Abstract
Given the high prevalence of chronic conditions and multimorbidity in older adults, there is a need to better conceptualize and measure self-care and self-management to promote a person-centered approach. This scoping review aimed to identify and map instruments measuring self-care and self-management of chronic conditions by older adults. We searched six electronic databases, charted data from the studies and tools and reported the results in accordance with the PRISMA-ScR guidelines. A total of 107 articles (103 studies) containing 40 tools were included in the review. There was substantial variation in the tools in terms of their aims and scope, structure, theoretical foundations, how they were developed, and the settings in which they have been used. The quantity of tools demonstrates the importance of assessing self-care and self-management. Consideration of the purpose, scope, and theoretical foundation should guide decisions about tools suitable for use in research and clinical practice.
• This review provides an overview of existing tools used to measure self-care and self-management of chronic conditions by community-dwelling older people and describes their theoretical and practical characteristics. • This review identified a large number of tools, reinforcing the importance of measuring self-care and self-management as a core outcome measure within research and healthcare settings.
• This review identifies disease-specific and non-disease-specific tools that measure self-care and self-management and describes characteristics that might make them suitable for use in older adults with chronic conditions and multimorbidity. • Certain characteristics of existing tools (e.g., length, scope, and dimensionality) can inform the choice of use in specific research and healthcare settings. • Tools capable of differentiating and quantifying the different dimensions of self-care and self-management can support person-centered assessment and management through the delivery of tailored interventions.What this paper adds
Applications of study findings
Introduction
By 2030, the number of people aged 60 and over is projected to reach 1.4 billion, and by 2050, this figure is expected to rise to 2.1 billion (World Health Organization [WHO], 2022a). The rapid aging of the population has raised serious public health concerns related to the increasing prevalence of chronic conditions and multimorbidity (the co-occurrence of at least two chronic conditions). Multimorbidity in older adults is complex due to the potential overlap of physical and mental health conditions, polypharmacy, and frailty (Yarnall et al., 2017). Studies have estimated that between 55% and 98% of older adults have multimorbidity (Marengoni et al., 2011), and a recent meta-analysis found that 72% of those with frailty also have multimorbidity (Vetrano et al., 2019). Older people are therefore more likely to live with multiple chronic conditions associated with lower quality of life, reduced functional ability, increased healthcare utilization, and higher mortality (National Institute for Health and Care Excellence [NICE], 2016; Palladino et al., 2016; Ryan et al., 2015; Vogeli et al., 2007). Furthermore, fragmented or conflicting care can result in a higher treatment burden (Mair & May, 2014). As mortality rates decline and the population continues to age, managing chronic conditions and multimorbidity will become increasingly challenging for health systems (Fabbri et al., 2015; Kingston et al., 2018). Current models of care for older people have been criticized for not being sufficiently proactive and responsive to individuals’ diverse needs, priorities, and environments (Cesari et al., 2022; Tinetti & Fried, 2004). In addition to strengthening healthcare system factors, principles of person-centered care and “minimally disruptive medicine” are increasingly seen as critical to improving care for older adults with chronic conditions and multimorbidity (American Geriatrics Society Expert Panel on Patient-Centered Care, 2016; May et al., 2009; Muth et al., 2014; Wallace et al., 2015).
Interventions to manage chronic conditions and multimorbidity should be tailored to address known issues, such as lack of care coordination, duplication, disease and treatment burden, and significant polypharmacy (i.e., taking 10 or more medications regularly) (Skou et al., 2022). Furthermore, these interventions should consider the goals and priorities of the person receiving care, involve informal caregivers, deliver care with a focus on interprofessional expertise and collaboration, and support self-care and self-management (Dineen-Griffin et al., 2019). Self-care and self-management support interventions are widely used in many single-disease programs and have the potential to improve outcomes for older people with chronic conditions and multimorbidity in primary care and community settings (Skou et al., 2022). However, the evidence to support their effectiveness is still limited (Smith et al., 2021).
Defining and Measuring Self-Care and Self-Management
Self-care and self-management are critical for people with chronic conditions. It is estimated that more than 99% of the daily care for chronic conditions is performed by individuals and family carers (Riegel et al., 2017). Although both terms are widely used, they are associated with various conceptualizations and definitions, contributing to a lack of clarity and consensus (Barlow et al., 2002; Grady & Gough, 2014; Matarese et al., 2018; Richard & Shea, 2011; Van de Velde et al., 2019). Despite the lack of consensus, self-management is generally understood as a component of self-care occurring in the context of a recognized health condition with a degree of healthcare provider input (Matarese et al., 2018). Specifically, self-management is defined as “the intrinsically controlled ability of an active, responsible, informed, and autonomous individual to live with the medical, role, and emotional consequences of [their] chronic condition(s) in partnership with [their] social network and healthcare provider(s)” (Van de Velde et al., 2019, p. 10). Self-care is a broader concept that refers to “the ability of individuals, families, and communities to promote health, prevent disease, maintain health, and cope with or without the support of a healthcare provider” (WHO, 2022b). Self-care, according to the Middle-Range Theory of Self-Care of Chronic Illness (Riegel et al., 2012), consists of three dimensions: treatment adherence and health-promoting practices (self-care maintenance); behavior and condition monitoring (self-care monitoring); and managing signs and symptoms when they occur (self-care management). Commonly used models include the Chronic Disease Self-Management Program (Lorig et al., 1999), the Chronic Care Model (Wagner et al., 1996), and the Flinders Chronic Condition Management Program (Battersby et al., 2007). These models endorse the notion of commonality among chronic conditions and are intended for use with diverse conditions and populations.
