Abstract
Introduction:
Accidental toxicity by organophosphate (OP) agents may occur among farmers during spraying season due to improper use and handling. Plasma cholinesterase (ChE) activity measurement is recommended to monitor the extent of exposure to the OP agent. The aim of the current study was to measure plasma ChE activity before and after exposure with OP pesticides.
Methods:
This was a prospective study conducted on 36 farmers working in the farm field. The plasma ChE level was measured before spraying and 2 days and 8 weeks after spraying season and exposure to OP agent. Farmers were observed for clinical signs and symptoms of toxicity after exposure.
Results:
Vertimac was the most common agent used by farmers followed by diazinon and chlorpyrifos. The plasma ChE level significantly decreased after exposure by over 50%. The level returned to preexposure level after 8 weeks.
Conclusion:
Exposure to OP pesticide is a major concern in the developing countries. More than 50% reduction in the plasma ChE activity after spraying is an alarming message for health-care system and policy makers. Furthermore, workplace evaluation, serial ChE monitoring, and appropriate training and education to exposed individuals would be initial important steps to avoid the toxicity or reduce the severity of poisoning.
Introduction
Pesticides are the important hazards in agriculture causing serious morbidity and mortality throughout the world, particularly in the developing countries. Of the estimated 3 million acute pesticide poisoning that occurs each year, 250,000 die. 1,2 This figure includes 30% of the total number of intentional poisoning leading to deaths. 1 Ninety five percentage of all fatal poisoning occurs in the developing countries. In Iran, there are more than 500 types of pesticides used in agriculture. 3 Previous studies have reported that pesticides are the third most common cause of poisoning and is the main cause of fatal poisoning in Iran. 3 –5
Mortality following deliberate poisoning with pesticides in the geographical areas with extensive agriculture and in the developing countries including Sri Lanka due to the easy availability, misuse, and inadequate treatment after toxicity has been reported to be very high. 6,7 Accidental poisoning due to inappropriate use of pesticides is another concern in the agricultural areas. In Iran, in Northern provinces such as Mazandaran, agricultural pesticides especially organophosphate (OP) pesticides have been widely used. Thus, occupational poisoning is considered a serious problem in this region. 7
Exposure to OP agents causes a series of illness. In most cases, the initial cholinergic phase may only be observed. In 20% of the toxicity, the cholinergic phase may progress to the intermediate syndrome. Both the acute cholinergic phase and the intermediate syndrome are associated with a high mortality, and in the severe cases, subjects are managed in an intensive care. The final phase, OP-induced delayed polyneuropathy, occurs in 1–3 weeks after exposure to an OP agent. 8 Most OPs are highly lipid-soluble agents and are well absorbed from mucous membranes, conjunctiva, skin, respiratory airway, and gastrointestinal tract. The onset, severity, and duration of toxicity are determined by many factors including dose, route of exposure, physicochemical properties, rate of metabolism, and type of OP agent. 9
Inhibition of cholinesterase (ChE) is considered to be the main mechanism of OP pesticides. There are two types of ChEs present in the body: erythrocyte ChE, also known as acetylcholinesterase (EC 3.1.1.7) or true ChE, which is attached to erythrocytes and hydrolyzes acetylcholine in red blood cells (RBCs), myoneural junctions, cholinergic nerve ends, and the central nervous system, and plasma ChE (EC3.1.1.8), also known as butyrylcholinesterase, which is found in plasma and different organs of the body such as liver and muscle, which hydrolyzes acetylcholine and other choline esters mainly in the plasma. Clinical measurements of these enzymes are the most sensitive biomarkers of exposure to anti-ChE compounds including OPs and carbamate (CB) pesticides in mammals, birds and fish. 10 –13
As assay for blood ChE activity is considered a relatively simple procedure, it is used for assessing the extent of human exposure to OP. Based on preexposure value of less than 30% inhibition to blood ChE is indicative of minor and reversible toxicity, required working condition need to be examined to avoid exceeding such a level. A 30–60% reduction in the activity of blood ChE is compatible with minor damage and presence of initial clinical signs and symptoms of toxicity requiring temporary removal from exposure and analysis of working conditions to prevent further damage. 14
Previous studies have shown that serial measurements of ChE in the spraying season may be helpful in monitoring OP exposure and toxicity. 15 The aim of this study was to evaluate the extent of exposure to phosphorus pesticides measured by seasonal change (before and after exposure) in the plasma ChE enzyme activity in farmers, who used OP pesticides during spraying seasons.
