five viscera (Zhang & Fang, 2023). In TCM, the clinical symptoms of depression are usually divided into different syndromes, such as “depression,” “lily disease,” and “visceral restlessness.” Depression syndrome refers to a type of disease characterized by qi stagnation, organ dysfunction, and symptoms such as emotional disorders and rib pain caused by emotional distress. Wang Chong’s “Lun Heng” states: “The Qi of heaven and earth are in harmony, and all things arise naturally.” Zhang Zai’s “Zhengmeng Taihe Chapter” states: “Taixu cannot be without Qi, Qi cannot gather and become all things, and all things cannot remain dispersed and become Taixu.” Qi is the functional vitality of all tissues and organs, such as the Qi of organs and meridians. In terms of pathogenesis, Qi hyperactivity refers to the syndrome of excessive heat and excessive function; Qi deficiency refers to the syndrome of functional decline and diffuse yin and cold. The obstruction of Qi is characterized by Qi stagnation, Qi reversal, or transformation into Qi stagnation and stasis (Zhang & Fang, 2023). The concept of “Yu Zheng” (depression syndrome) can be traced back to the earliest records in the “Neijing.” In the “Suwen Liu Yuan Zheng Ji Da Lun,” it was proposed that “Yu Ji should occur and be treated according to the times.” The Suwen Ling Lan Mi Dian Lun further classified emotional activities into wood depression, fire depression, soil depression, gold depression, and water depression. Xu Chunfu proposed six types of visceral depression based on the Comprehensive Collection of Ancient and Modern Medical Sciences, including heart depression, liver depression, spleen depression, lung depression, kidney depression, and gallbladder depression. Professor Jia Hongxiao believes that liver qi stagnation, spleen deficiency, and insufficient kidney yang are the core pathogenesis of depression syndrome. Liu et al. (2021) suggest a strong correlation between the smooth flow of lung qi and the onset of depression syndrome. Depression (Yu syndrome) is characterized by symptoms such as low mood and delayed thinking (Xie et al., 2022). Its main pathogenesis is related to emotional internal injury and poor circulation of qi, blood, and body fluids, involving the function of the five viscera.
Acupuncture and Moxibustion Treat Depression in Five Internal Organs
Acupuncture and Moxibustion Treatment Based on Liver
The liver is responsible for storing blood, and when the blood is affected, it can lead to emotional disturbances. If depression and anger damage the liver, it disrupts the regulation of liver qi and the nourishment of blood, resulting in emotional symptoms such as melancholy, sadness, and a tendency to cry. These emotional imbalances can also lead to physical symptoms such as fatigue and disturbed sleep. According to “Yi Bian,” liver and wood diseases are often associated with feelings of discomfort and depression (Park et al., 2016). Excessive anger can cause the liver qi to rise excessively, leading to disruptions in qi and blood circulation and increased mental activity. This can manifest as symptoms such as insomnia, headaches, red face and eyes, belching, nausea, vomiting, and acid reflux (Lam Ching et al., 2023). Long-term frustration can also affect the liver’s ability to relieve stress, resulting in liver qi stagnation and low mental activity (Xiong et al., 2020). This can lead to symptoms such as joy, sadness, crying, depression, chest and rib pain, breast pain, and a generally low mood. Treating depression from the perspective of the liver is a common approach, focusing on soothing the liver, regulating qi circulation, and nourishing the blood (Chen & Jia, 2018).
According to the theory of Jueyin and Shaoyang, the regulation of qi should be focused on the liver and gallbladder. Acupuncture and moxibustion commonly use acupoints such as Ganshu, Qimen, Taichong, Sanyinjiao, Dadun, Danshu, Fengchi, and Benshen for the treatment of depression. These acupoints on the liver and gallbladder meridians are frequently used, accounting for 20.21% of all acupoints used in the treatment of depression (Nating et al., 2021). Sanyinjiao is said to represent the heat under the feet, and when the heart is sad, the qi goes against the stomach. These statements guide the use of acupuncture and moxibustion in the treatment of depression. Additionally, there is a saying in the Classics of Acupuncture and Moxibustion and Moxibustion Questioning that “all diseases caused by wood stagnation can be treated by puncturing the acupoints at the gate of the stage, as the liver dominates these diseases.”