Qualitative research and several systematic reviews have found that self-care and self-management consist of various aspects or domains, including the different skills, attitudes, and abilities that people use to address the challenges of living with chronic conditions (Audulv et al., 2012; Boehmer et al., 2016; Liddy et al., 2014; Schulman-Green et al., 2016; Van de Velde et al., 2019). However, scholarly literature that addresses the conceptual dimensions of self-care and self-management in older adults is relatively limited. The following characteristics have been identified as defining attributes of self-care and self-management of chronic conditions and multimorbidity among older people: using financial resources to manage chronic conditions; acquiring health-related education; making use of social supports; responding positively to health changes; continuing engagement with the health system; and active participation in chronic condition management (Garnett et al., 2018). Additionally, (Lawless et al., 2021) identified seven core theoretical constructs that are essential for older adults’ self-care and self-management: temporal and spatial context; stressors; personal resources; informal social resources; formal social resources; behavioral adaptations; and quality of life outcomes. Assessing the various domains of self-care and self-management can help individuals, carers, and healthcare providers identify the specific challenges experienced by older people with chronic conditions and multimorbidity so that appropriate resources, programs, and supports can be accessed, delivered, and evaluated effectively.
Developing and implementing appropriate tools to assess self-care and self-management can inform care delivery and is necessary to demonstrate the effectiveness of programs, policies, and interventions (Nichols et al., 2020). Instruments that accurately measure self-care and self-management can allow assessment of individuals’ capacity to care for themselves so that the right level of support can be provided at the right time across healthcare and community settings (Coulter et al., 2015). Developing and implementing measurement tools should occur alongside coordinated efforts to redesign the structure and financing of long-term services and supports to provide comprehensive care for older people (Fulmer et al., 2021). Although several tools have been developed to measure self-care and self-management of chronic conditions in the general adult population (e.g., Jaarsma et al., 2003; Riegel et al., 2009; Toobert et al., 2000), there is a paucity of evidence on the characteristics and validity of tools used in older adults with chronic conditions and multimorbidity. It is unclear whether existing instruments measuring self-care and self-management validated in older adults with chronic conditions are structurally and conceptually similar or different. The number of disease-specific (i.e., intended for use based on a named disease) and non-disease-specific (i.e., intended for use across diagnoses) instruments can present challenges when selecting an appropriate instrument. Furthermore, there appears to be variation in their intended purpose, structure, theoretical foundations, how they have been developed, and the settings in which they have been used.
Previous reviews have examined disease-specific and non-disease-specific instruments measuring self-care or self-management (Ausili et al., 2014; Cameron et al., 2009; Caro-Bautista et al., 2013; Han et al., 2014; Hudon et al., 2021; Lu et al., 2015; Matarese et al., 2017; Packer et al., 2018; Sidani, 2011). These reviews provided insight into disease-specific and non-disease-specific instruments for measuring self-care and self-management in adult (≥18 years) populations. However, they were not specific to older adults with chronic conditions or multimorbidity, who often experience greater healthcare utilization, higher treatment burden, and geriatric syndromes such as frailty. To our knowledge, there have been no previous reviews of instruments measuring self-care and self-management by older adults living with chronic conditions. Hence, the aim of this scoping review was to identify the range of tools measuring self-care and self-management of chronic conditions by community-dwelling older adults (≥60 years).
Methods
Design
We conducted a scoping review following the methodological framework developed by Arksey and O'Malley (2005) and advanced by others (Daudt et al., 2013; Levac et al., 2010). The review consisted of five steps: (1) identifying the research question; (2) identifying relevant studies; (3) selecting studies based on pre-defined criteria; (4) charting the data; and (5) collating, summarizing, and reporting the results. A sixth step, consultation, is considered optional when the research team is multidisciplinary. Our research team includes a range of backgrounds (cancer, cardiovascular and older peoples’ nursing, psychology, and sociology) with expertise in self-care and self-management theory, fundamental nursing care, integrated care models, survivorship, and implementation science. Scoping reviews are conducted to examine the type and range of evidence available on topic, clarify key concepts and definitions, and identify knowledge gaps in the literature to inform future research (Munn et al., 2018). A scoping review was chosen due to the large number and variability of tools in the literature. We used the Preferred Reporting Items for Systematic Reviews and Meta-analyses for Scoping Reviews (PRISMA-ScR) (Tricco et al., 2018) to guide reporting and enhance fidelity. We registered an a priori protocol with the Open Science Framework (Lawless, 2022).
