Abstract
Objective:
To investigate patterns and predictors of help seeking and met/unmet needs for mental health care in a national population health survey.
Method:
Participants were respondents to the 2012 Canadian Community Health Survey on Mental Health (CCHS-MH; n = 25,133). We used regression to identify the diagnostic and sociodemographic predictors of the use of informal supports, primary care, and specialist care, as well as perceived unmet needs.
Results:
Eleven percent of Canadians reported using professionally led services for mental health or substance use in 2012, while another 9% received informal supports. Two-thirds of people with substance use disorders did not receive any care, and among those who did, informal supports were most common. Seventy-four percent of people with mood/anxiety disorders and 88% of those with co-occurring disorders did access services, most commonly specialist mental health care. Men, older people, members of ethnocultural minorities, those not born in Canada, those with lower education, and those with higher incomes were less likely to receive care. Unmet needs were higher among people with substance use disorders.
Conclusions:
Gaps in services continue to exist for some potentially vulnerable population subgroups. Policy and practice solutions are needed to address these unmet needs. In particular, the convergence of research pointing to gaps in the availability and accessibility of high-quality services for substance use in Canada demands attention.
Clinical Implications
Efforts should be made to increase the use of primary and specialist care among people with substance use disorders.
Outreach efforts may be warranted for older people, those with low education, members of ethnocultural minorities, and immigrant populations, who are less likely to seek care for mental health and substance use.
Limitations
Temporal relationships between disorders, perceived needs, and service use cannot be determined.
Meeting the criteria for a diagnosis as determined by a lay interviewer is not equivalent to a clinical diagnosis.
Epidemiological research has consistently found that only a minority of people with mental or substance-related problems seek professional help. 1 –5 This finding has been replicated across studies and countries, despite differences in health care systems and populations. Many people who meet the criteria for a disorder in population surveys do not perceive a need for services, and, indeed, many of these cases are mild or self-limiting. 6,7 Others perceive a need for care but, for a variety of reasons, do not seek or receive it. 1,6,8 Although the likelihood of seeking help increases with problem severity, 1 –3,5,9 data from the World Mental Health Surveys estimate that between a third and half of serious cases of mental disorders go untreated within a given year. 2,5 The interplay between diagnoses, perceived needs for care, and service use is of interest because it informs our understanding of help-seeking processes and highlights potential barriers and inequities in the service system.
An international body of research has demonstrated that, relative to those with mood or anxiety disorders, people with substance use disorders (SUDs) report lower impairment and lower perceived need for services. 10 –12 Even after controlling for generalised distress, people with SUDs are less likely than those with other mental disorders to seek care. 3 Older people, men, and people with lower education also tend to be less likely to perceive a need for 6,7,10 and receive care. 5 In studies conducted in Canada, where the availability of universal health insurance can be expected to minimise at least some barriers to many types of services, female sex, younger age, and higher education are linked with the use of a variety of service types. 3,13,14 Service use is also consistently lower among immigrant populations than among those born in Canada. 15 –17 Such findings are important because they point to potential gaps in care within particular vulnerable subgroups, despite universal, albeit incomplete, health insurance.
Not all people who meet criteria for disorder perceive a need for care, and not everyone who receives care will feel their needs have been met. Perceived need for mental health care plays a role in service use, inasmuch as people who do not recognise a need will not ordinarily seek care. Self-reported unmet needs among service users do not necessarily mean care was ineffective; however, it comprises part of the overall help-seeking experience and may affect future help-seeking behaviours. In Canada, perceived unmet needs are associated with co-occurring mood/anxiety and SUDs, 8,18 younger age, lower income, and greater psychological distress. 8,19 –22 The link between education and unmet needs varies in direction depending on the type of barrier and the population under study. 19,21,23 Findings that sizable proportions of past-year service users report unmet needs during the same time period highlight the importance of not limiting the evaluation of unmet need to those who have not received care or to equating service use with met need. 19,20
In Canada, most national population-level studies of service use for mental health and substance use were conducted using data collected in 2002, when the first national survey of mental health was conducted. An updated look at the sociodemographic predictors of specific care patterns and whether or not perceived needs are met is needed to evaluate equity in service delivery and system planning. Furthermore, the 2002 survey did not ask respondents to distinguish between perceived met and unmet needs for care. Information on patterns of perceived met and unmet needs for mental health care adds to the overall understanding of need for mental health services and how that need is distributed across the population. 22
In this analysis, we use data from a 2012 national population survey to evaluate whether help seeking and met/unmet needs for mental health care vary by sociodemographic characteristics that may characterise social vulnerability and that have been previously linked with help seeking. Our objectives were to 1) identify characteristics associated with receipt of specialist care, primary care, and informal supports and 2) evaluate whether there are differences across sociodemographic subgroups in terms of whether perceived needs for care are met.
Methods
Sample and Data Collection
Participants were respondents to the 2012 Canadian Community Health Survey on Mental Health (CCHS-MH; n = 25,133). The target population was Canadians aged 15 years and older, excluding those living in the territories, in institutions, on reserves, and on military bases. The sample is weighted to be representative of the approximately 28 million people within this sampling frame. 24 The response rate was 68.9%.
