Abstract
Background:
Several studies have been carried out assessing the prevalence of undernutrition and possible determinants among schoolchildren in Ethiopia, but there is a lack of systematically gathered and analyzed information.
Objective:
This systematic review and meta-analysis aimed to summarize epidemiological data on undernutrition and possible determinants among schoolchildren in Ethiopia.
Methods:
We conducted a systematic review using open access articles that report the prevalence of stunting and wasting/thinness among schoolchildren from PubMed Central, Scopus, and Science direct. The pooled prevalence was determined using a random-effect model while heterogeneities between studies were evaluated by I 2 test.
Results:
A total of 24 716 schoolchildren were included in the 39 eligible articles. The prevalence of stunting and wasting/thinness among schoolchildren in Ethiopia were 23.1% (95% CI: 19.0-27.0) and 22% (95% CI: 17-26), respectively. There was a marked difference in the prevalence of stunting and wasting/thinness across regions of Ethiopia. The risk of stunting was increased with meal frequency ≤3 times a day (odds ratio [OR] = 3.02, 95% CI: 1.90-4.14), age >10 years (OR = 2.16, 95% CI: 1.47-2.85), and family size ≥5 (OR = 1.88, 95% CI: 1.40-2.35). Similarly, the risk of wasting/thinness was increased with male sex (OR = 2.06, 95% CI: 1.54-2.58), low family income (OR = 2.16, 95% CI: 1.30-3.01), and age >10 years (OR = 1.78, 95% CI: 0.74-2.82).
Conclusion:
This study revealed that more than one-fifth of schoolchildren are stunted or wasted/thin in Ethiopia. Large family size, male sex, and student age were consistently associated with stunting and wasting/thinness among schoolchildren. This study highlights the importance of an integrated effort to reduce undernutrition in Ethiopia.
Introduction
Nutrition-related problems are one of the major problems globally, but the problem is severe in developing countries. Malnutrition and undernutrition are the 2 terms used to describe nutrition-related problems. The 2 terms are usually used interchangeably, but malnutrition is a broad term that includes undernutrition. Malnutrition refers to all deviations from the optimum body needs (it can be undernutrition or overnutrition). It is mainly caused by unbalanced, inadequate, or excessive intake of nutrients. Undernutrition refers to insufficient intake of dietary energy and nutrients that fulfill the body’s demand for optimum function. 1 Undernutrition is caused by inadequate intake of food, poor absorption, and increased losses of nutrients as a result of parasitic infection.
Undernutrition is one form of malnutrition and the most common one in low- and middle-income countries. It is one of the major causes of child morbidity and mortality in developing countries. Undernutrition manifests in the form of stunting, underweight, wasting/thinness, and deficiency of vitamins and minerals. 2 Stunting is a chronic form of undernutrition which is caused by inadequate nutrition over a long period that fails to attain optimum growth while wasting/thinness is an acute form of undernutrition that indicates a recent food shortage and/or infectious diseases that leads to rapid and severe weight loss. 3 Parasitic infection may also contribute to stunting and wasting of children as a result of poor absorption and loss of the limited available nutrients. Underweight is caused by a combination of factors, and underweight children may be stunted, wasted, or both. 2
According to the World Health Organization (WHO), stunting and wasting affect 150 million and 52 million children, respectively. 4 The problem of undernutrition is severe in sub-Saharan Africa and Southeast Asia, where more than 90% of stunted and underweight preschool children are living in the 2 regions. 5,6 The global prevalences of stunting and wasting among preschool children were 26% and 8%, respectively, in 2011. 5 Despite the millennium development goals (MDG) targeting the reduction of undernutrition, the problem is still high in sub-Saharan African countries. As stated in the 2015 MDG report, 23% of children in sub-Saharan Africa are undernourished. 7 The prevalence of child undernutrition is even higher among school-aged children. According to a recent report, stunting and thinness affecting 20% to 30% and 15% to 35% schoolchildren in developing countries, respectively. 8 Chronic undernutrition poses a serious problem in children health, physical growth, and school performance. This makes undernutrition is still one of the major problems of schoolchildren in developing countries.
Undernutrition is one of the serious health problems among children in Ethiopia, where more than half of the population is younger than 20 years. According to the 2007 population census, school-aged children (7-18 years of age) account for 34.3% of the total population of Ethiopia. 9 In line with this, the 2008 national nutritional survey indicated that 22.3% and 23.1% of schoolchildren were stunted and thin, respectively. 10 The number of published articles on the prevalence of undernutrition and possible risk factors in the country is significantly increased since the 2008 national survey. However, the prevalence of undernutrition and their potential risk factors are varied among published studies depending on locally available specific causes. To my best of knowledge, there was no summarized data on the prevalence of undernutrition and potential determinants among schoolchildren in Ethiopia. Therefore, this systematic review and meta-analysis aimed to summarize online available published studies on the prevalence of undernutrition and possible determinant factors in Ethiopia.
Methods
Children Age Category in Ethiopia
This study is conducted in Ethiopia, which is the second most populous country in Africa, with an estimated population of 105 million and area coverage of 1104, 300 km2. Of the total population, 55.6% of them are children younger than 19 years. In Ethiopia, children are supposed to enroll in primary school at the age of 7 years and spent an average of 12 years at school. The formal school structure is 4:4:2:2 in Ethiopia. The elementary school is completed in 8 years; which divide into cycles; the first cycle is from grade 1 to 4 (7-10 years) and the second cycle from grade 5 to 8 (11-14 years). The secondary education is completed in 4 years, which divide into 2 stages; high school from grade 9 to 10 (15 to 16 years) and preparatory school from grade 11 to 12 (17 to 18 years). Thus, school-aged children in Ethiopia are range from 7 to 18 years of age. Therefore, most studies included in this systematic review and meta-analysis were conducted on schoolchildren at the age of 7 to 18 years.
