Abstract
Keywords
Introduction
The global demographic landscape is shifting, with the proportion of people aged 65 years and older expected to rise significantly, reaching an average of 28% throughout the Organization for Economic Co-Operation and Development countries by 2050, with some countries like Japan, Spain, Portugal, Greece, and Korea forecasting a share as high as 40%.1 Similar trends are anticipated in countries like China, the United States, Mexico, and Israel, where higher fertility and migration rates are also contributing factors. 1 The COVID-19 pandemic further integrated new challenges among older adults and their caregivers, intensifying stress levels and reducing access to social support networks. 2 This shift carries implications for healthcare, particularly with the rise in dependency and the prevalence of chronic illnesses and disabilities among older adults, leading to an increased demand for palliative care services. 1 Chronic diseases have become the primary causes of death globally, with 60% of all cancer diagnoses occurring in individuals aged 65 years or older.3,4
Many older adults express a preference to remain at home during their final years, receiving care either from family members or through home assistance services. 5 Home-based palliative care (HBPalC) also has found to decrease hospital visits and be more cost-effective than hospital care. 6 In a cohort study of older adults 65+ years from hospital-based multiprofessional palliative care units in London, Dublin, and New York, the home was the most preferred place of death, followed by in-patient palliative care hospice units. 7 The hospital was the least preferred. Likewise, an American study on patients with advanced cancer cared for in a specialized palliative care unit or at home with outpatient specialized palliative home care showed that 58% of the patients in specialized palliative care units preferred their home for the place of death, as did 72% of the patients receiving outpatient care. 8 Research strongly supports that family and/or informal caregiving is crucial in facilitating home care,9-11 but this often comes at a substantial cost to the caregivers themselves. 12 Informal caregivers are defined as individuals responsible for providing care to the patient at home and executing specific instructions from healthcare providers. 13 In the United States alone, unpaid family members provide an estimated $500 billion worth of care annually, forming a critical but often unsupported pillar of the healthcare system. 14 Numerous studies have recognized the challenges of caregiving, particularly the decline in informal caregivers’ quality of life.15,16 Many of these caregivers are spouses who are also aging and may have functional limitations or serious illnesses, yet nearly half manage caregiving duties without any external help. 17 The provision of care without adequate training, respite, or reimbursement leads to significant burden, and the healthcare system has yet to offer practical solutions to support or compensate these caregivers appropriately. 14
Despite the critical role of informal caregivers, literature reviews on the specific challenges they face, particularly when caring for older adults receiving palliative care at home, are lacking. Ventura et al. 18 conducted a systematic literature review on the self-reported unmet needs of patients and caregivers in HBPalC. While the study reported important findings, it lacked the sole focus on older adults and sampled all age groups. Jika et al. 19 conducted a comprehensive scoping review exploring the experiences of informal caregivers while caring for older adults in chronic illness. However, their study, despite significant findings, did not specifically address the unique aspects of HBPalC. Older adults in HBPalC tend to have multiple comorbidities which makes caregiving a complex process. 20 Thus, this scoping review seeks to address these gaps in the literature and provide a foundation for future research. This scoping review addressed the following research question: What challenges do informal caregivers of older adults receiving home-based palliative care experience while carrying out their responsibilities? This scoping review did not require Institutional Review Board approval.
Method
This scoping review followed the methods outlined by Arksey and O’Malley 21 and Levac et al. 22 and followed five steps: (1) identifying the research question, (2) identifying relevant studies, (3) selecting the studies, (4) charting the data, and (5) collating, summarizing, and reporting the results. In addition, this scoping review was conducted using Preferred Reporting Items for Systematic Reviews and Meta-Analyses statement for reporting scoping reviews (PRISMA-ScR) to show the numbers of publications identified and screened for eligibility during the scoping review process.21-23 The protocol was published in the Open Science Framework (OSF) and can be accessed at osf.io/jehtq.
