Abstract
The use of age-appropriate care as an organized framework for care delivery in the NICU is founded on the work of Heidelise Als, PhD, and her synactive theory of development. This theoretical construct has recently been advanced by the work of Gibbins and colleagues with the “universe of developmental care” conceptual model and developmental care core measures which were endorsed by the National Association of Neonatal Nurses in their age-appropriate care of premature infant guidelines as best-practice standards for the provision of high-quality care in the NICU. These guidelines were recently revised and expanded. In alignment with the Joint Commission’s requirement for healthcare professionals to provide age-specific care across the lifespan, the core measures for developmental care suggest the necessary competencies for those caring for the premature and critically ill hospitalized infant. Further supported by the Primer Standards of Accreditation and Health Canada, the institutional implementation of these core measures require a strong framework for institutional operationalization presented in these guidelines. Part B will present the recommendations and justification of each steps behind the present guidelines to facilitate their implementation.
Introduction
Part A of this article presented the background and rationale behind the present guidelines and their condensed table of recommendations (Milette, Martel, & Ribeiro da Silva, 2017). They are essential to the comprehension of this part that will focus on the recommendations and justification for the successful implementation of each step of the five phases of the Guidelines. They are presented in an algorithm form in Figure 1. The Guidelines were developed by an inter-professional team, reviewed by a board of experts in the field from different nursing associations, and is thus a joint position statement from the Canadian Association of Neonatal Nurses, Canadian Association of Perinatal and Women’s Health Nurses, National Association of Neonatal Nurses, and Council of International Neonatal Nurses. The Guidelines involve changes in all aspects of the health care institution: clinical care, education, management, and research. Accordingly, these Guidelines are operationalized over different phases and steps over time, and outcomes are measured for quality improvement as well as for research publication purposes. These phases and steps might sometimes occur in parallel, while others might be delayed, depending on the need and priorities of each unit. Likewise, they can work in circularity, where one change might influence another. The Guidelines therefore aim at providing a framework for the standardization of the implementation of developmental neuroprotective care while allowing some flexibility to suit the different needs of each individual unit and its programs.
