Abstract
On March 11, 2020, the World Health Organization declared infection related to a novel coronavirus (SARS-CoV-2) a pandemic. The role and impact of imaging predates this declaration and continues to change rapidly. This article is a consensus statement provided by the Canadian Society of Thoracic Radiology and the Canadian Association of Radiologists outlining the role of imaging in COVID-19 patients. The objectives are to answer key questions related to COVID-19 imaging of the chest and provide guidance for radiologists who are interpreting such studies during this pandemic. The role of chest radiography (CXR), computed tomography (CT), and lung ultrasound is discussed. This document attempts to answer key questions for the imager when dealing with this crisis, such as “When is CXR appropriate in patients with suspected or confirmed COVID-19 infection?” or “How should a radiologist deal with incidental findings of COVID-19 on CT of the chest done for other indications?” This article also provides recommended reporting structure for CXR and CT, breaking diagnostic possibilities for both CXR and CT into 3 categories: typical, nonspecific, and negative based on imaging findings with representative images provided. Proposed reporting language is also outlined based on this structure. As our understanding of this pandemic evolves, our appreciation for how imaging fits into the workup of patients during this unprecedented time evolves as well. Although this consensus statement was written using the most recent literature, it is important to maintain an open mind as new information continues to surface.
Introduction
On March 11, 2020, the World Health Organization declared COVID-19 a global pandemic. At the time of writing, there were 28 893 cases of COVID-19 in Canada, with 2 056 055 worldwide. An unprecedented amount of effort has been put into learning about this disease across the globe with a focus on slowing its spread, improving its detection, finding treatment, and developing a vaccine. On March 30, 2020, the Canadian Society of Thoracic Radiology (CSTR) posted its first position statement regarding thoracic imaging during the pandemic. As a result of ongoing data collection and research, we follow this up with an updated consensus statement which is based on the expert opinion of 6 thoracic radiologists from across the country and 1 thoracic imaging fellow with input from the Canadian Association of Radiologists Executive Board. The focus of this update is foremost on chest imaging rather than imaging logistics and infection control during the pandemic. We have tackled this update by addressing frequently asked questions in the radiology community, primarily the role of chest radiography (CXR), chest computed tomography (CT), and lung ultrasound (LUS).
When Is CXR Appropriate in Patients With Suspected or Confirmed COVID-19 Infection?
Chest radiography is often the initial imaging modality of choice for clinicians who are evaluating patients with known or suspected COVID-19 pneumonia. However, chest radiographs are insensitive for the diagnosis of COVID-19 pneumonia and a negative chest X-ray does not rule out COVID-19 infection. 1 The reverse transcription polymerase chain reaction (RT-PCR) assay remains the gold standard for diagnosis. Chest radiography should not be used to exclude COVID-19 infection. It lacks sensitivity (69%) and is often normal early in the disease. 1,2 Even when present, the imaging features of COVID-19 pneumonia are nonspecific, but when present, increase the clinical pretest probability of COVID-19 infection. The chest X-ray is most useful when an alternative diagnosis is found that completely explains the patient’s presenting symptoms such as, but not limited to, pneumothorax, pulmonary edema, large pleural effusions, lung mass, or lung collapse. At all times, it is important to limit imaging to those in whom results are expected to change management to avoid the risks of potential virus transmission to health care professionals.
Protecting health care personnel and reducing the risk of transmission: When deemed necessary, chest X-rays should be performed using a portable radiography unit. Digital radiography is preferred over computed radiography if available. The use of portable radiography will avoid patient transport to the radiology department, thus limiting exposure to health care workers and other patients in the imaging department. Portable X-ray machines, detectors, and cassettes are also easy to clean, and detectors and cassettes can be protected by a plastic cover that can be changed between patients. Portable radiographs can also be obtained through a glass door, potentially conserving personal protective equipment (PPE). If a patient does require an X-ray to be performed in the radiology department, there should ideally be consideration for a preassigned room to limit department exposure. After imaging, the room should be appropriately cleaned.
In COVID-19 assessment centers and family physician outpatient clinics
If a family physician is concerned for COVID-19 infection, further evaluation at a dedicated COVID-19 assessment facility and RT-PCR testing are recommended.
A chest X-ray is not recommended in individuals presenting with mild symptoms because imaging is often normal 2 and this may be falsely reassuring. Patients should be instructed to stay home, self-isolate, and monitor symptoms while awaiting the result of the RT-PCR test.
In patients presenting with moderate to severe symptoms, CXR, if available, may be useful in addition to clinical judgment to determine whether there is a need for additional assessment in a hospital setting.
In the emergency department setting
In a patient with concerning symptoms, when the RT-PCR assay is not yet available, a chest radiograph is useful. Although the imaging features of COVID-19 pneumonia are nonspecific, when present, they increase the pretest probability of the patient having the disease. Findings suggestive of an alternative diagnosis (pneumothorax, large pleural effusions, lung mass, etc) that requires treatment are also extremely useful.
Immunocompromised and high-risk individuals are more susceptible to severe infection. 3 High-risk individuals have been identified as having risk factors such as age >65 years, cardiovascular disease, diabetes, chronic respiratory disease, and hypertension. 4 Although a chest X-ray may be of limited value for COVID-19 diagnosis, an abnormal result may be a useful adjunct for clinicians in their management decisions. An imaging algorithm for this clinical scenario is outlined in Figure 1.
If a patient with an initial negative RT-PCR result returns to the emergency department with worsening symptoms, a chest X-ray may be useful to detect COVID-19 pneumonia and complications. As the number of days increases from initial symptom onset, the chest radiograph has an increased likelihood of being abnormal. 1,5 A negative chest X-ray still does not exclude the possibility of COVID-19 infection, and repeat RT-PCR testing is still required. An imaging algorithm for this clinical scenario is outlined in Figure 2.
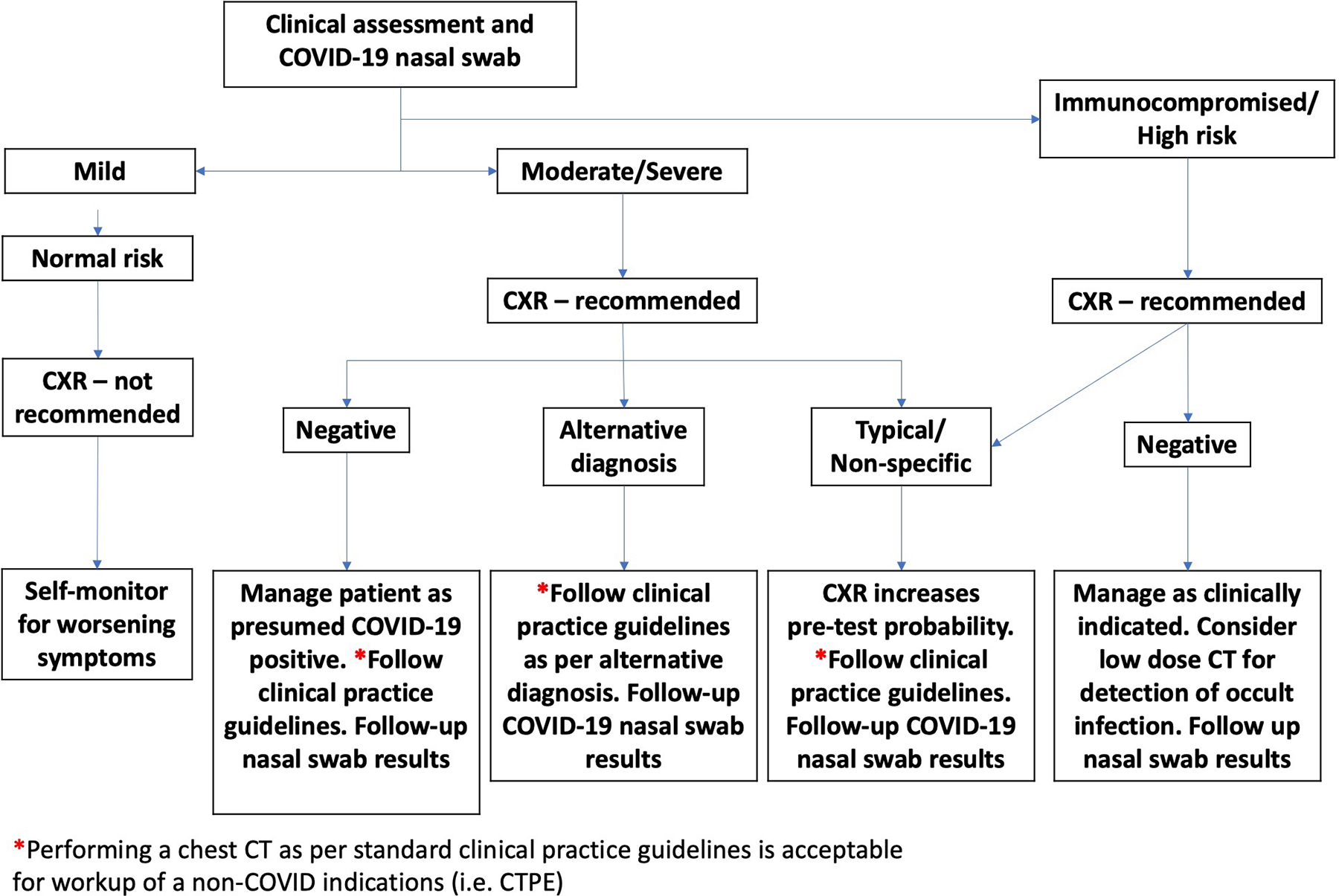
COVID-19 chest imaging algorithm for initial presentation. *Performing chest computed tomography as per standard clinical practice guidelines is acceptable for workup of a non-COVID indication (ie, CT pulmonary angiography [CTPA]). CXR indicates chest X-ray, CT, computed tomography.
