Abstract
In the past decade, a lot of work has been reported on the use of polyvinylidene fluoride (PVDF) based thermoplastic composites as energy storage devices, and implant materials. But hitherto little has been reported on the dimensional stability and surface characteristics of 3D-printed PVDF composites after autoclaving for implant applications. In this study, the effect of autoclaving on surface characteristics (Shore-D hardness, surface roughness (Ra), morphological characteristics), and dimensional stability of 3D printed PVDF-hydroxyapatite (HAp)- chitosan (CS) composite has been reported for implant applications. The signal-to-noise (S/N) ratio approach was used to ascertain the best setting of process parameters for 3D printing by fused filament fabrication (FFF) process. This study suggests that the best setting for the FFF process, for the 3D printing of PVDF composite (90%PVDF-8%HAp-2%CS) are the nozzle temperature (NT) of 225°C, raster angle (RA) 0°, and printing speed (PS) 40 mm/s, resulting in Shore-D hardness 48.5 HD (before autoclaving) and 55.0 HD (after autoclaving), dimensional deviation 0.01 mm (after autoclaving). The results are supported by scanning electron microscopy (SEM) and Fourier transmission infrared (FTIR) spectroscopy analysis.
Keywords
Introduction
Fused deposition modeling (FDM) or FFF 1 is one of the established 3D printing processes, that uses a variety of thermoplastics/thermoplastic composites. This process entails stacking and fusing thermoplastic materials to produce three-dimensional objects. 2 Due to the better adaptability, affordability, and capacity for quick prototyping and manufacturing of complicated geometries, this process has attracted researchers in the fields of biomedical instruments, implant fabrication, aerospace, automobile, etc. 3 Utilizing computer-aided design (CAD) software, the procedure starts with the creation of a 3D model. After this, using slicing software, the model is divided into thin cross-sectional layers, which produce guidance for the 3D printer on how to construct each layer. 4 One of the main components of the FFF process is thermoplastic filaments made of polyethylene terephthalate glycol (PETG), acrylonitrile butadiene styrene (ABS), PVDF, and polylactic acid (PLA), etc. 5 Each material has unique strengths, flexibilities, temperature resistance, and aesthetic qualities. The thermoplastic composite 6 is extruded onto a construction platform layer by layer by the 3D printer using a heated nozzle. The sliced model gives the nozzle instructions on how to travel along the X, Y, and Z axis. 7 The temperature of a heated bed of a 3D printer promotes adherence to the initial layers. As the filament is extruded in layers, each layer fuses with the one before it cools and hardens. The correct bonding between layers is ensured by the printer's exact control of the platform and nozzle temperatures.7,8 Temporary bases can be generated to avoid material drooping during printing when overhangs or complicated geometries are present. Following the completion of the print, these supports are taken out. 9
In typical biomedical/implant applications 10 to get rid of microbes, the autoclaving process is being commercially used, 11 which involves high-pressure saturated steam/high temperature as a sterilizing agent. 12 It is commonly utilized in the healthcare and pharmaceutical sectors, particularly for aseptic-condition equipment like implants, and prostheses. 13 In a typical autoclave setup, a specialized pressure vessel employs high temperature and pressure to ensure the eradication of bacteria, viruses, spores, and other microbes. Temperatures in autoclaves ranges from 100°C to 140°C. 14 Effective sterilizing depends on the greater pressures and temperatures that autoclaves can produce. The autoclave's steam-generated pressure boost helps to achieve temperatures over the boiling point of water. Depending on the required temperature, pressures may vary between 0.1 and 0.2 MPa. 15 To achieve total eradication of germs, the exposure duration at the appropriate temperature and pressure is essential. It depends on things like the microbial load and the type of item being sterilized. To remove any remaining moisture from the implant, tool, and medical equipment that has been sterilized, many autoclave cycles also include a drying phase. 16
After being inserted into the body, implants come into touch with tissues and biological fluids.17,18 By ensuring their sterility, germs that can cause serious infections or problems are kept out of the environment. Implants may be sterilized using the autoclave without losing their biocompatibility. 19 The material’s characteristics may be changed by harsh chemical processes, which would change how it interacts with the body. Post-operative infections can harm the patient’s health and recovery, although autoclaving dramatically lowers that risk. Since implants are medical equipment, they must adhere to strict regulatory guidelines, which suggest that there must be no microbial contamination on implants that might cause infections. 20 To maintain aseptic conditions, autoclaving efficiently eradicates even extremely resistant germs. Thermoplastics, metals, and biocompatible materials are used to make a lot of implants. Compared to more aggressive sterilization techniques, autoclaving maintains the materials’ structural and chemical integrity.21,22 The pressured steam in the autoclave provides even penetration into intricate geometries and porous objects, efficiently locating possible microbial hiding places. In comparison to less expensive options like ethylene oxide gas sterilization or gamma radiation sterilization, which might not be appropriate for all implant materials, autoclaving is a cost-effective sterilization technique. Autoclaving is more ecologically friendly than chemical sterilizing treatments since it uses heat and water, which don't produce any hazardous byproducts. 23
Dimensional stability is the capacity of a substance or item to preserve its initial form, size, and dimensions under a variety of circumstances, including temperature fluctuations, mechanical stress, humidity changes, and other environmental influences.24,25 Dimensional stability is critical in many domains and applications, particularly in those where accuracy, precision, and reliable performance are crucial. Dimensional stability is crucial in several important fields, including healthcare, manufacturing, engineering, etc. The normal anatomy of the patient must be smoothly incorporated into orthopedic implants. 26 Poor dimensional stability can cause changes in size or form, which can cause the implant to fit incorrectly, become unstable, or even fail. This may lead to discomfort, restricted movement, and the requirement for further procedures. To guarantee uniform weight distribution and natural mobility, orthopedic implants must transmit mechanical loads and stress effectively. Dimensional instability may result in a different load distribution, which might put too much stress on the bones and tissues nearby. 27 Dimensional stability is essential to guarantee that the personalized implant precisely meets the patient's needs and keeps its form over time. Orthopedic implants must adhere to stringent safety, functionality, and quality criteria, according to regulatory agencies. 28
The bibliometric analysis was performed with a Web of Science database of the last 20 years for the keywords autoclaving of the implant (Figure 1(a)). The bibliometric analysis and literature review revealed that in the past two decades, a lot of work has been reported on the use of PVDF-based thermoplastic composites as energy storage devices, and implant materials. But hitherto little has been reported on the dimensional stability and surface characteristics of 3D-printed PVDF composites after autoclaving for implant applications as shown in Figure 1(b). Some previously reported studies have recommended the use of 3D-printed PVDF-HAp-CS composite for biomedical applications,8,29–34 so there is a need to understand how the sterilization process affects the material’s dimensional stability for this composite. It may be noted that there are several sterilization techniques commonly used in the medical and biotechnology fields to ensure that materials, instruments, and devices are free from viable microorganisms. Some of the most prevalent sterilization methods are autoclaving, gamma irradiation, ethylene oxide sterilization, chemical sterilization, dry heat sterilization, filtration, and UV light sterilization. For the present case study dry heat sterlization method has been selected. In this study, the effect of autoclaving on surface characteristics (Shore-D hardness, Ra, and other morphological characteristics), and dimensional stability of 3D printed PVDF- HAp- CS composite has been reported for implant applications as an extension of previously reported studies.30,31 The tensile properties of PVDF composite (90%PVDF-8%HAp-2%CS) were reported as peak load 394.87 N, peak strength 33.92 MPa, Young modulus 2.606 MPa, modulus of toughness 0.484 MPa.
30
The compressive properties of PVDF composite were reported as peak load 1321 N, break load 1188.9 N, and strength at peak 10.83 MPa.
29
Torsional strength of PVDF composite was reported as 3.44 N-m at the angle of 0-800°.
