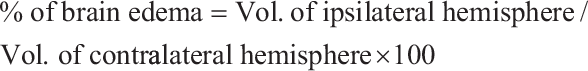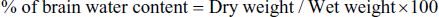Abstract
Background
Cerebral ischemia is a syndrome that occurs due to the restricted flow of oxygen-rich blood to the brain, causing damage to the brain cells. Globally, ischemia ranks second in causing mortality and third in causing disability in stroke patients. Nerolidol is a bioactive compound present in the essential oil of plants with a floral odour. It is a natural sesquiterpene alcohol used in cosmetics, perfumes, and as a food flavouring agent. It also possesses antioxidant, antimicrobial, anti-inflammatory, and anticancer properties.
Materials and Methods
In this study, we assessed the anti-ischemic property of nerolidol in cerebral ischemia-induced mice. Healthy male Wistar rats were induced into cerebral ischemia with middle cerebral artery occlusion (MCAO) and treated with 10 mg and 20 mg nerolidol for 21 days. The brain morphometric, antioxidant, and MMP levels were estimated in the brain tissue of MCAO-performed and nerolidol-treated rats. The cerebral infarct-alleviating potency of nerolidol was analysed by estimating the levels of inflammatory cytokines and apoptotic proteins. It was further confirmed by assessing the levels of COX-2/PGE-2 signalling proteins in brain tissue from MCAO-performed in rats.
Results
Nerolidol significantly reduced the cerebral infarct volume and brain edema via increased antioxidant levels and decreased MMPs. It also decreased the pro-inflammatory cytokines and proapoptotic proteins in brain tissue. The inflammatory signalling proteins NFκB, COX-2, and PGE-2 were significantly decreased in nerolidol-treated MCAO-performed rats, confirming the antiischemic property of nerolidol.
Conclusion
Our results prove nerolidol significantly alleviates cerebral ischemia in rats, and it can be subjected to further trials to be formulated as an anti-ischemic drug.
Introduction
The brain that accounts for only 2% weight of the whole body requires about 20% of oxygenated blood for its function. Since the brain requires a high level of oxygen and ATP for its neuronal functions, it is extremely sensitive to oxidative damage.1, 2 Stroke is a clinical condition that occurs due to the interrupted oxygenated blood supply to the brain. Global statistics data report ranks stroke, to be second among mortality-causing diseases. 3 Worldwide about 5.5 million mortalities and 116 million stroke patients suffering from stroke-associated morbidities have been reported. 4 Stroke can be classified into two based on the disease condition ischemic stroke and hemorrhagic stroke. About 80% of people suffer from an ischemic stroke which occurs due to blockage of the blood vessel causing reduced blood substantially resulting in brain infarction. Twenty percentage of people suffer from a hemorrhagic stroke which causes due to the rupture of the blood vessel. 5
Neuroinflammation is a double-edged sword which enhances the stroke-induced infarct and also promotes the recovery process after acute stroke. 6 Cyclooxygenase-2/prostaglandin-E2 (COX-2/PGE-2) signalling pathway mediates inflammatory process in neuronal cells thereby inducing neuronal death. 7 Celecoxib, COX-2 inhibitor down-regulates PGE-2 release thereby delaying the onset of neuronal and prolonging the survival of neurons. 8 The role of COX-2/PGE-2 signalling in ischemic stroke and the neuroprotective role COX-2 inhibitors was not yet elucidated.
Existing drugs used to treat ischemic stroke possess only any one of the mechanisms of action such as scavenging free radicals, preventing thrombolysis, anti-inflammatory, and antiplatelet.9, 10 Hence these drugs are not effective and require long-term administration which causes many side effects.11, 12 Also the inflated prices of these drugs cause most countries to spend about 3−4% of their nation’s expenditure. 13 Therefore discovering a potent cost-effective drug with nil side effects to treat ischemic stroke will be a great relief. Phytomedicines practised traditionally tends to be a potent alternative to these synthetic drugs. Phytomedicine is potent, safe, and affordable for users. 14 Past two decades numerous researches were focused to discover the mechanism of action of phytochemicals in treating neurological disorders.