Anthropometric Indicators
Anthropometric indicators namely stunting, underweight, and wasting or thinness were used based on WHO 2007 growth standards. 11 The nutritional indicators were labeled as stunting (height-for-age < −2 standard deviation [SD]), underweight (weight-for-age < −2SD), and wasting/thinness (weight-for-height or body mass index (BMI)-for-age < −2SD). 3,11 Weight-for-height is applicable for children younger than 10 years to determine wasting while BMI-for-age is used for children from 5 to 19 years of age to assess children’s thinness. 11 Therefore, all articles selected and included in this meta-analysis were based on National Center for Health Statistics/WHO growth reference parameters.
Search Strategies
Relevant original articles were systematically searched from 3 online databases (PubMed Central, Scopus, and Science Direct) using the following keywords and Boolean operators: “undernutrition” OR “malnutrition” OR “acute undernutrition” OR “chronic undernutrition” OR “stunting” OR “wasting” OR “thinness” AND “Ethiopia.” Searching of relevant articles used for this meta-analysis was conducted from December 2018 to January 2019. The systematic review and selection of relevant articles were conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-analysis guidelines (Supplemental Table 1). 12
Inclusion and Exclusion Criteria
Original articles reporting the prevalence of undernutrition (stunting and wasting/thinness) and possible predictors in schoolchildren in Ethiopia were included in the study. Articles containing the prevalence of stunting, wasting/thinness, and associated risk factors along with age range of students, total study population, and study area were included for this systematic review and meta-analysis. All articles included in this meta-analysis were written in English and published between 2009 and 2018. Nutritional studies conducted on preschool children, community-based study, specific groups (only female or male students), patients, reports form review papers, or conference abstracts were excluded from this meta-analysis.
Methods of Data Extraction
Original articles were extracted from online databases using a data extraction protocol developed by the author. The data extraction protocol consists of sample size, method of participant selection, age-group, study design, study regions, year of publication, the prevalence of stunting and wasting/thinness, and risk factors of undernutrition. The summarized information was used to determine the overall prevalence of undernutrition among schoolchildren in Ethiopia.
Quality Assessment and Publication Bias
The quality of individual studies included in this meta-analysis was assessed by using Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist. 13 The checklist is used to assess internal validity (measurement biased) and external validity (selection biased) of studies included in this meta-analysis. Among the 22 STROBE items, we select 8 quality assessment parameters namely sample size, sampling methodology, response rate, statistical analysis, ethical consideration, outcome measure, confounding, and study limitation (Supplemental Table 2). Studies were assigned either 1 (if the criterion was met) or 0 (if the criterion was not met). The overall quality score was determined by adding the assigned number for each parameter and classified as low quality (≤3), medium quality (4-6), or high quality (≥7) as described elsewhere. 6 In addition, the presence of publication bias was assessed using the symmetry of funnel plot.
Statistical Analysis