Huang et al. conducted a study using acupuncture and moxibustion treatment on acupoints related to the liver, such as Siguan, Ganshu, and Qimen. The results showed a significant reduction in depressive symptoms in patients (Huang et al., 2022). Yuhao et al. (2019) treated 21 patients with depression accompanied by suicidal ideation using liver-soothing and qi-regulating acupuncture, with a total effective rate of 90.48%. Wang et al. (2015) conducted a randomized study of 60 patients with depression, dividing them into a treatment group and a control group. The treatment group received moxibustion on acupoints Ganshu, Xinshu, and Tanzhong, while the control group received Milnacipran tablets. The treatment group showed significant improvement in Hamilton Depression Rating Scale (HAMD) scores, comparable to the control group, with no side effects (Wang et al., 2015). In the depression non-acupoint group, acupuncture led to decreased fALFF values in bilateral inferior parietal lobules and the left occipital lobe (Yi et al., 2012). Qiao et al. found that acupuncture at points such as Taichong, Ganshu, Yanglingquan, and Sanyinjiao can calm the heart and mind, regulate qi and blood, and promote meridians and collaterals. This can lead to a beneficial adjustment of the hypothalamic–pituitary–adrenal (HPA) axis function and a gradual normalization of physiological status (Qiao & Zhang, 2017). Animal experiments have also shown that acupuncture at acupoints such as Taichong and Sanyinjiao in rats with chronic restraint stress depression can increase pleasure and autonomous activity, as evidenced by increased consumption of glucose and water, as well as increased horizontal and vertical movements. The underlying mechanism may be related to changes in glial fibrillary acidic protein (GFAP) content in the hippocampus and prefrontal cortex, as well as serum interleukin-10 (IL-10) content (Dong et al., 2018). It shows that acupuncture and moxibustion treatment from liver-related Ganshu, Qimen, Taichong, and Sanyinjiao can effectively improve the depressive symptoms of mice and clinical patients, and its possible mechanism is to reduce the content of patients’ fibrillary acidic protein (GFAP) and the level of serum inflammatory factors.
Acupuncture and Moxibustion Treatment Based on Spleen
The spleen is responsible for movement and transformation, and its essence and qi are the material basis of the spleen consciousness. The spleen ensures that the organs are filled with qi, blood, and body fluids. Improper diet can lead to a loss of control of the spleen’s movement and transformation, resulting in a lack of energy and blood, and a loss of nourishment in the organs and brain marrow. This can lead to symptoms such as decreased appetite and excessive thinking. The Book of Classics, Volume 15, states that the spleen is responsible for central qi, and its suppression can hinder business expansion, resulting in depression and worry. Suwen Ju Tong states that thinking can lead to the retention of the heart, the return of the spirit, and the retention of positive qi, resulting in the stagnation of qi. This reflects the relationship between the spleen and the conscious thinking activities of the human spirit, and changes in the function of the spleen can affect the mental and volitional state of the human body. A survey has shown that patients with gastrointestinal disorders are more likely to have psychological problems such as depression, anxiety, and emotional instability (Li, 2015). Patients with depression often exhibit spleen and stomach disorders, which can exacerbate their depressive state (Liu et al., 2020). Therefore, treating depression from the perspective of the spleen is also a common approach.
The commonly used acupoints for acupuncture and moxibustion in the treatment of depression include Spleen Shu, Weishu, Sanyinjiao, Taibai, Dadu, Zusanli, Fenglong, and others. These acupoints on the spleen and stomach meridians are frequently used, accounting for 17.42% of all acupoints used in the treatment of depression (Yang et al., 2021). Acupuncture and moxibustion Dacheng records that acupuncture and moxibustion on the Stomach Meridian of Foot Yangming and the Spleen Meridian of Foot Taiyin can treat sadness and unhappiness, with specific acupoints such as Jiexi, Shangqiu, Liugu, Daheng, and Gongsun. The Compilation of Points along the Meridians states that “Zhongwan, Qimen, Shanglian” are effective for wheezing, and that “all diseases of the spleen and stomach can be treated everywhere.” This highlights the importance of regulating the spleen and stomach, resolving stagnation, and dispersing depression. The Four Sages Heart Source mentions that the source of harmonizing the five internal organs lies in the central palace. The physiological activities of qi, blood, yin, yang, and the viscera rely on the harmonization of the qi mechanism of the central energizer. When treating diseases, it is important to focus on the spleen and stomach, using acupuncture and moxibustion on relevant acupoints to strengthen the central energizer and regulate the central qi.