Nerolidol also known as peruviol is natural aliphatic sequiterpene alcohol found in the essential oil of floral-scented flowers and plants.15, 16 It is isolated from plants such as neroli, lemongrass, tea tree, ginger, and rose.17, 18 Globally per annum about 10−100 metric tons of nerolidol was used in cosmetics, food, and other products such as detergents. 19 Nerolidol is US FDA-approved food flavouring agent. 20 It possesses antioxidant, antimicrobial, anti-inflammatory, antinociceptive, and anticancer properties.15, 21 The neuroprotective effects of nerolidol were already reported in different models.22, 23 But, its therapeutic roles in ischemic stroke were not studied yet. Therefore, herein we evaluated the anti-ischemic role of nerolidol in vivo model. In the present study, we evaluated the neuroprotective role of nerolidol and its effect on COX-2/PGE-2 signalling pathway in the middle cerebral artery occlusion (MCAO)-performed rat model.
Materials and Methods
Chemicals
Nerolidol and other chemicals were purchased from Sigma Aldrich, USA. The ELISA assay kits were purchased from Cayman Chemical, Invitrogen, and Abcam, USA.
Experimental Animals
Healthy male 10 weeks old Wistar rats weighing about 250−280 g were used for the present study. The rats were acclimatized in the laboratory condition with 22 ± 1°C temperature and 60 ± 5% relative humidity. The 12-h/12-h light and the dark cycle were strictly maintained. Rats were housed in each clean propylene cage and fed a standard laboratory pellet diet and water ad libitum. The autoclaved rice husk bedding was used for the rat’s cage and it was changed daily. The rats were handled with utmost care and concern. All the procedures carried out on animals were approved by the institutional animal ethical committee.
MCAO Surgical Procedure
The rats were subjected to overnight fasting before the MCAO surgery. Before surgery, the rats were anaesthetized by inhalation of 3% isoflurane along with 80% oxygen. The anaesthetized rats were fixed onto the surgical table in a supine position and an incision was made on the midline neck. The right common carotid artery was isolated from the vagus nerve and 6-0 nylon monofilament was inserted from the external carotid artery incision to the middle cerebral artery to create an occlusion. The occlusion was maintained for a period of 1 h and the nylon filament was removed for reperfusion. During the whole surgical procedure, the rats were monitored for temperature, blood pressure and heart rate. The sham-operated rats have also undergone the same surgical procedure only the insertion of monofilament into the middle cerebral artery was not done. 24
Experimental Design
After MCAO surgery the rats were grouped into four with six rats in each group (n = 6), the Sham-operated rats are group I control rats. Group II are MCAO-induced rats which do not receive any treatment. Group III are MCAO-induced rats which were treated with 10 mg/kg nerolidol through oral gavage 2 h after the MCAO procedure. Group IV are MCAO-induced rats which were treated with 20 mg/kg nerolidol through oral gavage 2 h after the MCAO procedure. The nerolidol treatment was given for a period of 21 days. After the treatment period, the rats were euthanized and the blood and brain tissue samples were collected for further investigations.
Brain Morphometric Analysis
Infarct Volume
The brain tissues of ischemia-induced untreated and nerolidol-treated rats were coronally sectioned with an interval of 2 mm and the alternative sections of brain tissue slices were treated with 2% 2,3,5-triphenyltetrazolium chloride for a period of 30 min at 37˚C and then fixed with 4% paraformaldehyde solution for further analysis. The tissue sections were viewed under a microscope and the images were analysed and the area of infarction was measured using Image J software. The infarct volume of brain slices was measured by multiplying the infarct area by the thickness of brain slices and the total infarct volume is the sum of the infarct volume of brain slices.