The prevalence of undernutrition (stunting and wasting/thinness) was calculated by dividing the number of positive participants by the total study participants. The heterogeneity among studies used for this meta-analysis was assessed using I 2 test. 14 Heterogeneity is defined as the degree of variability across studies. The heterogeneity of the studies was classified as low, moderate, and high based on the I 2 value less than 25%, 25% to 50%, and above 50%, respectively. 15 Considerable heterogeneity was observed among the studies included in the meta-analysis. Thus, a random-effect model at 95% CI was used for estimating the overall effect. The meta-analysis was conducted using Stata software (version 14, STATA Corp), where P < .05 was considered as statistically significant.
Results
Characteristics of the Eligible Studies
A total of 358 studies about undernutrition in schoolchildren in Ethiopia were available in the selected online databases. Of those articles, 141 articles were excluded based on duplication while 112 articles were excluded during the title and abstract screening. The remaining 105 full-text articles were assessed for their eligibility. Of those, a total of 66 articles were excluded from the analysis based on specific exclusion criteria (Figure 1). The remaining 39 articles were included for this systematic review and meta-analysis. The detailed characteristic of eligible articles included in this meta-analysis was presented in Table 1.

PRISMA flow diagram of publications considered for the review on undernutrition (stunting and thinness/wasting) among schoolchildren in Ethiopia. PRISMA indicates Preferred Reporting Items for Systematic Reviews and Meta-analysis.
Characteristics of the Study Participants Included in the Eligible Articles Used for This Review.
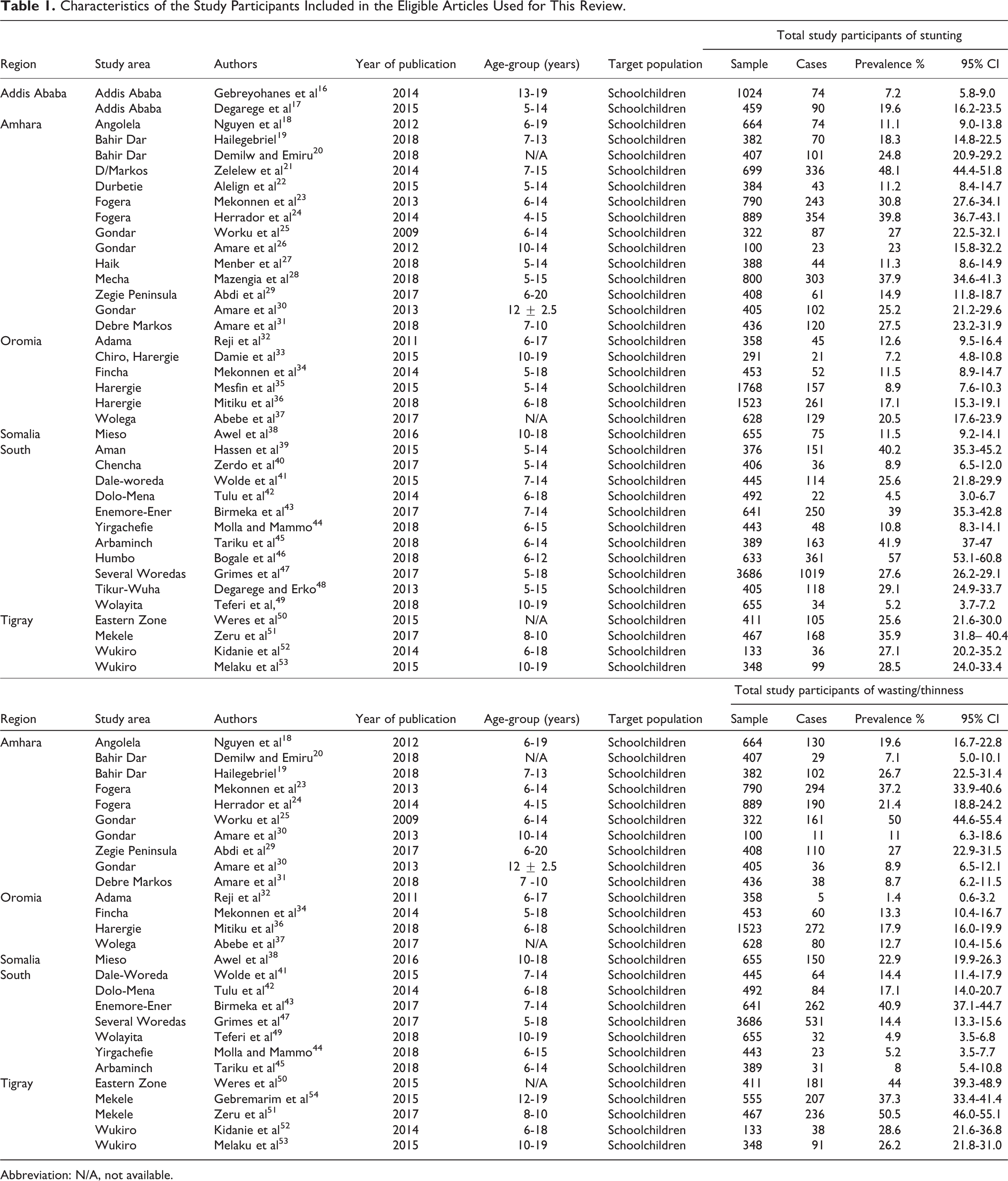
Abbreviation: N/A, not available.
The 39 eligible original articles were obtained from 5 regions (Amhara, Oromia, Somali, South Nations, and Nationalities Peoples [SNNP] and Tigray) and 1 city administration (Addis Ababa). These regions and city administration accounted for more than 95% of the total population of Ethiopia. A total of 24 716 schoolchildren were included in the 39 eligible articles. Among the eligible articles, 26 of them include data for both stunting and wasting/thinness while 13 articles treating either stunting or wasting/thinness. Therefore, 38 articles 16 -53 and 27 articles 18-20,23-26,29-32,34,36,37,38,41-45,47,49,50-54 were used for the analysis of stunting and wasting/thinness, respectively. All studies included in this meta-analysis were conducted on schoolchildren with a minimum age of 4 years and the upper limit was not mentioned in a few studies.
Quality Assessment and Possible Publication Bias
The overall quality assessment of each article included in this meta-analysis was moderate to high-quality score; 7 studies (17.9%) with moderate quality scores while 32 studies (82.1%) with high-quality scores (Supplemental Table 3). The presence of publication bias was assessed using the symmetry of funnel plot. The funnel plot (Supplemental Figures S1 and S2) indicates the presence of publication bias among studies. The cause of this bias might be associated with the difference in the criteria to select study participants and nature of study participants.
Prevalence of Stunting Among Schoolchildren in Ethiopia
The pooled prevalence of stunting was 23.1% (95% CI: 19.0-27.0) among schoolchildren in Ethiopia (Table 2 and Figure 2). The highest pooled prevalence of stunting was 29.5% (95% CI: 27.6-32.5), which was observed from the Tigray region while the lowest prevalence of stunting was 12.9% (95% CI: 8.9-16.9) obtained from the Oromia region (Table 2). Lower prevalence of stunting was observed from the Somali than other regions of Ethiopia. However, only one study was available in the region and may not be wise to compare with pooled results from other regions.
Pooled Prevalence of Stunting and Thinness/Wasting Among Schoolchildren in Ethiopia by Region.
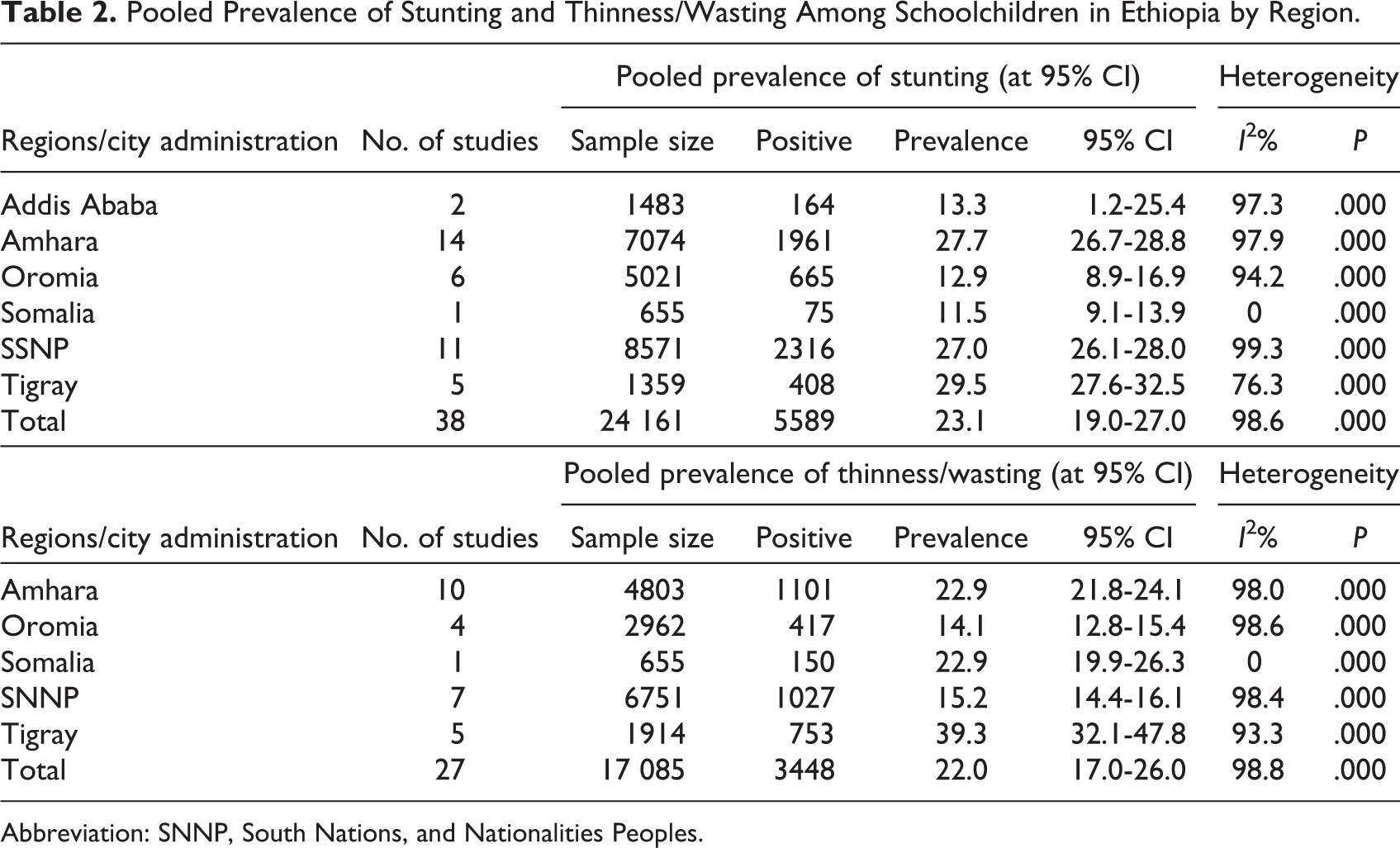
Abbreviation: SNNP, South Nations, and Nationalities Peoples.