Algorythm version of the Guidlines for the institutional implementation of developmental neuroprotective care in the NICU.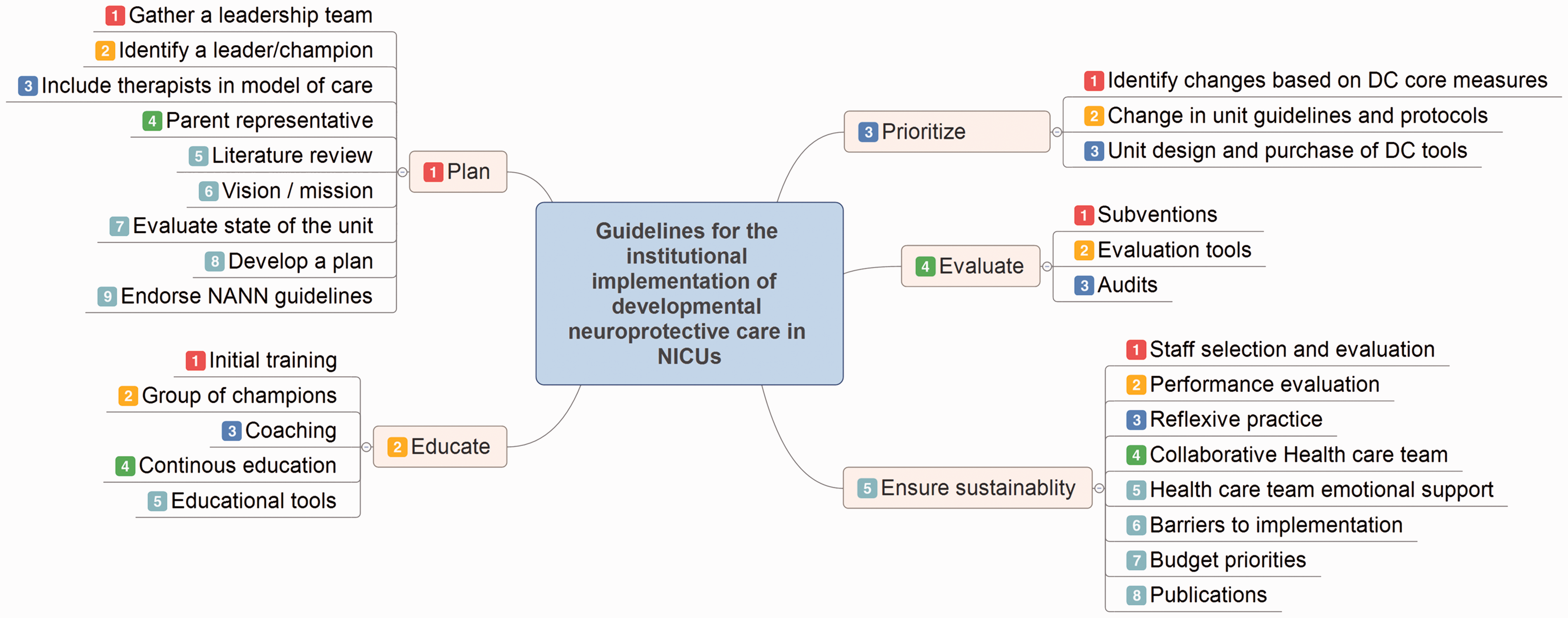
Methodology
Development of the institutional implementation of developmental care (DC) guidelines based on the literature review—recommendations, rationale, and outcome review.
Phase 1—Plan
This phase is equivalent to the exploration and installation stages of the National Implementation Research Network (NIRN) (Bertram, Blase, Shern, Shea, & Fixsen, 2011).
Step 1—Create an inter-professional developmental neuroprotective care leadership quality improvement team
Any long-term change involving a new philosophy will take time and meticulous planning to make sure new practices will be adopted by all. It must also be sustainable; a formal process that is endorsed by every professional on the unit is therefore a pre-requisite (Bertram, Blase, & Fixsen, 2015). In fact, it is essential for systemic adoption of a DC framework (Als, 1996). Robison (2003) identified a model for the continuum of leadership to ensure an effective developmental program, described as an inter-professional collaboration and developmental leadership representing three distinct groups: professionals with influence, those with authority, and those with power:
Professionals with influence have the knowledge, insight, and understanding of DC and include DC specialist, occupational therapist (OT), and physical therapists (PT), as well as nurses and parents. Their role on the unit would be related to the education, performance assessment, consultation, and program development. Phillips (2015) mentions the importance of having the affected staff to be intimately involved in the process. Professionals with authority manage resources and staff accountability with maintenance of competencies. They include standards committee, NICU managers, head nurses, coordinators, and hospital administrators (Bertram et al., 2011). Their roles imply guidance of the project, staff development, staff accountability, as well as budget and resource allocation. Professionals with power include those in direct medical care who control caregiving practices. They are the physicians and the nurse practitioners. Their role should be to support the implementation by attaining the required knowledge and collaborating in the decision-making with the rest of the inter-professional team.
These are individuals or teams of people with content and implementation knowledge who support, guide, and help adjust the organizational implementation (Bertram et al., 2015). Their role includes a review of existing practice standards and guidelines, performing an assessment of the unit, and the drafting of an action plan (Coughlin, 2016). Meetings should take place on a monthly or bi-monthly basis (Als, 1996). Subsidization of these meetings is recommended as a strategy to improve participation (Phillips, 2015).
