Abstract
Objective
Cervical cancer represents a major health problem in Romania. A national population-based cervical cancer screening programme was launched in 2012. The aims of the study were to assess the participation rate and to estimate the prevalence of epithelial cell abnormalities in the first four years of the programme in North Eastern Romania.
Methods
The participation rate, representing the proportion of eligible women screened in the programme, was evaluated for 2012–2016. The prevalence of cytological abnormalities was estimated by age group and calendar year.
Results
Of 107,968 Pap smears taken, 312 were unsatisfactory (0.3%). The number of smears decreased by year. The participation rate over the four years was 16.9%. Of the 107,656 satisfactory smears, 6.5% were positive for squamous and/or glandular lesion, among which 0.5% contained high-grade squamous intraepithelial or worse lesions.
Conclusion
The participation rate in the first four years of the programme was low. The effectiveness of the screening programme should be improved by attendance monitoring of the target population, and follow-up of screen-positive women. Measures should be taken to raise coverage and assure quality at all steps of the screening chain. The data collected should include all screening tests from both opportunistic and organized settings.
Introduction
Cervical cancer continues to represent a major health problem as one of the leading causes of cancer mortality among women. It can be effectively controlled by primary prevention (prophylactic human papillomavirus (HPV) vaccination) and secondary prevention (cervical screening). Romania has the highest incidence of and mortality from cervical cancer in Europe. 1 The 2004 mortality rate from cervical cancer in Romania was 11.1. 2 It has steadily been increasing during the last two decades, and cervical cancer incidence rates have also risen from 15.7 cases per 100,000 in 1982 to 28.7 per 100,000 in 2012. 3 Most cases are diagnosed in the advanced stages of the disease because of the lack of organized screening programmes. Based on these data, cervical cancer and its prevention are critical issues for public health in Romania.
Several primary and secondary prevention initiatives were undertaken to improve this situation. Two attempts to introduce a vaccination programme, in 2008 and 2009, were both stopped because the participation rate was extremely low.4,5 In 2012, a national population-based cervical cancer screening programme was initiated, targeting women aged 25–64, both insured in the National Health Fund or uninsured. There are no personalized invitations (letters, telephone calls, etc.) sent to the patients. Advice from general practitioners and gynaecologists, along with media advertising, made the information about this programme available to the population. At a general practitioner visit, information and instructions were given to women aged 25–64. Data were entered and further completed by the gynaecologist and the pathologist on a specific form. One single conventional Pap smear per woman is performed free of charge at five-year intervals. The general practitioner or gynaecologist collects the Pap smear sample, and a consultant pathologist or cytologist evaluates the slide.
This study reports the first results on the participation of the target population, as well as the proportion of cytological abnormalities observed in the first four years of the programme in North Eastern Romania.
Methods
All data were extracted from the archives of the Regional Management Department. The participation rate was defined as the proportion of eligible women screened within the programme per year over four years (2012–2016). The results of Pap smears were reported according to the Bethesda System for Reporting Cervical Cytology. Unsatisfactory Pap smears were excluded from the evaluation of observed prevalence of abnormalities.
Descriptive statistics were used, and numbers and percentages were tabulated. Variation in observed proportions was assessed by age group and calendar year.
Results
In the North Eastern part of Romania in the four-year period, 107,968 cervical Pap smears were taken, representing about 16.9% of targeted women. We compared the results per year by grouping the data into 12 month periods, starting with September 2012 when the national programme commenced. There were 54,235 (50.2%) Pap tests performed in the period September 2012–August 2013, and 20,877, 20,277 and 12,579 (19.3%, 18.8% and 11.6%) cases in the following years, respectively. A continuous decrease in the number of patients screened per 12-month period was observed (Figure 1). The distribution of the cytological findings (Bethesda category) per year is shown in Table 1; 312 women had unsatisfactory specimens. Of the 107,656 slides that were adequate for interpretation, 100,684 (93.5%) were negative for intraepithelial lesions, and 6.972 (6.5%) presented epithelial cell abnormalities; 6073 Pap smears (5.6%) contained squamous abnormalities (atypical squamous cells of undetermined significance (ASCUS) or worse) and 899 cases (0.8%) had glandular lesions (atypical glandular cells (AGC) or adenocarcinoma).