31
In the present study S/N ratio approach was used to ascertain the best setting of process parameters for 3D printing (by FFF process). (a) Bibliometric analysis for the keywords “autoclaving of implants”. (b) Research gap for the keywords “sterilization method”.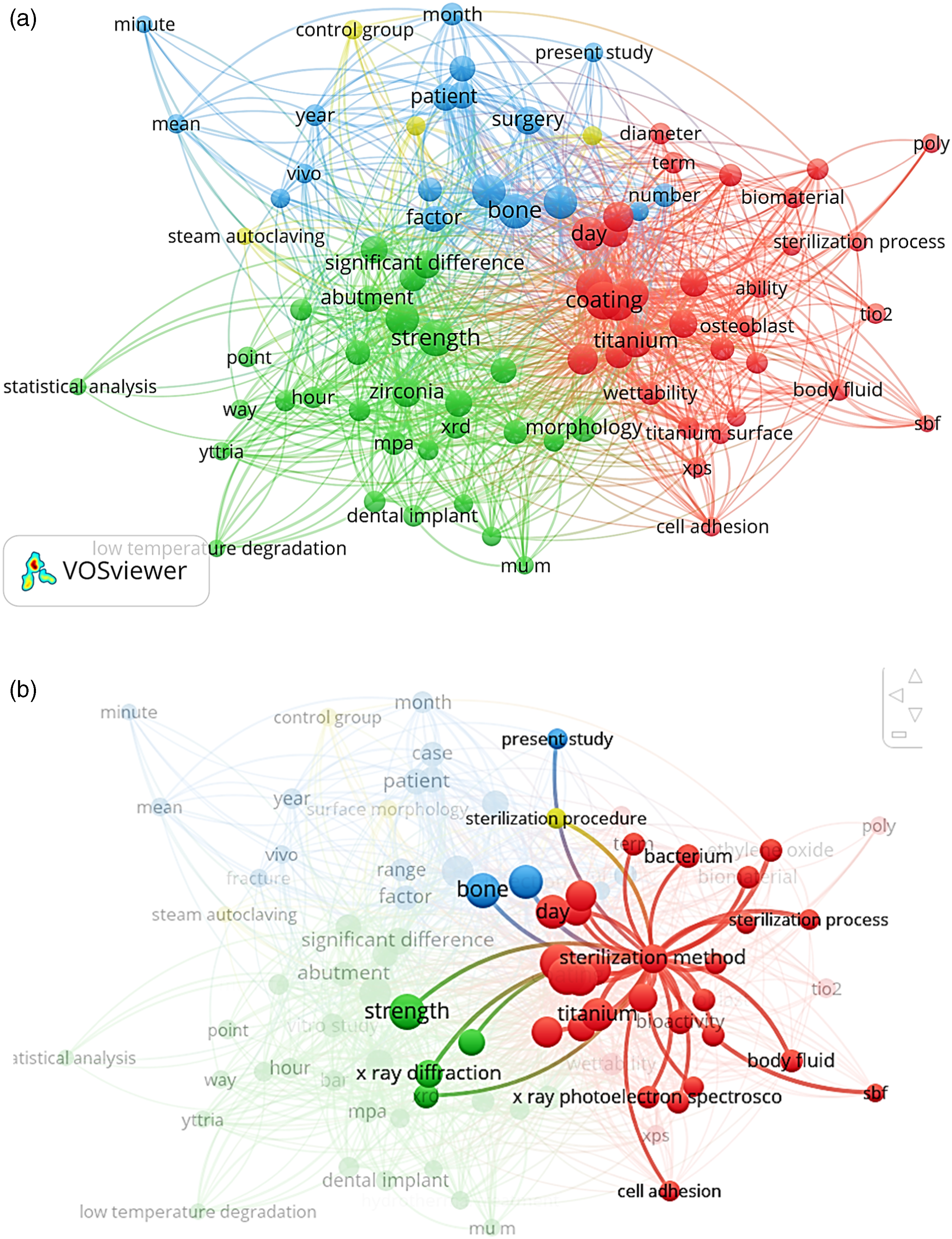
Materials and methods
The PVDF extrusion grade thermoplastic was procured in pallet form from a local market (Solvay, Gujarat, India). The pellet has a density of 1.75 g/cm3, a melting point between 200 and 210°C, and a glass transition temperature (Tg) of −40°C, respectively. The CS (degree of deacetylation 90%, PH 7.0–9.0) and HAp (colorless and brittle) were procured from Marine Hydrocolloids, Kochi, Kerala, India, (CAS number: 1306-06-5). The composition/proportion of the PVDF composite matrix was selected based on previously reported studies.29,31 The filament of PVDF composite (90%PVDF-8%HAp-2%CS) was fabricated on a single screw extruder (Figure 2(a)) at 7 r/min of screw speed and barrel temperature of 225°C.
31
The methodology adopted for this study is shown in Figure 2(b). The autoclave setup (supplied by Hally Instruments, Mumbai, India) was used in this study at a temperature range of 30 °C–250 °C, internal size of 45 × 45 × 50 cm. Filament fabrication process (a), adopted methodology (b).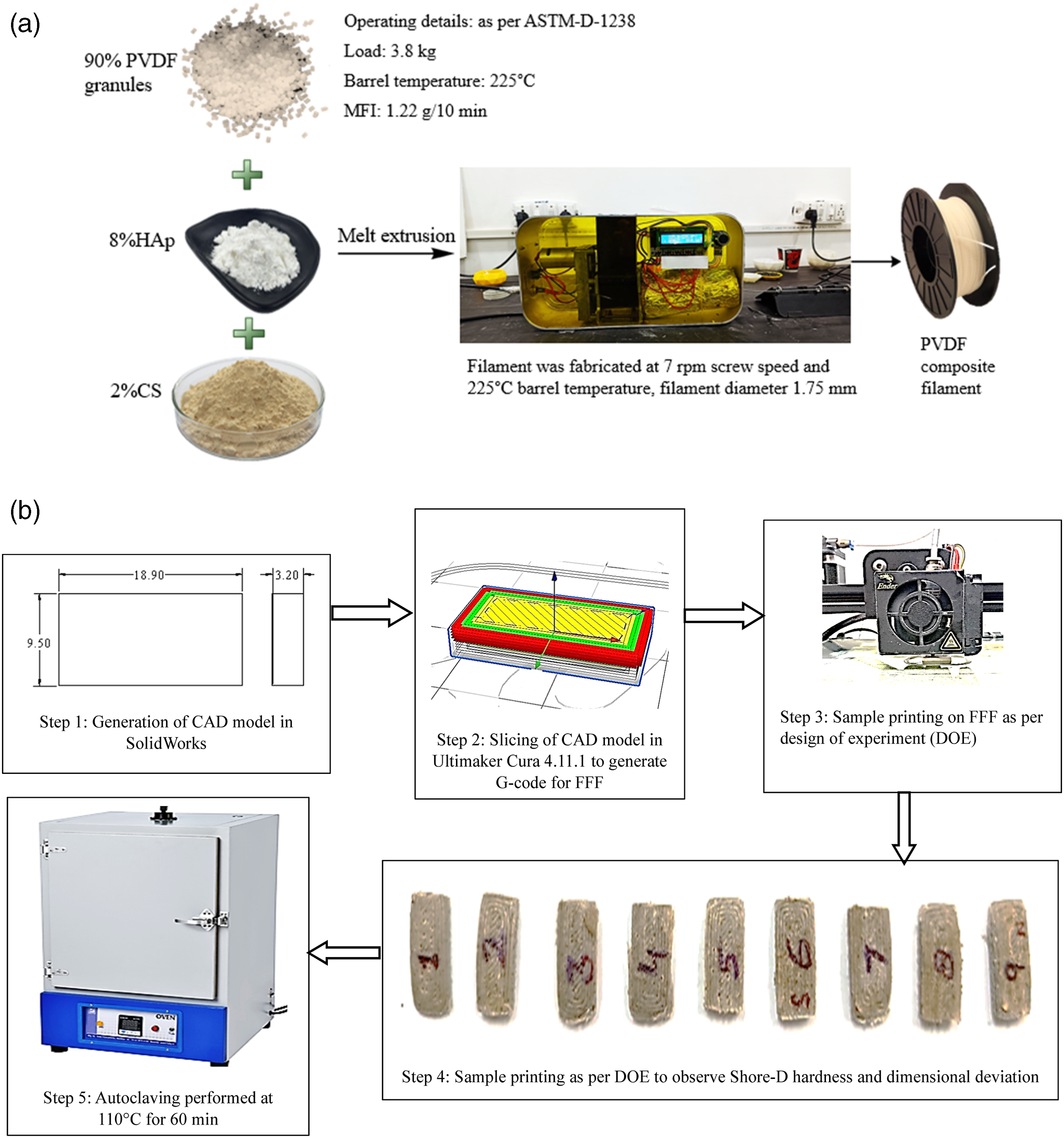
Factors and levels selected for the FFF process.

Shore-D hardness of the implant prototype PVDF composite before and after repeated cycles of autoclaving.
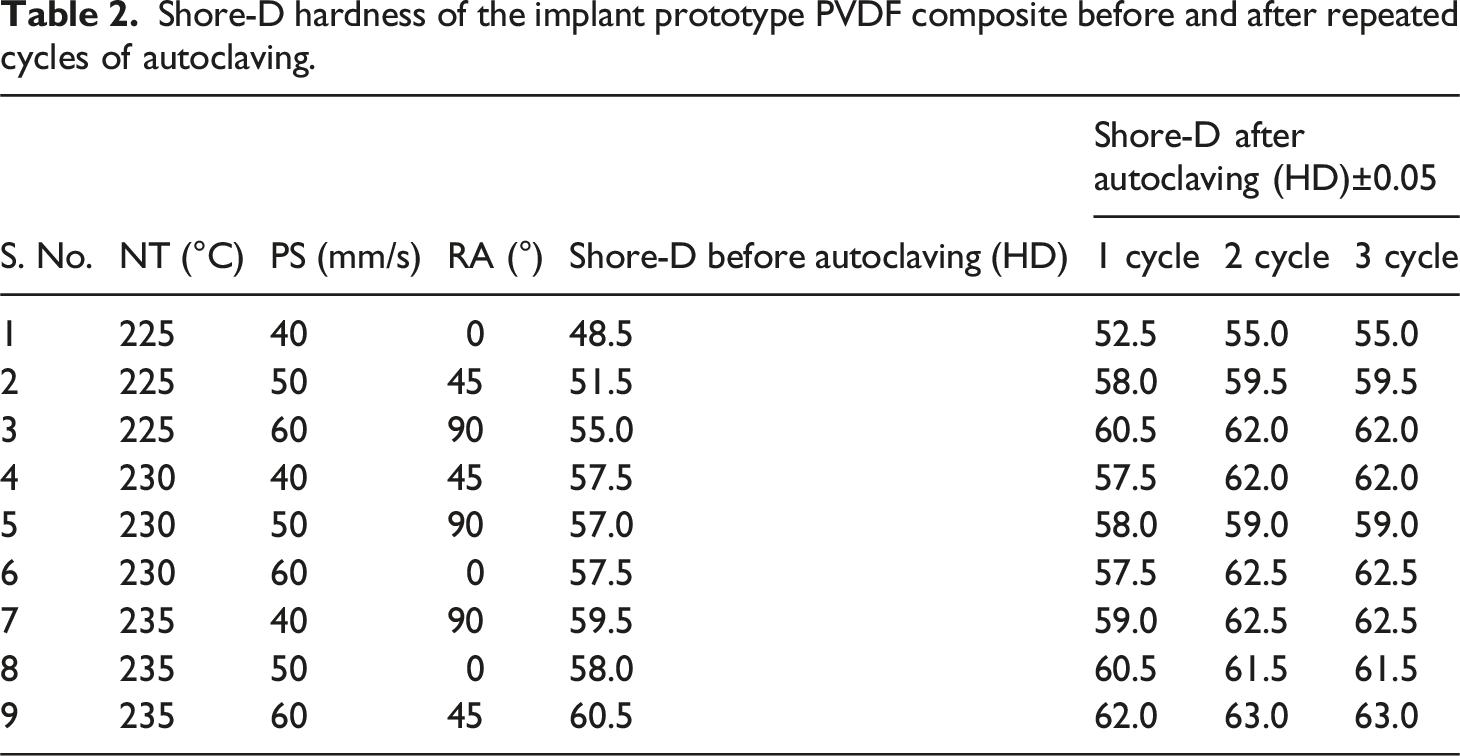
Nine sets of samples were printed as per Table 2 (with five repetitions) and surface hardness (Shore-D) was measured before and after (03 repeated cycles of autoclaving at 110°C for 60 min). The observations for Shore-D hardness are shown in Table 2.