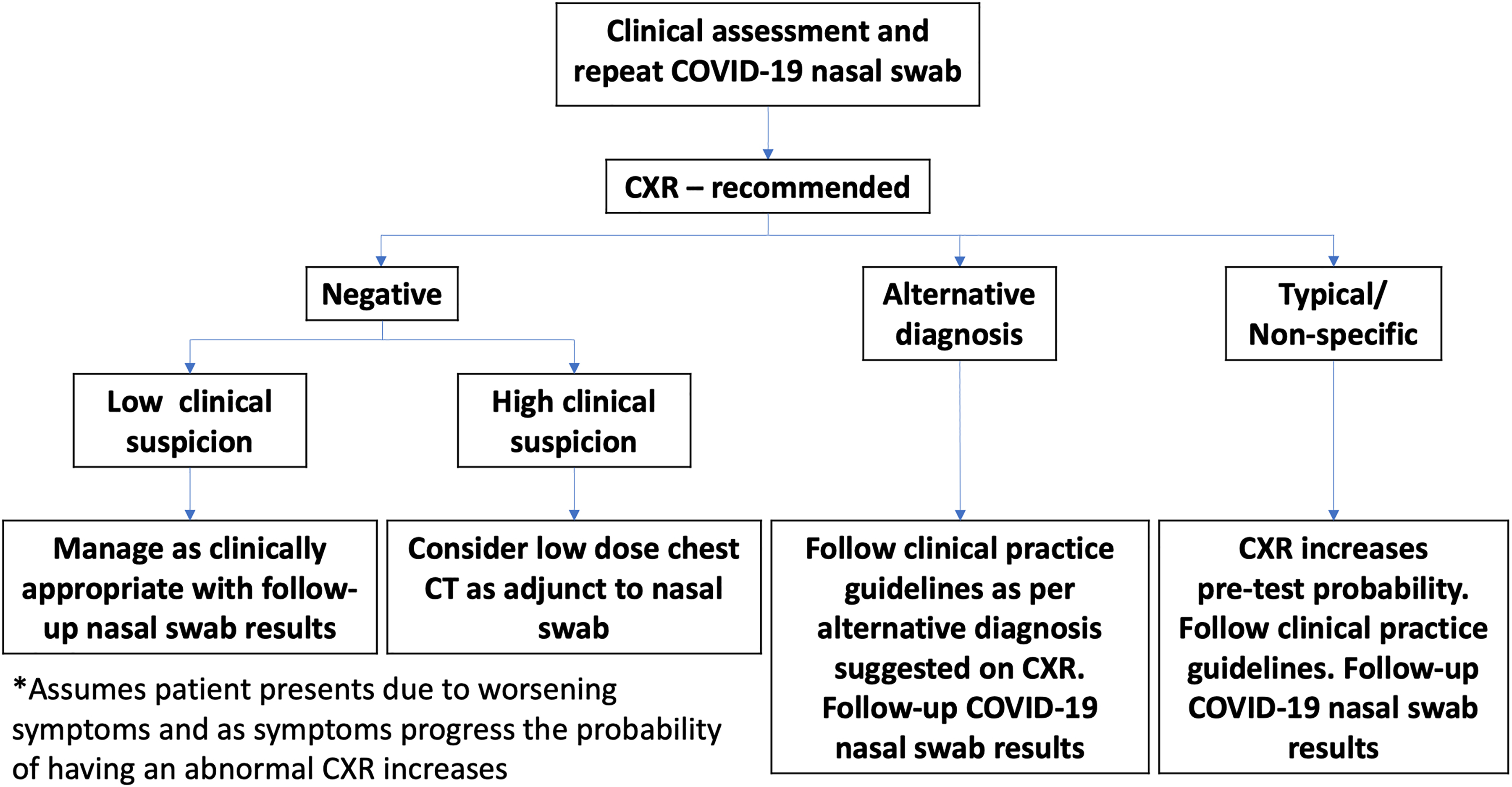
COVID-19 imaging algorithm for repeat presentation and initial negative COVID-19 reverse transcriptase polymerase chain reaction test. *Assumes patient presents due to worsening symptoms, and as symptoms progress, the probability of having an abnormal CXR increases. CXR indicates chest X-ray.
In the inpatient setting
Chest X-rays are useful in clinically worsening patients, but daily chest X-rays in stable patients are not necessary and may increase the risk of viral transmission 6,7 to health care workers.
The role of CXR to monitor disease progression is unknown. In systematic reviews of patients with lower respiratory infections and patients in the intensive care unit (ICU), follow-up chest X-rays did not result in a change in management that shortened duration of patient symptoms or reduced the incidence of adverse events. 7,8 In a study of patients with COVID-19 pneumonia in Wuhan, China, who had follow-up CTs and PCR, less than half (42%) showed improvement on chest CT prior to converting to a negative PCR. 1 Thus, CT was not helpful in monitoring disease progression. Results could be extrapolated to CXR. 6
Recommendations on Reporting Chest Radiographic Findings
Adoption of standardized language is recommended by the CSTR. Analogous to standardized reporting of CT, it is felt that this will lessen variability in the interpretation of chest radiographic findings and facilitate correct identification of frequently and infrequently reported imaging features in this clinical context. Further rationale for using standardized reporting language is outlined in the section on reporting CT findings.