Methods
This was a cohort study (from March to October 2011) on farmers of a suburb region in Mazandaran, the northern province of Iran. Farmers using one of the OP compounds during spraying season were interviewed by the researcher and eligible people were recruited for the study. After obtaining informed consent form and collecting primary information, the blood sample was taken three times, before spraying (preexposure sample), within 2 days after spraying (exposure sample), and 8 weeks after spraying (postexposure sample).
Inclusion criteria for the study were: farmers working on the field and using OP compounds in the spraying season, male gender, aged between 25 and 85 years, living in the county of Farahabad, a suburb region of Mazandaran province in Iran, without any previous known history of liver or other chronic underlying disease according to the history and liver enzyme test checkup, capable of understanding the study, and sign the informed consent form. The blood samples were taken three times, that is, in March, April, or May (for preexposure seasons sample); in June, July, or August (for spraying or exposure season sample); and in August, September, or October (for postspraying or exposure season sample). Blood samples were sent to a local laboratory in the city (Fajr Laboratory) within 2 h after collection for later analysis of liver function tests (alanine aminotransferase, aspartate aminotransferase, alkaline phosphatase, and bilirubin) and plasma ChE activity. Farmers were observed for the development of clinical signs of toxicity by the researcher few days after exposure. A clinical response was regarded as positive if a farmer showed any of the typical symptoms of OP poisoning, including profuse salivation, miotic pupils, ataxia, dysphonea, diarrhea, and muscle twitching.
Other information including type of OP used for spraying, interval between spraying and the onset of signs and symptoms of toxicity, and medical history were collected. Laboratory results and other collected information from the participants were entered into SPSS data analysis sheet anonymously. Statistical analysis was performed using SPSS version 19. Data were presented as mean ± SD. Comparison was performed using Student’s t test and analysis of variance for two and three groups’ comparison of continuous data. p < 0.05 was considered as statistically significant. The study was approved by the local ethics committee. Plasma ChE activity was measured using Elman techniques, which is of colorimetric type that is based on produced choline and its reaction with coloriogenic reagents. 16
Results
A total of 36 farmers, all male gender, were recruited in the study. Most of the participants belong to 40- to 60-year-old group (n = 17, 47.2%) followed by 20–40, 60–80 and >80 year-old group by 30.6%, 19.4%, and 2.8%, respectively. Vertimec was the most common OP pesticides used for spraying (33%). Other common OP compounds used for spraying were diazinon (19.4%) and chlorpyrifos (13%). The area sprayed by farmers was between 2 and 4 hectares (18 famers), less than 2 hectares (16 farmers), and over 4 hectares (2 farmers). No one developed significant signs and symptoms of toxicity. Five persons developed headache, three persons complained from dizziness, and one from rhinorrhea. All study participants had normal liver enzyme level before entering into the study (Table 1).
Liver function test before spraying season (preexposure) in the study participants.
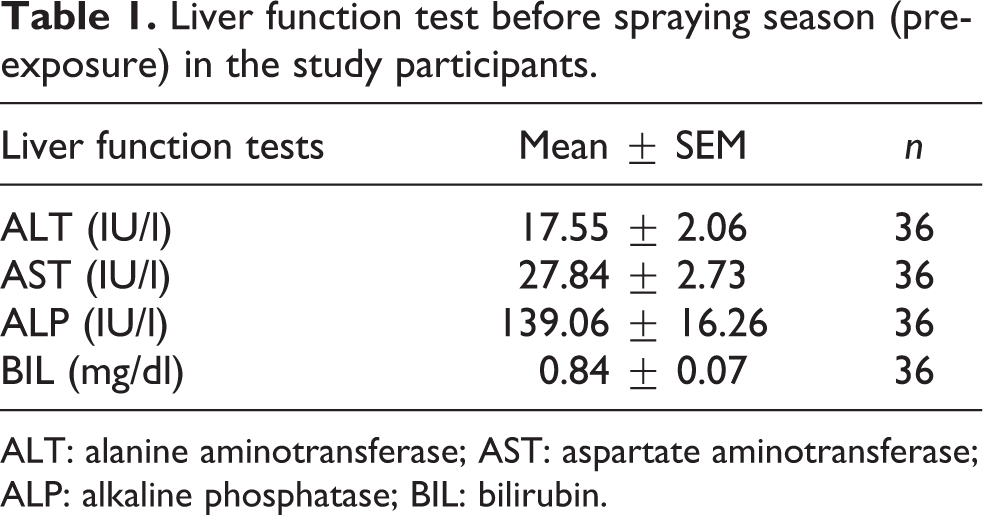
ALT: alanine aminotransferase; AST: aspartate aminotransferase; ALP: alkaline phosphatase; BIL: bilirubin.
