Abstract
Objective
Screening participation is spread differently across populations, according to factors such as ethnicity or socioeconomic status. We here review the current evidence on effects of interventions to improve cancer screening participation, focussing in particular on effects in underserved populations.
Methods
We selected studies to review based on their characteristics: focussing on population screening programmes, showing a quantitative estimate of the effect of the intervention, and published since 1990. To determine eligibility for our purposes, we first reviewed titles, then abstracts, and finally the full paper. We started with a narrow search and expanded this until the search yielded eligible papers on title review which were less than 1% of the total. We classified the eligible studies by intervention type and by the cancer for which they screened, while looking to identify effects in any inequality dimension.
Results
The 68 papers included in our review reported on 71 intervention studies. Of the interventions, 58 had significant positive effects on increasing participation, with increase rates of the order of 2%–20% (in absolute terms).
Conclusions
Across different countries and health systems, a number of interventions were found more consistently to improve participation in cancer screening, including in underserved populations: pre-screening reminders, general practitioner endorsement, more personalized reminders for non-participants, and more acceptable screening tests in bowel and cervical screening.
Keywords
Introduction
To achieve their desired public health impact, population cancer screening services require high levels of participation. While it is agreed that decisions to participate in cancer screening should be free from undue pressure, and should be well-informed, it is also frequently observed that there are considerable inequalities in participation in cancer screening.1–3 In the United Kingdom (UK), screening participation rates are lower in areas of deprivation and among certain ethnic groups.3–5 There is a wide range of potential interventions to improve access to cancer screening services and, therefore, increase participation. Given the perceived need to address health inequalities, 6 one tactic would be to improve uptake of public health measures such as screening programmes in currently underserved populations. We review the evidence on effects of interventions to improve screening participation, with particular reference to effects on inequalities. To inform policy and practice, such a review should identify those measures most and least likely to be effective, including any findings with respect to inequalities, or effects of interventions in deprived or otherwise underserved populations.
