Abstract
Objective
Loneliness – distress that arises from discrepancies between perceived and desired relationships – is increasingly prevalent and recognized as a major public health concern due to the association with negative health outcomes. People living with schizophrenia (PLWS) experience higher rates of loneliness than the general population and may be particularly vulnerable to these adverse outcomes. In the general population, loneliness fluctuates throughout the lifespan, but the relationship between loneliness and age in PLWS is not well understood.
Method
271 adults, 141 adults with a diagnosis of schizophrenia or schizoaffective disorder (PLWS)and 130 adults with no history of major psychiatric illness (NCs) aged 27–69 completed clinical interviews and self-report measures assessing loneliness, perceived social support, and mental and physical health. Participants also completed blood draws for biomarkers of inflammation and hyperglycaemia. Locally Weighted Scatterplot Smoothing (LOWESS) regression modelling was used to examine potential non-linear relationships between loneliness and age for both groups and to select the polynomial that best fit the observed relationship.
Results
We observed an age by diagnostic group interaction (log estimate = −0.005, SE = 0.003) such that PLWS reported higher loneliness scores compared to NCs of similar age. Patterns of loneliness differed with age between diagnostic groups such that loneliness remained relatively stable and high for PLWS while for NCs loneliness increased from age 40 to age 60. In both groups, loneliness was associated with worse self-reported physical health, depression, and, among PLWS, positive symptoms.
Conclusion
Results suggest different patterns of loneliness across adulthood for PLWS and NC, reflecting the different social milestones for NCs during this age period that are not as commonly experienced by PLWS, such as marriage, empty nesting and retirement. Loneliness is linked with poor physical and mental health outcomes among PLWS and may be an important target for improving morbidity and mortality for PLWS.
Plain Language Summary Title
Loneliness and Aging in Schizophrenia
Loneliness, distress that arises from discrepancies between perceived and desired relationships, is increasingly prevalent and now recognized as a major public health concern for older adults due to its association with negative health consequences. This study examines the relationship of loneliness with age and health outcomes in people living with schizophrenia who are at particularly high risk for poor social functioning. We found differences in the relationships between loneliness and age in people with schizophrenia and non-psychiatric comparison participants, such that loneliness remained relatively stable and high for people with schizophrenia and increased from age 40-60 years for non-psychiatric groups. Loneliness was associated with worse self-reported physical health, depression, and positive symptoms.
Introduction
Schizophrenia is associated with significant disability, which contributes to poor social functioning and lower quality of life, as well as increased risk of loneliness.1–3 Loneliness is defined as subjective distress arising from a mismatch between desired and perceived social relationships. 4 People living with schizophrenia (PLWS) have higher rates of loneliness compared to the general population. 5 High levels of loneliness are associated with poor cognitive, mental and physical health, as well as increased mortality risk.6–8 PLWS may be particularly vulnerable to the adverse outcomes stemming from loneliness due to their existing comorbidities, 9 social structures 10 and social cognitive deficits. 1
In the general population, loneliness levels fluctuate across the lifespan.7,11–13 Overall, loneliness is typically high in young and late adulthood; one study reported that loneliness declines from a peak at age 20 and then increases again from age 70 onward. 14 Other studies have identified an additional peak in loneliness between ages 50 and 60, yielding a W-shaped curve of loneliness levels across the lifespan.7,12 This fluctuation has been attributed to changes in living situation and social networks that occur with life milestones and aging (e.g., loss of partners, changes in household, increased physical disability, decreased social integration).
Although loneliness appears to change throughout the lifespan in the general population, the relationship between loneliness and age in PLWS has not been well characterized. PLWS tend to have higher rates of loneliness than the general population that may be attributable to a number of social and economic factors. PLWS typically have relatively small social networks 14 and often do not experience the same milestones across the lifespan as adults in the general population such as romantic partnership 15 and employment. 16 Housing status may contribute to the relatively high levels of social isolation and loneliness, as there are differences in social networks for PLWS living in supportive housing compared to PLWS living independently and PLWS living with family. 10 PLWS often have social cognitive deficits that may impact their responses to social interactions.17–19 The impact of aging on loneliness among PLWS has not been previously examined.
