Abstract
The study is an attempt to find out vital areas related to doctors’ attitude towards generic medicines limiting its mass use. Attitude of medical practitioners, one factor amongst several, was chosen to evaluate doctors’ behaviour towards generic medicines. Most of the countries in the world, rich or poor, are taking more interest in generic medicines due to rising healthcare costs. In India, out of pocket expenses towards healthcare costs are one of the highest in the world besides affordability issue due to its demographics. Generic medicines offer as an alternative to expensive medicines. Government is promoting use of generic medicines; doctors are being advised to write prescription in generic names; however, there are several challenges in its mass use. The study is of national importance as it addresses the issue of low generic prescriptions despite unaffordable access to expensive branded medicines. A questionnaire constructed descriptive, cross-sectional study was conducted in North India in 2020 amongst 228 medical practitioners at primary, secondary and tertiary healthcare centres. Spearman’s rank correlation computed to assess the association between attitude and prescription of generic medicines was found to be positively correlated between the two variables indicating a significant moderate association between them.
Attitude of doctors towards generic medicines has been found to be playing a significant role in influencing doctors in prescribing generic medicines which explains limited use of generic drugs.
Keywords
Introduction
Medicines are available under a brand name or a generic name (chemical name of a drug). Innovation (newly discovered molecule through research) by an inventor is protected as a patent (legal protection) under intellectual property rights. A patent holder has the exclusive right to manufacture, market and eventually profit from the drug which provides an opportunity to the innovator to recoup its investment in research and development in discovery of a novel drug with a market free of price controls and generate free cash flows to support future endeavour in research. Generic drugs (copycats) are introduced without the brand names on expiry of patent of a drug.
The commonly understood terms ‘generic drug’ or ‘generic medicine’ mean a pharmaceutical product which does not require an authorisation from an innovator company whose innovation is covered under patent, to manufacture and market after the expiry of the patent. As a prescription or dispensation practice, generic medicine is generally intended to be interchangeable with an original or branded drug (FDA, 2018; WHO, 2021). The original drug and its generic are alike, meant to do the same thing but have huge price difference. Generic manufacturers are able to sell medicines at low prices as they do not have to repeat expensive clinical trials conducted by the originator.
Several brands may be available as substitute to each other; however, there is only one generic name for each medication. The brand name is usually the largest writing on the packet. Augmentin, for instance, is the brand name for the generic medication amoxicillin plus clavulanic acid which is the original research molecule of GSK; however, besides Augmentin there are several other brands known as branded generics available in the Indian market with the same medication such as Bactoclav (Micro Labs), Novaclav (CIPLA) and others. Also available at Jan Aushadhi stores (Indian government supported initiative) is a pure generic of amoxicillin plus clavulanic acid (without a brand name). The strength, dosage, intended use, route of administration, effects, side-effects, safety and risks of generics/branded generics are the same as the innovator product.
Indian pharmaceutical market is dominated by branded generics, medication in generic name sold under different brand names. Mostly, the branded generic medicines are promoted to doctors for their support in getting prescriptions and are priced higher than the generics (without any brand name) sold through Jan Aushadhi (generic drug stores). However, some of the branded generic medicines are not promoted to doctors but offered to chemists (or pharmacists) at huge discounts making it attractive for them to push or substitute as generics. The huge discount offered on branded generics has also been found attractive in dispensation at in-house chemists of privately managed clinics and secondary care hospitals.
Doctors play an important role in prescribing medicines for treatment of medical illness of patients. Prescribing branded medicines or by generic names is the decision of a doctor. Prescribing of generic medicines is being promoted in many countries for affordable access to medicines by patients.
One major challenge is acceptance of quality of generics by doctors, a proportion of whom are hesitant to prescribe medicines in generic names as they are not sure of effectiveness of generics; besides, safety of generic drugs and their availability are impediment to practitioners’ prescription of generics (Colgan et al., 2015; Dhale et al., 2020; Kamejaliya et al., 2017; Roy & Rana, 2018).