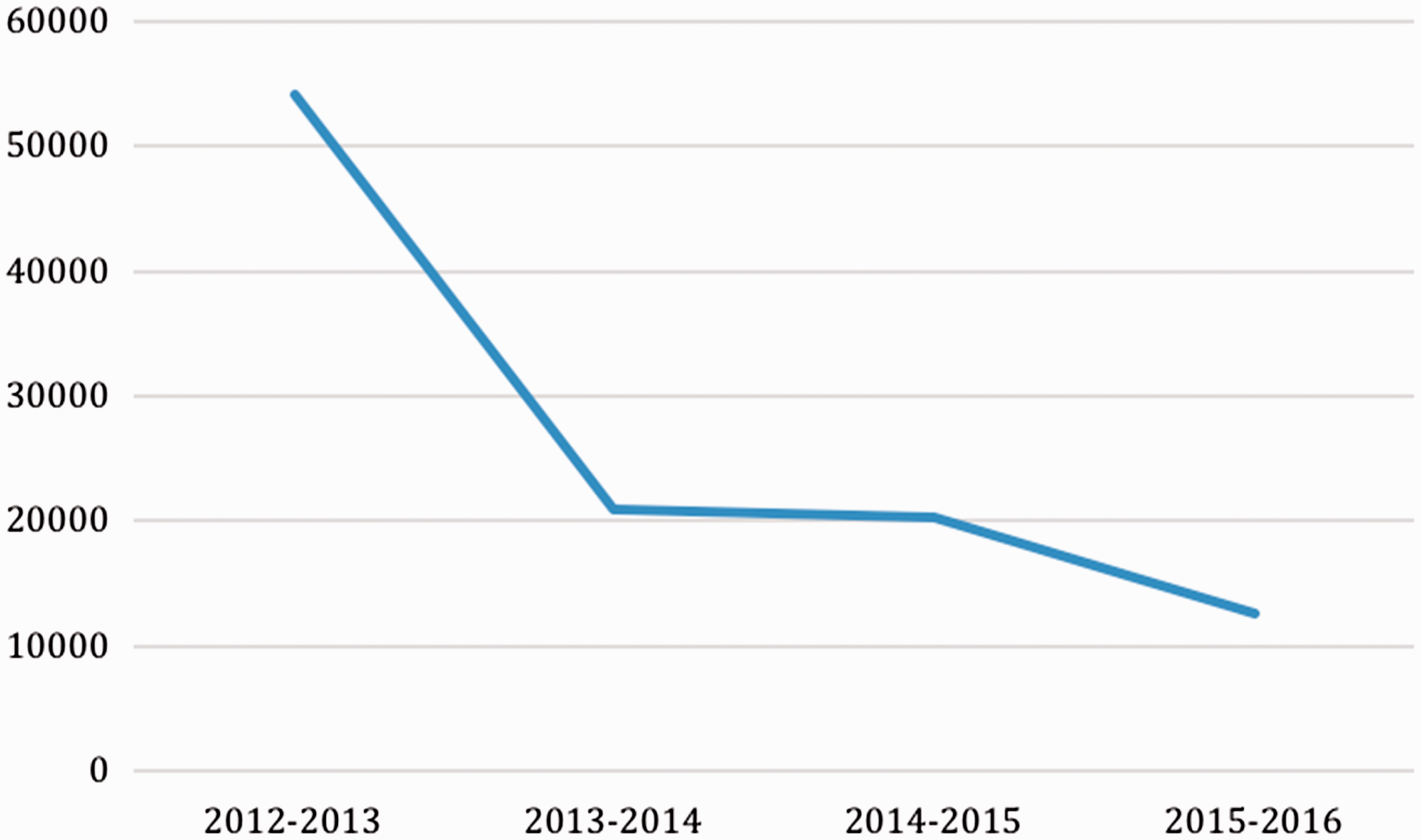
The number of cases analysed per 12 months intervals.