Results and discussion
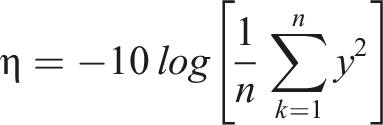
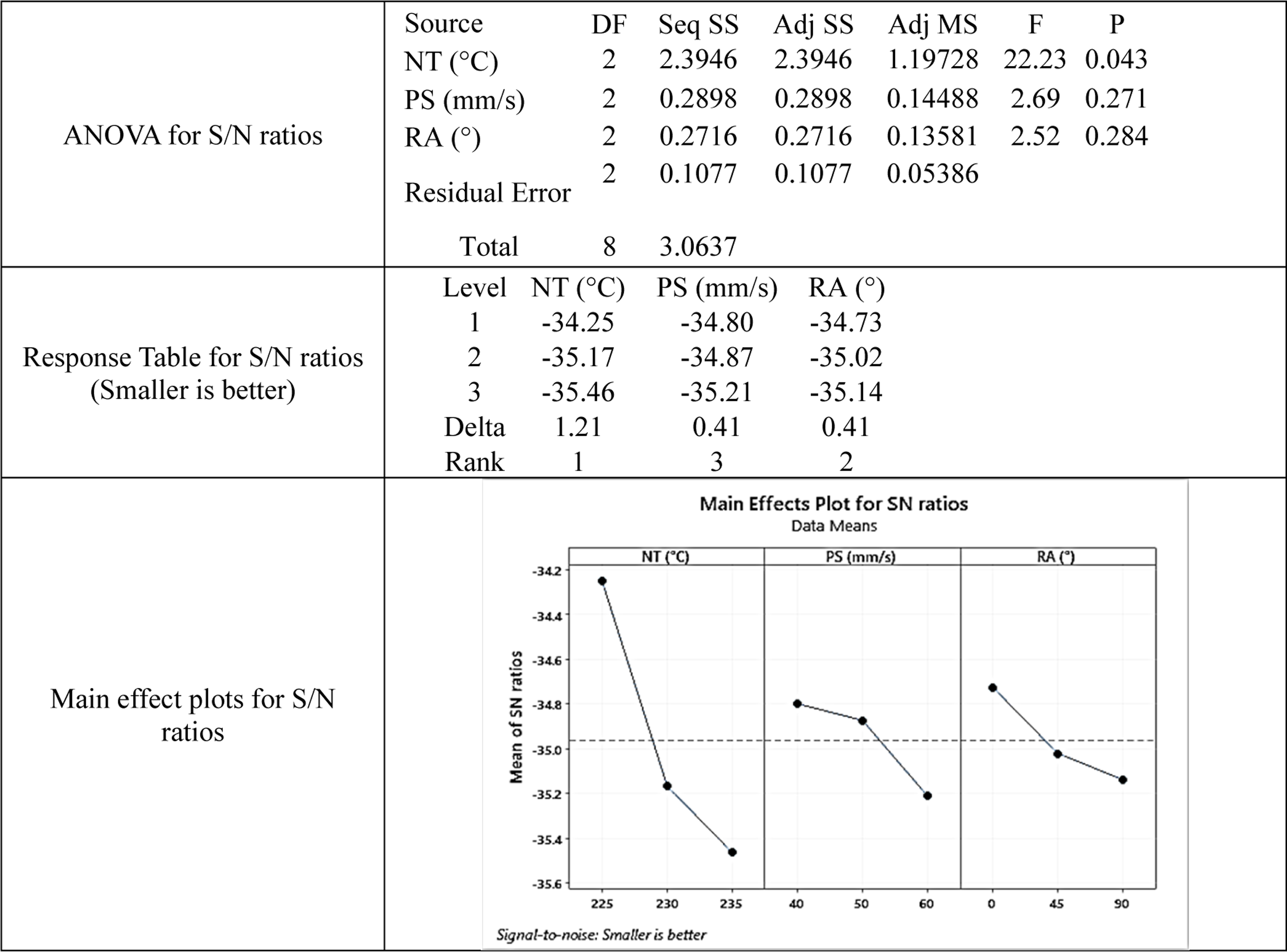
Shore-D hardness optimization (smaller is better).
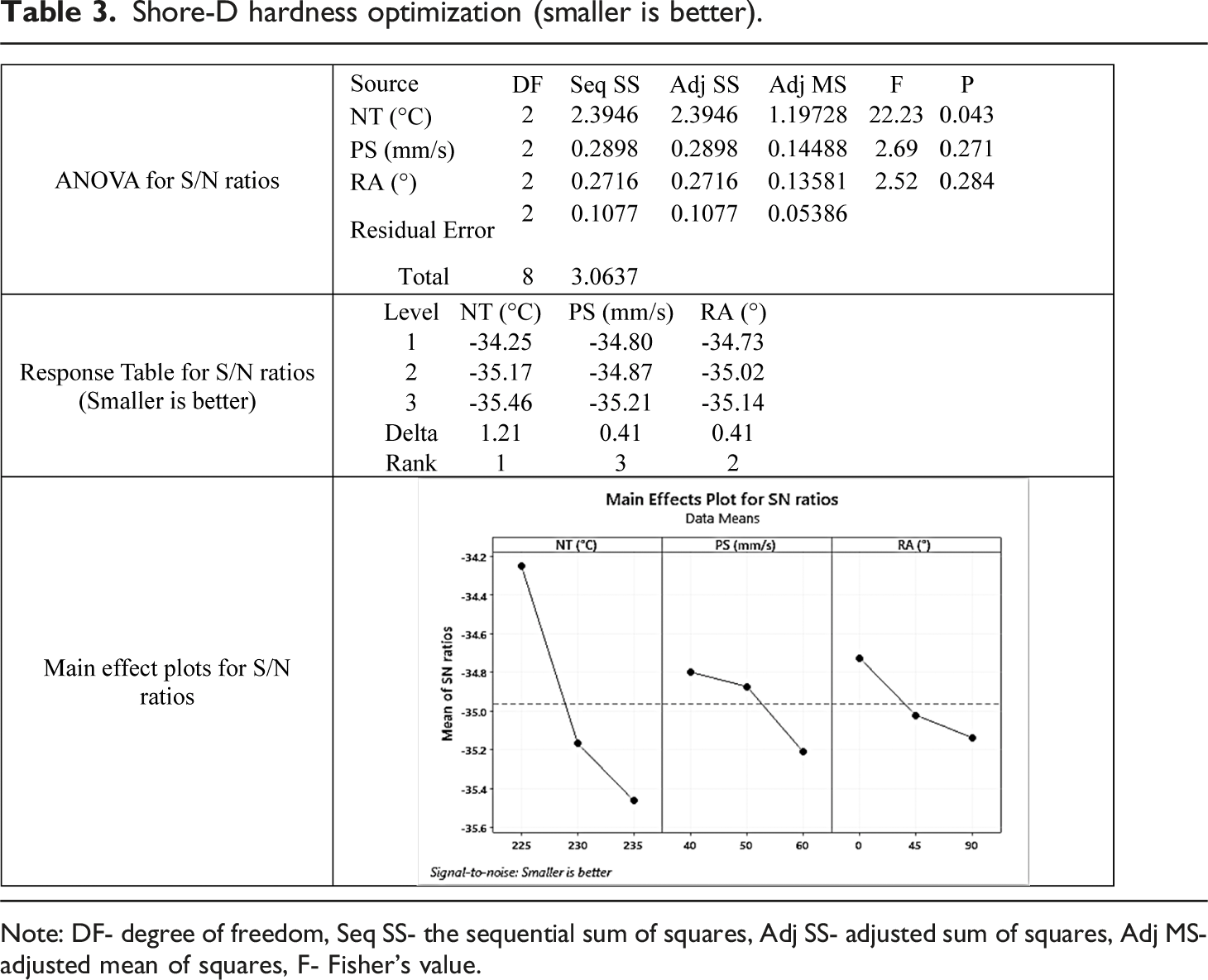
Note: DF- degree of freedom, Seq SS- the sequential sum of squares, Adj SS- adjusted sum of squares, Adj MS- adjusted mean of squares, F- Fisher’s value.
