Abstract
Cross-sectional work suggests that higher neuroticism and lower conscientiousness are consistently related to more subjective cognitive complaints. Little is known about the longitudinal associations. We used data from the Interdisciplinary Longitudinal Study of Adult Development to examine how personality and cognitive complaints jointly unfolded over 20 years. Participants came from a midlife (n = 502, Mage = 43.7) and an older age group (n = 500, Mage = 62.5). Random-intercept cross-lagged panel models were used to test the personality-complaint associations at the between-person and within-person levels. Analyses controlled for gender, education, subjective health, objective health, and memory. At the between-person level, higher neuroticism and lower conscientiousness were associated with more cognitive complaints over 20 years, and these associations were stronger in older than middle-aged adults. Among older adults, lower extraversion, openness, and agreeableness were longitudinally associated with more cognitive complaints. At the within-person level, all five traits were concurrently related to cognitive complaints, with small to medium-sized effects, but not across all measurement occasions. Few cross-lagged effects were found, with no consistent pattern across time or age cohorts. This work provides longitudinal evidence of personality-complaint associations and suggests that these associations varied more across individuals than within individuals over time.
Plain Language Summary
Higher neuroticism (i.e., the tendency to worry) and lower conscientiousness (i.e., the tendency to be disorganized) are related to higher levels of cognitive complaints (i.e., negative judgments about one’s cognitive functioning). Little is known about the associations between neuroticism, conscientiousness, and cognitive complaints over years. We used data from the Interdisciplinary Longitudinal Study of Adult Development to examine how neuroticism, conscientiousness, and cognitive complaints jointly unfolded over 20 years. Participants came from a midlife (n = 502, Mage = 43.7) and an older age group (n = 500, Mage = 62.5). Analyses controlled for gender, education, subjective health, objective health, and memory. Higher neuroticism and lower conscientiousness were associated with more cognitive complaints over 20 years between and within individuals. This work adds to the literature that the associations between neuroticism, conscientiousness, and cognitive complaints are evident over two decades in both middle-aged and older adults.
Keywords
Introduction
Growing literature indicates that the Five-Factor-Model (FFM) personality traits (McCrae & John, 1992)—particularly neuroticism and conscientiousness—are associated with various measures of cognitive health. For example, higher neuroticism and lower conscientiousness are associated with more cognitive complaints and subjective cognitive decline (Aschwanden et al., 2020; Kliegel et al., 2005; Koller et al., 2019; Reynolds et al., 2022; Smit et al., 2021; Sutin et al., 2020; Zullo et al., 2021), worse performance on standardized cognitive tasks (Caselli et al., 2016; Luchetti et al., 2016), more in vivo markers of amyloid and tau accumulation (Terracciano et al., 2022), less resilience to Alzheimer’s Disease neuropathology (Graham et al., 2021; Terracciano et al., 2013), and a shorter cognitive health span (Yoneda et al., 2022). Within the field of cognitive health, there has been a long-standing interest in subjective cognition, such as cognitive complaints and subjective cognitive decline, because these self-reports may be indicators of actual cognitive decline and incident impairment (Hertzog et al., 2018; Hertzog & Pearman, 2014; Jessen et al., 2014, 2020; Petersen et al., 1999). The current literature on personality and cognitive complaints lags behind as it is limited by a predominant use of cross-sectional data (Aschwanden et al., 2020). The present study aimed to fill this gap by examining the longitudinal association between the FFM personality traits and cognitive complaints over two decades. Such research is important to better understand how the personality-complaint associations change over time and to provide insights into the temporal direction of these relationships.
The role of cognitive complaints in cognitive health
Cognitive complaints are defined as negative judgments about one’s cognitive functioning, such as confusing names and dates, or having difficulties to follow the train of thoughts of others (Mascherek et al., 2011). Cognitive complaints are common and most people experience them from time to time, due to, in part, factors that range from situational (Robertson et al., 1997) to neurological (van Norden et al., 2008). With increasing age, cognitive complaints are common too (Jonker et al., 2000; Ponds et al., 2000). For example, statistics from 2018 show that 53% of Germans aged 40–79 years reported memory concerns (Luck et al., 2018), while 10.8% of Americans aged 45–64 years and 11.7% of Americans aged 65+ years perceived confusion or memory loss over the last 12 months (Centers for Disease Control and Prevention, 2018). Cognitive complaints have predictive value for cognitive decline (Mendonça et al., 2016) but seem to mainly evaluate cognitive dysfunction in daily life that has limited overlap with the abilities assessed by standardized cognitive tasks in laboratories or clinics. Still, cognitive complaints are risk factors for cognitive impairment (Jessen et al., 2014), but not all individuals who report cognitive problems will develop cognitive impairment (Mitchell et al., 2014). As such, the relationship between cognitive complaints and cognitive function is complicated. Cognitive complaints should not serve as alonestanding proxies for cognitive decline but rather be considered an important marker of everyday cognition in their own right. Cognitive decline, on the other hand, is also a natural part of aging, and there are interindividual differences in the rate of change (Wilson et al., 2002). The literature on cognitive complaints and cognitive performance/decline is inconsistent, with some studies reporting significant effects and others reporting null results (Burmester et al., 2016; Crumley et al., 2014; Hülür et al., 2014, 2015; Mascherek & Zimprich, 2011). It is hence a challenge to determine the individual risk for future cognitive impairment from the presence or absence of such complaints (Jessen et al., 2014). Regardless of the etiology, cognitive complaints may limit personal growth, reduce quality of life, and increase fear of dementia, and thus should be treated (Metternich et al., 2010).
Cognitive complaints are heterogeneous, with many possible underlying causes besides cognitive dysfunction, including a variety of age-related chronic conditions (Hill et al., 2021), negative attitudes towards aging (Siebert et al., 2020), depressive symptoms (Hülür et al., 2014; 2015; Zimprich et al., 2003), daily stress (Mahoney et al., 1998), and tiredness (Broadbent et al., 1982). Among the many factors associated with cognitive complaints, personality has been recognized as a relevant factor in the field of cognitive health (Molinuevo et al., 2017). To date, it is unclear whether individuals with certain personality traits (e.g., higher neuroticism and lower conscientiousness) are more likely to report cognitive complaints due to general health-related concerns and trait-related mental processes or if they are inherently more sensitive to subtle cognitive changes (Koller et al., 2019; Reid & MacLullich, 2006)—it is probably a mixture of various processes. Although the clinical consequences are yet to be understood, consideration of personality (that may contribute to responses to some assessment of subjective cognitive impairment/decline) is already important for instrument refinement and early identification (Jessen et al., 2020; Molinuevo et al., 2017; Rabin et al., 2015). This study aimed to expand the basic knowledge of personality-complaint associations by shedding light on its long-term linkages.
Previous research on personality and cognitive complaints
A cross-sectional meta-analysis including 10–17 samples (Aschwanden et al., 2020) showed that higher neuroticism and lower conscientiousness were related to more cognitive complaints with moderate effect sizes. Lower scores on extraversion, openness, and agreeableness were also associated with more cognitive complaints, yet to a weaker extent. The meta-analysis identified only three longitudinal studies (Aschwanden et al., 2018; Comijs et al., 2002; Lane & Zelinski, 2003), but none included extraversion, openness, or agreeableness, nor did they disentangle between-person variation from within-person variation. Associations at the between-person level do not necessarily translate to how these variables are related at the within-person level (Molenaar, 2004). For instance, between-person variation provides knowledge about whether people with higher neuroticism also tend to report more cognitive complaints over time, whereas within-person variation yields knowledge about whether changes in neuroticism precede changes in cognitive complaints, the other way around, or neither. In previous longitudinal work, Lane and Zelinski (2003) examined the relationship between neuroticism, conscientiousness, and four factors of self-rated memory (frequency of forgetting, seriousness of forgetting, retrospective functioning, and mnemonic use) using hierarchical linear models in 97 participants aged 30–81. There was a negative zero-order correlation between neuroticism and the 16-year change slope of frequency and seriousness of forgetting and a positive correlation for conscientiousness. In conditional analyses, the authors examined the effects of neuroticism and conscientiousness on memory ratings at baseline, but not on changes in ratings. In a sample of 1,669 individuals aged 55–85, Comijs and colleagues (2002) examined the association between neuroticism and changes in memory complaints over six years, using logistic regression analysis that controlled for socio-demographics as well as physical and psychological health factors. Results showed that participants with high neuroticism (dichotomized at the 50th percentile of the mean score) were more likely to report memory changes over the follow-up. In a previous analysis with the older cohort of the Interdisciplinary Longitudinal Study on Adult Development (N = 500, aged 60–64), the mediating role of cognitive complaints on the 12-year longitudinal association between neuroticism and cognitive functioning has been examined (Aschwanden et al., 2018). The zero-order correlation showed that higher neuroticism at baseline was associated with more cognitive complaints 12 years later.
Potential mechanisms
Lifespan models of personality and health have theorized mechanisms through which personality traits contribute to health outcomes such as longevity (Friedman et al., 2014). These models have been used in personality-cognition research to identify mechanisms between personality and cognitive performance (Luchetti et al., 2016) as well as personality and cognitive complaints (Aschwanden et al., 2020; Sutin et al., 2020).