Loneliness is associated with a host of negative physical and mental health consequences, 20 including higher risk for cardiovascular disease and metabolic disorders, and importantly, increased risk of early death. PLWS who are lonely also have increased risk of cardiometabolic disorder, premature mortality,21,22 more severe depressive symptoms and more frequent suicidal thoughts. 23 Understanding how loneliness may worsen health outcomes for older PLWS, a highly vulnerable group with high medical burden, may help to target specific PLWS for future interventions. Understanding how loneliness may worsen health outcomes for older PLWS, a highly vulnerable group with high medical burden, may help to target specific PLWS for future interventions.
While age-related changes in loneliness have been observed in the general population, the relationship between age and loneliness in PLWS is understudied and impacts the health of older adults. To address these gaps in the literature, the present study examines cross-sectional relationships between age and loneliness, compares loneliness levels between PLWS and non-psychiatric comparison (NC) groups, and assesses relationships between loneliness and key health outcomes in PLWS and NCs. First, we hypothesize that loneliness will have a non-linear relationship with age among PLWS. Second, we hypothesize that the severity of loneliness will be higher among PLWS compared to NCs. Finally, we will explore the relationships of loneliness with worse physical, mental and cognitive health outcomes.
Methods
Participants
The current study includes data from a longitudinal study of accelerated aging in schizophrenia that was approved by the UC San Diego Human Research Protections Program (IRB Protocol #101631). All study participants provided written informed consent to participate. The aims of the present study are novel from prior published works using this dataset. 24
English-speaking participants aged 26 to 65 with a diagnosis of schizophrenia or schizoaffective disorder (i.e., PLWS) or no history of major psychiatric illness (i.e., NCs) were recruited from the greater San Diego area. NCs were recruited via the ResearchMatch website, flyers, media in the community, advertisements in local media and word of mouth. To verify their diagnoses, PLWS were screened using the DSM-IV-TR Structured Clinical Interview (SCID-IV 25 ) administered by study staff who received hands-on and didactic training, with annual reviews to ensure high fidelity. All PLWS included in the study met criteria for a DSM-IV diagnoses of schizophrenia or schizoaffective disorder and were stable outpatients at the time of enrolment. The DSM-IV-TR SCID-IV was used as the DSM-5 had not been published at the start of the study. NCs were screened for psychiatric comorbidities with a combined diagnostic interview.25,26 Study exclusion criteria included other present DSM-IV-TR Axis I diagnoses; non-tobacco-related substance abuse or dependence within the last 3 months; diagnosis of intellectual disability, major neurological disorder, or dementia; and/or a medical disability that would impede the participant's ability to participate in the study. The study aimed to recruit a sample that was balanced by baseline age cohort in order to have equal numbers of participants at each baseline age binned by half-decade (e.g., 21–25, 26–30, etc.). Participants were enrolled consecutively until the bins were filled, resorting to oversampling until each bin was filled. All study procedures were conducted at either the participant's group home or at the clinical research offices. The final sample included participants ages 27 to 69.
Measures
Social support was assessed via the Perceived Support scale, derived from the MacArthur Studies of Successful Aging. 29 The scale consists of three subscales (emotional support, instrumental support, and negative social interactions) with items rated on a 4-point Likert scale ranging from “Never” to “Frequently,” and has a test-retest correlation of r = 0.83. For the current study, each subscale was treated as a separate variable. Higher scores on the emotional support, instrumental support and negative social interaction subscales indicate greater perceived emotional support, greater perceived instrumental support and more frequent negative social interactions respectively.
Positive and negative symptoms were assessed with the Scale for the Assessment of Positive Symptoms and Negative Symptoms (SAPS/SANS 33 ).
Statistical Analysis
Missingness was noted for specific covariates (1 missing value for marital status; 23 for emotional support, instrumental support and negative social interactions). Of the sample of 271 participants, we found 0.4% of participants had missing data on marital status and 8.5% had missing data on emotional support, instrumental support and negative social interactions. To reduce potential bias due to missingness under the missing at random mechanism (missingness of a covariate depends on the observed data of other covariates and predictors), we employed the predictive mean matching method with ten imputations for the missing data by the Multivariate Imputation by Chained Equations Chained Equations using the R “mice” package. 37
A third-degree polynomial regression was fitted for the loneliness and age relationship based on the LOWESS curve. The initial model included the following covariates: psychiatric diagnosis, marital status, living situation, marital status, personal income level, education, race/ethnicity, emotional support, negative social interactions and the interaction of age by psychiatric diagnosis (to examine the potential moderation effect by diagnostic group on the association of loneliness with age). Variable selection was performed using the backward elimination method with a threshold of a P-value >0.2 to trim the model. For final model selection, we compared the final models using QIC (quasi information criterion), a goodness of fit metric for semiparametric GEE akin to Bayesian information criterion for parametric models.39,40 We present the final models based on the best model fit.