Bioequivalence study establishes performance of a generic drug by comparing absorption and its rate in the blood stream at the site of drug action of an active pharmaceutical ingredient of generics with the original branded medicines. Regulations in generic product registration in India require bioequivalence studies to be performed on drugs with low solubility. However, the eligibility for bio-waivers include drugs that are highly soluble in water which are considered to be likely easily absorbed in the body, hence may not require bioequivalence study. There are drugs which are exempted for bioequivalence studies. In the absence of stringent quality enforceable measures like that in USA, doctors in India rely on reputation of a company like CIPLA, Dr Reddy’s Lab, Sun Pharma and others who over the years have demonstrated their commitment to quality (Soans, 2022).
Moreover, marketing promotional practices being followed by pharma companies with the engagement of medical representatives who provide product information and seek prescription support from doctors are leading to branded prescription practices (Aivalli et al., 2018).
The directive towards a legal framework to make doctors prescribe generic drugs followed by advisories issued by Medical Council of India (MCI) asking medical practitioners to prescribe generic drugs as much as possible has failed to gather full support of medical practitioners mostly in the private sector. Doctors so far seem unwilling to prescribe medicines in generic name. Therefore, it is important to acknowledge the unwillingness in doctors to prescribe generic drugs by understanding the knowledge, attitude and prescription behaviour amongst them. This study primarily focusses on understanding the attitude of medical practitioners towards generic medicines.
Review of Literature
Affordable access to treatment is the main reason to make generic medicines popular by the government. For a long time, generic medicines have been recognised as contributing to reduction in healthcare expenses. Multiple studies have established that savings in the range of 9% to 89% can be realised in developing countries by way of substituting originators’ brand by low-priced generic medicines (Cameron et al., 2012).
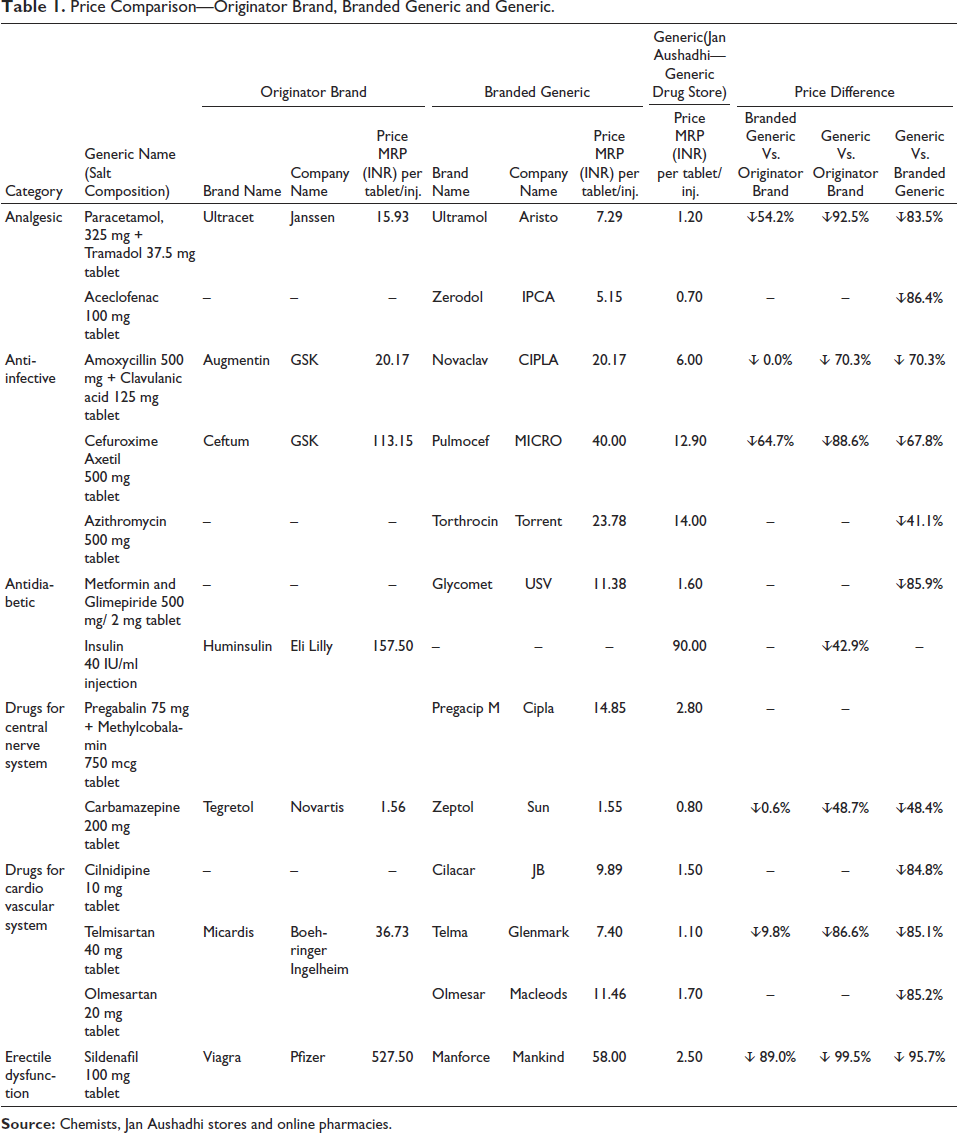
Price comparison of few leading brands and their generic alternative available at Jan Aushadhi stores for which the price is fixed by the department of Government of India is given in Table 1.