The “cognitive abilities” model (Aschwanden et al., 2020) postulates that personality is associated with health behaviors that have cascading effects on cognitive health, which in turn may affect cognitive complaints. Specifically, personality has been associated with smoking (Hakulinen et al., 2015), physical inactivity (Sutin et al., 2016), body mass index (Sutin et al., 2018), diabetes (Jokela et al., 2014), inflammation (Stephan et al., 2024), cognitively stimulating activities (Stine-Morrow et al., 2014), and educational achievement (Sutin et al., 2017)—all these factors are associated with cognitive functioning (Sabia et al., 2009). Such a model assumes that cognitive complaints reflect cognitive health, but as previously stated, evidence for the association between cognitive complaints and cognitive performance is mixed.
The “mental processes” model (Aschwanden et al., 2020) suggests that personality influences cognitive complaints through mental processes characteristic of the FFM personality traits. For example, people with higher neuroticism ruminate more, and rumination can distract from ongoing behavior (Munoz et al., 2013), thus leading to higher levels of cognitive complaints. In contrast, the structured mindset of conscientious individuals may help to focus on ongoing behavior and result in lower levels of cognitive complaints (Fleeson & Gallagher, 2009; Sutin et al., 2020). Behavioral factors, such as poor sleep (Duggan et al., 2014), may also affect mental processes (i.e., daytime sleepiness leading to more cognitive lapses). To date, the mental processes model has not yet been tested, and research on personality and characteristic mental processes is scarce (Flehmig et al., 2007; Robinson & Tamir, 2005).
The “reporting bias” model (Aschwanden et al., 2020) specifies that individuals judge themselves based on their personality, which could lead to biases in cognitive complaints. For example, individuals high in neuroticism tend to be more critical about their cognitive functioning (Colvin et al., 2018), which may make them more likely to complain about their cognition. However, findings from ecological momentary assessment studies (P. L. Hill et al., 2020; Lange & Süß, 2014) weaken this model by reducing memory bias and heuristic processing (Conner & Mehl, 2015), and allow measurement of behavior when it occurs.
Directionality
Previous studies have focused on personality traits as predictors of cognitive complaints; however, reciprocal effects may exist. Indeed, in the literature, bidirectional hypotheses have been proposed—that is, how personality influences cognitive complaints, and how cognitive complaints influence personality. When considering the first direction (personality → cognitive complaints), the hypotheses are mainly based on the three models mentioned before. For example, neuroticism is characterized by greater mental noise and vulnerability to rumination (Flehmig et al., 2007; Robinson & Tamir, 2005), which may distract from ongoing behavior and action (Munoz et al., 2013), and lead to more cognitive complaints (mental processes model). Moreover, highly conscientious individuals tend to be more organized and use a more efficient step-by-step processing strategy to achieve a goal (Stock & Beste, 2015), which may help to focus on ongoing behavior and result in fewer cognitive complaints (Könen & Karbach, 2018; Sutin et al., 2020). Also, individuals with lower neuroticism and higher conscientiousness may have more cognitive and psychological reserve to manage stress (Connor-Smith & Flachsbart, 2007) and maintain cognitive functioning (Graham et al., 2021), therefore reporting fewer cognitive complaints (cognitive abilities model). When considering the opposite direction (cognitive complaints → personality), perceiving cognitive problems may lead to increasing anxiety, which could result in higher neuroticism (Curtis et al., 2015; Wagner et al., 2016). Moreover, correlated change is a third possibility (Allemand & Martin, 2016), with personality and cognitive complaints developing in tandem due to a common cause or a common mechanism. For instance, decline in cognitive ability may cause both increases in neuroticism (Wagner et al., 2016; Wahl et al., 2010) and increases in cognitive complaints (Mascherek & Zimprich, 2011). These hypotheses are not mutually exclusive and reciprocal effects are plausible.
The present study
Meta-analytic work has summarized the link between (a) personality and cognitive abilities (Stanek & Ones, 2023), (b) personality and cognitive complaints (Aschwanden et al., 2020), and (c) cognitive complaints and cognitive abilities (Burmester et al., 2016), but an empirical integration of these links in a time-ordered manner with cognitive complaints as outcome is lacking. The present study thus examined how personality traits and cognitive complaints jointly unfold over 20 years. Using the same data set, the temporal unfolding of these constructs has been examined separately (i.e., personality) (Graham et al., 2020) or in combination with other variables (i.e., cognitive complaints and change in attitude towards aging) (Siebert et al., 2020), but not like we did in the present work.
This study aimed to extend previous work in several ways. First, this study is longitudinal with a follow-up of 20 years and considers bidirectional effects and all FFM traits. Previous work has focused on unidirectional effects of mainly neuroticism and conscientiousness on cognitive complaints, neglecting potential reverse effects of cognitive complaints and the remaining three FFM traits. Second, prior longitudinal research did not disentangle between-person variation from within-person variation when examining personality and cognitive complaints. Distinguishing between-person from within-person variability in personality and cognitive complaints is important for understanding their stability and change over time. For cognition-personality research, it is important to understand what it means for one person to vary from another and what it means for individuals to vary from themselves over time (Mroczek et al., 2003). Studying associations at the within-person level is important as it helps to better understand whether the between-person associations are limited to a description of co-occurrences of differences between individuals or can be included in the characterization of the ongoing, internal psychological functioning of individuals. Moreover, between-person correlations have implications for evaluating whether personality changes could lead to changes in cognitive complaints, or vice versa. If such associations can be replicated, possible intervention strategies can be derived subsequently (e.g., a personality intervention designed to increase conscientiousness and reduce neuroticism, thereby also reducing cognitive complaints). Third, past research focused on older adulthood (aged 65+ years). Midlife, however, is a critical, understudied period of life—prior to when impairments start to manifest and during the transition to older adulthood—and is considered a critical window of opportunity for interventions to prevent or delay cognitive decline (Lachman et al., 2015). We analyzed data from both middle-aged (40+ years) and older adults (60+ years) to examine whether the personality-complaint association varied between midlife and late life. While cognitive complaints are common in older adults, the relation with age is not yet clear. Aging may be linked to increases in some types of complaints such as memory (Luck et al., 2018; Rast et al., 2009), but some evidence suggests cognitive complaints are unrelated to chronological age (Könen & Karbach, 2018) or even more common in younger (<44.63 years) than older adulthood (Sutin et al., 2020). As such, cognitive complaints are not a direct indication of objective cognitive function (Burmester et al., 2016; Carrigan & Barkus, 2016) and can occur due to other causes that are unrelated to age (e.g., stress, tiredness, and low mood) (Broadbent et al., 1982). The personality-complaint association may be different at different ages as the underlying cause for the complaints may change with age. For example, there may be more work-related stress in midlife that may limit the ability to focus, while cognitive abilities may decline and lead to more cognitive complaints in late life. Fourth, we include openness, agreeableness, and extraversion in addition to neuroticism and conscientiousness in our analyses, as these traits have been neglected by previous research. The literature suggests potential negative associations, but they are less consistent and weaker than neuroticism and conscientiousness. For example, individuals who are excitement-seekers, assertive, and cheerful (i.e., high in extraversion) are more likely to engage in complex social situations that keep them involved in cognitively rich activities (Stephan et al., 2014), thereby supporting their cognitive functioning and buffer against cognitive complaints (Curtis et al., 2015). Likewise, individuals higher on openness are more likely to engage in intellectually demanding activities (Stephan et al., 2014) that, in turn, may enhance their cognitive reserve (Curtis et al., 2015; Soubelet & Salthouse, 2010), and prevent cognitive complaints. Further, being less forgiving and more aggressive (i.e., lower agreeableness) may interfere with the ability to follow through on cognitive actions, leading to higher levels of cognitive complaints (Sutin et al., 2020).
Based on the largely cross-sectional literature, we formulated five hypotheses, which were not preregistered: (1) Higher neuroticism will be associated with higher levels of cognitive complaints over 20 years in both cohorts. (2) Lower conscientiousness will be associated with higher levels of cognitive complaints over 20 years in both cohorts. The hypotheses are based on how the characteristic mental processes of neuroticism and conscientiousness are theoretically related to cognitive complaints and may persist over decades: Higher neuroticism may be linked to more cognitive complaints because of rumination and distraction that is inherent to this trait (Denovan et al., 2019). Higher conscientiousness may be associated with lower levels of cognitive complaints because of its association with organization (Gosling et al., 2002), which may help to keep the focus on ongoing behavior and result in fewer cognitive lapses. Or, based on the cognitive abilities model: Higher neuroticism has been linked to higher levels of inflammatory markers (Stephan et al., 2024), which are detrimental to cognitive function (Lupien et al., 2009), and thus could result in higher levels of cognitive complaints. Likewise, as higher conscientiousness has been linked to lower levels of inflammation (Mõttus et al., 2013), more favorable nocturnal blood pressure dipping (Terracciano et al., 2014), and to other healthier metabolic and cardiovascular markers (Sutin et al., 2018), individuals with higher conscientiousness may report lower levels of cognitive complaints due to better cognitive functioning and less physiological stress.
We anticipated larger effect sizes in the midlife cohort since previous work reported stronger personality-complaint associations at younger ages (Sutin et al., 2020). We expected some similarity across the between-person and within-person associations (Luo et al., 2022) and further hypothesized (3) higher levels of cognitive complaints and higher neuroticism at the within-person level at the same measurement occasions. Likewise, we hypothesized (4) higher levels of cognitive complaints and lower conscientiousness at the within-person level at the same measurement occasions. Finally, we expected that (5) increasing cognitive complaints will be associated with increasing neuroticism at subsequent measurement occasions within the same individuals. Noticing an increase of cognitive complaints could be followed by worry and anxiety, which could be reflected in higher neuroticism years later, but not necessarily the other way around (Aschwanden et al., 2018): Increases in neuroticism could lead to health-promoting behaviors (e.g., participation in a memory training) due to anxiety-provoked vigilance (Friedman, 2000) and extenuate cognitive complaints.
