Abstract
The use of age-appropriate care as an organized framework for care delivery in the neonatal intensive care unit is founded on the work of Heidelise Als, PhD, and her synactive theory of development. This theoretical construct has recently been advanced by the work of Gibbins and colleagues with the “universe of developmental care” conceptual model and developmental care core measures which were endorsed by the National Association of Neonatal Nurses in their age-appropriate care of premature infant guidelines as best-practice standards for the provision of high-quality care in the neonatal intensive care unit. These guidelines were recently revised and expanded. In alignment with the Joint Commission’s requirement for health-care professionals to provide age-specific care across the lifespan, the core measures for developmental care suggest the necessary competencies for those caring for the premature and critically ill hospitalized infant. Further supported by the Primer Standards of Accreditation and Health Canada, the institutional implementation of theses core measures requires a strong framework for institutional operationalization, presented in these guidelines. Part A of this article will present the background and rationale behind the present guidelines and their condensed table of recommendations.
Keywords
Introduction
Over the last 30 years, advancement in the field of technology as well as new knowledge has improved survival and decreased the incidence of major long-term disabilities among premature infants (Wilson-Costello et al., 2007). However, neurodevelopmental outcomes for this vulnerable patient population remain a major concern (Baron, Erickson, Ahronovich, Baker, & Litman, 2011; Hack et al., 1994, 2009) and are still heavily influenced by the environment of care which is more often than not intensive, stressful, and sometimes traumatic (Als et al., 1994; Altimier & Phillips, 2013; Chau et al., 2013; Coughlin, 2014). Based on Als’ Synactive Theory (Als, 1986), developmental care (DC) has emerged as a neuroprotective care concept aimed at preventing the long-term consequences associated with the physical environment, promoting the optimal organization and neurological development of preterm infants in the neonatal intensive care unit (NICU) as well as integrating parents as care partners (Altimier, Kenner, & Damus, 2015; Coughlin, Gibbins, & Hoath, 2009; Kenner & McGrath, 2014). Neuroprotective care includes several strategies, such as family-centered developmental care, that promote normal development and prevent disabilities (McGrath, Cone, & Samra, 2011). Both terms, neuroprotective care and family-centered developmental care, are used in these guidelines to reinforce the importance and relevance of DC as a neuroprotective measure for premature infants admitted in the NICU while the ability to influence neural connectivity is at its greatest for potential long-term outcome-benefits (McGrath et al., 2011). Regardless of terminology, the objectives of these practice paradigms remain the same, and their results demonstrate a positive impact (Als et al., 2003, 2004; Buehler, Als, Duffy, McAnulty, & Liederman, 1995; Byers, 2003; Kleberg, Westrup, & Stjernqvist, 2000; Kleberg, Westrup, Stjernqvist, & Lagercrantz, 2002; Melnyk et al., 2005; Westrup, Kleberg, von Eichwald, Stjernqvist, & Lagercrantz, 2000). To further support DC, the Cochrane review states that Developmental care interventions may help preterm infants cope better with the environment of the Neonatal Intensive Care Unit (NICU). There is concern that an unfavourable environment in the NICU can … negatively affect the infant’s growth, with the brain being particularly vulnerable. DC refers to a range of strategies designed to reduce the stresses of the NICU. The review of trials suggests that these interventions may have some benefit … in enhancing neurodevelopmental outcomes. (Symington & Pinelli, 2006, p. 2)
The only professional association worldwide to have guidelines in DC is the National Association of Neonatal Nurses (NANN). In 1995, they published their first content on the subject with their Infant and Family-Centered Developmental Care Guidelines, updated in 2000 (NANN, 1995). These evolved with their advance competency in DC (McGrath & Task force, 2008) as well as their DC specialist designation (McGrath & Task force, 2010) to be replaced in 2011 by their Age-Appropriate Care of the Premature and Critically Ill Hospitalized Infant – Guidelines for Practice (Coughlin, 2011). These guidelines were based on years of literature review, expert consultations, a conceptual model (The Universe of Developmental Care) (Gibbins, Hoath, Coughlin, Gibbins, & Franck, 2008) and Core Measures for Developmentally Supportive Care (Coughlin et al., 2009; Gibbins et al., 2008). This work culminatines into the publication of the official professional association reference book on DC: Developmental Care of Newborns and Infants—A guide for health-care professionals (Kenner & McGrath, 2014). Like most publications available on DC, this precious and essential resource focuses mostly on individual practice guidelines, allowing only one chapter for implementation.