Identifying Relevant Studies
A scoping review was conducted between June 2024 and August 2024. This review utilized the following electronic databases to identify potentially relevant studies from various disciplines in the EBSCO platform: Academic Search Complete, AgeLine, APAPsycArticles, Cumulative Index to Nursing and Allied Health Literature (CINAHL) Complete, Global Health, Medline, PsycINFO, Social Work Abstracts, and Web of Science. Search results were then imported into Zotero reference management software for organization. Those results were then uploaded into Covidence, a review management software for screening. 24
The search strategy was informed by the Population, Concept, and Context framework 25 and completed using a combination of terms in these three areas: population (eg, “informal caregiver” or “family caregiver”), concept (eg, “barrier” or “problem”), and context (eg, “older adults in palliative care at home” or “home-based palliative care of older adults”). A key search strategy was employed using Boolean operators and modifiers, including the asterisk (*) to search for any word containing the stem or letters before the asterisk 26 (Search strings, supplementary file).
Inclusion and Exclusion Criteria
The following eligibility criteria were used for the inclusion of articles for use within this review. To broaden our search strategy, we searched for articles published before June 1, 2024, and did not restrict by publication date. To be eligible for inclusion, articles must have been peer-reviewed, published within an academic journal and written in English. The population considered for inclusion in this review comprised of individuals who were caring or being responsible for providing care for HBPalC patients. This included any non-professional caregiver who provided care for the patient in their home, and for the purpose of this paper are being defined as carer, home-based carer, informal carer, spousal carer, and informal caregiver. For this paper, HBPalC was operationalized as medical and supportive care provided to patients with a life limiting or chronic disease within their home environment. Lastly, we focused on patients with a mean age greater or equal to 65 years, consistent with the National Institute of Health 27 definition of “older adults.”