Variance inflation factors (VIFs) were used to assess potential multicollinearity among the variables. VIF values were <2.5 for the UCLA loneliness scores and all explanatory variables for all three regression models, indicating that multicollinearity would not have a significant impact on model performance. We found higher VIFs for diagnostic group (binary indicator) and personal income (3-group categorical variable) (VIF = 1.91 for diagnostic group and VIF = 1.93 for personal income). A follow-up logistic regression model found that diagnostic group was a significant predictor of personal income (P < 0.001), so we removed personal income from the model and included only the diagnostic group indicator in our analyses.
General linear models were conducted to assess the association of loneliness with outcomes, while controlling for age, diagnostic group, race/ethnicity and sex due to their links with metabolic and physical health outcomes. We used false discovery rate (FDR) methods to correct for multiple comparisons. 41 Analyses were performed using the “geepack” and “mice” packages within R Statistical Software version 4.3.2.37,42 Significance was defined as α < 0.05 (two-tailed) for all analyses.
Results
The sample included 141 PLWS and 130 NCs with comparable age and sex distribution between diagnostic groups (Table 1). Participants in the PLWS group reported fewer years of education, had a higher proportion of non-white participants, and smoked more cigarettes per day than the NC group. The PLWS group also reported more severe depressive symptoms and performed worse on cognitive measures compared to the NC group. Regarding physical health, PLWS had worse physical-well-being scores, more physical comorbidities, higher BMI, and elevated hs-CRP levels compared to NCs. Overall, PLWS reported higher levels of loneliness, lower perceived emotional support and more negative social interactions than the NCs. The diagnostic groups did not differ in levels of instrumental support.