Identifying the Research Question
The objective of this scoping review was to identify and describe the range of tools available to measure self-care and self-management of chronic conditions by older adults (see Supplementary File 1 for definitions of key terms). The specific review question was “what tools are available to measure self-care and self-management of chronic conditions by community-dwelling older adults?” We identified two specific objectives: 1. To identify tools that measure self-care and self-management by people (aged ≥60 years) that can be used for assessment and evaluation in clinical practice and research. 2. To map the characteristics, including their aims and scope, structure, theoretical foundations, how they have been developed, and the settings in which they have been used.
Identifying Relevant Studies
The search aimed to locate peer-reviewed studies published between January 2002 and March 2022. This date range was chosen to ensure relevance to current self-care and self-management interventions and theory. We developed the search strategy based on recommendations for conducting scoping reviews, previous examples from the literature, and the advice of a university librarian. We searched six electronic databases: CINAHL, Scopus, ERIC, PsycINFO, MEDLINE/PubMed, ProQuest. We chose these databases for their breadth and diversity of disciplines represented. We used a combination of Medical Subject Heading (MESH) terms and keyword searches were to identify publications meeting the inclusion criteria. The search strategy used for MEDLINE/PubMed is available in Supplementary File 2.
Selecting Studies
The inclusion criteria are shown in Supplementary File 3. We included studies reporting on the development, validation, or testing of tools measuring self-care or self-management in adults aged ≥60 years. This age was chosen based on the United Nations (2019) and the WHO (2022a) definition of older people as individuals aged over 60 years. Only studies with a specified theoretical foundation were included in this review based on the expectation that complex population health interventions require robust and explicit theorization for successful implementation and to function as expected in terms of change mechanisms (Hastings et al., 2020; Moore et al., 2021). Articles reporting on older adults with chronic conditions that did not specify a theoretical underpinning were excluded. Included chronic conditions were identified from a list of prevalent conditions published by the Office of the Assistant Secretary for Health (OASH) in the United States Department of Health and Human Services (Goodman et al., 2013). From this list, we selected 10 prevalent chronic conditions associated with significant morbidity and mortality in older people worldwide: coronary artery disease, hypertension, heart failure, stroke, arthritis, asthma, cancer, chronic kidney disease (CKD), chronic obstructive pulmonary disease (COPD), and type 2 diabetes. These conditions were among 20 chronic conditions selected by OASH for a standard classification scheme (Goodman et al., 2013). They are prevalent among older people across low-, middle-, and high-income countries (Ofori-Asenso et al., 2019; Vancampfort et al., 2017) and are frequently investigated in research on self-care and self-management interventions for adult patients (Riegel et al., 2021). From this list, we excluded studies that focused exclusively on severe mental illness or advanced dementia as these individuals often have limited capacity to participate actively in self-care or self-management in a manner consistent with current definitions. Articles reporting on instruments developed for use with older adults (≥60 years) without the identified chronic conditions were excluded. We excluded studies that reported exclusively on inpatient, hospital, residential aged care, or palliative care settings. No limitation was placed on the upper age, gender, ethnicity, or geographical location of participants.
Following the search, all retrieved references were imported into Endnote (Clarivate Analytics, PA, USA) and Covidence systematic review platform (Veritas Health Innovation, Melbourne, Australia) and duplicates were removed. Prior to title and abstract screening, the first four authors discussed a representative sample of studies to ensure consistency among their interpretation of the eligibility criteria. The full texts were assessed by two reviewers against the inclusion criteria using a standardized screening form. Studies that appeared to meet the inclusion criteria were retrieved in full text and a second meeting was held to verify a random selection of each reviewer’s studies and to discuss any studies about which a reviewer was unsure, after which a group decision was made to exclude or include. Finally, we searched the reference list of each included article to identify additional studies. Consistent with scoping review methodology, critical appraisal of the studies was not undertaken (Levac et al., 2010).
Charting the Data
Two reviewers independently conducted data extraction in Covidence and compared the completed tool to maintain consistency during the extraction process. We used a standardized data extraction tool (Supplementary File 4) to extract information about the study, including the setting, chronic conditions under study, and the tool used. Data extracted in relation to the tool included its aims and scope, definitions of self-care and self-management, theoretical foundation, method of development, structure, and contexts of use. Disagreements or inconsistencies were resolved through group discussion.
Collating, Summarizing, and Reporting the Results
The extracted data were mapped and summarized using a narrative descriptive approach to expose commonality and heterogeneity among the studies (Barnett-Page & Thomas, 2009). Results are reported following the PRISMA-ScR guidelines (Tricco et al., 2018). The PRISMA-ScR checklist is available in Supplementary File 5.