Methods
We specified in advance that the studies of relevance to this review had to report on interventions aimed at participation in cancer screening services (not randomized trials of screening). The focus of interest was population screening programmes (as opposed to surveillance of specific genetic or other high-risk groups). To be eligible, a study had to report a quantitative estimate of the effect of the intervention on participation rates. We only included studies published since 1990. Studies which assessed the effect of personal invitation against no invitation were not included, as the NHS Cancer Screening Programmes in the UK would always send personal invitations in any case.
Results of successively broadening the search terms until newly identified papers potentially eligible on title review was less than 1% of the total papers found by the search.
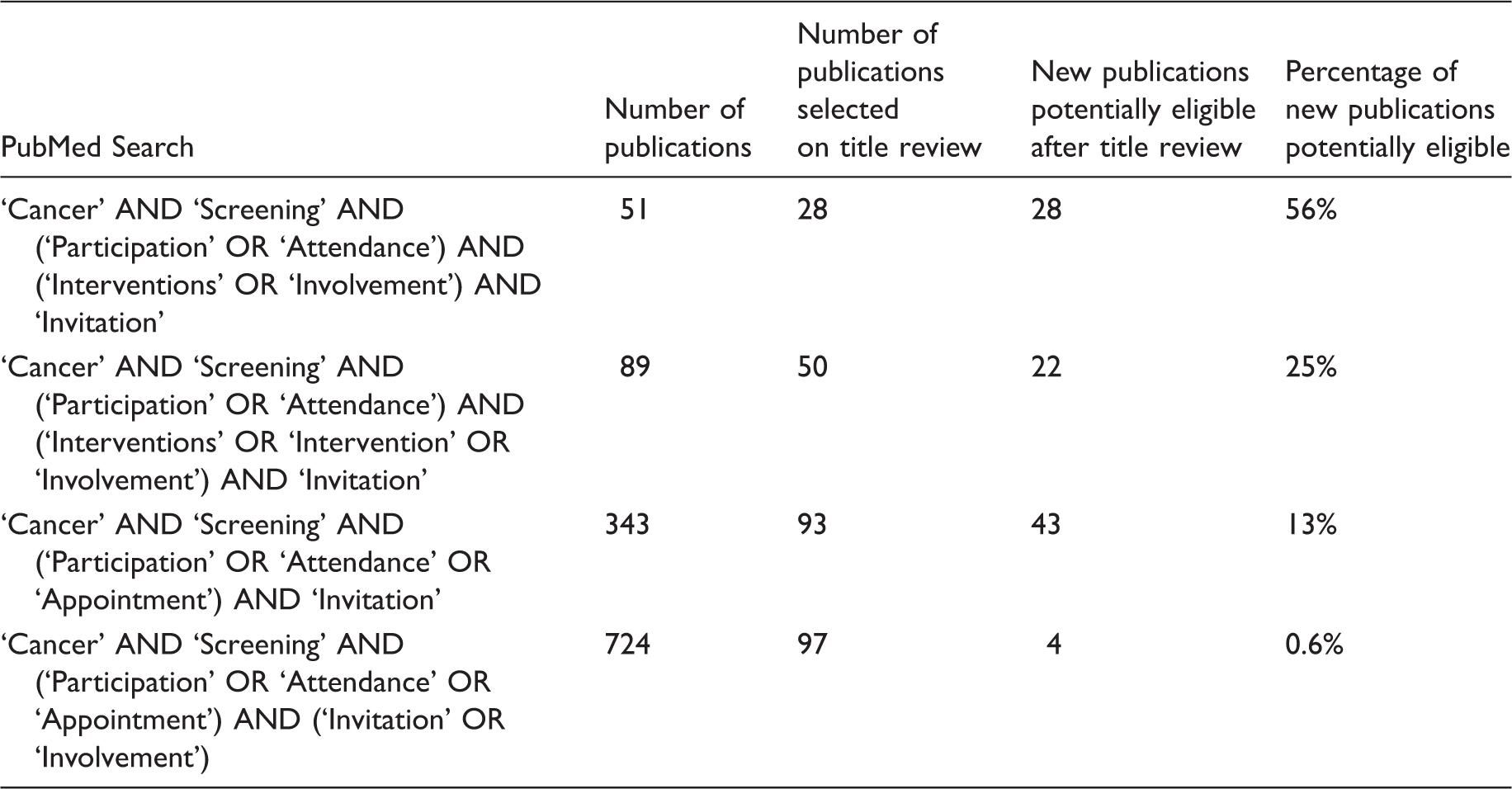
Papers passing title review underwent abstract review. Those remaining eligible after abstract review underwent full paper review. In addition to original papers, our searches identified five reviews.11–15 From these, and from the reference lists of the papers eligible after full paper review, we identified further potential papers which, in turn, were subject to abstract and, if eligible, full paper review. Finally, colleagues identified evaluations of eight interventions published in three papers since the searches took place.16–18
Papers were reviewed for the effect of the intervention by the cancer for which they were screening and by intervention type (reminders in addition to usual invitation; primary care endorsement; additional interventions in non-participants; enhanced invitation materials or varying invitation strategy; direct contact; varying the screening test). Interventions can occur at various stages of the process, from advance notice communications sent prior to first invitation to screening, to the offer of a different screening test at the screening episode some years following non-participation in a previous episode (see Figure 1). We deal with the arbitrary nature of the classification below (see Discussion section). In addition, interventions were studied to identify effects by different socioeconomic or ethnic grouping, if any, and to identify any other inequality dimension in the work.