We did not formulate hypotheses for openness, agreeableness, or extraversion. We report the results of all FFM traits to provide a more comprehensive picture about the longitudinal association of cognitive complaints with personality.
Methods
Transparency and openness
The present research is based on data from the Interdisciplinary Longitudinal Study on Adult Development (ILSE), a population-based, representative, and widely used data set (Allemand et al., 2015; Kliegel & Zimprich, 2005; M. Luo et al., 2021; Sattler et al., 2017; Siebert et al., 2020; Wahl et al., 2010; Wettstein et al., 2020; Zimprich et al., 2009). We are not allowed to release the data used for the present analyses due to the ILSE’s conditions of use. The samples sizes were determined using the existing data. The hypotheses and statistical analyses were not preregistered. The scripts for the analyses are available. The link to the statistical scripts and our Open Policy Statements can be found at the end of the manuscript.
Participants
Participants were randomly selected and recruited via city registers from East and West Germany. Assessments took place in 1993–1996 (Time 1; T1), 1997–2000 (Time 2; T2), 2005–2008 (Time 3; T3), and 2014–2016 (Time 4; T4). Participants came from two age cohorts, a midlife cohort (born 1950–1952; n = 502 at T1) and a late-life cohort (born 1930–1932; n = 500 at T1). The present study used both cohorts to provide new knowledge about whether the personality-complaint association was different across middle-aged and older adults. The midlife group (48.2% women) was followed from their early 40s to their early 60s (T1 Mage = 43.70, SD = 0.92; T2 M = 47.61, SD = 0.91; T3 M = 54.99, SD = 0.96; T4 M = 63.49, SD = 1.18), whereas the older age group (48.0% women) was followed from their early 60s to their early 80s (T1 Mage = 62.46, SD = 0.96; T2 M = 66.44, SD = 0.95; T3 M = 73.89, SD = 0.89; T4 M = 82.80, SD = 1.16). Of the old cohort, 8% did not participate at T2, 37% did not participate at T3, and another 49% of the remaining participants dropped out at T4, reducing the sample sizes to nT2 = 447, nT3 = 307, and nT4 = 151. Compared with dropouts, those participating in the fourth measurement occasion had better objective health (d = .52) and more years of education (d = .20) at baseline, but they did not differ with respect to gender, self-reported health, cognitive complaints, memory performance, nor the personality traits. In the midlife group, 11% did not participate at T2, 34% did not participate at T3, and another 10% of the remaining participants dropped out at T4, reducing the sample sizes to nT2 = 443, nT3 = 330, and nT4 = 298. In the midlife cohort, participants who remained in the sample up to the fourth measurement occasion had more years of education (d = .29), better objective health (d = .24), and were more open to new experiences (d = .24) at baseline; there were no differences with regard to gender composition, self-reported health, cognitive complaints, memory performance, nor the remaining personality traits. More information on the sample, recruitment, study design, as well as detailed attrition analyses has been reported elsewhere (Miche et al., 2014; Sattler et al., 2017). The study was carried out in accordance with the Declaration of Helsinki and approved by the Ethics Committee of the University of Heidelberg.
Measures
Personality
The FFM personality traits were assessed using the German version of the NEO-Five-Factor Inventory (NEO-FFI) (Borkenau & Ostendorf, 1993). Each subscale consisted of 12 items that were rated on a 5-point response scale from 1 (completely disagree) to 5 (completely agree). Mean scores for each trait were computed. The internal consistency (Cronbach’s alpha) and test–retest correlations are shown in Tables S1 and S2, respectively.
Cognitive complaints
Subjective cognitive complaints were measured with six items from the German Nuremberg Self-Assessment List (NSL) (Oswald & Fleischmann, 1995). These items were selected based on previous literature (Aschwanden et al., 2018; Martin & Zimprich, 2003; Mascherek & Zimprich, 2011). Participants were asked to report cognitive problems in everyday life (e.g., confusing names, phone numbers, dates, or having difficulties to follow the train of thought of others). Items were rated on a 4-point scale ranging from 1 (completely wrong) to 4 (completely true). A mean score was computed. Cronbach alphas are reported in Table S1; test–retest correlations are displayed in Table S2.
Covariates
Gender (0 = men, 1 = women), education (in years), subjective health, objective health, and memory performance were selected as plausible confounders of the hypothesized associations. Gender and education were selected because they are common sociodemographic covariates in the field of personality and cognitive complaints (Steinberg et al., 2013; Sutin et al., 2020). As personality and cognitive complaints share common associations with many psychosocial and health-related variables, we aimed for a parsimonious model and included subjective health and objective health, which potentially subsume various psychosocial and health-related confounders (Aichele et al., 2016; Ocampo, 2010). Further, we included episodic memory performance because it is sensitive to age effects and often the earliest and most central deficit of Alzheimer’s Disease (Budson, 2009; Jessen et al., 2014), appearing up to 15 years before objective cognitive deficits (Rabin et al., 2017).
Subjective health was measured at baseline with one item where participants rated their health from 1 (very bad) to 6 (very good). Baseline objective health comprised an anamnesis, a blood analysis, a geropsychiatric assessment, and a medical checkup conducted by one to two trained study geriatricians (Miche et al., 2014). The professionals aggregated the data and rated the participants’ state of health on a 6-point scale from 1 (very bad) to 6 (very good). The correlation between subjective and objective health was r = .39 (p < .001) in the midlife cohort and r = .23 (p < .001) in the old cohort. Episodic memory at baseline was assessed using a wordlist task from the Nuremberg Inventory of Old Age (Oswald & Fleischmann, 1995). Participants listened to a list of 12 words and were asked to immediately recall as many words as possible after the encoding phase (immediate recall). After a delay of approximately 30 minutes, participants were presented with the original 12 words along with 12 new words, and the task was to differentiate the old words from the new ones (delayed recognition). The words were presented orally to the participants. For each word, participants were asked whether it was on the previous list (from the immediate recall). Participants were instructed to reply “yes” if the word belonged to the previous list and “no” if it did not. Scores from immediate recall and delayed recognition were summed up (max. 24 points). Higher scores indicated better memory performance. Furthermore, birth cohort (1930–1932 vs. 1950–1952) was used as a grouping variable to conduct differential analyses for the midlife and the old age cohorts.
Statistical analysis
