Abstract
Background: Alteration in cytokine levels are known to be involved in the pathogenesis of schizophrenia.
Objectives: To estimate the serum levels of interleukin-17 (IL-17) and interleukin-10 (IL-10) and their association with disease progression in schizophrenia.
Methods: A total of 67 schizophrenia cases were enrolled in the present study. IL-17 and IL-10 were estimated by enzyme-linked immunosorbent assay. Positive and Negative Syndrome Scale (PANSS) was used to evaluate disease severity.
Results: IL-17 was positively correlated with positive symptom score (
Conclusion: IL-17 and IL-10 are associated with disease severity in schizophrenia but are not good markers for predicting the disease progression.
Abbreviations
IL-17: interleukin-17; IL-10: interleukin-10; PANSS: positive and negative syndrome scale
Introduction
The prevalence of schizophrenia is increasing worldwide, including India. According to recent National Mental Health Survey, its prevalence is around 0.5% in India. 1 While the etiology of schizophrenia is considered multifactorial, several studies support the alterations of inflammatory processes in its pathogenesis. 2
Interleukin-17 (IL-17), a Th17 cytokine increases the production of other proinflammatory cytokines like IL-6 and IL-8. 3 IL-17 is involved in the pathogenesis of several neurological disorders. 4 Autism spectrum disorder development was found to be associated with the dysregulation of IL-17A. 5 The previous studies in schizophrenia have documented contradictory reports related to IL-17 levels. El Kissi et al have reported elevated IL-17 levels, whereas Dimitrov et al have reported reduced values of IL-17 in patients with schizophrenia when compared with controls and demonstrated that IL-17 was negatively associated with negative symptoms of schizophrenia.6, 7