Measures
Diagnostic algorithms and distress
The CCHS-MH used the World Health Organization–Composite International Diagnostic Interview (WHO-CIDI) version 3, 25 which uses the diagnostic categories of the fourth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV), to assess the following conditions: major depressive episode, bipolar disorder I and II, generalised anxiety disorder, alcohol abuse and dependence, and abuse and dependence for other drugs, collapsed across substances. 24,26 We constructed a 4-level categorical variable representing past-year disorder status: no CCHS diagnosis, SUD only (including both abuse and dependence), mood/anxiety disorder only, and co-occurring mood/anxiety and SUD. It should be noted that people who do not meet the criteria for the disorders covered by the survey may still have another mental disorder and that people not meeting criteria in the past year may nonetheless have had 1 or more disorders earlier in life. We use the term no CCHS diagnosis to reflect this group’s status. Generalised distress in the past month was assessed using the K-10, 27 which varies from 0 to 40, with higher scores indicating greater distress.
Service use
Respondents reported on an array of professionally led services and informal supports for mental health and substance use. We created a hierarchical variable to describe past-year service use: specialist care (hospitalisations and visits to psychiatrists, psychologists, social workers, or counsellors), primary care without specialist care (visits to family doctors, general practitioners, or nurses, in the absence of specialist care), informal supports only (had no primary or specialist care but spoke to family, friends, or colleagues; used Internet-based supports or telephone helplines; or attended self-help groups), and no care. Among those who used specialist care, we also tallied the number of visits to specialist care providers (psychiatrist, psychologist, counsellor, or social worker) in the past year.
Perceived met and unmet need
Met and unmet needs for services in the past year were assessed with the Perceived Need for Care Questionnaire. 28 Respondents were asked whether they had accessed information (about mental health or substance use or about services), medication, counselling or therapy, and/or other services and whether their needs for each type of assistance were met. We collapsed across the 4 types of assistance and classified respondents into 3 mutually exclusive groups: 1) no perceived needs, 2) all perceived needs met, and 3) at least some unmet needs.
Sociodemographic variables included sex (male vs. female), age groups (15-24, 25-34, 35-44, 45-54, 55-64, and 65+), respondent education (high school or less vs. postsecondary), annual household income (15 categories ranging from ≤$5000 to ≥$149,000), ethnocultural minority (yes vs. no, with “yes” representing all those who identified as nonwhite, including Indigenous peoples), and lifetime immigration (yes vs. no). We modeled age as a categorical variable because of evidence of nonlinear relationships with help seeking and perceived needs.
Analysis
We first calculated rates of past-year service use by diagnostic group. We used multinomial logistic regression to identify variables discriminating among users of different types of services (reference = none). For the subset of respondents who had visited a specialist care provider in the prior year, we used negative binomial regression to investigate predictors of the number of visits. Predictors included diagnostic group, distress, and sociodemographic characteristics. The analytic sample excluded 248 people (1.0%) who had missing values for any variable (final n = 24,875).
We then cross-tabulated perceived needs for care by diagnostic group and used logistic regression to identify the diagnostic and sociodemographic predictors of perceived unmet needs, controlling for past-year service use. The analytic sample excluded 1351 people (5.4%) who had missing values for any variable (final n = 23,782).
Analyses were conducted in Stata (StataCorp LP, College Station, TX) and SAS (SAS Institute, Cary, NC); α = 0.05. Parameter estimates were bootstrapped (500 replications) using a set of sample weights constructed by Statistics Canada for this purpose. This process aligned the sample with the Canadian population and accounted for the complex design of the CCHS-MH.
Results
One in 10 Canadians met the criteria for a past-year disorder: 3.3% for SUD only, 6.0% for mood/anxiety disorders only, and 1.1% for co-occurring disorders.
Use of Services and Supports
One in 5 Canadians reported using services or supports for mental health or substance use in the year prior to the survey (Table 1). This varied across diagnostic groups, being highest among those with co-occurring disorders. Sixty-five percent of people with SUDs did not seek any services. Among those who did, informal supports were most commonly accessed. In contrast, most people with mood/anxiety disorders (74%) or co-occurring disorders (88%) did access services, most commonly specialist mental health care. Specialist care was uncommon among those with SUDs. Past-year hospitalisations were comparatively rare in all groups, ranging from 3% to 4% among those with mood/anxiety or SUD to 10% of those with co-occurring disorders.
