Abstract
This study aimed to investigate the antihyperlipidemic and anti-inflammatory effect of zingiberene (ZBN) on isoproterenol-(ISO) induced myocardial infarction in rats. ZBN (10 mg/kg b.wt.) was orally administered to rats for 21 days and ISO (85 mg/kg b.wt.) was subcutaneously injected into the rats at 24 h intervals for the last 2 consecutive days. We observed increased serum creatine kinase, creatine kinase-MB, cardiac troponin T, and I levels in ISO-treated MI rats. Conversely, ZBN oral administration significantly prevented in cardiac marker enzyme activities in ISO-mediated rats. We also noticed that ZBN oral administration prevented ISO-induced expression of lipid peroxidative markers, total cholesterol, triglycerides, phospholipids, free fatty acids, very-low-density lipoprotein cholesterol (VLDL-C), low-density lipoprotein cholesterol (LDL-C) to the normal basal level. Furthermore, ZBN restored ISO-mediated antioxidant status, increased level of high-density lipoprotein cholesterol (HDL-C), and tissue phospholipids to the near-normal levels. Besides, ZBN pre-treatment significantly reduced the level of inflammatory markers (TNF-α, IL-6, NF-κB, and IL-1β) in ISO-induced MI in rats. We noticed that ZBN pretreatment inhibited the pro-apoptotic proteins Bax and cytochrome c and increased the Bcl-2 expression in ISO induced rats. The gene expression profiling by qRT-PCR array illustrates that ZBN treatment prevents the ISO mediated activation of cardiac markers, inflammatory, and fibrosis-related genes in the heart tissue. Taken together, pre-treatment with ZBN attenuated ISO-induced MI resolved exhibits the anti-inflammatory and antiapoptotic effect.
Introduction
Myocardial infarction (MI) is acute necrotic damage to the heart muscles which might be the major reason for mortality in the developed countries. 1 Ischemic heart disease is currently at the top of the mortality list. As per 2016 statistics, about 2,303 deaths occur every day due to cardiovascular diseases. 2 Sudden blockage of coronary arteries minimizes a portion of myocardial tissue from the constant blood supply. A most common phenomenon of MI is the development of coronary atherosclerosis that has strongly been associated with hyperlipidemia, oxidative changes, and inflammatory signaling. 3 The lifestyle factors mainly nutrition plays an important role in the development of MI. Experimental studies illustrate the enlarged infarct size during ischemia in rat models. 4,5 Epidemiological studies indicate that an increased risk of coronary heart disease (CHD) is associated with high levels of serum total cholesterol, triglyceride, and decreased levels of high-density lipoprotein (HDL). 6 –8
Cardiac markers are enzymes or factors released to the bloodstream due to the necrotic death of cardiac myocardial tissue. Myoglobin, creatine kinase-MB, troponin I/T are the major gold standard cardiac markers, and analyzing these markers in the serum or plasma might be useful during MI. 9 Isoproterenol hydrochloride (ISO) is a β-adrenergic agonist that causes necrotic damage in the heart tissue. 10 ISO generates free radicals which may be an underlying factor for irreversible damage to the myocardial membrane. 11 Reactive oxygen species (ROS) induces several biochemical events associated with atherogenesis. ISO has been reported to increases lipids such as total cholesterol, triglycerides (TGs), free fatty acids (FFAs), and phospholipids (PLs) in circulation. 12 It also increases the levels of low-density lipoprotein cholesterol (LDL-C) in the blood which causes the buildup of harmful lipid deposits in the blood vessels. 13
MI-mediated cellular damages are implemented by manly signaling molecules. Activation NF-κB has been reported during ISO-induced MI. 14 NF-κB has been considered as a key regulator in the condition of inflammation and fibrosis. The ISO administration induces phosphorylation of NF-κB which initiates the intracellular signaling cascade that resulted in the overexpression of pro-inflammatory cytokines such as TNF-α, IL-6, IL-1β as well as cardiac-specific markers. 15 The matrix metalloproteinases specifically MMP-2 and MMP-9 play a major role in the degradation of myocardial fibrillar collagen. 16 The ISO treatment induces acute proteolytic activity thereby induces myocyte loss and finally causes MI and heart failure. The hypoxia-induced angiogenesis takes place in ISO-treated cardiac tissues. Inducible nitric oxide synthase (iNOS) and endothelial nitric oxide synthase (eNOS) play an important role in reducing the infarct size during ISO mediate MI. 17 The iNOS-derived NO and VEGF were reported to promote survival of ischemic tissue by stimulating angiogenesis. 18 Apoptotic cell death is a major contributor for MI and acute heart failure. The ISO administration activates proapoptotic protein such as Bax and Bad resulted in the instability of outer mitochondrial membrane which causes the release of cytochrome-c into the cytosol. In the cytosol, cytochrome c activates caspase-9, which cleaves and activates caspase-3, causing the induction of apoptosis. 19
The regular consumption of antioxidant phytochemicals is associated with the prevention of atherogenesis and ischemia. The bioactive secondary metabolites present in the medicinal plants were endowed with potential pharmacological properties. It has been postulated that the antioxidant nature of the phytochemicals scavenges ISO-induced free radicals formation thereby terminates subsequent heart injury. 20 Treatment with phytochemical formulations shows attenuated inflammation-related (TNF-α, IL-6, MMP-9) and oxidative stress-related (ox-LDL, MDA, SOD) indicators in CHD patients. 21 Sesquiterpenes are a group of terpenoids modulates ISO-induced lipid peroxidation, mitochondrial dysfunction and histological alterations. 22,23 Zingiberene (ZBN) is a monocyclic sesquiterpene, mainly present in ginger with oil content (Zingiber officinale). It can contribute up to 30% of the essential oils in ginger rhizomes. 24 ZBN has several pharmacological properties such as antioxidant, 25 anticancer, 26 antiulcer, 27 antibacterial, 28 and antiviral 29 effect. ZBN possess the ability to modulate the inflammatory PI3K/AKT/mTOR pathway in human cells. 30 Although the ginger and its active compound ZBN have well been investigated for various pharmacological properties the anti-inflammatory and antiapoptotic effect of ZBN in ISO-induced myocardial infarction has not yet been revealed. Therefore, we assessed the preventive effect of ZBN on ISO-induced cardiac serum markers, lipid peroxidative markers, antioxidant status, lipid profile, inflammatory markers, and apoptotic markers in MI rats.