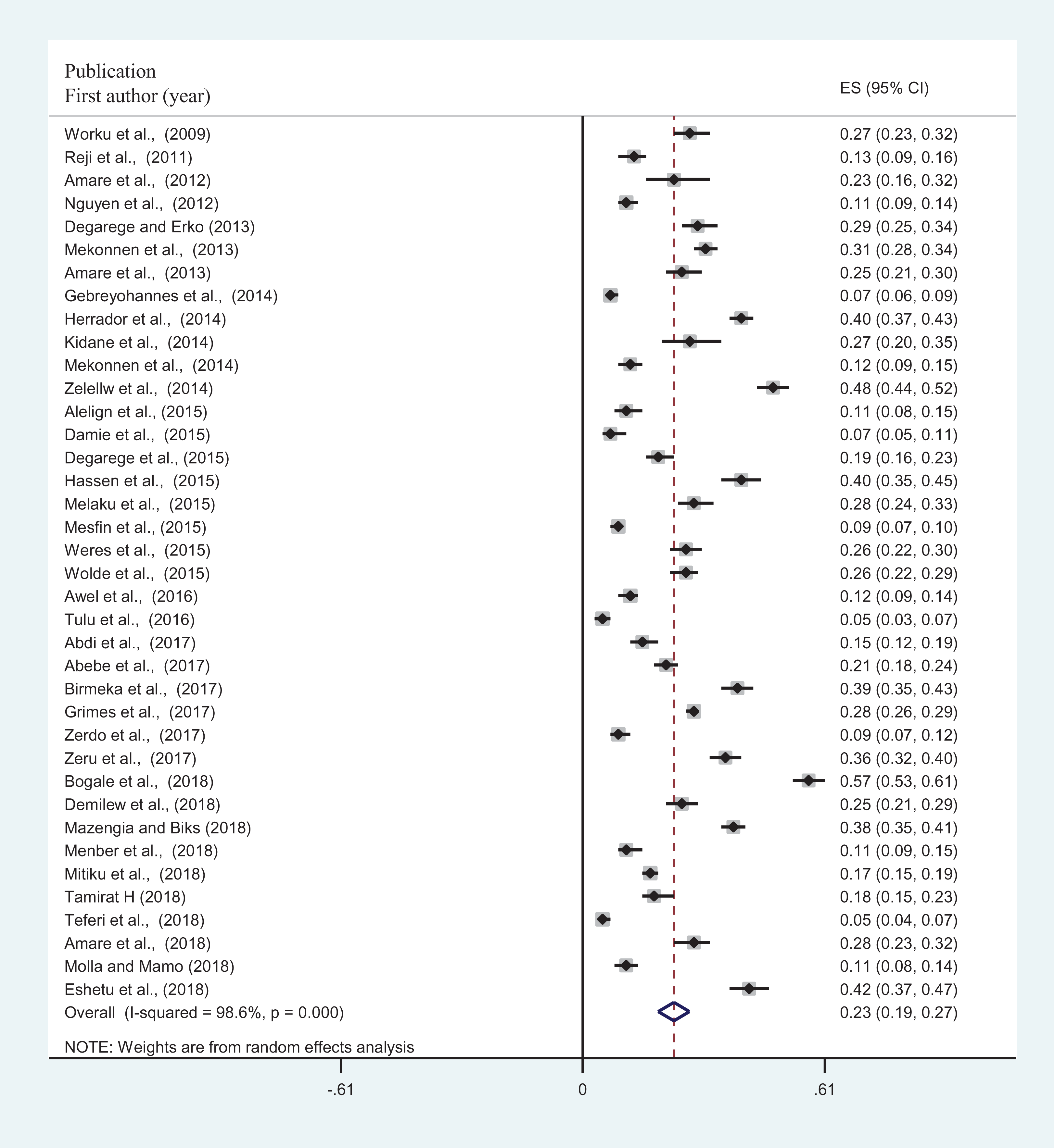
Forest plot for the prevalence of stunting among schoolchildren in Ethiopia. Each square represents effect size (ES) of individual studies and the horizontal line represents the 95% CI. The diamond indicates the pooled effect and the vertical dash lines indicate the overall estimate.
