Abstract
Alocasia, the Araceae family, is a genus of more than 100 species of perennial, herbaceous, diminutive to extremely large, usually robust herbs with a clear-to-milky latex. They are distributed throughout subtropical and tropical Asia and in the tropical western pacific as well as eastern Australia. Despite easy access to A odora, there have been no published reports in English regarding the toxic symptoms following the ingestion of raw A odora. Here, the clinical manifestations of 2 patients that ingested raw A odora are described. Two patients experienced oral numbness and intractable tongue pain, and 1 patient required endotracheal intubation because of upper respiratory tract obstruction. Although conservative treatment is the primary approach to A odora poisoning, physicians should be aware of the potential for upper respiratory obstruction in patients exposed to A odora, as well as the need for controlling tongue pain.
Introduction
Most genera of the Araceae Family contain calcium oxalate crystals; their needle shape can cause anything from minor skin irritations to total loss of vision as well as death, if enough is consumed. Alocasia, Arisaema, Caladium, Colocasia, Dieffenbachia, and Philodendron belong to this family. 1 The ingestion of Dieffenbachia and Philodendron are the most well-known in terms of their medical toxicity, which can manifest as mild edema of the mouth to airway obstruction and death; however, extreme complications are uncommon.2–4 Colocasia and Alocasia are commonly referred to as the “Elephant’s Ear” plant due to the large leaves and striking appearance. The patients exposed to Colocasia show mild symptoms, including pain of the mouth or tongue and hypersalivation or no symptoms.5,6
Alocasia is a genus of more than 100 species of perennial, herbaceous, diminutive to extremely large, usually robust herbs, with a clear-to-milky latex. 7 They are distributed throughout subtropical and tropical Asia and in the tropical western pacific as well as eastern Australia. 7 Because it is such a common ornamental plant, it may be frequently involved in accidental or intentional poisoning.
Alocasia odora (A odora), a widespread and common Alocasia, has a height of about 2.5 m, a stem erect to decumbent, and large leaves clustered at the tips of the stem. 7 It has also been referred to as the night-scented lily, giant upright elephant ear, and is commonly known in Vietnamese as bac ha. It is used as a green vegetable in Southeast Asian cuisine. Its rhizomes are used to treat abdominal pain, cholera, hernia, stomach ache, pulmonary tuberculosis, as well as snake and insect bites in China.7,8 In South Korea, A odora along with Alocaisa cucullata (A cucullata) are popular as ornaments. Despite easy access to A odora, there have been no published reports in English regarding the toxic symptoms following the ingestion of raw A odora. Here, the clinical manifestations of 2 patients that ingested raw A odora are described.
Case 1
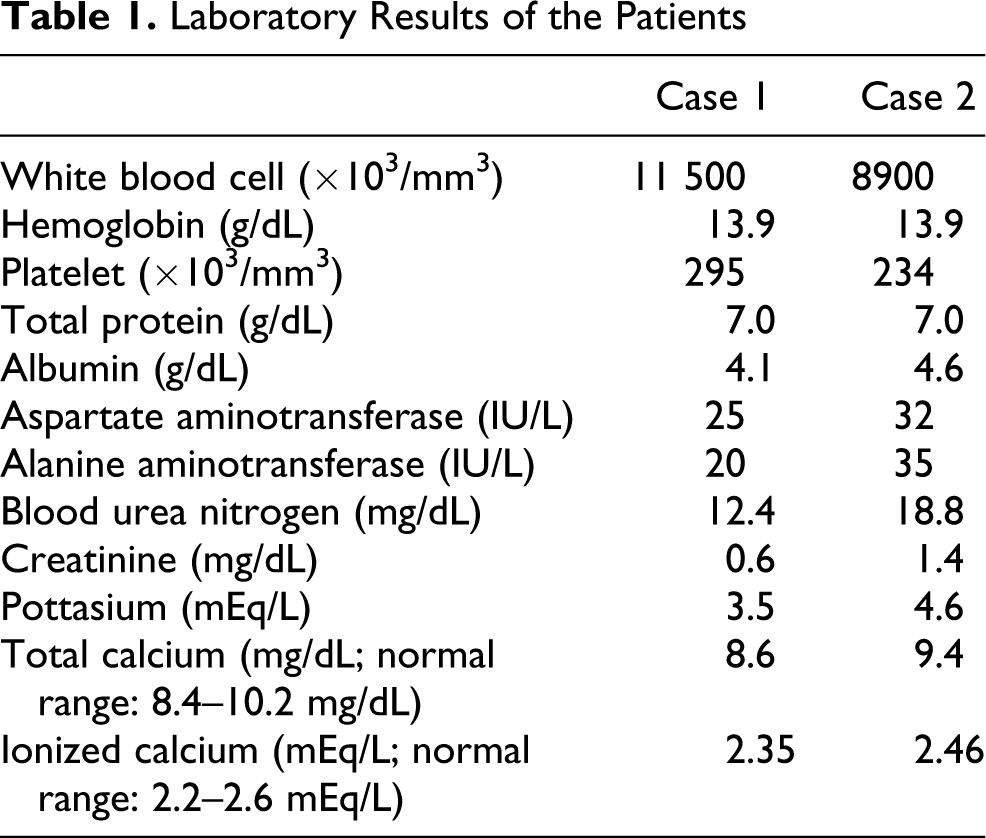
A 43-year-old woman presented with oral numbness, hoarseness, dyspnea, and a filling sense in the throat. The family reported that she bit the root stock of a plant but spit it out instantly, while in an inebriated state 2 hours before presentation. The plant was displayed as an ornament. On arrival, the vital signs were as follows: blood pressure 110/70 mmHg, heart rate 120/min, and respiratory rate 29/min. The patient was oriented and showed no focal neurological deficits. Endotracheal intubation was performed and the physician performing the intubation noted a swollen uvular and epiglottis. Intravenous administration of 4 mg of chlorpheniramine and 125 mg of methylpredinisolone were provided. Laboratory examinations such as liver function tests, blood urea nitrogen (BUN), creatinine, and calcium levels, were all within normal range, except a mild leukocytosis (Table 1 ). The chest x-ray showed no abnormal findings. The family brought the plant to the hospital. An expert in the department of Agriculture at the university was contacted and confirmed that the plant was A odora (Figure 1 ).