Suggested Categorization and Reporting Language
When typical findings
1,2
are identified on a chest X-ray, the term
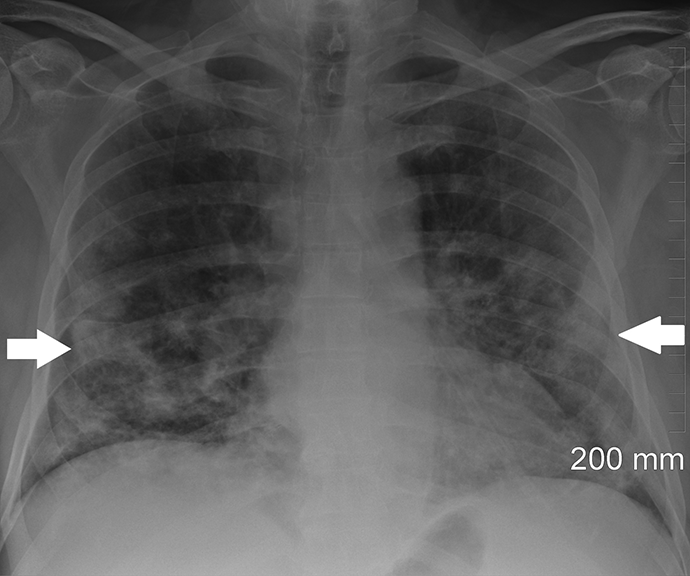
Chest radiograph depicting “typical appearance.” A 66-year-old man with chronic lymphocytic leukemia presented to the emergency department with a history of fever, worsening shortness of breath, night sweats, myalgia, and diarrhea. He had tested positive for coronavirus disease 7 days earlier. Chest radiographic findings include lower zone predominant bilateral and peripheral opacities (arrows).
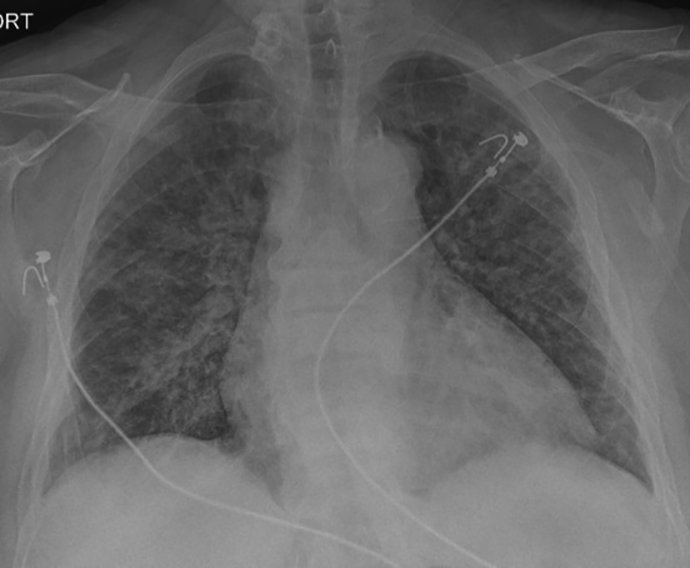
Chest radiograph depicting “nonspecific appearance.” A 55-year-old woman with chronic renal insufficiency presented to hospital with a 1-week history of cough, shortness of breath, malaise, and low-grade fever. Reverse transcription polymerase chain reaction was positive for COVID-19. Chest radiographic findings include diffuse bilateral opacities with no zonal predominance.
Proposed Reporting Structure for Chest Radiography in Patients With Suspected or Confirmed COVID-19.
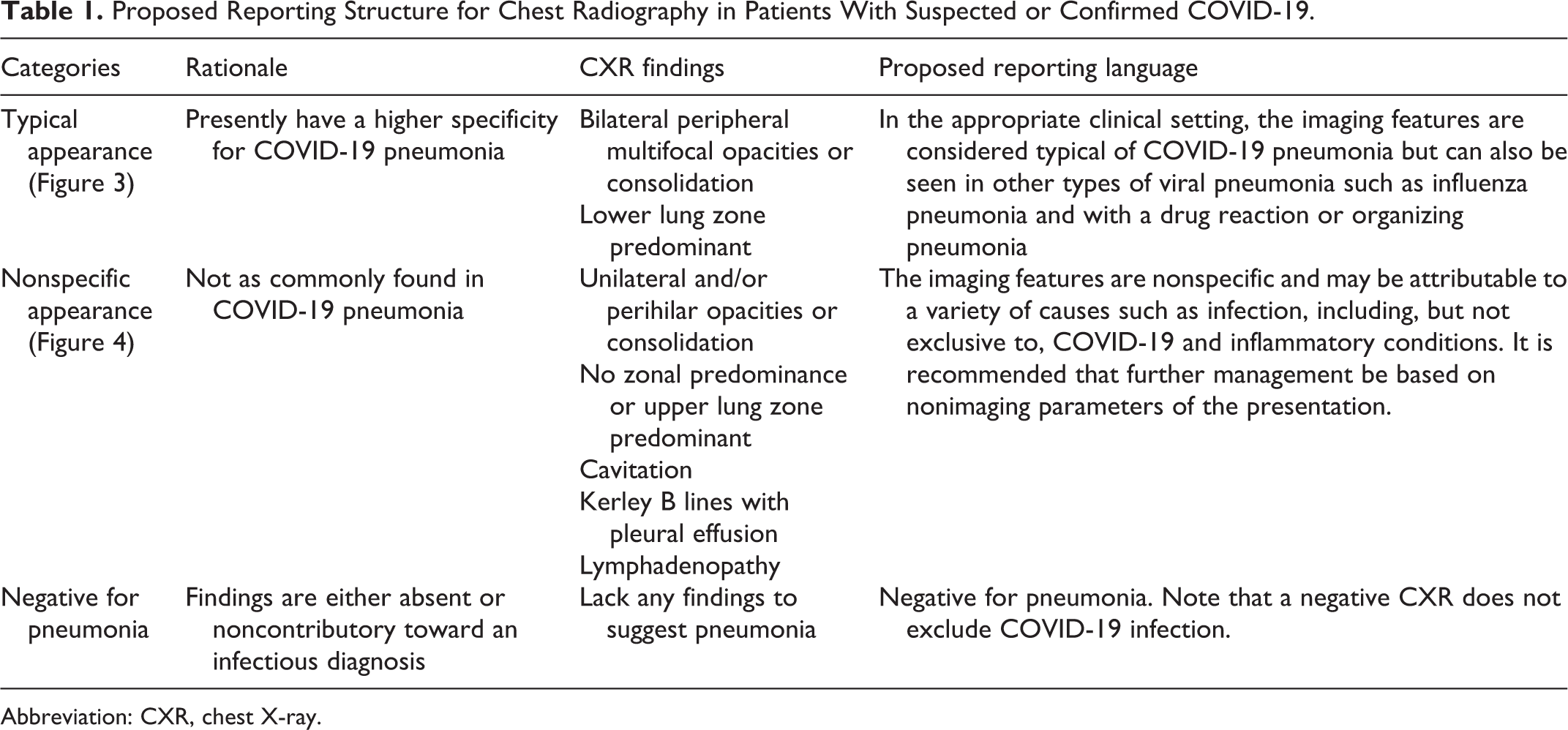
Abbreviation: CXR, chest X-ray.
When Is Chest CT Appropriate in Patients With Suspected or Confirmed COVID-19 Infection?
Historically, standard dose CT chest was superior for the detection of subtle ground-glass opacities (GGOs) as compared to low-dose technique. 9 With the advent of iterative reconstruction algorithms to reduce the visibility of image noise and maintain image quality, low-dose chest CT is appropriate in the majority of patients. 10
Similar to CXR, CT should only be performed if the results are expected to influence patient management. Performance of chest CT requires patient transport to the imaging department and therefore entails careful planning to mitigate the risk of potential infection of health care workers and other patients. Computed tomography should not be used to routinely screen patients for possible COVID-19. The following is a list of potential indications or clinical scenarios for which CT chest may be warranted (Figure 5). It is not meant to be prescriptive.