Brain Edema
The brain edema was in control and experimental rats were calculated using the following formula:
Brain Water Content
The whole brain tissue was weighed immediately after dissection and the tissue was incubated at 100ºC to remove water content and the dry tissue weight was measured. The brain water content was measured using the formula
Antioxidant Measurement
Superoxide Dismutase (SOD) Estimation
The activity of superoxide dismutase was measured using the protocol of Marklund and Marklund. 25 The enzymatic inhibition of nitroblue tetrazolium photoreduction was measured to estimate the enzymatic activity of SOD. The inhibition of pyrogallol autoxidation was measured at 420 nm and the SOD activity was expressed as U/mg protein.
Catalase Estimation
The catalase activity of the control and experimental samples were measured according to the method of Hadwan and Abed. 26 The catalytic activity of the samples was measured by estimating the decomposition of hydrogen peroxide. The reaction was stopped using ammonium molybdate and molybdate hydrogen peroxide complex was measured at 374 nm. The results were expressed as U/mg protein.
Glutathione Peroxidase (GPx) Estimation
The GPx activity of the control and experimental samples were measured using the protocol of Sabarathinam et al. 27 The sample was mixed with reduced glutathione, hydrogen peroxide, EDTA, sodium azide, and incubate at 37˚C for 10 min. TCA was added to the mixture to stop the reaction and the supernatant was mixed with DTNB solution. The final mixture absorbance was measured at 420 nm. The GPx activity was expressed as U/mg protein.
Glutathione Estimation
The levels of glutathione in the control and experimental group were measured with Ellman’s reagent. 28 Glutathione in the sample reacts with DTNB to form TNB chromophore which was spectrophotometrically measured at 412 nm. The TNB adduct concentration is directly proportional to the level of glutathione. The glutathione levels were expressed as U/mg protein.
Quantification of Nitrate
Nitrate levels in the samples of ischemic-induced untreated and nerolidol-treated rat’s brain tissue were measured using the nitrate/nitrite colorimetric assay kit procured from Cayman Chemical, USA. Initially, the nitrate was converted to nitrite utilizing the nitrate reductase enzyme. Upon addition of Griess reagent I, the nitrite is reduced to nitrogen oxide and it further reacts with Griess reagent II to form the stable product. The final product absorbance was measured at 550 nm to determine the levels of nitrate.
Quantification of Lipid Peroxidation
The level of lipid peroxidation in brain tissues of ischemia-induced untreated and nerolidol-treated rats was measured by estimating the levels of malondialdehyde (MDA) using an assay kit procured from Abcam, USA. The MDA present in the sample reacts with thiobarbituric acid to form an MDA-TBA adduct which was spectrophotometrically quantified at 532 nm.
Quantification of Matrix Metalloproteinase
The MMP-2 and MMP-9 levels in the brain tissues of ischemia-induced untreated and nerolidol-treated rats were measured using the ELISA kits procured from Invitrogen, USA. The experiment was performed as per the guidelines of the manufacturer. The experiment was performed in triplicates. The levels of MMPs were estimated with a standard curve plotted with the absorbance value of standard concentration.
Estimation of Apoptotic and COX-2/PGE-2 Signalling Proteins
Apoptotic proteins Bcl-2, Bax, and Caspase-3 and COX-2, NFκB were measured using the ELISA kit procured from Invitrogen, USA. All the assays were done as per the protocol provided in the manufacturer’s manual.
Estimation of Inflammatory Cytokines
Pro-inflammatory cytokines TNF-α, IL-1β, IL-6, and anti-inflammatory cytokine IL-10 in the brain tissues of ischemia-induced untreated and nerolidol-treated rats were measured using a commercially available ELISA kit (Sigma Aldrich, USA). The assay was performed according to the assay protocol provided in the kit manual. The absorbances of samples and standards were measured at 450 nm.