Prevalence of Thinness/Wasting Among Schoolchildren in Ethiopia
The pooled prevalence of thinness/wasting was 22% (95% CI: 17-26) among schoolchildren in Ethiopia (Table 2 and Figure 3). The overall prevalence of wasting/thinness was higher in Tigray region, 39.9% (95% CI: 32.1-47.8), followed by Amhara and Somali regions, 22.9% (95% CI: 21.8-24.1), and Somali region, 29.9% (95% CI: 19.9-26.3), while lower pooled prevalence was obtained from Oromia region, 14.1% (95% CI: 12.8-15.4; Table 2).
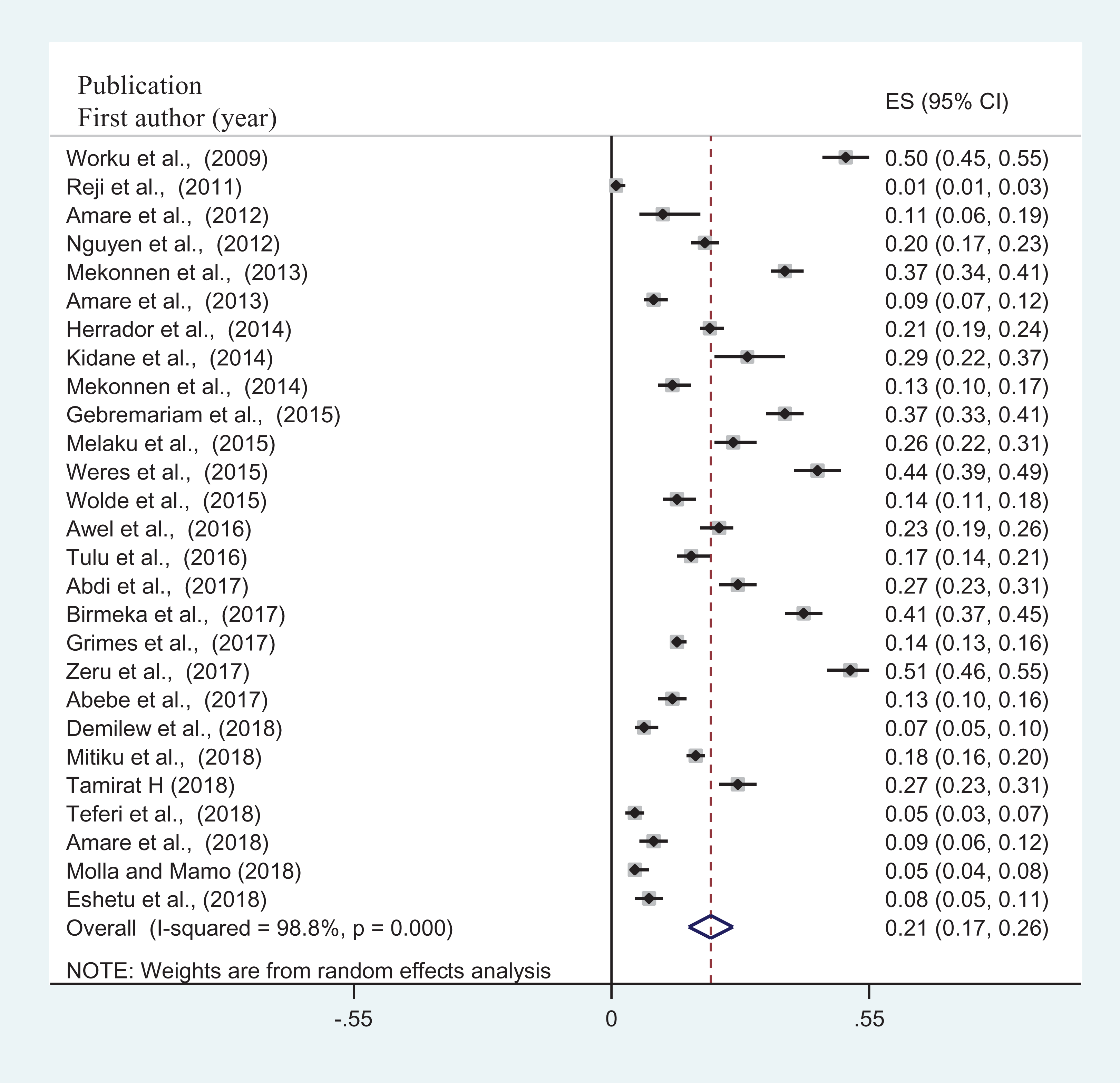
Forest plot for the prevalence of wasting/thinness among schoolchildren in Ethiopia. Each square represents effect size (ES) of individual studies, and each horizontal line represents the 95% CI. The diamond indicates the pooled effect and the vertical dash lines indicate the overall estimate.
Associated Factors of Stunting Among Schoolchildren in Ethiopia
We have reviewed and analyzed potential determinants of stunting among schoolchildren from 21 eligible articles in Ethiopia. Age and sex of the students, family size, meal frequency, mother education, rural residence, and presence of parasitic infections were associated with the stunting of schoolchildren in Ethiopia (Figure 4). The pooled results of 14 studies 21,24,28,35,36,38,39,41,44,45,46,47,49,53 showed that students older than 10 years were 2.16 times more likely to be stunted than students younger than 10 years (odds ratio [OR] = 2.16, 95% CI: 1.47-2.85; Figure 4A). The pooled results of 5 studies 17,19,20,21,38 showed that students with meal frequency 3 times or less in a day were 3.02 times more likely to be stunted as compared to students with meal frequency more than 3 times a day (OR = 3.02, 95% CI: 1.90-4.14; Figure 4B).