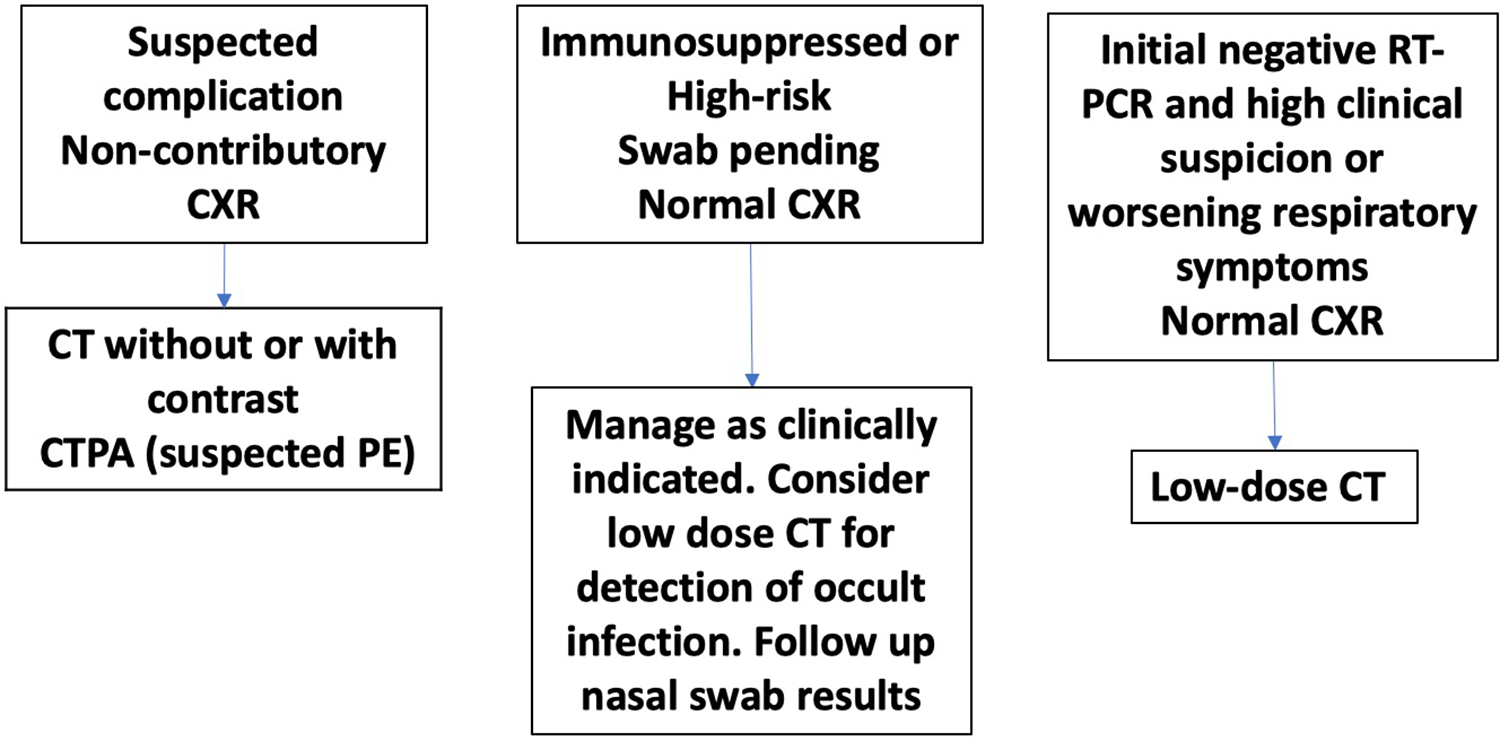
Potential clinical scenarios in which computed tomography (CT) of the chest may be helpful.
Detection of Intrathoracic Complications
Acute clinical deterioration that is not elucidated by a portable radiograph may require chest CT. Such examples include exclusion of an empyema or lung abscess. These necessitate different management approaches and are difficult to differentiate on CXR. If possible, contrast-enhanced CT is indicated in this clinical setting.
Computed tomography pulmonary angiography should be performed in the setting of suspected acute pulmonary embolism (PE). The actual incidence of venous thromboembolism (VTE) in this population is not well established. Unpublished data from colleagues around the world suggest a high incidence of VTE, despite the use of thromboprophylaxis, for example, 26 of 110 CT performed upon admission in the ICU were positive for PE (Strasbourg, France), 15% in Cremona, Italy. In Cornell, New York, an overall incidence of 3% was observed in patients with COVID-19 regardless of severity, with an 8.4% incidence among intubated patients.
Immunosuppressed or High-Risk Patients With Suspected Respiratory Infection and a Negative Chest Radiograph
Immunosuppressed patients are at higher risk of opportunistic infections, including viral infections. Recent data from Italy suggest that unlike other viruses such as influenza, respiratory syncytial virus, and adenovirus, the family of coronaviruses that includes SARS-CoV-2 responsible for COVID-19 disease is not associated with more severe disease in immunosuppressed patients. Rather, it is the host’s innate immune response that is the driver of acute lung injury related to infection. 11 However, COVID-19-positive patients with solid malignant tumors who were immunosuppressed due to chemotherapy and those with recent immune therapy or radiation treatment had worse outcomes in Wuhan, China. 12 Therefore, due to the higher risk of lung infection in immunosuppressed patients in general, it is reasonable to image these patients with CT of the chest.
Another group of high-risk individuals has been identified in a large cohort of patients from Wuhan, China. These patients have a higher incidence of disease progression and worse outcomes. High-risk factors include age >65 years, cardiovascular disease, diabetes, chronic respiratory disease, and hypertension. 4
COVID-19 lung infection is often associated with subtle GGOs that may be difficult to visualize or occult on chest radiographs. 6 Therefore, in the immune-suppressed populations, chest CT may be considered to evaluate for COVID-19, just as it is routinely used in some institutions to evaluate for pulmonary infection in patients with leukemia with febrile neutropenia. This may be especially important if there are delays in obtaining RT-PCR results or local constraints on RT-PCR testing. However, a normal chest CT does not exclude COVID-19 infection.
Initial Negative RT-PCR Result but Ongoing High Clinical Suspicion or Clinical Deterioration After a Normal Chest Radiograph
In the early stages of infection, viral load may be too small to be detected by RT-PCR and reports in the literature suggest that chest CT findings may be present even in asymptomatic COVID-19-infected patients. 13 Furthermore, the CT of the chest may be useful to identify an alternative cause for a patient’s symptoms. When there is clinical deterioration, chest CT can be performed for reevaluation of the patient who may have had a previous negative RT-PCR swab result or noncontributory chest radiographs to evaluate for underlying causes. This indication is also endorsed by the recently published Fleischner Society statement. 6
In certain health care settings, due to local circumstances, the use of chest CT has been expanded to include patients undergoing CT for other reasons or planned for urgent surgery or intervention. In this developing expanded indication, a CT of the head or abdomen is already requested and the CT of the chest is added.
Such clinical scenarios include: stroke code patients, patients in need of urgent interventional radiology procedures, patients with acute abdominal pain potentially in need of urgent abdominal surgery (ruptured appendicitis, etc), and Patients with abdominal pain of unknown cause undergoing CT of the abdomen.
The use of chest CT in the first 3 scenarios may be motivated by the needs of anesthesia and surgical departments to triage the use of PPE to adequately protect health care workers, to risk stratify patients, and to appropriately allocate health care resources. In many hospitals, RT-PCR results may take up to 24 hours and there may be reductions in “real-world” sensitivity due to problems with sampling technique (nasopharyngeal swab may have greater sensitivity vs throat swab). 14
When there is a need for an urgent intervention or procedure, waiting 24 hours for the swab result to decide on the level of PPE required is impractical. The chest CT is used as supplementary information to guide the use of PPE. Full PPE precautions are used when the RT-PCR is pending or unknown, and the CT chest demonstrates typical or nonspecific findings of COVID-19. A positive CT chest can also help risk stratify patients because asymptomatic lung infection may influence the decision to proceed with surgery or delay if clinically feasible.