Statistical Analysis
All the tests were performed in triplicates and the results were statistically analysed with one-way ANOVA followed by the post hoc Dunnett’s test. The statistical analysis was performed with GraphPad Prism software. The results were represented as mean ± SD of triplicates and the statistically significant difference was considered as a p value less than .05.
Results
Nerolidol Protective Effect on Brain Morphometry of Cerebral Ischemia-induced Rats
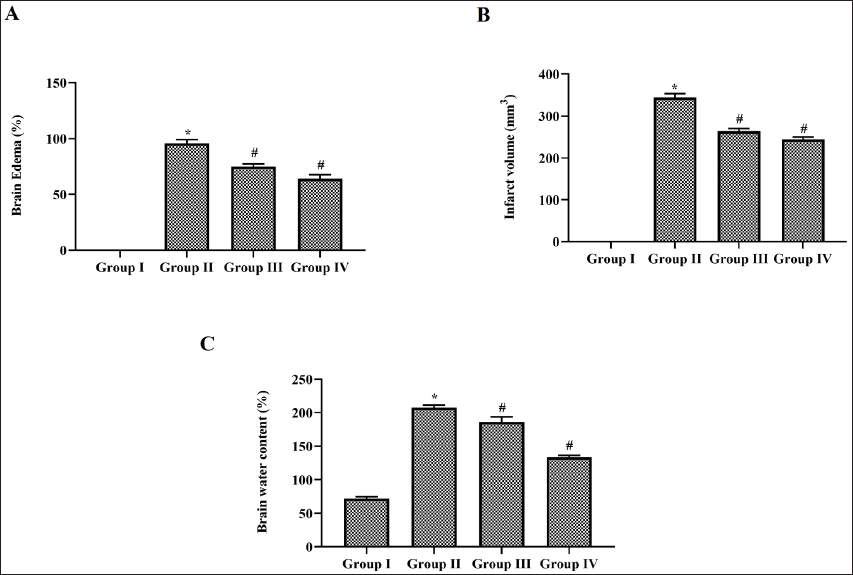
The neuroprotective effect of nerolidol on cerebral ischemia-induced rats was assessed by evaluating the infarct volume, percentage of brain edema, and brain water content and the results were illustrated in Figure 1. No infarct or brain edema was reported in the control rats whereas the MCAO-performed untreated rats showed 350 ± 5 mm3 infarct volume and 90 ± 3% of brain edema. Nerolidol-treated MCAO-performed rats showed a decrease in the infarct volume and brain edema compared to the MCAO-performed untreated rats. 10 mg/kg nerolidol-treated rat shown 275 ± 8 mm3 of infarct volume and 73 ± 4% brain edema whereas it is decreased to 263 ± 4 mm3 and 65 ± 6%, respectively in higher dose 20 mg/kg nerolidol-treated rats. 70 ± 8% water content was observed in the control rat’s brain whereas it was drastically increased to 215 ± 6% in MCAO-performed untreated rat’s brain. Nerolidal treatment significantly decreased the brain water content in MCAO-performed rats.