Materials and methods
Chemicals
ISO (catalog No. 15627) was obtained from Sigma Aldrich (St Louis, Missouri, USA). ZBN (Catalog No. 495-60-3) was purchased from Guidechem Chemical Network (China). All the primary antibodies such as Bax (SC-20067), Bcl-2 (SC-7382), Cytochrome c (SC-13156), Caspase-3 (SC-56053) and β-actin (SC-8432) were purchased from Santa Cruz Biotechnology, USA. TNF-α (ab236712), IL-6 (ab234570), NF-κB (ab176647), and IL-1β (ab255730) ELISA kits were procured from Abcam Scientific Company, USA. All the other chemicals of analytical grade used in the study.
Myocardial infarction and treatment plan
Wistar albino rats (males) with the bodyweight of 160–180 g were used for MI experiments. The MI induction and treatment protocol was approved by the Institutional Animal Ethical Committee. The ZBN was dissolved in 0.05% DMSO and ISO-hydrochloride were dissolved in physiological saline. ZBN was given oral administration for 21 consecutive days. The experimental dose of ZBN was selected by acute toxicity studies (Table 1). MI was induced by injection of 85 mg.kg bw (s.c.) ISO on the 20th and 21st days. The dose of ISO used for MI induction was selected as per the previously published literature.
19,31
The rats randomly divided into four experimental groups with six rats (n = 6) in each group. The animals were given food and water ad libidum during the experimental period. The animals were maintained normal dark and light cycle. Group I: Control rats (received 0.5% DMSO s.c., for 21 days). Group II: Control+ ZBN (10 mg/kg BW, s.c., for 21 days). Group III: ISO control (85 mg/kg BW, s.c., for 20th and 21st day). Group IV: ZBN (10 mg/kg BW, s.c., for 21 days) + ISO (85 mg/kg BW, s.c., for 20th and 21st days).
Effect of various concentrations of ZBN on the acute toxicity study of male albino Wistar rats.

Different doses of ZBN (5–1000 mg/kg. b.wt.) were administered to rats and mortality for 21 consecutive days.
After 24 h of the last ISO and/or ZBN treatment, the rats were anesthetized using ketamine hydrochloride (24 mg/kg b.wt.) and were sacrificed by cervical dislocation.
Assessment of acute toxicity of ZBN in male albino Wistar rats
The acute toxicity study of ZBN was determined according to Begum et al. 32 Briefly, the animals were allowed to fast by withdrawing the food and water for 18 hours. The fasted animals were divided into differenet groups of six each. Each group of animals were given different doses (5, 10, 20, 50, 80, 100, 200, 300, 400, 500, 800 and 1000 mg/kg b. wt.) of freshly prepared ZBN. The animals were provided with food and water immediately after the drug administration. The animals were observed continuously for 21 days, for any signs of morbidity, mortality and behavioral toxicity.
Analysis of cardiac markers in serum
The measurement of cardiac markers in serum plays a major role in the early diagnosis of MI. In this study, we measured the activity of creatine kinase-MB (CK-MB) and Creatine kinase (CK) during ISO and/or ZBN by the methods described by Okinaka et al. 33 Troponins are released to the bloodstream during MI. We measured the serum levels of cTn T and cTn I using commercial ELISA kit. 34,35 We strictly followed the methods and calculations as per the manufacturer’s protocol.
