Abstract
Background
The presence of metastatic disease is one of the most important factors limiting survival in patients with uveal melanoma. Studies on proteins associated with metastatic mechanisms are sparse in the literature.
Methods
Enucleation samples from 15 patients with metastatic uveal melanoma (Group 1), liver metastasectomy samples from 8 patients with metastatic uveal melanoma (Group 2), and enucleation samples from 20 patients with non-metastatic uveal melanoma as controls (Group 3) were included in the study. Antibodies against heat shock protein 27 (HSP-27), BRCA1-associated protein-1 (BAP1), C-C chemokine receptor 7 (CCR7), B-Raf proto-oncogene serine/threonine-protein kinase V600E (BRAF V600E), and programmed death-ligand 1 (PD-L1) were used to detect immunoreactivity in each sample by immunohistochemical methods. Correlations between these expressed proteins and selected histopathological and clinical features, and metastatic process were investigated.
Results
The frequencies of HSP-27 (median score: Group 1: 8, Group 2: 12, Group 3: 4) and BRAF V600E expressions (number of samples: Group 1: 4 (26.7%), Group 2: 1 (12.5%), Group 3: 0 (0%)), and BAP1 expression loss (number of samples : Group 1: 12 (80%), Group 2: 8 (100%), Group 3: 9 (45%)) were higher in samples from patients with metastatic uveal melanoma (Group 1 + 2) than in those from patients with non-metastatic disease (Group 3) (P = 0.001, P = 0.034, and P = 0.007, respectively). CCR7 expression (median score: Group 1: 0, Group 2: 2, Group 3: 3) was similar among these three groups (P = 0.136). No samples exhibited PD-L1 expression (P = 1.000). One-unit increases in the HSP-27 expression level and BAP1 expression loss were significantly related to 1.375- and 7.855-fold increases in the risk of metastasis, respectively (P = 0.007 and P = 0.017).
Conclusion
HSP-27 and BAP1 are considered to be associated with metastasis, indicating these proteins as potential treatment targets in metastatic uveal melanoma.
Introduction
Uveal melanoma is the most common primary intraocular tumor in adults, which originates from melanocytes in uveal tissues, including the iris, ciliary body, and choroid. Although the incidence of cutaneous melanoma has increased over time, the incidence of uveal melanoma has remained steady for many years. 1 Fifty percent of patients develop metastasis over the course of the disease, generally in the liver. The expected 10-year survival rate is approximately 60%, but if metastasis is present, the average life expectancy decreases to 5–8 months. 2 Despite substantial medical improvements in cancer diagnosis and treatment to date, no systemic adjuvant treatment options for metastatic disease have been confirmed to effectively reduce the risk of metastasis. The early detection of metastatic disease will substantially affect the prognosis and facilitate the development of tailored treatment regimens. However, the molecular mechanisms underlying disease pathogenesis have not yet been fully elucidated. The molecular prognostication of metastasis is potentially helpful in the management of the disease. Several molecules have previously been investigated in the literature as predictors of the metastatic potential; these molecules include heat shock protein 27 (HSP-27), BRCA1-associated protein-1 (BAP1), C-C chemokine receptor 7 (CCR7), B-Raf proto-oncogene serine/threonine-protein kinase V600E (BRAF V600E) and programmed death-ligand 1 (PD-L1).3–7
HSP-27 is a protein chaperone that responds to heat shock and facilitates the appropriate refolding of damaged proteins. 8 This protein plays an important role in developmental organization, cell apoptosis, drug resistance, and cancer metastasis; it is also considered an indicator of a poor prognosis for patients with many diseases. 8 BAP1 plays a critical role in cellular activities such as cell cycle regulation, DNA repair, and protein trafficking. The loss of BAP1 expression is strongly correlated with BAP1 mutations and is associated with the development of metastasis of uveal melanoma.5,9,10 BRAF is a serine/threonine kinase in the MAPK2 pathway that transmits signals from RAS family members to MEK1/2 and is associated with metastasis in many cancers. CCR7 is a chemokine receptor produced by multiple subtypes of immune cells that facilitates the transmigration of numerous subpopulations of T cells and antigen-presenting dendritic cells (DCs) to lymph nodes. CCR7 plays a role in regulating integrin signaling and promotes the invasion of cancer cells via migration through the extracellular matrix; it is also associated with various carcinogenesis processes. PD-L1 is a protein expressed on the tumor surface that interacts with activated T cells, leading to immune exhaustion, anergy, and ultimately, avoidance in T cells, and is associated with tumor pathogenesis. The aim of this study was to evaluate the histomorphological features and expression of these proteins in liver metastases and enucleated eyes from patients with uveal melanoma, and to identify a possible correlation between the presence of metastatic disease and the levels of these proteins.