We used longitudinal structural equation modeling (SEM) to examine how personality traits and cognitive complaints jointly unfolded over 20 years and how these relations varied within and across individuals. Specifically, we used a multi-group random-intercept cross-lagged panel model (RI-CLPM; see Figure 1 for an illustration including results for neuroticism). The RI-CLPM is an extension of the traditional cross-lagged panel model (CLPM) and separates the between-person time-invariant components of each construct from the within-person time-varying components, leaving the within-subject variation free from the time-invariant components. In a nutshell, the model decomposes the repeated measures of the constructs into person-mean and person-mean-centered latent components (Hamaker et al., 2015). While some people are likely to have overall higher scores of cognitive complaints and neuroticism across the 20 years than others, we were interested in whether increases in cognitive complaints were associated with a subsequent increase in neuroticism within the same individual. A simplified two-cohort RI-CLPM depicting the relationship between neuroticism (Neu) and cognitive complaints (CogCom) across four measurement occasions (T1–T4). Dashed lines indicate non-significant paths. Between-person level: A = association between random intercepts. Within-person level: B = autoregressive effects; C = cross-lagged effects, whereas C1 specifies the effect of cognitive complaints on neuroticism at the subsequent measurement occasion, and C2 specifies the effect of neuroticism on cognitive complaints at the subsequent measurement occasion; D = concurrent associations. H1 = Hypothesis 1: Higher neuroticism will be associated with higher levels of cognitive complaints over 20 years in both cohorts. H3 = Hypothesis 3: Higher levels of cognitive complaints will be associated with higher neuroticism at the same measurement occasions. H5 = Hypothesis 5: Increasing cognitive complaints will be associated with increasing neuroticism at subsequent measurement occasions within the same individuals. Note that Hypotheses 2 and 4 are not shown as they refer to conscientiousness.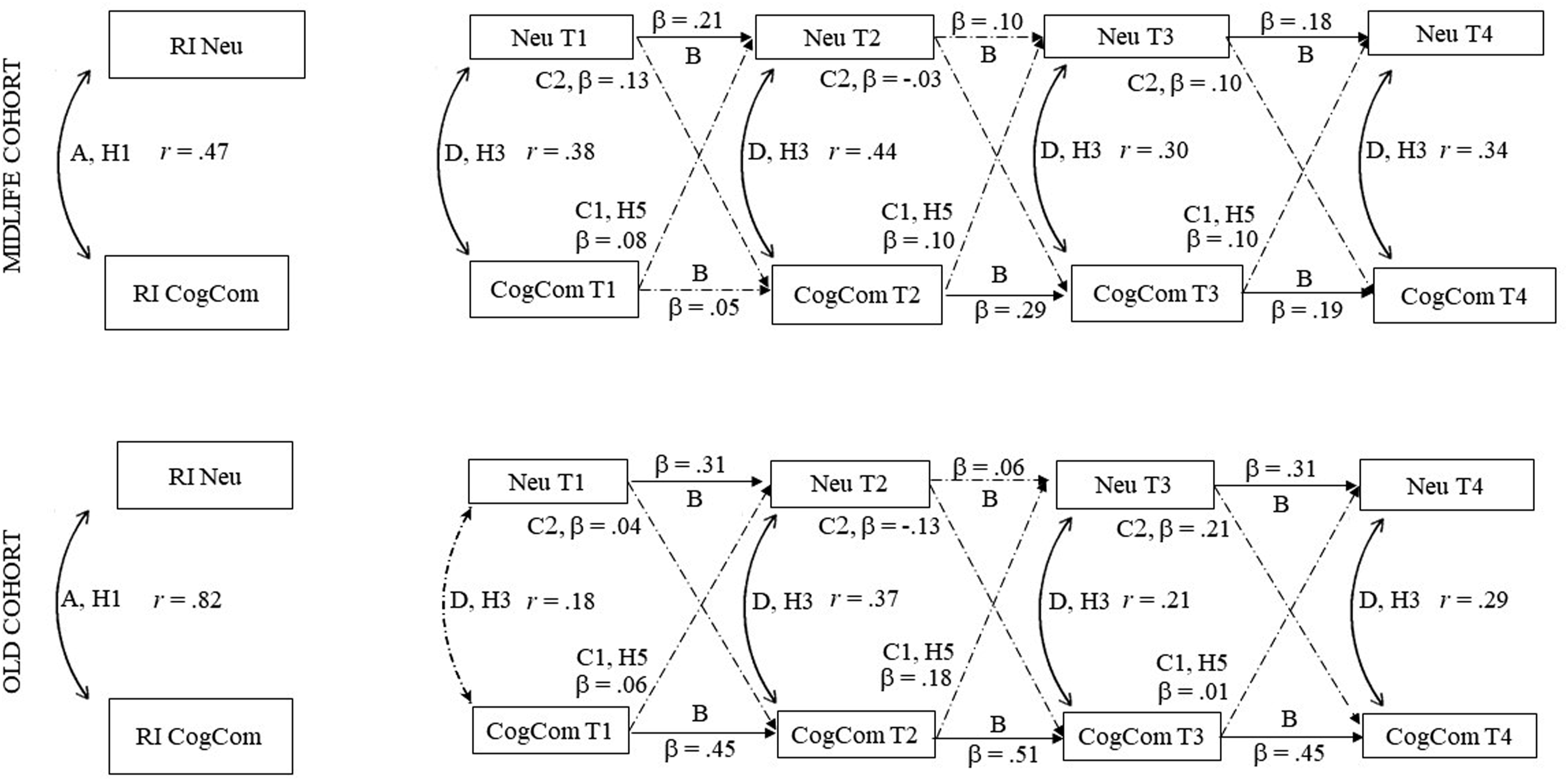
Through the inclusion of random intercepts, the RI-CLPM accounts for stable between-person differences (Figure 1, Path A) and estimates three types of within-person processes: autoregressive (Figure 1, Path B), cross-lagged (Figure 1, Path C), and concurrent processes (Figure 1, Path D). The autoregressive parameters represent the within-person relationship of personality and cognitive complaints with their previous level. If an autoregressive effect is positive, it implies that measurement occasions on which an individual scored above his or her expected score are likely to be followed by measurement occasions on which he or she still scores above the expected score again, and vice versa. The cross-lagged regression parameters evaluate the extent to which within-person change in personality is associated with the individuals’ prior cognitive complaints, and the extent to which within-person change in cognitive complaints is associated with personality at the previous measurement occasion. For example, a positive cross-lagged effect between neuroticism and cognitive complaints suggests that neuroticism above the individual’s own average at one measurement point is associated with a subsequent above-average score on cognitive complaints at the next measurement occasion. The concurrent parameters refer to correlated change (i.e., change correlations between residuals) between personality and cognitive complaints when their autoregressive effects and cross-lagged associations are controlled. For instance, a positive concurrent relation between neuroticism and cognitive complaints shows to what extent deviations of neuroticism from the person-specific average are accompanied by deviations of cognitive complaints from the person-specific average (over and above those predicted by the autoregressive and cross-lagged effects).
For each personality trait, a separate RI-CLPM was run. We used manifest rather than latent variables as models showed poor fit or did not converge with the latent approach. We did not use correction for multiple testing to reduce the risk of false negatives (Perneger, 1998) and because we tested evidence-based hypotheses. All analyses controlled for gender, education, subjective health, objective health, and memory. We used Full Information Maximum Likelihood (FIML) estimation to accommodate missing data. Instead of imputing or discarding incomplete cases, FIML utilizes all available information in the data set to estimate model parameters. We did not constrain the lagged regression coefficients nor the residual variances and covariances of the within-person components over time, as they depend on the time interval between repeated measures, and the time intervals in ILSE were unequal across the four measurement occasions. If lags between subsequent occasions vary, qualitatively different autoregressive and cross-lagged effects between each pair of adjacent measurements are estimated. The advice is to not constrain these parameters over time, as this would lead to an uninterpretable blend of different lagged relationships (Mulder & Hamaker, 2021).
To evaluate the goodness of fit of the models, the chi-square (χ2), comparative fit index (CFI), and root mean square error of approximation (RMSEA) were examined. CFI values above .97 and RMSEA values below .06 are considered a good fit (Hu & Bentler, 1998). To test if the reciprocal effects between personality and cognitive complaints were different for middle-aged and older adults, we performed multi-group analyses (Mulder & Hamaker, 2021). The two cohorts were analyzed simultaneously with birth cohort as the grouping variable. We first fitted a series of RI-CLPMs in which the autoregressive, cross-lagged, and concurrent coefficients as well as the random intercept covariance were allowed to differ across the two cohorts. In the next step, we constrained these parameters to be equal across both cohorts (Mulder & Hamaker, 2021). We then used nested chi-square (χ2) tests to compare the unconstrained model with the constrained model. A significant chi-square test indicated a significant cohort effect (i.e., associations differed across age groups). A non-significant test indicated that the associations were similar across age groups. Moreover, we concluded that the models differed when ΔCFI ≥ .01 and ΔRMSEA ≥ .015 (Chen, 2007).
Analyses were performed with Mplus 8 (Muthén & Muthén, 1998). We report 95% confidence intervals (CIs) for the unstandardized estimates, standard errors, and p-values from the RI-CLPMs as well as the standardized estimates. A post hoc power analysis was run in R version 4.3.2 (R Development Core Team, 2023) with the R package lavaan (Rosseel, 2012). Attrition analysis was run using IBM SPSS Statistics (Version 29) (IBM Corp., 2024).
Results
Descriptive statistics
Descriptive Statistics for ILSE Participants at Baseline (T1).
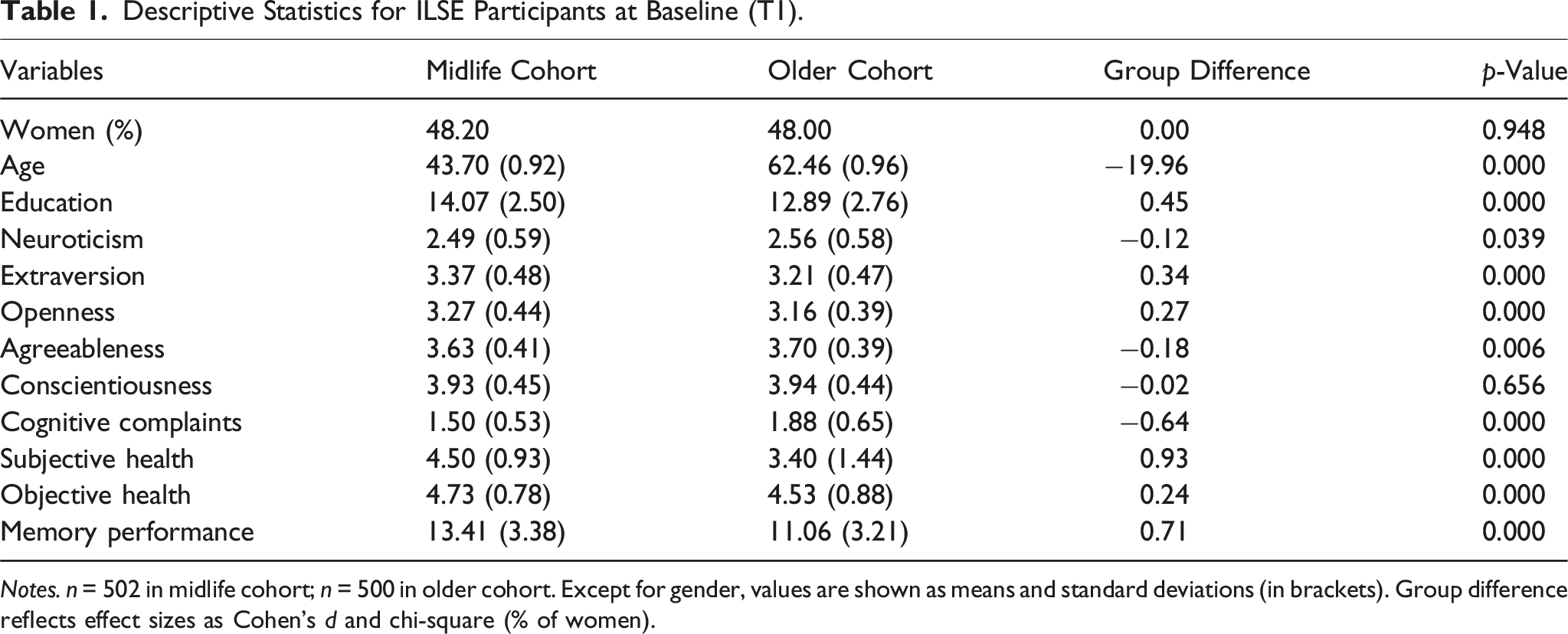
Notes. n = 502 in midlife cohort; n = 500 in older cohort. Except for gender, values are shown as means and standard deviations (in brackets). Group difference reflects effect sizes as Cohen’s d and chi-square (% of women).