Schematic diagram showing the categories of intervention by time point on the screening pathway at which the intervention takes place, with references to the relevant studies in parentheses.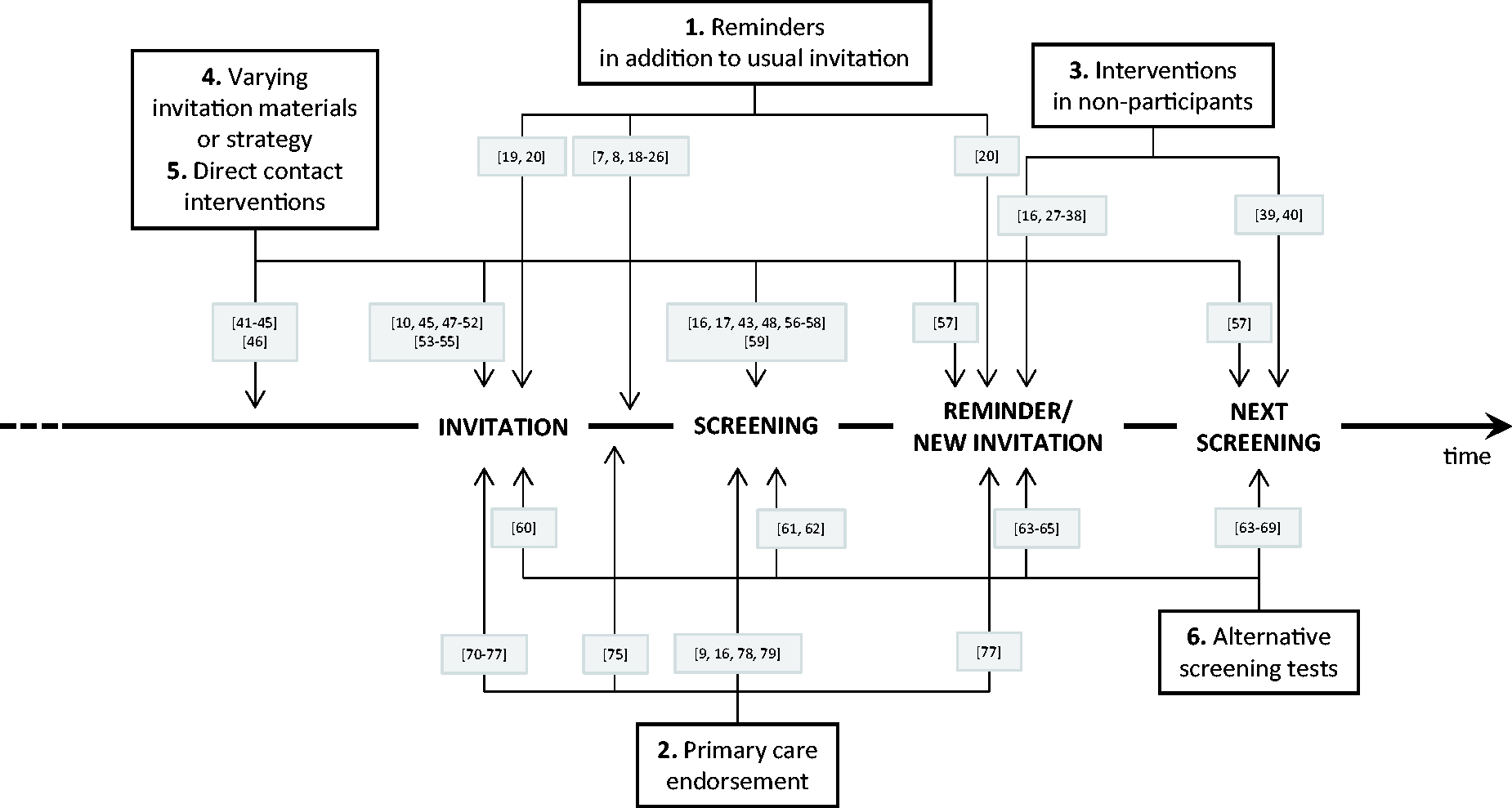
In the description of results of interventions below, percentage increases in participation refer to absolute increases; for example, a 5% increase would refer to a difference between 20% and 25% (an absolute increase of 5%) rather than 20% and 21% (a 5% relative increase).
Results
After abstract review, 62 papers were deemed eligible. On full paper review, two were excluded, leaving 60. From reference lists and reviews, after full paper review, further five papers were added. As noted above, colleagues identified another three papers published since the searches, bringing the total to 68 papers included, although one reports on four separate trials and is therefore included four times in the tables of results. 16
Reminders in addition to usual invitation
Studies of reminders additional to usual invitation.

Primary care endorsement
Primary care endorsement studies.

GP: general practitioner; FOBT: faecal occult blood test; FIT: faecal immunochemical test; FIT: faecal immunochemical test.