Distribution of smear test results for each year of the study.
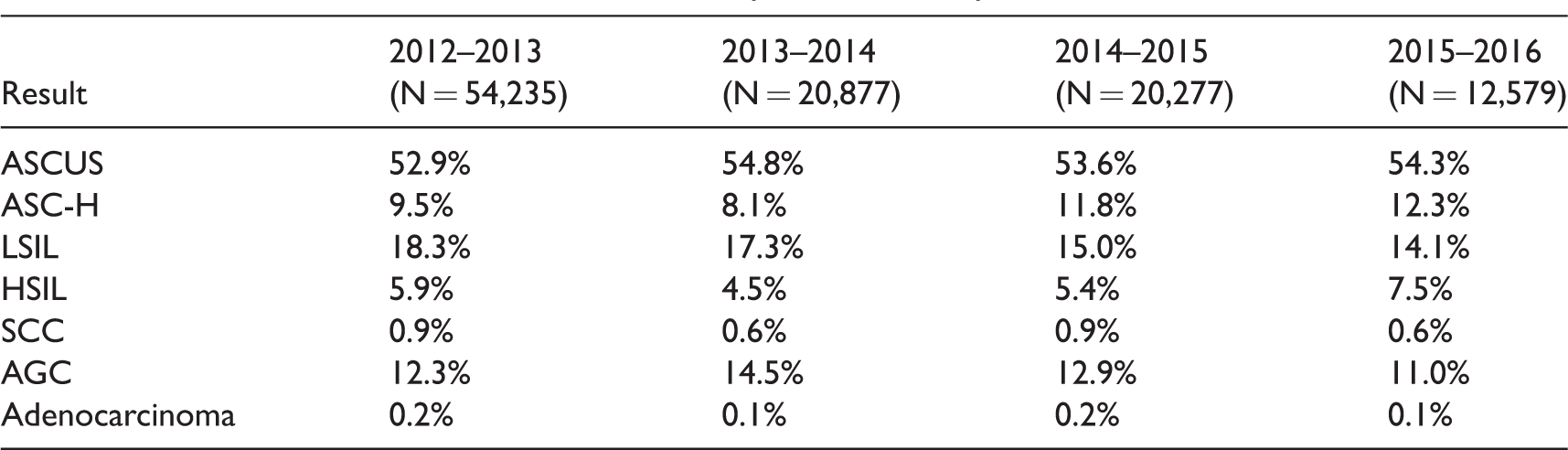
N: number of screened eligible women; ASCUS: atypical squamous cells of undetermined significance; ASC-H: atypical squamous cells, cannot exclude HSIL; LSIL: low-grade squamous intraepithelial lesion; HSIL: high-grade squamous intraepithelial lesion; SCC: squamous cell carcinoma; AGC: atypical glandular cells.
The distribution of cytological anomalies was as follows: ASCUS 3.5%, atypical squamous cells, cannot exclude HSIL (ASC-H) 0.6%, low-grade squamous intraepithelial lesion (LSIL) 1.1%, high-grade squamous intraepithelial lesion (HSIL) 0.4%, squamous cell carcinoma (SCC) 0.05%, AGC 0.8%, and adenocarcinoma 0.01%. There were 60 cases of SCC and 12 cases of adenocarcinoma diagnosed. The variation in the observed prevalence of cytological abnormalities by age group is plotted in Figure 2. No age data were recorded during 2012, so the calculations took into account only the data from 2013 to 2016.