Past-Year Service Use for Mental Health and Substance Use in the Canadian Population in 2012.a
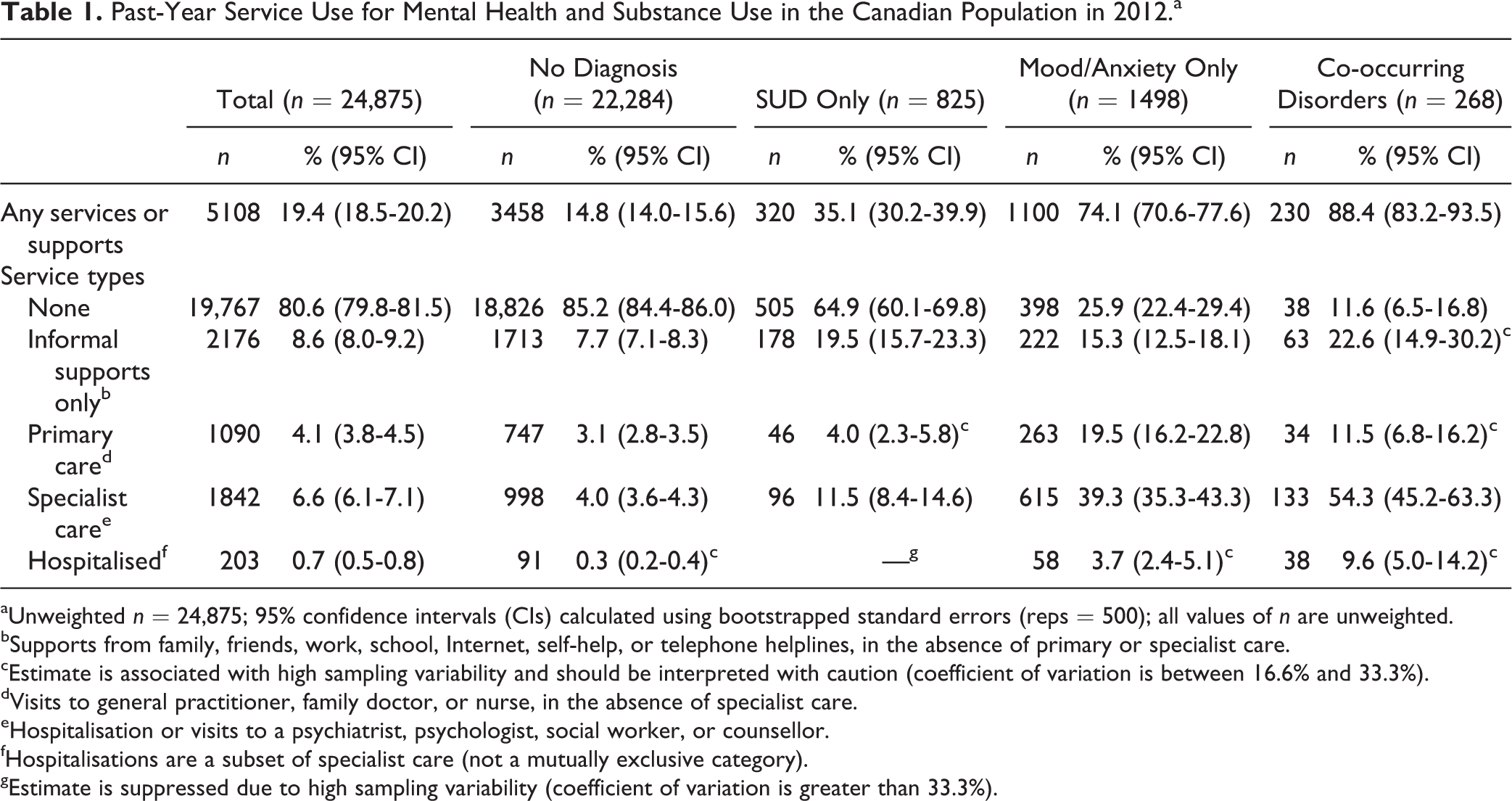
aUnweighted n = 24,875; 95% confidence intervals (CIs) calculated using bootstrapped standard errors (reps = 500); all values of n are unweighted.
bSupports from family, friends, work, school, Internet, self-help, or telephone helplines, in the absence of primary or specialist care.
cEstimate is associated with high sampling variability and should be interpreted with caution (coefficient of variation is between 16.6% and 33.3%).
dVisits to general practitioner, family doctor, or nurse, in the absence of specialist care.
eHospitalisation or visits to a psychiatrist, psychologist, social worker, or counsellor.
fHospitalisations are a subset of specialist care (not a mutually exclusive category).
gEstimate is suppressed due to high sampling variability (coefficient of variation is greater than 33.3%).
These associations between service type and diagnostic group persisted in multivariable models controlling for sociodemographic characteristics and distress (Table 2). Across service types, people with co-occurring disorders had the highest odds of help seeking. Those with SUDs were likelier to seek care than those with no CCHS diagnosis but had lower odds than other diagnostic groups. The odds of service use also increased with distress. Use of informal care only was higher among young people and declined with age, while use of specialist care was less common among those older than 55 years, and especially among those 65 years or older. Use of primary care only was somewhat more common among people aged 35 to 64 years than among older or younger respondents. Across service types, use of care was rarer among men and among those not born in Canada and more common among those with a postsecondary education. The odds of service use also declined with increasing income, with no difference by service type. Belonging to an ethnocultural minority was associated with lower odds of specialist care.