Results
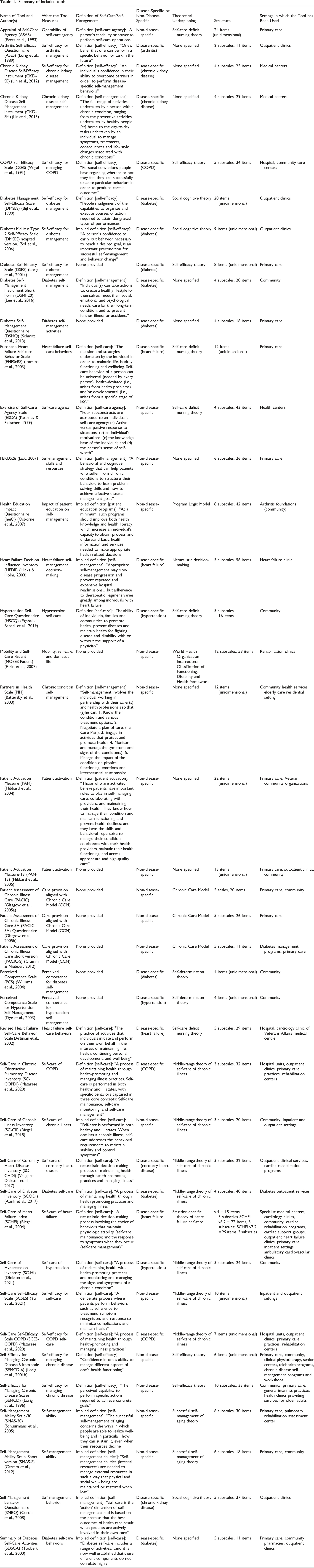
Database searching identified 1891 articles and searching the reference lists of included studies identified an additional 19 articles. After duplicates were removed and screening of titles and abstracts, 628 articles were assessed for eligibility and 540 were excluded based on the inclusion criteria. A total of 107 articles from 103 studies were included in the final review (Figure 1). In total, 40 measurement instruments were included in the review (Table 1). Of the 40 tools, 23 (57.5%) were disease-specific. The most common conditions were type 2 diabetes (20.0%, n = 8), heart failure (7.5%, n = 3), hypertension (7.5%, n = 3), COPD (7.5%, n = 3), and CKD (7.5%, n = 3). Seventeen tools (42.5%) were non-disease-specific, meaning that they were developed to be applicable irrespective of diagnosis. Eleven tools (27.5%) were used to measure self-care or self-management in people with multimorbidity (i.e., ≥2 chronic conditions). Supplemental Table 1 provides a summary of the included studies. Prisma flow chart. Summary of included tools.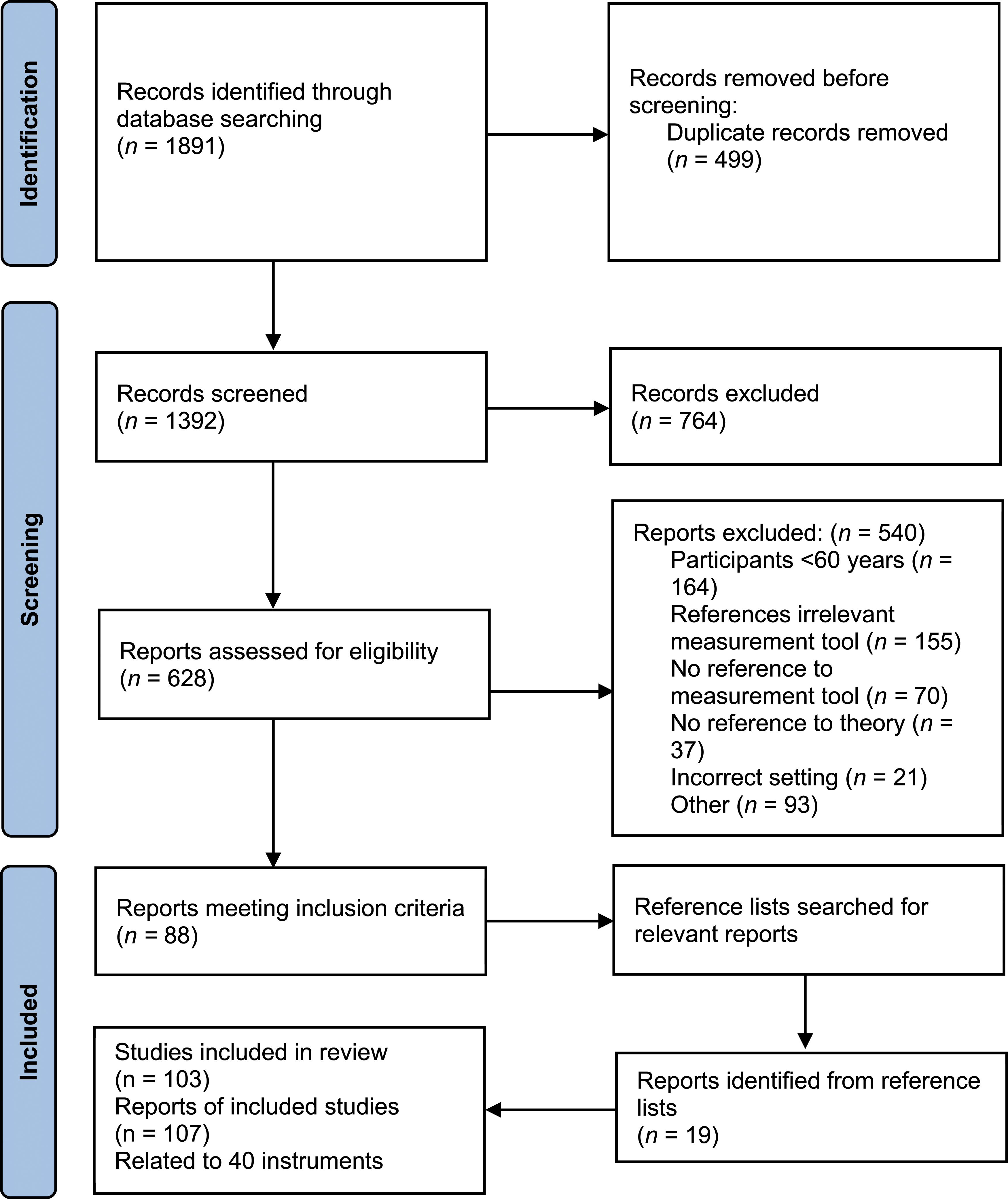
Frequency of Use of Each Tool
The Self-Care of Heart Failure Index (SCHFI) was the most frequently used tool among the included studies (15.0% n = 16), followed by the Self-Efficacy to Manage Chronic Disease 6-item scale (SEMCD-6) (13.1%, n = 14), the Patient Assessment of Chronic Illness Care (PACIC) (10.3%, n = 11), the Self-Efficacy to Manage Chronic Disease scales (SEMCD) (9.3%, n = 10), and the Summary of Diabetes Self-Care Activities (SDSCA) (7.5%, n = 8). Twenty-two (55.0%) of the 40 tools were used in only one study.
Aims and Scope of Included Tools
The aims and scope of the included tools (i.e., what the tool is intended to measure) is reported in Table 1. Thirteen of the 40 tools (32.5%) measured self-care or elements of self-care, such as self-care agency (e.g., Exercise of Self-Care Agency scale [ESCA]) and self-care behaviors (e.g., European Heart Failure Self-Care Behavior Scale [EHFScBS]). Eleven tools (27.5%) measured self-management or elements of self-management, including self-management skills and resources (e.g., FERUS26), and perceived competence for self-management (e.g., Perceived Competence Scale [PCS]). Ten tools (25.0%) measured self-efficacy related to chronic disease self-care or self-management, such as the Self-Care Self-Efficacy Scale (SCSES). The remainder of the tools measured patient activation (e.g., Patient Activation Measure-13 [PAM-13]) and care provision aligned with the Chronic Care Model (e.g., PACIC). Only three tools (7.5%) (ASAS, SMAS-30, SMAS-S) were developed to measure self-care or self-management in older adults.