Zhang et al. conducted a study on 30 patients with depression, randomly dividing them into two groups. The treatment group received acupuncture at Yinlingquan and Gongsun, as well as electroacupuncture at Baihui, Yintang, Sanyinjiao, and Zusanli. The control group received acupuncture at Zhubin and Zhaohai, as well as electroacupuncture at Baihui, Yintang, Weizhong, and Taixi. The results showed a statistically significant difference in the P300 latency induced by positive emotional images in the frontal area before and after treatment in the treatment group (p < 0.05) (Zhang et al., 2018). Research by Yang et al. (2019) analyzed experimental data and found that TP53 is the target with the highest network degree in the treatment of gastritis. Data show a correlation between TP53 and mental disorders, confirming the feasibility of treating depression syndrome based on stomach syndrome differentiation (Yang et al., 2019). Ding et al. (2016) conducted a study on rats with spleen deficiency and found that they exhibited depressive behavior, accompanied by decreased food consumption and body mass. The direct cause was a decrease in ATP content in the hippocampus, dysfunction of hippocampal mitochondria, and apoptosis of serotonin or dopamine neurons (Ding et al., 2016; Yu, 2018). Experiments have shown that acupuncture at Zusanli point in rats can stimulate the Qi and blood of the Foot Yangming Stomach Meridian, increase the content of CREB in the entire hippocampal tissue, clear serum inflammatory cytokines, reverse metabolic disorders, and have an antidepressant effect (Ye et al., 2022). Another study showed that acupuncture at “Baihui” and “Yintang” can inhibit microglia polarization imbalance by upregulating the content of triggering receptor-2 (TREM-2) in the prefrontal cortex medullary cells of depression model rats, thereby reducing the release of inflammatory factors and inhibiting central inflammatory response (Li, Xu, et al., 2021). Yue et al. (2018) found that electroacupuncture at “Baihui” and “Yanglingquan” can inhibit microglia polarization dysregulation by downregulating the expression of nucleotide-binding oligomerization domain-like receptor 3 (NLRP3) in the hippocampus of depression model rats, thereby reducing the release of inflammatory factors such as IL-1β, IL-6, IL-18, and TNF-α. Another study showed that the “Tiaoren Tongdu” acupuncture method can exert antidepressant effects by increasing the abundance of probiotics such as Bifidobacterium, Ruminococcus, and Clostridium (Yang, 2021). It shows that acupuncture and moxibustion can effectively treat depression by intervening Zusanli, Baihui, Yanglingquan, and other acupoints from the perspective of spleen and stomach, reducing the production of inflammatory factors, inhibiting the polarization of macrophages, and adjusting intestinal flora.
Acupuncture and Moxibustion Treatment Based on Kidney
The concept of the kidney in TCM plays a vital role in understanding depression. According to TCM theory, the kidney stores essence and refines it, while the marrow connects to the brain. Insufficient kidney essence or damage to the kidney due to fear can lead to weakened kidney consciousness, resulting in symptoms of depression such as fatigue, low mood, cognitive decline, decreased abilities, and skills. The kidney is considered the innate foundation, and ample kidney essence is necessary to nourish the essence of the five viscera and six viscera. Therefore, treating depression by focusing on the kidney is particularly important in perimenopausal depression, elderly depression, and poststroke depression. The “Ling Shu Hai Lun” states that the brain is the sea of marrow, where true qi gathers, and the kidneys refine the marrow, filling the brain marrow, which is essential for the formation and functioning of the brain (Qiu et al., 2019). The “Lingshu·Bencang” emphasizes the importance of a harmonious will in maintaining a straight spirit, preventing the dispersion of the soul, and avoiding negative emotions such as regret and anger. Kidney deficiency refers to the lack of nourishment in the five viscera and six viscera, the inability to maintain one’s will, and the impact on spiritual and conscious activities, which can eventually lead to depression syndrome (Li, 2015). Therefore, kidney deficiency is considered one of the core pathological mechanisms of depression. A calm mind helps stabilize kidney essence, while a lax and scattered mind can easily deplete kidney essence (Liu et al., 2019). Clinical observations have shown that focusing on tonifying the kidneys in patients with menopausal depression, elderly depression, and poststroke depression can correct internal functional disorders, significantly improve depressive symptoms, and alleviate the condition (Meng, 2017).