Predictors of Past-Year Service Use for Mental Health and Substance Use.a
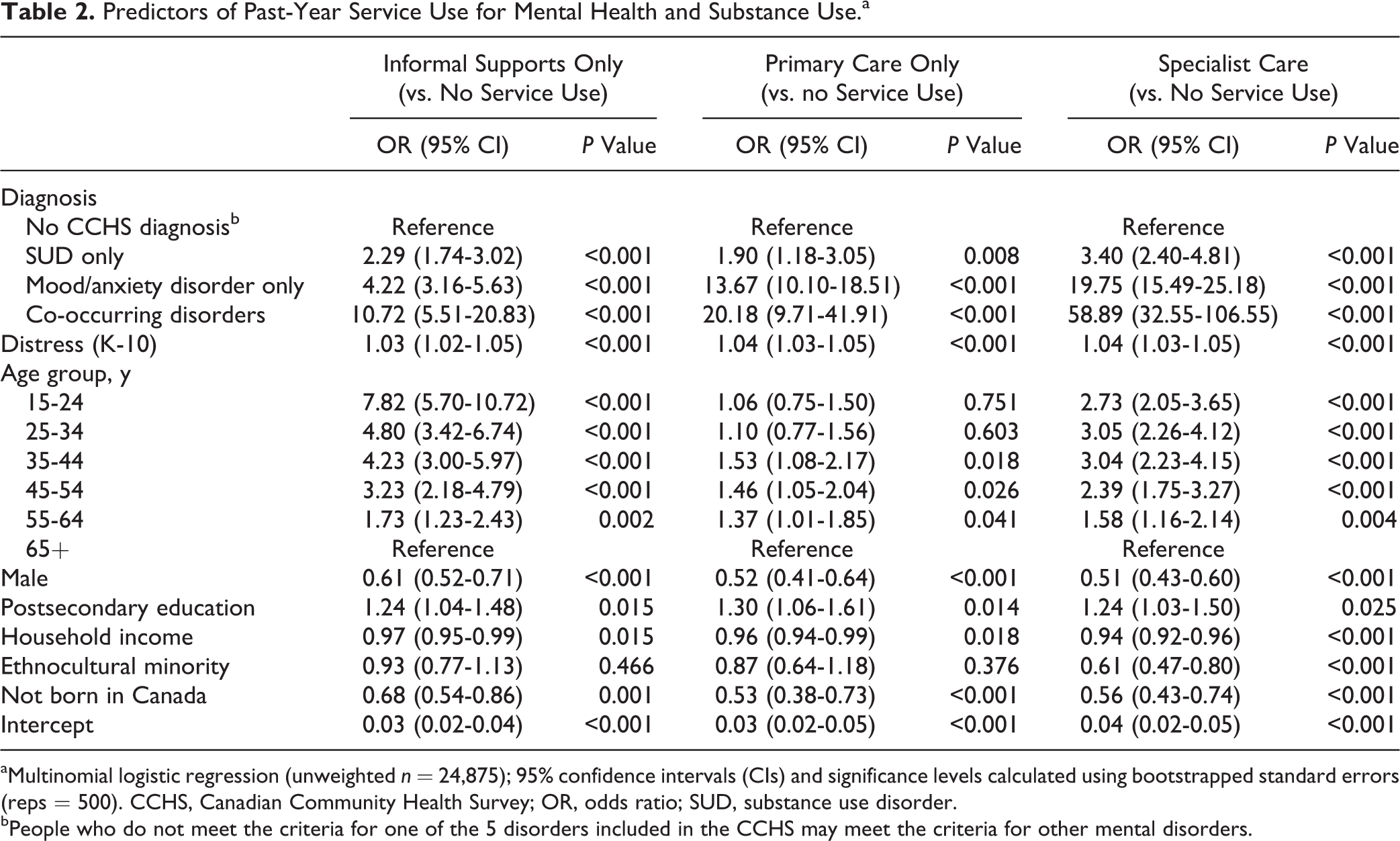
aMultinomial logistic regression (unweighted n = 24,875); 95% confidence intervals (CIs) and significance levels calculated using bootstrapped standard errors (reps = 500). CCHS, Canadian Community Health Survey; OR, odds ratio; SUD, substance use disorder.
bPeople who do not meet the criteria for one of the 5 disorders included in the CCHS may meet the criteria for other mental disorders.
Among those who had visited a specialist care provider (n = 1750), the mean number of visits in the previous year (to psychiatrists, psychologists, social workers, and counsellors combined) was 14.4 (95% confidence interval [CI], 11.9-17.0) among those with no CCHS diagnosis, 18.6 among those with SUD only (95% CI, 11.7-25.4), 30.5 (95% CI, 22.4-38.5) among those with mood/anxiety disorders only, and 20.4 (95% CI, 14.7-26.2) among those with co-occurring disorders. Controlling for sociodemographic variables and distress, the number of specialist visits was significantly higher for those with mood/anxiety and co-occurring disorders, relative to those with no CCHS diagnosis (Table 3). The number of visits across age groups showed an inverted U-shaped distribution, being highest among those 35 to 44 years old. The number of visits also declined with increasing income. No other variables were associated with the number of specialist visits.