Step 2—Identification of a DC project manager/leader/specialist
In order to facilitate and support the implementation of DC, two salaried positions are needed for a 40–50 bed unit (a DC specialist and a nurse educator) (Als, 1996). The DC specialist should hold a master’s degree in a developmental discipline (psychology, developmental pediatrics, social worker, occupational or physical therapists, neonatal clinical nurse specialist, and/or neonatal nurse practitioner) and have knowledge/expertise of the NICU. Specific competencies should include communicating and supporting staff, supporting infants and families, teaching, and sharing developmental knowledge. This role is the leader of DC and should be someone with leadership experience and a passion for DC (Phillips, 2015). The DC nurse educator should also hold a master’s degree and have a minimum of three years’ experience in the NICU. This professional is a role model and a teacher. S/he is the link between the leadership team and the bedside team, working on systematic implementation.
Step 3—Inclusion of neonatal therapists in a preventive model of care
Therapists can make invaluable contribution to the care of the high-risk infant by involving preventive intervention from birth while improving physiological functioning and neurobehavioral development (Robison, 2003). As per the NANT (National Association of Neonatal Therapist), neonatal therapists should be an essential part of the NICU team. NANT defines a neonatal therapist as: An occupational therapist, physical therapist or speach language therapist who delivers holistic direct patient care and consultative services to premature and medically complex infants in an NICU … while using an integrated, neuroprotective, family-centered model of practice … to support optimal development, prevent sequelae and nurture the infant-family dyad. (p.25)
Step 4—Identification of a parent representative and endorsement of the FiCare approach
The creation of a parent representative or parent council to promote education and interaction with the health care professional facilitates DC implementation. DC has also been called family-centered (Carrier, 2002) or family-integrated DC (Bracht, O'Leary, Lee, & O'Brien, 2013), which demonstrates the importance of family collaboration, not only in the care of their child, as defined in the core measures and age-appropriate guidelines (Coughlin, 2011), but also as an integral partner within the health care team: parents as partners (D'Agata & McGrath, 2016). In Canada, Family Integrated Care is an example of a “care-by-parent” model to involve parents in the care of their infant by providing them the opportunity to be the primary caregivers for their infant in the NICU (Warre, O'Brien, & Lee, 2014). This kind of approach is endorsed through the age-appropriate guidelines. The role of parent as an and advocate has been documented to improve communication as well as collaboration with the healthcare team, by improving the match between the implementation program and the population’s needs (Bertram et al., 2015). There are some programs available to help parents get involved in the care of their infant in the NICU as well as becoming a member of the health care team (Melnyk et al., 2005; Warre et al., 2014). For increased efficiency, a budget to the height of at least 10% of a full-time equivalent is recommended to be set aside for such a position. In some hospitals where such a position was created, it was the hospital foundation who assumed this budget to ensure its sustainability, as opposed to the unit’s operational budget (Macdonell et al., 2013).
Step 5—Literature review
One of the most important and critical strategies in a process of change remains the review and identification of current knowledge, evidence-based practices, recommendations, standards, and/or guidelines in the field. The review and analysis of the DC literature is an essential step in their implementation (Coughlin, 2010, 2016; Mambrini, Dobrzynski, Ratynski, Sizun, & de Parscau, 2002; Phillips, 2015; Sizun, Ratynski, & Mambrini, 1999).
Step 6—Identification and endorsement of a DC vision/mission
A DC vision should clearly define the philosophy and goals of the unit and what steps will be undertaken to achieve these goals. Als (1996) identified this step as an essential component of DC implementation as it clearly defines what we are, what we want to achieve, and how to get there, making the adoption of a new philosophy easier to follow. Coughlin’s 2016 guidelines for trauma-informed, age-appropriate care expand on the NANN guidelines, updating the five core measures with the latest evidence-based best practices.