Price Comparison—Originator Brand, Branded Generic and Generic.
WHO health expenditures data disclose that out-of-pocket expenditure (OOPE) as a proportion of current health expenditure was 65% in India against the world average of 20% in 2016. Medicines account for single largest expenditure, share of which in OOPE has gone down to 43% in 2015–2016 from 51% in 2013–2014. Hence, cost of medicines is an important area to dwell on (Singh et al., 2022).
In 2020, 65.07% of India’s population lived in the rural areas (Index Mundi, 2022). Access to healthcare and affordability in rural areas has been a challenge where proportion of population below the poverty line is higher than the urban areas. According to a WHO report, a majority of Indian population (nearly 68%) has either inadequate availability or no access to essential medicines.
Negative perceptions about generic medicines compared with their branded equivalents are being held by a majority of doctors, pharmacists and lay people who perceive generic medicines low in quality, hence less safe and less effective. Probably such attitudes serve as barriers to the extensive use of generic drugs. A review of observational studies based on 52 articles on perception of generic medicines amongst population, physicians and pharmacists was conducted (Colgan et al., 2015). The publication included data from 27 countries from 1987 to 2015. On effectiveness, a majority of general population (35.59%) believed generic drugs were not as effective as branded equivalents compared to doctors (28.68%) and pharmacists (23.60%). On quality, minimum 25% from each group (pharmacist 33.39%, physicians 28.04%, general population 25.11%) believe generic medicines are not as par on quality compared to branded medicines. On side effects of generics compared to branded equivalents, 24.43% doctors, 17.56% pharmacists and 18.76% lay people believed generics caused more side effects. On safety, a higher number of doctors (28.54%), pharmacists (21.44%) and general population (17.97%) perceived generic medicines less safe compared with branded medicines. A higher number of lay people (34.03%) felt negatively about substitution of branded drugs with generics, compared to doctors (24.11%) and pharmacists (11.04%). It is likely these attitudes amongst medical practitioners towards generic medicines act as barriers to wider use of generics.
Concerns amongst resident doctors about effectiveness, safety and availability of generic medicines are the key for choosing branded medicines. In a study (Kamejaliya et al., 2017) conducted at a tertiary care teaching hospital in West India, it was found that the majority of the respondents held the opinion that generic medicines are low in prices because of low-grade quality (71.9%), have unsure efficacy in serious diseases (44.6%), can be prescribed in all diseases (61.9%) and prescription of generic medicines should be mandatory (37%). The doctors preferred brand over generic medicine due to reasons such as concern about efficacy (100%), concern about safety (61.57%), poor availability of generic medicines (57.85%), inadequate availability of information (33.06%). Majority of the respondents did not agree to substitution of brand medicine with a generic one by pharmacist due to doubts about quality, effectiveness and safety of generic medicines and hence, may not desire substitution of former.
Patients’, doctors’ and pharmacists’ perceptions mostly favoured branded medicines despite comparable quality of generic and branded equivalents found in testing. Negative perceptions on quality of generic drugs and doctors’ oriented promotional activities by pharmaceutical companies for branded drugs are leading to choosing expensive branded drugs in the private sector (Aivalli et al., 2018).