Studies were excluded if, they focused on the perspectives of palliative care patients, health professionals, or paid caregivers, or failed to specify the age of the individual receiving palliative care, or were reviews, unpublished works or were not published in a peer-reviewed, and lastly, studies that sampled care recipients receiving care at a facility.
Study Selection Process
The first author led the study selection process and completed this review through periodically consulting with the university social science librarian. Potential articles for inclusion from primary searches were imported to Covidence, a review management software. 24 When potential articles were identified, they were sequentially evaluated by title and abstract. The research team then completed full text reviews of selected studies. When there were conflicts, the research team revisited the articles and reached consensus together.
Data Charting
Data charting followed the descriptive-analytical method described by Arksey and O’Malley. 21 The content was charted and extracted utilizing Covidence and followed these general content descriptors: author(s) and year of publication; title of study; study population(s) with brief descriptive statistics; the purpose of the study; research design of the study; outcome measures; and key findings (see Table 1).
Data chart.
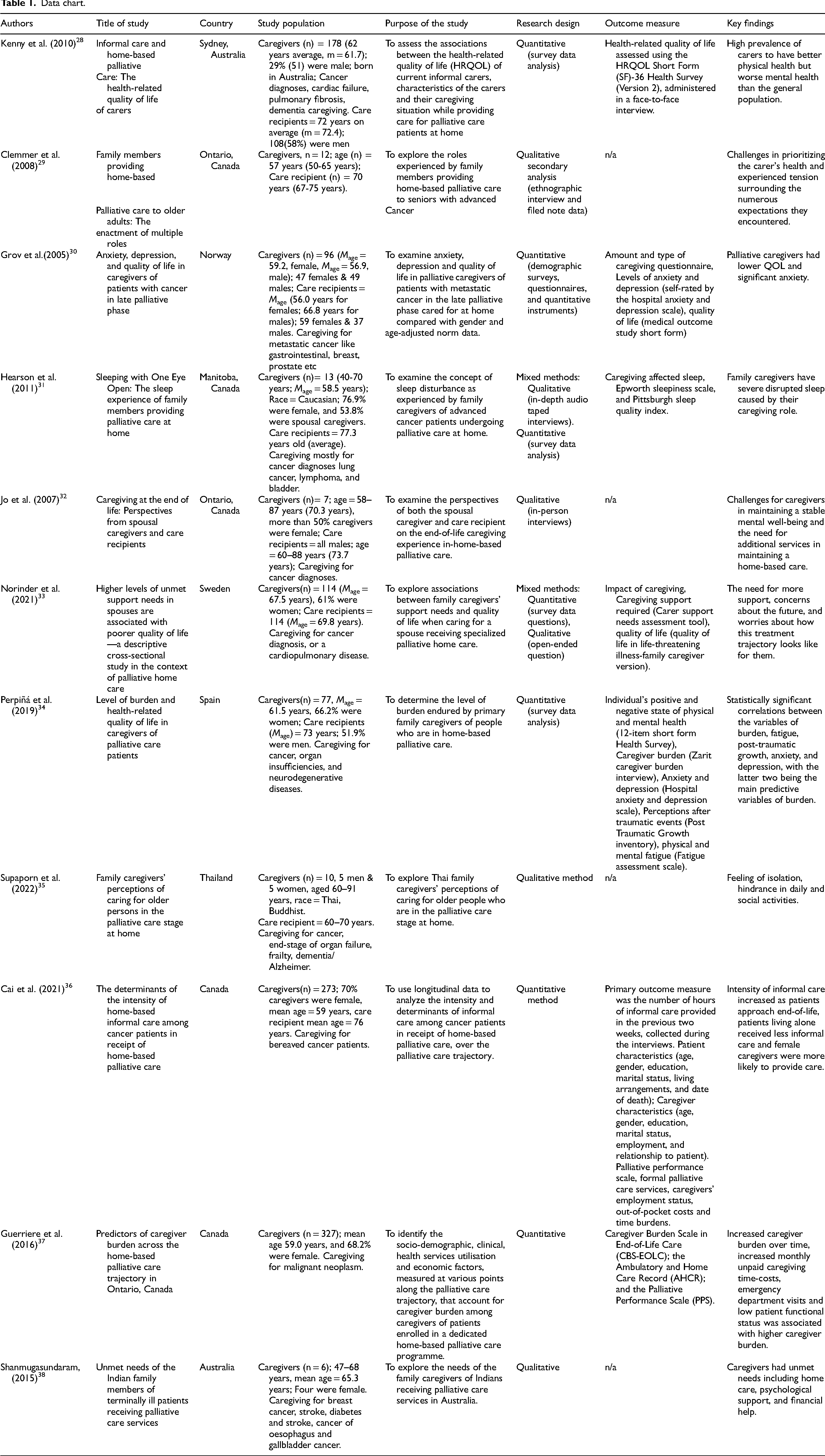
The PRISMA flow chart (see Figure 1) presents a visual summary of the screening process through different phases of a scoping review. Titles and abstracts of 3859 articles were initially screened, and 2003 articles were fully reviewed for eligibility. Upon completion of each stage of the screening process, 11 studies remained for inclusion.29-39 A total of 108 studies were excluded for reasons such as insufficient specificity regarding the patient's age, the patient not being an older adult, or the patient not receiving palliative care, among others. The 11 included articles mostly (n = 5) utilized quantitative methods28,30,34,36,37 or qualitative methods29,32,35,38 (n = 4), with (n = 2) studies utilizing a mixed methods31,33 approach. The oldest article identified through the search was dated in 1988. Among the included studies, spousal caregivers were the most identified, followed by children, and non-family members (eg, friends). The caregivers’ age ranged from 35 to 70 years across the studies. The diagnoses of the individual receiving care varied from Alzheimer's disease and related dementias, cancer, cardiac failure, pulmonary fibrosis, cardiopulmonary disease, neurodegenerative disease, and organ insufficiencies.