Step 7—Evaluation of the actual state/knowledge of the unit
An initial appraisal of individual and unit practice in DC is essential (Mambrini et al., 2002; Robison, 2003). This allows the identification of a starting point for implementation, as well as different specific areas which require more attention than others. In fact, examining the status of a unit helps identify and overcome obstacles affecting progress (Carrier, 2002). Furthermore, Bertram et al. (2015) suggested an assessment of resources, characteristics, and needs of the population to ensure the best possible match with the new suggested changes (Bertram et al., 2015). Few evaluation/self-assessment tools in terms of DC knowledge and state of unit practice are available. Robison (2003), the newborn individualized developmental care and intervention program (NIDCAP), and the Wee Care have institutional evaluation tools that are not published but mention importance of such tools (Cardin et al., 2015). In 2011, the NANN published a “Core measure in DC: Self-Assessment” to be employed at the individual and unit level with the goal of targeting improvement initiatives and identifying steps to achieve positive changes (Gibbins, Coughlin, & Hoath, 2011). Many units have reported using it effectively, and it has been adapted in other languages as well (Zhang, Lee, Chen, & Liu, 2016). Recently, another psychometric scale for the assessment of the quality of DC in a NICU was published in Iran—yet another demonstration that these kinds of tools are in demand (Soleimani, Torkzahrani, Rafiey et al., 2016).
Step 8—Development of an implementation plan based on the endorsement of DC core measures recommendations and unit priorities
This step is crucial and the implementation plan should identify achievable, measurable goals rather than long-term steps (Als, 1996). Rapid, small successes will ensure future involvement and help in reducing resistance to change more rapidly than long arduous ones (Bareil, 2004). The implementation plan should answer specific unit needs and priorities in addition to answering evidence-based practice guidelines (Coughlin, 2011; Coughlin, Gibbins, & Hoath, 2009; Robison, 2003).
Step 9—Development of DC guidelines/neuro-protective protocol—Establish standards of care
To systematically address each of the structural components of its implementation drivers (steps in the implementation process), the NIRN strongly recommends the development of protocols to measure fidelity (Bertram et al., 2011). Robison (2003) advised establishing standards of care to provide guidance, define direction, and professional accountability. Her four standards of care were later taken on by the NANN to organize its DC for newborns and infants reference book (Kenner & McGrath, 2010). The core measures in DC (Coughlin et al., 2009) as well as the NANN age-appropriate guidelines (Coughlin, 2011), and now their expansion (Coughlin, 2016), should herewith be an essential part in the development of any unit guidelines or protocol in developmental neuro-protective care, if not simply endorsed as is.
Phase 2—Educate
Training and coaching are an integral part of the NIRN installation phase (Bertram et al., 2011): successful, efficient, and sustainable implementation requires behavior change from professionals, their supervisor, and the organization. Teaching and coaching are the primary means to attain this in the early stages of implementation. Training provides knowledge and sets the stage for coaching. For the NIRN, effective modalities of training are necessary to have greater impact on knowledge acquisition, including lectures, demonstrations, and behavior rehearsals. This is supported by many experts (Als, 1996; Phillips, 2015; Ratynski, 2014).
Step 1—Initial training of 30% of the health care professionals
Als (1996) was the first to suggest the training of a core group of 10% of the nursing staff for a minimum momentum, in order to obtain successful implementation of unit-wide DC. She also suggests choosing nurses from all three shifts to ensure modeling, trust building, and teaching skills. They should also be full-time nurses, for more effective influence on the rest of the team. Robison (2003) supports this in her step 4—Structuring a program (e.g., NIDCAP). However, as DC is not only a nursing issue, it should be endorsed by all professionals who come into contact with the infant—nurses, nurse practitioners, neonatologists, residents, fellows, neonatal therapists, social workers, respiratory therapists, pharmacists, lab technicians, etc.— a recommendation also endorsed by the Wee Care program (Altimier, Kenner, & Damus, 2015). More importantly, whichever training program is chosen for the unit’s team of professionals (NIDCAP, Wee Care, Caring Essentials Collaborative, Programme de formation en soins du développement (PFSD)/Developmental care training program, or another), the core measures in DC are to be included in its pedagogic content (Altimier et al., 2015; Coughlin, 2014, 2016). The inclusion of administrators and supervisors in this training program is also an essential part in ensuring their support in regards to any required change in clinical practice. However, 10% of the staff might not be sufficient enough for a beneficial momentum in a large neonatal unit, as a sizeable number of professionals could be very difficult to influence. In fact, Carrier (2002) mentions that the size of the unit (in terms of number of beds as well as professionals) could be a barrier to implementation. It is therefore essential to lead a change in DC culture with a strong core group of professionals. Thus, a minimum of 30% might be necessary for a successful momentum in large NICUs. These recommendations are all endorsed by the present guidelines. This step involves the selection of a training program and a team comprised of the health care professionals to participate in the program, and that have the suitable pre-requisites for their inclusion in the team (full-time position, informal leader amongst peers, formal leader like nurses in charge, NNPs, etc.).