Interleukin-10 (IL-10) is considered as neuroprotective cytokine, which prevents neuronal dysfunction. 8 Alzheimer’s disease and multiple sclerosis were found to be associated with the alteration in IL-10 levels.9, 10 IL-10 based treatment modalities have been found to be useful in the treatment of neuroimmune diseases. 11 Xiu et al have demonstrated that reduced IL-10 levels in schizophrenia were related to cognitive impairment and negative symptoms. 12 Maes et al have reported an increase in IL-10 levels on treatment with neuroleptics. 13 Dimitrov et al have suggested that IL-10 is associated positively with severity of schizophrenia. 7
Since an imbalance in pro- and anti-inflammatory cytokines plays a role in the development of schizophrenia, the objective of the study was to estimate IL-17 and IL-10 levels and their relation with disease progression in schizophrenia.
Materials and Methods
It is a case control study done in a tertiary care hospital in southern India. A total of 67 schizophrenia patients in the age group of 18–45 years were enrolled in the study. Schizophrenia was diagnosed according to
The study was approved by JIPMER Ethics Committee (Reg. no. JIP/IEC/2015/20/708, dated 30/10/2015). A written informed consent was obtained from all the subjects or their legally acceptable representatives. A 5 mL of blood sample was collected, and the serum obtained was used to estimate IL-17 and IL-10. Enzyme-linked immunosorbent assay (ELISA) technique (Diaclone kits, France) was used to estimate IL-17 and IL-10. Positive and Negative Syndrome Scale (PANSS) was used to evaluate severity of schizophrenia. 14
Statistical Analysis