Model fit
Model Fit of RI-CLPMs Between Personality and Cognitive Complaints.
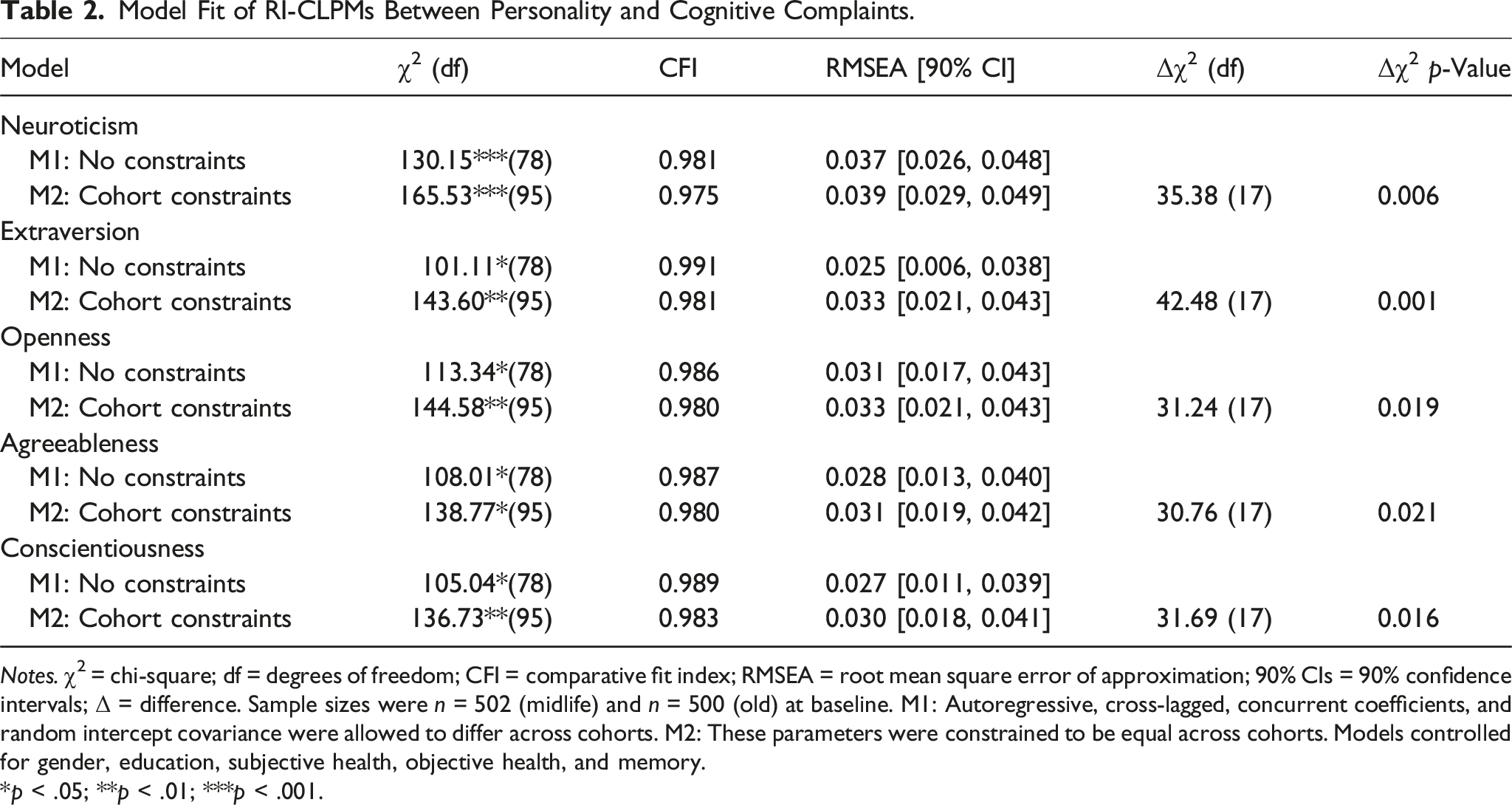
Notes. χ2 = chi-square; df = degrees of freedom; CFI = comparative fit index; RMSEA = root mean square error of approximation; 90% CIs = 90% confidence intervals; Δ = difference. Sample sizes were n = 502 (midlife) and n = 500 (old) at baseline. M1: Autoregressive, cross-lagged, concurrent coefficients, and random intercept covariance were allowed to differ across cohorts. M2: These parameters were constrained to be equal across cohorts. Models controlled for gender, education, subjective health, objective health, and memory.
*p < .05; **p < .01; ***p < .001.
Personality and cognitive complaints
Parameter Estimates From the RI-CLPM for Neuroticism and Cognitive Complaints in Each Cohort.
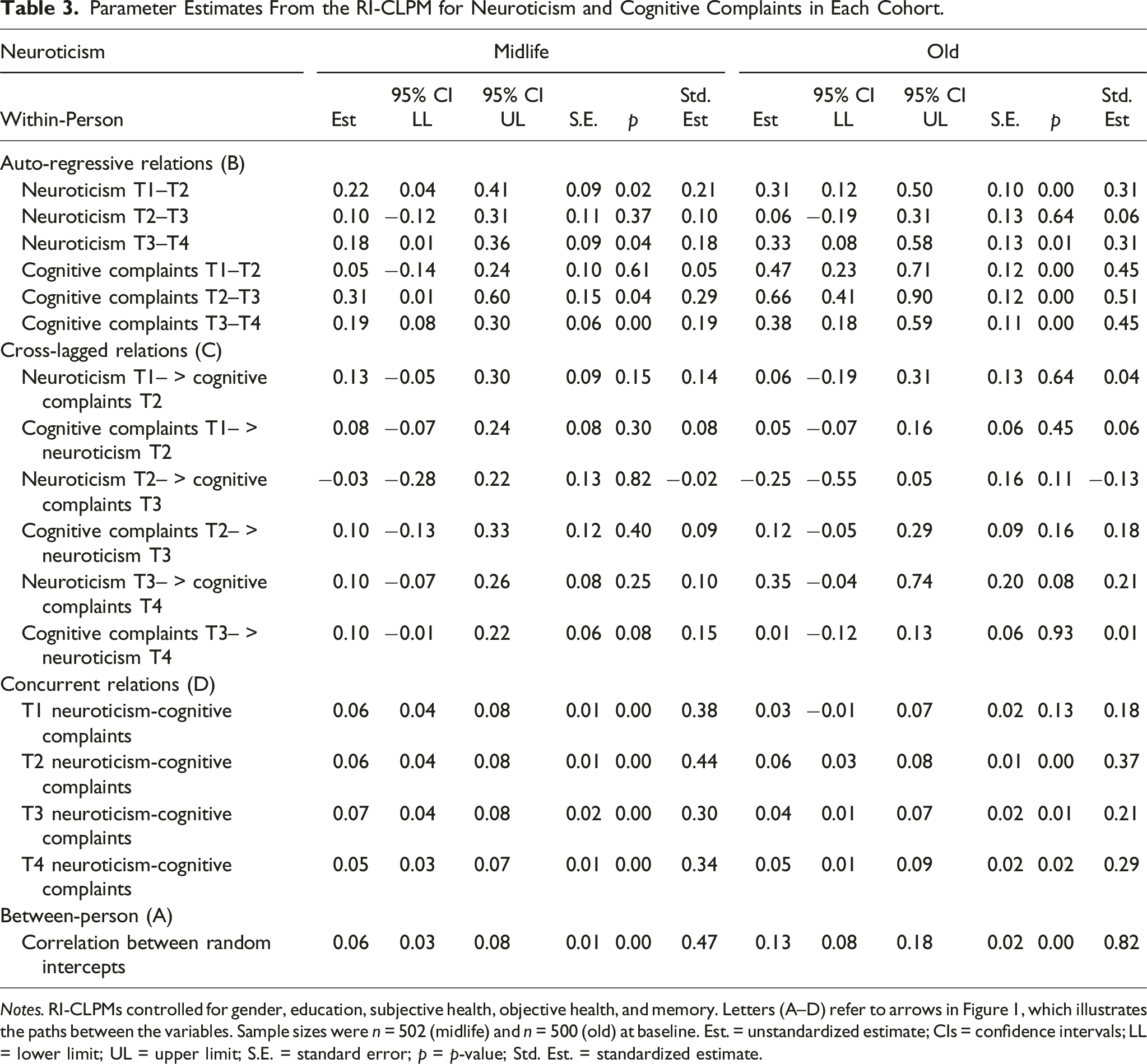
Notes. RI-CLPMs controlled for gender, education, subjective health, objective health, and memory. Letters (A–D) refer to arrows in Figure 1, which illustrates the paths between the variables. Sample sizes were n = 502 (midlife) and n = 500 (old) at baseline. Est. = unstandardized estimate; CIs = confidence intervals; LL = lower limit; UL = upper limit; S.E. = standard error; p = p-value; Std. Est. = standardized estimate.