Step 2—Specialized training of a group of champions
Many experts recommend the training of a specialized champion group in DC to act as role models and “trainers,” namely as potential resources for the bedside clinician (Altimier et al., 2015; Bertram et al., 2011; Cardin et al., 2015; Carrier, 2002; Mambrini et al., 2002; Ratynski, 2014; Robison, 2003). Their presence and expertise would guide and support the implementation of DC both at the organizational level, as they would be involved in strategic planning, but also at the bedside, where they would act as role models. Some champions can come from the leadership quality improvement team, but most are bedside professionals chosen for their natural leadership and positive influence on the unit. Additionally, the NIRN recommends that coaches are well selected and trained to emply the improvement cycle loop technique (observe—coach—feedback—plan—re-observe) (Bertram et al., 2011).
Step 3—Clinical integration through coaching
The NIRN mentions that competent and confident use of new practice is more effectively developed through skillful on-the-job coaching (Bertram et al., 2011). This ensures the development of new capabilities rather than reverting to previous, less effective approaches. This is supported by Carrier (2002), who also mentions that knowledge alone is not sufficient to support the application of DC. Since DC requires the acquisition of concepts and changes in philosophy, as opposed to a mere practical “recipe,” the teaching process needs to involve bedside teaching as well as theoretical teaching (Mambrini et al., 2002). Case-based learning or experiential learning also needs to be used (Carrier, 2002). This is supported by Als (1996), Cardin et al. (2015), and McGrath and Valenzuela (1994), which recommends multiple modalities for learning, such as video-feedbacks, external experts, case study presentations, role modeling and mentoring, positive reinforcement, and even DC rounds (Mambrini et al., 2002; Ratynski, 2014).
Step 4—Development of continuous education program and resources
Initial training is essential, but ongoing professional education related to DC is a necessary strategy for successful implementation (Wyly, Allen, Pfalzer, & Wilson, 1996). The NIRN mentions that training and coaching are primary means to influence behavior change but in-service training (using multiple means) during subsequent implementation after the initial phase is an efficient and essential means to develop and ascertain shared knowledge (Bertram et al., 2011). Multiple educational modalities should be available to ensure better retention of clinical changes in practice: hand-outs, posters, intra-hospital web-based education, and hands-on skill demonstration are a few of them (Phillips, 2015). The training/orientation of newly arrived health care professionals is also important and needs to be considered in this step, as supported by Als (1996).
Step 5—Development of educational tools and resources for parents
The NIRN suggests the use of multiple educational tools when creating teaching resources for the population served by the program (Bertram et al., 2011). As DC is a family-centered or family-integrated approach, the role of parents is appropriately central to the success of any change or implementation in a neonatal unit. Teaching parents should therefore begin as early as possible during their hospitalization to maximize their parental competence (Melnyk et al., 2004) and use as many tools and resources as possible to facilitate every learning style (Coughlin, 2016). In order for these resources to be useful, the identification of their needs and the development of support tools should be undertaken in collaboration with them (Phillips, 2015). Essentially, with family-integrated care, this process is done by parents for other parents, which has been demonstrated to be very effective (Bracht et al., 2013; Macdonell et al., 2013; O'Brien et al., 2013, 2015).