Methods
This retrospective study was conducted with samples from 457 patients with uveal melanoma who were treated between 2005 and 2015 at the Ocular Oncology Service, Hacettepe University Hospital, Ankara, Turkey. Patients with metastatic disease who had undergone primary enucleation and/or liver metastasectomy were identified for further analysis. Eight liver metastasectomy samples from patients with metastatic uveal melanoma were obtained. In line with this number, a suitable number of enucleated eye samples from patients with non-metastatic uveal melanoma and at least 10 years of metastasis-free survival records was randomly selected and included in the study as the control group. All samples were numbered, and the evaluated samples were selected by generating a random number via an online system.
The collected data included patient age and clinical features of the uveal melanoma, recurrence, and distant metastasis, if any, and histomorphological features of the primary ocular tumor and metastatic tumor that was excised or biopsied from the liver. Patients with accompanying cutaneous melanoma were excluded from the study. The study protocol was approved by Hacettepe University Non-Interventional Clinical Research Ethics Board (GO 16/163), and this study was conducted in accordance with the tenets of the Declaration of Helsinki. The requirement for obtaining informed consent from participants was waived by the ethics board.
For each case, one tissue microarray (TMA) sample was constructed from representative areas of each paraffin block. Every sample core was 3 mm in diameter, and 4-µm-thick sections were obtained for analyses. Immunohistochemistry was performed with an autostainer system (Leica Bond Max, Newcastle, UK). Every slide was stained with antibodies against BAP1, BRAF V600E, CCR7, HSP-27, and PD-L1 according to the manufacturer's instructions. Positive and negative controls were performed during the procedure (Supplementary Table 1). Antibodies were detected using a red chromogen (Bond Polymer Refine Red Detection, Catalog No: DS9390, Leica Biosystems, Newcastle, UK). All antibodies were compatible with the autostainer system and were certified by the manufacturers.
The immunohistochemically stained sections were examined by a single pathologist who was blinded to the clinical prognostic parameters. For BAP1, tumors were scored as positive or negative based on nuclear expression, regardless of the staining intensity. For BRAF V600E, positive staining was recorded when the tumor cells showed diffuse moderate and/or strong cytoplasmic staining. Tumors with diffuse weak staining, faint isolated cytoplasmic staining or any nuclear staining were considered negative. 11 Staining for CCR7 and HSP-27 was evaluated in a similar manner as described below. The score for the percentage of positive cytoplasmic staining in the tumor cells was multiplied by the staining intensity score. Consequently, the total number of points ranged from 0 to 12. The extent of staining was classified as 0% (score = 0), 1–24% (score = 1), 25–49% (score = 2), 50–74% (score = 3), or 75–100% (score = 4); staining intensity was classified as none (score = 0), weak (score = 1), moderate (score = 2), or strong(score = 3). 12 Membrane staining in more than 5% of the cells was accepted as positive staining for PD-L1.13,14 Macroscopic images of the stained TMA slides are shown in Figure 1.

Macroscopic image of the stained TMA slides; the isolated slides served as the positive controls.
Statistical methods
Medians (minimum-maximum) and means ± SDs are presented for continuous variables; absolute and percentage frequencies are presented for categorical variables. The normal distribution of variables was assessed using visual (histograms and probability plots) and analytical (Kolmogorov–Smirnov test) methods.
Categorical variables were compared with the chi-square test (continuity correction) or Fisher's exact test, as appropriate. After the chi-square test, the z-test was applied for the variables that were different between the three groups (post-hoc test for categorical variables). The Mann–Whitney U test was performed to compare non-normally distributed continuous variables between two groups. For data with a non-normal distribution, differences among the three groups were analyzed using the Kruskal–Wallis test followed by Dunn's multiple comparison test (post hoc test for variables that are non-normally distributed)
Spearman's rho correlation coefficients were calculated to examine associations between quantitative variables. The phi or Cramer's V coefficient was calculated for categorical variables. Enter method was used for the multiple binary logistic regression analysis to investigate the effect of the independent variables (HSP-27 expression level and loss of BAP1 expression) on the development of metastatic disease. (Among metastatic (Group 1–2) and nonmetastatic (Group 3)) Variables with P < 0.05 in univariate analysis were included in the multivariable model. Odds ratios with 95% confidence intervals (CIs) were calculated for potential predictors of metastatic disease with a logistic regression model. A post hoc power calculation was applied to determine the resulting power of the study. The power was calculated using G*Power 3.1 software. Loss of BAP1 is the most accepted condition for metastatic progression of uveal melanoma. Since our priority is to evaluate the loss of BAP1, the power of the study has been calculated based on this parameter.
