Abstract
Introduction:
Carbon monoxide (CO) is one of the leading causes of poisoning; it inhibits oxygen delivery, subsequently causing ischemic changes and ultimately death by multiorgan failure. Furthermore, thromboembolic episodes due to CO poisoning have been reported. However, intracardiac thrombus formation following exposure to CO has been very rarely described. Here, a case of right atrial large thrombus formation after CO poisoning is presented.
Case presentation:
A previously healthy 24-year-old woman was referred for CO poisoning. She has attempted suicide, and her initial mental status was drowsy with focal memory loss. Her initial CO fraction was 16%, and initial laboratory data showed creatinine kinase-myocardial bound of 90.6 ng/mL (upper limit 5 ng/mL) and troponin I of 1.899 ng/mL (upper limit 1.5 ng/mL). A transthoracic echocardiography was performed 24 h after the accident, revealing a 30 × 15 mm nodular echogenic mass in the right atrium. Anticoagulation with low-molecular-weight heparin was started along with hyperbaric oxygen therapy. After 7 days of heparinization, the large thrombus in right atrium had resolved.
Conclusion:
This report describes an intracardiac thrombus formation induced by CO poisoning. Because intracardiac thrombus can result in pulmonary embolism and cerebral embolic infarction, its consideration following CO poisoning is important.
Introduction
According to the Centers for Disease Control and Prevention, in the United States, 50,000 patients were admitted annually to the emergency department due to carbon monoxide (CO) poisoning, 1 with approximately 2700 annual deaths from this condition. 2 In addition, CO inhalation is one of the leading methods of suicide in the United States. 3
Although the exact toxic mechanism following exposure to CO remains unclear, the major cause of death is multiorgan failure and encephalopathic brain death by tissue hypoxia. 4 Because the affinity of carboxyhemoglobin is 200 times higher than that of oxyhemoglobin, CO poisoning causes a leftward shift in the oxyhemoglobin dissociation curve. 5 In addition, the release of oxygen free radicals, cellular apoptosis, and atherogenesis are important mechanisms of CO toxicity. 4 Therefore, CO poisoning may cause thromboembolic episodes in several systemic organs such as the heart, mesenteric artery, brain, and skin. 6 However, few reports exist on intracardiac thrombus formation following CO poisoning. In this report, we describe a rare case of intracardiac thrombus formation after severe CO intoxication.
Case presentation
A previously healthy 24-year-old woman was referred to the emergency department for CO poisoning. She had been found at a motel with a burning and smoking coal briquette. She had attempted suicide and was transferred to the nearest hospital; her initial mental status in the other hospital was drowsy with focal memory loss, and her initial CO fraction was 16%. With prompt oxygen supply, she was referred to our hospital which is a tertiary university hospital for hyperbaric oxygen therapy.
In the initial evaluation at our institution, the patient’s blood pressure was 132/101 mmHg, pulse was 87 beats/min, respiration rate was 20 breaths/min, body temperature was 35.4°C, and oxygen saturation of peroxymeter (SpO2) was 100% under 100% oxygen supply. When she arrived at our hospital, her mental status was alert with a Glasgow Coma Score of 15.
In the initial laboratory tests, a fraction of CO (carboxyhemoglobin (COHb)) of 1.0%, lactic acid of 1.7 mmol/L, Partial oxygen tension in arterial blood (PaO2) of 380.0 mmHg, creatinine kinase of 3306 IU/L (reference range 50–250 IU/L), Creatinine kinase-myocardial bound of 90.6 ng/mL (upper limit 5 ng/mL), troponin I of 1.899 ng/mL (upper limit 1.5 ng/mL) and blood glucose level of 107 mg/dL were observed. In addition, including coagulation tests, other laboratory data were not significantly abnormal. Urine pregnancy test was also negative. No abnormal findings except QT prolongation (corrected QT interval was 500 ms) were seen by electrocardiograph.