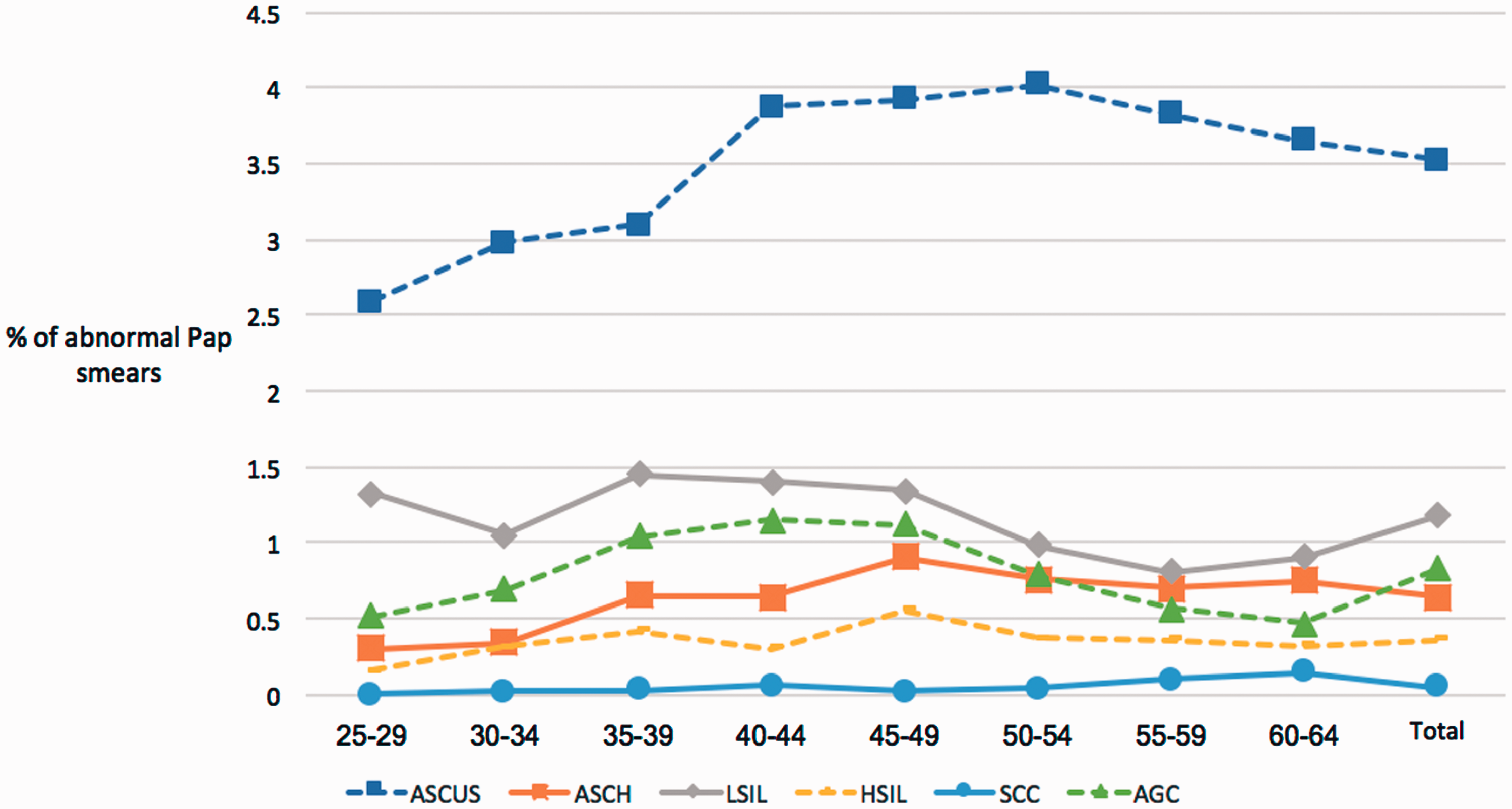
Prevalence of the different cell abnormalities based on age groups.
