Abstract
Introduction
The need for breast radiologists is increasing but the workforce supply does not match the demand. A 2009 United States (US) study forecasted the low number of newly graduated radiologists going into this field would result in reduced breast imaging (BI) workforce over the next 15-20 years. 1 Likewise, BI is deemed to be one of the top subspecialties for prospective hires in Canada, especially in the Prairie Provinces and Quebec. 2 While there has been increased interest in BI fellowship training in the past decade (0-1% in 2016 and 7% in 2009-2011) among Canadian residents, this field is still considered by many to be less attractive compared to other subspecialties.3,4 There is a continued onus to recruit more radiology trainees to BI.
Early clinical exposure, good curriculum, mentorship, and research opportunities are essential for recruiting trainees to any subspecialty in radiology.4,5 The purpose of this study is to assess the level of interest in BI among current trainees, explore their perspectives and exposure to BI, and identify factors preventing them from pursuing this field. To our knowledge, this is the only Canadian study dedicated to assessing trainees’ perception of BI. Both medical students and residents were surveyed to draw comparisons between the 2 groups and propose solutions to increase interest in BI early in training.
Methods
REB approval was obtained through the Ottawa Hospital Research Institute. Need for consent was waived. This study gathered information on training, actual vs preferred timing of breast rotations during residency, fellowship choices, perceived positive and negative attributes of BI, and opinion of how artificial intelligence (AI) will impact BI. The electronic survey was created using Google Forms and contained 10 questions in the version for medical students and 8 additional questions in the version for radiology residents with multiple-choice (both “select one” and “select all that apply”) and open-ended questions.
The survey was sent to all 16 radiology programs’ chief residents and all 17 medical schools’ radiology interest group or Aesculapian society representatives in Canada via email, and they were asked to distribute it to all residents in postgraduate years (PGY) 1-5 and all medical students from years 1-4. The survey was advertised on the Canadian Society of Breast Imaging (CSBI) website and social media. Trainees were encouraged to send an email to CSBI if they had questions regarding the survey or were interested in connecting with a mentor. A reminder was sent 2 weeks after chief residents and medical school representatives were first contacted. Responses were collected from November 2020 to February 2021.
Frequencies and statistical analyses were computed using IBM SPSS Statistics and SAS software.6,7 The significance level was set at .05.
Chi-square tests (or Fisher’s exact tests, when expected cell counts were <5) were performed to determine associations between: (1) perceptions about BI, and whether trainees were a medical student or resident and (2) perceptions about AI on BI, and whether trainees were interested in BI/women’s imaging (WI) fellowships. Though some programs are transitioning away from using “women’s imaging” toward more gender-neutral terminology, at the time of our survey “women’s imaging” was the term most often used by Canadian radiology programs.
Odds ratios (ORs) and 95% confidence intervals (CIs) were computed using univariate logistic regression to determine the impact of (1) perceptions about BI on interest in pursuing a BI/WI fellowship for all respondents, with subgroup analyses for medical students and residents and (2) time of first breast rotation (PGY1-2, PGY3, or PGY4-5) on interest in BI/WI fellowships for residents. For negative perceptions of BI, the event of interest was not choosing BI/WI fellowship. For positive perceptions of BI, the event of interest was choosing BI/WI fellowship.
Results
Survey Respondent Demographics
Demographics of Survey Respondents by Region and Level of Training.
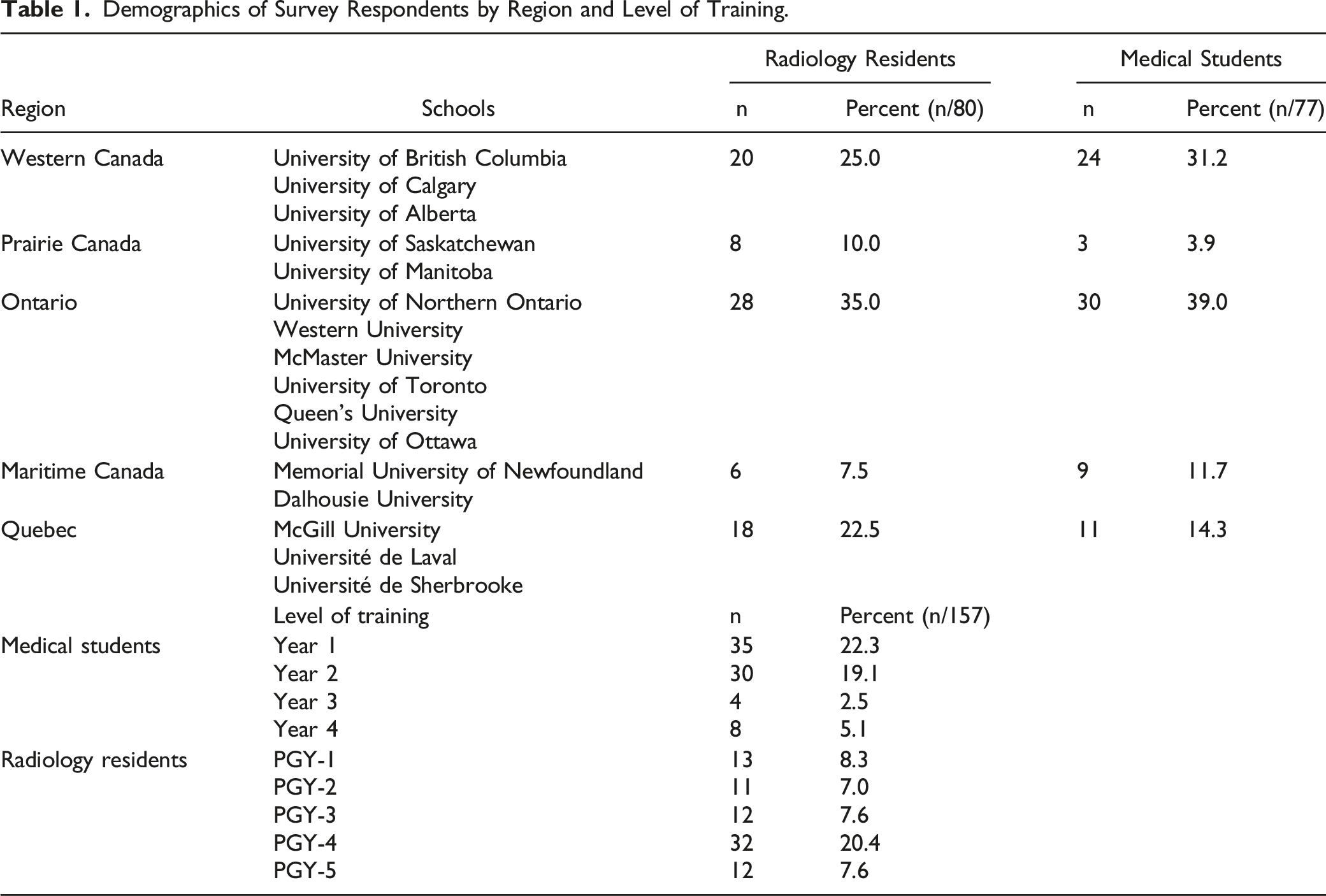
Top Fellowships Desired by Respondents
Radiology Subspecialty Interests of Radiology Residents and Medical Students. This was a Select-all-that-Apply Question, Each Respondent Could Choose More than 1 Option.