In cases where the RT-PCR result is unknown or pending and the patient needs urgent intervention or surgery, a negative chest CT is felt to indicate a lower risk of COVID-19, especially in a low pretest likelihood patient who is asymptomatic from a respiratory standpoint. A lower level of PPE could potentially be used in these patients. It is important to note that early in disease course, chest CTs can be entirely normal in patients with a positive RT-PCR. Bernheim et al 13 demonstrated this in 20 (54%) of 36 patients within 2 days of symptom onset. Therefore, a normal CT of the chest may be falsely reassuring and may not be helpful to inform on the type of PPE used.
Chest CT is also unlikely to be useful if full PPE precautions are employed in all patients undergoing urgent surgery or intervention (all patients treated as if they were COVID-19 positive). This strategy is also impractical if there are local constraints with respect to CT scanner availability.
The rationale to add a chest CT to an abdomen CT in patients with undifferentiated abdominal pain stems from the fact that COVID-19 pneumonia may present with upper abdominal symptoms secondary to disease in the lung bases. The clinical differentiation between lower chest and upper abdominal pain may be challenging. Less commonly, COVID-19 infection presents with abdominal symptoms rather than fever, dry cough, and shortness of breath. In a recent meta-analysis, a pooled prevalence demonstrated that 17.6% of COVID-19-infected patients had gastrointestinal symptoms and 48.1% had viral RNA detected in stool samples. 15
In summary, there is currently no published data demonstrating outcome benefit to adding chest CT to head or abdomen CT and several current society guidelines do not specifically mention or endorse this strategy. The recently published Fleischner Society statement specifically states that no imaging is required for mild cases of COVID-19 infection but does not address scenarios involving asymptomatic patients. 6 Our understanding of the utility of chest CT in the evaluation of COVID-19 continues to evolve and will be informed by ongoing data collection and research.
Recommendations on Reporting Chest CT Findings
Adoption of standardized language is recommended by the CSTR and has also been advocated by other radiological societies, including the RSNA 16 and the Fleischner Society. 6 It is felt that this will lessen variability in the interpretation of CT findings and facilitate correct identification of frequently and infrequently reported imaging features in this clinical context. It is hoped that in this manner, consultation and relay of diagnostic information is enhanced between the radiologists and their referring colleagues, resulting in better clinical decision-making. Our recommendations are based on the available scientific evidence to date and are subject to revision in the near future as more scientific data on COVID-19 are gathered and analyzed. 17 Implementation of structured reporting is preferably carried out in consultation with clinical colleagues at each facility as this practice may potentially introduce certain limitations in patient management if the terminology “COVID-19” is incorporated into a patient’s report.
It is suggested that the provided template and language be utilized at the discretion of the interpreting radiologist and in the setting of suspected pneumonia, which could include COVID-19 as a diagnostic possibility. The template does not apply to lung findings on CT done for other indications. It is strongly recommended that radiologists review and familiarize themselves with CT findings, which have been frequently
13,18
-20
and infrequently
13,20
reported with COVID-19 pneumonia. The CSTR recommends consolidation of all imaging features that are not typical or seen rather infrequently with COVID-19 into a single category termed
Suggested Categorization and Reporting Language
If the examination shows typical findings, the term
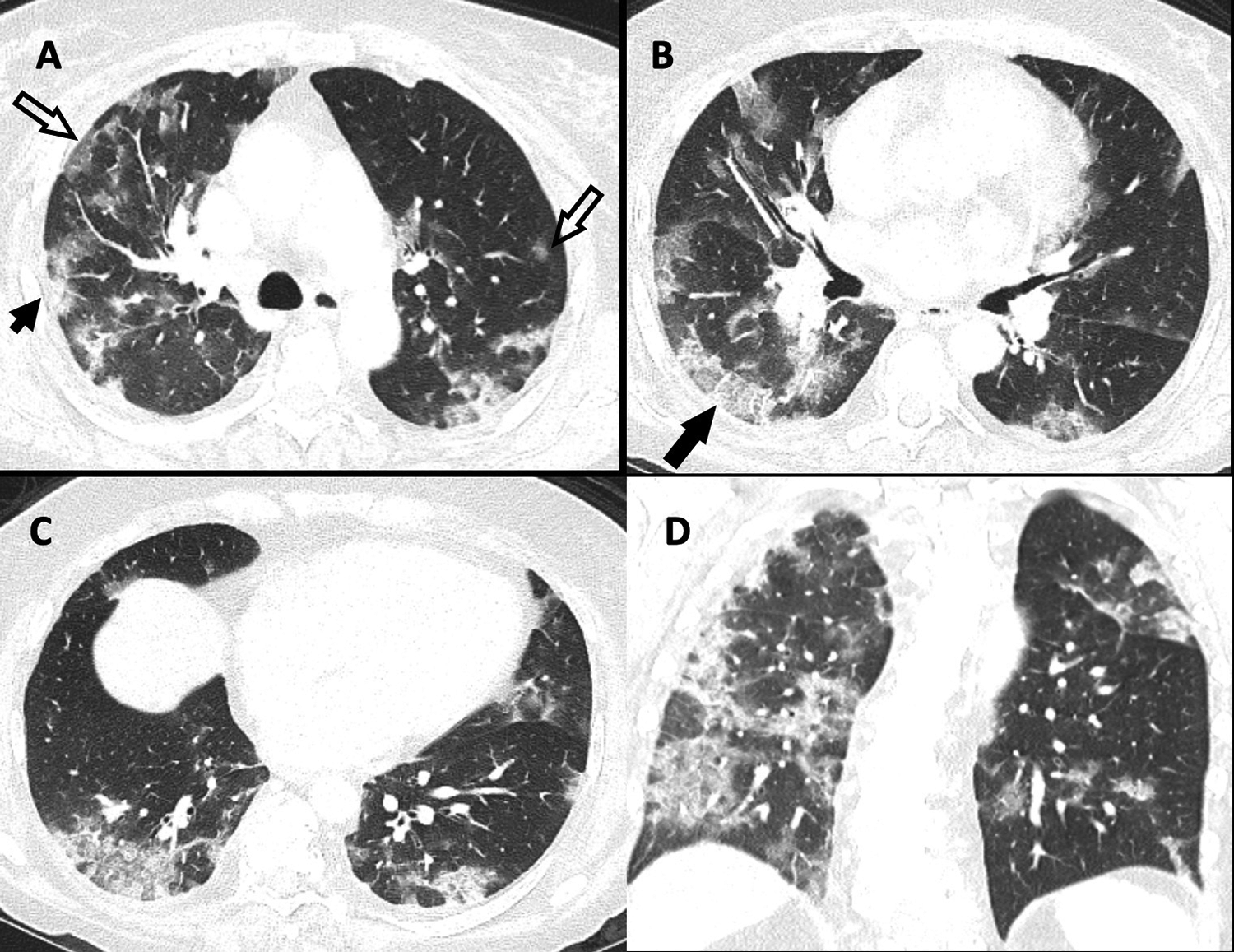
Computed tomography (CT) of the chest depicting “typical appearance.” Select thin-section axial (A-C) and coronal (D) images of the lungs from an unenhanced CT in a 61-year-old woman with a positive reverse transcription polymerase chain reaction presenting to the emergency department with a 10-day history of progressive shortness of breath, fever, cough, malaise, and watery diarrhea. There are multifocal, peripheral, and occasionally rounded ground-glass opacity (open arrows) with consolidation (short arrow) and crazy paving (long arrow).