Sociodemographic and Clinical Factors Compared Between People Living with Schizophrenia (PLWS) and Non-Psychiatric Comparison Participants (NCs).
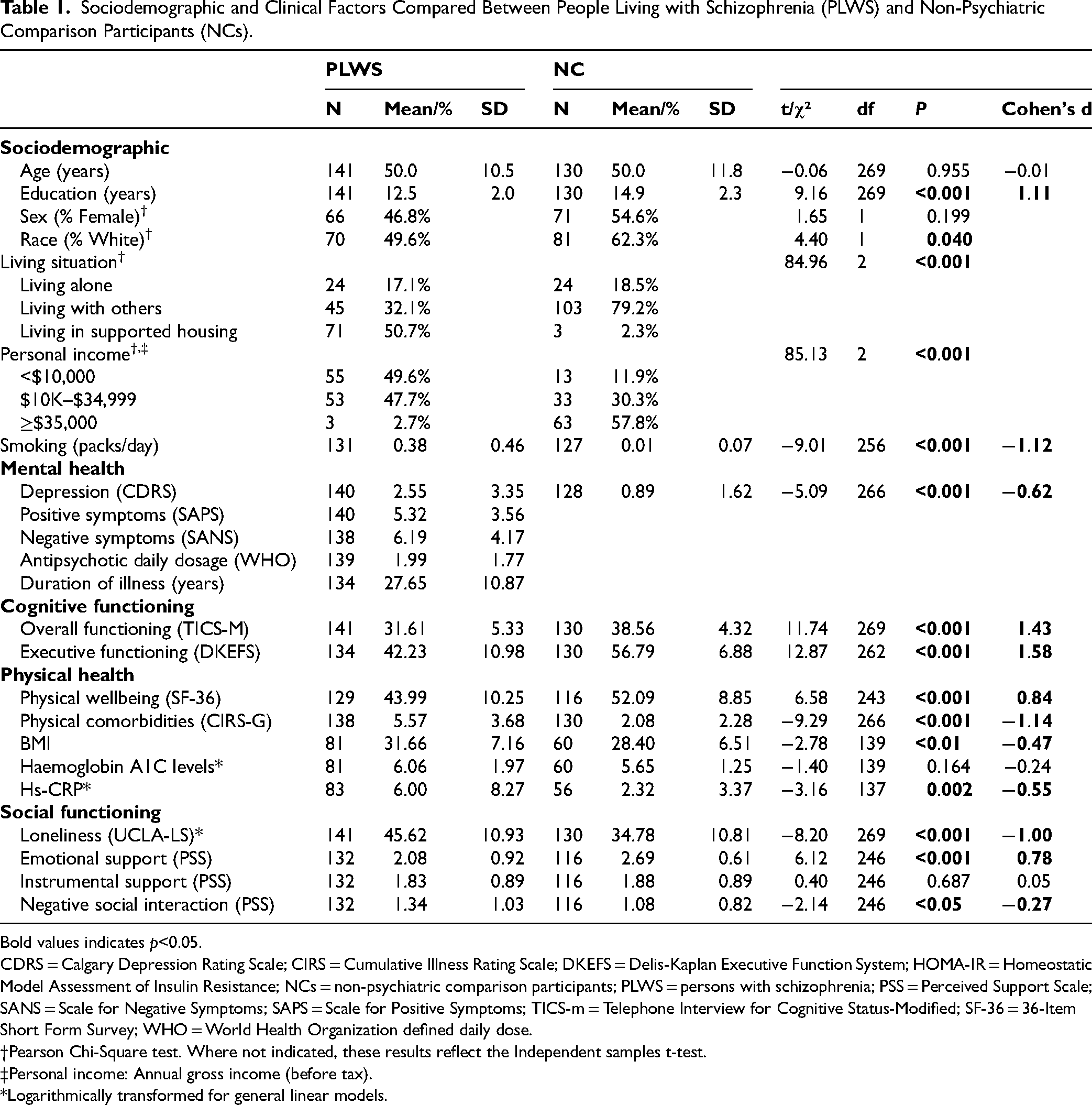
Bold values indicates p<0.05.
CDRS = Calgary Depression Rating Scale; CIRS = Cumulative Illness Rating Scale; DKEFS = Delis-Kaplan Executive Function System; HOMA-IR = Homeostatic Model Assessment of Insulin Resistance; NCs = non-psychiatric comparison participants; PLWS = persons with schizophrenia; PSS = Perceived Support Scale; SANS = Scale for Negative Symptoms; SAPS = Scale for Positive Symptoms; TICS-m = Telephone Interview for Cognitive Status-Modified; SF-36 = 36-Item Short Form Survey; WHO = World Health Organization defined daily dose.
Pearson Chi-Square test. Where not indicated, these results reflect the Independent samples t-test.
Personal income: Annual gross income (before tax).
*Logarithmically transformed for general linear models.
We examined the relationship of age with loneliness and found that the best-fit model included both first- and third-degree polynomial terms, with smaller (∼2%) QIC weights than the model with only linear terms (Table 2). The best-fit model was plotted over the LOWESS curve for loneliness and age by diagnostic group (Figure 1). There was a significant group by age interaction (log estimate: −0.005, SE = 0.003, P = 0.04)) such that PLWS reported higher loneliness scores compared to the NCs within the same age group. While loneliness severity appeared to stabilize between ages 40–60 among PLWS, loneliness severity appeared to increase among NCs. Over the age of 60, loneliness appears to have an inverse relationship with age in PLWS. In terms of social factors included in this model, higher loneliness was associated with lower levels of emotional support (B = −0.12, SE = 0.02, P < 0.001; Table 2). and a greater number of negative social interactions (B = 0.08, SE = 0.02, P < 0.001; Table 2). We did not observe a relationship between loneliness and relationship status (B = 0.06, SE = 0.04, P = 0.11; Table 2).