A P < 0.05 was considered statistically significant. Statistical analyses were performed using the IBM SPSS Statistics 23.0 software package (Statistical Package for Social Sciences; SPSS Inc., IBM, Armonk, NY, USA).
Results
Fifteen enucleated eyes (Group 1) and 8 liver samples (Group 2) from 20 patients with metastatic uveal melanoma and 20 enucleated eyes from 20 patients with non-metastatic uveal melanoma (Group 3) were included in the study. The mean ages were 55.9 ± 10.4 years for patients with metastatic uveal melanoma from whom enucleated eyes were collected, 57.0 ± 11.75 years for patients with metastatic uveal melanoma from whom liver samples were collected, and 50.3 ± 12.7 years for patients with non-metastatic uveal melanoma (P = 0.251). Primary demographic and histopathological characteristics of patients are shown in Supplementary Table 2. The tumor was located in the choroid in 31 (88.5%) patients, the ciliary body in 3 (8.5%) patients and the iris in 1 (3%) patient. Nine (60%) patients only presented metastasis in the liver, 3 (20%) patients exhibited metastasis in both the liver and lungs, 2 (13.3%) patients experienced metastasis to both the liver and skin, and 1 (6.7%) patient only presented lung metastasis. Three patients with metastatic uveal melanoma had both liver and enucleation samples. The specified patients are listed in detail in Supplementary Table 2 (patients 1, 4, 14).
Median expression scores for HSP 27 were 8, 12, and 4 in groups 1, 2, and 3, respectively. For CCR7 median expression scores were 0, 2, and 3 in groups 1, 2, and 3, respectively. BRAF V600 expression was present in 4 (26.7%) samples in Group 1 and 1 (12.5%) sample in Group 2. BRAF V600E was not expressed in Group 3. Loss of BAP 1 expression was observed in 12 (80%) samples in Group 1, in 8 (100%) samples in Group 2, and in 9 (45%) samples in Group 3. The frequencies of HSP-27 expression (P = 0.001), BRAF V600E expression (P = 0.034), and a loss of BAP1 expression (P = 0.007) were significantly different among three groups. The post hoc subgroup analysis of the HSP-27 expression level and loss of BAP1 expression showed that these results were derived from enucleated eyes obtained from patients with non-metastatic uveal melanoma (P = 0.004 and P < 0.05, respectively). However, no significant differences in CCR7 or PD-L1 immunoreactivity were observed among the groups (P = 0.136 and P = 1.000, respectively) (Supplementary Table 3). Corresponding sections showing positive staining for each protein are presented in Figures 2 to 5. In the histopathological evaluation, all parameters were statistically similar among the groups (Supplementary Table 4). No correlation was observed between the histopathological parameters and the positive expression of these molecules. In the logistic regression analysis, one-unit increases in the level of HSP-27 expression and the loss of BAP1 expression were significantly related to 1.375- and 7.855-fold increases, respectively, in the risk of metastasis (P = 0.007 and P = 0.017, respectively) (Supplementary Table 5). The model did not work optimally for BRAF V600E because BRAF V600E expression was not observed in the non-metastatic group, and thus this P-value was unable to be evaluated in the logistic regression analysis. The calculated effect size was 0.471. With a probability of error set to 0.05 and a total sample size of 43 samples, the post hoc power of this study was calculated to be approximately 80% using the chi square test for loss of BAP1.