Acupuncture and moxibustion therapy commonly use acupoints such as Shenshu, Mingmen, Taixi, Yongquan, and Zhaohai, with Shenshu and Taixi being particularly important (Yang et al., 2021). Taixi is the original acupoint of the kidney meridian, Yongquan is the good acupoint of the kidney meridian, and Shenshu is the acupoint where the energy of the kidney meridian is infused into the waist and back. The combination of these acupoints can tonify kidney yin and kidney yang. According to the Dacheng records of acupuncture and moxibustion, acupuncture and moxibustion at Foot Shaoyin Kidney Meridian points, including Yongquan, Dazhong, and Zhaohai, can treat sadness and unhappiness. In a study by Zhang et al. (2021), 60 patients with perimenopausal depression were randomly divided into two groups. The treatment group received acupuncture at Baihui, Yintang, Fengchi, Neiguan, Sanyinjiao, Taichong, and Taixi points, as well as acupuncture at Ganshu, Shenshu, Mingmen, and Yongquan points. The control group received fluoxetine hydrochloride capsules. The treatment group showed significant improvements in HAMD score and Kupperman score compared to the control group (p < 0.05) (Zhang et al., 2021). Animal experiments have shown that using the “kidney-brain balance” theory as a guide and using electroacupuncture and moxibustion to treat perimenopausal depression in rats can significantly improve the hippocampal environment (Jing et al., 2018). This is achieved by increasing the Bcl-2/Bax ratio, BDNF, and CREB content, regulating proteins on the Notch pathway, regulating the expression of DKK1, LRP-5, and LRP-6 proteins in the hippocampus, affecting the Wnt/β-catenin signaling pathway, promoting hippocampal cell proliferation, repairing hippocampal neurons, inhibiting hippocampal neuronal cell apoptosis, and regulating the HPA axis (Deng & Ren, 2017; Jing et al., 2018). Acupuncture at Baihui, Neiguan, Zusanli, and Taichong acupoints can inhibit the expression of TXNIP in rat serum and NLRP3 in the rat hippocampus, indicating a decrease in inflammation and a positive therapeutic effect on rats with comorbid depression and coronary heart disease (Deng & Ren, 2017). It is suggested that acupuncture and moxibustion can intervene Shenshu, Mingmen, Yongquan, and other acupoints, and achieve the effect of treating depression through anti-apoptosis and anti-inflammation.
Acupuncture and Moxibustion Treatment Based on Heart
The heart plays a crucial role in TCM theory, as it governs blood and houses the spirit. Adequate heart blood is necessary for the proper regulation of the liver soul, lung soul, spleen intention, and kidney consciousness by the heart spirit. Insufficient heart blood can lead to dysfunction of the heart spirit, resulting in disturbances in consciousness, spirit, thinking, and behavior. Emotions, especially extreme emotions, can cause initial damage to the heart and mind. The “Lingshu·Evil Guest” states that the heart is the master of the five viscera and six viscera, and the mind is the place where the spirit resides. Zhang Jingyue also emphasizes that all emotions and feelings belong to the heart, and it is the heart that controls the entire spirit of the body. The heart acts as the master of the five viscera and six viscera, and when the mind is in charge of the normal function of the gods, it regulates the emotions and feelings of the five viscera, ensuring orderly human life activities. This highlights the heart’s commanding and regulating role in the emotions and feelings of the five viscera. Recent research has shown a bidirectional relationship between cardiovascular disease and depression and anxiety. Cardiovascular disease can cause and worsen depression and anxiety, while depression and anxiety can induce and worsen cardiovascular disease, significantly impacting the prognosis of cardiovascular disease (Rothenbacher et al., 2015; Zhou & Zhang, 2021). Clinical observations have found that for patients with depression and cardiovascular disease, dual heart therapy or nursing can help alleviate negative psychological emotions, improve patient compliance, enhance their quality of life, and achieve better outcomes compared to conventional treatment or nursing (Huang & Liu, 2019). Therefore, the treatment of depression often focuses on addressing the heart’s role and its connection to emotions and cardiovascular health.