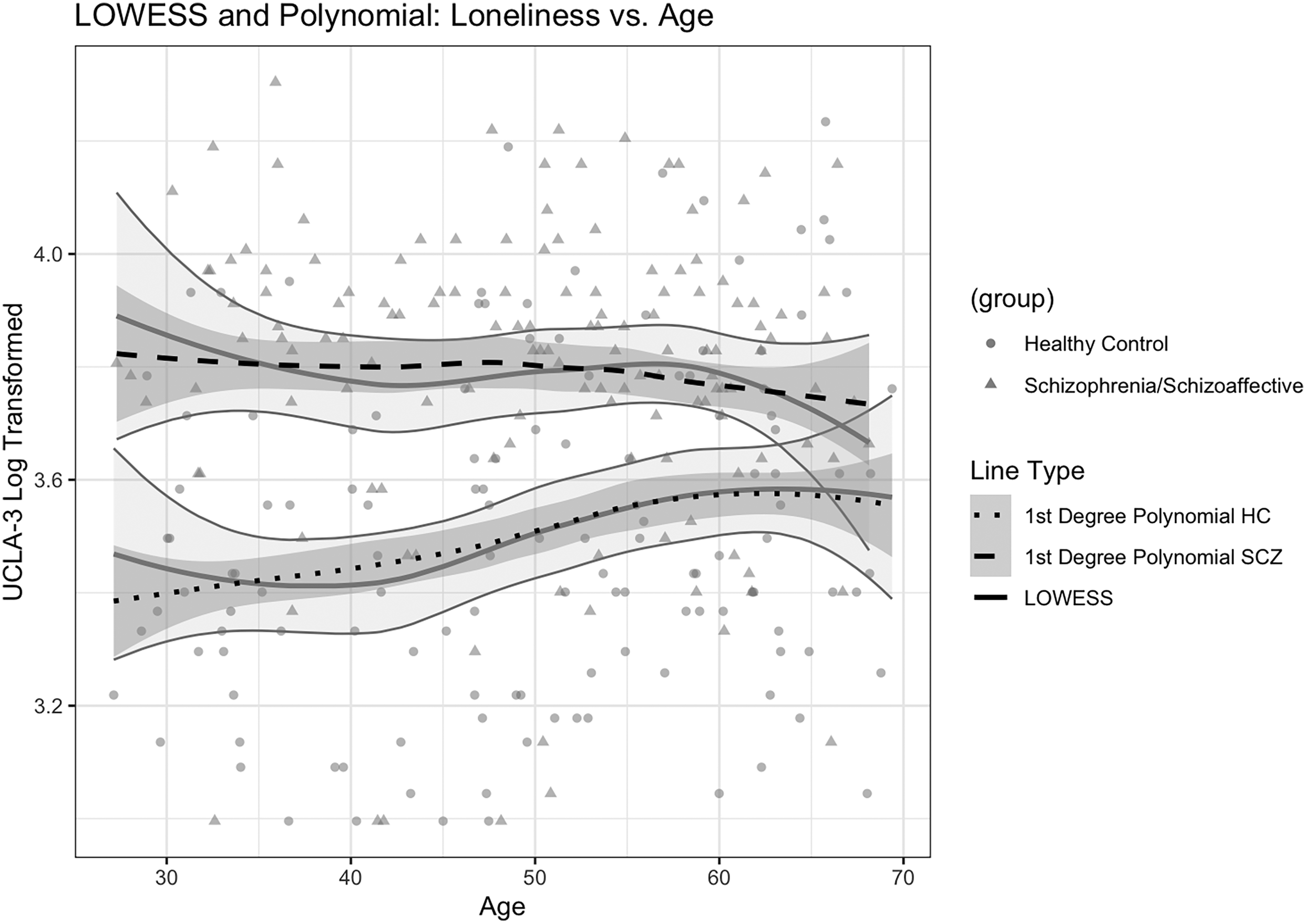
Relationship between loneliness and age among people living with schizophrenia (PLWS) and non-psychiatric participants (NCs).
Trimmed* Polynomial Regression Model Predicting Loneliness (Log-Transformed) in People Living with Schizophrenia (PLWS) and Non-Psychiatric Comparison Participants (NCs).

Bold values indicates p<0.05.
NCs = non-psychiatric comparison participants; PSS = Perceived Support Scale.
*Initial model included the following covariates: psychiatric diagnosis, marital status, living situation, marital status, personal income level, education, race/ethnicity, emotional support, negative social interactions and the interaction of age by psychiatric diagnosis (to examine the potential moderation effect by diagnostic group on the association of loneliness with age).
In terms of physical health, we found that loneliness was associated with lower self-reported physical well-being (B = −0.17, SE = 0.05, P < 0.01, ηp2 = 0.04; Table 3A) regardless of diagnostic group. However, loneliness was not associated with objective physical health outcomes (i.e., physical comorbidities, BMI, inflammation, metabolic outcomes; Supplemental Tables 1A-1D).