One-way ANOVA was used to compare the clinical characteristics and interleukins among subgroups of schizophrenia based on PANSS score. Pearson’s correlation analysis was used to investigate the relation between interleukins and PANSS scores. Receiver operating characteristic (ROC) curve analysis was performed to identify the cutoff value, specificity and sensitivity of IL-17 and IL-10 in schizophrenia cases with increase in PANSS score. All the statistical tests were considered significant if the
Results
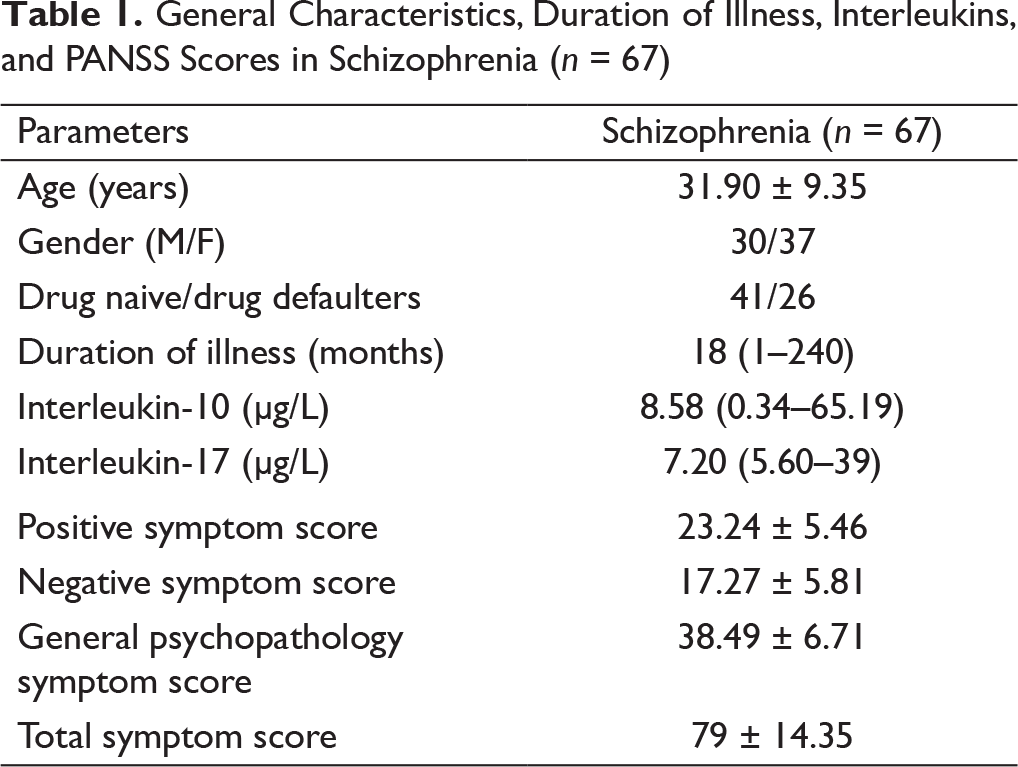
The clinical characteristics and interleukins are shown in Table 1. The mean duration of illness in schizophrenia was 18 months (range: 1–240 months). A total of 41 patients were drug naive and 26 were drug defaulters. The median (ranges) value for IL-10 was 8.58 (0.34–65.19) and for IL-17 was 7.20 (5.60–39). The mean positive symptoms score was 23, negative symptom score was 17 and total symptom score was 79. Among drug naive and drug defaulters, the difference in PANSS scores, IL-17 and IL-10 was not significant (data not shown).
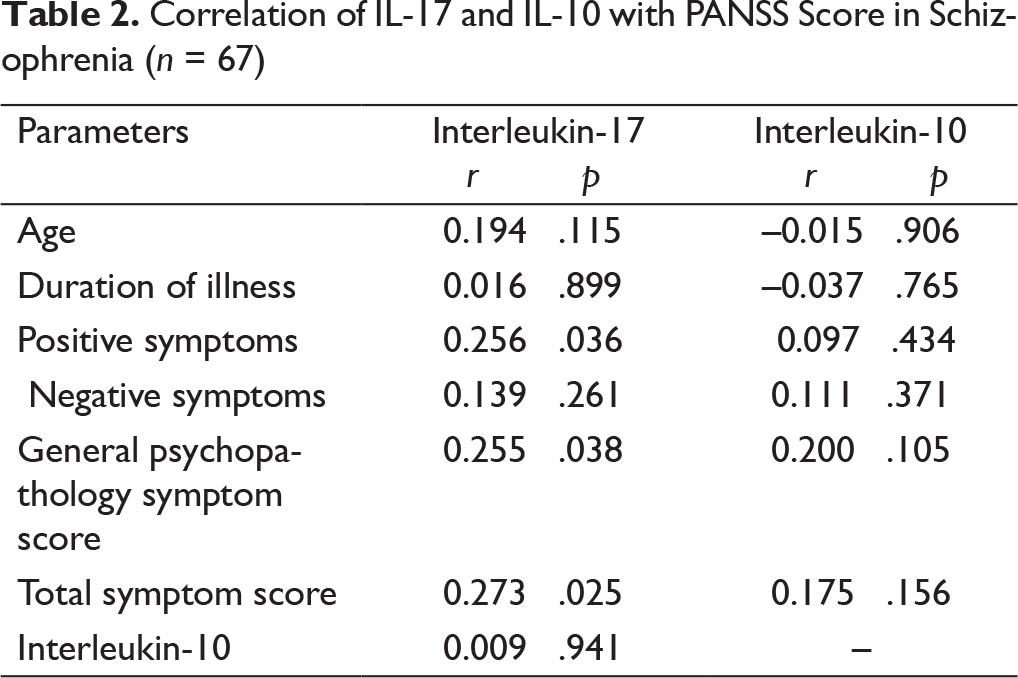
Table 2 shows the correlations of interleukins with PANSS scores. IL-17 was significantly associated with positive symptom score (
General Characteristics, Duration of Illness, Interleukins, and PANSS Scores in Schizophrenia (n = 67)
Correlation of IL-17 and IL-10 with PANSS Score in Schizophrenia (n = 67)
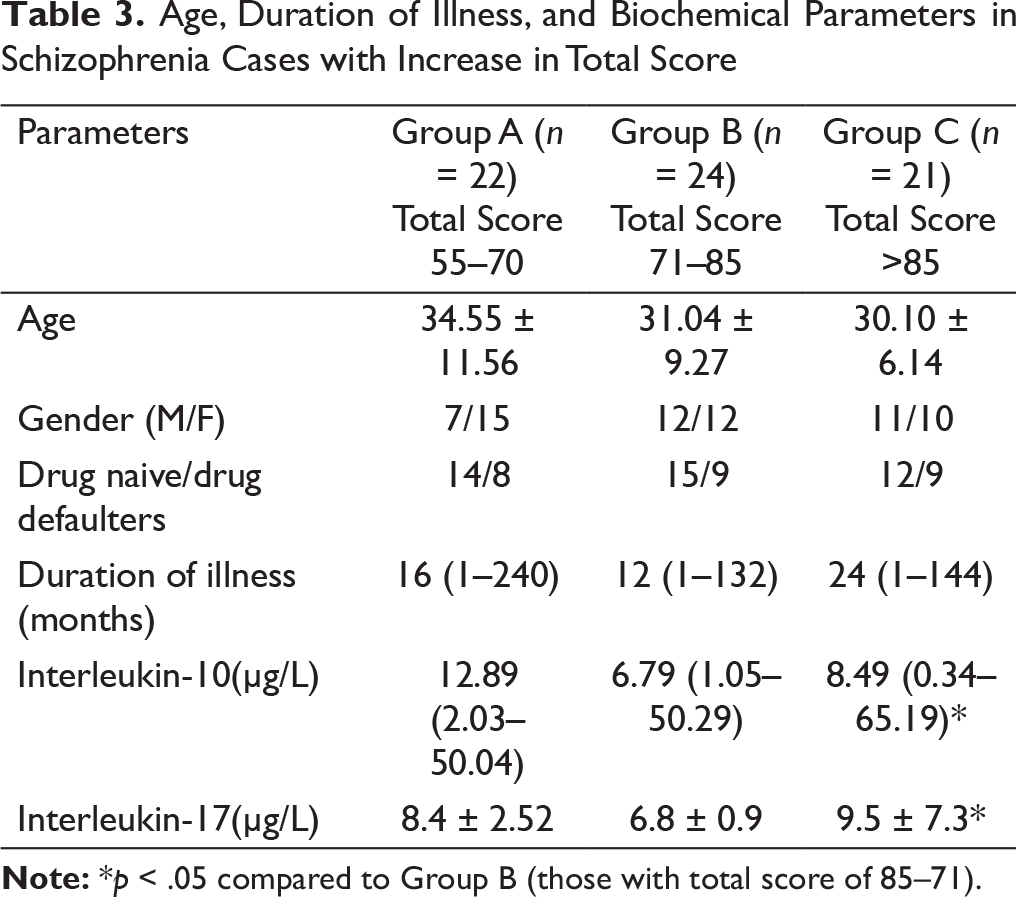
Age, Duration of Illness, and Biochemical Parameters in Schizophrenia Cases with Increase in Total Score
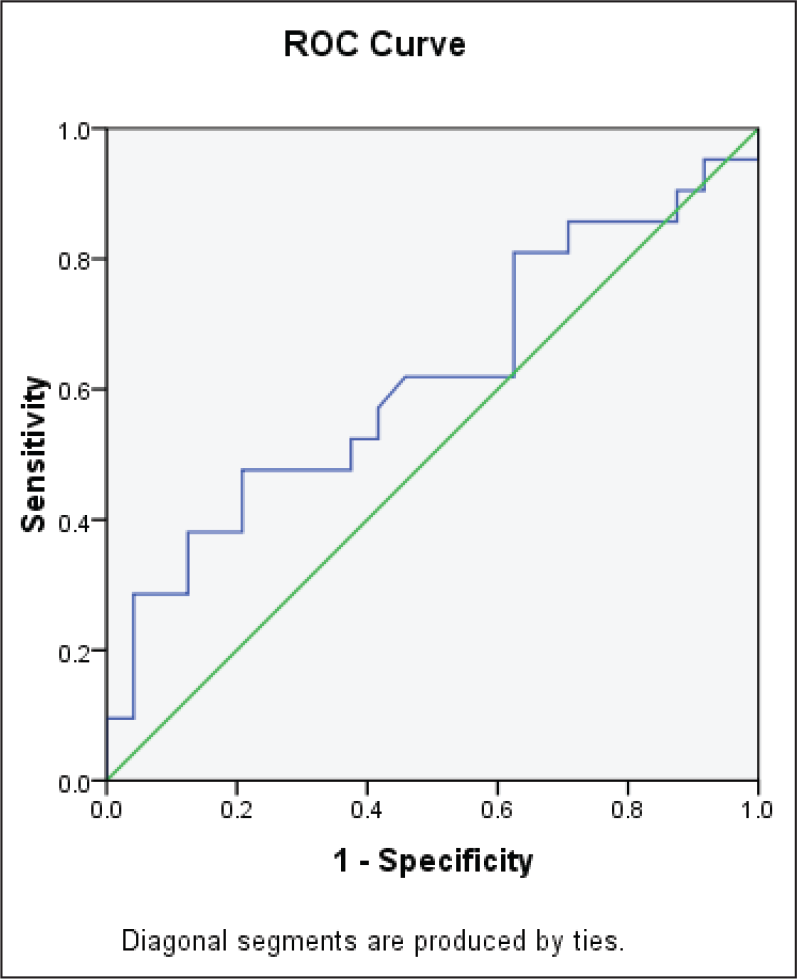
ROC curve analysis revealed IL-17 can predict the progression of schizophrenia at cutoff level of 6.95, specificity—54%, sensitivity—52% (Figure 1). At cutoff level of 7.59 µg/L, we found that IL-10 can predict the progression of schizophrenia with 57% sensitivity and 58% specificity (Figure 2).
ROC Curve Analysis of IL-17 Between Two Groups of Schizophrenia (Area Under the Curve [AUC]—0.625; Cutoff 6.95, Specificity—54%, Sensitivity—52%)