In an article ‘Prescribing generics: All in a name’ (Roy & Rana, 2018), it was highlighted that the lack of confidence in physicians and patients on the quality of generics is a major reason for prescribing branded medicines. Pharmaceutical companies engaged in aggressive promotion of branded generic medicines further augments the problem. A major concern regarding safety and effectiveness of generic drugs is due to non-adherence to Good Manufacturing Practices by pharma companies.
In a study that examined the opinion of medical practitioners and pharmacists about medicines in generic and brand name (Dhale et al., 2020), it was found that 59% of the respondents perceived the effectiveness of generic drugs at par with original drugs; however, 23% believed that generics were ineffective based on their experienced difference in quality between the generics and original drugs. A gap has been identified between the knowledge and generic perspective on new drugs. Less than two-third of respondents (64%) agreed with the safety of generics as with innovators’ medicine. Less than half (46%) agreed that generics were inferior. More than two-third of the respondents (70%) felt that for generics to be accepted, more confidence in patients should be built. A total of 61% of medical practitioners and pharmacists, while prescribing drugs take into account the socio-economic position of patients. About a quarter of physicians and pharmacists think that generic medicine causes a higher side effect compared to the innovator’s drug. Equal number of physicians and pharmacists (47%) have a contra view of the effectiveness of generics compared to branded drugs. These beliefs can represent an important obstacle to increased use of genetics and can lead to higher costs in health care. The efficacy, safety and quality of medicines were of paramount importance to doctors and pharmacists when prescribing/dispensing drugs.
The issue with medicines in India is not about pricing of branded medicines which are expensive compared with generics but lack of assurance of quality in medicines. Doctors trust branded generic medicines from companies such as Cipla, Dr Reddy’s Lab or Sun Pharma because of the quality assurance from well-known companies. Medical representatives numbering close to a million have contributed significantly in building trust of doctors in the company’s brands by widely promoting the branded medicines. Generics manufactured by unknown companies cannot be simply trusted by doctors. If a medical practitioner prescribes medicine in generic name, it may get dispensed by chemist with another branded generic or generic of suspicious quality (Soans, 2022).
In a study conducted to determine the association between the quality of generic medicine and brand equity of branded drugs and to evaluate doctors’ opinion in determining generic drugs for selected medical conditions in India (Sanyal & Datta, 2011), the results showed that the brand equity is affected by the judged quality of branded drugs through the mediating variables, internal (product information) and external (price, product name, country of origin, retailer reputation, advertising level). The results also showed that doctors experience with quality leads to quality expectations, with the exception of small differences in drug quality in five common but serious diseases in India.
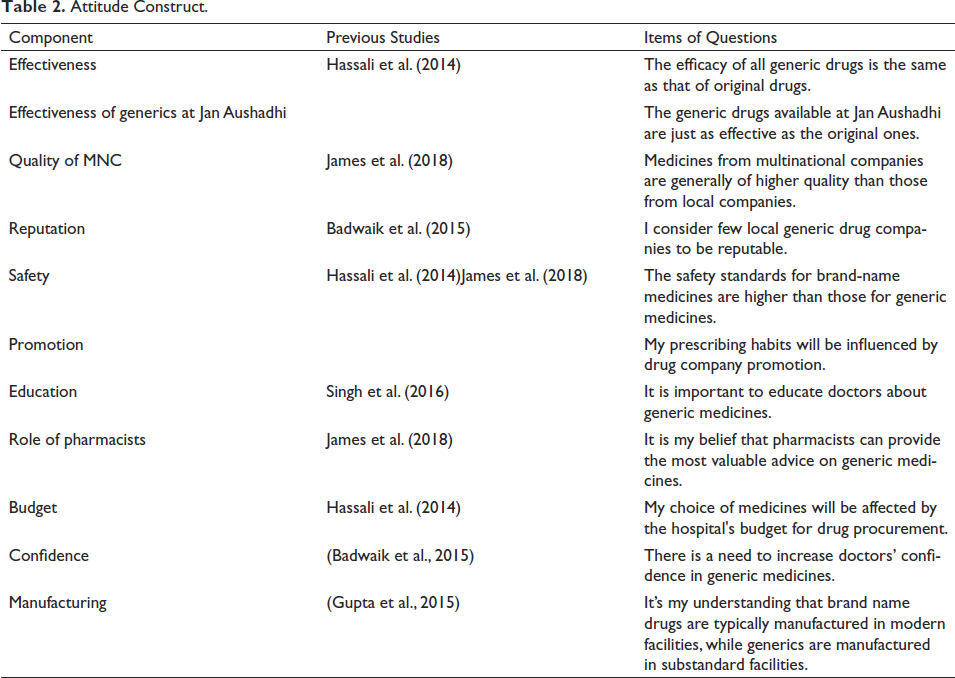
Based on the literature review as illustrated previously, the questions for the study have been identified which are given in Table 2.