Laboratory Results of the Patients

Root stock of Alocasia odora which the patient ate.
After 12 hours of observation, the patient was extubated; there was mild swelling of the arytenoids and epiglottis on flexible laryngoscopy. The patient continued to complain of oral numbness and severe tongue pain, which was uncontrolled by 75 mg of intramuscular diclofenac sodium and prevented eating 24 hours after presentation. The patient was transferred to a local hospital close to home to receive nutritional support and pain control.
Case 2
A 50-year-old man presented with oral numbness, pain of the tongue, and nausea. The patient reported tasting the raw root stock of an ornamental plant 2 hours before presentation. The plant was brought to the emergency department and it was confirmed to be A odora based on the previous experience with case 1.
On arrival, the vital signs were as follows: blood pressure 140/90 mmHg, heart rate 88/min, and respiratory rate 18/min. The throat looked slightly inflamed. The level of calcium was within normal range as were the other laboratory tests (Table 1). Treatment with intravenous metoclopramide-HCl reduced the nausea. However, the patient complained of severe unresolved tongue pain despite the administration of morphine. The patient went home 7 hours after presentation against medical advice.
Discussion
Despite the many plants in the Alocasia genus, and its wide geographical habitat, there have been very few reports on its toxicity in humans. There are 2 reports on intoxication after exposure to raw Alocasia macrorrhiza (A macrorrhiza).8,9 It is commonly called elephant ear taro. The stems of A macrorrhiza were traditionally eaten as a starchy food in tropical Asia during times of famine. 7 It contains 16%–21% of starch and is low in protein. 10 It is thought to have once been a major staple food in Micronesia that became extinct there prior to the introduction of the related taro species (for example Colocasia esculenta).7,11 The stems were boiled in water or with added coconut milk, lightly salted, and served. 12 In addition, A macrorrhiza has been used medicinally. The plant juice mixed with vinegar and ginger was used to heal snake, bee, and insect bites in China. 13 In the Philippines, the leaf stalks have been used to relieve toothaches and the roots and leaves have been used to relieve pain and redness in Java. 12 Today, A macrorrhiza is now found in pan-tropic locations as an ornamental plant. It has also shown promise in sewerage treatment, as it grows rapidly in wetland conditions and has a propensity to accumulate metal contaminants such as zinc. 14 It is very similar to A odora. However, A odora has slightly peltate leaves, and proportionately a much shorter spadix appendix. 7 Chan et al. reported that a patient experienced oral numbness and abdominal pain after ingesting the raw root of A macrorrhiza and the symptoms persisted for 3 days. 8 Lin et al. reviewed 25 patients that consumed a portion of raw or cooked A macrorrhiza. 9 The most common symptom was sore throat followed by oral numbness, salivation, dysphonia, abdominal pain, and ulcers of the oral cavity, similar to our cases. Most of the symptoms subsided within a week; however, numbness of the mouth tended to last more than 1 week. They suggested that the calcium oxalate that is distributed throughout the entire plant might be the cause of local inflammation and symptoms.