Many whom have criticized DC have mentioned the inconsistency in its implementation and the lack of institutional operationalization framework making outcomes very difficult to compare from one setting to another, and limiting research reproducibility (Carrier, 2002; Laudert et al., 2007; Wallin & Eriksson, 2009; Zhang, Lee, Chen, & Liu, 2016). The fact that this care model consists of multiple interventions with multiple outcomes also renders its evaluation and comparison more complex (Symington & Pinelli, 2006). Consequently, its implementation remains challenging, very sporadic, inconsistent, and variable from one setting as well as from one professional to the next, despite the presence of multiple recommendations, experts in the field, and the availability of training programs (Phillips, 2015; Zhang et al., 2016). In fact, despite the documented benefits, Coughlin et al. (2009) concluded that “… confusion about the existing theoretical construct and the inability to identify and measure relevant clinical outcomes reliably has resulted in inconsistent adoption of developmental care and under-mined its potential as a revolutionary and transformative healthcare philosophy and practice paradigm” (p. 2240).
In order for implementation of DC to be successful and sustainable, it requires adoption at many different levels: individual practice changes (practice), institutional implementation (organizational), and national/international guidelines to be created and endorsed (system level) (Bertram, Blase, & Fixsen, 2015; Fixsen, Blase, Naoom, & Wallace, 2009; Fixsen, Naoom, Blase, Friedman, & Wallace, 2005). Therefore, institutional guidelines are essential.
Background and purpose
Individual practice guidelines in DC
Developmental care core measures and NANN age-appropriate care guidelines (Coughlin, 2011; Coughlin et al., 2009).

Institutional implementation guidelines in DC
Since institutional implementation and operationalization of DC is a priority in neonatology, some standardized guidelines for implementation should be available, as it would greatly help with the process of institutional operationalization but also in the field of comparative research. Some experts have presented recommendations for implementation that are extremely useful and necessary for the development of the present guidelines but incomplete for a consistent holistic institutional implementation of developmental neuroprotective care methodology. They will be presented below. Gilkerson and Als (1995) were the first ones to establish a process in the institutional implementation of developmentally supportive care in the NICU with reflective practice, known as the newborn individualized developmental care and intervention program (NIDCAP), which has demonstrated multiple clinical benefits to date (McAnulty et al., 2013; Ohlsson & Jacobs, 2013; Peters et al., 2009). This reflective practice was later put into a model for “Reflective practice in Developmental care – Individualized family-centered developmental care (IFDC) standards” by Carrier (2002). This model involved three general stages progressing from exploration/conceptualization of the new paradigm of DC through a mindful practice of IFDC principles, ending with the assimilation of the IFDC standards applied into practice but is difficult to operationalize.
In 1996, Als published the NIDCAP recommendations for the institutional implementation of DC which she called “component” of training and staff development at that time. To our knowledge, they have not yet been publicly updated. They included the following:
Training a DC specialist and nurse educator. Training a multi-disciplinary leadership support team. Training a core group of at least 10% of the nursing staff. Creating a salaried position for the DC specialist and educator. Creating a salaried position of a parent representative.
In the same publication, she also recommended several “specific components of unit development” in the following focus areas (p.133):
Development of a mission and vision statement. Drawing up a unit plan. Prioritizing changes. Creating a task force on specific topics. Increasing integration of family in care. Developing strategies and resources to improve consistency. Developing a format and training structure for staff. Developing evaluation and reflexive process.