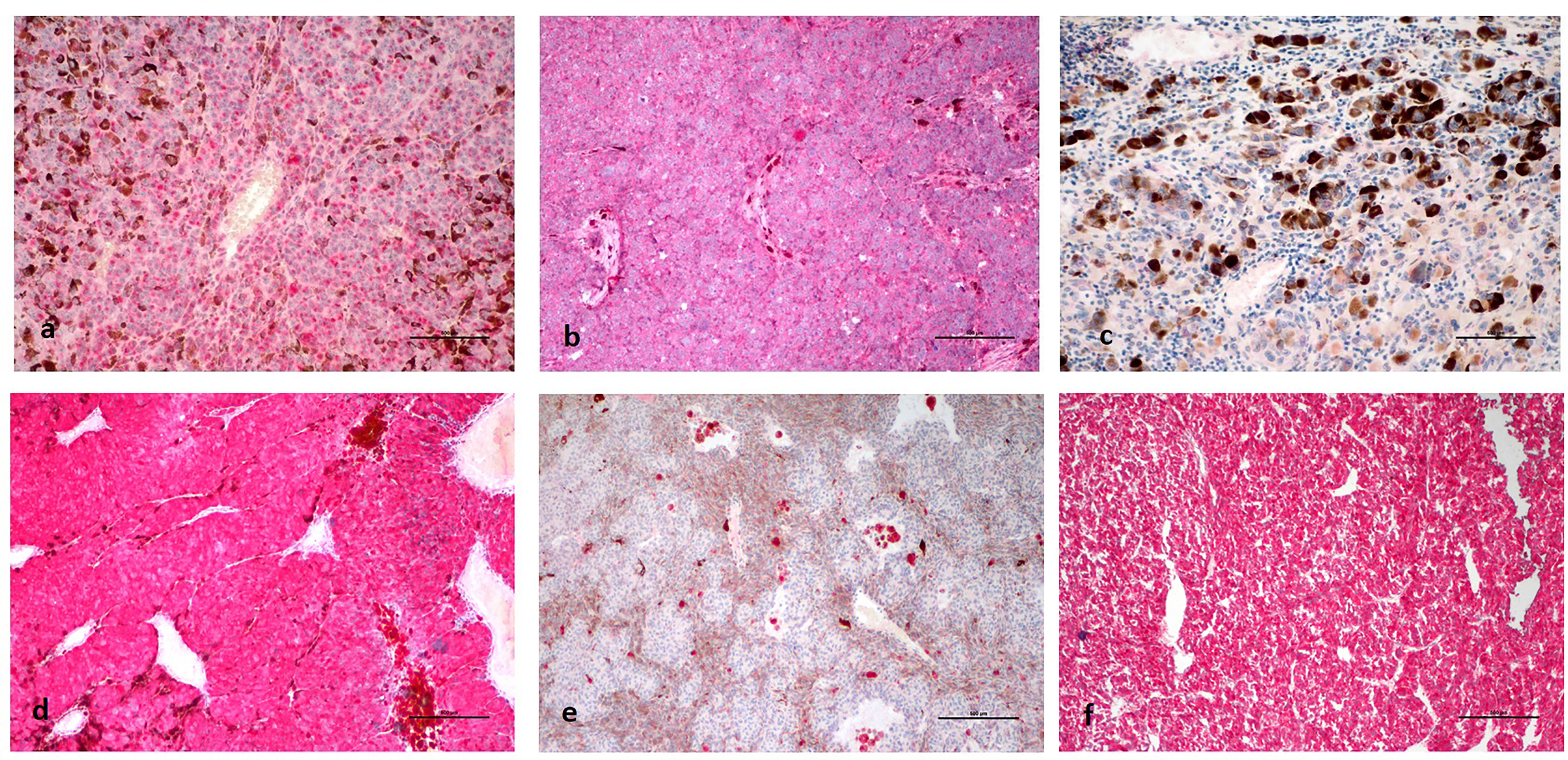
(a): Decreased BAP1 expression in tumor cells in an enucleated eye sample of metastatic uveal melanoma. (b): Diffuse BAP1 expression in tumor cell nuclei in an enucleated eye sample of non-metastatic uveal melanoma. (c): Diffuse loss of BAP1 expression in metastatic uveal melanoma cells in the liver. (d): Diffuse and strong cytoplasmic HSP-27 expression in an enucleated eye sample of metastatic uveal melanoma. (e): Diffuse loss of HSP-27 expression in an enucleated eye sample of non-metastatic uveal melanoma. (f): Diffuse and strong cytoplasmic HSP-27 expression in metastatic uveal melanoma in the liver.