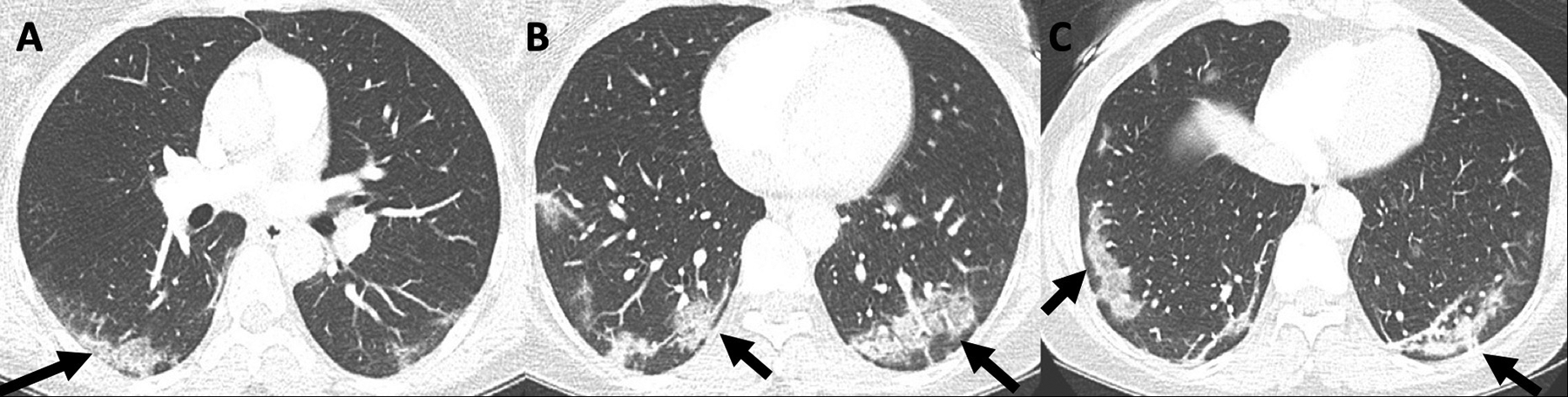
Computed tomography (CT) of the chest depicting “typical appearance.” Axial images of the lungs (A-C) from a CT pulmonary angiogram in a 48-year-old woman with a history of remote deep venous thrombosis who presented to the emergency department with chest pain and hemoptysis and subsequently had a positive reverse transcription polymerase chain reaction test for COVID-19 demonstrating peripheral and multifocal ground-glass opacity and consolidation with an organizing pneumonia pattern (arrows).
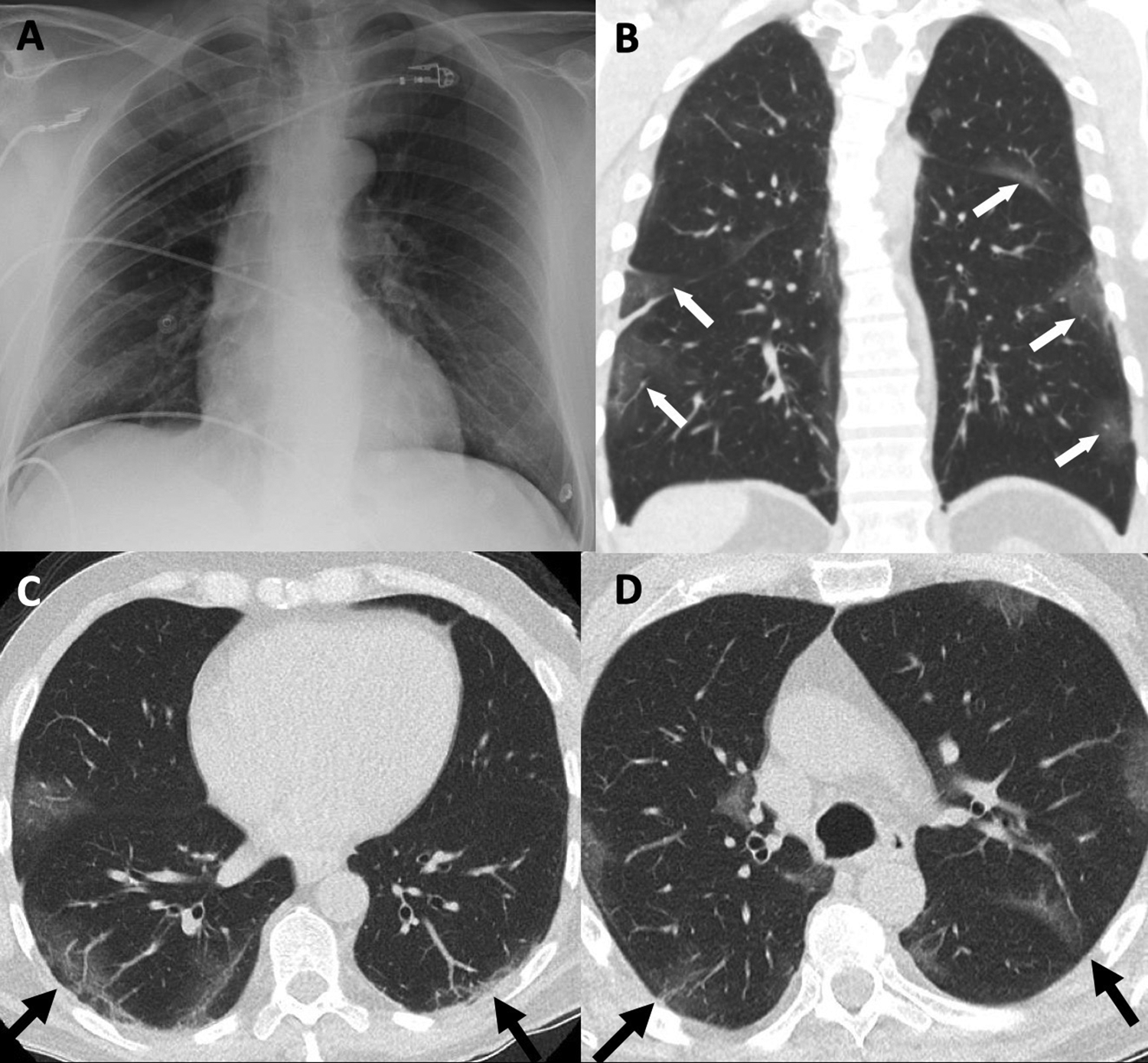
Typical appearance of a 58-year-old man with positive reverse transcription polymerase chain reaction assay for COVID-19 with a 9-day history of worsening symptoms including shortness of breath. Normal or near-normal portable chest radiograph (A) and coronal (B) and axial low-dose computed tomography (C & D) obtained 1 hour later demonstrate peripheral ground-glass opacity with slight lower zone predominance (arrows).