Parameter Estimates From the RI-CLPM for Conscientiousness and Cognitive Complaints in Each Cohort.
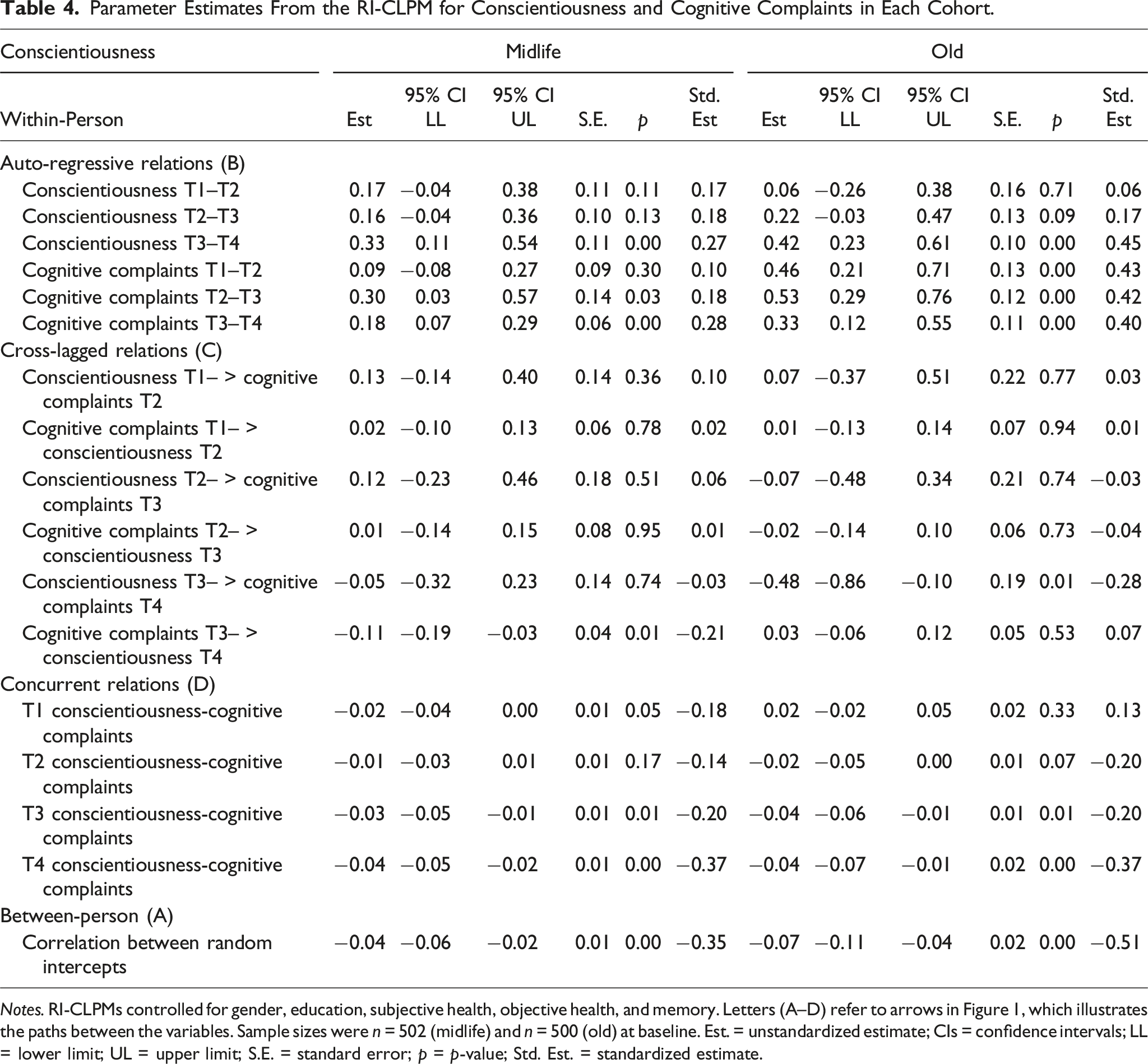
Notes. RI-CLPMs controlled for gender, education, subjective health, objective health, and memory. Letters (A–D) refer to arrows in Figure 1, which illustrates the paths between the variables. Sample sizes were n = 502 (midlife) and n = 500 (old) at baseline. Est. = unstandardized estimate; CIs = confidence intervals; LL = lower limit; UL = upper limit; S.E. = standard error; p = p-value; Std. Est. = standardized estimate.
At the between-person level, neuroticism and conscientiousness were related to cognitive complaints in both cohorts. On average, higher neuroticism and lower conscientiousness were associated with higher levels of cognitive complaints, and this association was substantially stronger among older than middle-aged adults (i.e., rold = .82, 95% CI [0.08, 0.18] vs. rmidlife = .47, 95% CI [0.03, 0.08] for neuroticism and rold = −.51, 95% CI [−0.11, −0.04] vs. rmidlife = −.35, 95% CI [−0.06, −0.02] for conscientiousness). In both cohorts, the effect of neuroticism was stronger than for conscientiousness. In the older cohort (but not in the midlife cohort), lower extraversion (r = −.44, 95% CI [−0.10, −0.03]), lower openness (r = −.29, 95% CI [−0.06, −0.01]), and lower agreeableness (r = −.30, 95% CI [−0.06, −0.01]) were also associated with higher levels of cognitive complaints.
At the within-person level, we found stable autoregressive effects of cognitive complaints across 20 years in the older cohort, with effect sizes around β = 0.4. In the midlife cohort, the autoregressive effect of cognitive complaints was weaker (β′s around 0.2) and only evident after the second measurement occasion (T2–T3 and T3–T4). We also found autoregressive effects of personality, although the pattern was less consistent. For example, in both cohorts, the autoregressive effects of neuroticism were significant at T1–T2 and T3–T4 but not at T2–T3. For conscientiousness, the effect was only significant at T3–T4 in both cohorts. The autoregressive effects of extraversion and agreeableness were significant in the midlife cohort but not (or less consistent, respectively) in the older cohort, which could indicate more fluctuating changes across time—that is, less “carry-over effects” or no tendency for a continuous change trend over time as may be behind (positive) autoregressive coefficients.
No significant within-person cross-lagged relations between cognitive complaints and neuroticism were found in either cohort. In general, few cross-lagged effects were found. Among middle-aged adults, higher levels of cognitive complaints at T3 were associated with lower extraversion (β = −.20, 95% CI [−0.20, −0.03]) and lower conscientiousness (β = −.21, 95% CI [−0.19, −0.03]) at T4. In the older cohort, higher levels of cognitive complaints at T2 were associated with lower extraversion at T3 (β = −.29, 95% CI [−0.27, −0.02]). In addition, lower conscientiousness at T3 was related to higher levels of cognitive complaints at T4 (β = −.28, 95% CI [−0.86, −0.10]).
We found evidence for concurrent within-person relations between all personality traits and cognitive complaints, although not across all measurement occasions. Consistent with expectations, we found small- to medium-sized change within-person correlations between the residuals of neuroticism and cognitive complaints (β′s = .21 to .44) across all measurement occasions in the midlife cohort and at T2–T4 in the older cohort, respectively. We also found concurrent relations between conscientiousness and cognitive complaints at T3–T4 in both cohorts (β′s = −.20 to −.37). This suggests that higher within-person variation of neuroticism and lower within-person variation of conscientiousness were associated with higher within-person variation of cognitive complaints.
Post hoc power analysis
Cross-Lagged Regression and Occasion-Specific Correlation Power Analysis.
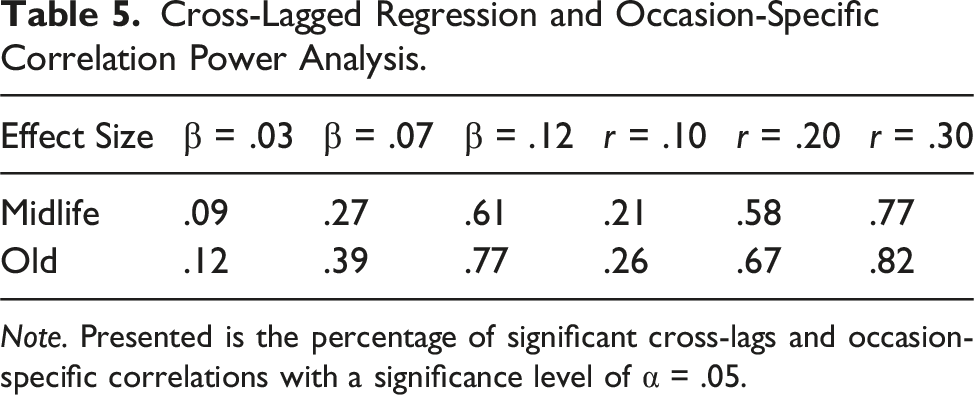

Note. Presented is the percentage of significant cross-lags and occasion-specific correlations with a significance level of α = .05.
Discussion
Using data from two cohorts spanning 20 years, we studied how personality traits and cognitive complaints jointly unfolded between and within middle-aged and older individuals. Four of our five hypotheses were supported: At the between-person level, (1) higher neuroticism and (2) lower conscientiousness were associated with higher levels of cognitive complaints over 20 years; although, in contrast to expectations, the effects were larger in older than middle-aged adults. At the within-person level, we found correlated changes between higher levels of cognitive complaints and (3) higher neuroticism as well as (4) lower conscientiousness. The last hypothesis was not supported by the data, as (5) increasing cognitive complaints were not associated with increasing neuroticism at subsequent measurement occasions within the same individuals. Briefly, the effects were mostly evident at the between-person level, suggesting that the personality-complaint associations varied more across people than within individuals over time. Further, the associations between personality traits and cognitive complaints differed between middle-aged and older adults.