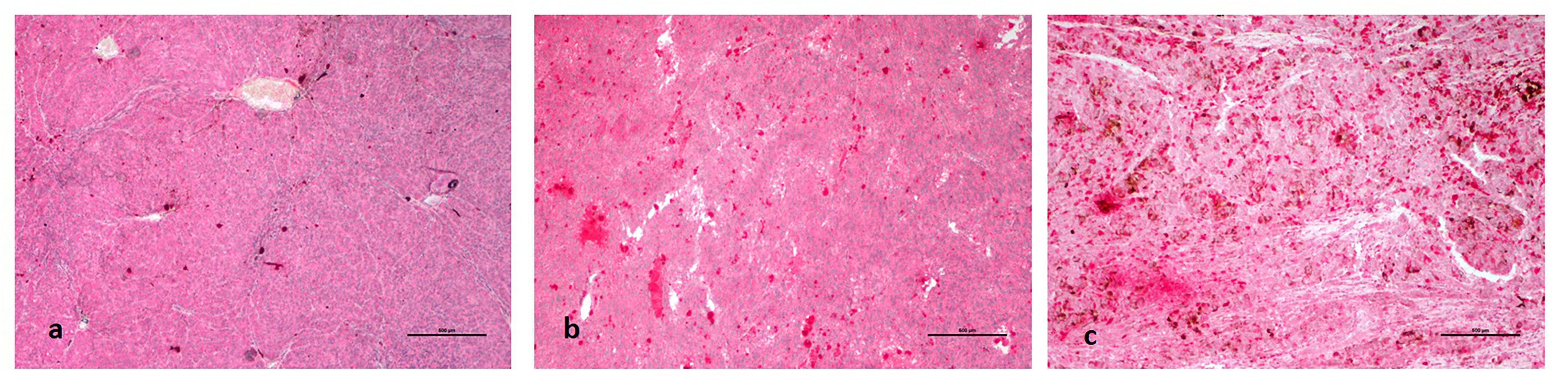
(a): Diffuse and strong cytoplasmic CCR7 expression in an enucleated eye sample of metastatic uveal melanoma; (b): in an enucleated eye sample of non-metastatic uveal melanoma; and (c): in metastatic uveal melanoma in the liver.
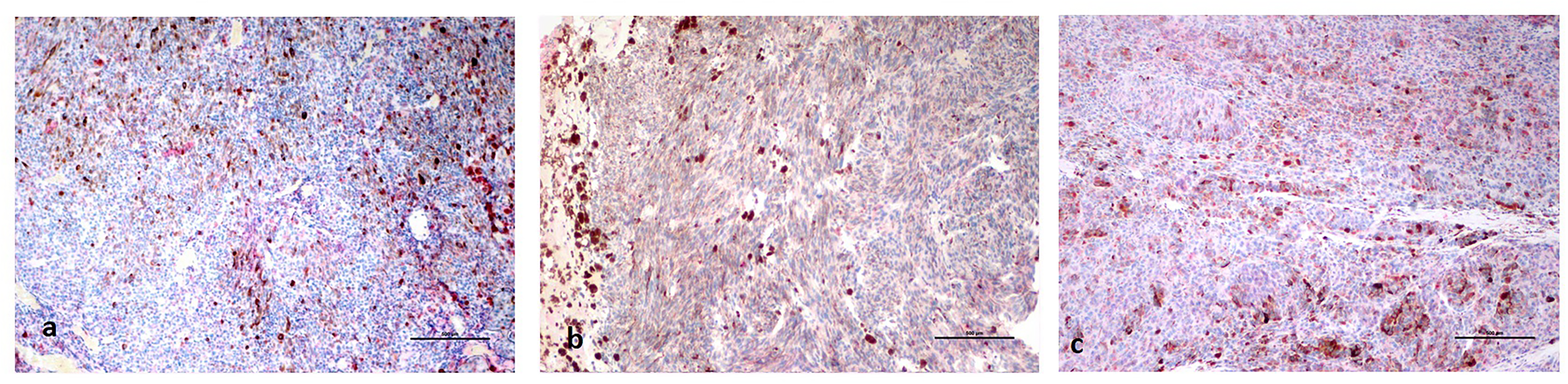
No PD-L1 expression was detected (a): in an enucleated eye sample of metastatic uveal melanoma; (b): an enucleated eye sample of non-metastatic uveal melanoma; or (c): in metastatic uveal melanoma in the liver.