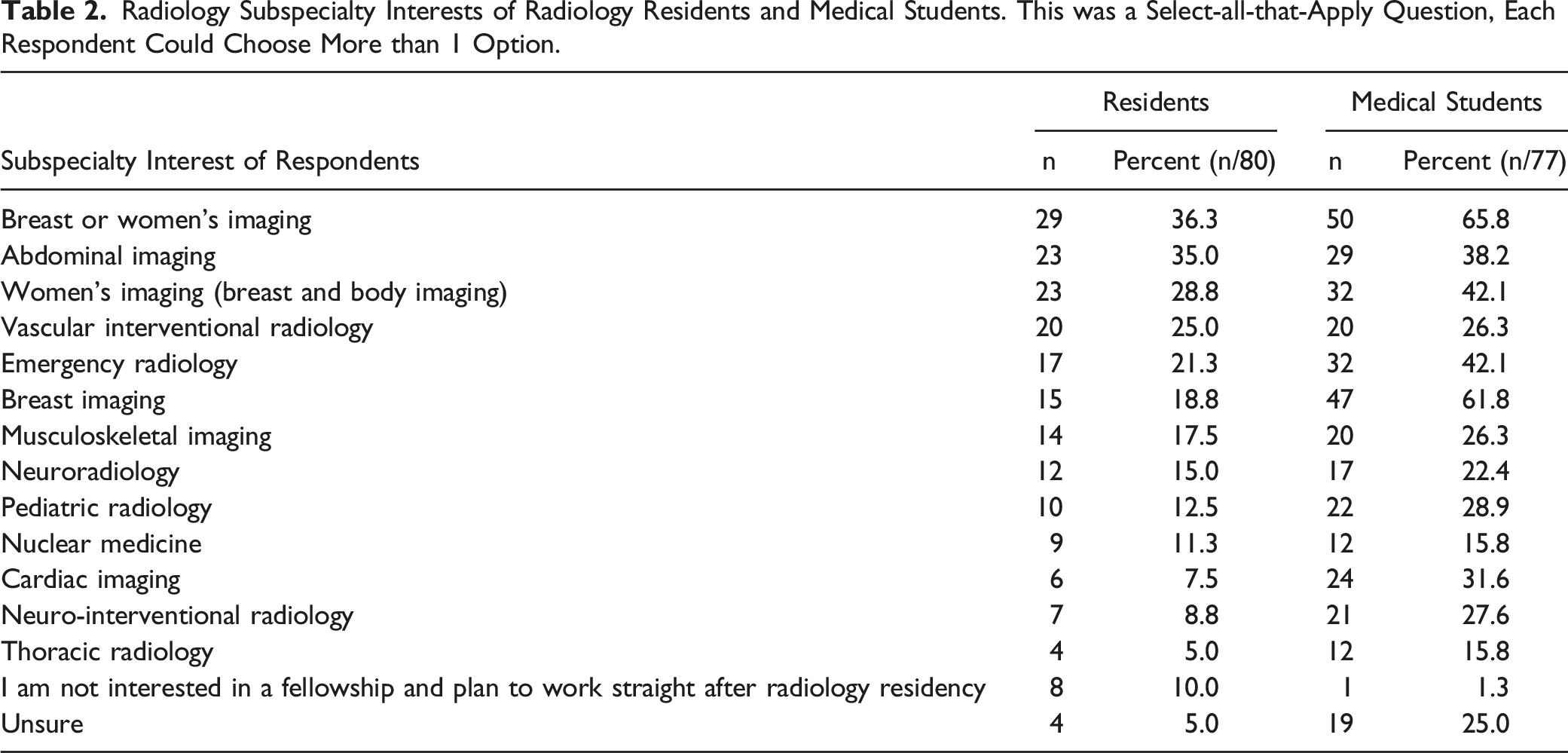
Mentorship and Research
Thirty-seven percent of the trainees (59/157), comprising 22.5% residents (18/80) and 53.2% medical students (41/77), indicated interest in connecting with a BI mentor. However, only 6 trainees emailed CSBI and were matched with a local mentor. A small proportion of medical students (1.3%, 1/77) and residents (21.3%, 17/80) had conducted BI research.