Discussion
In the first four years, approximately 17% of women aged 25–64 in the North Eastern region of Romania participated in the new cervical cancer screening programme. European Guidelines for Quality Assurance in Cervical Cancer Screening suggest that a well-organized screening programme should be accepted by the population and coverage and must be ensured at all levels. 6
The data concerning coverage of Pap smear are incomplete because during that time period opportunistic screening occurred, in addition to organized population-based screening. The opportunistic screening is practiced in Romania either at private gynaecological clinics or at some of the units that cooperate with the National Health Fund, and Pap smear tests are taken in these settings as part of a comprehensive gynaecological examination. This opportunistic screening, usually initiated by the woman herself or her gynaecologist, occurs even in countries with organized programmes. A study from Denmark, a country with a well-established screening programme, showed that one-fourth of the Pap smear tests in this country are conducted opportunistically. 7 The authors of this study consider that opportunistic testing might serve as an important supplement to the systematic screening programme, by including non-participating women who may otherwise be tested with a delay, or not tested at all. In contrast to Denmark, in Romania, all the results from the opportunistic screening are not reported and registered in the national database. For a better assessment of the situation, it is recommended that the results from both the organized and opportunistic screenings should be registered in future.
About 7% had cytological abnormalities and 0.5% had high-grade or worse lesions. The prevalence of ASCUS increased up to age 44 and remained stable in older women. The cases with SCC were more frequent in the age groups 35–39 and 60–64, which may be explained by the patterns of the HPV infection peaks described in the literature. The first peak in HPV infection is among the youngest age group (age: 15–19), and the second is among the age group 50–60. 8
A study published in 2014 investigated the prevalence of abnormal cells in Romania and presented the results of an opportunistic screening. The prevalence of cytological lesions in this study was 5.9% out of 50,436 smear tests analysed. Most of the abnormal results fell into the category of ASCUS (2.6%), while HSIL represented 0.9% of all smears. 9 The prevalence of epithelial cell abnormalities reported in our study is above the prevalence in the opportunistic screening reported in the abovementioned study, but the prevalence of HSIL or worse was lower in our study.
To compare the prevalence of abnormal Pap smears in Romania with that in other countries, a PubMed search was conducted. Based on the analysis of the studies in different developed or developing countries, the prevalence of cell abnormalities varies between 1.8 and 5.8%.10–14 The prevalence of cytological abnormalities observed in our study exceeds those reported from other developed or developing countries in the same decade. The high prevalence of cervical abnormalities (6.65%) in Romania underscores the need for a continuous national screening programme. The detection of cervical cytological anomalies depends on the background risk (determined by exposure to risk factor), the risk spectrum of the population attending screening and the experience of the cytologists and cytology technicians evaluating the smears. To assess the background risk, HPV prevalence estimates may provide more objective information.
In addition to the high prevalence of precursor cervical lesions, our study revealed that the utilization of the screening programme is low. Because of these two facts, several urgent measures should be taken to increase participation in the screening programme. To have an impact on cervical cancer incidence and mortality, efforts must be focused on increasing the awareness of women about cervical cancer and the prevention methods, through an intensive promotional campaign to encourage participation. At the same time, general practitioners should be more actively involved in the programme, as they play a key role in counselling the women. In addition, an HPV self-sampling strategy would be interesting to implement in Romania, taking into account that this could be a useful screening method for non-attenders. 15
A weakness of this study resides in the lack of data from opportunistic screening and the lack of follow-up findings. It will be necessary to conduct studies in the future to investigate the reason for low utilization of the screening, and how this can be improved.
Conclusion
Evaluation of the first four years of the screening programme reveals low participation among the eligible population and a high prevalence (6.6%) of cervical precursor lesions. These findings underscore the importance of the continued implementation of the national screening programme. Policy makers should take new measures to increase participation in this screening programme, and monitoring of the screening programme should include both opportunistic and organized settings.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