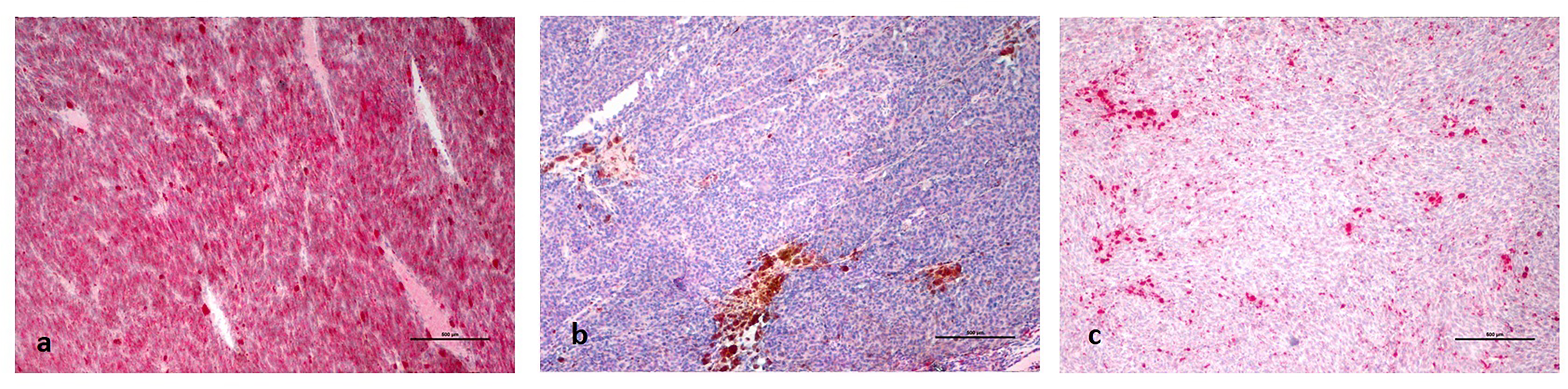
(a): Diffuse BRAF V600E expression in an enucleated eye sample of metastatic uveal melanoma. (b): Loss of BRAF V600E expression in an enucleated eye sample of nonmetastatic uveal melanoma. (c): Decreased BRAF V600E expression in metastatic uveal melanoma in the liver.
Discussion
Recent advances in the genetics and molecular biology of uveal melanoma spearheaded by multi-omics studies will likely revolutionize the management of this tumor and its distant metastases. In our study, the histomorphological features of the patients with metastatic disease were similar to patients with non-metastatic disease. Regardless of the histomorphological features that are known risk factors for metastatic disease formation and genetic parameters, such as the chromosome 3 status, the effects of these proteins that have been suggested to be related to the prognosis were evaluated and correlated directly with the presence of metastatic disease.
Matrix metalloproteinase (MMP) activity is reduced upon inhibition of the protease; thus, processes of proliferation, migration, and carcinogenesis are accelerated. 8 However, the role of HSP-27 protein in uveal melanoma is unclear. Missotten et al. 15 did not observe correlations between HSP-27 expression and important prognostic factors, such as the basal tumor diameter, tumor height, cell type, mitosis rate, and tumor localization, in patients with uveal melanoma, which is consistent with the results of our study. On the other hand, Coupland et al. 4 and Jmor et al. 16 reported a correlation between low levels of the HSP-27 protein and monosomy 3, which indicates a poor prognosis. Additionally, Coupland et al. 4 reported a 10% (n = 10) prevalence of metastatic disease, but Jmor et al. 16 reported no information on the metastatic status; moreover, neither of those studies included a metastatic subgroup. In our study, 15 (34.8%) samples exhibited clinically evident metastasis. Higher HSP-27 expression was observed in liver metastasis samples and enucleated eyes from patients with metastatic uveal melanoma than in enucleated eyes from patients without metastasis. The HSP-27 expression level indirectly correlated with genetic parameters in other studies but was clinically correlated with the presence of metastasis in our study. In addition, higher HSP-27 expression was observed in the liver metastasis samples than in the enucleated eye tissue samples from patients with metastatic and non-metastatic uveal melanoma, suggesting that HSP-27 expression might be associated with the development of metastatic disease. One biomarker strongly associated with class 2 uveal melanoma with a high metastatic activity is hypoxia-inducible factor 1 (HIF-1), the main regulator of the hypoxic response. 17 HIF-1 signaling increases the invasive capacity of uveal melanoma cells under hypoxic conditions. 18 Whitlock et al. 19 reported an association between HIF-1 activation and the protective effects of ischemic preconditioning and HSP-27 upregulation. Presumably, increased ischemic conditions in metastatic disease caused by these mechanisms may upregulate HSP-27 expression in samples from metastatic patients. Phase 2 studies of apatorsen, whose mechanism of action is associated with HSP-27 inhibition, are ongoing in patients with non-small cell lung, bladder, prostate, and pancreatic cancers in the adjuvant setting. Studies examining the therapeutic effect of this molecule on uveal melanoma are needed.
Studies have detected somatic BAP1 mutations in 47.4% of patients with primary uveal melanoma and suggested a role for BAP1 in the pathogenesis of uveal melanoma.5,20 Szalai et al. 6 comparatively evaluated the effects of tumor size, histological features, nuclear, and cytoplasmic BAP1 immunoreactivity and outcomes in patients with metastatic and non-metastatic uveal melanoma; they found that decreased nuclear BAP1 immunoreactivity was a significant independent risk factor only for the presence of metastasis. The loss of BAP1 expression is strongly correlated with the BAP1 mutation status and is associated with metastatic disease development.5,9,10 The loss of BAP1 expression is more common in class 2 uveal melanoma with high metastatic activity. 20 In our study, enucleated eyes from patients with metastatic disease exhibited lower immunoreactivity than samples from patients with non-metastatic disease; furthermore, all liver metastasis samples exhibited a loss of BAP1 expression. This finding confirms the role of this protein in the development of metastasis in patients with uveal melanoma. BAP1-targeted therapies are being evaluated as treatments for some types of cancer, such as mesothelioma and renal cell carcinoma. However, further studies are needed to elucidate the role of this protein in the treatment of uveal melanoma.