Attitude Construct.
Objective and Methodology
The objective of the article is to discover association between attitude and prescription of generic medicines by doctors with an aim to bring forth suggestions including marketing aspects of generic medicines that the pharmaceutical companies need to take into consideration that may lead to increase in prescribing generic medicines.
The questionnaire-based descriptive observational study was conducted at Dehradun district spanning over a year in 2020 among 228 doctors practicing in primary, secondary and tertiary healthcare centres.
Research Design
The basic research design process used in the study is descriptive. Further, the study is cross- sectional in nature so as to describe the statistical significance in association between the variables.
Instrument Development
The steps followed in the development process of the instrument are as follows: Identification of questions from various studies Refinement and paraphrasing of items One-on-one interviews for the improvement of questionnaire Pilot scale testing for further improvement of questionnaire Finalisation of questionnaire
The questionnaire constructed for the study comprised of 11 items related to attitude in Likert-type scale.
Sampling
The membership list of doctors of Indian Medical Association Uttarakhand located within the talukas of Dehradun district formed the population of the study which comprised 671 doctors. Systematic random technique was used to determine the sample.
Sample Size
Assuming the highest variability of 50% and designing for a ±5% sample error at 95% level of confidence, the number of respondents estimated is 179 (Burns & Bush, 2003).
Calculations for sample size (n) was determined as follows:
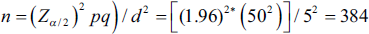
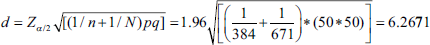
where
N = population size,
p = 50% unknown,
q = 50% (100 – p), d = 5%,
α= 5% level of significance.
Minimum sample size

Type of Survey
The questionnaire designed for the study was self-administered amongst medical practitioners with face-to-face interaction. Due to restrictions imposed during the COVID-19 pandemic, telephonic interviews, email and Google-form were used to collect responses from the medical practitioners.
In all, 228 doctors responded to the survey instrument.
The sample data were compiled in excel and analysed using SPSS 25 for analysis. P values of ≤ .05 < .05 were considered to indicate statistical significance.
Analysis and Interpretations
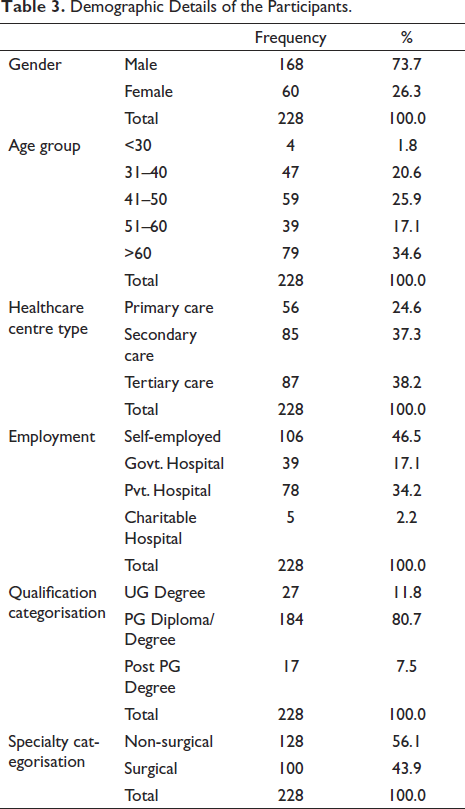
Table 3 summarises the demographic of the participants.
Demographic Details of the Participants.