Interventions targeted specifically on non-participants
Interventions in non-participants.

GP: general practitioner; FOBT: faecal occult blood test.
Varying invitation materials or strategy
Enhanced invitation materials/varying invitation strategy.

GP: general practitioner; FOBT: faecal occult blood test; FIT: faecal immunochemical test.
Direct contact interventions
Direct contact interventions.
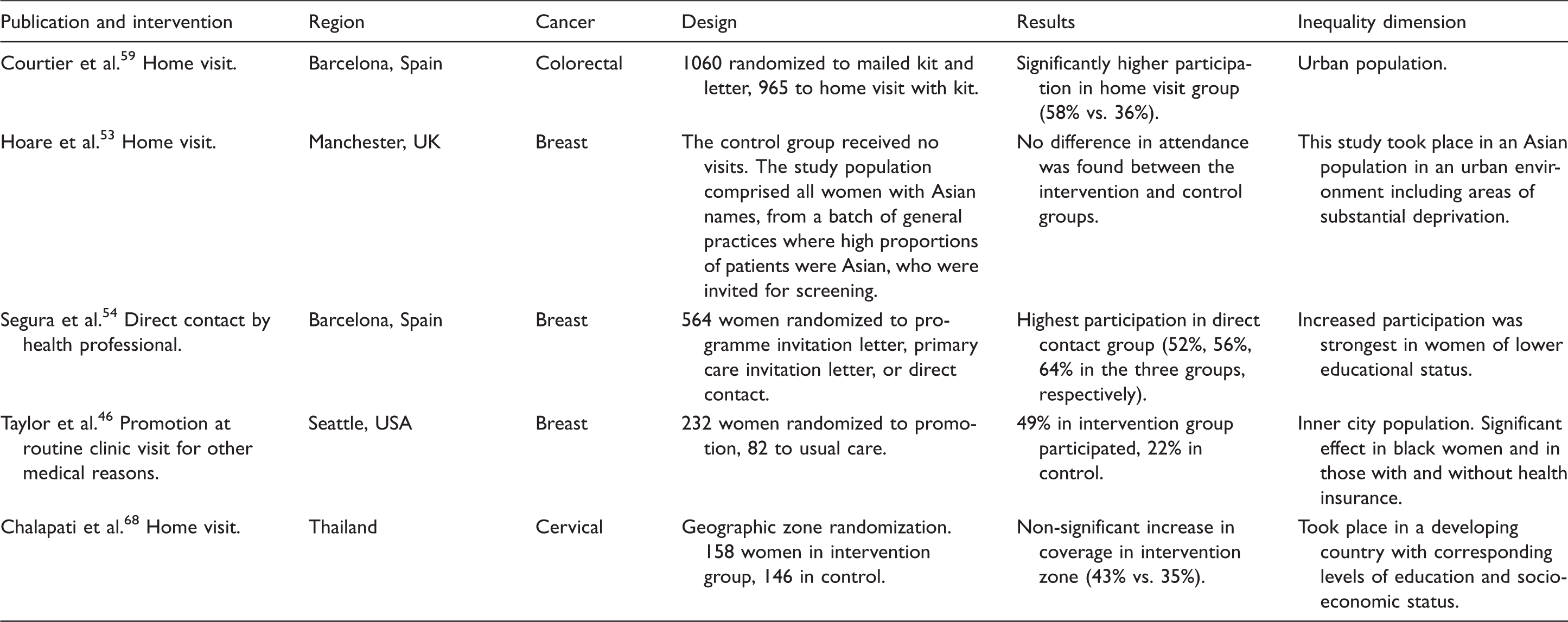
Varying the screening test
Alternative screening tests.

FOBT: faecal occult blood test; HPV: human papillomavirus; OP: out patient; gFOBT: guaiac-based faecal occult blood test; FIT: faecal immunochemical test.