After initial hyperbaric oxygen therapy, a transthoracic echocardiography (TTE) was performed 24 h after the accident. The patient’s ejection fraction was 42%, and she presented apical grade 3 akinesia, ischemic insult of left anterior descending territory, and a 30 × 15 mm nodular echogenic mass in the right atrium (RA). When TTE was performed, COHb was already normalized (1.0%). Multidetector-computed tomography (Figure 1) was conducted on the same day to rule out coronary artery disease. Cardiac magnetic resonance image (MRI) (Figure 2) and transesophageal echocardiography were performed for RA mass evaluation on the following day. No coronary stenosis was found, and the nodular mass was a thrombus in the RA appendage. There were not any findings of myocarditis or myocardial infarction on the cardiac MRI.
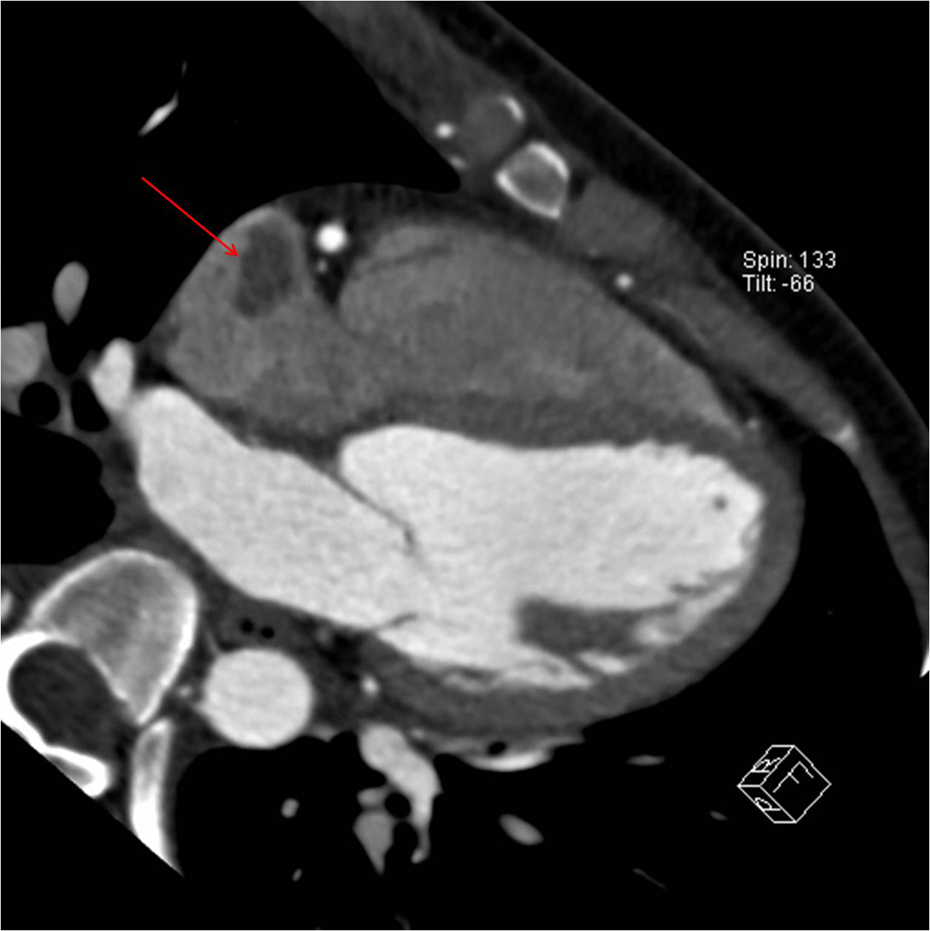
Multidetector-computed tomographic finding of intracardiac thrombus (arrow) in right atrium.

Cardiac magnetic resonance image (TI600) of intracardiac thrombus (arrow) in right atrium.