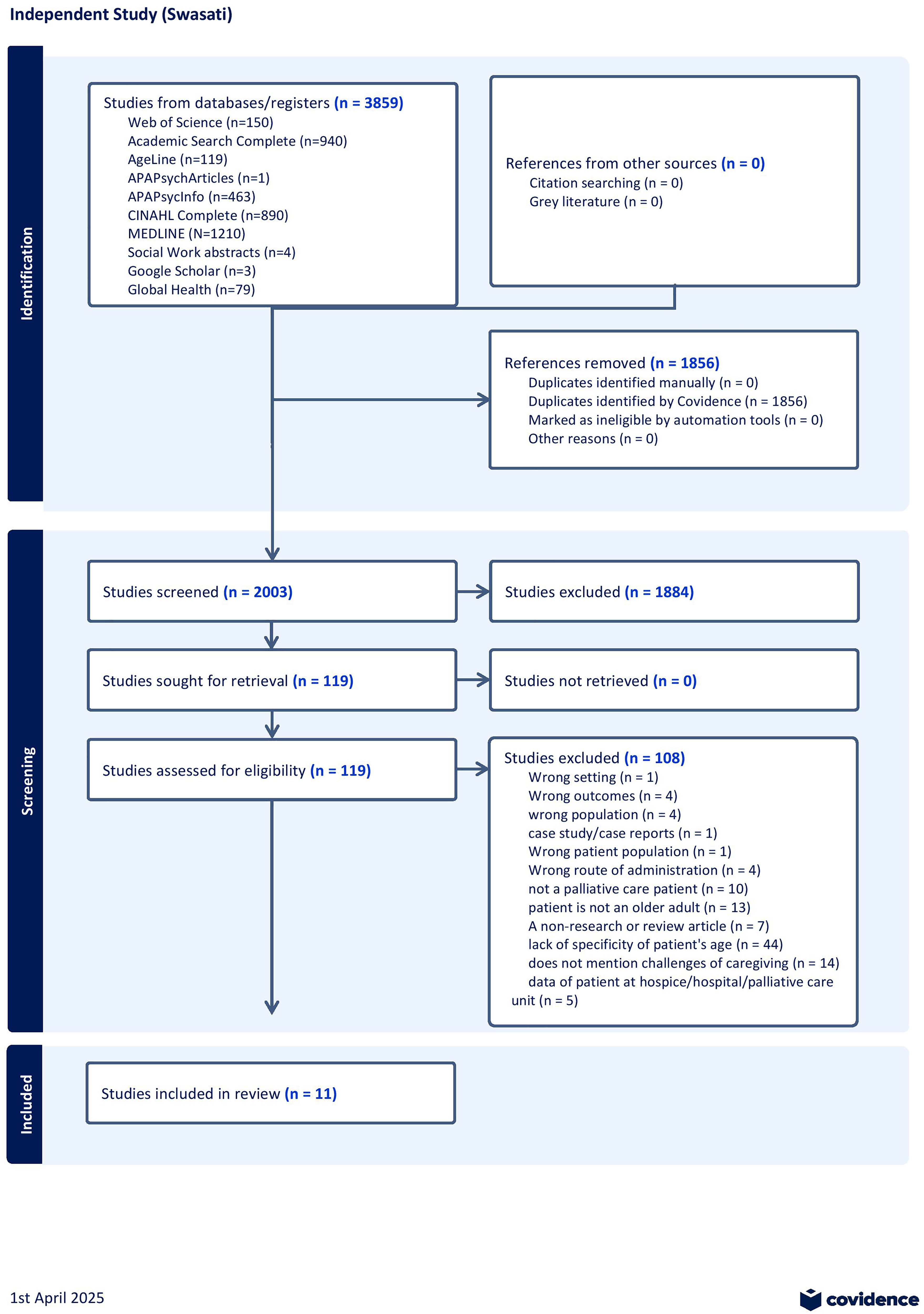
PRISMA flow-chart.
Data Synthesis
Thematic content analysis was used to articulate identified themes among the key findings from each study. 28 While the authors did not use predefined sub-questions, they did employ an inductive approach that allowed themes related to social and structural variation to emerge organically. The authors noted all descriptions and findings from the included studies which were relevant to our research question and to the topic of challenges experienced by informal caregivers of older adults in HBPalC. The authors then added codes from each of the studies (eg, reported inadequate healthcare support relevant to caregiver concerns), and followed this process throughout this phase of data analysis. Each collection of codes was designated as an initial theme (eg, financial strain). These themes and codes were re-examined to ensure consistency among all the included studies. The authors met and discussed these codes and their resultant themes.
Results
Exhaustion and Health Deterioration
Seven out of 11 studies indicated that caregivers encounter numerous health challenges due to their caregiving responsibilities and the unique needs of their loved ones who were receiving palliative care.29-32,35-36 Kenny et al. 29 observed that 35% of caregivers with loved ones receiving HBPalC reported declining overall well-being within a year. Specifically, caregivers attending to the needs of care recipients during nighttime faced an additional layer of burden and pressure due to disrupted sleep patterns. This nighttime caregiving often involved helping loved ones move, use the bathroom, or manage their pain and distress, which contributed to physical exhaustion for caregivers. Challenges in caregivers’ sleep health were consistent with those of Hearson et al., 32 who found that 100% of caregivers suffered from moderate-to-severe sleep disturbances, averaging only 5.3 h of sleep per night. Furthermore, a significant portion (38.5%) of caregivers reported excessive daytime sleepiness led to fatigue, reduced cognitive function, and emotional distress.