Twenty-three tools (57.5%) included a clearly labeled definition of self-care, self-management, or related concepts such as self-efficacy, which provided insight into the intended focus of the tool (Table 1). Eight tools (20%) alluded to definitions or used vague language without clearly identifying the construct being measured (implied definitions). Nine tools (22.5%) did not provide a definition. Definitions ranged from specific and disease-focused (e.g., “self-monitoring of blood glucose, eating a low-saturated-fat diet, and checking one’s feet”; SDSCA) to broader definitions (e.g., “a person’s capability or power to perform self-care operations”; ASAS). Definitions provided by developers of 17 tools (42.5%) focused on behavioral/medical strategies, including actions undertaken to maintain a healthy lifestyle (with and without a chronic condition) and manage medical aspects of chronic conditions (e.g., monitoring/managing symptoms, treatment adherence). In comparison, those used by authors of 15 tools (37.5%) focused on cognitive/decision-making strategies, including the intellectual processes used for decision-making or to develop self-care and self-management skills. Definitions provided by the developers of the Partners in Health Scale (PIH) and the Health Education Impact Questionnaire (heiQ) focused on resource utilization and health navigation.
We originally intended to map and synthesize the items in the scales and subscales of the tools to assess their scope and breadth, as well as the extent to which each tool measures discrete or overlapping concepts. However, this proved problematic because of the variability in how the tools described and operationalized self-care and self-management. For example, some items measured individual knowledge, skills, and attitudes related to maintaining health and managing chronic conditions, such as “How confident are you that you can keep the fatigue caused by your disease from interfering with the things you want to do?” (SEMCD-6). Other items measured behaviors performed by the person who is ill to maintain health, limit the risk of illness, and control chronic disease, such as “How often do you monitor for medication side-effects?” (Self-Care of Chronic Illness Inventory [SC-CII]) and “I weigh myself every day” (EHFScBS). In several instances, studies did not report the label of subscales or describe the scale in sufficient detail to allow a synthesis.