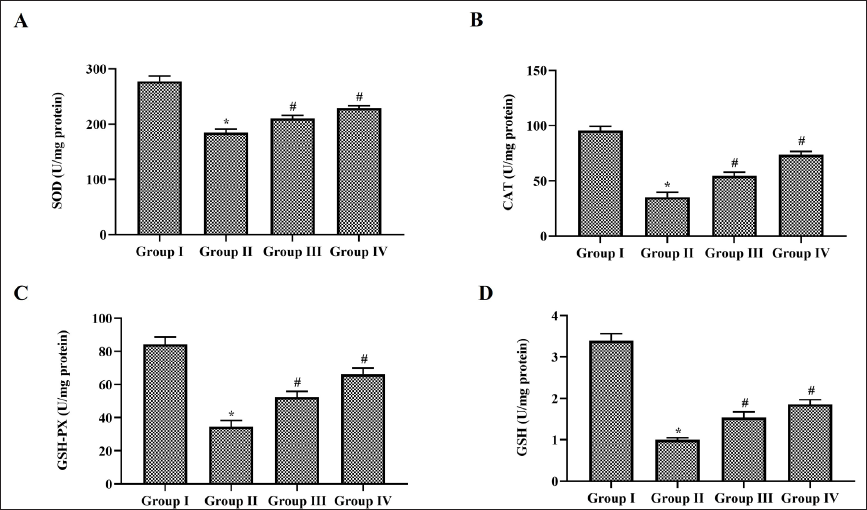
Effect of Nerolidol on Antioxidants in Cerebral Ischemia-induced Rats
Scavenging free radicals plays a key mechanism in repairing cerebral infarct hence we assessed the antioxidant status in nerolidol-treated MCAO-performed rat’s brain tissue. MCAO in rats lead to a drastic decrease in both enzymatic and non-enzymatic antioxidants compared to the Sham-operated control rats. Nerolidol treatment significantly increased the levels of enzymatic antioxidants SOD, CAT, GPx, and non-enzymatic antioxidant glutathione in MCAO-performed rats (Figure 2). Compared to low-dose nerolidol-treated rats the higher dose 20 mg/kg nerolidol treated showed a significant increase in the antioxidants levels.
Effect of Nerolidol on Nitrate Levels in Cerebral Ischemia-induced Rats
The metabolism of nitrate, nitrite, and nitric oxide is precisely related to endothelial injury in stroke conditions therefore we assessed the levels of nitrate in the cortex and striatum of MCAO-performed untreated and nerolidol-treated rats. A significant increase in the levels of nitrate was observed in both cortex and striatum tissue compared to the control rats. Nerolidol treatment significantly decreased the levels of nitrate in a dose-dependent manner (Figure 3A).
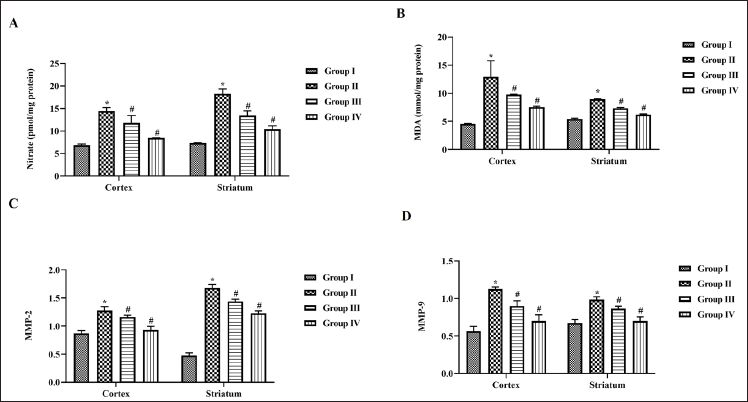
Effect of Nerolidol on Lipid Peroxidation Inhibition in Cerebral Ischemia-induced Rats
Figure 3B depicts the levels of oxidative stress biomarker MDA evaluated in cortex and striatum tissues of MCAO-performed untreated and nerolidol-treated rats. Compared to control rats the MCAO-performed untreated showed increased levels of MDA content. Both the low- and high-dose nerolidol treatment significantly decreased the levels of MDA. Compared to striatum tissue the cortex tissue exhibited an increased level of MDA in MCAO-performed untreated rats.
Effect of Nerolidol on Matrix Metalloproteinase in Cerebral Ischemia-induced Rats
Inhibitors of matrix metalloproteinase act as a potent drug to alleviate stroke conditions hence we estimated the levels of MMPs in nerolidol-treated and untreated MCAO-performed rats (Figure 3C and D). Both MMP-2 and MMP-9 levels were significantly increased in MCAO-performed untreated rats whereas nerolidol treatment decreased the levels of MMPs in both the cortex and striatum tissues. Control rats expressed decreased levels of MMP-2 and increased levels of MMP-9 in striatum tissue compared to cortex tissue.