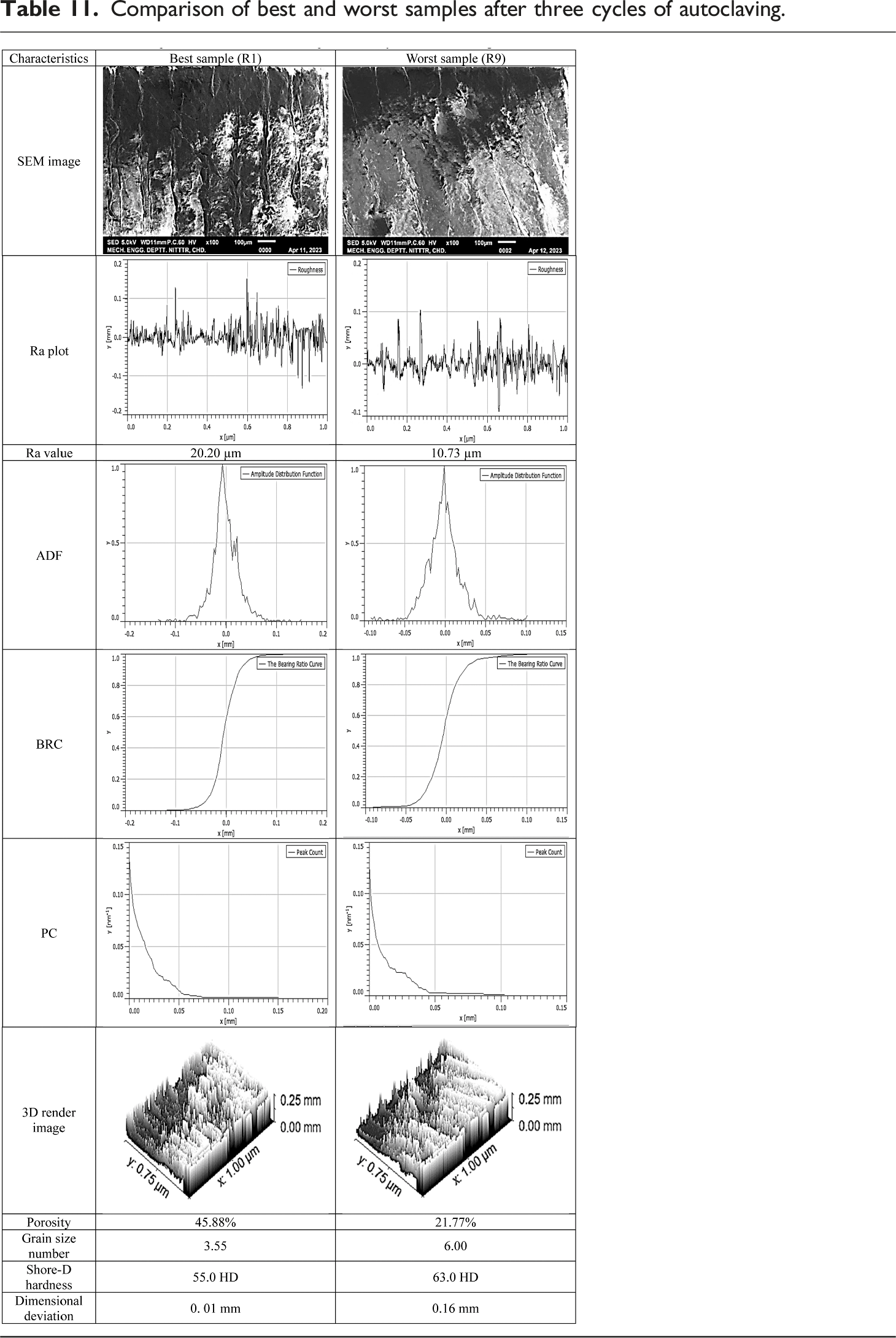
It was observed from the main effect plot (Table 3) that, with the increase in temperature Shore-D hardness also increases. This may be due to better layer adhesion with an increase in temperature. The same may be counter-verified by optical photomicrographs. Based on analysis of variance (ANOVA) analysis as per literature,3,5,12 NT was only found significant, having a probability (p)-value less than 0.05, and the best setting for minimization of Shore-D hardness is NT 225°C, PS 40 mm/s, RA 0°. Further, the best and worst sample was found as R1, and R9 respectively (Table 2).
Dimensional stability of PVDF composite-based implant prototype (before and after repeated cycles of autoclaving).
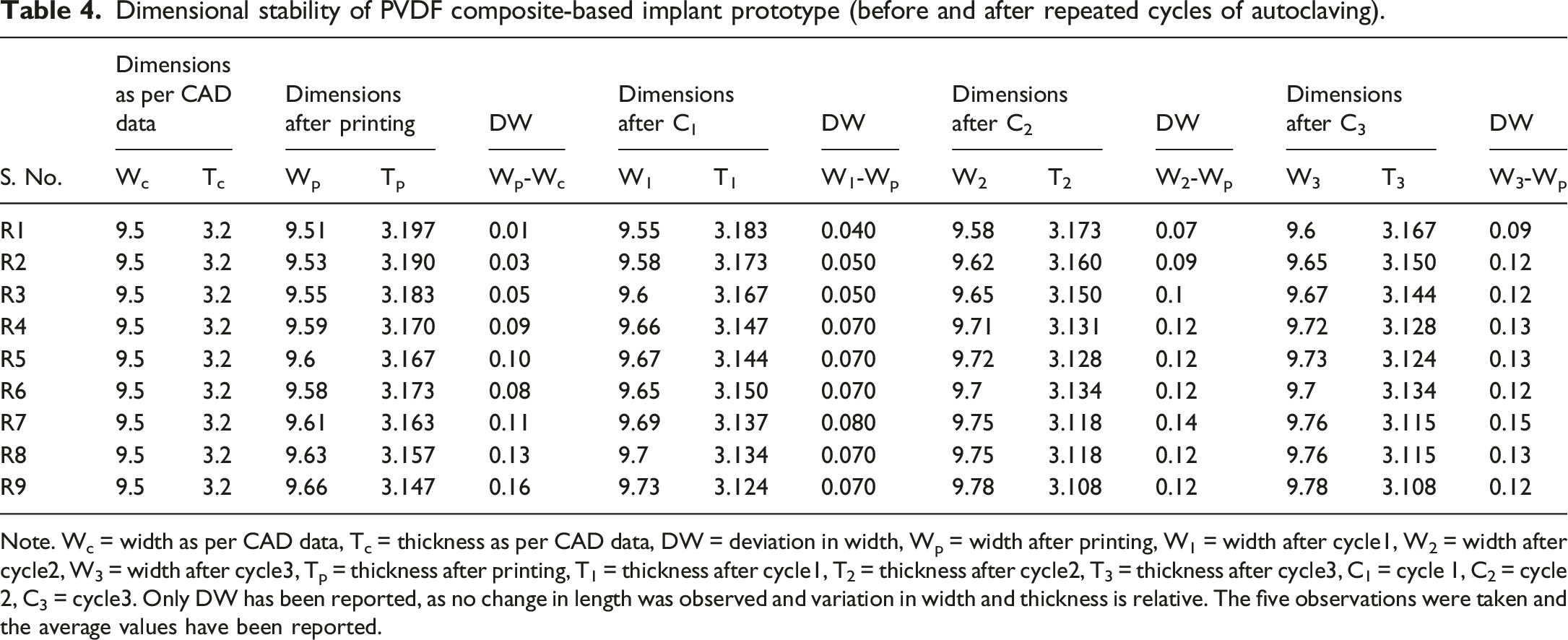
Note. Wc = width as per CAD data, Tc = thickness as per CAD data, DW = deviation in width, Wp = width after printing, W1 = width after cycle1, W2 = width after cycle2, W3 = width after cycle3, Tp = thickness after printing, T1 = thickness after cycle1, T2 = thickness after cycle2, T3 = thickness after cycle3, C1 = cycle 1, C2 = cycle 2, C3 = cycle3. Only DW has been reported, as no change in length was observed and variation in width and thickness is relative. The five observations were taken and the average values have been reported.