The commonly used acupoints for acupuncture and moxibustion treatment are Shenmen, Xinshu, Neiguan, Jueyin shu, and so on. The frequency of use of the acupoints on Shaoyin and Jueyin meridians for treating depression syndrome is about 24.04% (Zheng et al., 2023). Shenmen and Neiguan have the effect of calming the heart and calming the mind; Heart Yu and Jueyin Yu should be located in the heart, which are the acupoints for the infusion of heart qi. They have the functions of regulating qi and blood, calming the heart and calming the mind. Acupuncture and moxibustion and Moxibustion Dacheng, Heart Spleen and Stomach Gate, said that “the heart is arthralgia, sorrow and fear: Shenmen Daling Yuji,” and acupuncture and moxibustion Juying, Sixty-six Point Song also recorded that acupuncture at Shenmen was used to treat “heartache and madness.” In the acupuncture and moxibustion and Moxibustion Atlas of Tongren Acupoints, acupuncture and moxibustion at heart meridian points can also be used to treat “laughter, hunger, sadness, and panic.” Lou et al. used the Ningxin Jieyu acupuncture method to take bilateral Shenmen, Shaohai, Neiguan, and Daling to treat the brain from the heart and alleviate poststroke depression symptoms (Lou et al., 2023). Li Hua et al. randomly divided 160 patients with poststroke depression into two groups. The treatment group consisted of 80 patients who received acupuncture treatment at Sanyinjiao, Neiguan, Shenmen, Gongsun, Baihui, Yintang, and Shenting, while the control group consisted of 80 patients who received conventional Western medicine treatment. Result: the treatment group significantly improved the HAMD-17 score, Health Questionnaire (PHQ-9) score, 5-hydroxytryptamine (5-HT), dopamine (DA), brain-derived neurotrophic factor (BNDF), and neuron specific enolase (NSE) levels in patients with depression (Li, 2023). Song et al. found that electroacupuncture stimulation of Shenmen and other acupoints in chronic stress-induced depression rats increased their food intake, body weight, percentage of sucrose water consumption, and the number of crawling and standing times in open field experiments, verifying that electroacupuncture can effectively improve the behavioral performance of chronic stress-induced depression rats (Song & Wang, 2020). It shows that acupuncture and moxibustion can regulate BNDF and NSE to effectively treat depression by intervening in heart-related Xinshu, Neiguan, Jueyin shu, and so on.
Acupuncture and Moxibustion Treatment Based on Lung
Sorrow and sadness are considered normal emotional reactions in the human body and are based on the material foundation of lung essence and lung qi. However, excessive sorrow can disrupt the descending function of the lungs, leading to poor circulation of qi and weakened lung spirit. This can manifest as symptoms of depression, such as lack of energy, laziness, solitude, and reluctance to engage with the outside world. The pathogenesis of depression syndrome is attributed to the disorder of qi movement in and out. Excessive sorrow can damage the essence and qi of the lungs, leading to lung dysfunction and qi stagnation, which can contribute to the development of depression. Modern medical research has also found a connection between respiratory diseases and depression. For example, a study on patients with chronic obstructive pulmonary disease (COPD) found that a significant percentage of them also experienced varying degrees of depression. The longer the duration of COPD, the higher the risk of depression (Wenqing et al., 2018). In clinical practice, the use of the Wenyang Xuanfei Shugan method, which focuses on warming and nourishing the lungs, has been shown to improve depressive mood and achieve similar therapeutic effects to conventional antidepressant medications but with reduced adverse reactions (Cheng et al., 2016). Wu Haoxin proposed four methods for treating depression from the perspective of the lungs: promoting lung depression, clearing lung depression, moistening lung depression, and warming lung depression (Da & Haoxin, 2018). These approaches highlight the importance and feasibility of addressing depression by starting from the lungs. In summary, the lungs play a significant role in the development and treatment of depression and approaches that focus on regulating lung function and promoting the flow of qi can be effective in managing depression symptoms.
The commonly used acupoints for acupuncture and moxibustion in the treatment of depression include Hegu (LI4), Taiyuan (LU9), and Feishu (BL13) (Yang et al., 2021; Xuanyin et al., 2017). According to the Suwen Acupuncture Theory, needling the origin of Taiyin in the hand, among other points, is used to prevent lung diseases and strengthen the spirit and root. This helps to maintain the presence of positive qi in the body and prevent the intrusion of pathogenic factors. By targeting acupoints such as Hegu, Taiyuan, and Feishu, acupuncture and moxibustion aim to regulate the flow of qi and restore the balance of the body’s energy.