Reasons why Respondents were Not Interested in BI/WI
Impact of Negative Perceptions of Breast Imaging (BI) on Interest in Pursuing Breast/Women’s Imaging (BI/WI) Fellowships. The Perception Questions in Table 3 and Table 4 were Select-All-That-Apply Questions. “Other” perception Indicates Free Text Responses. Frequencies, OR, 95% CI, and P Values are Shown. Asterisk (*) Indicates P < .05. For (a), the Event of Interest was Being Disinterested in Breast/Women’s Imaging Fellowship. “.” Indicates that the Analysis Could Not be Performed due to Zero Observations Under one of the Groups. P^ Columns in Table 3 and Table 4 Show Associations Between Each Perception and Whether Trainees were a Medical Student or a Resident.
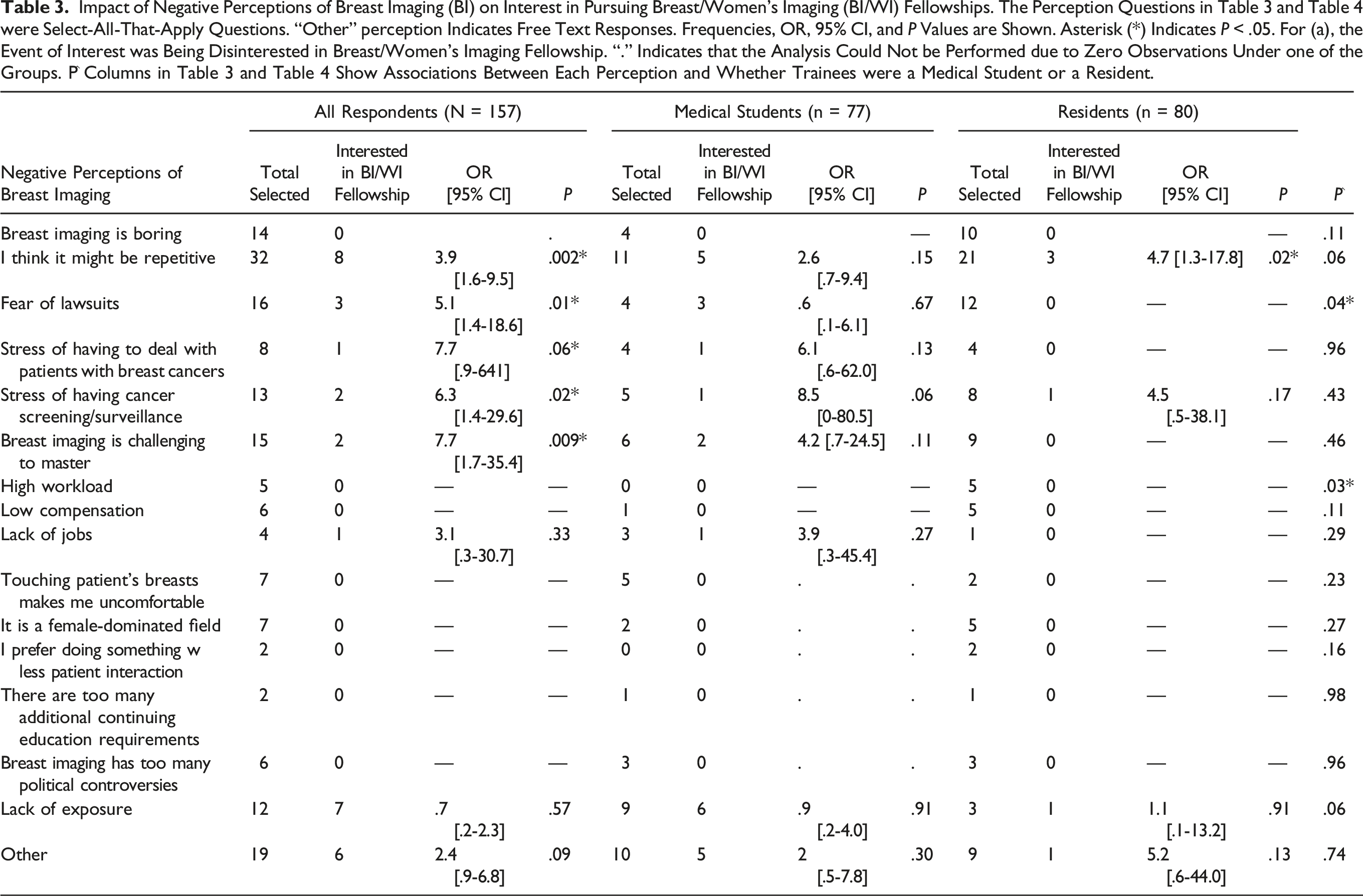
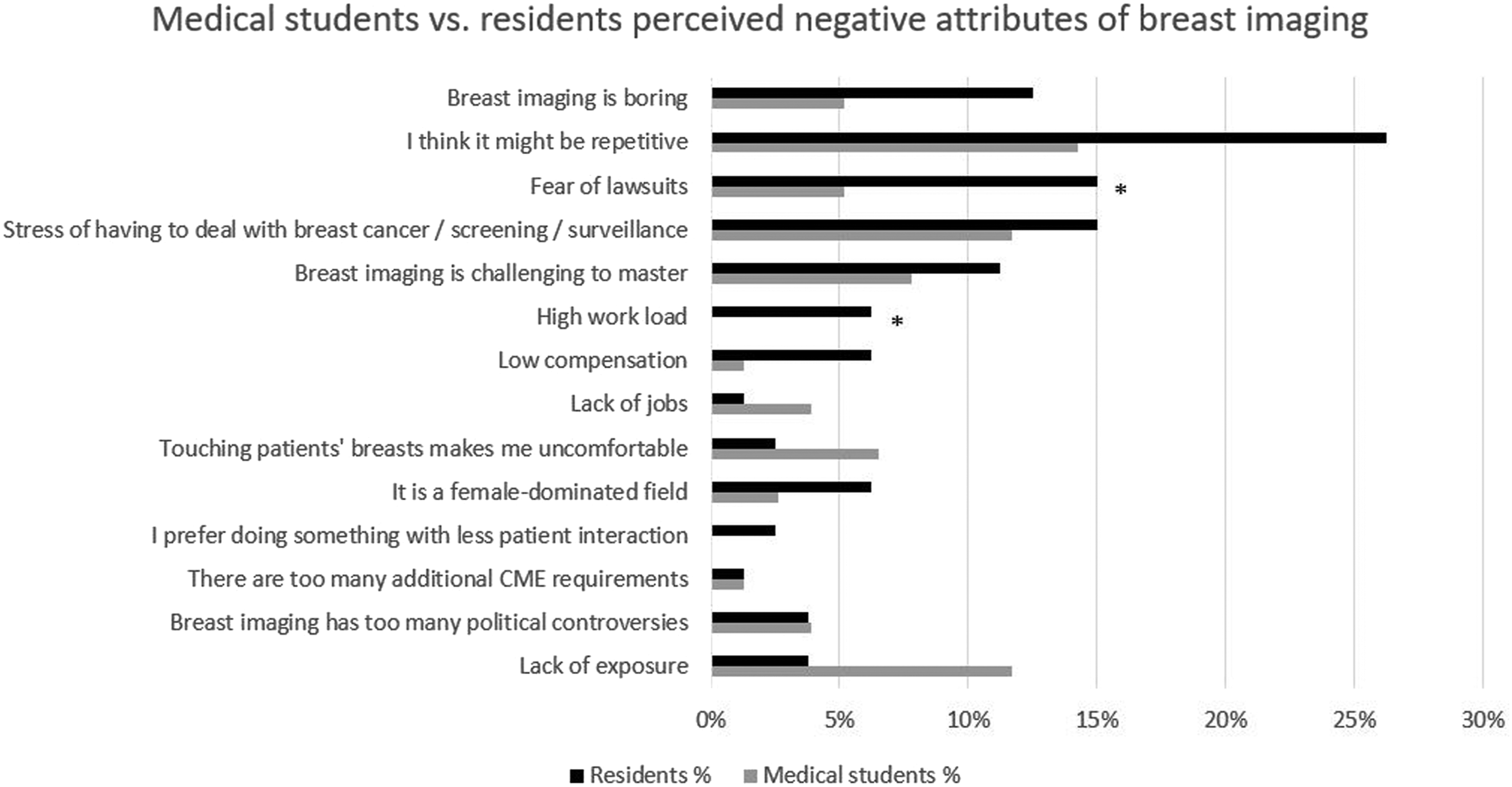