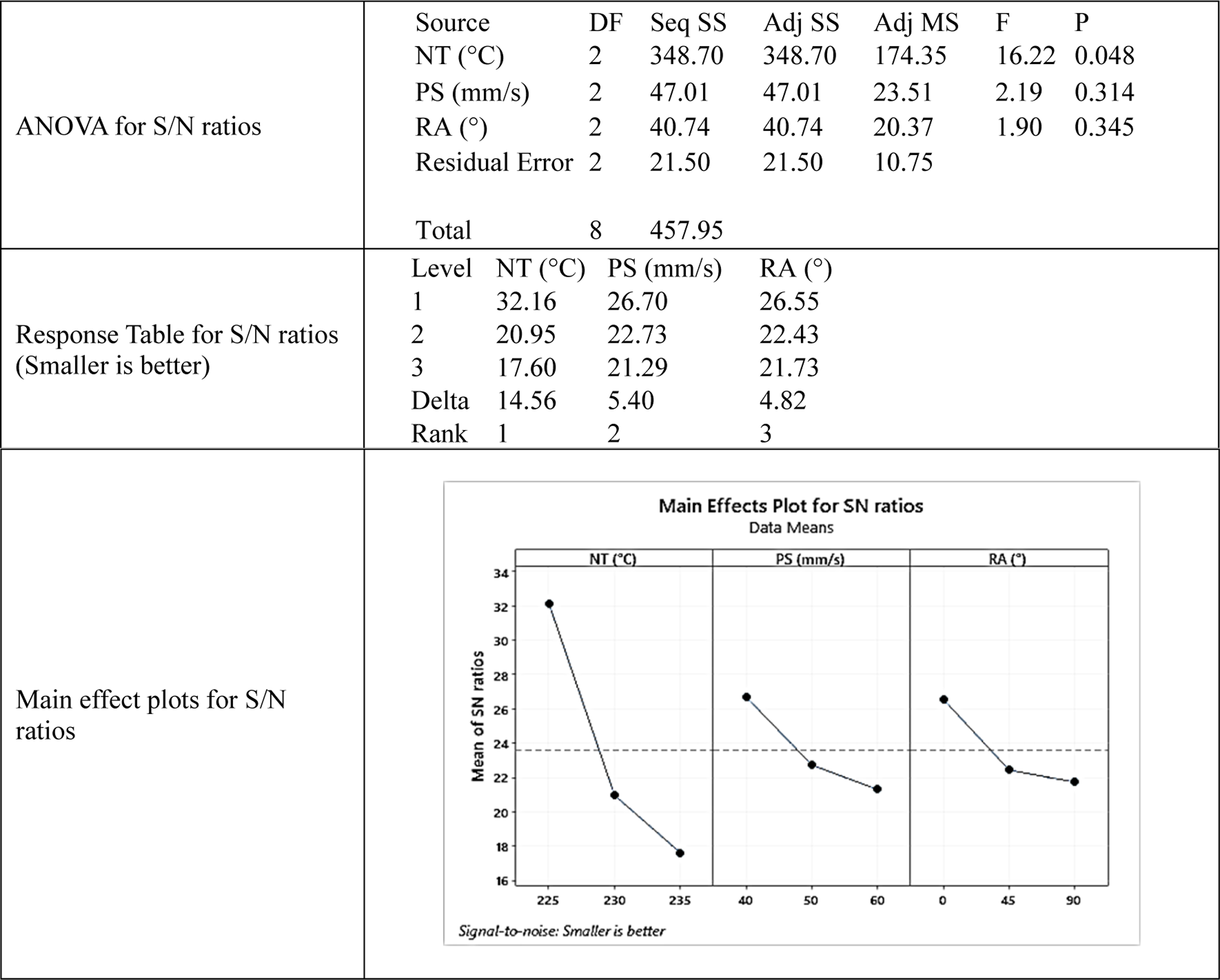
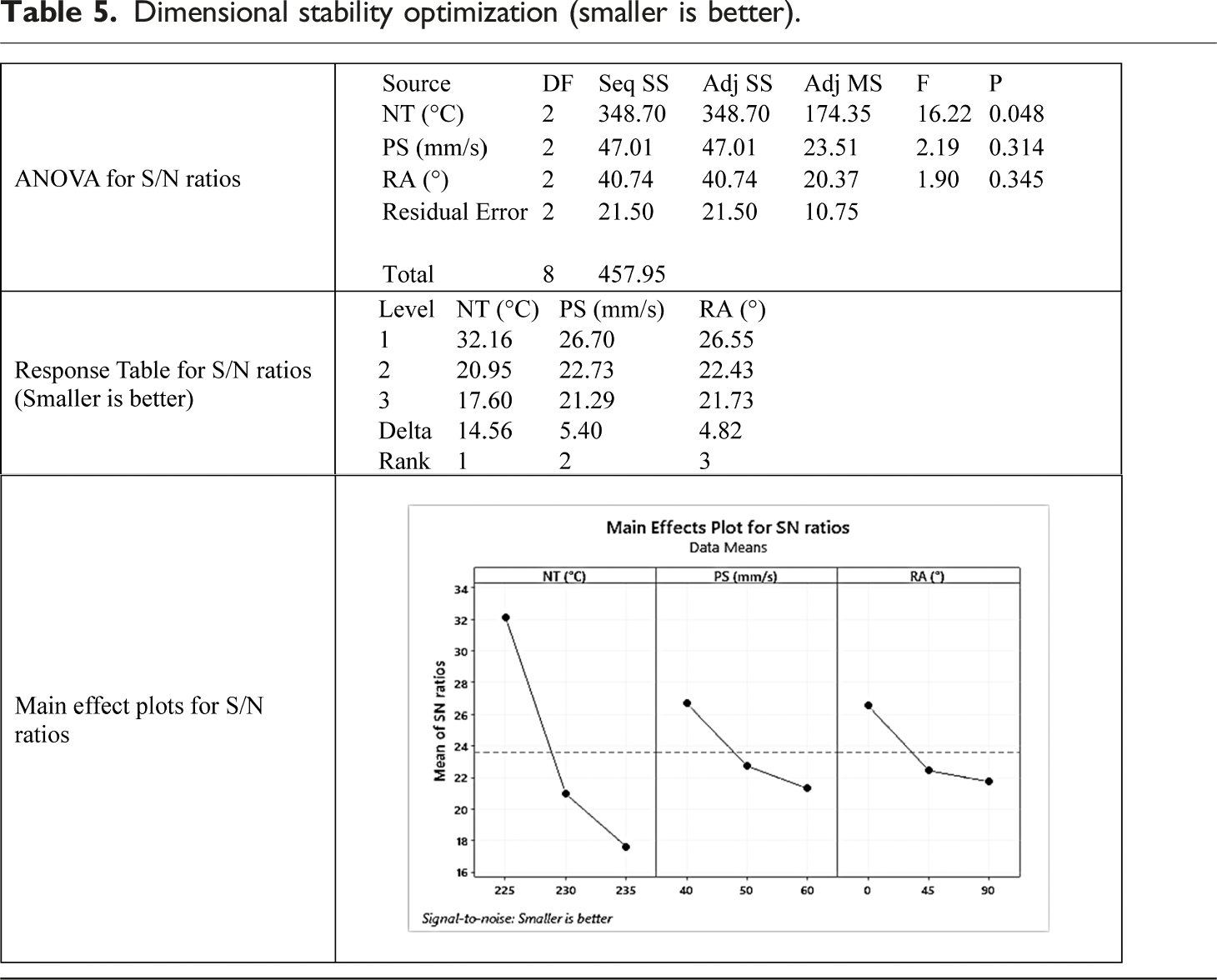
Dimensional stability optimization (smaller is better).
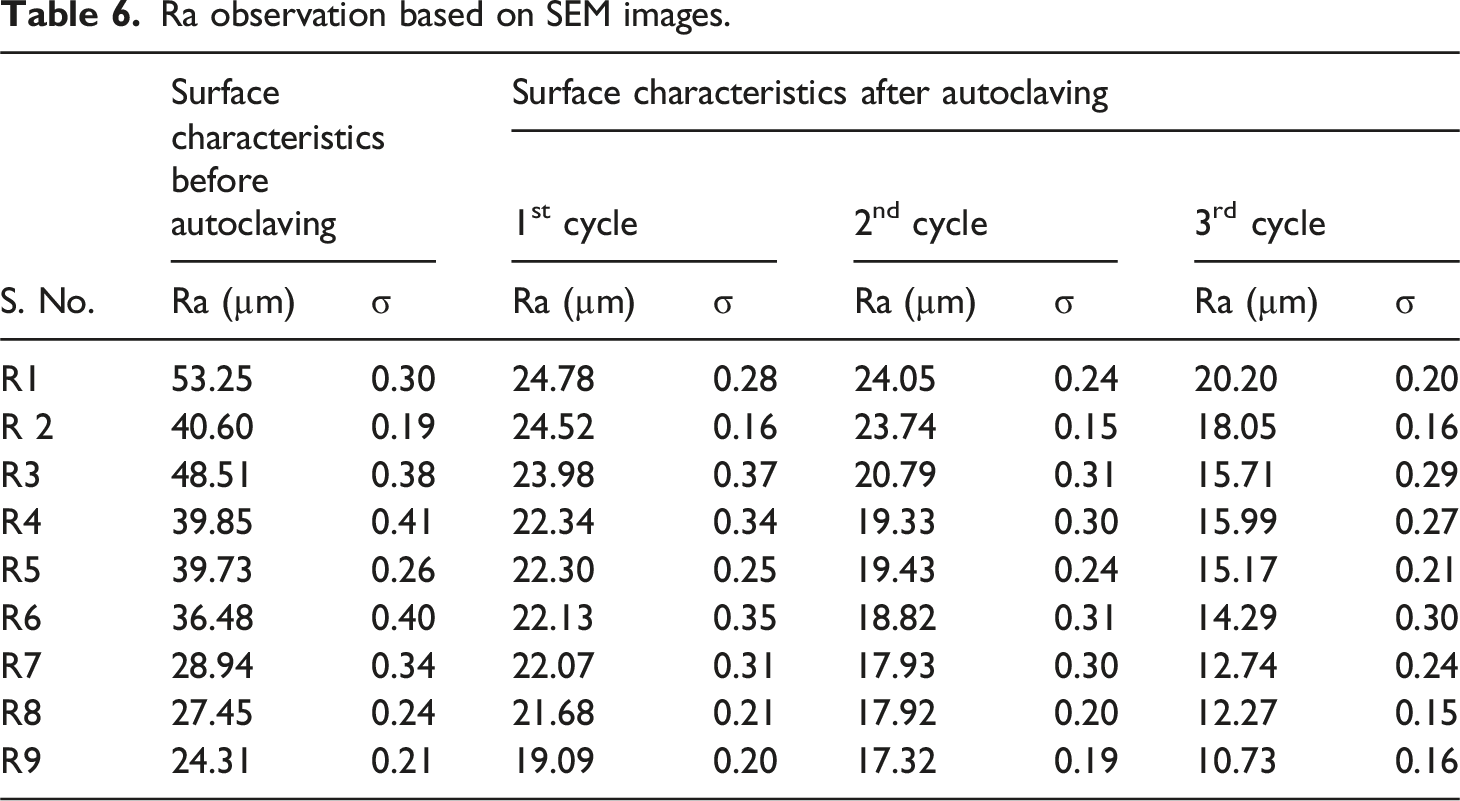
Ra observation based on SEM images.