Clemmer et al. 30 reported that family members experienced overwhelming stressors and strains, including witnessing the decline in their relative's health and managing household tasks. Interestingly, a study from Grove et al. 31 reported that male caregivers had lower mental health scores due to strain from having multiple roles as a man in the traditional expectation. Norinder et al. 34 found that 63% of caregivers expressed a need for assistance in managing their emotional distress, which was directly related to their loved one's health and future. Perpiñá et al. 35 found that 41.6% of caregivers experienced intense burden due to increased stress and strain from caregiving tasks such as providing emotional support, managing medical responsibilities, and coping with the recipient's health management. These findings were similar to those from Grov et al., 31 who reported that caregivers experienced higher levels of anxiety compared to age- and gender-adjusted norms, indicating significant emotional strain. Supaporn et al. 36 found that several caregivers experienced declining physical health while caring for their loved ones, leading to depressive symptoms and even suicidal thoughts.
The Strain of Multifaceted Obligations
Five out of 11 studies reported that the multifaceted obligations and responsibilities due to simultaneous caregiving, managing the household, and working had imposed a significant toll on caregivers.29,30,33-35 Kenny et al. 29 found that employed caregivers faced the challenge of balancing work with caregiving duties, leading to heightened levels of physical discomfort and emotional strain. Similarly, Clemmer et al. 30 observed that caregivers often had to prioritize their caregiving role over their professional responsibilities. In addition to tending to the care recipient, caregivers also found themselves shouldering additional household duties such as grocery shopping, cooking, and banking. Jo et al. 33 noted that caregivers expressed a lack of time to fulfill their daily activities due to the additional roles they had to assume alongside caregiving, which placed restrictions on their time for several duties. More than half of caregivers in the study of Norinder et al. 34 reported that they needed more assistance with daily tasks such as household chores and childcare while they were providing care to their loved ones at home. The article also discussed how caregivers felt exhausted from their various roles with limited support and opportunities to rest and recharge. In line with these findings, Perpiñá et al. 35 highlighted that the juggling act of caregiving and other life responsibilities had adverse effects on caregivers’ physical health, contributing to the onset of fatigue.
Insufficient Medical Support and Training for Caregivers
Dissatisfaction with the healthcare system and the failure to meet caregivers’ needs was a recurring theme in four studies.30,32-34 Clemmer et al. 30 highlighted the expectation for informal caregivers to provide palliative care even in the presence of nurses, with most care being shouldered by the family caregiver. In these cases, nurses were seen more as aides rather than the primary care providers, leaving the bulk of caregiving duties to the family members. These expectations placed an immense burden on caregivers, who often lacked the necessary skills or support to manage complex needs. Hearson et al. 32 reported that healthcare professionals often overlooked the needs of informal caregivers, despite palliative care's holistic approach. Caregivers frequently experienced sleep problems that received limited attention, as the focus was primarily on the patient's needs. Jo et al. 33 noted the lack of consistency in professional service providers, leading to communication gaps and disconnects in information dissemination when providers changed. Caregivers expressed their difficulties in having their needs heard and found healthcare providers unapproachable for inquiries. Additionally, Norinder et al. 34 highlighted the lack of clear information and transparency regarding the care recipient's disease progression and future expectations. A significant proportion (69%) of caregivers expressed the need for more information about their care recipient's disease and their caregiving needs.