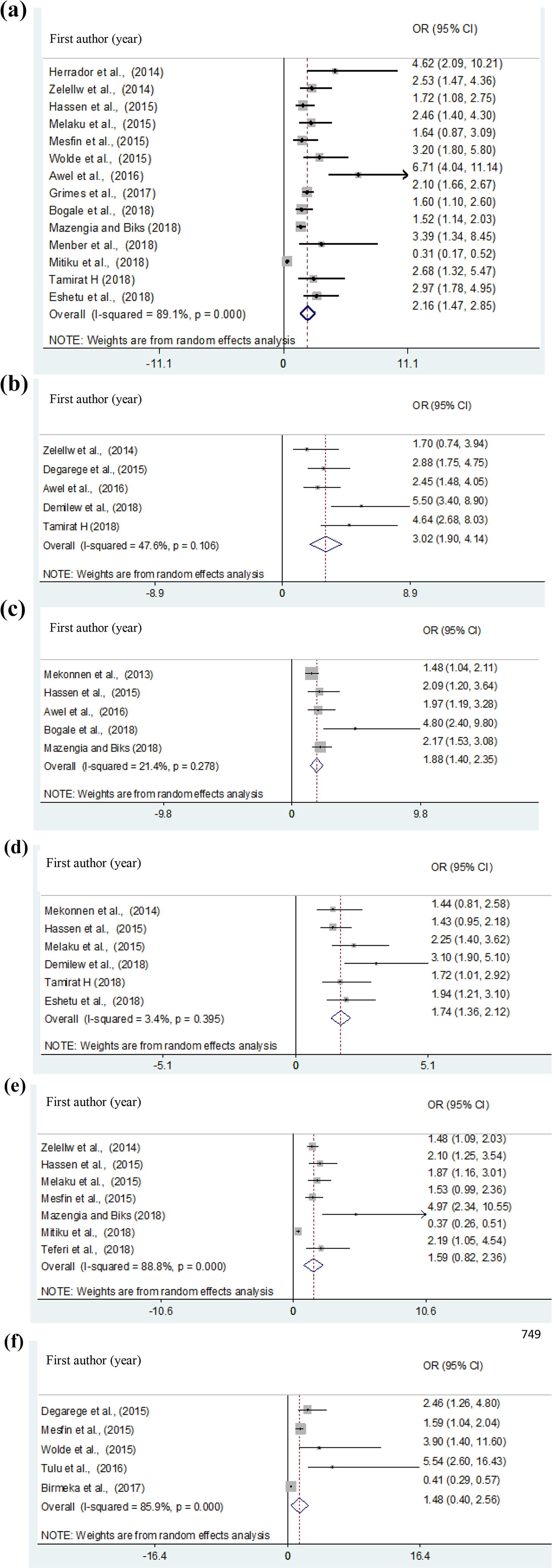
Forest plot showing the pooled odds ratio of the association between stunting and its possible determinants among schoolchildren in Ethiopia. A, age; B, meal frequency; C, family size; D, sex; E, rural residency; F, parasitic infection.
The pooled effect size of 5 studies 23,28,38,39,46 showed that students with larger family size were 1.88 times more likely develop stunting than students with small family size (OR = 1.88, 95% CI: 1.40-2.35; Figure 4C). The pooled results of 6 studies 19,20,34,39,45,53 revealed that male students were 1.74 times more stunted than female counterparts (OR = 1.74, 95% CI: 1.36-2.12; Figure 4D). The pooled effect size of 7 studies 21,28,35,36,39,49,53 indicated that students from rural residency were 1.59 more likely stunted than students from urban areas (OR = 1.59, 95% CI: 0.82-2.36; Figure 4E). Similarly, the pooled results of 5 studies 17,35,41 -43 indicated that students infected with parasite organism were 1.48 times more likely develop stunting than students without parasitic infection (OR = 1.48, 95% CI: 0.40-2.56; Figure 4F).
Associated Factors of Thinness/Wasting Among Schoolchildren in Ethiopia
We have reviewed and analyzed potential determinants of thinness/wasting among schoolchildren in Ethiopia from 13 eligible articles. Sex of students, age of students, family size, presence of parasitic infections, and family income were associated with thinness/wasting among schoolchildren in Ethiopia (Figure 5). The pooled results of 6 studies 34,47,49,50,53,54 revealed that male students were 2 times more likely to be thin/wasted than female counterparts (OR = 2.06, 95% CI: 1.54-2.58; Figure 5A). Based on the pooled results of 3 studies, 19,38,41 students living with a low family income were about 2 times more likely to be thin/wasted than students living with better income family (OR = 2.16, 95% CI: 1.30-3.01; Figure 5B).
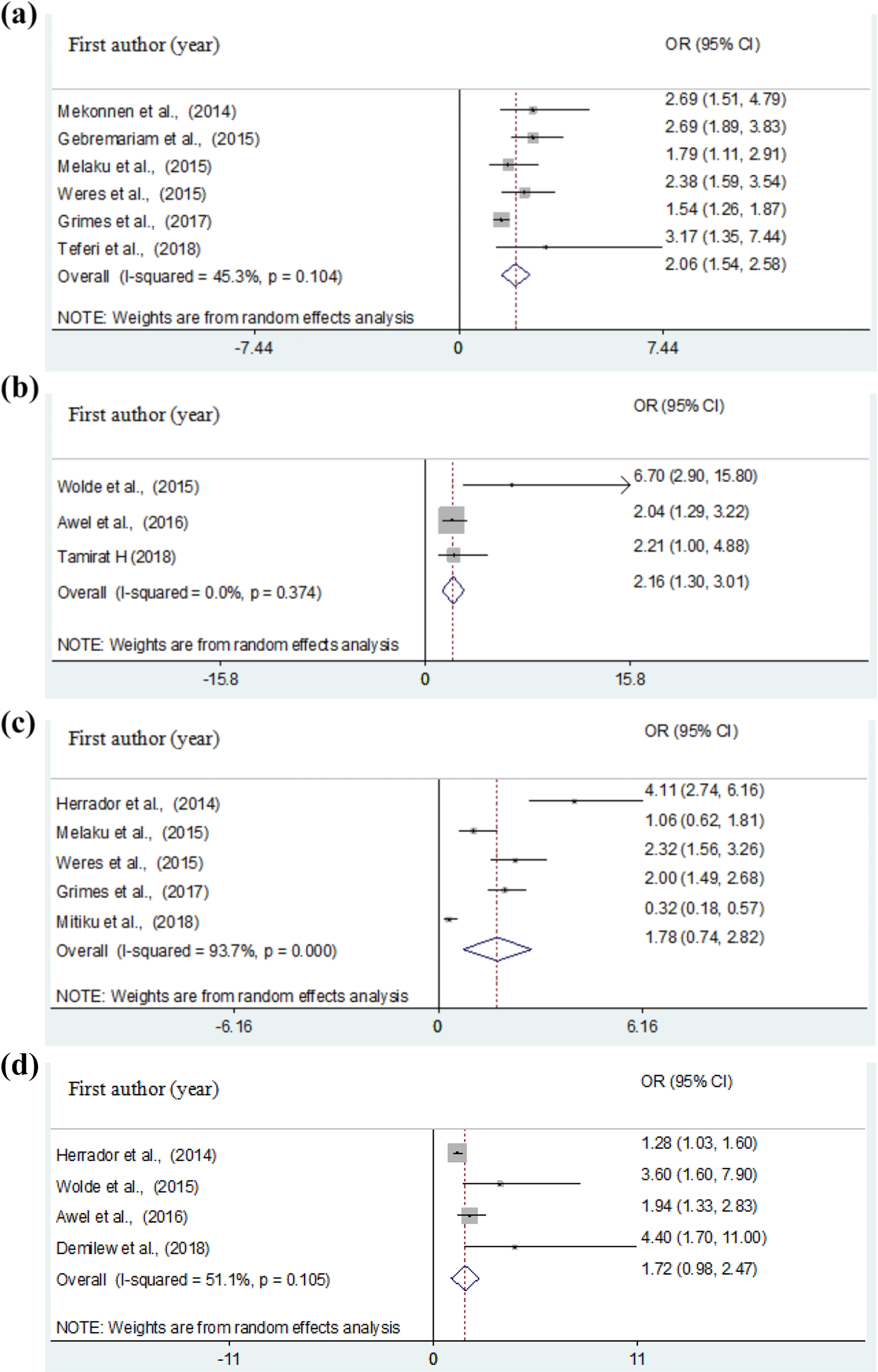
Forest plot showing the pooled odds ratio of the association between wasting/thinness and its possible determinants among schoolchildren in Ethiopia. A, Sex; B, family income; C, age; D, family size.
The pooled results of 5 studies 24,36,47,50,53 revealed that students older than 10 years were 1.78 times more likely to be thin/wasted than students younger than 10 years (OR = 1.78, 95% CI: 0.74-2.82; Figure 5C). Moreover, the pooled effect size of 4 studies 20,24,38,41 showed that students with family size above 5 were 1.72 times more likely to be thin/wasted as compared with students living with a lower family size (OR = 1.72; 95% CI: 0.98-2.47; Figure 5D).
Discussion
Child malnutrition is one of the major global problems that affect millions of children worldwide. The problem is severe in developing regions, particularly in sub-Saharan Africa and South Asia where more than 20% of children are affected by undernutrition. 55 The prevalence of childhood undernutrition is unacceptably high in Ethiopia. In line with this, the government of Ethiopia implemented the second national nutrition program from 2016 to 2020. 56 In addition, the government launched the “Seqota” Declaration in 2016 to end child undernutrition by 2030 through nutrition-specific interventions. 57 These programs aim to provide optimal complementary feeding, prevention of micronutrient deficiency, provision of safe drinking water, sanitation and hygiene (WASH), deworming of school-aged children, food fortification, and school feeding programs. These programs mainly target rural populations and low-income urban dwellers to improve health conditions and undernutrition. School-based feeding programs and deworming mainly target schoolchildren in Ethiopia.