Reasons residents and medical students were not interested in breast/women’s imaging. Asterisk (*) indicates a significant difference in the proportion of medical students compared to residents who considered this as a reason not to pursue breast imaging.
Reasons Why Respondents were Interested in Breast Imaging/Women’s Imaging
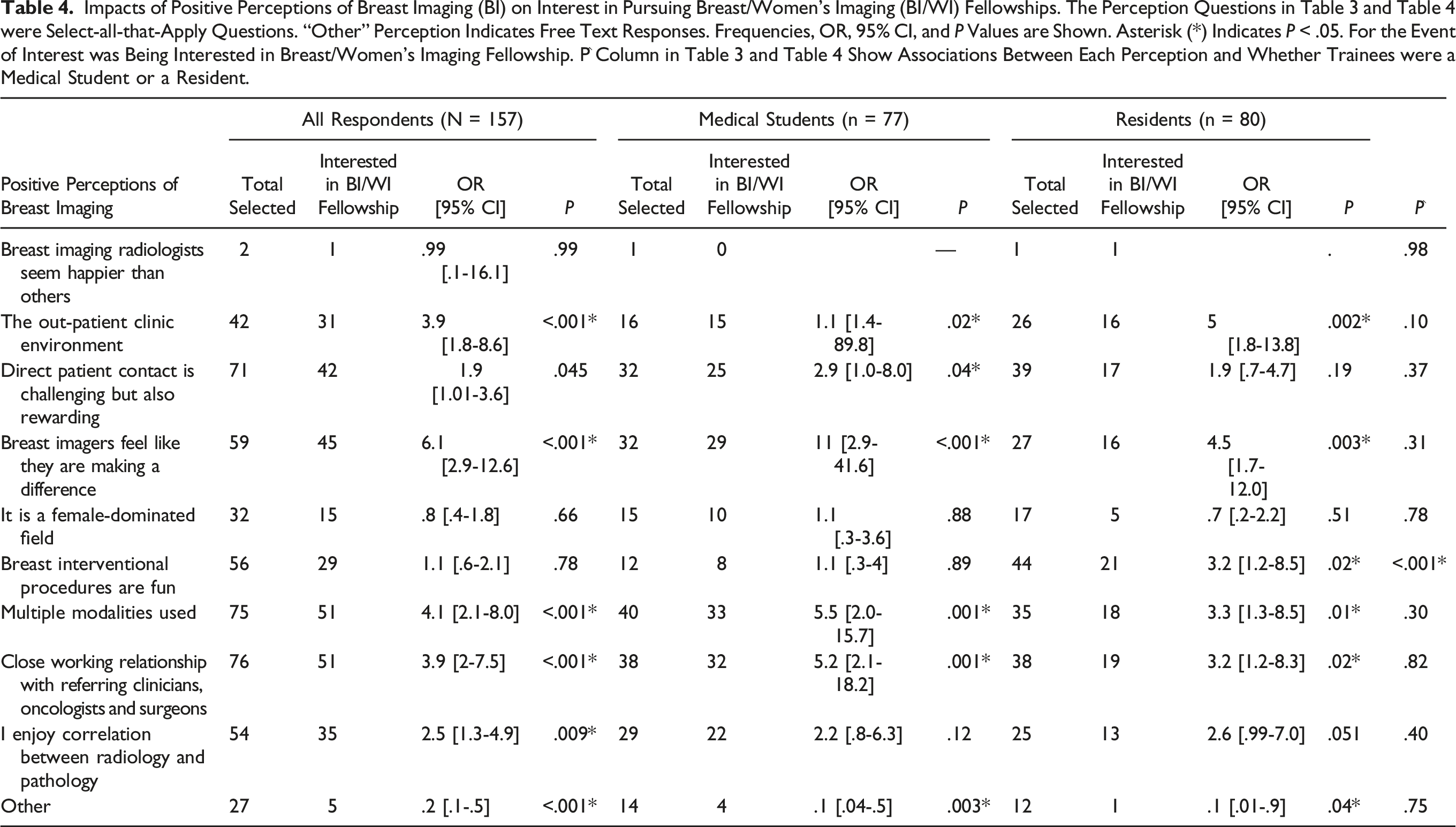
The reason unique to medical students was “Direct patient contact is challenging but also rewarding” (OR = 1.9, 95% CI: 1.0-3.6, P = .0045). The reason unique to the resident cohort, was “breast interventions are fun” (OR = 3.2, 95% CI: 1.2-8.6, P = .02). Compared to radiology residents, significantly fewer medical students considered procedures as a reason to pursue BI/WI (16% vs 55%, respectively, P < .001). All other reasons had similar response rates (P > .05) between residents and medical students (Figure 2 and Table 4). Reasons residents and medical students were interested in breast