Of note, cognitive complaints were not associated with memory performance in neither cohort. One possible explanation of these null findings may be that cognitive complaints reflect only difficulties that have not been successfully ameliorated through compensation strategies (Burmester et al., 2016). Another explanation is that cognitive complaints reflect cognitive problems in everyday life, while cognitive performance reflects “pure” ability assessed using a task in the laboratory or clinic. A disconnect between “true” cognition in the real life and “pure” cognition in the laboratory has been frequently observed and indicates that individuals’ everyday life is governed not by the decline in cognitive abilities as often measured in the laboratory but by a multitude of compensatory mechanisms (Verhaeghen et al., 2012).
Personality-cognitive complaint associations between individuals
At the between-person level, higher neuroticism and lower conscientiousness were associated with higher levels of cognitive complaints over 20 years in both cohorts, which is consistent with the broad literature on personality and subjective cognition (Aschwanden et al., 2020; Koller et al., 2019; Könen & Karbach, 2018; Sutin et al., 2020). The characteristic mental processes underlying neuroticism and conscientiousness may explain these associations. For example, people with higher neuroticism tend to be more prone to rumination, which may distract from ongoing behavior (Munoz et al., 2013), while, in contrast, the structured mindset of conscientious individuals may help to focus on ongoing behavior (Fleeson & Gallagher, 2009; Sutin et al., 2020). Behavioral factors linked to the traits may further affect such mental processes: Higher neuroticism and lower conscientiousness have been associated with poor sleep (Duggan et al., 2014), which may contribute to daytime sleepiness and impair mental processes, leading to more cognitive complaints.
The associations were almost twice in magnitude for older than middle-aged adults. This contrasts with previous cross-sectional work that found stronger associations at younger ages (Sutin et al., 2020). The present findings indicate the opposite, such that over time, personality may be more predictive of cognitive complaints among older adults. The divergence of findings may be partly due to differences in methodology across the two studies, such as the design (cross-sectional vs. longitudinal), the age range considered (18–92 years vs. early 40s and 60s), the type of analysis (moderation vs. multi-group), and assessment of subjective cognition (25 items to assess cognitive failures vs. six items to measure cognitive complaints). Beyond methodological differences, it is likely that the rate of cognitive complaints affects the strength of the association: In the cross-sectional study, age was negatively associated with cognitive failures (r = −0.24, p < .01), suggesting that younger individuals reported higher levels of cognitive lapses (Sutin et al., 2020). In the present study, the older cohort reported higher levels of cognitive complaints than the midlife cohort (T1: d = 0.64, p < .01). It could be that the personality-complaint association is U-shaped, with the weakest association in middle age. At younger ages, cognitive failures associated with the traits’ processes may be more observable than at older ages, when cognitive failures may become more the norm (Sutin et al., 2020). At older ages, age stereotypes and attitudes toward own aging may become more salient and personality traits may predispose to certain attitudes (Diehl et al., 2014; Kornadt et al., 2019). For example, lower neuroticism and higher conscientiousness have been related to more positive attitudes (Kornadt et al., 2019; Moor et al., 2006) and awareness of age-related gains (Rupprecht et al., 2019). As such, individuals with higher neuroticism and lower conscientiousness may be more vulnerable to negative aging attitudes and report higher levels of cognitive complaints, even in the absence of objective cognitive difficulties.
The stronger association between neuroticism (but also conscientiousness) and cognitive complaints in the older cohort suggests that cognitive complaints appear to be part of the neuroticism spectrum, whereas this seems to be less likely in middle-aged adults. If replicated, this finding may have theoretical implications for personality assessment. For example, it could be useful to adopt an age-sensitive measure of neuroticism (and conscientiousness). As a first step towards this direction, it would be helpful to compare the extent of age-related information captured by different levels of the personality trait hierarchy (traits, facets, and nuances; indexed by individual items) in middle-aged and older adults. Nuances may show age trends different from their traits and facets, and thus capture unique developmental information (Hang et al., 2021; McCrae, 2015). Documenting nuance-specific associations could help researchers to characterize age differences in personality traits in more detail and to develop new measurement models of personality, thereby allowing for more comprehensive personality assessment (Condon et al., 2020; Mõttus & Rozgonjuk, 2021).
Among older adults, lower extraversion, openness, and agreeableness were associated with higher levels of cognitive complaints over time. Previous longitudinal studies focused on neuroticism and conscientiousness (Aschwanden et al., 2018; Comijs et al., 2002; Lane & Zelinski, 2003); thus, the present study seems to be the first examining all FFM personality traits and cognitive complaints over time. Although there is cross-sectional meta-analytic evidence that extraversion, openness, and agreeableness are associated with cognitive complaints (Aschwanden et al., 2020), these associations tend to be less robust and less consistent than for neuroticism and conscientiousness—a pattern that has been found in the present study too and extends to the general cognitive aging literature (Graham et al., 2021; Kliegel et al., 2005; Luchetti et al., 2016; Terracciano et al., 2022; Wettstein et al., 2017). Nevertheless, it could be that individuals high in extraversion are more likely to engage in complex social situations that stimulate them cognitively (Stephan et al., 2014) and buffer against cognitive complaints (Curtis et al., 2015). Or, as individuals high in extraversion tend to have greater global self-efficacy, they may make more positive evaluations of their cognition and report lower levels of cognitive complaints (Sutin et al., 2020). Likewise, people with high openness tend to have a stronger belief in their intellectual capacities and creativity (Goldberg, 1999), which may lead to fewer perceived cognitive problems and result in lower levels of cognitive complaints. It is also possible that individuals higher on openness have better cognitive reserve because they are more likely to be cognitively engaged (e.g., learning a new skill or language) (Curtis et al., 2015; Stephan et al., 2014) and thus have lower levels of cognitive complaints. On the other hand, being less forgiving and more aggressive (i.e., lower agreeableness) may lead to more rumination (Pronk et al., 2010) and interfere with the ability to focus on cognitive actions, which in turn may result in higher levels of cognitive failures (Sutin et al., 2020).
Personality-cognitive complaint associations within individuals
At the within-person level, we found positive autoregressive effects for both personality and cognitive complaints across most measurement occasions. These findings align with previous between-person research on rank-order stability of personality (Olaru & Allemand, 2021; Roberts & DelVecchio, 2000; Terracciano et al., 2006) as well as our between-person test–retest correlations (Table S2), suggesting that both constructs are relatively stable within and between individuals over time. Moreover, all five traits were concurrently related to cognitive complaints, with small to medium-sized effects (although not across all measurement occasions). For example, higher within-person variation of neuroticism and lower within-person variation of conscientiousness were associated with higher within-person variation of cognitive complaints in both cohorts. This implies that on measurement occasions when individuals reported higher neuroticism and lower conscientiousness, they also reported higher levels of cognitive complaints. This is consistent with findings from both the cross-sectional literature (Aschwanden et al., 2020; Koller et al., 2019; Könen & Karbach, 2018; Sutin et al., 2020) and the present longitudinal between-person perspective. As such, it could be that changes in personality and cognitive complaints are systematically related to each other. This perspective of correlated change is strongly linked to common factor theories, such as the common cause hypothesis (Allemand et al., 2007; Baltes & Lindenberger, 1997). It would mean that personality and cognitive complaints have a common cause (and may or may not be causally related to each other), such as stress, for example, that may cause both increases in neuroticism as well as increases in cognitive complaints. Or, changes in cognitive complaints may be caused by changes in neuroticism (or vice versa) through the mechanisms discussed earlier (e.g., mental processes and behavioral factors like sleep). An important avenue for future research is to identify common causes and/or underlying mechanisms of correlated change between personality and cognitive complaints, as the concept of correlated change has great potential for research implications (Allemand & Martin, 2016)—namely, it could inform future intervention programs aimed at maintaining cognitive health and psychological well-being. If decreases in neuroticism and increases in conscientiousness are systematically associated with decreases in cognitive complaints, personality interventions (Stieger et al., 2021) could be developed to support cognitive aging and well-being in general (Aschwanden & Allemand, 2020), considering that cognitive complaints can lead to anger and increased stress (Metternich et al., 2010).
No significant cross-lagged relation between cognitive complaints and neuroticism was found, indicating that within the same person, changes in cognitive complaints did not predict changes in neuroticism (and vice versa) at subsequent measurement occasions. In general, only few cross-lagged effects were found and evidence for bidirectionality was limited, such that there was no consistent pattern across time or cohorts. The lack of within-person cross-lagged effects may imply, for example, that increases in cognitive complaints do not necessarily increase individuals’ neuroticism at a subsequent measurement occasion, as increases in cognitive complaints may lead to help-seeking behavior (e.g., visiting a memory clinic) or be explained meaningfully (e.g., “I have a stressful phase at work that will pass”), thereby extenuating potential increases in neuroticism and resulting in a null cross-lagged effect. It may also be that increases in cognitive complaints are not impactful enough to shape changes in personality traits, or, maybe only in specific facets or nuances, which may further depend on the cause for the complaints (cognitive dysfunction vs. stress at work). For example, the onset of cognitive impairment may be upsetting and lead to increases in the anxiety facet of neuroticism. As such, some personality changes may be different from age-related patterns that can occur in individuals without incident impairment (Wagner et al., 2016; Wettstein et al., 2020).