General Linear Models of Loneliness with Physical and Mental Outcomes.
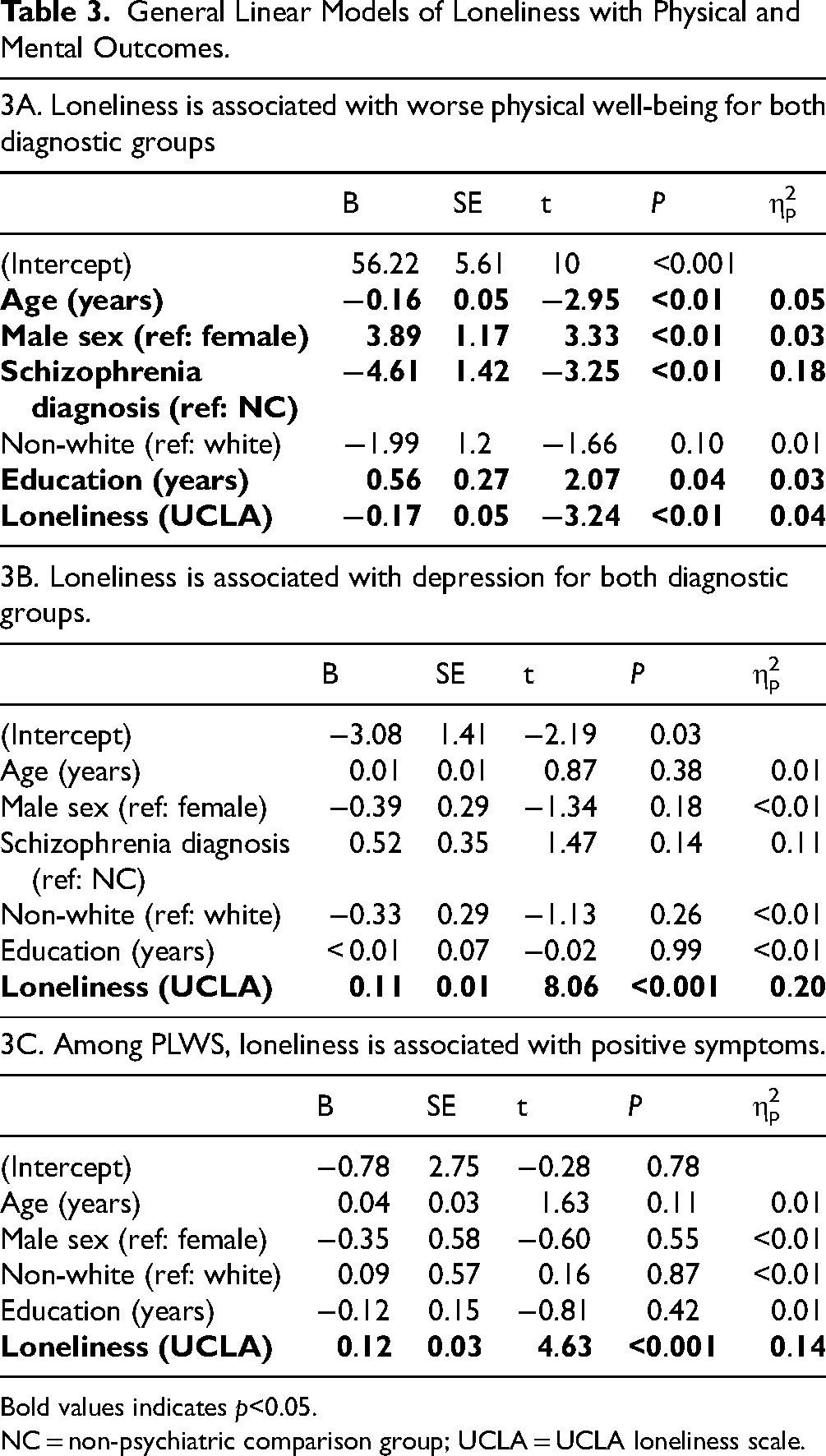
Bold values indicates p<0.05.
NC = non-psychiatric comparison group; UCLA = UCLA loneliness scale.