Measurement of lipid peroxidative markers in plasma and heart tissue
The ISO-treatment induces lipid peroxidation and elevates the levels of peroxidative products like TBARS and lipid hydroperoxides (LHP) in the bloodstream. We measured the plasma and heart TBARS levels during ISO and/or ZBN treatment the method of Niehaus and Samuelsson. 36 We measured plasma and cardiac tissue lipid hydroperoxides (LHPs) were carried out as per the method of Jiang et al. 37
Estimation of intracellular antioxidant defense system
The ISO administration severely hampers the intracellular antioxidant status. We measured the levels of reduced glutathione (GSH) and activities of catalase (CAT), glutathione peroxidase (GPx) and superoxide dismutase (SOD) during ISO and/or ZBN was estimated by the following methods 38 –41 in plasma, erythrocytes, and heart tissue.
Estimation of lipids in plasma and heart tissue
We extracted myocardial tissue lipids and plasma lipids as per the protocol described by Folch et al. 42 after the ISO and/or ZBN treatment. Then, we analyzed the levels of TC, TG, FFA, and PL by the protocols of Allain et al., 43 McGowan et al., 44 Falholt et al., 45 and Zilversmit and Davis 46 respectively. Plasma high-density lipoprotein-cholesterol (HDL-C) was estimated by the method of Izzo et al. 47 and low-density lipoprotein-cholesterol (LDL-C), very low-density lipoprotein cholesterol (VLDL-C) in the plasma was calculated by Friedwald’s 48 formula. Then, we calculated LDL-C and VLDL-C fractions as per the following formula: VLDL-C = TG/5 and LDL-C = TC − (HDL-C + VLDL-C).
Determination of inflammatory markers
The inflammatory proteins were the prominent markers to understand the ISO-induced MI. We measured the serum level of TNF-α, IL-6, NF-κB, and IL-1β during ISO and/or ZBN treatment by ELISA kits procured from Abcam Scientific Company. We followed the methodology and calculations as per the manufacturer’s protocol. Briefly, 50 µL of standard or experimental sample was added to designated wells. Then, 50 µL of antibody cocktail was added to all the wells. Then, the plates were incubated at room temperature for 1 hour. After washing with wash buffer 100 µL of TMB substrates were added to each well and incubated for 10 minutes. After the addition of a 100 µL stop solution the color developed was read OD at 450 nm using Tecan Multimode Reader.
Protein expression by western blot analysis
Protein expression studies were done by the western blotting technique by standard protocol. 19 Pro and anti-apoptotic markers such as Bax, Bcl-2, cytochrome c, and caspase-3 were examined by western blotting. The proteins were extracted from heart tissue by RIPA buffer contained cocktail protease enzyme. The proteins were located to SDS-PAGE (10%) and the gel was reallocated to the membrane (PVDF). Then the membrane was blocked with bovine serum albumin (5%) for 2 hrs at room temperature. Then, membranes were incubated with primary antibodies (Bax, Bcl-2, cytochrome c and caspase-3) luminescence underlying substance, and band illumination were analyzed by software image J.
Analysis of inflammatory, angiogenesis and fibrotic related gene expression by a qRT-PCR array
The total RNA content was isolated from control, ISO control, ISO plus ZBN treated heart tissues using an RNeasy mini kit, and used for qRT-PCR arrays. The purity of the isolated RNA was measured by Nanodrop spectrophotometer. The cDNA was reverse transcribed using a First Strand cDNA Synthesis Kit and used for PCR amplification by SYBR green chemistry using the Qiagen kit. Briefly, the total of 25 µl of reaction mixture contains 100 ng of RNA (100 ng), primers (2.5 μl), PCR master mix (12.5 μlof SYBR Green) and reverse transcriptase enzyme (0.25 μl). The relative expression pattern of cardiac markers (CK, CKMB, cTnT, cTnI), transcription factors (NF-κB), proangiogenic and fibrotic related molecules (TNF-α, IL-6, IL-1β, p-eNOS, iNOS, MMP-2, MMP9), growth factors (VEGF) and signaling molecules (AKT) were analyzed by a qRT-PCR array. The fold changes of gene expression were calculated as per 2^(−ΔΔCt) and plotted as cluster grams. The heat map was developed by clustering the normalized signal values. The heatmap was produced using Cluster/Treeview software. The GAPDH was used as internal control.
Statistical analysis
The experimental data was generally expressed as mean ± standard deviation (SD) unless otherwise stated. We used SPSS® software platform for the comparison of mean values between experimental groups. We employed One Way ANOVA followed by DMRT was used to analyze the statistical significance between control, ZBN, ISO, and ISO plus ZBN groups. The level of significance was considered as p < 0.05.
Results
Effect of various concentrations of ZBN on the acute toxicity study of male albino Wistar rats
The administration of different concentration of ZBN (5, 10 20, 50, 80, 100, 200, 300 and 400 mg/kg b.wt.) has not induced mortality during the 21 days observation period. However, 16.6% and 33.33% animals died when the ZBN dose was raised to 500 and 800 mg/kg b.wt. A further increase in the dose ZBN (1000 mg/kg.b.wt.) resulted in 50% mortality. The concentration between 5 to 400 mg/kg b.wt of ZBN produce no mortality. In this study, we used just 10 mg/kg b.wt. ZBN for myocardial infarctions study (Table 1).