Anticoagulation with low-molecular-weight heparin (enoxaparin 1 mg/kg subcutaneous injection, twice per day) was commenced and three additional rounds of hyperbaric oxygen therapy (2.5 atmospheres and 90 min per round, once a day) were administered. After the levels of cardiac enzyme decreased and normalized, we conducted a follow-up TTE. Within 7 days of heparinization, the large thrombus in the RA disappeared and heparinization was therefore terminated. In the followed electrocardiograph, although QT interval was normalized, diffuse T-wave inversion was found and permanently remained. Without any other medical complications, the patient was referred to the psychiatric department for management of depression and suicide tendencies. After 5 days of psychiatric management, she was discharged without any further problems.
Discussion
Although thromboembolic accidents following CO poisoning are not uncommon, intracardiac thrombus formation is very rare with only two cases reported previously in the literature in English by Yildirim et al. 7 and Lee et al. 8 (Table 1). Because intracardiac thrombus can cause embolic infarction in vital organs such as the lung, brain, and kidney, its management is very important.
Clinical features of three cases of intracardiac thrombus formation following CO poisoning.

CK-MB: Creatinine kinase-myocardial bound; RBBB: Right bundle branch block; RWMA: Regional wall motion abnormality; EF: Ejection fraction.
The pathophysiologic mechanisms underlying thrombus formation by CO poisoning are not fully understood. CO poisoning activates nitric oxide and other oxygen free radicals. 5 Oxygen free radicals can alter platelet aggregation and blood flow, contributing to endothelial damage. 9 Moreover, free oxygen radicals inhibit endothelium-derived relaxation factor and prostacycline production by influencing vessel tone and platelet function. 10 Other pathogenic effects by free radicals include increases in platelet stickiness, polycythemia, and alterations of the fibrinolytic pathway. 11 Endocardial ischemic injury following CO poisoning can induce intracardiac thrombus formation, especially in cases of stress-induced cardiomyopathy or dysrhythmias such as atrial fibrillation.
In our present case, the patient did not have any previous medical history of coagulation; she was a non-smoker and not pregnant. Because of her cardiac enzyme elevation, we performed a TTE for cardiac evaluation. After the right atrial mass was detected incidentally and confirmed by transesophageal echocardiography, we conducted an MRI to rule out the cardiac tumor. The MRI revealed a large thrombus; we therefore commenced heparinization to prevent aggravation of thrombus formation. In contrast to the two previously reported cases of cardiac thrombus, we continued heparinization for 7 days and combined hyperbaric oxygen therapy. After 7 days of therapy, the thrombus disappeared completely. If the thrombus migrated to another site, then it would be caught in the pulmonary artery. Because the patient was asymptomatic, it is unlikely that the thrombus migrated to the pulmonary artery. We believe that the clot was dissolved by natural thrombolysis, with further thrombosis prevented by heparinization.
CO poisoning management (e.g. hyperbaric oxygen therapy) recovers normal fibrinolytic activity. In addition, anticoagulation therapy may also affect this pathway. Multiorgan failure following CO poisoning is known to occur because the high affinity of CO to hemoglobin reduces oxygen delivery, causing tissue hypoxia. Because of cardiac enzyme elevation and electrocardiographic change, we believe that our case also had myocardial infarction by CO poisoning without coronary stenosis. In addition, thromboembolic accidents induced by CO poisoning are associated with high morbidity and mortality. However, there is yet no consensus for the evaluation and management of cardiac thrombus following CO intoxication. Therefore, additional cases and studies are required to investigate the diagnosis and duration of anticoagulation therapy.
Conclusion
CO poisoning causes various harmful cardiac effects by disturbing oxygen delivery. Moreover, it can enhance coagulation pathways. This report describes the formation of an intracardiac thrombus induced by CO poisoning and reviews two similar previous reports. Because intracardiac thrombus can cause pulmonary embolism and cerebral embolic infarction, its consideration following CO poisoning is important. Further studies on the evaluation and management of intracardiac thrombus after exposure to CO are required.
Footnotes
Conflict of interest
The authors declared no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