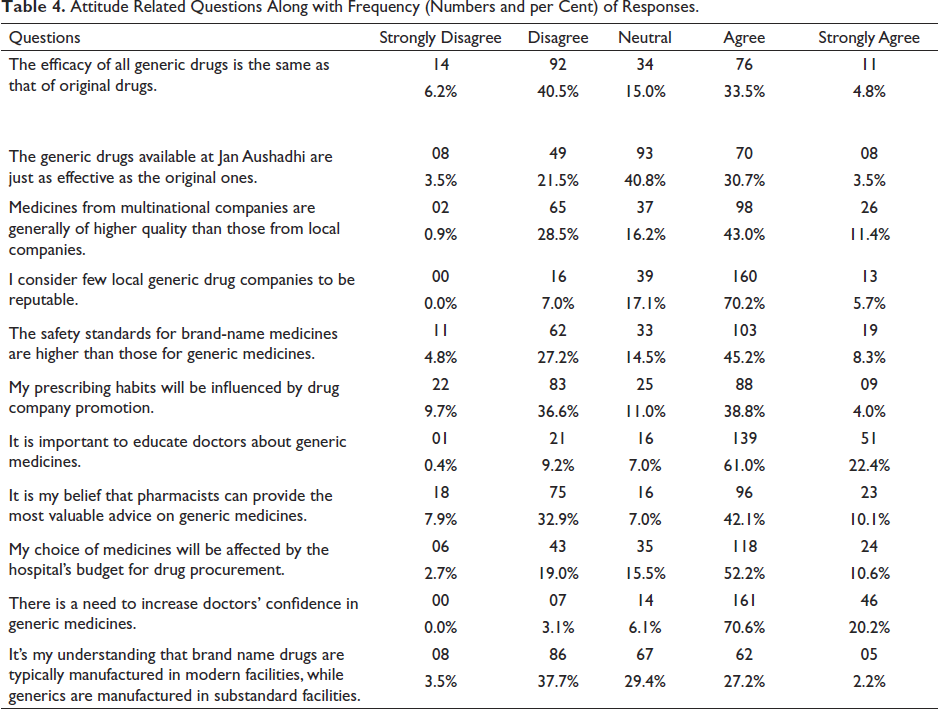
Frequency of responses of the respondents against the attitude-related questions is shown in Table 4 and graphic representation is shown in Figure 1.
Attitude Related Questions Along with Frequency (Numbers and per Cent) of Responses.
Graphic Representation of Attitude Related Responses.
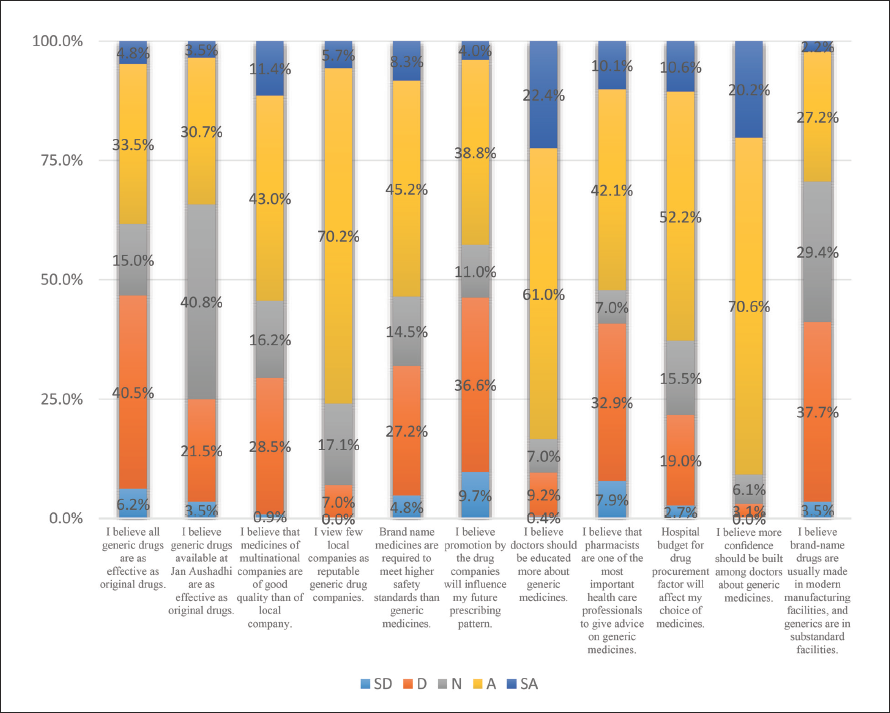
It was found that less than 50% of respondents (38.3%) believe that generic medicines work like the innovator drugs, but when it comes to generic performance in Jan Aushadhi’s programme, 34.2% of doctors believe generic medicines are as effective as original drugs whereas majority of the doctors, 40.8% (the highest neutral response amongst all the items), have neither a positive response nor a negative response. A total of 54.4% of doctors believe that medicines of multinational companies are superior in quality over local companies. Majority of the doctors (75.9%) believe that not all domestic companies have a good reputation. More than 50% of physicians, 53.5%, believe that branded drugs are needed to meet the highest levels of safety over generic medicines. A total of 42.8% of physicians believe that drug companies engaged in promotion influence prescription pattern of medical practitioners while 46.3% of physicians have the opposite belief. Overwhelmingly, 83.4% of respondents (second positive response to all items) believe that physicians should be educated more on generic drugs. Most doctors, 52.2%, believe that pharmacists are among the most important health professionals to give advice on generic drugs. A total of 62.8% of doctors say the hospital budget influences their choice of medication. Overwhelmingly, 90.8% of physicians (the best response of all) believe that more confidence should be built among physicians about generics. About one-third of physicians, 29.4%, believe that brand-name drugs are commonly manufactured in modern manufacturing facilities and generics in below the required standards and other equal number of respondents have a neutral view.
The responses of doctors in prescribing generic drugs are shown in Table 5.