A national survey was conducted in 2008 to determine the prevalence of undernutrition among Ethiopian children. 10 Since then, several epidemiological data are available online on the prevalence of undernutrition and possible risk factors in Ethiopia. To the best of my knowledge, this is the first systematic review and meta-analysis on undernutrition and possible determinants among schoolchildren in Ethiopia. Summarized information is important to determine the overall prevalence of undernutrition, which helps to evaluate the ongoing intervention strategies as well as to identify areas change by policy-makers.
The pooled prevalence of stunting among schoolchildren in the present study is similar to the 22.3% prevalence reported in the 2008 national survey in Ethiopia, 10 22% from African countries average, 8 and 21.7% among young adolescent in Africa. 58 However, the pooled prevalence of stunting in this study was lower than 35% reported in a meta-analysis from schoolchildren in Karnataka, India, 59 and 60% from Bangladesh. 60 Despite the ongoing intervention strategies, the prevalence of stunting is still high in Ethiopia. Stunting is a result of chronic and recurrent undernutrition associated with inadequate and inappropriate food intake as well as frequent illness in early life. The Ethiopian government implements the Seqota declaration to end childhood stunting from Amhara and Tigray regions by the year 2030. Integrated efforts are needed to address the underline causes of stunting at childhood in the country.
The pooled prevalence of thinness/wasting among schoolchildren in Ethiopia is similar to that of the 2008 national survey. 10 However, the present finding was low as compared with 36% reported from a meta-analysis in Africa 8 and 28% from India. 59 The high prevalence of thinness and wasting might be linked with low family income. Wasting and thinness are an acute form of undernutrition directly associated with family monthly income, which determines the meal frequency, dietary diversity, and provision of appropriate medication on time during infection. The Ethiopian government and other stakeholders are working on food supplementation through school feeding programs for selected schools. School feeding programs are known to bring a positive impact on student’s school attendance, academic performance, as well as physical growth. 61 The government should expand the coverage of the ongoing school feeding programs to alleviate acute malnutrition in Ethiopia.
This study revealed that there are marked differences in the prevalence of stunting and wasting/thinness across regions of Ethiopia. The pooled prevalence of stunting was higher in Tigray, Amhara, and SNNP regions than other regions of Ethiopia. Similarly, the pooled prevalence of wasting/thinness was higher in Tigray, Amhara, and Somalia regions than other regions of Ethiopia. The high prevalence of undernutrition in Tigray, Amhara, and Somali regions might be associated with recurrent drought and insufficient food production. In addition, sociodemographic and cultural differences and variation in the number of studies published from each region may contribute to the difference in the prevalence of undernutrition in Ethiopia. Moreover, the high prevalence of wasting/thinness and lower prevalence of stunting observed in Somali region may be related to body shape. Children from the pastoral community of Somali tend to have longer limbs and lower sitting-to-standing ratio than children from Amhara region. 62 Studies reported from Somalia showed that the WHO standards weight-for-height (WHZ) and height-for age (HAZ) may underestimate stunting 63 and overestimate acute malnutrition 62 in Somalia children. The government and other stakeholders should give priority for implementing nutrition-specific intervention strategies of the Seqota declaration for regions with high prevalence of stunting and wasting/thinness.