These recommendations might not have been publicly updated, but they are still used widely in many NIDCAP implementations. Furthermore, although their outcomes were not published in terms of implementation strategy and results, they still presented improved population outcomes. Bertram et al. (2015) mention that improved population outcomes depend upon changes made within the organization, thus supporting this program model in terms of implementation outcomes. Their recommendations were therefore largely used in the development of our institutional implementation of developmental neuroprotective care guidelines.
Robison’s organizational guide for an effective developmental program in the NICU (Robison, 2003).
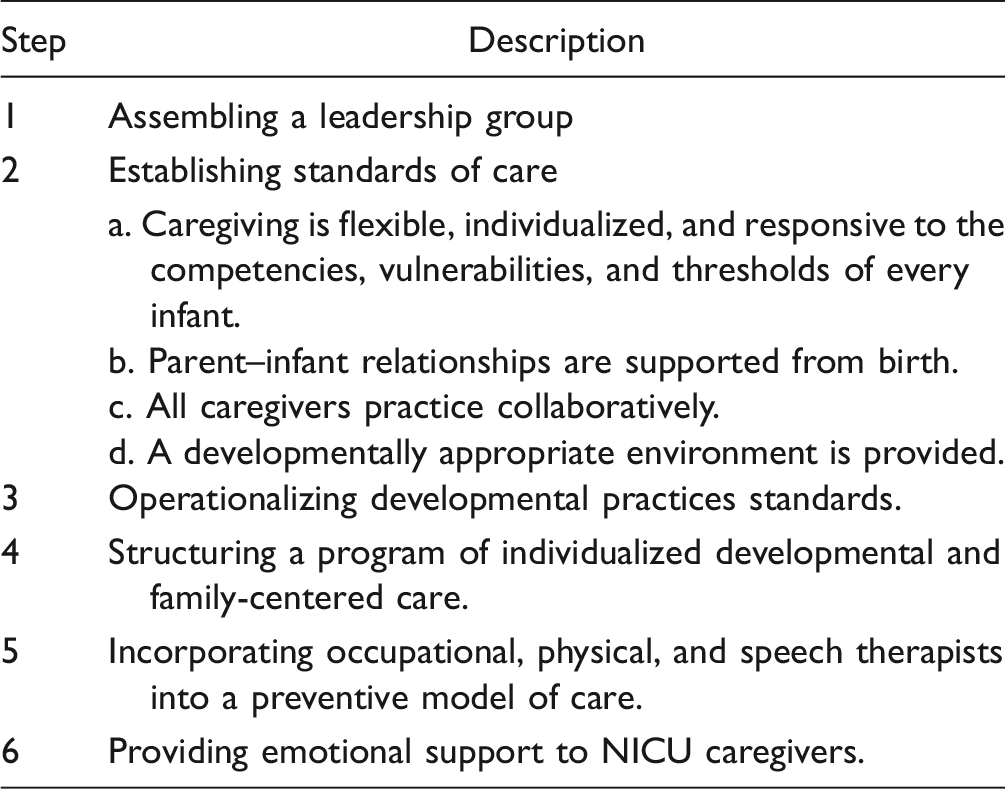
Finally, very recently, Phillips (2015) presented steps in the implementation of the seven core measures of neuroprotective family-centered DC program, which are very similar to Robison’s. They were implemented in her unit with positive results. They included the following:
The identification of a champion. The recruitment of a neuroprotective committee. The creation of a neuroprotective steering committee. The identification of select interventions with measurable outcomes. The development of educational modalities for professionals and parents.
These steps are essential, but insufficient and incomplete for institutional implementation as they mostly focus on planning, but not operationalization. Part of the Wee Care implementation strategies were presented by Cardin et al. (2015), who mention that the transformational education program provides education, change management principles, resources, and consultation for full implementation. Their strategies, although very thorough, are not specific and clear enough for other units to replicate. The strategies used in their program included the following:
Pre-and post-program site assessment. Unit champions preparation. Medical grand rounds. Onsite education session. In unit consultation with care provider—DC rounds. Plan-Do-Study-Act (PDSA) process. Research and publication.