Responses (Frequency and per Cent) of Doctors in Prescribing Generic Drugs.
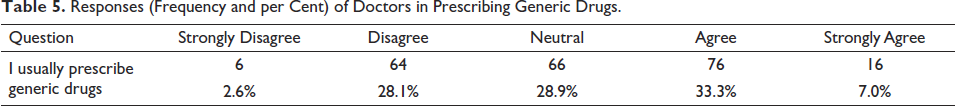

In order to determine the statistical significance between the attitude (generic medicine) and the doctor’s prescription, the research question was framed, ‘Does attitude towards generic medicines play a significant role in influencing medical practitioners in recommending generic medicines?’ Spearman’s rank correlation coefficient was computed to assess the statistical significance between attitude and prescription of generic medicines.
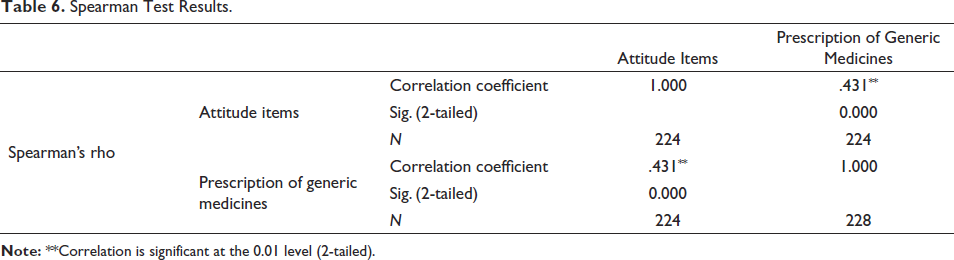
A positive correlation was found between the two variables, r (222) = 0.43, p < .001 indicating a significant moderate association between attitude towards generic medicines in doctors and prescription of generic medicines. Thus, the finding supports alternate hypothesis and it may be concluded that negative attitude towards generic medicines plays a significant role in influencing doctors in prescribing less of generic medicines. Spearman test results are summarised in Table 6.
Spearman Test Results.
According to the analysis of the responses, it can be concluded that doctors have attitude towards generic drugs. However, there is no difference in attitude towards generic medicines amongst doctors who provide primary, secondary and tertiary healthcare as results of Kruskal–Wallis test did not show statistical significant difference among doctors at different healthcare centres (primary, secondary and tertiary), H (222) = 2.161, p = .339. No statistical significant difference is found in attitude towards generic medicines in male and female doctors H (222) = 0.007, p = .933 and in different age groups H (225) = 2.267, p = .687. However, statistical significant difference is found in different employment status (self-employed, govt. hospital, private hospital) of doctors H (225) = 16.462, p = .001. No difference in attitude is seen in doctors with different levels of education (UG degree, PG diploma/degree, post-PG degree), H (225) = 3.955, p = 0.138 and doctors having nonsurgical and surgical practice H (225) = 1.596, p = .206.