Predictors of the Number of Specialist Visits in the Past Year.a
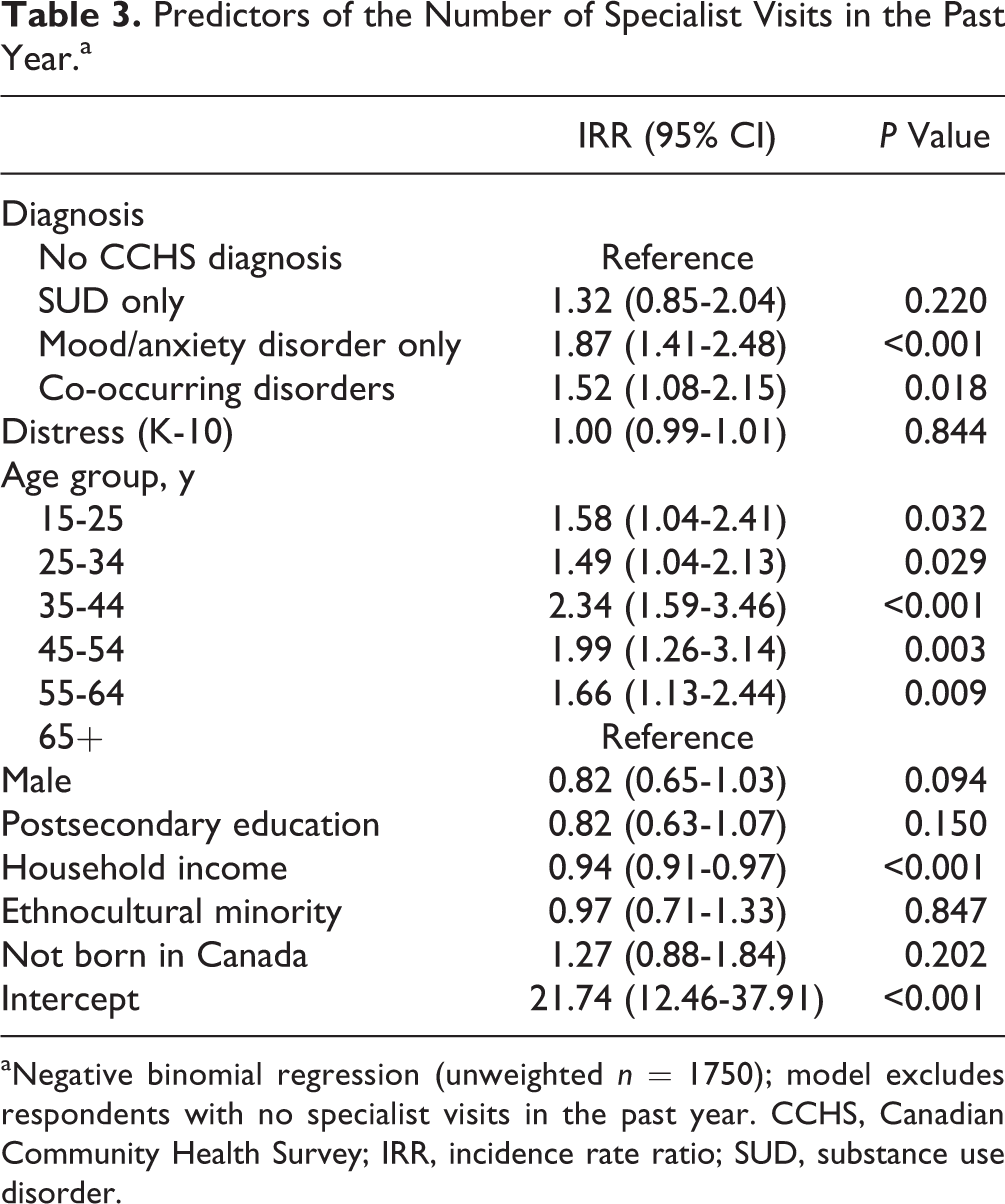
aNegative binomial regression (unweighted n = 1750); model excludes respondents with no specialist visits in the past year. CCHS, Canadian Community Health Survey; IRR, incidence rate ratio; SUD, substance use disorder.
Perceived Met and Unmet Needs for Services
Approximately 1 in 6 Canadians reported perceiving a need for services in the past year (Table 4). People with SUDs were less likely to perceive a need for care than were those with mood/anxiety or co-occurring disorders. Among those who perceived a need for care, the proportion of people whose needs were met ranged from 47% of those with co-occurring disorders to 72% among those with no CCHS diagnosis.