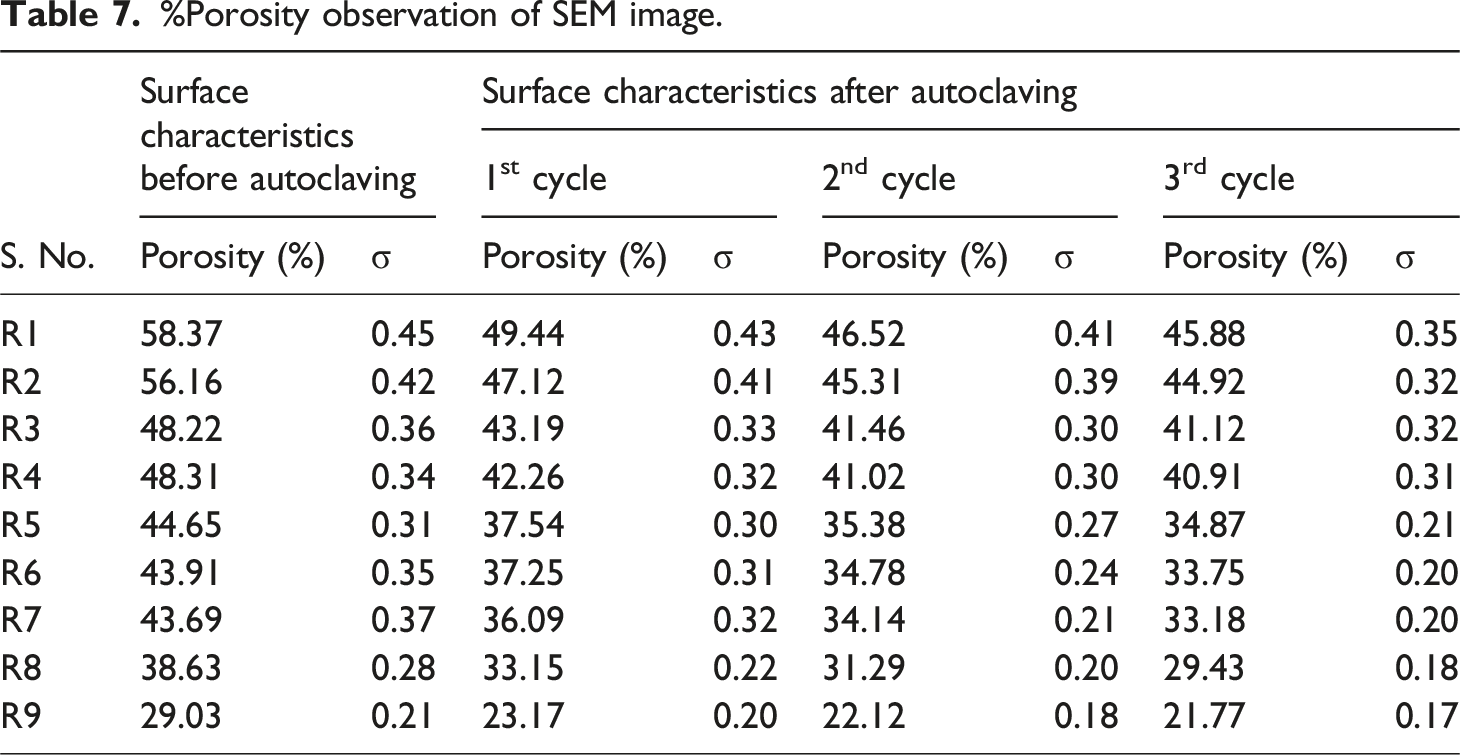
%Porosity observation of SEM image.
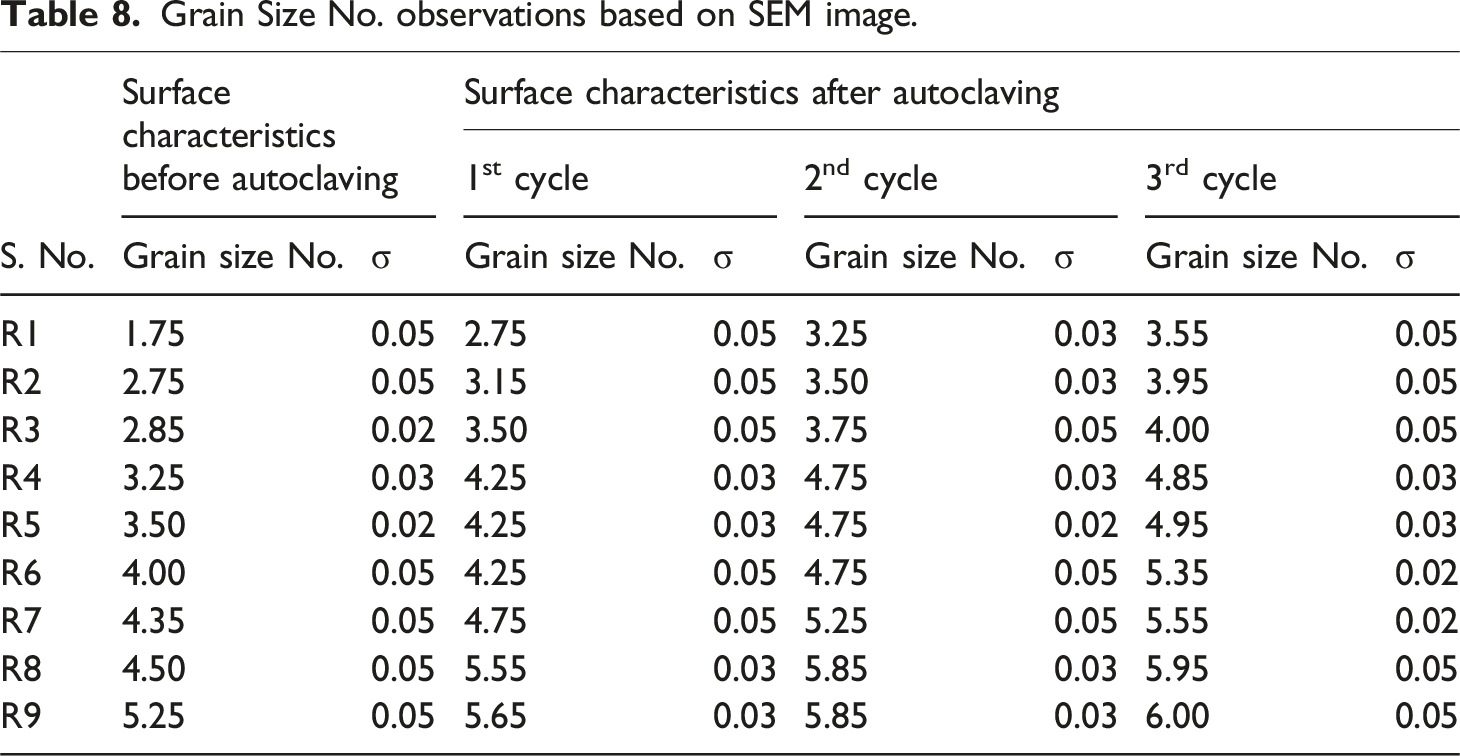
Grain Size No. observations based on SEM image.