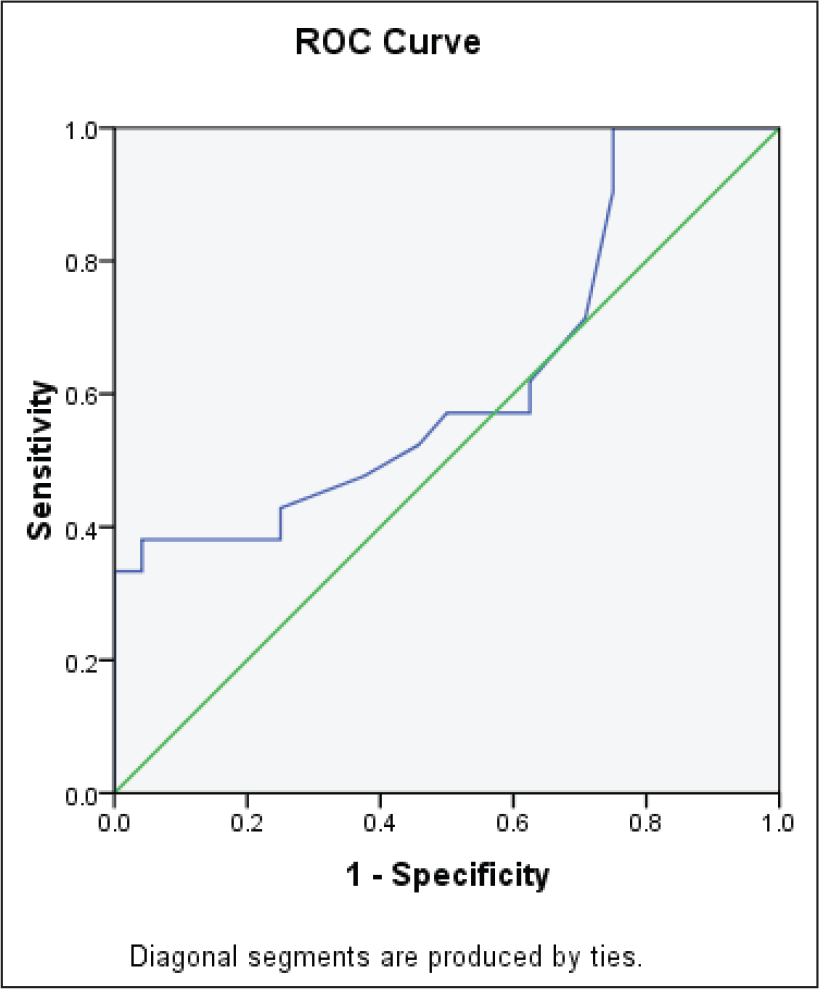
ROC Curve Analysis of IL-10 Between Two Groups of Schizophrenia (Area Under the Curve [AUC]—0.616; Cutoff 7.59, Specificity—58%, Sensitivity—57%)
Discussion
Dysfunction of immune system is considered to increase the progression of schizophrenia. Schizophrenia is linked with chronic low-grade inflammation, and several investigators have demonstrated aberrant cytokine levels in these patients. 15 The present study is the first study to investigate IL-17 and IL-10 levels and its association with progression of schizophrenia in Indian population.
Interleukin 17A is a pro-inflammatory cytokine, produced by T helper 17 cells (lympocyte). The reports about IL-17 levels are inconsistent with investigators demonstrating either elevated or reduced values in schizophrenia.6, 7 The effect of antipsychotics on IL-17 levels has been investigated by earlier studies. Ding et al have reported decreased IL-17 levels, and Himmerich et al have demonstrated elevated IL-17 levels after treatment with antipsychotics in patients with schizophrenia.16, 17 In the present study, there was a significant association of IL-17 with positive score (
Several evidences have supported the involvement of IL-10 in schizophrenia. Earlier researchers have shown reduction in blood IL-10 levels in schizophrenia patients with relapse of symptoms. 20 Subjects with lower IL-10 production genotypes were reported to be at increased risk of developing schizophrenia suggesting that low anti-inflammatory cytokines increase inflammation, which in turn increases the risk of schizophrenia. 21 In the present study, IL-10 was not associated with PANSS score significantly. In contrast, a previous study has documented an association of IL-10 with symptoms of schizophrenia. 