BRAF plays an important role in the pathogenesis of cutaneous melanoma. Most skin melanomas harbor activating mutations in BRAF, the most prevalent form of which is the BRAF V600E mutation. 21 The BRAF V600E antibody provides highly sensitive (85–100%) and specific (90–100%) insights into the BRAF V600E mutation status.22–29 The RAF/MAPK pathway has been reported to be activated in 50% of uveal melanoma metastases. 30 The role of BRAF mutations in the pathogenesis of uveal melanoma metastasis has not been completely elucidated, and BRAF and BRAF-related molecules are not considered targets in the current treatment regimens. However, studies describing the possible effect of the BRAF mutation have been conducted. In a study by Henriquez et al. 31 examining 19 iris melanoma samples, 9 samples (48%) presented the BRAF mutation, which was associated with the presence of recurrent tumors. Zuidervaart et al. 32 investigated the BRAF mutation in 11 uveal melanoma cell lines, and a related mutation was detected in one cell line (9%). Calipel et al. 33 reported the presence of the BRAF mutation in three short-term cell cultures derived from patients with choroidal melanoma. The authors also observed a 10-fold increase in the activity of endogenous BRAF from melanoma cells compared to endogenous wild-type BRAF in normal melanocytes. Kiliç et al. 34 also reported the frequency of the BRAF mutation (9%) in a uveal melanoma cell line. Maat et al. 35 described the frequency of the BRAF mutation in both primary uveal melanoma cells and a uveal melanoma cell line (13% and 18%, respectively). OCM cell lines originate from uveal melanoma and have been used in many studies for this purpose.36,37 Malaponte et al. 38 documented the presence of the BRAF mutation in primary choroidal melanoma tissue. Janssen et al. 39 identified the BRAF mutation in 4 of 20 (20%) ciliary body and 11 of 30 (40%) choroidal melanoma samples. Furthermore, Goh et al. 40 detected the BRAF V600E mutation in 36 of 39 (92%) uveal melanoma samples. In our study, four enucleated eyes (26.7%) and one liver sample (12.5%) from patients with metastatic uveal melanoma exhibited BRAF V600E immunoreactivity, but no samples from patients with non-metastatic uveal melanoma exhibited BRAF V600E immunoreactivity. Zhao et al. 41 investigated the effect of starvation-triggered autophagy, which depends on BRAF V600E, on survival in human uveal melanoma cell lines and found that starvation-triggered autophagy prolongs cancer cell survival. In addition, vemurafenib (a BRAF V600E inhibitor) induces autophagic cell death rather than promoting cell survival in BRAF V600E-mutated uveal melanoma. Thus, the combination of an autophagy activator with a BRAF inhibitor may increase tumor cell death in patients with uveal melanoma. In our study, BRAF V600E immunoreactivity was observed in uveal melanoma.
According to Wang et al., 42 CCR7 facilitates the invasion of metastatic squamous cell carcinoma cells by activating PI3 K. Kuhnelt-Leddihn et al. 43 reported a strong correlation between high CCR7 expression and poor clinical outcomes in patients with cutaneous melanoma; however, in contrast to the results of that study, Roberts et al. 44 showed a correlation between high CCR7 expression and better clinical outcomes in patients with melanoma. The role of CCR7 in the pathogenesis and in the metastatic progression of uveal melanoma remains controversial. In our study, the expression of this protein was similar among the three groups (P = 0.136). Studies investigating the effect of CCR7 on uveal melanoma are limited. In a study conducted by van den Bosch et al. 7 with 19 patients with metastatic uveal melanoma and 30 patients with non-metastatic uveal melanoma, higher CCR7 expression was observed in patients with metastatic disease and was associated with a poor prognosis. Dobner et al. 45 investigated the effect of chemokine receptors on the metastatic progression of uveal melanoma and reported a significant association between liver metastases and the CCR7 level in blood. However, in that study, only samples obtained from patients with uveal melanoma after enucleation and transscleral resection were evaluated, and the CCR7 level in the metastatic liver samples was not determined. These differences may be attributed to differences in the sample sizes and the lack of evaluation of metastatic tissues.