Perceived Needs for Services for Mental Health and Substance Use in the Canadian Population in 2012.a
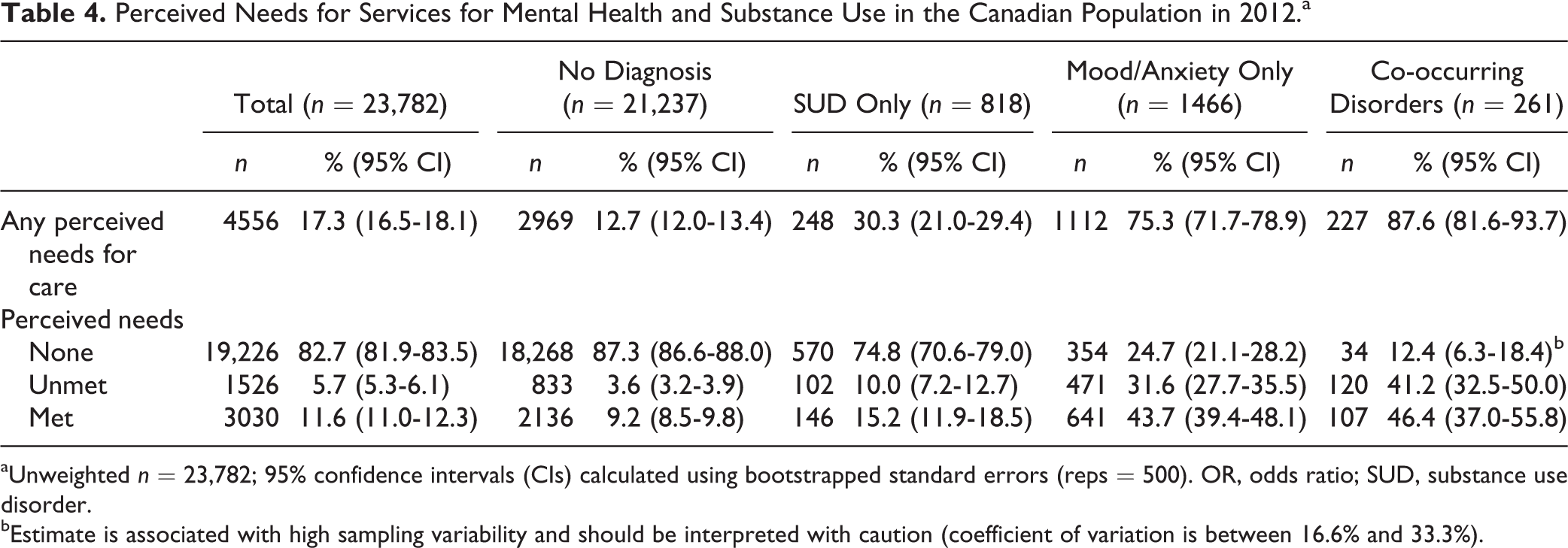
aUnweighted n = 23,782; 95% confidence intervals (CIs) calculated using bootstrapped standard errors (reps = 500). OR, odds ratio; SUD, substance use disorder.
bEstimate is associated with high sampling variability and should be interpreted with caution (coefficient of variation is between 16.6% and 33.3%).
In the multivariable model, type of service use was strongly associated with whether perceived needs were unmet (Table 5). People who received professionally led services were less likely to report unmet needs; informal supports alone did not improve the odds of needs being reported as met. Controlling for service use, unmet needs were more likely among people with SUDs, those with greater distress, and people younger than 65 years. No other variables predicted whether or not perceived needs were met.
Predictors of Unmet Needs Among Those Who Perceived a Need for Mental Health Care.a
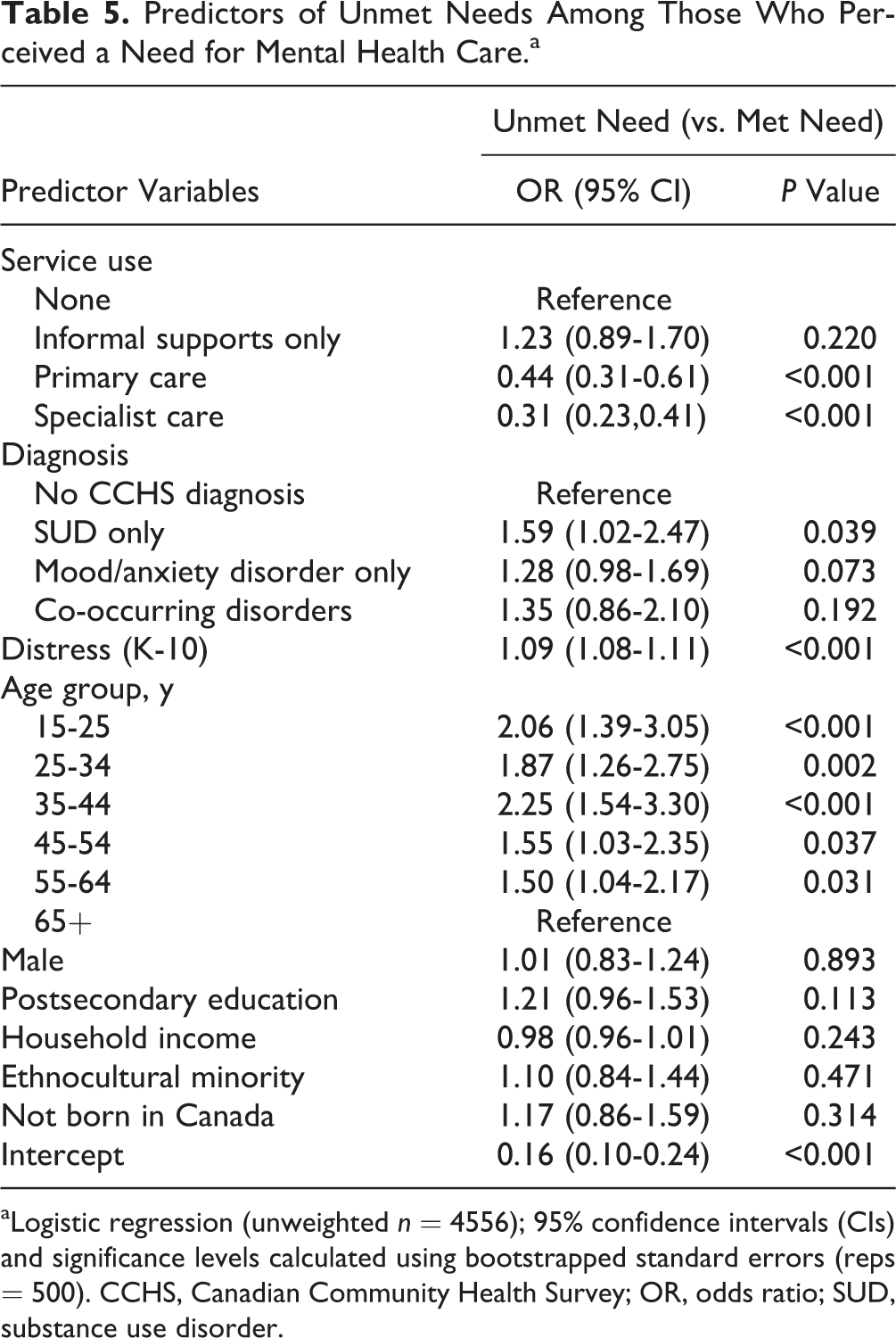
aLogistic regression (unweighted n = 4556); 95% confidence intervals (CIs) and significance levels calculated using bootstrapped standard errors (reps = 500). CCHS, Canadian Community Health Survey; OR, odds ratio; SUD, substance use disorder.