Effect of ZBN on ISO-induced serum cardiac marker enzymes
Figure 1(a) and (b) show the effect of ZBN treatment on the activities of CK, CK-MB, cTn T, and cTn I. ISO treatment significantly increased the activities of these cardiac marker enzymes. Conversely, a significant decrease in the activities of CK, CK-MB cTn T, and cTn I was observed in ZBN plus ISO-treated rats. The ZBN alone treatment does not alter the activities of cardiac markers when compared to the sham control p-value ≤ 0.05 (DMRT).

Effect of ZBN on ISO-induced serum cardiac marker enzymes. (a) Effect of ZBN on CK and CK-MB in the serum of control and ISO-induced rats. (b) Effect of ZBN on cTn T and cTn I in the serum of control and ISO-induced rats. Values are given as means ± S.D (n = 6). Values not sharing a common marking superscript (a, b, c) are different significantly at p value ≤ 0.05 (DMRT).
Effects of ZBN on ISO-induced lipid peroxidation in plasma and heart tissue
Rats induced with ISO showed increased levels of lipid peroxidation products such as TBARS and LOOH levels when compared to the sham control group. Both, the heart tissue and rat plasma showed increased lipid peroxidative products during ISO-administration. However, ZBN administration significantly reduced ISO-induced TBARS and LOOH as compared to MI alone induced group. The ZBN alone treatment does not alter the levels of these lipid peroxidative markers when compared to the sham control (Table 2).
Effect of ZBN on the levels of TBARS and LOOH in the plasma and heart of experimental rats.

Values are expressed as means ± S.D for six rats in each group. Values not sharing a common superscript (a, b, c) differ significantly at p ≤ 0.05 (DMRT).
Effects of ZBN on ISO induced antioxidant status
We measured the antioxidants enzyme status in the blood erythrocytes and the reduced GSH levels in the plasma. Further, we also analyzed these antioxidants status in the heart muscles of experimental rats (Tables 3 and 4). Animals treated with ISO had drastically reduced in the activity of enzymatic antioxidants such as SOD, catalase, and GPx and decreased the GSH levels when compared to the untreated control group. Whereas, ZBN pretreatment prevented the ISO-induced loss of antioxidant enzymes. The ZBN treatment alone does not alter the antioxidants status in the heart tissue as well as in the rat plasma when compared to the sham control p-value ≤ 0.05 (DMRT).
Effect of ZBN on the activities of SOD, catalase, GPx in erythrocytes and GSH levels in the plasma of experimental rats.
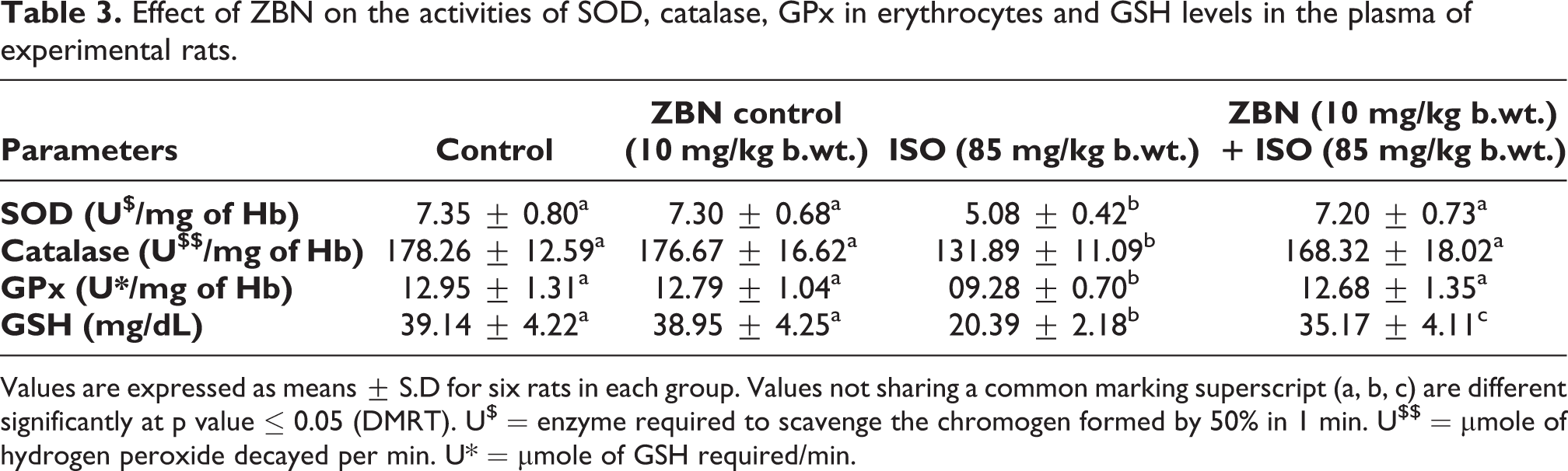
Values are expressed as means ± S.D for six rats in each group. Values not sharing a common marking superscript (a, b, c) are different significantly at p value ≤ 0.05 (DMRT). U$ = enzyme required to scavenge the chromogen formed by 50% in 1 min. U$$ = µmole of hydrogen peroxide decayed per min. U* = µmole of GSH required/min.