Phase 3—Prioritize
Step 1—Changes in specific prioritized clinical practices based on DC core measures, and
Step 2—Changes in unit protocols or guidelines to endorse DC core measures
Change in clinical practice is the main goal of program implementation (Bertram et al., 2011). Moreover, changes in clinical practices and implementation of the five core measures through the age-appropriate guidelines of the NANN are at the basis of these steps and essential for successful DC implementation (Altimier et al., 2015; Altimier & Phillips, 2013; Coughlin, 2011, 2014, 2016; Coughlin et al., 2009; Phillips, 2015). However, it is also important to consider the state of the unit, its needs, and priorities to make sure those changes are sustainable, as they answer an identified need by the team (Coughlin, 2016; Phillips, 2015). As well, those priorities should also be considered for their potential rapid success—as it is easier to implement a short rapid change that we know will be successful to encourage and convince the team that DC works and be able to later make further more complex changes that will take more time. Bertram et al. (2011) calls this the transformation zone in their initial implementation phase.
Step 3—Unit design and the purchase of different tools/resources to support DC
Part of the installation phase of the NIRN highlights the importance of a practical approach to program launch. Creating a project budget and ensuring there is available space to house any equipment purchases deemed necessary for program must be done thoughtfully (Bertram et al., 2011). Coughlin (2016) suggests that units assess their physical, human, and system environments to determine what resources are required to ensure the consistently reliably provision of age-appropriate care. In terms of unit design, those recommendations are highly supported by the committee to establish recommended standards for newborn intensive care unit design. It presents 27 NICU standards for newborn intensive care newly built environment, although most have broader application for the care of ill infants and their families (White, 2007, 2012). Multiple experts support those recommendations (Als, 1996; Altimier & Phillips, 2013; Ratynski, 2014). Their recommendations are also endorsed by the present guidelines.
Phase 4—Evaluate
The NIRN recommends that process and outcome data must be collected, analyzed, and used to inform decision-making from the initial to full implementation phase (Bertram et al., 2011). It is thus essential to evaluate both population outcomes and implementation outcomes. Population outcomes are well documented in DC but not implementation outcomes like knowledge improvement, behavior improvement, changes in practices, and staff satisfaction. To do so, it is important to allow funding for audits and research. This is supported by Coughlin (2014, 2016) as well.
Step 1—Research and program grant acquisition
As stated above, the NIRN (Bertram et al., 2011) and Coughlin (2016) both mention the importance of establishing funds needed for implementation success. Financial resources are the most difficult to obtain, but the most essential as well. In order to convince establishments to invest in DC implementation, a demonstration of its beneficial outcomes for the patients might be necessary, but even more the cost effectiveness of such care on the system. The DC patient’s outcomes are well recognized but Petryshen, Stevens, Hawkins, and Stewart (1997) were the first to document that DC implementation in a NICU decreased operational cost by $4340/infant before discharge which they believed might provide administrators with essential information to justify the cost of nurse training. However, the overall lifelong savings for the health care system, in having healthier infants, more competent parents, and caring health care professionals is unknown, although assumed to be very favorable. As DC implementation might seem an enormous endeavor at first, we recommend to get funding for more specific clinical practice priorities that are, as mentioned above, rapid successes to demonstrate the feasibility but also their outcomes. This will allow for more funding in the future. Many sources of funding are available, but sometimes not known. We recommend looking for foundation funding, specific department project funding, research grants, and affiliated university funding.
Step 2—Acquisition or development of evaluation tools
As the evaluation of results/outcomes is essential, the development of evaluation tools for audit is also paramount to assess a program/project’s success. Audits or evaluation tools can be purchased, if available, or created to better suit the needs and reality of the unit. Unfortunately, few audit/evaluation tools are available related to DC clinical practice changes.