A cucullata is found in Sri Lanka and Taiwan. 7 It is smaller than 1 m in height, has many branched stems, and broadly ovate lamina. In China, all parts are used externally for treatment of snake bites, abscess, and rheumatism. 7 Two fatal cases after ingestion of the A cucullata fruit had clinical manifestations including liver impairment, metabolic acidosis, and arrhythmia, consistent with cyanogenic glycoside poisoning. 15 Although cyanide could not be demonstrated in the tissue post-mortem, the cyanide component was thought to be the main cause of the fatalities. However, Goonasekera et al. demonstrated that the quantities of hydrogen cyanide liberated from the A cucullata fruit were not sufficient to cause toxic symptoms, and the 2 fatal cases were unlikely to have died due to cyanide poisoning. 16
Even though the chemical composition of A odora has not been sufficiently investigated, it is known that A odora has insoluble calcium oxalate, saponin, and alocasin. 8 Direct mucocutaneous contact or the eating of raw or inadequately boiled plants may result in poisoning. 8 The patients reported here were exposed to raw A odora and showed locally irritation; the symptoms were similar to A macrorrhiza toxicity. The saponin and/or calcium oxalate may cause the local irritant symptoms such as oral numbness and tongue pain. An insoluble calcium oxalate crystal shaped like needles is contained in the plant and it may mechanically damage cells following ingestion and cause the clinical signs. 17 In addition, the damage to cells may provide a cellular entrance for other toxins. The proteolytic enzymes, which trigger the release of potent kinins and histamines by the body, could be attributed to toxicity and the calcium oxalate may aggravate this toxicity. 18 It is well-known that saponin, insoluble like calcium oxalate, can irritate the gastrointestinal tract, and a large amount can cause respiratory failure or cardiac dysfunction. 8 However, the specifics of Alocasia toxicity remain unclear.
Conservative treatment is the primary approach to Alocasia poisoning; there is no specific antidote. To reduce oral pain, drinking 120–240 mL of ice water has been recommended. 9 After ingesting the plant, drinking milk may be helpful in order to precipitate soluble oxalate by combining it with calcium. 19 Inducing vomiting and gastric lavage have not been recommended in cases with severe ulcerative damage of the gastrointestinal tract. 9 For the patient exposed to A macrorrhiza, amyltriptline was administered. However, the effects could not be evaluated because the symptoms were already improving prior to administration. 8 If necessary, for the pain, systemic analgesics may be recommended similar to the cases reported here rather than a topical anesthetic because of the concerns with regard to bite injuries of the tongue following excessive local anesthetic effects. 1 In case 1, antihistamine and steroid were provided in order to reduce the edema of the larynx. We did not assess whether these medications were effective in treating the edema because of the retrospective design. However, the administration of antihistamine is controversial for the management of Araceae family poisoning because some studies failed to show a protective effect of antihistamine and the involvement of histamine in edema remains unclear. 20 The pretreatment with antihistamine failed to reduce the edema of the tongue in guinea pigs exposed to Dieffenbachia, a member of the Araceae family. However, some studies have shown a protective effect in animals. 21 Fochtman et al. found that corticosteroid only delayed onset of the inflammation reaction in an animal study of Dieffenbachia poisoning. 18 In a clinical study, antihistamine and corticosteroid treatment did not alter the clinical course in patients exposed to Dieffenbachia. 2
In addition, the physician should evaluate the swelling of the pharynx because of the risk for upper respiratory obstruction caused by irritation; especially in patients exposed to A odora.
Despite the fact that calcium oxalate is insoluble, large amounts of calcium oxalate can be dissolved in the stomach to form oxalic acid, which combines with calcium in the blood and may cause hypocalcemia as well as renal and hepatic impairment. After ingesting a considerable amount of Alocasia, the patient should be monitored for hypocalcemia and related complications, such as muscle cramps, weak irregular pulse, hypotension, and cardiac arrhythmias. In this case, calcium chloride and gluconate should be given along with fluids.
Footnotes
There is no conflict of interest and there are also no copyright constraints.
This research received no specific grant from any funding agency in the public, commercial, or not for-profit sectors.