The mean plasma ChE activity was 6876.0 ± 389 IU/l before spraying. This measure reached to 4155.0 ± 275 IU/l in 2 days and to 6615.0 ± 392 IU/l in 8 weeks after spraying samples. Plasma ChE activity after exposure dropped by 54.01 ± 0.03% and returned almost to preexposure limit by 91.15 ± 0.03 IU/l after 8 weeks postexposure (Table 2). There was significant difference in plasma ChE activity between before and few days after exposure (p < 0.05). There was no significant difference in plasma ChE activity before and 8 weeks after spraying.
Plasma cholinesterase activity before exposure, within 2 days postexposure, and 8 weeks postexposure to organophosphate agents in the study participants.a

a Significant difference between preexposure and within 2 days postexposure (p < 0.05); within 2 days postexposure and 8 weeks postexposure (p < 0.05). No significant difference was found between preexposure and 8 weeks postexposure.
Discussion
In the current study, plasma ChE was inhibited by 54% on average after exposure to one of the OP agents. Over 50% inhibition in plasma ChE activity, although clinically did not cause significant signs and symptoms, it is considered an alarming exposure requiring further field investigation, education, and training to avoid significant toxicity. In the United States, California and Washington are the only states currently monitoring ChE (RBC and plasma) of OP and CB handlers. In other states, ChEs are determined if exposure are suspected. 10 In the developing countries, there is no such restricted regulation and monitoring and the ChE levels are performed only on individuals with exposure to large amounts of toxins either due to improper use or mostly with suicidal intentions. 10,17 –19
In California, the workplace is investigated if ChE levels of RBC and/or plasma are <80% of baseline. Workers are required to leave the workplace if levels are <70% for RBC and <60% for plasma ChE. Workers cannot return to the field until enzyme activity has recovered to 80% of baseline. New employees are checked after 30 days and then examined every 60 days thereafter. 20 In the state of Washington, ChEs of mixers, loaders, and applicators are monitored by a single-state laboratory. A 20% or greater depression of ChE activity compared with baseline leads to investigation of the worksite; 30% or greater depression of RBC ChE or 40% of plasma ChE requires removal of workers from the field; they may return when their blood levels reach 80% of baseline. 21,22
In another study performed in the same geographical region in Iran, the RBC ChE activity of 35 farmers who were exposed to OP agents for several days was measured. 23 The authors compared this value with RBC ChE activity of 35 people, who were not exposed. They showed a significant drop in the RBC ChE activity of individual who had exposure to OP agents. They also reported that the enzyme inhibition was more prominent in men than in women. In this study, a different group of people who were not exposed to the OP agent were entered into the study as a control group. Considering the interindividual variability in the ChE activity, the result of previous study might not accurately show the extent of exposure. Measurement of ChE activity (RBC or plasma) continues to be used widely for diagnosing exposure to OPs; however, the interpretations of these estimations are not without problems. There are many factors including genetic, physiological (age, gender, pregnancy, and so on), iatrogenic (therapeutic agents), liver disease, and many other factors that interfere and affect the enzyme activity. 8 In the current study to eliminate some of the interfering factors with the enzyme activity, we only included men who were medically healthy according to their medical history and liver function test. We measured the enzyme activity pre- and postexposure in the individual. As the common OP agent used by famers was plasma ChE sensitive, the change in the activity of plasma ChE was measured. Additionally, a previous study suggested that plasma ChE activity is a more reliable and has lower variability and thus RBC ChE is preferred for monitoring purposes. 10
Conclusion
Exposure to OP pesticide is a major concern in the Northern Province, one of the main agricultural regions of Iran. More than 50% reduction in the plasma ChE activity is an alarming sign for further workplace evaluation. Routine ChE activity measurement in a reference laboratory in the province is recommended to determine the accurate extent of exposure. The appropriate training and education to exposed individuals in regard to handling, and application of these agents in the workplace, symptoms of toxicity, and prevention are important initial steps to avoid the toxicity or reduce the severity of poisoning. Due to easy access to these materials, intentional toxicity to this compound also needs to be taken into consideration by health professional. It should also be noted that many of the toxicity cases may arise from exposure to vegetable exposed with this toxins. Thus, appropriate washing with copious amount of water before usage of these vegetable is recommend.
Footnotes
Conflict of Interest
The authors declared no conflicts of interest.
Funding
This study was financially supported by a grant from Pharmaceutical Sciences Research Center, Mazandaran University of Medical Science, Iran.