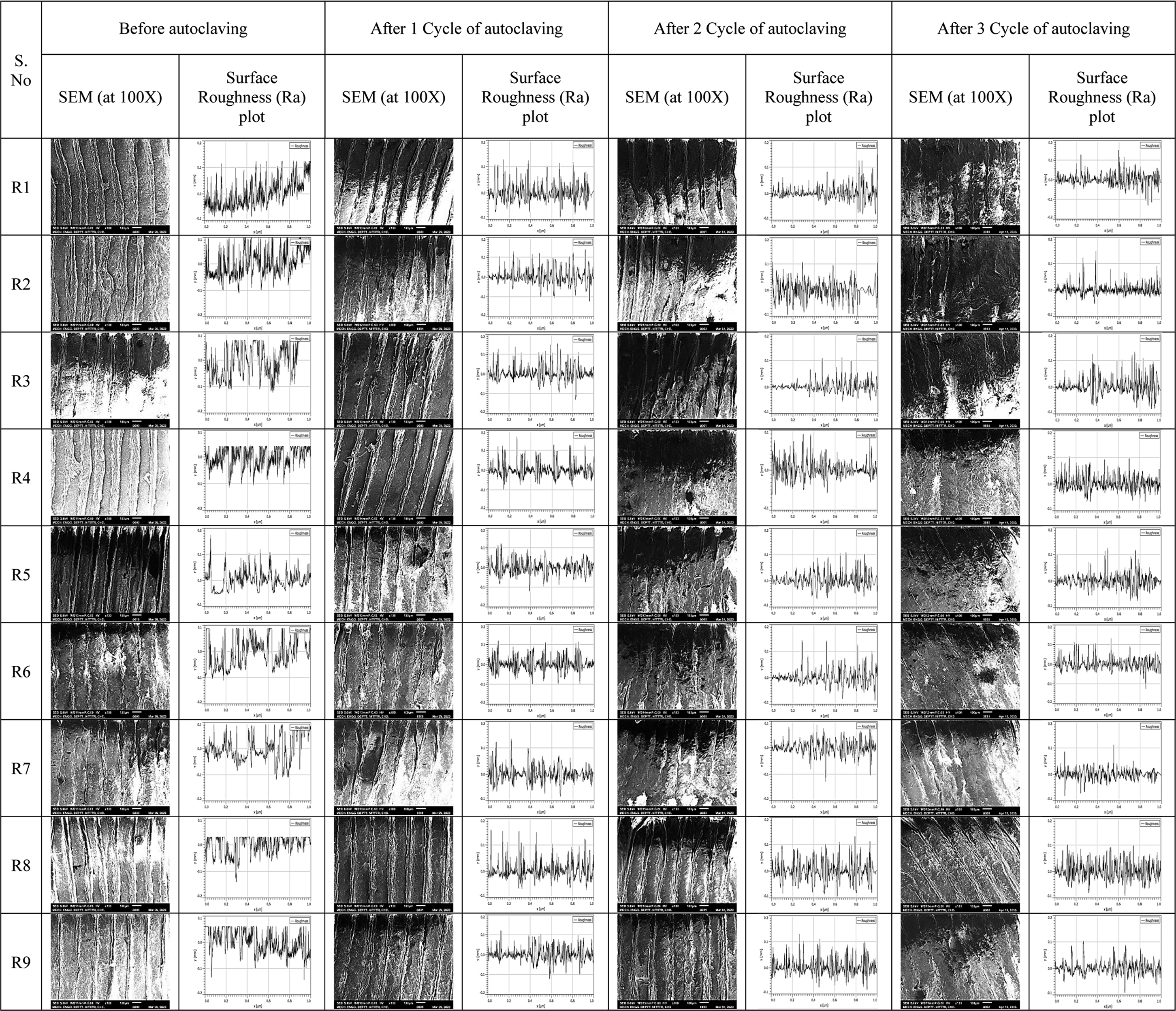
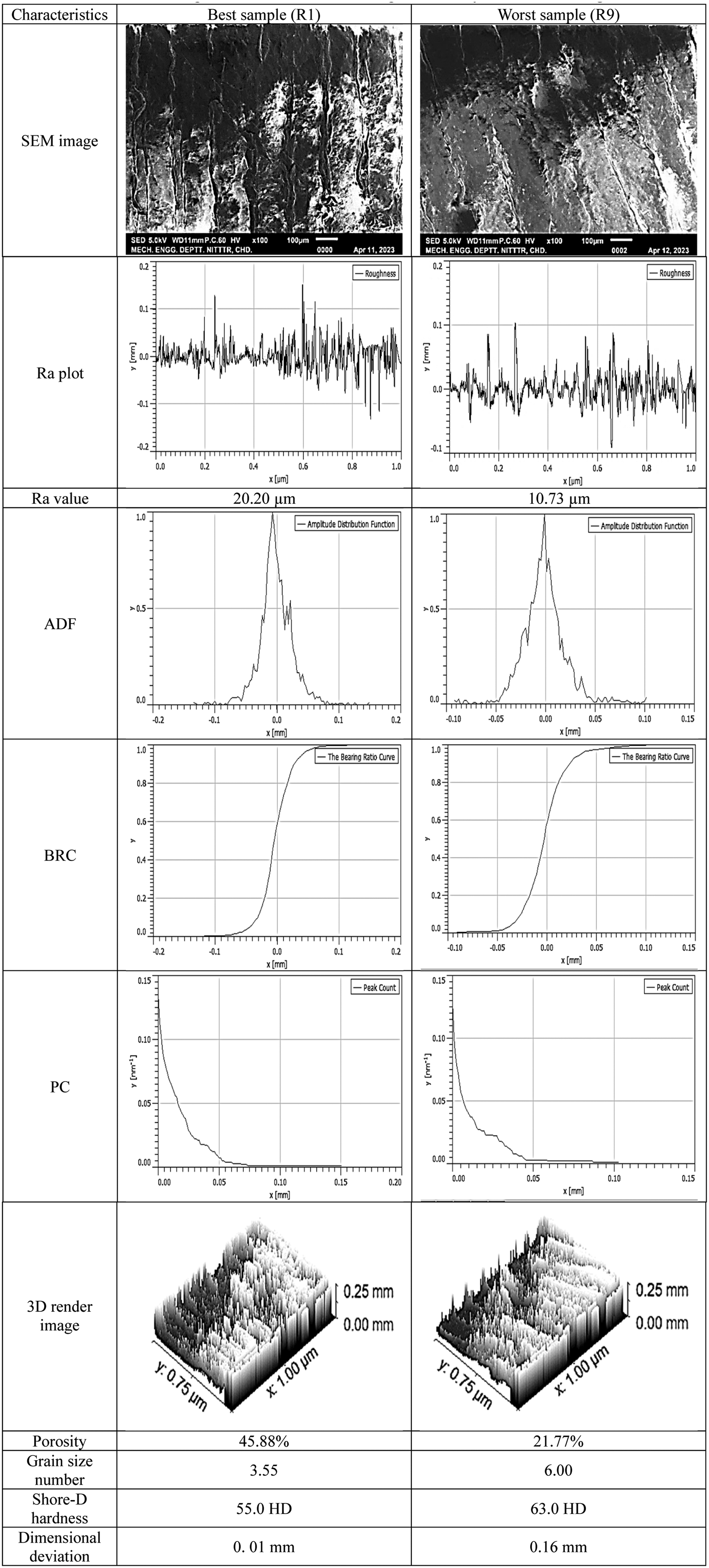
SEM images and surface characteristics (as per Table 4).
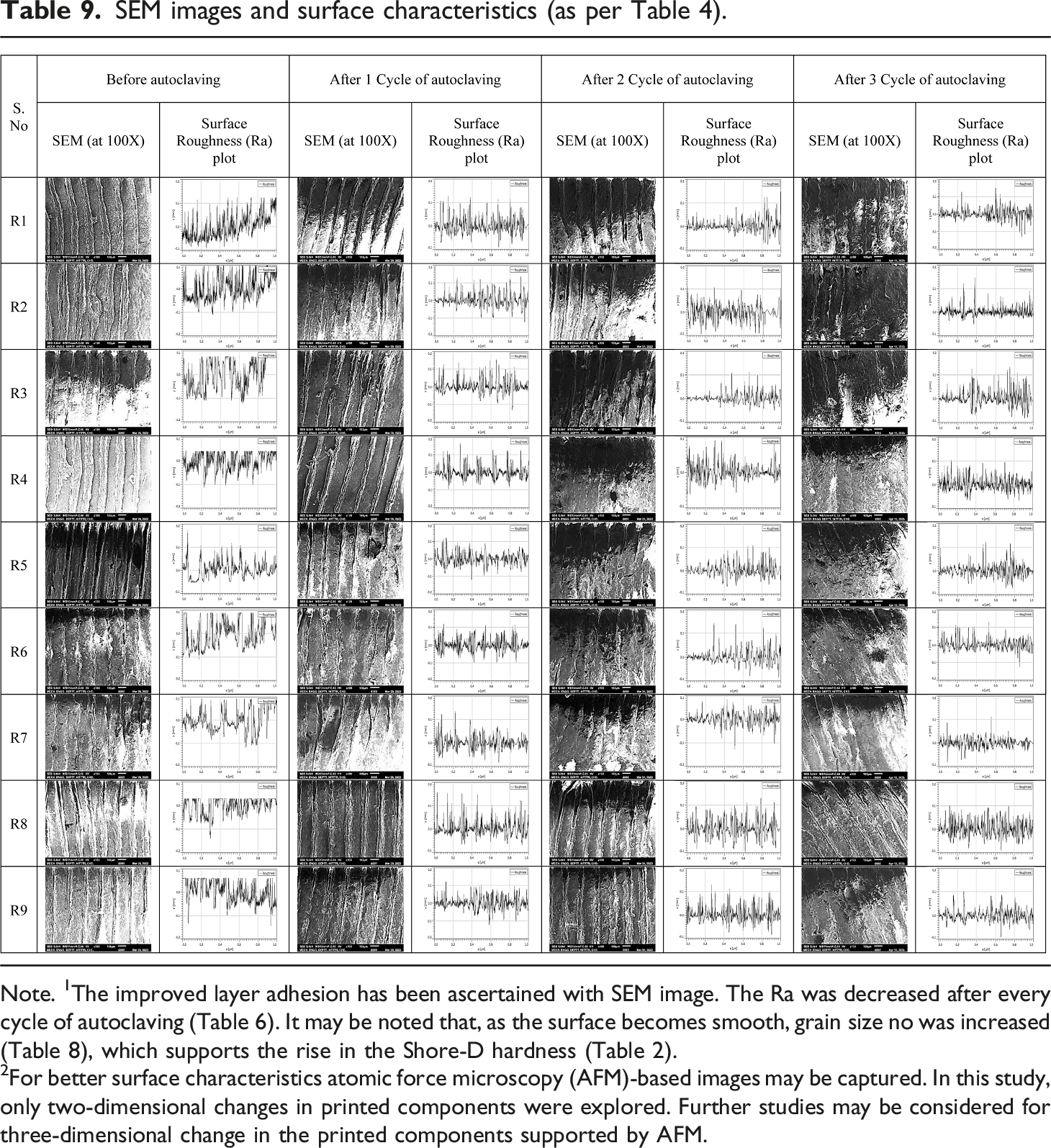
Note. 1The improved layer adhesion has been ascertained with SEM image. The Ra was decreased after every cycle of autoclaving (Table 6). It may be noted that, as the surface becomes smooth, grain size no was increased (Table 8), which supports the rise in the Shore-D hardness (Table 2).