or women’s imaging. Asterisk (*) indicates a significant difference in proportion of medical students compared to residents who considered this as a reason to pursue breast imaging. Impacts of Positive Perceptions of Breast Imaging (BI) on Interest in Pursuing Breast/Women’s Imaging (BI/WI) Fellowships. The Perception Questions in Table 3 and Table 4 were Select-all-that-Apply Questions. “Other” Perception Indicates Free Text Responses. Frequencies, OR, 95% CI, and P Values are Shown. Asterisk (*) Indicates P < .05. For the Event of Interest was Being Interested in Breast/Women’s Imaging Fellowship. P^ Column in Table 3 and Table 4 Show Associations Between Each Perception and Whether Trainees were a Medical Student or a Resident.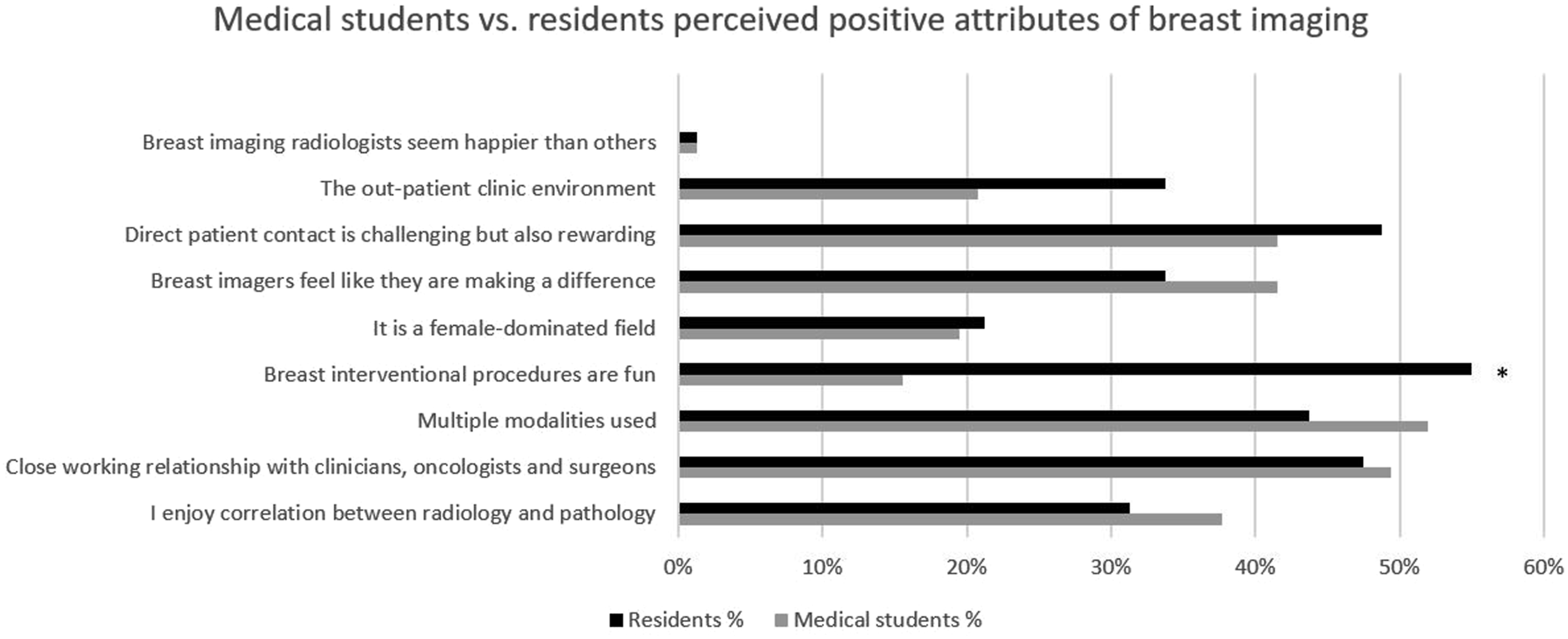
Timing of Breast Rotations
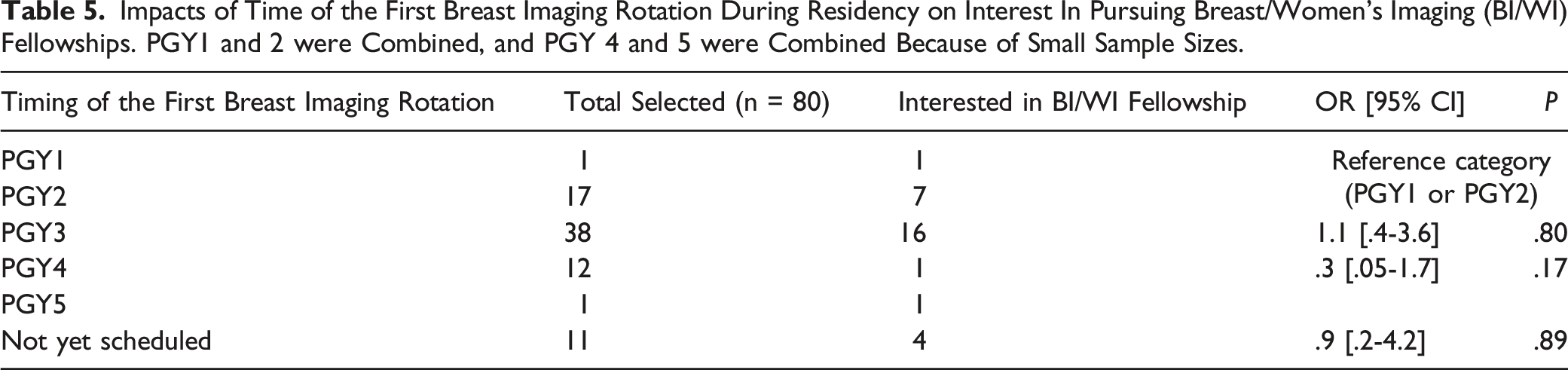