Step 3—Audits
The planning and performance of audits might be the only opportunity to evaluate, not only patient outcomes but also implementation outcomes (Bertram et al., 2011). It is thus important to develop an audit tool and collect baseline information before the implementation phase. This data becomes the benchmark for progress and improvement. Re-evaluations of practice improvements should occur regularly, to ensure the maintenance of the clinical practice change on the unit (Bertram et al., 2011; Development, 2008).
Phase 5—Ensure sustainability
The NIRN mentioned that sustainability is not the end stage of implementation as significant changes may require reorganization over time (Bertram et al., 2015). In fact, full implementation occurs when most of the practitioners are routinely providing the evidence-based practice with good fidelity which is more likely to achieve the desired patient outcomes. They suggest that maintaining expertise and leadership amid staff turn-over (programmatic sustainability) is as essential as maintaining funding streams (financial sustainability). Coughlin supports this furthermore in indicating that the establishment of high reliability evidenced-based DC is a function of technical competence, collaboration, communication, leadership, and process design (Coughlin, 2014; Riley, Parrotta, & Meredith, 2012).
Step 1—Program sustainability—administration endorsement—staff selection and evaluation
The NIRN mentions that administrators must diligently and continuously identify and reduce organizational barriers to successful implementation (Bertram et al., 2011). One of the main goals of a facilitative administration is to adjust work conditions to accommodate new functions. They must be proactive. This involves changes in operational as well as financial resources (Coughlin, 2016). In addition to performance assessment above, staff selection, retention, and evaluation should be considered in terms of DC. Thus, recruitment strategies, interview protocols, and staff selection criteria should all include the model elements, theory base, and change as well as description of roles, responsibilities, and expectation for accountability (Bertram et al., 2011; Coughlin, 2016).
Step 2—Program sustainability—administration endorsement—performance evaluation/assessment
Performance evaluation is critical component for any health care professional to maintain competence as well as sustain the success of any implementation with high fidelity. In fact, the NIRN calls it a competency driver (Bertram et al., 2011) that should involve two forms: practitioner performance and organizational performance. Coughlin (2016) pushes this step further to ensure not only competency but accountability as well. She wants us to create, empower, and sustain a just culture of individual accountability across all individuals who interface with the NICU. She thus recommends the following steps: (1) Evaluate if the organization provides clarity around individual and organizational responsibilities for accountability, (2) outline the steps necessary to realize individual accountability in your unit, (3) develop a test of change to evaluate the effectiveness of your ideas, (4) ensure cross disciplinary leadership support, (5) consider expert consultation, and (6) audit and provide feedback to staff.
Step 3—Program sustainability—administration endorsement—reflexive practice
Gilkerson and Als (1995) established a process in the institutional implementation of developmentally supportive care in the NICU with reflexive practice, largely used in NIDCAP, which has demonstrated multiple benefits to date (McAnulty et al., 2013; Ohlsson & Jacobs, 2013; Peters et al., 2009). This reflexive practice was later put into a model for “Reflexive practice in DC – IFDC standards” by Carrier (2002). In fact, she mentions that “leadership can use reflection to review progress, gain insight, discuss issues and identify areas of improvement” (p. 31). Establishing and consistently monitoring responsive and transparent feedback loops for implementation is essential (Als, 1996; Bertram et al., 2011). In fact, initiative champions and influential persons at each level must be engaged to create, facilitate, and sustain necessary organizational culture, climate, policies, regulatory practices, and funding mechanisms so that the new practices thrive and achieve the desired outcomes (Bertram et al., 2011). Effective implementation of a reflexive model implies three key elements: (1) commitment to security and trust among staff and leaders, (2) consistent time to meet where discussion is safe, (3) activities that allow reflection on work towards DC (Carrier, 2002).