Methods of Tool Development
Items included in the tools were developed based on a review of the academic literature, clinical guidelines, theoretical constructs, or existing validated instruments (n = 18), qualitative methods, such as focus groups and interviews (n = 7), and assessment of content validity by an expert panel (n = 17). Items in four tools were adapted from previous tools or subscales embedded within previous tools. The method of development was not reported for eight tools. Items in less than half of the tools (n = 19) were developed by researchers in combination with clinicians or other experts, such as specialist physicians (n = 8), nurses (n = 8), case managers or service coordinators (n = 3), diabetes educators (n = 3), and physiotherapists (n = 2). Five tools had some level of patient/consumer involvement in item development or refinement, such as assessing items for relevance, comprehensibility, and comprehensiveness (e.g., SC-COPDI).
Theoretical Foundation
Theoretical foundation was defined as any reference to, or application of, a model, theory, or framework to inform or underpin the development of the measurement tool. Most of the tools (75.0%, n = 30) were based on a named theory, model, or framework, as stated by the original authors of the tool. The most common theories, models, and frameworks underpinning the tools were the Middle-range Theory of Self-Care of Chronic Illness (17.5%, n = 7), Self-Efficacy Theory/Social Cognitive Theory (17.5%, n = 7), Self-Care Deficit Nursing Theory (12.5%, n = 5), and the Chronic Care Model (7.5%, n = 3). 10 tools did not explicitly specify a theory, model, or conceptual framework.
Contexts of Use
The 103 studies included data collected from the USA (n = 36), Italy (n = 10), Australia (n = 10), Canada (n = 9), Germany (n = 9), the Netherlands (n = 8), China (n = 7), and the UK (n = 6). Countries with five or less studies included Switzerland (n = 3), Iran (n = 2), South Korea (n = 2), Brazil (n = 2), Mexico (n = 2), Finland (n = 1), France (n = 1), Singapore (n = 1), Spain (n = 1), and Thailand (n = 1). Two studies included data obtained from more than one country. Of the 40 tools, 12 (30.0%) were used in more than one country. Of the 40 tools, most were used in outpatient clinics (n = 20), community (n = 17), primary care (n = 17), rehabilitation (n = 6), and hospital or inpatient settings (n = 6). Eighteen tools were used in more than one setting.
Structure of the Tools
The length of the tools ranged from four items (PCS) to 58 items (MOSES-Patient). The number of subscales or domains in each tool ranged from one to 12. Thirteen tools (32.5%) were unidimensional, meaning that they measured a single underlying construct or dimension (e.g., self-efficacy). Many of the tools had multiple variations or iterations. A “variation” was defined as a revision or modification to the structure or administration of a tool such that the number of items (i.e., number of items administered), language, scales/subscales, or scoring modality differed from the published version. Short forms of existing tools reported in a peer-reviewed publication were considered a separate tool rather than a variation. In addition, minor changes in wording, such as to reflect an accompanying person (e.g., family member) completing the tool, or the administration of an individual subscale from a tool, were not considered indicative of variation. Of the 40 tools, six had more than one variation.
Discussion
Our review identified 40 tools and found that most were developed to measure a specific construct or assess self-care or self-management of a specific condition. Only three tools were developed specifically for adults aged over 60 years with chronic conditions. Although several tools have been validated in samples of older adults, based on this review, none of the identified tools can be fully recommend for use to measure self-care or self-management among older people with chronic conditions and multimorbidity. Like earlier reviews (e.g., Hudon et al., 2021; Packer et al., 2018), we found considerable variation in the definitions of self-care and self-management used, reflecting ongoing conceptual inconsistency and fragmentation within the literature. Although many authors stated that their tool measured self-care or self-management, closer inspection revealed that many tools measured related constructs such as self-efficacy or patient activation, replicating previous studies. This lack of conceptual precision raises questions about whether tools claiming to measure self-care and self-management are measuring consistently defined constructs. The different ways in which self-care and self-management are conceptualized and operationalized might partly explain the mixed evidence of effectiveness of interventions in chronic illness (Lee et al., 2022). The terms self-care and self-management continue to be used interchangeably, despite efforts over the last decade to delineate the concepts (Grady & Gough, 2014; Matarese et al., 2018; Richard & Shea, 2011; Van de Velde et al., 2019). Instruments developed for specific conditions often use the terminology that is standard within that scientific community. This reflects the reality of clinical practice, which is often compartmentalized into silos. For example, self-management is predominantly used in diabetes, COPD, coronary artery disease, arthritis, and asthma, whereas self-care is the term predominantly used in heart failure. Riegel et al. (2021) note that the inconsistency might be traced to early adoption of the self-management theories of Bandura (1997) and Lorig et al. (1999) versus early adoption of the self-care theory of Orem (1985). Many authors have since written about the similarities and differences between concepts (e.g., Matarese et al., 2018). Reaching agreement on the meaning and use of the terms may contribute to bridging disciplinary silos currently precluding effective knowledge exchange (Jaarsma et al., 2020).