Based on Level II evidence (Johnson, Handberg, Dobalian, Gurol, & Pearson, 2005), DC operationalization is presented in one of the five NANN core measures, the healing environment (Coughlin, 2011; Coughlin et al., 2009) where one of the attributes of the core measure is related to evidence-based policies, procedures, and resources that should be available to sustain the healing environment over time. This attribute includes the following criteria:
Core measures of DC provide the standard of care for all patient care providers. Resources to support the implementation of DC as defined by the core measures are always available. A system for staff accountability in the practice of DC as outlined by the core measures is operational.
Recently published in a book, updated and expanded core measures for trauma-informed, age-appropriate care have been endorsed by the NANN (Coughlin, 2016). These new recommendations now include organizational implementation strategies in DC that were also operationalized in different phases and steps of the present guidelines (Coughlin, 2016). To integrate the core measure into practice, Coughlin (2016) suggests the following strategies:
Create a multi-disciplinary task force to review existing practice standards and guidelines. Identify gaps between existing practice guidelines/standards and the core measures. Draft a priority plan, include reasonable timelines, and identify responsible individuals. Consider external expert consultation. Initiate the P-D-S-A model for testing change—it will be described below. Measure, evaluate, revise, implement. Monitor progress, engage leaders, and establish performance metrics. Measure and publish results.
Strategies to integrate practice expectations for age-appropriate care into the annual performance evaluation and ensure balanced accountability for the delivery of age-appropriate care are also suggested. These recommendations reinforce the current knowledge base in DC implementation but are not specific enough to use as guidelines for implementation. However, they were greatly valuable in the development and validation of our current guidelines.
Institutional implementation guidelines/strategies in health-care fields other than in DC
Few organizations have institutional or system implementation guidelines and even fewer focus their work on health-care priorities. The American National Implementation Research Network’s (NIRN) mission is to contribute to the science of implementation and its best practices, organizational change, and system reinvention to improve outcomes across the spectrum of human services. A major goal of the NIRN is to help establish an evidence base for implementation processes and practices of evidence-based programs. NIRN guidelines were used to develop the general methodology of the implementation process of the present guidelines. Their active implementation framework provides a mid-range theory to:
organize current knowledge into useful frameworks, develop strategies to support implementation and scale up of evidence-based programs, establish relevant measures of implementation factors in practice, and develop a better laboratory in which imputed causal mechanisms can be studied, in order to improve the predictive validity of the theoretical frameworks and the precision of the measures.
In 2005, the NIRN published a monograph (meta-review) based on three decades of empirical implementation studies over a wide range of endeavors, for exploration, purposeful selection, clarification, improvement, and systematic implementation of a program model of any kind (Fixsen et al., 2005). To this day, their recommendations still stand (Bertram et al., 2015) and were supported by a multi-agency Consensus National Policy Paper (Bertram, Blase, Shern, Shea, & Fixsen, 2011). This Consensus was supported by the American Center for Mental Health Services, Mental Health America, the National Association of State Mental Health Program Directors, Vanguard Communications, as well as the NIRN. Although mostly about mental health prevention and promotion, these recommendations echo the AAP position statement on toxic stress and their ecobiodevelopmental framework as well as one of the main concerns of DC: infant mental health.
Of note, this model has been supported by European NIDCAP instructors and specialists (Ratynski, 2014). Their recommendations were thus endorsed by the present guideline.
A NIRN consensus brief (updated meta-review from 2005) outlined key components for effective implementation of prevention/promotion initiatives such as skill-based programs and offered a structural and procedural framework (Bertram et al., 2011). Looking at different practice models as well as their implementation and outcomes, the NIRN concluded that even with an effective program based on best-practices and core measures, ineffective implementation will lead to ineffective and unsustainable program and outcomes (Bertram et al., 2015) which is one of the major issues in DC implementation.
Consequently, the need to follow an implementation process with functional strategic stages is essential and can take up to 4 years to unfold. The NIRN’s model includes four functional stages of implementation: exploration, installation, initial implementation, and full implementation.