Discussion
A number of results seem to be observed consistently between studies and across different countries and health systems. Both pre-screening reminders and GP endorsement led to higher participation rates (albeit modest increases) and were observed to do so in deprived and otherwise underserved populations.16–18,21,22,74,75,79 More personalized reminders for non-participants, whether by enhanced written materials or telephone contact (notably from primary care), were effective in increasing participation. These interventions too were successful in populations of low socioeconomic status.16,30,33,40 Primary care endorsement and enhanced reminders for non-participants would incur almost no expense (other than the cost of screening larger numbers of people). In the UK, they might be expected to result in small, but arguably worthwhile, increases in participation. Larger increases might be expected in more deprived populations with lower current participation rates. 16
The choice of screening test itself is associated with participation. FIT is clearly more popular than other bowel screening modalities and was observed to increase participation by 15%–20%. HPV self-sampling raised participation rates, notably in previous non-participants, by around 10%. This is likely to be effective in socioeconomic or ethnic populations traditionally less easy to reach with cervical screening. 62 Less consistent results were observed for different invitation strategies and home visits. Inclusion of questionnaires for research along with the invitations seemed to have a negative effect. 38
It is accepted that interventions to promote cancer screening should be non-coercive and should respect the principle of informed choice. 80 However, it is also the case that there is a strong socioeconomic gradient in participation in screening, with lower participation being associated with lower socioeconomic status, 3 and there is evidence that non-participants often report not having read the information provided. 81 The search for interventions to remedy this would, therefore, seem to be ethically justified.
The classification of studies by intervention was arbitrary. For example, most of the HPV self-sampling studies included in Table 7 as interventions varying the screening test could have been included in Table 4 as interventions targeting non-participants. Similarly, some of the latter could have been included as primary care endorsement studies. However, the results are generally clear. It is also worth noting that, in classifying the studies, a degree of oversimplification was inevitable, in that some multi-component interventions have been classified into one category or another. One example is the study by Bell et al., 72 which is classified as primary care endorsement, but which also included multilingual approaches and offers of transport to screening centre.
The magnitude of effects varied considerably, even within intervention types. The effects tended to be larger in environments where participation rates were relatively low. For example, reminder studies showing particularly large effects on participation were that of Baker et al. 21 in Chicago, where opportunistic rather than organized screening was taking place, and one in inner north-east London, where there are large deprived populations, high levels of ethnic diversity, and usually low screening participation rates.8,22 Similarly, in the primary care endorsement studies, greatest effects were seen in populations with previously low participation.72,75
In the studies identified, the patient navigation approach, 82 whereby a ‘navigator’ guides the patient/invitee through the complexities of a screening, diagnostic, or therapeutic process, was largely absent. However, some of the telephone interventions involved detailed scripts and briefing of the staff, so that they were able to answer questions; indeed, one such study in the context of bowel cancer screening showed good results. 22 The concept of patient navigation is already established in the USA and may well spread to Europe in the immediate future.
We did not sub-classify the studies by design or quality but have noted in the tables whether the studies were randomized trials or observational studies. Of the 71 intervention studies, 52 (73%) were randomized, either by individual or cluster. The majority of positive results were seen in randomized studies.
As noted in the Methods section, due to time and resource considerations, we restricted our search to peer-reviewed publications listed in PubMed and adopted an unconventional expanding search strategy rather than a comprehensive search followed by successive narrowing by abstract and paper review. Although we only ceased the search expansion when it yielded relatively small numbers of potentially eligible publications and built in a safeguard by specifying that the search had to include a number of key publications, it is possible that some eligible material has been missed. 83 Watt et al. 84 advocate not a standard methodology for rapid review, but clear reporting and transparency with respect to the methods used. We have tried to adhere to this in terms of the description in the Methods section and the information in Table 1. It would be interesting if another group with the time and resources carried out a traditional systematic review, to see what, if anything, we have missed.
Conclusion
Interventions which were found most consistently to improve participation in cancer screening, including in underserved populations, were pre-screening reminders, general practice endorsement, more personalized reminders for non-participants, and offering a more acceptable screening test in cervical and bowel screening, both of which may suffer from social and cultural taboos.
Footnotes
Acknowledgements
We thank Dr Anne Mackie, Director of Programmes, UK National Screening Committee, for helpful discussion.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This work was supported by the UK National Screening Committee.