Step 4—Program sustainability—administration endorsement—building collaborative health care teams
Coughlin (2014) identified three essential elements to collaborative health care teams: (1) communication, (2) caring, and (3) collaboration. She identifies communication as a “fundamental requisite for all human encounters” (p.74) and suggests the use of structured communication strategies to ensure efficient and consistent communication between staff as well as with parents and infants. For her, caring includes self-care, transpersonal care, and relationship-based care (p. 76)—they will be discussed in our next step. Finally, she mentions that power dynamics and trust impact interprofessional collaboration (McDonald, Jayasuriya, & Harris, 2012). Thus, it is essential to address and resolve interpersonal challenges to have effective patient-oriented teams committed to DC in the NICU (Coughlin, 2014). This is an important mandate for a facilitative administration.
Step 5—Program sustainability—administration endorsement—professionals emotional support
Als (1996) strongly recommended the development of frameworks and resources toward the support of the emotional well-being of all staff. Working in the NICU can be difficult physically, emotionally, and morally at times. Taking constant humane care for little patients and their family can also be draining. Coughlin (2014) mentions that self-care in nursing is often overlooked but crucial in the delivery of quality care, and that caring for colleagues is vital for effective team work and patient safety. It is thus important to make sure that our staff is healthy. DC involves a philosophy of care humanization, and it should apply to our patients as well as each other. Communication, collaboration, and team support is thus essential for the success of DC implementation, this is one of Robison (2003) standards of care. Carrier (2002, 2010) recommends strategies like focus groups and discussion, mental health professional, and counselor availability for the staff, mentoring, and a DC specialist to support them at the bedside in this implementation.
Step 6—Program sustainability—administration endorsement—barriers to implementation
Many authors suggest that financial, linguistic, and the highly flexible approach that is DC are all barriers to its implementation (Als, 1996; Mambrini et al., 2002; Ratynski, 2014). Carrier (2002, 2010) identified six potential barriers for DC implementation that should be considered and even anticipated if possible. These are (1) anxiety from the staff regarding the change, (2) staff patterns or inconsistency of caregivers, (3) high staff turnover, (4) high census and acuity, (5) physician/resident rotation, and (6) staff resistance (p. 32). To these, she suggests multiple possible solutions that require administrative involvement and endorsement at every level.
Step 7—Financial sustainability—administration endorsement—operational budget priorities
Financial sustainability is as essential to full implementation as it was in the initial phase. Often it is a lack of planned financial investment that causes failure in implementation and sustainability (Bertram et al., 2011). In DC, the support of a salaried position for an implementation leader/DC specialist and a parent representative, as presented in Phase 1/steps 2 and 3, should be an essential part of any DC implementation plan. As well, the allocation of operational funds for the maintenance of the tools and the equipment related to DC and continuous health care professional training should be allotted and prioritized. Besides the strategies for funding identified in phase 4, step 1, other strategies are essential, like prioritizing DC in the operational budget.
Step 8—Sustainability—data reports, publications of results and guidelines
Decision support data systems create the condition under which data can be understood and used to make timely decisions in order to improve implementation outcomes. These systems should be useful and accessible to the implementation team at all times (Bertram et al., 2011). It is thus important to report outcomes to the team, to enable readjustment if need be, but also positive reinforcement and celebration of actual success (Coughlin, 2014). As well, the publication of results is essential to inform the scientific and health care community of cost-effective and successful quality improvement implementation to ensure their possible use elsewhere. Pushing this further also means that creating guidelines for implementation when none are available helps with the implementation of the quality improvement team in other units and ensures consistency of care between units (Bertram et al., 2011). This is particularly important when parents get transferred to step-down units closer to their home and expect the same kind of evidence-based quality care in their new environment.
Conclusion
A minimum of three to five years and even 10 years in bigger or more complex units might be needed to change culture and attitudes significantly (Carrier, 2002). The best chance for a successful integration of DC philosophy and its implementation as an organization is patience, endurance, and persistence (McGrath & Valenzuela, 1994). Clearly defined standards, accountabilities, and strong leadership are needed to sustain a cultural shift. The present guidelines will provide an evidence-based systematic approach to their successful implementation in NICU.
Footnotes
Author Note
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors received funding for the Open Access publication of this article from the CANN as well as the TD Bank.