Although an increasing proportion of older patients experience multimorbidity and complex needs, we found that disease-specific instruments were more common than non-disease-specific instruments, a finding reported in previous studies (Packer et al., 2018). Thirteen of the included tools were unidimensional, while the remainder mostly measured specific dimensions of self-care and self-management, such as symptom monitoring or treatment adherence. Several reviews demonstrate that self-care and self-management comprise multiple interacting domains, including the intrinsic and extrinsic resources that people use to address the daily challenges of living with chronic conditions (Audulv et al., 2012; Boehmer et al., 2016; Lawless et al., 2021; Van de Velde et al., 2019). Although unidimensional instruments might be beneficial due to their brevity and provide clinically useful information, they might have limited ability to identify specific care needs, as well as intrinsic and extrinsic resources, to guide care tailored to patients’ individual circumstances. Other instruments provide a single composite score despite analysis providing evidence of underlying multidimensionality. Whilst single-score instruments might be valid, reliable, and brief, they have limited utility in identifying individual patients’ self-care and self-management support requirements or in personalized care planning (Coulter et al., 2015; Packer et al., 2020). Instruments capable of assessing the various domains of self-care and self-management are needed to move beyond “one size fits all” approaches that are responsive to people’s diverse and changing needs. Research into the active ingredients of interventions and advancing a person-centered approach also depends on the ability to distinguish and measure separate domains of self-care and self-management.
Developing accurate and comprehensive measures to assess self-care and self-management by individuals and support across health services has the potential to promote integrated and personalized care and support for older people with multimorbidity (Keddy et al., 2021; Nichols et al., 2020; Shepherd et al., 2022; WHO, 2015). Personalized care planning, defined as a series of discussions between a patient and a health professional to clarify goals, options, and preferences and develop an agreed plan of action, embodies the core principles of person-centeredness and shared decision-making (Coulter et al., 2015). The aim of personalized care planning is to support individuals and carers to self-manage their health and wellbeing, typically using a combination of behavior change techniques (e.g., goal setting, action planning, health coaching, motivational interviewing) to achieve collaborative outcomes (Ahmed et al., 2021). Personalized care planning provides an opportunity to advance a proactive and person-centered approach that expands the traditional medical focus of care to a more comprehensive, socially oriented approach. Personalized care plans should contain various components including a package of multi-component interventions, management of underlying chronic diseases and geriatric syndromes, social care and support, and support for self-care and self-management. To deliver person-centered and feasible treatment programs, healthcare providers therefore need to appreciate the limits and possibilities of people’s capacity to enact self-care and self-management across different domains (e.g., physical, personal, emotional, social, financial, environmental) (Boehmer et al., 2018). Although self-care and self-management are components of personalized care planning, it remains unclear whether existing self-care and self-management tools are suitable as part of integrated person-centered assessment and pathways for older people.
Strengths and Limitations
This review used the rigorous methodology developed by Arksey and O'Malley (2005) and advanced by Levac et al. (2010). Searching of reference lists allowed us to identify additional articles and instruments. A limitation of this review was the difficulty in locating and classifying relevant instruments resulting from the lack of accepted conventions for naming tools and the various repositories for outcome measures. Some tools with unique names were found to be variations or duplicates of another tool with a different name, which had undergone revisions or modifications (e.g., to apply to a specific chronic condition). Moreover, as noted by Packer et al. (2018), unless a measure has been commercialized, often it is hard to determine whether versions modified for other languages or cultures exist, or which is the most recent version of the tool. These difficulties were mitigated by referring to the original articles describing the development and/or validation of the tool and cross-checking tables and independently completed data extraction forms. It is possible that some tools were not included in the review because we focused on studies reporting on older adults with prevalent chronic conditions and excluded studies that reported exclusively on asymptomatic, acute, and psychiatric diagnoses; we excluded studies that reported exclusively on inpatient, hospital, residential aged care, or palliative care settings; and we only included tools were items could be located and viewed. However, the large number of studies and tools identified through database searching allowed us to describe the extent and range of the existing literature. The variability of the items in the tools, as explained above, meant that we were unable to synthesize the items in a meaningful and precise way; this should be a key aim of future research.