Taiyu et al. (2020) conducted a study on patients with chronic transmission constipation and divided them into three groups. The treatment group received acupuncture at Zusanli, Feishu, and Zhigou, along with moxibustion at Qihai and Guanyuan. The acupuncture and medicine treatment group received acupuncture at Zusanli, Feishu, and Zhigou, along with medication. The results showed that the treatment group had significant improvements in SAS and SDS scores, as well as serum VIP and SP levels (Taiyu et al., 2020). In another study by Kaixuan et al. (2021), patients with depression were randomly divided into two groups. The treatment group received acupuncture at Jiaji acupoints corresponding to Feishu, Xinshu, Ganshu, Pishu, and Shenshu, along with oral administration of Yueju Baohe Wan. The control group received treatment with amitriptyline hydrochloride tablets. The treatment group showed significant improvements in HAMD score, HAMA score, TESS score, alpha wave frequency, and amplitude in the electroencephalogram, and serum 5-HT and DA levels. The treatment group also had better short-term and long-term efficacy compared to the control group (Kaixuan et al., 2021). Animal experiments conducted by Peng et al. (2016) showed that electroacupuncture at acupoints such as Hegu and Taichong increased the glucose preference rate and delayed eating time in poststroke depressed rats. The behavioral indicators of depressed rats also improved. The mechanism of action may be related to the expression levels of BDNF/mTORC1 pathway proteins, synaptic-related proteins PSD95, Synapsin I, and GluR1, dendritic spine density, and synaptic plasticity. These studies suggest that acupuncture and moxibustion, particularly when targeting acupoints such as Feishu and Hegu, can effectively improve mental illness symptoms and behavioral indicators associated with depression (Peng et al., 2016). It is suggested that acupuncture and moxibustion can interfere with Feishu and other acupoints, and effectively achieve depression by regulating BDNF/mTORC1 and other signal pathways.
Conclusion
Acupuncture and moxibustion treatment for depression has shown remarkable efficacy, minimal side effects, and high clinical value. Its mechanism of action is primarily related to neurotransmitters, receptors, the endocrine system, and the brain-gut axis. Acupuncture and moxibustion treatment provides a new direction for clinical depression treatment. However, there are still some challenges and areas for improvement in acupuncture and moxibustion treatment for depression: (a) lack of comprehensive understanding: While doctors approach the treatment of depression by regulating the five zang organs and six fu organs from different angles, further research is needed to identify the preferred acupoints for treating depression based on specific organ recuperation and recovery. (b) Integration of the five zang organs: in current research, there is a focus on the liver, heart, and spleen when treating the five zang organs individually, while the lung and kidney are often neglected. There is a need for more standardized and comprehensive research on the integrated application of the five zang organs in acupuncture and moxibustion treatment for depression. TCM studies have explored this aspect, but there is a lack of sufficient research specifically on acupuncture and moxibustion. In clinical practice, commonly used acupoints such as Tai Chong (LV3), San Yin Jiao (SP6), Neiguan (PC6), Shen Men (HT7), Zu San Li (ST36), He Gu (LI4), and Tai Xi (KI3) are often selected. Further research is needed to validate the rationality and effectiveness of acupuncture and moxibustion treatment for depression. Rigorous clinical and mechanism studies on this treatment approach should be a focus for future research. Additionally, there is a need for more comprehensive research on the integrated application of the five zang organs, as well as more studies specifically focused on acupuncture and moxibustion treatment for depression, to address the existing gaps and provide new research directions.
Abbreviations
CCK: Cholecystokinin; CGRP: Calcitonin gene-related peptide; COPD: Chronic obstructive pulmonary disease; GFAP: Glial fibrillary acidic protein; HAMDv: Hamilton Depression Rating Scale; IBS: Irritable bowel syndrome; IL-10: Interleukin-10; NLRP3: Nucleotide-binding oligomerization domain-like receptor 3; TCM: Traditional Chinese medicine; TREM-2: Triggering receptor-2; VIP: Vasoactive intestinal peptide; WHO: World Health Organization.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval and Informed Consent
Not applicable.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the National Natural Science Foundation of China (Grant no. 81303044), Natural Science Foundation of Heilongjiang Province (Grant no. LH2022H082), Postdoctoral Research Initiation Grant Project of Heilongjiang Province (Grant no. LBH-Q19185), Project of Heilongjiang Provincial Administration of Traditional Chinese Medicine (Grant no. ZHY2020-120), and Postgraduate Innovative Scientific Research Project of Heilongjiang University of Traditional Chinese Medicine (Grant no. 2020yjscx016).