Impacts of Time of the First Breast Imaging Rotation During Residency on Interest In Pursuing Breast/Women’s Imaging (BI/WI) Fellowships. PGY1 and 2 were Combined, and PGY 4 and 5 were Combined Because of Small Sample Sizes.

Frequency of Breast Imaging Interpretation or Procedures by Residents
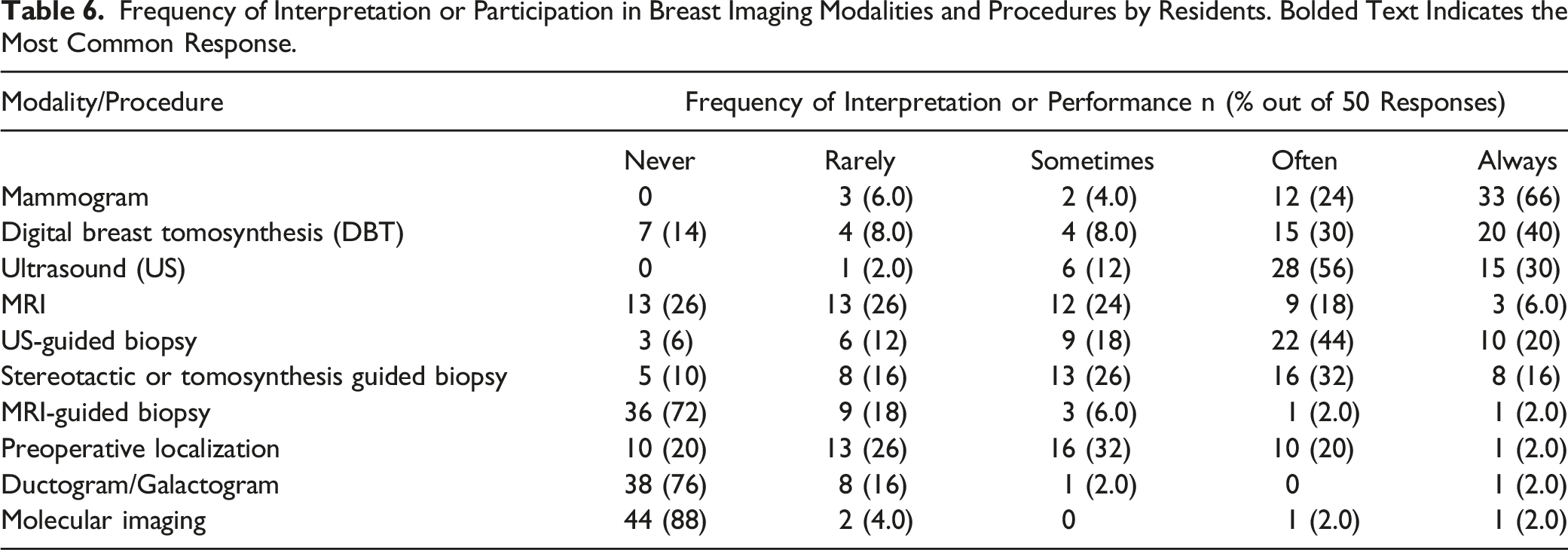
Frequency of Interpretation or Participation in Breast Imaging Modalities and Procedures by Residents. Bolded Text Indicates the Most Common Response.
Breast Imaging Educational Resources
The most common educational resources used by radiology residents are BI-RADS atlas (n = 57), 8 electronic textbooks (n = 50) and in-person didactic lessons (n = 40). Trainees were allowed to select more than 1 choice. BI-RADS atlas (P < .01), question bank (P < .01), online textbook (P < .01), and flashcards (P = .02) were significantly associated with increased level of training in radiology.