22 Among different schizophrenia subgroups, we observed that IL-10 levels were more in patients with PANSS score more than 85 compared to those with score of 71–85. At cutoff level of 7.59 µg/L, we found that IL-10 can predict the progression of schizophrenia with 57% sensitivity and 58% specificity.
The main limitation of this study was noninclusion of control group due to financial and ethical constraints. Also, we did not analyze other proinflammatory cytokines due to financial constraints. ELISA was performed on the stored sample as it can be done only when adequate samples are collected, and inadequate technical resources do not allow fresh samples to be analyzed.
Conclusion
IL-17 and IL-10 are associated with disease severity in schizophrenia, but they cannot be used as predictive biomarkers of disease progression in schizophrenia. Future research works are needed to investigate the central nervous system source and mechanism of IL-17 and IL-10 release specifically during schizophrenia. Further studies are needed to evaluate the effect of anti-inflammatory agents on IL-17 levels and progression of schizophrenia.
Footnotes
Acknowledgments
This work was supported by an intramural grant from JIPMER, Puducherry to the corresponding author. Technical assistance of Mrs Durgadevi, laboratory technician, is greatly appreciated.
Author Contributions
RC: Data acquisition and analysis
HN: Concept and design of the study, statistical analysis, manuscript preparation
SK: Design of the study, data acquisition, manuscript editing and review
NDN: Analysis, manuscript editing and review
Ethical Statement
The study protocol was approved by the JIPMER ethics committee and informed consent was obtained from all the subjects and or their wards.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Institute (JIPMER) intramural fund.