2For better surface characteristics atomic force microscopy (AFM)-based images may be captured. In this study, only two-dimensional changes in printed components were explored. Further studies may be considered for three-dimensional change in the printed components supported by AFM.
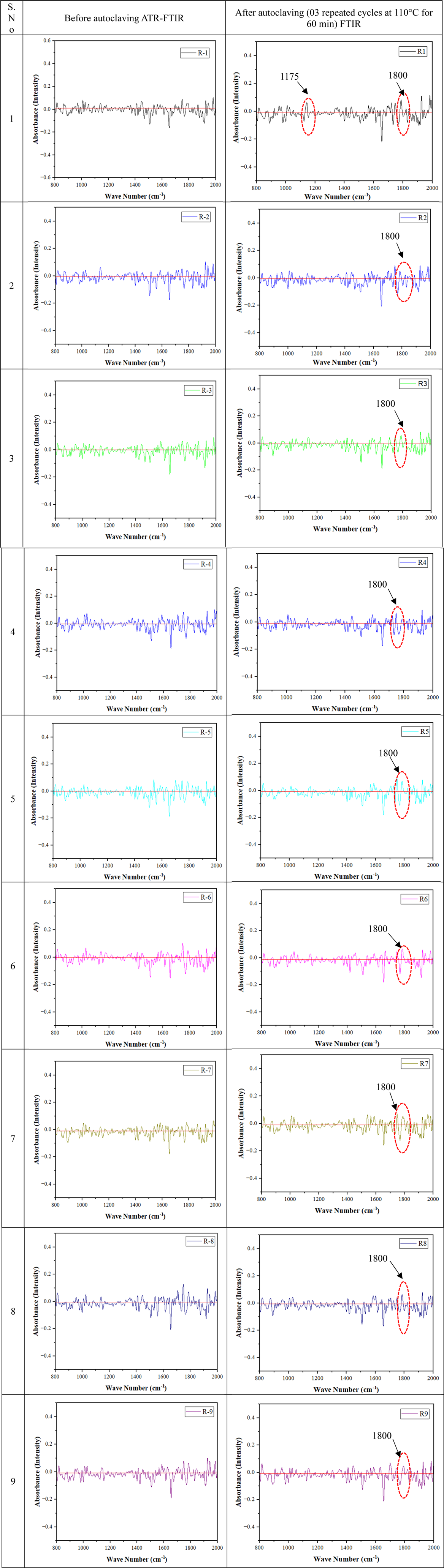
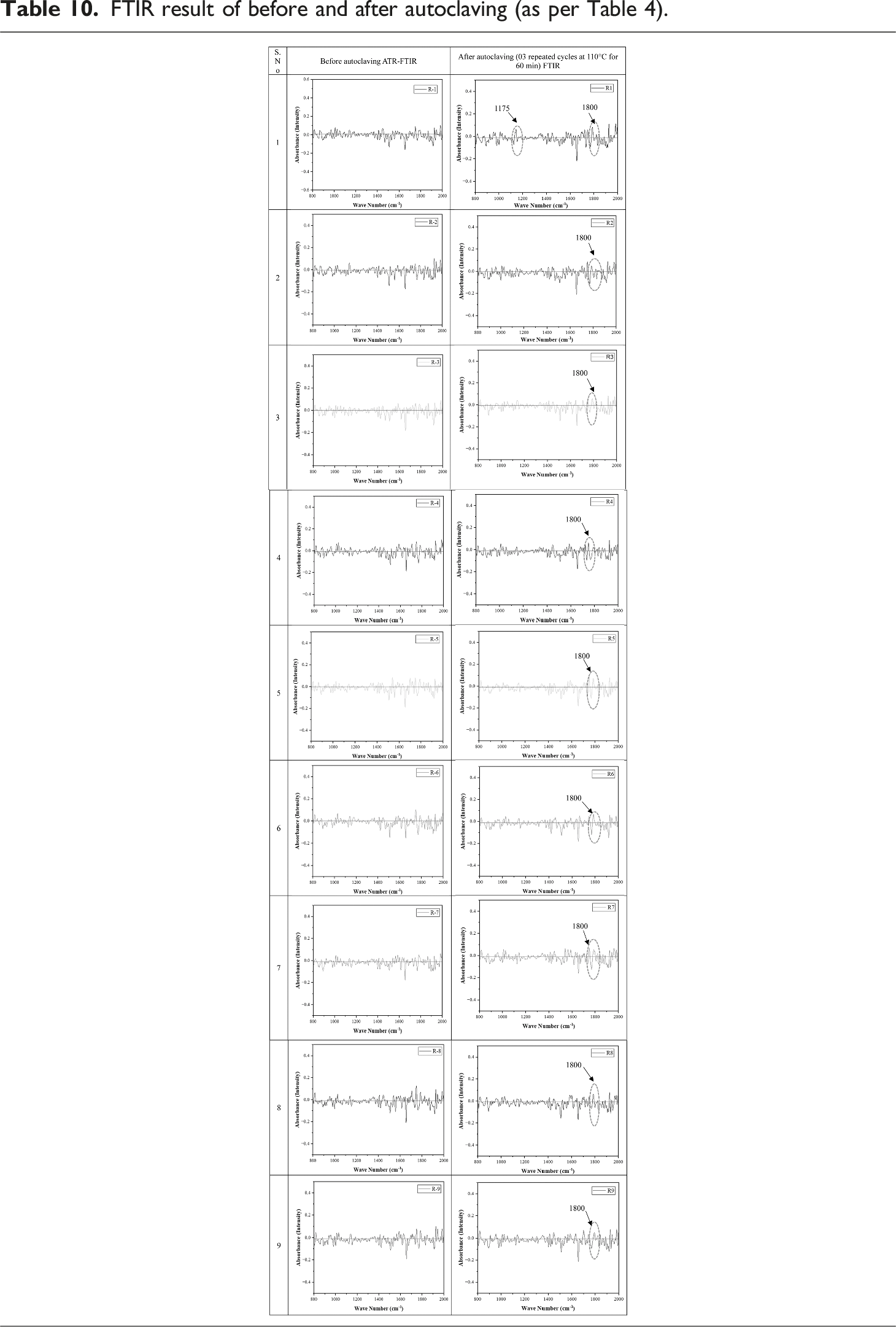
FTIR result of before and after autoclaving (as per Table 4).
Comparison of best and worst samples after three cycles of autoclaving.
Conclusions
The autoclaving was performed for 03 cycles in this study because it can fulfill the unique requirements of implants while still being affordable and ecologically friendly. The dimensional stability directly affects fit, functioning, biocompatibility, and long-term performance in implants, and it is of the utmost significance. The necessity of maintaining constant size and form, assuring patient well-being, and lowering the risk of problems is further highlighted by the requirement for these implants to smoothly integrate with the intricate biomechanics of the human body. In this study, the S/N ratio was used to ascertain the best setting of process parameters for the minimum (smaller is better) Shore-D hardness and minimum dimensional deviation of PVDF-HAp-CS composite for the possible application to help in better adhesion or growth of osteoblast cells within the implant. This study suggests that the best setting of the FFF process, for the 3D printing of PVDF composite (90%PVDF, 8%HAp, 2%CS) for smaller is better are the NT 225°C, RA 0°, and PS 40 mm/s, resulting in Shore-D hardness 48.5 HD (before autoclaving) and 55.0 HD (after autoclaving), dimensional deviation 0.01 mm (after autoclaving). In the comparison of the FTIR spectrum plot before and after autoclaving, it was noticed that after autoclaving a prominent peak was developed at wave number 1800 cm−1, and the corresponding absorbance value was reduced which was responsible for increased Shore-D hardness.
In this study, only two-dimensional changes in printed components were explored post-autoclaving. Further studies may be considered for three-dimensional change in the printed components supported by AFM. Also, actual biomedical implants of PVDF composite matrix may be prepared and their in vitro, in vivo analysis may be performed along with analysis of their mechanical, morphological, thermal, and dimensional stability before going for clinical trials.
Footnotes
Acknowledgements
The authors acknowledge the research support provided by the National Institute of Technical Teachers Training and Research, Chandigarh (India).
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Department of Science and Technology for funding under FIST Level-0, Project No. SR/FST/College-/2020/997.