If the examination shows nonspecific findings, the term
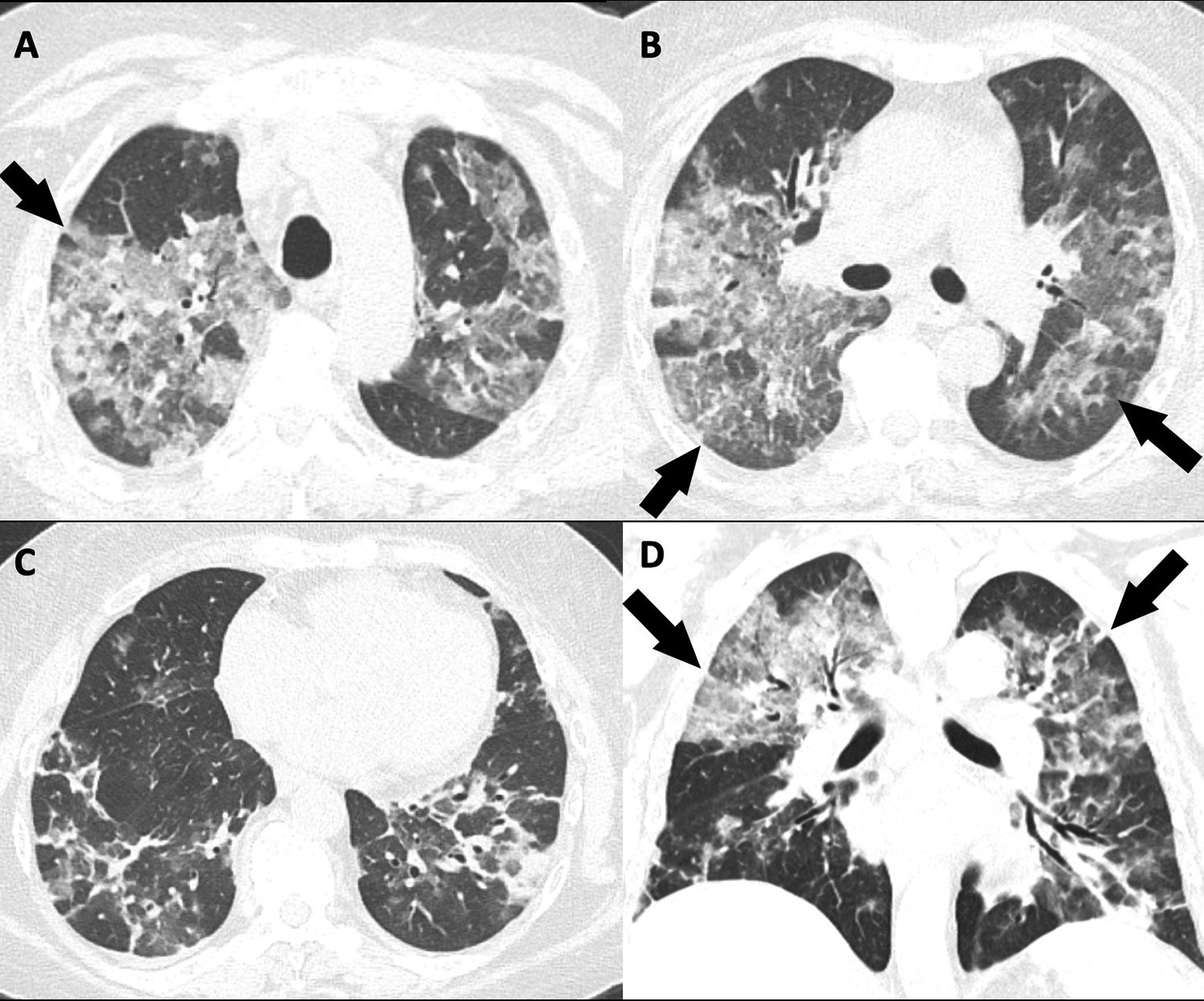
Computed tomography (CT) of the chest depicting “nonspecific appearance.” Unenhanced axial (A-C) and coronal (D) CT images (lung reconstruction) in a 55-year-old woman with chronic renal insufficiency presenting to hospital with a 1-week history of cough, shortness of breath, malaise, and low-grade fever. Reverse transcription polymerase chain reaction was positive for COVID-19. CT reveals nonrounded, nonperipheral ground-glass opacity with upper zone predominance (arrows).
If the examination shows no findings that could be attributable to any type of pneumonia, the term
Proposed Reporting Structure for CT Imaging in Patients With Suspected or Confirmed COVID-19.
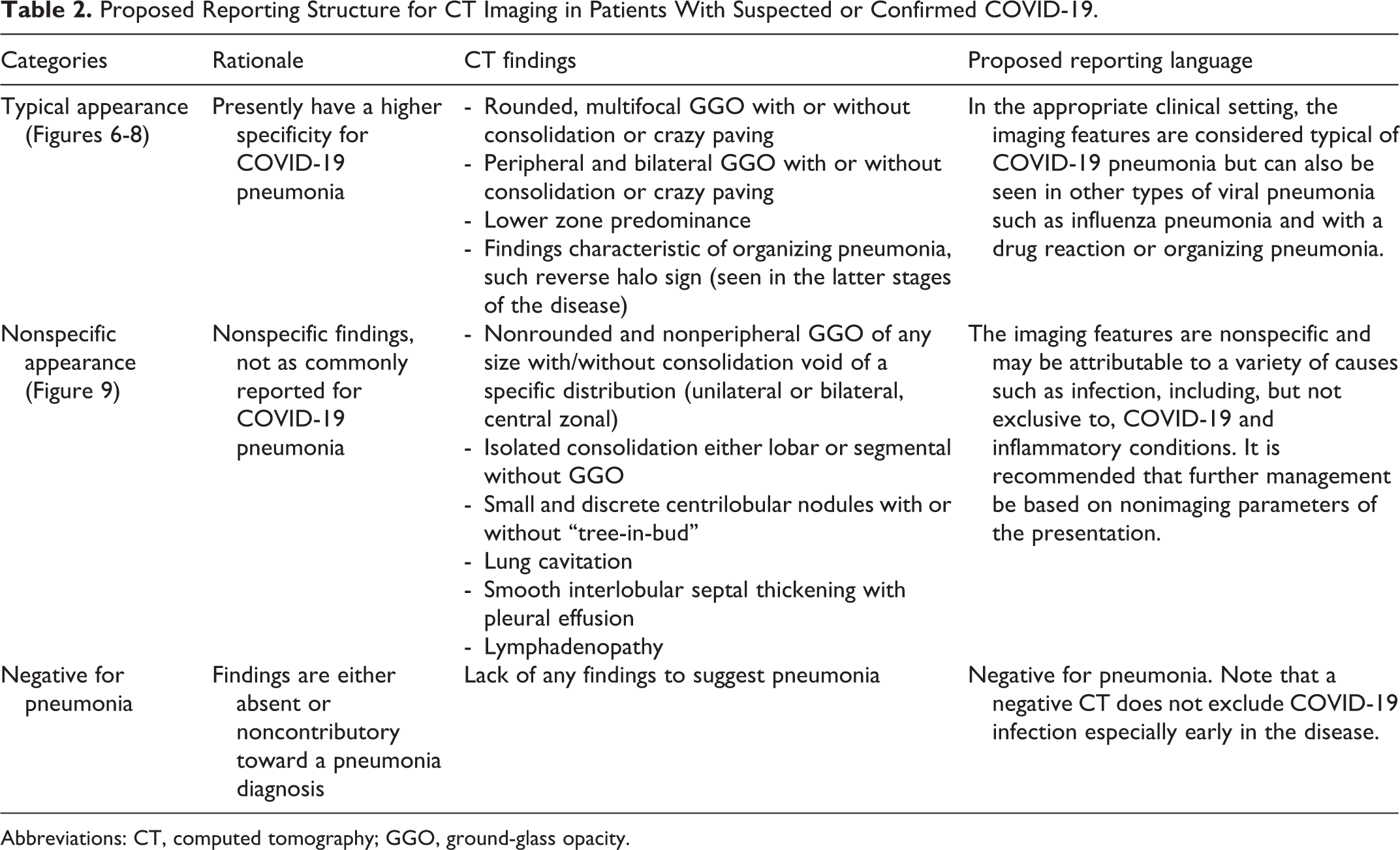
Abbreviations: CT, computed tomography; GGO, ground-glass opacity.
How Should a Radiologist Deal With Incidental Findings of COVID-19 on Chest CT Done for Other Indications?
When typical or nonspecific features of COVID-19 pneumonia are seen as an incidental finding in endemic areas, the CSTR recommends that the interpreting radiologist should contact the most responsible provider directly to discuss the likelihood of viral infection. Caution must be exercised in the wording of the radiology report as documentation of “COVID-19” may constrain clinical decision-making and treatment options. The RSNA recommendations emphasize the use of direct communication with the referring physician and wording such as “viral pneumonia” may be preferable in the setting of incidentally detected lung abnormalities. 16
The reporting template and suggested language for CT done in patients with suspected pneumonia described previously does not apply to lung findings on CT done for other indications. There are currently few reports on the detection of CT findings suggestive of a diagnosis of COVID-19 pneumonia as an incidental finding on chest CT done for other clinical indications. Albano and his colleagues reported on 65 patients in Italy who underwent positron emission tomography/CT for routine oncology indications during the third week of March 2020. Patients were screened by questionnaire for symptoms and exposure and there was no indication to suspect COVID-19 infection. Of these 65 patients, 6 showed signs of pneumonia on CT as an incidental finding and 5 of 6 subsequently tested positive for COVID-19. 26 Although not a study of incidental findings on chest CT, imaging findings in 112 cases of COVID-19-positive patients on board the “Diamond Princess” cruise ship were analyzed. 27 Fifty-four percent of asymptomatic patients who tested positive for COVID-19 had abnormal findings on chest CT. No significant differences in age, gender, or comorbidities were identified in symptomatic versus asymptomatic cases. Asymptomatic patients showed a lower CT severity score and predominant GGO, whereas symptomatic patients showed predominant consolidation.