Effect of ZBN on the activities of SOD, catalase, GPx and the levels of reduced GSH in the heart of experimental rats.
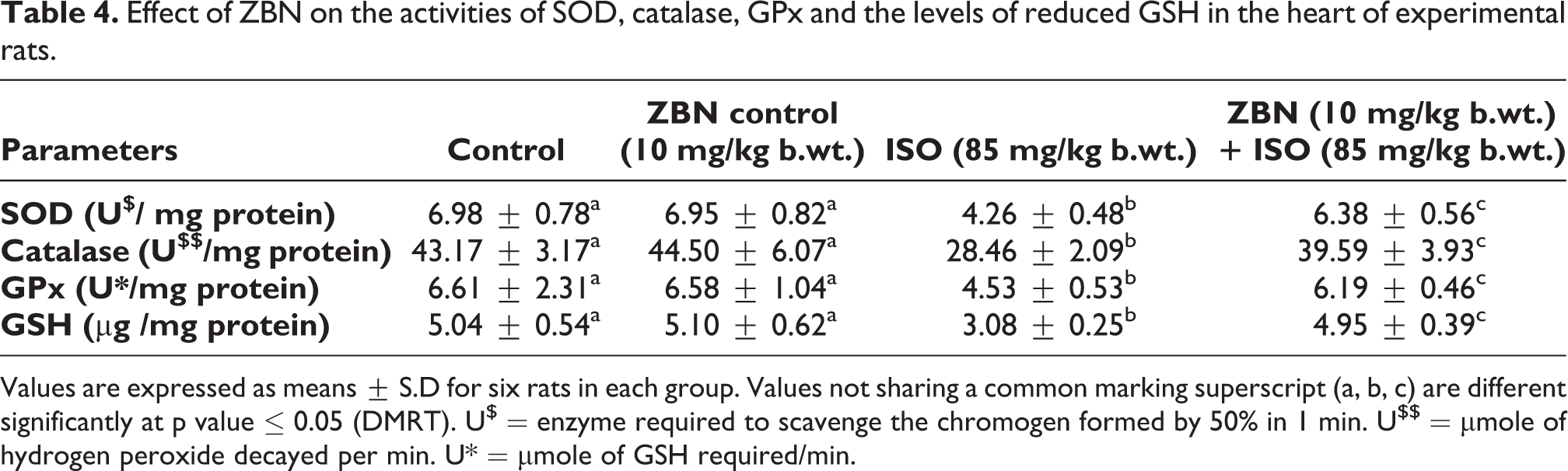
Values are expressed as means ± S.D for six rats in each group. Values not sharing a common marking superscript (a, b, c) are different significantly at p value ≤ 0.05 (DMRT). U$ = enzyme required to scavenge the chromogen formed by 50% in 1 min. U$$ = µmole of hydrogen peroxide decayed per min. U* = µmole of GSH required/min.
Effect of ZBN on ISO-induced lipid profile and lipoproteins in plasma and heart tissue
We measured the lipid profile and lipoprotein status in the plasma of experimental rats. We observed that the ISO-administration elevated the levels of TC, TG, FFA, PL, LDL-C, and VLDL-C and decreased the levels of HDL-C in the blood plasma. Conversely, the ZBN pretreatment prevented ISO-mediated circulating lipoproteins levels and significantly (p-value ≤ 0.05 (DMRT) brought back to near-normal levels (Figure 2(a) and (b)).