Lack of Respite Care
The provision of HBPalC for patients placed significant emotional and physical demands on informal caregivers. Findings from five studies underscored the pressing need for respite services, which were reported to be lacking.30,32,34,36,37 Clemmer et al. 30 highlighted the unavailability of community resources for caregivers, pointing out that the offered programs often coincided with the working hours of professionals, rendering them inaccessible. Additionally, Hearson et al. 32 noted that caregivers expressed a lack of information regarding available respite services. Moreover, caregivers expressed apprehension about entrusting outside workers when seeking respite services. Norinder et al. 34 highlighted caregivers’ recognition of the importance of respite care in preserving their physical and emotional well-being, despite their disappointment with the limited availability of such services. Similarly, Supaporn et al. 36 acknowledged the necessity of respite care in supporting caregivers and alleviating the physical and emotional burden associated with caregiving responsibilities. Cai et al. 37 demonstrated that informal caregiving hours increased as the care recipient approached the end of their life. The physical and emotional strain of caregiving, combined with inadequate support, left caregivers vulnerable to burnout and health deterioration.
Financial Strain in Caregiving
Six studies highlighted financial struggles as a significant challenge in the context of caregiving.29,30,32,33,38,39 Kenny et al. 29 observed that caregivers with lower income encountered difficulties in social functioning due to the added emotional burden of financial stress. Clemmer et al. 30 documented that caregivers experienced a loss of income because of their care recipient's cancer diagnosis and the responsibilities that came with caregiving. Moreover, for some caregivers, taking time off work to attend respite programs was challenging due to resultant loss of income, and financial barriers also hindered the feasibility of considering nursing home placement. Hearson et al. 31 highlighted that maintaining employment kept the caregivers mentally active even though they were physically exhausted. Furthermore, Jo et al. 33 identified significant costs associated with equipment and medications, including out-of-pocket expenses for medical equipment and medications, which placed a considerable strain on caregivers’ household budgets and long-term savings. Guerriere et al. 38 reported that families who used personal support workers (PSWs) occasionally experienced an additional financial strain in addition to caregiving. Moreover, even with PSW care, caregivers continued to experience a high burden. Shanmugasundaram et al. 39 added that the significant cost of medical equipment like wheelchairs, hearing aids, and medicines was overwhelming for participants.
Discussion
In this comprehensive scoping review, studies examining the challenge of informal caregivers friends, family, neighbors or unpaid carers for older adults receiving HBPalC were reviewed and analyzed. While many articles have focused on informal caregivers, few have specifically explored the challenges or experiences of those caring for older adults who are receiving HBPalC. Notably, only two articles in this review have specifically addressed those caring for older adults in a HBPalC setting.30,36 Despite the limited number of targeted studies, the reviewed studies came from a wide range of countries from various continents offering insights into the barriers faced by informal caregivers. This highlights a need for structured respite and nighttime support services as previously mentioned by Norinder et al., 34 Supaporn et al., 36 and Cai et al., 37 to preserve the caregivers’ overall well-being and functionality. The review also uncovered gender-based differences in caregiving dynamics, revealing how traditional gender roles influence the expectations and experiences of caregivers. Women often took the responsibility of caregiving duties, attributable to a feeling, a sense of obligation to care and being referred to as the “nurturing” ones.30,37 In contrast, male caregivers were reported to have lower mental health scores, likely due to the added strain of taking on roles typically outside their traditional expectations. 31 These findings emphasize the need for separate caregiving models which account for the different gendered expectations.
Expenses associated with medical supplies and the inability to hire care services create an additional layer of stress, on top of the caregiving responsibilities for the caregivers. 33 In contrast, caregivers within the healthcare systems like the Swedish healthcare model, reported less stress and higher quality of life due to their robust support. 34 Moreover, caregivers may not be fully aware of existing support programs which could assist in decreasing the financial burden, such as the National Family Caregiver Support Program (NFCSP) in the United States and Compassionate Care benefits in Canada. The NFCSP program primarily provides state funding to support families and informal caregivers of older adults, 40 while Compassionate Care benefits provide financial assistance while caregivers are away from work to care for or support a loved one who is critically ill and/or needing end-of-life care. 41 Both programs have been proven to help individuals from low socio-economic status.42,43 Therefore, it is essential that social workers and healthcare professionals remain aware of current policies and programs that may benefit caregivers.