The Institute for Healthcare Improvement (IHI, 2016a) in the USA is another organization that recommends the use of the P-D-S-A Model for Improvement. The Model for Improvement, developed by Associates in Process Improvement, (Vasquez-Ruiz et al., 2014) is a simple, yet powerful tool for accelerating improvement. The PDSA cycle is shorthand for testing a change by developing a plan to test the change (Plan), carrying out the test (Do), observing and learning from the consequences (Study), and determining what modifications should be made to the test (Act) (IHI, 2016b). It is often the last two steps that are the most difficult to implement. Care should be taken to ensure the importance of adjusting the strategy to the response of the medium (study) to complete the PDSA and Act. This model is not meant to replace change models or implementation guidelines but rather to accelerate improvement.
This model is also supported by NANN (Carrier, 2002) as well as having been used in other DC implementation programs (Coughlin, 2016). It is our opinion that it should be used as an implementation strategy jointly with the current guidelines to reinforce implementation and accelerate success and improvement.
Guidelines for institutional implementation of developmental neuroprotective care in the NICU—Condensed table of recommendations.
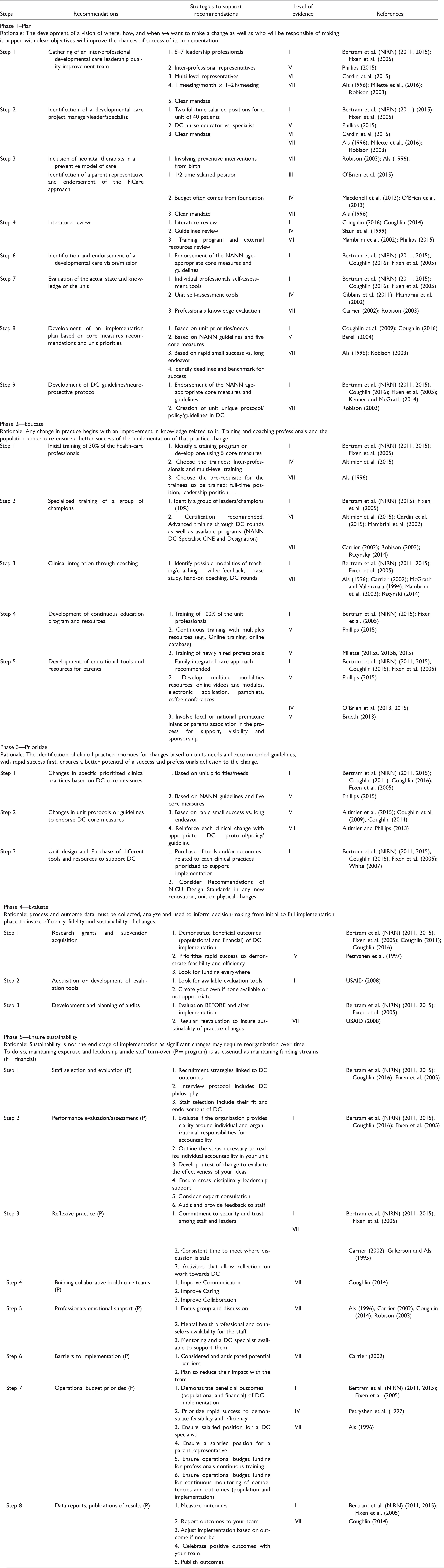
Methodology
The following methodology of research and presentation is based on the NANN Instructions for Writing Clinical Practice Guidelines (NANN, 2009).
Focus
These guidelines focus on institutional implementation of developmental neuroprotective care to improve the operationalization of the DC core measures which include protecting sleep, decreasing pain and stress, implementing age-appropriate activities of daily living, implementing family-centered care, and promoting a healing environment (Coughlin, 2011). A methodological framework of organizational changes and strategies are presented to maximize and implement clinical practice improvement at a unit/institutional level.
Objective
To improve the quality of care provided to the premature and critically ill hospitalized infant in NICUs or special care nurseries by the adoption and implementation of institutional developmentally supportive, neuroprotective care guidelines that align with the core measures for age-appropriate care (Coughlin et al., 2009).