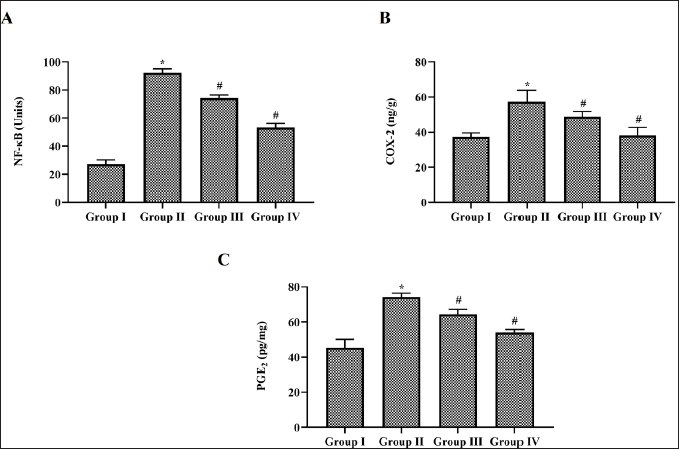
Effect of Nerolidol on COX-2/PGE-2 Signalling Protein in Cerebral Ischemia-induced Rats
Figure 4 illustrates the level of COX-2/PGE-2 signalling proteins in MCAO-performed untreated and nerolidol-treated rats. Compared to control rats MCAO-performed rats showed increased levels of NFκB, COX-2 and PGE-2 indicating the occurrence of inflammation. Nerolidol treatment significantly decreased the levels of NFκB, COX-2 and PGE-2 in MCAO-performed rats.
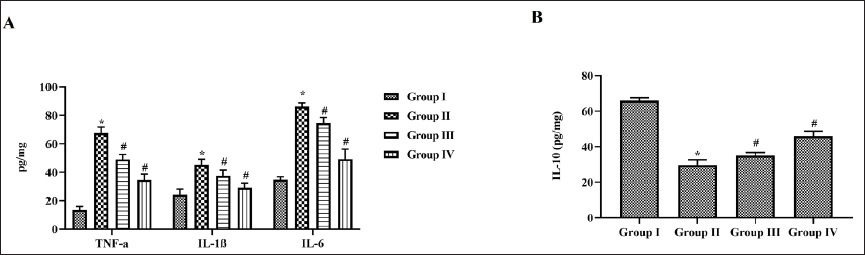
Effect of Nerolidol on Inflammatory Cytokines in Cerebral Ischemia-induced Rats
Figure 5 shows the results of proinflammatory cytokines and anti-inflammatory cytokines levels in MCAO-performed untreated and nerolidol-treated rats. MCAO increased the levels of proinflammatory cytokines TNF-α, IL-1β, and IL-6 (Figure 6A) whereas decreased the level of anti-inflammatory cytokine IL-10 (Figure 6B). Dose-dependent decreases in the levels of proinflammatory cytokines TNF-α, IL-1β, and IL-6 were observed in the nerolidol-treated MCAO-performed rats. Nerolidol also significantly increased the levels of IL-10 in MCAO-performed rats compared to the untreated rats.