An important insight from the review was caregivers’ recognition of their limitations in providing care due to lack of training and resources. Several caregivers expressed anxiety and a sense of inadequacy, worrying about their ability to meet the needs of their loved ones.36,39 This finding emphasizes caregiver training programs or support services which could enhance their confidence and competence thus reducing their anxiety and improving their preparedness for end-of-life care. Moreover, this finding points to the necessity of enhancing communication and decision-making support within palliative care settings, as caregivers often felt unsure to make critical care decisions. 36 Thus, it is essential to understand and know the caregivers’ experiences in caregiving as this could inform interventions and raise awareness of providing resources at various stages of caregiving. 44
Strengths and Limitations
It is essential to note that like any other review, this study has strengths/limitations. We believe that our research team members were able to bring various practice experiences and interdisciplinary perspectives into our analysis to address some common limitations with scoping reviews (eg, data interpretation). Therefore, our study offers useful knowledge about the challenges of informal caregivers of older adults in HBPalC, highlighting the need for tailored interventions and services that provide effective support to informal caregivers, especially in the face of the looming increasing aging population. Despite our best efforts to conduct a comprehensive review, some limitations remain. While 11 studies included informal caregivers of older adults in HBPalC settings with various medical conditions, most of the studies focused on caregivers of cancer patients, which contribute to a lack of diversity across study participants. A further limitation is the lack of diversity across national healthcare systems. Of the 11, 10 studies included in this scoping review were from developed countries, which tends to have a more equitable healthcare system than many other countries. 45 This could be because HBPalC has yet to be integrated and formally introduced in the health settings, resulting in a relatively narrow current evidence base. Additionally, since the objective was not to analzse the methodological quality of the included studies, we did not conduct a quality assessment of the studies included in the final review. However, this paper did adhere to formal guidelines for conducting a scoping review. Lastly, the search was limited to English-language articles, and gray literature was not included which could have restricted the scope of the review.
Policy/Practice Implications and Future Directions
While the burdens of caregiving for older adults with other chronic conditions are well-known, adequate support systems for caregivers involved in HBPalC have not been effectively established. Our findings have highlighted the need for enhanced support systems, comprehensive training programs, financial assistance, respite care, and improved collaboration with healthcare professionals tailored specifically for patients and families in HBPalC settings. Services such as respite care, day programs, and home care, must be well implemented in place and must be widely spread across. These programs often tend to be a pilot run which is short-term and do not adequately support long-term caregivers. There is a need to recognize and support a wide array of informal caregivers to make more accessible resources and the existing benefits more customized to the unique needs of the informal caregivers of HBPalC patients.
Future research should aim to gather additional information to better inform policy implementation to provide more funding to strengthen the informal caregivers. This review provides a comprehensive overview, intended to stimulate future studies and policy advancements for palliative caregivers. While the studies contain herein show the valuable efforts of these caregivers, further research is critical to clarify its effectiveness and how practice and policy can best support these vulnerable populations.
Conclusion
This scoping review focuses specifically on HBPalC which enabled the synthesis of challenges faced by informal caregivers across multiple studies, providing a clearer understanding of the extent to which this population is affected. Very few or none of the caregivers in the included studies had any formal involvement or training on caregiving which might be one of the reasons behind the underrepresentation of caregiver concerns or needs. This might contribute to instances wherein the caregivers are unaware of their struggles and thus cannot identify a specific need. This is a gap in the literature which could be used for future studies. The incorporation of a palliative navigator or better at-home palliative care training for the informal caregivers can prepare them for their caregiver journey. 46 Various government reports, editorials and publications have acknowledged the urgent need for caregiver support programs and needs.47,48 As the world population ages, and more older adults require palliative care, the burden on caregivers will substantially increase. Thus, it is worth considering the formal recognition of family caregivers within the healthcare system.
Supplemental Material
sj-docx-1-pal-10.1177_08258597251348262 - Supplemental material for Invisible Pillars With Hidden Burdens: A Scoping Review on the Challenges of Informal Caregivers for Older Adults in Home-Based Palliative Care
Supplemental material, sj-docx-1-pal-10.1177_08258597251348262 for Invisible Pillars With Hidden Burdens: A Scoping Review on the Challenges of Informal Caregivers for Older Adults in Home-Based Palliative Care by Swasati Handique, Soeun Jang, Michael Bennett and Scott D. Ryan in Journal of Palliative Care
Footnotes
Acknowledgments
The authors would like to thank Hailey Carson, Research librarian, at the University of Texas at Arlington, for helping to create search strings used in this review.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable, because this article does not contain any studies with human or animal subjects
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