Given that there is now community spread in most areas in the country and asymptomatic patients can have positive CT findings in over 50% of cases, there is likely a significant chance of encountering findings suggestive of COVID-19 on chest CT performed for other indications in asymptomatic patients who do not have known COVID-19 exposure (Figures 10 and 11).
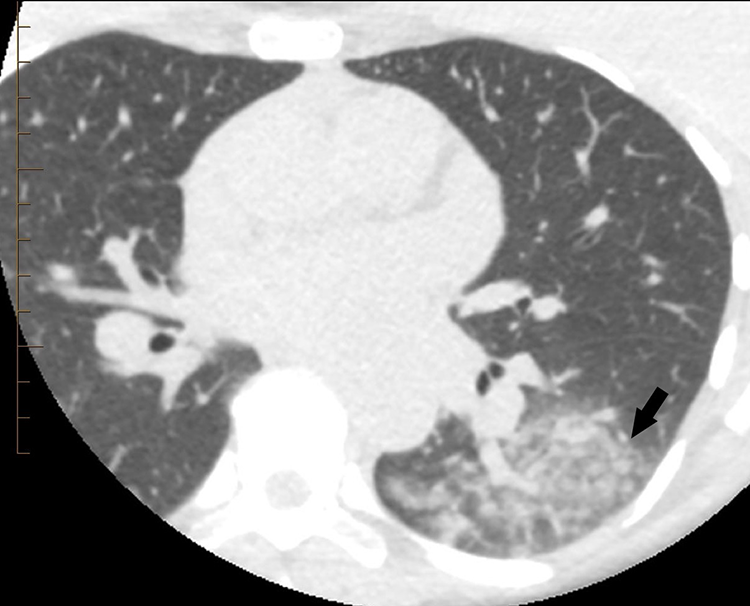
Incidental detection of COVID-19 pneumonia on computed tomography (CT) of the chest done for another clinical indication. Axial image (lung reconstruction) from a cardiac CT in a 50-year-old female nurse with asthma, a family history of coronary artery disease, and an 18-month history of ongoing chest discomfort depicts nonspecific mixed ground-glass and airspace opacities in the left lower lobe (arrow). The patient’s physician was alerted of the unexpected findings. Although asymptomatic from a respiratory standpoint, subsequent reverse transcription polymerase chain reaction swab was positive for COVID-19. Two days later, the patient developed a dry cough, but no other symptoms.
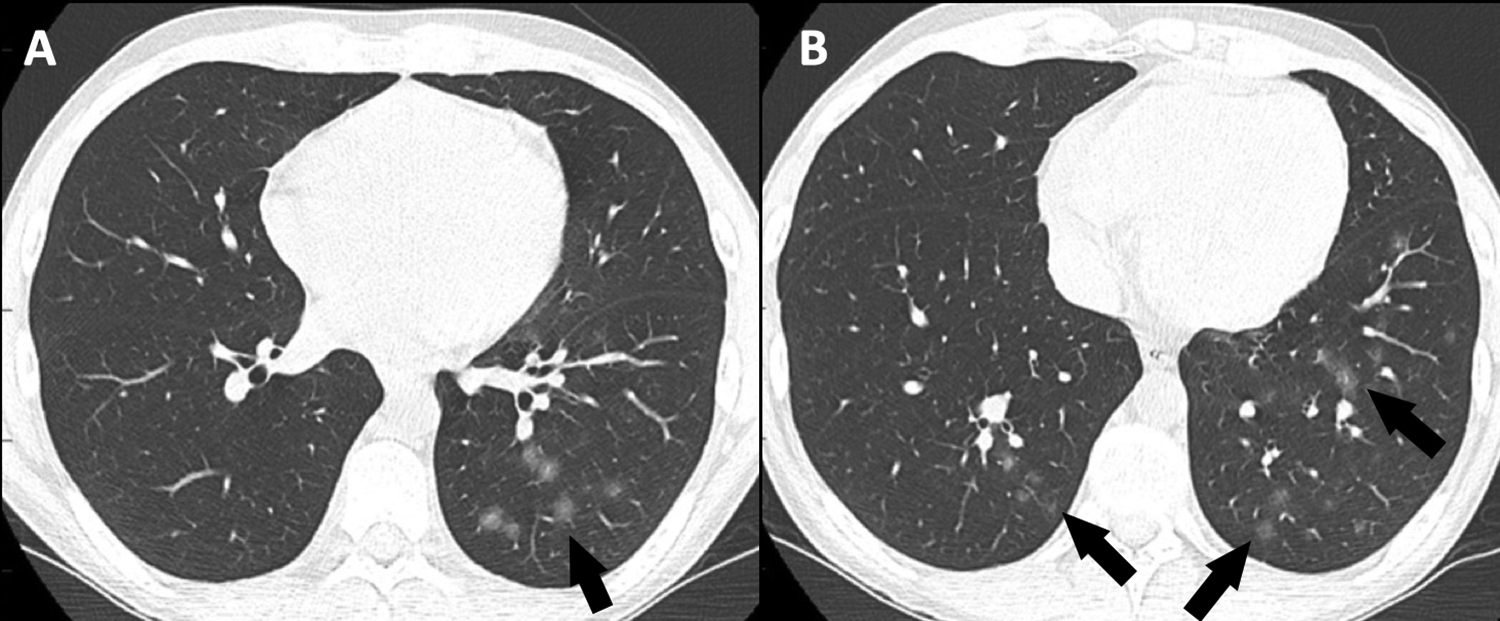
Incidental detection of ground-glass opacity (GGO) on computed tomography (CT) of the chest done for another clinical indication. Is this COVID-19 pneumonia? Select thin-slice axial images of the lungs (A and B) from an unenhanced CT performed to rule out posttransplant lymphoproliferative disorder in a 22-year-old asymptomatic man 3 years postrenal transplantation. Computed tomography shows subtle lower zone rounded GGO (arrows). The patient remained asymptomatic and had consecutive swabs for reverse transcription polymerase chain reaction testing, which were all negative for COVID-19.
Should Lung Ultrasound (LUS) Be Used to Diagnose or Exclude COVID-19 Pneumonia?
Lung ultrasound should not be used to diagnose or exclude COVID-19 pneumonia. Although there is a growing identification of LUS patterns in COVID-19 pneumonia, 28 -31 the overlap with other causes of respiratory distress is unknown. Small outcome studies have been performed in patients with other causes of acute respiratory distress 32 -34 but are insufficient to support the use of LUS to contribute to or supersede established prognostic tools, such as the Sequential Organ Failure Assessment score. 35 Any use of LUS in patients with COVID-19 should be done within the context of a controlled research study, ideally with operators blinded to other clinical markers of severity. Risks of viral exposure to operators are unknown, but some authors suggest the examination should only be performed by those already caring for the patient in another capacity. 28
Conclusion
The consensus statement above is based on knowledge acquired thus far as we navigate this uncertain time. As the evidence for imaging in COVID-19 evolves, our opinions and recommendations will be refined over time.
Footnotes
Acknowledgment
The authors thank Micheline Turnau for providing writing assistance and proofreading the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