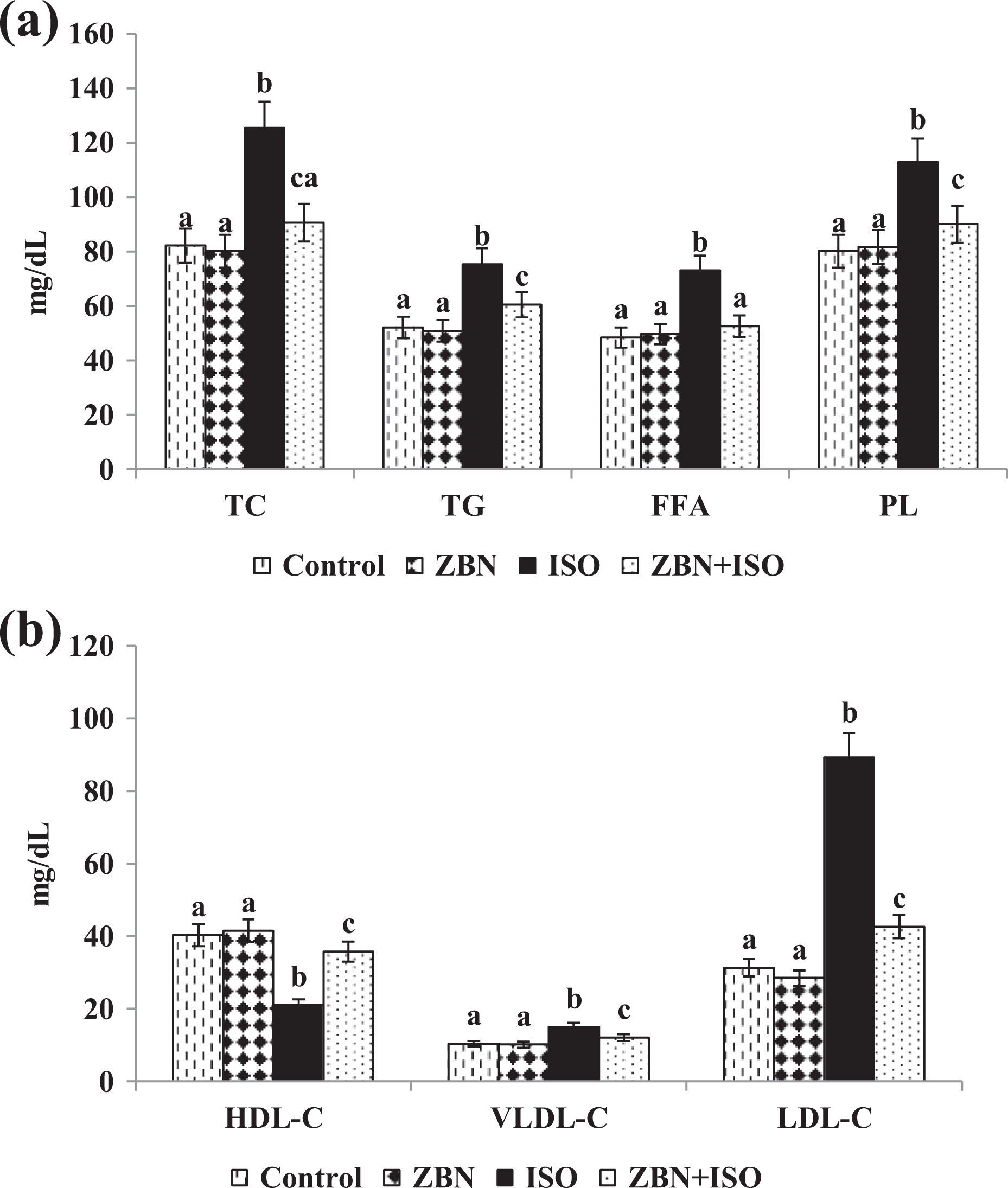
Effect of ZBN on ISO-induced lipid profile and lipoproteins. (a) Effect of ZBN on the levels of TC, TG, FFA and PL in the plasma of control and ISO-induced rats. (b) Effect of ZBN on the levels of lipoproteins in the plasma of control and ISO-induced rats. Values are given as means ± S.D (n = 6). Values not sharing a common marking superscript (a, b, c) are different significantly at p-value ≤ 0.05 (DMRT).
We also measured the levels of lipids in control and ISO-induced rats (Figure 3). The ISO-treatment elevated TC, TG, FFA levels accompanied by a decrease in PL levels. Conversely, ZBN pre-treatment prevented ISO-induced TC, TG, and FFA levels to near normal (p-value ≤ 0.05 (DMRT). The ZBN alone treatment does not alter the lipids and lipid peroxidation parameters in the plasma and heart tissue.

Effect of ZBN on the levels of TC, TG, FFA and PL in the heart tissue of control and ISO-induced rats. Values are given as means ± S.D (n = 6). Values not sharing a common marking superscript (a, b, c) are different significantly at p-value ≤ 0.05 (DMRT).
Effect of ZBN on inflammatory markers level in the serum
Inflammation is the primary event during ISO-mediated MI development. We measured the serum levels of inflammatory markers such as TNF-α, IL-6, NF-κB, and IL-1β in the experimental rats. The ISO administration significantly increased the levels of these inflammatory markers when compared to control rats (p-value ≤ 0.05 (DMRT). Whereas, ZBN pre-treatment significantly prevented ISO-induced activation of the TNF-α, IL-6, NF-κB, and IL-1β levels in the rat serum (Figure 4). The ZBN treatment alone does not alter the expression of the inflammatory markers in the serum.

Effect of ZBN on inflammatory markers level in the serum of control and ISO-induced rats. Values are given as means ± S.D (n = 6). Values not sharing a common marking superscript (*, **) are different significantly at p-value ≤ 0.05 (DMRT).
Effect of ZBN on ISO-induced apoptotic markers expression by western blot analysis
We isolated total proteins from the heart tissue upon completion of the experimental period. The ISO treatment significantly upregulated the expression of pro-apoptotic proteins such as Bax and cytochrome c in the heart tissue when compared to the sham control group. Conversely, the anti-apoptotic protein Bcl-2 was found to be down-regulated in ISO-administered rats. The pretreatment with ZBN significantly reversed the ISO-mediated apoptotic markers expression in heart tissue. No changes in the expression pattern of apoptosis markers were observed in sham control and ZBN alone treated rats (Figure 5(a) and (b)).