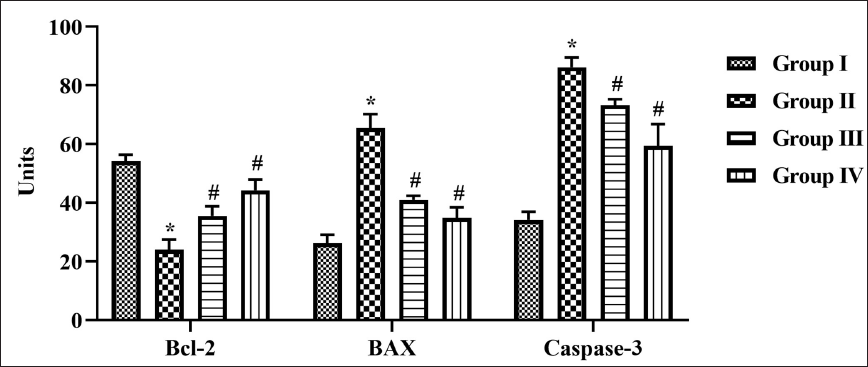
Effect of Nerolidol on Apoptotic Protein in Cerebral Ischemia-induced Rats
Apoptotic protein regulates the occurrence of cerebral infarct hence we measured the levels of both proapoptotic proteins Bax and Casp-3 (Figure 5), and antiapoptotic protein Bcl-2 (Figure 5) in MCAO-performed untreated and nerolidol-treated rats. Increased levels of proapoptotic proteins were estimated in the MCAO-performed untreated rat’s brain tissue. The antiapoptotic protein Bcl-2 level was significantly decreased in MCAO-performed on untreated rat’s brain tissue. Nerolidol treatment significantly decreased the levels of Bax and Casp-3 and increased the level of antiapoptotic protein Bcl-2 in a dose-dependent manner.
Discussion
Stroke is a predominant cerebrovascular disease which causes significant mortality and morbidity worldwide. It is broadly categorized as ischemic and hemorrhagic stroke where 80% of the patients experience ischemic stroke. Cerebral ischemic stroke occurs due to clogged blood vessels caused by thrombus or emboli which leads to interrupted blood flow. Thrombus occurs due to blood dysfunction caused due atherosclerotic disease, inflammation or arterial dissection within the blood vessel, whereas emboli which formed in other parts of blood vessels affect the cerebral blood vessel through blood flow.29, 30 Ischemic stroke initially evokes hypoxia-induced signals and further reperfusion-induced signals such as glutamate-induced excitotoxicity, oxidative stress, accumulation of matricellular proteins, and neuroinflammation causing cerebral infarct.31, 32
The middle cerebral artery (MCA) which streams blood to the lateral brain and basal ganglia is the primary artery affected by stroke. The disruption in the MCA causes dysfunction in the motor and sensory functions of the brain. 33 MCAO involves both ischemia followed reperfusion which causes a cascade of mechanism that occurs during ischemic stroke condition. Therefore in this study, we performed the MCAO model to induce stroke in rats. Brain edema is a common pathophysiology that occurs in many clinical conditions, especially during stroke. In ischemic conditions the glutamate, sodium, and calcium channel were disrupted which causes the excessive accumulation of water in the brain.34, 35 Cerebral infarct is another predictor of ischemic stroke which occurs due to the intracerebral artery occlusion.36, 37 Nerolidol treatment in MCAO-performed rats significantly decreased both brain edema and cerebral infarct proving the neuroprotective role against ischemic stroke.
Oxidative stress occurs during the initial reperfusion stage, accumulation of free radicals, and calcium overload causes excessive neuronal injury. Excessive generation of free radicals causes an imbalance in the brain antioxidant system leading to brain infarct.38, 39 Enzymatic antioxidants superoxide dismutase and catalase effectively scavenge oxygen free radicals superoxide, and hydrogen peroxide generated during the ischemic condition.40, 41 Cerebral ischemia significantly decreases the levels of antioxidants glutathione and GPx causing cell necrosis. 42 Nerolidol, a potent antioxidant significantly increased the levels of SOD, CAT, GPx, and glutathione thereby preventing brain tissue injury induced by MCAO.
Nitrate-nitrite-NO metabolic pathway was reported to be associated with inflammation. The metabolism of Nitrate-nitrite-NO affects the vasodilation and contraction function which eventually leads to neuroinflammation in ischemic conditions. Oxidative stress disturbs Nitric oxide signalling and induces inflammation. 43 Ischemic condition activates iNOS which in turn elevates nitric oxide which oxides the lipids, and protein causing cell injury. 44 In this study, the MCAO-performed rats showed increased levels of nitrate in cortex and striatum regions of the brain and also showed an increased level of lipid peroxidation confirming the cell infarct. Nerolidol treatment significantly decreased the levels of nitrate thereby reduced lipid peroxidation.