According to the analysis of the responses, a good percentage of respondents were found to be having attitude towards generic medicines. The overall findings were in contrast to a study (Gupta et al., 2018) wherein majority of the doctors had shown a positive attitude. However, similarity was seen in few areas such as manufacturing facility wherein majority of doctors in both the studies did not believe that generics are made in below the required standard facility as compared to brands. Another area of similarity was in education, where the majority of doctors felt that doctors should be more educated about generic medicines
Negative perception about generic medicines are being held by a majority of doctors, pharmacists and lay people who perceive generic medicines are low in quality, hence less safe and less effective. Probably such attitudes serve as obstacles to the extensive use of generic medicines. A review of observational studies (Colgan et al., 2015) based on 52 articles on perceptions of generic medicines amongst population, physicians and pharmacists was conducted. The publication included data from 27 countries from 1987 to 2015. On effectiveness, a majority of general population, 35.6%, believed generic medicines did not work as well as their branded equivalents compared to 28.7% of doctors and 23.6% of pharmacists. On quality, minimum 25% from each group (pharmacist 33.4%, physicians 28.0%, general population 25.1%) believe branded medicines are of higher quality than generic medicines. On safety, a greater proportion of doctors (28.5%), pharmacists (25.4%) and general population (18.0%) perceived generic medicines less safe compared with branded medicines. However, in the existing study, 46.7% of doctors believe generics are not effective as branded medicines, 29.4% of doctors believe quality of generics is inferior to medicines of multinational companies, 53.4% of doctors believe generics are low in safety standard compared with brands.
Choosing reputable medicines is driven by apprehensions about efficacy, safety and availability of generic medicines amongst resident doctors. In a study (Kamejaliya et al., 2017), conducted at a tertiary care teaching hospital in Gujarat, it was found that the doctors prescribed generic medicines but preferred brands over generic medicines due to reasons such as concerns about efficacy (100%), safety (61.5%), availability of generic medicines (57.8%). Majority of respondents did not agree to substitution of brand medicine with a generic one by pharmacist due to doubts about quality, effectiveness and safety of generic medicines and hence, may not desire substitution of former. In comparison to the above study, only 46.7% of doctors believe that generics do not work well as brands and 14.5% of doctors have given a neutral response to safety of generics compared to brands in the present study.
The findings of the present study draw similarity with another study (Roy & Rana, 2018). In their article ‘Prescribing generics: All in a name’, it was highlighted the lack of confidence in the quality of generics amongst physicians and patients is the prime reason for doctors not prescribing generics. The problem is further augmented by pharmaceutical companies who aggressively promote medicines. A major concern regarding safety and effectiveness of generic drugs is due to the lack of Good Manufacturing Practices by pharmaceutical companies.
Physicians and pharmacists, along with activities aimed at educating patients, have an important role to play in the promotion and recommendation of generic medicines more often. Research suggests that the majority of patients’ decision to accept generic medicines is based on learning about generic medicines from healthcare professionals (Babar et al., 2010; Nabil et al., 2008). The findings of present study show overwhelming response; 83.4% of respondents believe that doctors should be educated more about generic drugs and, overwhelmingly, 90.8% of doctors believe that more confidence should be built among doctors about generic drugs. Doctors can play a constructive role in acceptance of generics amongst patients. Therefore, educating doctors about generic medicines and building their confidence are the two major areas that may be addressed.
Conclusion
In a study conducted, it has been found that attitude towards generic medicines by medical practitioners has an influence on prescription of generic medicines. Low prescription of generic medicines can be explained by negative attitude of doctors towards generic medicines. Further research is needed to explore different interventions amongst doctors to nurture a positive attitude and patronage for generic medicines. Building a trust in generics of unknown companies in absence of promotion by medical representatives is an area that needs to be explored from marketing perspective of generics.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