Users and settings
Intended users of this guideline include all providers of direct and indirect care, clinical leaders, and agents of change as well as administrators of NICU and special care nursery settings.
Target population
Guideline recommendations apply to all providers of direct and indirect care, clinical leaders, and agents of change as well as administrators of NICU and special care nursery settings implementing a program of developmental neuroprotective care.
Evidence collection method
A comprehensive electronic search of articles published between 1980 and 2016 was conducted in Medline, Cumulative Index to Nursing and Allied Health Literature, the Cochrane Database, Psychology and Behavioral Sciences Collection, PsycINFO, and Google Scholar using the keywords: DC, trauma-informed care, age-appropriate care, neuroprotective care, infant, premature, implementation, institutional, organizational, guidelines, recommendations, and core measures. Articles were selected for inclusion if they identified specific interventions within the five core measures, NANN guidelines, implementation strategies or recommendations with evidence that improved short- or long-term outcomes for hospitalized infants as well as demonstrated efficacy towards implementation outcomes. Both French and English articles were included.
Recommendations grading criteria
Rating system for the hierarchy of evidence (Melnyk & Fineout-Overholt, 2010).
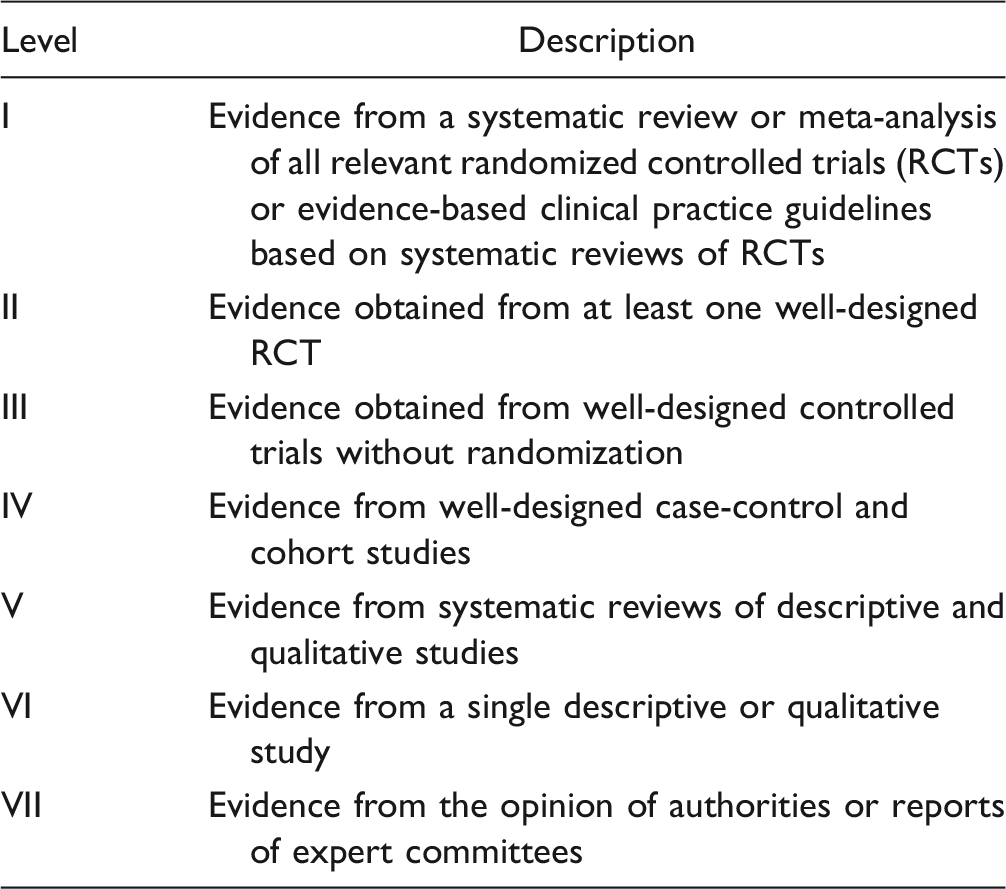
Method for synthesizing evidence
The quality of evidence was evaluated by three independent reviewers using a predetermined structured format. Systematic reviews and randomized controlled trials were considered the strongest level of evidence. When these were not available, cohort studies, case-controlled studies, consensus statements, and studies using qualitative methods were considered the strongest level of evidence for a phenomenon of interest. However, when those were not available, single well-executed independent studies were considered. As well, research outside of the field of DC was included if their main contribution included implementation strategies and guidelines.