Discussion
This study builds on prior work, conducted using data collected in 2002, by providing updated estimates of help seeking and perceived unmet needs for care. We report novel findings on population differences between those who did and did not receive specialist mental health care, as well as between those who reported that their needs for mental health care were met versus unmet. Findings highlight persisting gaps in addressing population need for services for SUD and point to possible sociodemographic inequities in the accessibility and acceptability of services.
One in 5 Canadians reported accessing services and supports for mood/anxiety and SUDs in 2012. Although this is about double the level of help seeking reported 10 years earlier, 3 differences in survey design, disorder coverage, and classification of services (particularly for informal supports) complicate comparisons. Consistent with findings from 2002, 3 and despite differences across the surveys, help seeking was more common for mood/anxiety conditions than for SUDs. Although people with co-occurring disorders were most likely to use services, the largest difference in help-seeking rates was between those who did and did not have mood/anxiety disorders. In addition, although people with co-occurring disorders most often perceived unmet needs for care (again in line with findings from the 2002 survey), 3 in the multivariable model controlling for service use, it was SUD that distinguished met from unmet needs.
The comparatively low rates of help seeking and perceived needs for care in people with SUDs have been documented previously. 3–4,10 We also found that people with SUDs relied more heavily on informal supports than on professionally led services. Among those who perceived a need for care, people with SUDs were less likely than those with mood/anxiety disorders to report that their needs had been met, independent of whether or not services were accessed during the year. Specialist mental health care, which was the most common form of services accessed by those with mood/anxiety disorders, was uncommon among those with SUDs. Once they accessed specialist care, people with SUDs, both alone or co-occurring with other mental disorders, also tended to make fewer visits. Although comparisons across surveys and countries must be made cautiously, the overall rate of use of specialty mental health care among people with SUDs in Canada appears to be lower than that reported for the United States. 4
There are many potential reasons for these findings. Although negative attitudes toward seeking mental health care are common in most populations, studies suggest that embarrassment and discomfort are particularly salient barriers to care among people with SUDs. 29,30 There are also well-documented gaps in substance use treatment systems and policy responses in Canada. These include a lack of services for common physical and mental health comorbidities of substance use, fragmentation and inconsistencies in the types of services provided across jurisdictions, and lack of attention to diversity and culturally and developmentally appropriate care. 31,32 This is compounded by the lack of a consistent policy response to substance use over the 2000s, with municipal and provincial policies favouring public health–oriented strategies and federal policies emphasising drug law enforcement. 32
It is notable that the majority of people receiving care or support did not meet past-year criteria for any of the disorders assessed in the CCHS-MH. It is not possible to say, however, how much of this is due to unnecessary treatment. First, both the “diagnostic” interview and self-report of care are subject to error. Second, people may have had mental health conditions not included in the CCHS-MH. Third, some people will have a history of disorder without meeting past-year criteria, perhaps because their condition is episodic or because they have received effective care. Finally, some people will use care and supports for issues that would not merit a formal diagnosis, including adjustment and relationship problems or other sources of distress. It is a consistent finding across countries that most of the past-year service users who do not meet the criteria for past-year disorders do meet criteria for a lifetime disorder or a past-year subthreshold disorder, or they have other indicators of potential need, such as a recent stressful life event. 33,34
Independent of diagnoses, informal supports (in the absence of professionally led services) were associated with a higher level of unmet needs. Although these supports may be sufficient in some cases, many people who received them still perceived a need for professionally led care. Informal supports were defined broadly to include everything from support from friends and family to participation in more structured mutual aid groups. Given that the items on perceived needs for care predominantly covered professionally led care, it may not be surprising that unmet needs were more common among those who had received only informal supports.