Future Directions
Building on the current review, further research is needed to assess the content and quality of the identified instruments to clarify which measures are appropriate for the target population of older people with chronic conditions and multimorbidity. Like previous studies (e.g., Hudon et al., 2021; Packer et al., 2018), the definitions and theoretical foundations used to develop the instruments included in this review were varied, indicating that the concepts of self-care and self-management require further clarification and refinement. Although self-care and self-management can be defined in various ways across chronic conditions and cultural groups, the use of consistent and coherent definitions can provide a shared language for communication across services and enable more robust measurement. Clearer terminology may also facilitate the implementation of self-care and self-management support in person-centered, integrated care for older adults with chronic conditions and multimorbidity. A shift towards embedding self-care and self-management support across health services requires the development of comprehensive, validated measures to demonstrate the effectiveness of policies, programs, and interventions. However, many existing measures are not designed to evaluate the effectiveness of complex self-care and self-management interventions with multiple interacting components. Theory-based approaches, such as the Medical Research Council framework, provide comprehensive and systematic methods for developing and evaluating complex interventions (Moore et al., 2015; O’Cathain et al., 2019). In addition, complex systems thinking could be used to gain insight into the complexity of chronic disease self-care and self-management and identify promising leverage points for interventions (Baugh Littlejohns & Wilson, 2019). These methods could be combined with a partnership approach, in which end users participate actively throughout the development process to understand the perspectives and wider context of the potential target population, including healthcare providers, carers, and older people (Slattery et al., 2020). A co-design process could be used generate novel self-care and self-management instruments designed for application in healthcare settings that incorporate the perspectives and values of older people.
Practice Implications
This review contributes to decision-making in clinical practice in terms of selecting appropriate instruments to measure self-care and self-management among older adults with chronic conditions and multimorbidity. The characteristics of existing tools (e.g., length, scope, and dimensionality) might inform the selection of a specific tool for use in clinical care. Ideally, the tool should assess the person’s individual needs and circumstances, as well as their values and preferences, aligned with recommendations on supporting self-care and self-management. Using dedicated tools in clinical practice would potentially contribute to improved delivery of care tailored to the needs of the person. Although comprehensive, multidimensional tools can enable measurement of different aspects of self-care and self-management, they can increase the response burden, thereby making them unfeasible for use in routine clinical practice. Conversely, instruments containing fewer items would reduce the response time required to administer them in a clinical context. However, they might lack adequate specificity in pinpointing individual support needs, as well as guiding tailored interventions and appropriate referral pathways. For use in routine practice, instruments should aim for brevity and must be feasible to administer yet provide enough specific information to support individualized patient care. A brief screening instrument might prove more practical to implement within busy primary care settings to identify individuals with reduced capacity to self-manage who would benefit from accessing additional resources and supports. Screening is a common practice in a variety of medical settings, such as mental health screening (Lee et al., 2018) and social support screening (Schultz et al., 2022). Screening tools can also be used to identify risk factors such as frailty using simple measures such as assessment of gait speed, timed-up-and-go tests, or the PRISMA-7 questionnaire (Ambagtsheer et al., 2020; NICE, 2016). Health and social care workers could carry out screening of older adults’ capacity to self-manage their chronic condition(s) in primary care and community settings to inform an individualized approach to assessment and management. Ideally, a positive result would then be followed up by a longer, more comprehensive assessment in which the person’s capacities and care needs are assessed in greater depth and a personalized care plan is created. Such assessments might incorporate existing metrics related to disease-related factors (e.g., disease severity), socio-economic factors (e.g., social support), multimorbidity (e.g., cognition, co-morbid conditions), and environmental factors (e.g., access to care, built environment) (Jaarsma et al., 2020).
Conclusion
We conducted this review to map the range of tools that measure self-care and self-management of chronic conditions by community-dwelling older adults and describe their characteristics. Identifying instruments that are suitable for use in research and clinical practice can guide healthcare providers in their selection. Robust and rigorous assessment and monitoring would allow verification of the effectiveness of any efforts undertaken by healthcare providers to support self-care and self-management. They would also support the implementation of person-centered care by refocusing care and support planning on what matters to older people and their carers, identifying unmet needs and areas of strength, and tailoring support accordingly. However, the number of tools, including duplication and variability within literature, highlights gaps between policy discourse and the rigor with which self-care and self-management of chronic conditions are currently conceptualized and measured. The variability in the literature makes it difficult to determine the potential utility of existing tools for measuring self-care and self-management in older people with chronic conditions and multimorbidity. Selecting a tool for use in a specific context depends on the rigor of the tool, its feasibility (e.g., length), and the applicability of the tool to that context. Some tools identified in this review appear suitable for use with older people. However, further research is needed to assess the quality of existing tools to assist researchers, policymakers, and clinicians in assessing self-care and self-management to promote tailored care for older adults with complex care needs.
Supplemental Material
Supplemental Material - Instruments Measuring Self-Care and Self-Management of Chronic Conditions by Community-Dwelling Older Adults: A Scoping Review
Supplemental Material for Instruments Measuring Self-Care and Self-Management of Chronic Conditions by Community-Dwelling Older Adults: A Scoping Review by Michael T. Lawless, Matthew Tieu, Raymond J. Chan, Jeroen M. Hendriks, and Alison Kitson in Journal of Applied Gerontology
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: RC receives salary support from Australian National Health and Medical Research Council (APP1194051). JH is supported by a Future Leader Fellowship provided by the Australian Heart Foundation.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