Yang et al. 46 conducted a study in which metastatic uveal melanoma cells were stimulated with IFN gamma in vitro and an increase in PD-L1 expression was observed. PD-L1 expression regulates T-cell functions by suppressing IL-2 production; thus, PD-L1 blockade is a potential T cell-based therapy for the treatment of metastatic uveal melanoma. The effects of atezolizumab and avelumab, which are PD-L1 inhibitors, on the treatment of uveal melanoma are being investigated. However, Keilholz et al. 47 conducted a study of 16 patients with “ocular melanoma”, and no objective response was achieved with avelumab. Algazi et al. 3 did not observe an adequate treatment response of patients with uveal melanoma to atezolizumab. Javed et al. 48 compared the level of PD-L1 expression in metastatic uveal melanoma and cutaneous melanoma, and the level of this protein was low in metastatic uveal melanoma compared to cutaneous melanoma; the authors postulated that treatment algorithms associated with this pathway might be ineffective in this patient group. On the other hand, Rossi et al. 49 investigated the effect of pembrolizumab, a PD-1 inhibitor that interacts with PD-L1, and reported that pembrolizumab is a well-tolerated drug that produces an objective response in a small percentage of patients with metastatic uveal melanoma. In our study, PD-L1 immunoreactivity was not observed in any of the samples.
Uveal melanoma tends to undergo hematogenous metastasis. Primary melanoma cells, which express c-kit at high levels, access the general circulation by invading the tumor vasculature and then infiltrate through the sinusoidal space; thus, the adhesion of cells to the sinusoidal endothelium is promoted by the production of proinflammatory cytokines. The liver metastasis of uveal melanoma is initiated by this mechanism. However, data showing the immunohistochemical specificity of liver metastasis samples from patients with uveal melanoma are limited. In the only study evaluating immunoreactivity in a liver metastasis sample from a patient with uveal melanoma conducted by Grossniklaus, 50 HMB45 and S100 immunoreactivity, which are well-known melanoma markers, were detected in liver metastasis samples from patients with uveal melanoma. In the present study, the frequencies of HSP-27 expression and loss of BAP1 expression were higher in liver metastasis samples, suggesting that these proteins may be associated with the development of metastasis in patients with this disease. Additionally, higher BRAF V600E expression was detected in enucleated eye samples from patients with metastatic disease compared to other samples. Although BRAF is not strongly correlated with the pathogenesis of uveal melanoma, our data support the presence of BRAF immunoreactivity in uveal melanoma samples, in line with previously reported studies in the literature.31,38,39
Our study is limited by its retrospective nature, relatively small number of patients, and lack of an accompanying genetic evaluation. In addition, GNAQ/GNA11 mutation could not be performed in our study, and this situation can be dealing in samples showing BRAF V600E immunoreactivity. Further studies are needed to clarify the contribution of this expression pattern in the development of metastatic disease and to determine if they can be used as therapeutic targets.
Supplemental Material
sj-pdf-1-jbm-10.1177_03936155221088886 - Supplemental material for Evaluation of HSP-27, BAP1, BRAF V600E, CCR7, and PD-L1 expression in uveal melanoma on enucleated eyes and metastatic liver tumors
Supplemental material, sj-pdf-1-jbm-10.1177_03936155221088886 for Evaluation of HSP-27, BAP1, BRAF V600E, CCR7, and PD-L1 expression in uveal melanoma on enucleated eyes and metastatic liver tumors by Abdullah Ağın, Hayyam Kiratli, Servet Guresci, Berrin Babaoglu, Jale Karakaya and Figen Soylemezoglu in The International Journal of Biological Markers
Footnotes
Acknowledgments
This work was presented in part at the 51st Turkish Ophthalmology Association National Congress (September 24–29, 2017, Antalya, Turkey) and received the second-best research project award.
Authors’ contributions
AA, HK, SG, BB, JK, and FS designed the study, analyzed the data, drafted the initial manuscript, and had full access to all the data in the study. All authors reviewed and revised the manuscript, approved the final manuscript as submitted, and agreed to be accountable for all aspects of the work. Author contributions are consistent with the ICMJE 4 authorship criteria, and all co-authors take full responsibility for the integrity of all parts of the manuscript.
Availability of data and material
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval and consent to participate
The study protocol was approved by Hacettepe University Non-Interventional Clinical Research Ethics Board (GO 16/163), and this study was conducted in accordance with the tenets of the Declaration of Helsinki. The requirement for obtaining informed consent from participants was waived by the ethics board.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Hacettepe University (grant number THD-2016-10817).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