Effect of ZBN on Bax, Bcl-2, cytochrome c and caspase-3 protein expressions in the heart tissue of experimental rats. (a) Bax, Bcl-2, cytochrome c and caspase-3 protein expressions by western blot analysis. Lane 1: control; 2: ZBN control; 3: ISO control; 4: ZBN + ISO. (b) Band intensity scanned by the densitometer. The graph depicts quantitation of three independent experiments (means ± S.D), with data normalized by the control group with Bax, Bcl-2, cytochrome c and caspase-3 as unit 1. Values not sharing a common superscript (*, **) differ significantly at p ≤ 0.05 (DMRT).
Effect of ZBN on ISO-induced gene expression by PCR array
We analyzed the transcriptional profile of target genes in the heart tissue of experimental animals. The relative mRNA expression pattern (RQ) of cardiac markers (CK, CKMB, cTnT, cTnI), transcription factors (NF-κB), proangiogenic and fibrotic related molecules (TNF-α, IL-6, IL-1β, p-eNOS, iNOS, MMP-2, MMP-9), growth factors (VEGF) and signaling molecules (AKT) were found to be overexpressed in the ISO-administered heart tissue when compared to the sham control. Conversely, the ZBN treatment prevented the ISO-mediated overexpression of inflammation, angiogenesis, and fibrosis-related gene expression toward a normal level (Figure 6(a) and (b)). The ZBN treatment alone does not alter the transcriptome pattern of inflammatory markers when compared to sham control.

Effect of ZBN on ISO-induced inflammatory, angiogenesis and fibrotic related gene expression by qRT-PCR array. (a) Hierarchical clustergram analysis of PCR array results for inflammatory, angiogenesis and fibrotic related gene expression in ZBN and ISO-induced rats. Bright red indicates the highest normalized signal values, bright bluerepresents the lowest signal values and white and light blue represents median signal values. The total mRNA was isolated from heart tissues and were detected using custom PCR array following the manufacturer’s instructions. (b) Relative gene expression levels of inflammatory, angiogenesis and fibrotic related gene expression in ISO and ZBN + ISO treated rats. The fold changes of gene expression were calculated as per 2^(−ΔΔCt).
Discussion
In this study, we noticed that ZBN prevented ISO-induced myocardial infarction in experimental rats. The subcutaneous ISO treatment conveniently induces myocardial injury and cardiac tissue dysfunction in the mice heart. Therefore, researchers widely employ ISO-treated animals for testing preventive effects of therapeutics. 49 The ISO administration induces the release of cardiac-specific inflammatory biomarkers into the bloodstream. The creatine kinases are generally present in the cellular partition and outflow into circulation in cardiac damage leads to degeneration of contractile component. 50 Further, the cardiac-specific markers like troponins T and I are highly specific and sensitive markers for cardiac diseases and also the desired markers for the diagnosis of MI. 51 Measurement of serum concentration of cardiac markers during ISO treatment might be a useful approach for pharmacological studies as well as for drug discovery purposes. 52 In this study, we found that there were elevated levels and activities of CK, CK-MB, cTnT, and I in MI rats. Conversely, pretreatment with ZBN significantly attenuated the actions of CK and CK-MB and decreased the levels of cTn T and I when compared to control rats. These results might be due to its potent efficacy in regulating membrane reliability by regulating the leakage of the cardiac enzymes into the flow. Ansari et al. reported that the ethanolic extract of Zingiber officinale pretreatment had a significant cardioprotective effect and maintains myocardial membrane integrity in ISO-induced in rats. 53
Lipid peroxidation has been considered as a major pathogenic process in cardiac injury. 19 The ISO administration in the cellular milieu generates quinone intermediates which subsequently generates highly reactive oxidative free radicals. 54 In this current study, we found augmented the levels of lipid peroxidation products (TBARS and LOOH) in ISO caused cardiotoxicity in rats due to increased free radical-mediated membrane destruction. Whereas, pretreated with ZBN reduced the levels of lipid peroxidation products in ISO induced MI rats due to its potent antioxidant activities. Thus, these results suggested that ZBN scavenges excessive free radical production by inductions of ISO rats as compared to untreated control rats. Similarly, the ZBN scavenges H2O2 induced oxidative changes in the neuronal cells through its antioxidative nature. 26 This protective nature of ginger phytochemicals against oxidative damages was further validated by maintaining normal levels of antioxidant enzymes. 55