Consistent with prior work, 3 –5 our findings point toward lower use of services by men and older people after controlling for indicators of need (i.e., disorders and distress). Younger people (under 25 years old) were much more likely than others to access informal supports without professionally led services, and the odds of informal supports declined steadily with increasing age. People aged 35 to 64 years were more likely than older people to access primary care without specialist involvement. Older people were less likely than others to receive any specialist care and, when they did, tended to have fewer visits. Among those who perceived a need for service, however, it was people under 65 years old who were more likely to report unmet needs, irrespective of whether they received services. This association was also reported in 2002, 8,21,22 signaling a need for work that identifies the underlying reasons in younger and middle-aged respondents (e.g., whether high-quality services are not available when needed or are not acceptable to those who could benefit from them).
Findings also supported associations between socioeconomic status and help seeking. To the extent that mental health tends to be poorer among those with lower socioeconomic status, 14,35,36 in the context of Canada’s universal health coverage, service use should be higher in lower socioeconomic groups. In our multivariable model, service use declined with increasing income, but people with postsecondary education were independently more likely to access all forms of mental health care. It may be that education affects service use through mental health literacy and/or related factors that influence both whether care is accessed and whether referrals are made and followed. 13 For many respondents, education may also have been completed in the past, possibly before onset of mental health conditions, while income may be affected by current impairment. Although some forms of mental health care are not covered by universal health insurance in Canada, it is a positive finding that low income did not appear to be acting as a barrier to service use. A prior cross-country comparison of barriers to mental health care found that financial barriers were much more likely to be endorsed in the United States, relative to Canada or the Netherlands, particularly by respondents with low income. 30 The CCHS-MH does not distinguish between paid and unpaid services. Further evaluation of access to mental health services that are typically not covered by universal health insurance (e.g., psychotherapy delivered by clinical psychologists) should be conducted to strengthen conclusions around the relation between income and access to mental health care in Canada.
People who identified as part of an ethnocultural minority were less likely to receive specialist care, while those who were not born in Canada were less likely to receive services of any kind. As these effects are independent of diagnosis and recent distress, the healthy immigrant effect is unlikely to explain them, except insofar as immigration status might be associated with variation in problem severity uncaptured in our data (e.g., co-occurrence of disorders not assessed in the survey) or with physical health problems that might bring people into contact with providers. Nonetheless, ethnocultural minorities and those not born in Canada appear to be underserved by all categories of providers. We did not distinguish by place of origin, admission class, or time since immigration—factors that can affect service use among immigrants. Although rates of mental health service use vary across admission classes and region of origin, they still tend to be consistently lower among immigrants, particularly newcomer populations, than among nonimmigrants. 15,16,37
It is notable that, although a number of sociodemographic characteristics predicted whether or not care was sought and/or obtained, aside from age, these characteristics did not predict whether people’s perceived needs for care were met. In the general population of Canada, at least, the factors that distinguished unmet and met needs for care were the types of services that were used and indicators of need (i.e., diagnoses and distress). Notwithstanding a need for efforts to improve the reach of services to different subgroups of the population, these findings reflect positively on mental health care services in Canada.
Our results should be considered within the context of various limitations. Potential biases stemming from survey nonresponse, problems with recall, and social desirability may have affected these findings. Although research suggests that self-report of recent service use is reasonably accurate and largely unaffected by individual characteristics, 38 there is evidence of overreporting the number of mental health visits with physicians in survey data relative to administrative data. 39,40 This does not necessarily threaten results of the model considering associations between individual characteristics and intensity of specialist care; however, it does mean that descriptive results on the amount of care received should be treated with caution.
Comparisons between the CCHS-MH and the 2002 CCHS 1.2 are complicated by differences in the disorders that were covered. CCHS-MH also assessed a small number of disorders, and so our diagnostic groupings are necessarily imperfect; in particular, some people with no CCHS-MH disorder may have had some other condition. Meeting the criteria for a diagnosis as determined by a lay interviewer is also not equivalent to a clinical diagnosis; although our diagnostic groups are likely indicative of at least some problems with mental health and/or substance use, they should not be equated with the need for professionally led or specialist care. As noted, it is not possible with these cross-sectional data to elucidate causal relationships between the experience of disorders, perceptions of needs, and use of services.
Conclusions
Our study offers both a replication of findings from prior population-based analyses of help-seeking patterns and contributes new findings on the factors that distinguish between use of specific types of care and between met and unmet needs for mental health care in Canada. We highlight gaps in services for key population subgroups often associated with greater vulnerability, including people with SUDs, older Canadians, people with lower education, members of ethnocultural minorities, and those who have immigrated. These are enduring findings and highlight the need for policy and practice solutions to address these gaps in care. Our findings related to SUDs are not surprising, given documented gaps in treatment systems and related policy measures in Canada. 31,32 Provincial governments need to take stock of the systems available in their communities and work toward implementing evidence-based practices and rationale policies to address challenges in meeting the needs of the population.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Urbanoski holds a Tier 2 Canada Research Chair in Substance Use, Addictions, and Health Services Research from the Canadian Institutes for Health Research.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this work was received from the Vancouver Island Health Authority.