Prerelease review
Review was provided during presentations of the material in three settings: at the 29th Annual Gravens Conference on the Physical and Developmental Environment of the High-Risk Infant in Clearwater Beach, FL (Milette & Martel, 2015); at the 6e congrès mondial des infirmières et infirmiers francophones (6th World Congress of francophone nurses), Montréal, Canada (Milette, 2015a), and at the 5th CAPWHN conference in Quebec, Canada (Milette, 2015b).
Discussion
The present guidelines provide a much-needed implementation framework to ensure consistency of care across settings, sustainability of a DC unit practice and institutional accountability for best practices. This step-by-step framework provides an implementation methodology and supporting strategies to improve health-care professional’s competencies and accountability for DC best practices at both the unit and institutional levels.
Patients’ preferences
These guidelines promote patients and their family, to be treated with dignity and respect and receive safe, quality evidence-based care. The family is here defined by the parents of the neonate.
Potential benefits and harms
The anticipated benefits in the consistent implementation of this guideline by all care providers include an improved consistency in the implementation of DC practices in multiple units (implementation outcome), an enhanced level of health-care professional’s competency and accountability for evidence-based DC best practices (implementation outcome), as well as an improved efficiency and quality in care delivery (patient outcome). We also anticipate a better sustainability of the practice change with the requirement for institutional involvement (implementation outcome). Potential harms are yet to be identified but they could relate to these guidelines being perceived as a strict protocol and prevent flexibility in their implementation. This could impede the input of the clinicians’ experience and their clinical judgments. However, it is important to remember that these guidelines are meant as a flexible framework to be implemented to suit different contexts and needs.
Implementation considerations
The NANN age-appropriate guidelines (Coughlin, 2011) anticipated barriers to implementation including the absence of an effective process for practice improvement. Organizational commitment to a culture of safety and high-quality patient care is critical to achieve buy-in and subsequent consistent and reliable provision of care. Although the present institutional implementation guidelines answer that recommendation and consist in the ultimate goal evidence-based practice of developmental neuroprotective care implementation, they might require major changes in health-care delivery in many units and countries. For those units were DC is already present, these guidelines could guide further development by providing a step-by-step approach to future changes. As well, stepwise progress in countries where DC is a new concept can be initiated, and this guideline can help guide these changes. Part B of this article will present the recommendations and justification for the successful implementation of each steps of the present Guidelines (Milette, Martel, & Ribeiro da Silva, 2017). They are essential to the comprehension of this part.
Update plan
The guidelines for the institutional implementation of developmental neuroprotective care in the NICU are scheduled for review in 2020.
Footnotes
Author Note
Author Biographies
Her research interests are developmental care, noise and light reduction in NICUs and PICUs, and neonatal intensive care design. In 2011, she acted as advisor for the NICU design team within the new CHUSJ specialised units building. In 2015, she also joined the leadership group on change at the CHU Sainte-Justine to perfect her work with health professionals. In 2016, she joined the Canadian Neonatal Brain Platform (CNCP) with her participation in the project to transform the neonatal unit of CHU Sainte-Justine into a neuro-neonatal unit for the neuroprotection of newborns at risk for brain damage. To ensure the advancement of development care in research, she becomes an associate clinician member of the Quebec Network on Nursing Intervention Research (RRISIQ). She is the author of several research articles on these subjects, co-author of a book in development care with a second edition in progress, scientific director of a reference book on clinical examination of the newborn and a perinatal educational book (Chenelière Education). She is also a lecturer and invited speaker in many academic and professional presentations, participant in national and international conferences, and clinical training of nurses and doctors in hospitals.