Matrix metalloproteinase are enzymes with a proteolytic activity that degrades extracellular matrix. Disruption in MMPs causes cerebral edema, BBB disruption, inflammation, and hemorrhage.45, 46 MMPs are classified as constitutive and inducible enzymes. Constitutive enzymes maintain integrity of the basement membranes whereas inducible enzymes upon activation causes neuronal cell damage. During acute stroke condition initially, the activation of MMP-2 occurs which disrupts the extracellular matrix proteins and further activates MMP-9 causing infiltration of inflammatory cells. 47 Nerolidol treatment decreased the levels of both MMP-2 and MMP-9 in MCAO-performed rats thereby preventing ischemic-induced BBB disruption this may be the reason for the decrease in brain edema in nerolidol-treated MCAO-performed rats.
Neuroinflammation occurs during ischemic intensifies the synthesis and release of cytokines infarct region. 48 COX-2/PGE-2 signalling pathway plays a key role in the inflammatory cascade mechanism in various diseases. COX-2 is an oxidoreductase enzyme which converts arachidonic acid into prostaglandins thereby activating an inflammatory cascade. 25 Cytokines are vital mediators in ischemic stroke-induced neuroimmunomodulatory changes and aggravate cerebral infarct progression.49, 50 Proinflammatory cytokines TNF-α, IL-1β, and IL-6 promote neuronal damage during ischemic conditions. Numerous animal and human studies have reported increased levels of TNF-α during ischemic conditions.51, 52 Antiinflammatory properties of nerolidol inhibited the COX-2, PGE-2, and NFκB signalling proteins thereby decreasing the levels of proinflammatory cytokines TNF-α, IL-1β, and IL-6 in MCAO-performed rats. It also increased the levels of anti-inflammatory cytokine IL-10 in MCAO-performed rats.
Reperfusion during cerebral ischemic conditions causes neuronal apoptosis which increases the cerebral infarct. Hence we analysed the antiapoptotic role of nerolidol in MCAO-performed rats. Nerolidol significantly increased the antiapoptotic Bcl-2 protein and decreased the levels of proapoptotic protein Bax and Casp-3 confirming the antiapoptotic potency of nerolidol during ischemic conditions.
Conclusion
Cerebral ischemic stroke is a deadly disease which not only increased the number of mortalities but causes numerous post-stroke complications causing lifetime disability in patients. At present treating stroke patients is much more expensive and most of the drugs cause other complications in long-term usage. In this study, we analysed the role of nerolidol a bioactive compound on MCAO-performed mice. Nerolidol treatment significantly increased the antioxidants and persuasively inhibited the COX-2/PGE-2 signalling pathway thereby reducing the synthesis of inflammatory cytokines. It also inhibited the apoptotic proteins and decreased the cerebral infarct. Nerolidol seems to be a potent and safe neuroprotective drug hence, it can be subjected to human trials in the future to treat cerebral ischemic stroke.
Footnotes
Abbreviations
SOD: Superoxide dismutase; CAT: Catalase; GPx: Glutathione peroxidase; MCAO: Middle cerebral artery occlusion; MDA: Malondialdehyde.
Acknowledgment
This work was supported by the School of Health, Binzhou Polytechnical College, No.919, Yellow River 12th Road, Binzhou City, Shandong Province, 256603, China.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Statement of Informed Consent and Ethical Approval
We have completed the animal experimental based on the animal ethical guidelines and same experimental procedures were approved by the committee.
Summary
Cerebral ischemia is a syndrome which occurs due to the restricted flow of oxygen-rich blood to the brain causing damage to the brain cells.
Nerolidol is a bioactive compound present in the essential oil of plants with a floral odour.
Nerolidol significantly reduced the cerebral infarct volume, and brain edema via increased the antioxidants levels and decreasing the MMPs.