The lack of within-person (cross-lagged) associations suggests that personality dynamics may be more complex and context-dependent than previously thought. Personality may interact with contextual factors in nuanced ways, influencing behavior differently across situations. Personality traits and cognitive complaints may fluctuate independently over time, or their relationship may be influenced by other unmeasured variables. There are also some statistical and conceptual considerations regarding the mainly null findings. On the statistical side, our study was underpowered to detect small and moderate cross-lagged effects (Table 5). It could be that we thus missed some effects. Conceptually, the time interval between the assessments was long (i.e., four and eight years). Given that associations are more dynamic at the within-person than between-person level, time intervals that are too short or too long based on the nature of the variables of interest can produce data that might be overly sensitive to measurement error or insensitive to variability and change (Hertzog & Nesselroade, 2003). Furthermore, it could be that interactions (or combinations) of personality traits are more relevant than single traits in predicting changes of cognitive complaints. For instance, someone with both high neuroticism and conscientiousness may show decreases in cognitive complaints because this person is (a) worried about their own (cognitive) health and (b) thus uses behavioral strategies to help reduce cognitive problems (e.g., participating in a cognitive training or improving stress management). On the other hand, someone with high neuroticism but low conscientiousness may show increasing cognitive complaints as this person is (a) worried about their own (cognitive) health but (b) does not engage in any (helpful) behavioral strategies. Moreover, personality traits may function as moderators in the relationship between cognitive complaints and cognitive functioning. For example, previous research (Hülür et al., 2015) showed that the positive association between levels of subjective memory and memory performance was stronger for more conscientious participants. People who are more conscientious may be more likely to accurately monitor memory problems on average and are perhaps also less likely to experience memory problems because they use behavioral strategies that help avoid memory errors (Hertzog & Pearman, 2014).
Strengths and limitations
The present study has several strengths, such as the long observational period of 20 years, the inclusion of two age groups, and the analytical approach that considered bidirectionality and allowed to disaggregate between-person differences from within-person variation. Nevertheless, the following limitations deserve consideration. Although the data are longitudinal, they are observational and do not allow to draw conclusions about causality. The time intervals between repeated assessments may have been too long, especially when investigating potential cross-lagged effects. Generalizability of findings is limited to some extent given the challenges involved in longitudinal studies. Reduction in sample size was particularly evident in the old cohort over 20 years, which is, however, practically unavoidable in samples of older adults. Of note, selective attrition was relatively modest (e.g., dropouts and continuers did not differ in memory performance or cognitive complaints in both cohorts). Nevertheless, while we still had a decent number of people for the between-person comparisons, our sample size was not powered for detection of cross-lags of β < .12 and occasion-specific correlations of r < .30. Moreover, the surveys were not developed to explicitly measure within-person variation. This may also partly explain why we found more between-person versus within-person variation in the personality-complaint association. Future studies could focus on shorter time scales (e.g., days). Experience sampling methodologies allow to measure cognitive complaints as they happen in daily life, but research on this area is sparse (Aschwanden et al., 2019; Könen & Karbach, 2018; Mogle et al., 2022). Moreover, our personality measure did not allow assessment of personality at lower levels of the personality trait hierarchy (facets and nuances). Such analyses could provide a more detailed picture of how the traits are associated with cognitive complaints (Sutin et al., 2020). With the present work, it is not possible to tell which of the three conceptual models explains how much of the associations or whether some trait associations are more likely than others to be accounted by the suggested models. In future studies, these models need to be tested and potential mechanisms need to be identified. For neuroticism, the mental processes model may explain more variance than the other models as mental noise is a characteristic process of neuroticism (Flehmig et al., 2007; Robinson & Tamir, 2005), and previous work (indirectly) weakens the models of cognitive abilities (Aschwanden et al., 2018) and reporting bias (Hill et al., 2020; Lange & Süß, 2014; Slavin et al., 2010; Sutin et al., 2019). For the remaining traits, it is difficult to suggest a specific model without speculating too much beyond the available data. Finally, in ILSE, the internal consistency for openness is low across all four measurement occasions, particularly in the old age group (Wettstein et al., 2020). However, we are confident that openness can be considered as a reliable measure, considering that we used the well-established NEO-FFI for personality assessment and Cronbach’s alpha corresponds to a conservative estimation approach (Shevlin et al., 2000). For example, the alpha may be lower due to a restricted interindividual item variability or to a heterogeneous item content because of different facets that are part of openness.
Conclusion
The cognitive health literature suggests that neuroticism and conscientiousness are both consistent cross-sectional correlates of cognitive complaints and robust long-term predictors of risk for poor cognitive health. The present study adds to this literature that the personality-complaint associations are not only evident cross-sectionally but also over two decades in both middle-aged and older adults. These associations were stronger in older than middle-aged adults, and in general, the associations varied more across people than within individuals over time. These findings further strengthen the idea that personality provides information to identify individuals with a vulnerable personality (high levels of neuroticism and low levels of conscientiousness) who may benefit most from preventive interventions to maintain cognitive health and psychological well-being. These individuals could also benefit from personality interventions (Stieger et al., 2021) that aim to decrease neuroticism and increase conscientiousness. Or, cognitive interventions themselves may have the potential to positively impact personality traits (Jackson et al., 2012; Sander et al., 2017), such as emotional stability (i.e., reversed neuroticism), which was found to be the primary trait domain of the FFM traits showing changes as a result of interventions (Roberts et al., 2017). Hypothetically, a combined cognitive–personality intervention that improves cognitive performance and reduces cognitive complaints may successfully maintain emotional stability and general well-being in older age (Aschwanden et al., 2018). Future research is required to identify the underlying mechanisms and factors that facilitate or inhibit such changes over time, before the applicability of a combined cognitive–personality intervention needs to be established as well the feasibility of a systematic application of personality surveys in public health needs to be determined.
Supplemental Material
Supplemental Material - Longitudinal associations between personality traits and cognitive complaints in midlife and older age across 20 years
Supplemental Material for Longitudinal associations between personality traits and cognitive complaints in midlife and older age across 20 years by Damaris Aschwanden, Mathias Allemand, Matthias Kliegel, Angelina R. Sutin, Martina Luchetti, Yannick Stephan, Oliver Schilling, Hans-Werner Wahl, Gabriel Olaru, and Antonio Terracciano in European Journal of Personality.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute on Aging of the National Institutes of Health under Award Numbers R01AG068093 (PI: Antonio Terracciano) and R01AG053297 (PI: Angelina R. Sutin). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. Data came from the Interdisciplinary Longitudinal Study of Adult Development and Aging (ILSE). ILSE’s fourth wave of data collection was supported by the Dietmar Hopp Foundation. Financial support for the previous waves came from the German Federal Ministry for Family, Senior Citizens, Women, and Youth (grant numbers 314-1722-102/16 and 301-1720-295/2). The study was carried out in accordance with the Declaration of Helsinki and approved by the Ethics Committee of the Medical Faculty of University of Heidelberg (No. S-371/2013) in Germany.
Open science statement
The hypotheses and statistical analyses were not preregistered. The samples sizes were determined using the existing ILSE data (nmidlife = 502 at T1; nold = 500 at T1). A post hoc power analysis was condcuted, showing that only large effects (cross-lags of β ≥ .12 and occasion-specific correlations of r ≥ .30) could be detected with (close to) adequate power (.80). Information on the measures used is reported in this manuscript as well as in more detail in the ILSE overview paper (Sattler et al., 2017). Due to legal restrictions, ILSE material can only be made available if a written data agreement has been signed. The materials (https://www.maelstrom-research.org/study/ilse) are available upon request (![]() analyzed data from 607 participants of the first measurement occasion and examined the cross-sectional association between cognitive test performance, negative age stereotypes, depressive symptoms, neuroticism, and conscientiousness on cognitive complaints. The present study differs in its research question, the analytical design, the consideration of all four measurement occasions as well as both age cohorts.
analyzed data from 607 participants of the first measurement occasion and examined the cross-sectional association between cognitive test performance, negative age stereotypes, depressive symptoms, neuroticism, and conscientiousness on cognitive complaints. The present study differs in its research question, the analytical design, the consideration of all four measurement occasions as well as both age cohorts.
Open data statement
We are not allowed to release the subsets of ILSE data used for the present analyses due to the ILSE’s conditions of use. Due to legal restrictions, ILSE data can only be made available if a written data agreement has been signed. The data are available upon request (
Reproducible script statement
Transformation and non-standard scoring statement
We did not transform any data for the reported analyses.
Covariates statement
Gender, education, subjective health, objective health, and memory performance were included as plausible confounders of the hypothesized associations. Gender and education were selected because they are common sociodemographic covariates in the field of personality and cognitive complaints (Steinberg et al., 2013; Sutin et al., 2020). Note that ILSE did not assess data on race or ethnicity. Further, personality and cognitive complaints share common associations with many psychosocial and health-related variables. We aimed for a parsimonious model and included subjective health and objective health as covariates, which likely subsume a broad variety of psychosocial and health-related confounders (Aichele et al., 2016; Ocampo, 2010). We controlled for memory performance as it is sensitive to age effects and often the earliest and most central deficit of Alzheimer’s disease (Jessen et al., 2014).
Effects statement
We report basic descriptive statistics, effect sizes, exact p-values, and 95% confidence intervals.
Supplemental Material
Supplemental material for this article is available online.
Note
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