Future of Breast Imaging
Most respondents (74.5%, 117/157) believed that “AI will improve BI in many ways.” Significantly more trainees disinterested in BI/WI fellowships compared to those who were interested believed that “AI will decrease the need for future breast radiologists” (20.5% vs 8.9%, 16/78 vs 7/79, P = .04) (Figure 3). Perceptions of residents and medical students on artificial intelligence and breast imaging.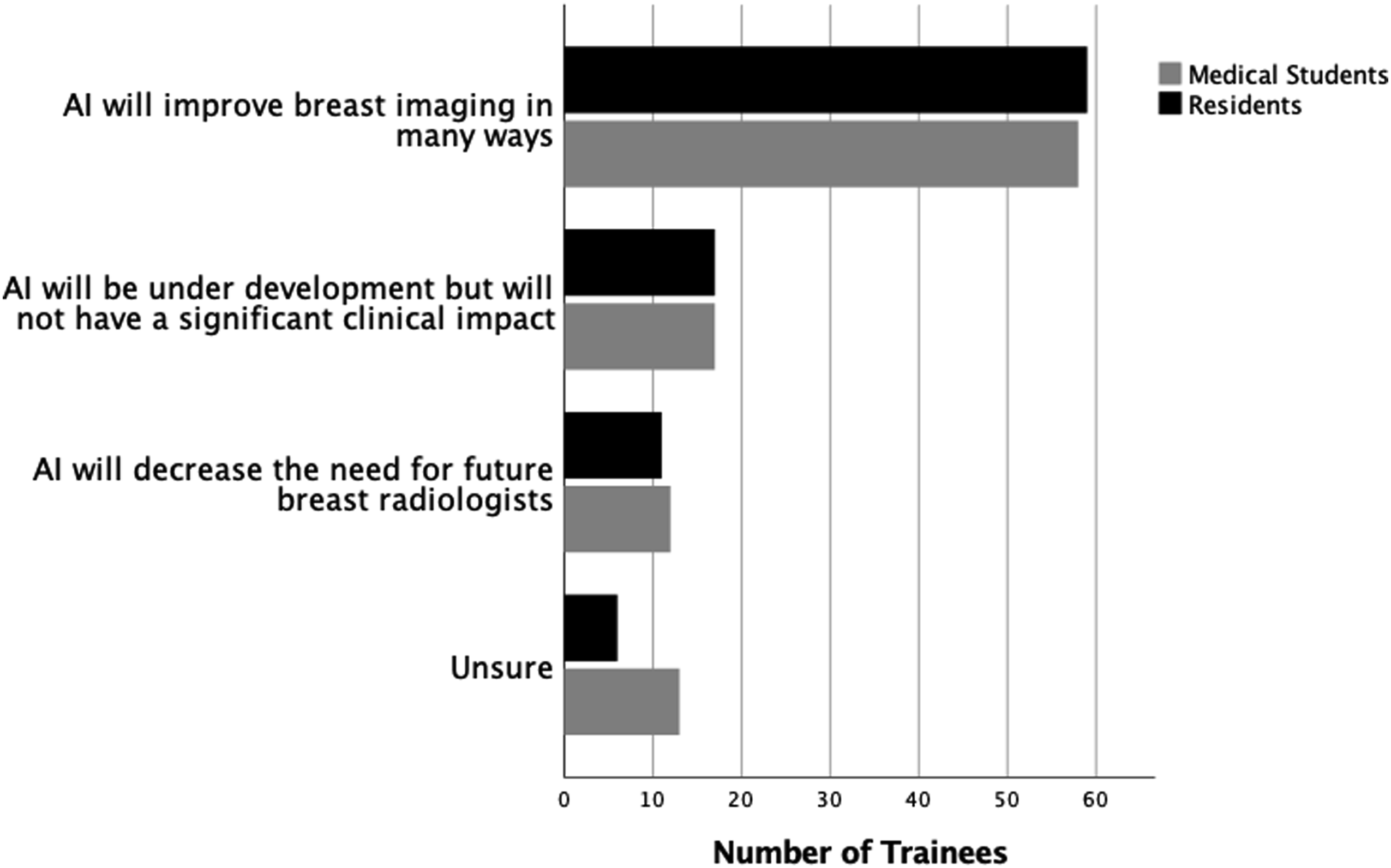
Discussion
A total of 157 responses from 80 radiology residents and 77 medical students were collected. The top 3 fellowship subspecialties desired by residents were BI/WI, abdominal imaging, and interventional radiology. The most common negative perception of BI shared by medical students and residents was repetitiveness. While the most common reason residents found BI appealing were procedures, this was not the case among medical students. Although the majority of the medical student respondents were interested in BI, only 1 had conducted research in this field. Most residents had their first BI rotation in the mid to later years of training. Forty percent of the residents reported that starting breast rotations in first or second year would affect their fellowship choice. The most common educational resources used by radiology residents were BI-RADS Atlas, textbooks (e-book/online format), and in-person didactic lectures. There were many areas where residents may not have received adequate training, including MRI interpretation, MRI-guided biopsy, ductogram/galactogram, and breast nuclear medicine. More trainees disinterested in BI/WI believed that AI will decrease the need for breast radiologists.
This is the first multi-institutional, Canadian study dedicated to exploring trainees’ interest in BI. It serves as an update from prior Canadian surveys on fellowship training in 2009-2011 and 2016 that identified the top fellowship subspecialties as musculoskeletal (12-20% and 19%, respectively), abdominal (19-30% and 17%) and interventional (6-18% and 14%) imaging.3,4 Responses from medical students and residents were directly compared in our survey, which facilitates the discussion of solutions to make BI more attractive to junior trainees, even before they become radiology residents.
Similar to our study, several US surveys identified “fear of lawsuits” as one of the most common reasons for not choosing breast radiology,9-11 which is unsurprising given the recent increase in mammography-related litigation. 11 While breast radiologists face higher litigation rates compared to other radiology subspecialties, they substantially overestimate their risk of a future malpractice lawsuit. 12 Workshops on how radiologists can avoid breast-related litigation may help relieve anxiety.
Other reasons identified were “not an interesting field”9,10 and “too stressful.”8,9 BI has many unique patient-facing, multi-modality and multidisciplinary workflows that may appeal to trainees. 13 Compared to other radiology subspecialties, breast radiology is a relatively hands-on field with many opportunities to perform procedures under sonographic, mammographic, or MRI guidance. Breast radiologists take ownership of patient care by having the ability to recall patients and may often be the first to disclose cancer diagnosis to patients. Furthermore, they play an active role in radiology-pathology correlation and multidisciplinary rounds for management of breast cancer patients. It would be worthwhile to explore specific aspects that make BI seem boring and stressful in future surveys.