The enzymatic antioxidants like SOD converted into superoxide to H2O2, Catalase and GPx are accountable for converting hydrogen peroxide to H2O. 56 The levels of GSH is an essential non-enzymatic antioxidant, which has straightly countered the free radicals and also it donates electron for the reduction of peroxides to the enzymatic reaction catalyzed by GPx. 57 Furthermore, our findings suggested that the declined the activities such as SOD, Catalase, GPx and GSH level indicating cardiac injury by ISO-induced rats of heart, erythrocytes, and plasma. These results attained that the ZBN acts as a strong antioxidant mediator when induced with ISO in MI rats. Further, ZBN possesses the potency to restores the activities of SOD, Catalase, GPx, and the reduced GSH levels toward normalcy. It might be due to the ability of ZBN to interact with hydroxyl and superoxide radicals thereby consequently having the protection of free radical scavenging activity. 58 The main source of ZBN from Zingiber officinale (ZO) gingerol 59 and zingerone and zingiberene. 60,61 The ZO compounds scavenge free radicals mediated thereby inhibits lipid peroxidation and maintain cellar homeostasis. 62 –64
Lipid parameters are useful in determining risk factors for cardiovascular diseases. Hyperlipidemia and hypercholesterolemia are risk factors for the development of heart failure. 65 In the present study, ISO-administration elevated TC, TG, and FFA in both the heart and plasma. Alterations of lipid profile during ISO in the heart tissue have already been reported. 66 The ISO-administration activates adenylate cyclase activity thereby increasing the formation cAMP. This mechanism has widely been accepted for lipolytic behavior of ISO 67 Then cAMP induces lipolytic activity resulting in the hydrolysis of stored triacylglycerol thereby caused hyperlipidemia. 68 ZBN pre-treatment significantly restored ISO-mediated hyperlipidemia and maintain membrane architecture in the myocardial tissue. ISO-induced rats showed an increase in the level of LDL-C, VLDL-C, and decreased in HDL-C. In the present study, it was evident that ZBN significantly reduced the lipid profile and elevate the HDL level. Bhandari et al. reported that the preventive effect of ZO extract against altered lipid metabolism in high cholesterol-fed rabbits. 69
Previous reports found that oxidative stress and inflammatory responses play an important role in the MI. 70,71 In the current study, the major inflammatory cytokines like TNF-α, IL-6, and IL-1β were significantly increased in the ISO-treated rats. The ZBN pretreatment prevented ISO-induced overexpression of TNF-α, IL-6, IL-1β probably by inhibiting the activation of the NF-κB signaling pathway. The ZBN pretreatment might inhibit free radical reactions and thus suppress the activation of NF-κB that resulted in the downregulation of various proinflammatory cytokines. Further, we observed, the ISO treatment induces several genes including VEGF and iNOS, and eNOS which thought to be potentially involved in angiogenesis. Conversely, ZBN treatment attenuated ISO-induced mRNA expression pattern of angiogenesis factors in the heart tissue. Similarly, rosuvastatin reverses isoproterenol-induced acute myocardial infarction through modulating iNOS and VEGF. 17 In this study, the ISO-treatment also induces the overexpression of MMPs. These MMPs induces cardiac myocyte loss through apoptosis and ultimately leads to heart failure. Radhiga et al. reported that ursolic acid attenuated MMPs expression in isoproterenol-induced MI in experimental rats. 72 AKT signal transduction pathway plays an important role in apoptotic cell death through modulating several anti-apoptotic proteins expression. Li et al. reported that ulinastatin against ISO-induced chronic heart failure through the PI3 K Akt, p38 MAPK, and NF-κB pathways. 73 In this study, the ZBN treatment prevented the mRNA expression pattern of AKT signaling molecules. Similarly, the ZBN treatment modulates mTOR/PI3K/AKT signaling events in colon cancer cells. 30 Overall, transcriptome analysis revealed that ZBN treatment modulated ISO-mediated the fibrotic and inflammatory signal transduction pathways in the heart tissue of rats.
Apoptosis plays an important role in the regulation of MI in experimental animals. Bcl-2 family members like Bcl-2 and Bcl-xL are a group of important factors which function as apoptotic inhibitors and Bid proapoptotic proteins like Bax, Bak and Bad known to promote apoptosis. 74 In the current study, we found that upregulated expression of pro-apoptotic expression of Bax, cytochrome c and caspase-3, while, down-regulated expression of anti-apoptotic protein Bcl-2 in ISO-induced rats indicating myocardial apoptosis. The ISO-induced ROS activates Bax to permeabilize the mitochondrial membrane which resulted in the release of cytochrome c. This released cytochrome then activates apoptotic protease-activating factor-1 (Apaf-1). The Apaf-1 forms apoptosome with caspase-9 which triggers the caspase-3 activation which leads to myocardial apoptotic cell death. 75 The western blot results clearly illustrate the ability of ZBN treatment against the ISO mediated activation of apoptotic markers expression. Similar to our present findings, several studies report the preventive potential of phytochemicals against ISO-induced apoptosis in the cardiac tissue. 19,76,77
Conclusion
In conclusion, the ZBN pretreatment significantly attenuated the ISO-induced cardiac markers expression, oxidative damages, alterations in the lipids profiles, inflammatory and apoptotic markers expression in the heart tissue. Therefore, ZBN may be considered as a potential cardioprotective agent and deserves further scientific validation.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