We observed several relationships between loneliness and psychiatric well-being. Higher loneliness was associated with higher self-reported depression regardless of diagnostic group (B = 0.11, SE = 0.01, P < 0.001, ηp2 = 0.20; Table 3B). For PLWS, a higher degree of loneliness was associated with higher levels of positive symptoms (B = 0.12, SE = 0.03, P < 0.001, ηp2 = 0.14; Table 3C). Loneliness was not associated with negative symptoms, antipsychotic dose, duration of illness or cognitive outcomes in either group (Supplemental Tables 1E-1I).
Discussion
Overall, our results partially supported our hypotheses. As expected, we observed a non-linear relationship between loneliness and age among PLWS and NCs, but the specific pattern differed between groups. PLWS between the ages of 40 and 60 had similar levels of loneliness, whereas NCs showed an increase in loneliness across this age range. We also found that overall, PLWS reported higher levels of loneliness, lower levels of perceived emotional support and more frequent negative social interactions than NCs. Loneliness was associated with self-reported physical and mental health outcomes, but not with objective physical health outcomes or cognitive outcomes among PLWS and NCs.
Our findings of greater loneliness and less social support among PLWS compared to NCs were consistent with other studies of PLWS43,44 using commonly used and validated loneliness scales. The increased loneliness among PLWS may reflect/could be reflective of the lower rates of marriage and/or having a stable partner.15,45 Indeed, our findings were similar to a 2022 study of social networks of PLWS and NCs, aged 55 + years, non-kin and formal social ties (e.g., contacts as part of a paid position) than NCs, showed that PLWS had fewer confidants, fewer reliable relationships and fewer sustenance relationships (i.e., relationships that provide food, money or other assistance) than NCs. 10 PLWS had smaller social networks than NCs overall, but had more. These findings reflect the commonly observed deficits in social functioning among people with serious mental illnesses as well as the potential generalizability of our findings to other community-dwelling PLWS.
Differences in Social Milestones
Loneliness levels appear to change with age for both groups, with a more drastic increase in loneliness from age 40 to age 60 among NCs compared to PLWS. The increased loneliness during this time period may reflect social milestones and changes in social networks that NCs, but not PLWS, tend to experience. The phenomenon of empty nesting, when adult children leave the home, is more common among NCs as PLWS are less likely to have children. 45 The departure of children from the home can increase isolation and can change much of the daily routine related to parenting for NCs. 46 Further, many PLWS in our sample (50.7%, n = 71) lived in assisted living facilities where social networks may primarily consist of non-kin relationships such as roommates and facility staff. Such relationships and household structures may remain more stable over time, compared to these life milestones commonly experienced by NCs. In addition to changes in household structure, NCs often have changes in job status and income level in older age that may increase risk for loneliness. 11 Retirement, especially involuntary retirement, may be linked to decreased social interactions from work and has been associated with increased loneliness in certain societies. 47 However, PLWS have lower rates of employment, in large part related to psychopathology and cognitive deficits, and thus, are less likely to experience retirement and related subsequent changes in income, etc. In sum, social and economic factors that change in NCs during middle- to late-life remain relatively stable for many PLWS. Further research is needed to examine aging-related changes in specific elements of social network structure and social support among PLWS and NCs in order to better support older adults.
Loneliness in Older age for PLWS
While our results suggest a possible decline in loneliness for PLWS after age 60, data is sparse at this older age range and more targeted inquiry is needed. As with all cross-sectional studies of PLWS, survivorship bias may impact the findings such that older PLWS in the study are exceptionally healthy, have less severe psychiatric symptoms, and are well-supported on average compared to younger PLWS. Younger PLWS may be more heterogeneous, including individuals who may not survive to age 60.48,49 Cardiovascular and metabolic disease are primary causes of premature mortality among PLWS, related to exposure to medications, smoking and sedentary lifestyles.9,50,51 Conversely, good social functioning is linked to more active and healthier lifestyles,52–58as well as better adherence to medical treatments. 59
Loneliness and Health
Our findings suggest that loneliness is linked to perceived physical health, rather than objective physical health measures. 15 These findings contrast prior studies that found links between loneliness and poor physical health and metabolic disturbances in the general older population.52–58 This apparent discrepancy may be explained by the relatively limited age range of the current NC sample (27–69 years) and high prevalence of poor physical health among PLWS for a wide variety of reasons. In addition, the findings could reflect the services provided in assisted living facilities. Our prior work found that PLWS in supportive housing (assisted living facilities for individuals with serious mental illnesses) often had worse prognostic indicators (younger age of onset, more physical comorbidities and elevated coronary heart disease risk) compared to PLWS living with family/friends/partners in houses/apartments. 60 However, possibly due to the services provided by the facilities (e.g., medication management, food, staff and peer support), the PLWS in supportive housing had better mental well-being, lower BMI and lower inflammatory biomarker levels compared to PLWS living in houses/apartments with others.