A third reason previously identified was low reimbursement,9,11 which may account for why 63% of radiology residents did not want to spend more than a quarter of their clinical practice time in mammography. 1 While this might be a more prevalent factor in the private health care setting, monetary compensation also drives many high volume community practices in Canada. 14 Radiologists can bring in greater earnings for their group by interpreting studies that are disproportionately better compensated than mammograms, such as musculoskeletal MRIs. Improving efficiency with protocols and workflows, as well as advocating for adequate billing for breast studies would level out the playing field. CSBI has recently released a statement on the benefits of digital breast tomosynthesis, which could be used in negotiations for appropriate compensation. 15
In a survey by Baxi et al. with 344 radiology residents in New York and New Jersey, respondents endorsed job availability, flexible work schedules, and fewer calls or emergencies as positive attributes of the practice. 9 While these reasons were not directly explored by our survey, benefits of the outpatient environment were considered by a third of our respondents’ as positive. These benefits could be emphasized in radiology interest groups, departmental dinners, “why radiology lectures,” mentorship, research and observerships/electives. 5 Incorporating hands-on breast interventions might attract more trainees to this field.
In a survey by Lee et al. with 2018-2019 applicants of the Society of Breast Imaging (SBI) Fellowship Match, 37% of residents had their first BI rotation in PGY2, 59% in PGY3, and 4% in PGY4. 13 Having earlier breast rotations is even more important for Canadians due to the earlier fellowship application timeframe. One reason for late introduction to BI might be due to the focus on core subspecialties important for call at the beginning of residency. Flexibility should be given to residents to rotate through BI during late PGY2 year after completion of core rotations, so that residents have enough time to make an informed decision regarding fellowship.
Royal College of Physicians and Surgeons requires residents to have “Four blocks of BI, which must include mammography, ultrasound, MRI, nuclear imaging, and interventional procedures under ultrasound and MRI guidance.” 16 However, many trainees had limited exposure to some of these modalities. Trainees should use a variety of educational resources to supplement key concepts and consider doing external electives at large breast centers to gain adequate exposure to the breadth and depth of BI. Fragomeni et al. demonstrated in a SBI-issued survey of 271 practicing breast radiologists that fellowship training in BI/WI is important in preparing trainees for future practice. 17 This study demonstrated that fellowship-trained radiologists were more likely to perceive that they received sufficient training vs those without fellowship training (84% vs 62% for screening mammography, 93% vs 57% for diagnostic BI, 65% vs 14% for breast MRI, and 93% vs 44% for breast procedures). 17 In addition, 18.7% of the respondents had not anticipated that they would have to interpret BI in their daily practice. 17 This highlights the importance of sufficient BI training, particularly in MRI and procedures, for all radiology trainees, even those who do not plan on specializing in BI. Addressing these inadequacies in the Canadian residency curriculum and encouraging pursuit of dedicated BI/WI fellowship would increase confidence in BI interpretation and procedures.
Greater interest in WI than pure breast fellowship is concordant with findings in a previous Canadian study by Ryan et al. from 2011. 3 Developing multiple skillsets may increase adaptability into community practice and suit those who have interests in multiple subspecialties. To our knowledge, there are only 3 Canadian universities (University of Toronto, McMaster University, and Western University) that offer combined (breast and abdominal/cross-sectional imaging) fellowships.18-20 Increased availability of such programs may promote trainees’ interests in BI.
The negative impact of AI on radiology (i.e. the potential decrease in the demand of radiologists as a result of increased productivity) is often exaggerated, producing pessimism and uncertainty in those who are considering radiology. 21 A survey of 322 Canadian medical students in 2018 found that the majority agreed AI would reduce the demand for radiologists, and anxiety related to radiologist “displacement” by AI discouraged medical students from pursuing radiology as a residency choice. 21 As technology rapidly advances, AI has potential to improve breast imagers’ confidence, direct focus on cancer-containing cases and act as double-read. 22 Increased exposure to radiology and understanding of AI were shown to reduce medical students’ anxiety level. Expert perspectives of the impact of AI on the future of medical imaging can be used to educate trainees at radiology conferences and in journal publications. 21 Trainee research in this field should also be encouraged to increase exposure to BI and to develop realistic expectations of the impact of AI on BI in the future.
Limitations
While the response rate of medical students of 1.2% makes it challenging to draw conclusions regarding the entire medical student body, this survey presumably reflects opinions of those already interested in radiology. One explanation for the low response rate of medical students is the low interest in radiology as a residency choice and how the survey was distributed. From 2019 to 2021, only an average of 2.9% ± .2% of Canadian medical students applied to radiology as their first-choice discipline. 23
The proportion of trainees interested in either BI, WI, or both fellowships in our study was substantially higher than other North American studies (36% vs 7%), likely attributed to response bias as the survey was sent out by CSBI.4,9 Gender was not collected in our survey. However, whether gender influenced interest in BI can be inferred by the greater proportion of trainees who considered “female-dominated field” as a positive attribute than negative attribute. Hardy et al. also did not find “female-dominated” field as a major deterrent to residents from pursuing BI. 11
Finally, timing of the first breast rotation, exposure to different modalities, and procedures during breast rotations may have been impacted by the COVID-19 pandemic, as screening mammography and elective surgeries for benign entities were suspended or delayed. 24
This study assessed the current level of Canadian trainees’ interest in BI and identified factors that influenced their decision to pursue this field. Trainees play an important role in advancing the future of breast radiology and evaluating their perceptions will help us curate opportunities to recruit more talent to this field. Solutions include increasing early exposure to breast radiology as well as addressing inadequacies in training during residency.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