We found that loneliness was linked to depression and positive symptoms among PLWS, which is consistent with prior studies. 5 While our results are cross-sectional and causality cannot be inferred, the links between loneliness and depression are likely complex and bidirectional. Loneliness may predict poorer depression outcomes over time. 61 One recent study of cognitive behavioural therapy for psychosis found that loneliness predicted subsequent depressive symptoms, while positive symptoms predicted subsequent loneliness. 62 Loneliness may also independently impact functioning, even when accounting for depressive and negative symptoms.43,63 Using loneliness as a dynamic measure of social functioning can be helpful to monitor PLWS and their needs for services and resources.
Limitations and Future Directions
These results should be considered in light of several limitations. First, the data in the current study is cross-sectional, and therefore cannot reveal causal links between loneliness and aging. Future work should include longitudinal measures of loneliness across the lifespan. Second, many participants in the PLWS group resided in board and care homes (i.e., assisted living facilities) at the time of this study (50.7%, n = 71), thus there may be an overrepresentation of participants living in supported housing and the results might not generalize to certain groups of PLWS. In addition, although our overall sample is relatively diverse, the PLWS and NC groups differ based on race and ethnicity. The NC group has a significantly greater proportion of participants who identify as White, which is important to consider when interpreting these results. Participants were excluded if their mental or physical functioning impeded their ability to participate in the study procedures, so these findings might not generalize to individuals with higher levels of disability. Finally, although our methodological decisions were evidence-based, our choice of statistical method (i.e., MICE, LOWESS) has influence over our final results. Different statistical methods, such as choosing not to use imputation, could yield slightly different results.
Taken together, these results provide insight into trajectories of loneliness for PLWS compared to NCs and have the potential to inform future interventions for loneliness across the lifespan. The effectiveness of loneliness interventions is limited in older adults, 64 so focusing interventions on prevention of loneliness prior to these age-related peaks could improve loneliness-related outcomes. 65
Supplemental Material
sj-docx-1-cpa-10.1177_07067437251355636 - Supplemental material for Non-Linear Relationships of Loneliness with Age in People Living with Schizophrenia and Non-Psychiatric Comparison Participants: Relations non linéaires entre la solitude et l’âge chez les personnes atteintes de schizophrénie et les personnes n’ayant aucun antécédent de maladie psychiatrique
Supplemental material, sj-docx-1-cpa-10.1177_07067437251355636 for Non-Linear Relationships of Loneliness with Age in People Living with Schizophrenia and Non-Psychiatric Comparison Participants: Relations non linéaires entre la solitude et l’âge chez les personnes atteintes de schizophrénie et les personnes n’ayant aucun antécédent de maladie psychiatrique by Andrea M. Coppola, Jerry McDonald, Amy M. Jimenez, Jin Cao, Lucy Shao, Yijia Xue, Bowei Zhang, Luke C. Valmadrid, Lisa Eyler, Xin M. Tu and Ellen E. Lee in The Canadian Journal of Psychiatry
Footnotes
Acknowledgments
We would like to acknowledge the contributions of all the study participants to this study.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported, in part, by the National Institute of Mental Health [an R01 grant (R01MH094151-01) and a K23 grant (K23 MH119375-01)], the National Institute of Health [NIH UL1TR001442 of CTSA (PI: Gary Firestein, MD)], a Havens Established Investigator Grant from The Brain & Behavior Research Foundation, the American Psychiatric Association, the Desert-Pacific Mental Illness Research Education and Clinical Center at the VA San Diego Healthcare System, and the Stein Institute for Research on Aging at the University of California San Diego.
Data Availability
Data from this paper will be available upon request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