We reviewed and analyzed risk factors associated with stunting and wasting/thinness of schoolchildren addressed by selected articles for this meta-analysis. The risks of developing childhood stunting and wasting/thinness were consistently associated with male sex, age above 10 years, and living with larger family size (above 5). The contributions of these factors to stunting and wasting/thinness were reported in a meta-analysis from sub-Saharan African countries. 6
The risk of developing stunting was higher among children taking a meal 3 or less in a day compared to their counterparts. It is known that meal frequency is directly associated with family income. Children living in an area where there is a problem of food shortage and low family income may have a higher chance of being stunted and underweight. 64 The levels of family income dictate the provision of a balanced diet as well as the optimum frequency of meals to their children. Long-term exposure for food shortage early in life leads to chronic undernutrition namely stunting. The level of meal frequency at early childhood plays a vital role in their physical growth and development.
This study revealed that the risk of stunting and wasting/thinness was higher among male children compared with female counterparts. This result is in line with several studies in sub-Saharan Africa. 6,58,65,66 This variation might be associated with differences in physical activity between male and female children in the region. In most sub-Saharan African countries, male children help their parents through involvement in energy-demanding on-farm and off-farm activities. Besides, male children are more physically active than their female counterpart particularly during childhood. 67 As a result, male children may lose their energy needed for normal growth and other physiological activities that may lead to thinness and stunting. The problem is more severe if this energy loss is accompanying by low meal frequency and a minimum diet.
The risk of stunting and wasting/thinness was higher among students older than 10 years compared with lower age-groups, which is in line with a meta-analysis reported from Iran 64 and sub-Saharan Africa. 6 Higher risk of stunting was reported from boys than girls at older ages from Tanzania, 68 Burkina Faso, 69 and Uganda. 66 In many African countries, older age children particularly males are involved in energy-demanding on-farm activities. Low-meal frequencies accompanied by several outdoor activities make male and older children vulnerable for undernutrition, especially for stunting and thinness.
There was a remarkable difference in undernutrition between children living within small and larger family size. The odds of being stunted and wasted/thin were higher in children living with a larger family size than those living with small family size. Children living within a large family size are exposed to nutritional-related problems due to shortage of adequate diet, poor living, and health conditions. Ethiopia is one of the sub-Saharan African countries known in large family size, which predispose children to nutritional-related problems. The contribution of large family size and low income to childhood undernutrition were reported in Pakistan 70 and sub-Saharan Africa. 6
The presence of parasitic infections increased the risk of stunting among schoolchildren in Ethiopia. Chronic parasitic infection particularly helminths are contributing to childhood undernutrition by competing for the available limited nutrients. 71 Conversely, malnourished children are susceptible to parasitic infections, which further aggravate the level of undernutrition. 72 The positive associations of soil-transmitted helminths and undernutrition were reported elsewhere. 73,74 School-aged children are vulnerable for parasitic infection due to poor environmental sanitation, low level of personal hygiene, unprotected drinking water, and poor awareness of their families. The government and other stakeholders need to expand the ongoing deworming and WASH programs to school-aged children in high-risk regions of the country.
This review revealed that children living in rural areas are at higher risk of stunting than children living in urban areas in Ethiopia. A similar association of stunting and rural residency was reported from adolescent 75 and preschool children in Ethiopia. 76,77 The high prevalence of stunting in a rural setting might be associated with larger family size, low level of environmental sanitation, limited access for pure drinking water and health facilities, low level of awareness about balanced diet, and optimum feeding of children. In addition, several studies indicated that there are high parasitic infections in rural than urban areas of Ethiopia. 78,79,80 Despite remarkable progress on water and sanitation programs observed in recent years, only 42% of rural residents obtain pure drinking water, and 35.6% practice open defecation in Ethiopia. 81 Therefore, the national WASH programs need to scale up to address all parts of Ethiopia, particularly rural and remote areas.
Significance/Contribution
Exposures of undernutrition during childhood are affecting health, physical growth, mental development, work capacity, and quality of life during the entire life span of an individual. Therefore, assessments of the nutritional status of schoolchildren are essential tools for policymakers to design appropriate intervention strategies. This study determines the pooled prevalence of stunting, wasting/thinness, major risk factors, and potential target regions for intervention in the country.
Strength and Limitations
This study provides the pooled prevalence of stunting and wasting/thinness among schoolchildren in Ethiopia. The present study identifies variations of stunting and wasting/thinness in schoolchildren across regional states in Ethiopia. This study also identifies major risk factors associated with stunting and wasting/thinness in Ethiopia, which are important intervention areas for policymakers. Despite these strengths, it also has a few limitations. First, this meta-analysis did not include underweight among schoolchildren due to the lack of consistency among the parameters used in the selected articles for this review. Second, the numbers of articles used in this study were not uniformly distributed across regions in the country. Third, the present study did not show the level of variation of stunting and wasting/thinness between sexes.
Conclusion
This study revealed that more than one-fifth of schoolchildren are still stunted or wasted/thin in Ethiopia. The present study identified several risk factors associated with stunting and wasting/thinness of school children in the country. Childhood stunting and wasting/thinness are consistently associated with male sex, age above 10 years and family size above 5. These risk factors might be important intervention areas for change by policymakers in the country. In addition, the finding of this review highlights the importance of integrated efforts to scale up the ongoing school feeding, WASH, and school-based deworming programs for schoolchildren in Ethiopia.
Supplemental Material
Supplemental Material, Funnel_plot_showing_possible_publication_bias_for_thinness - Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, Funnel_plot_showing_possible_publication_bias_for_thinness for Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, Funnel_plot_showing_publication_bias_for_stuning_and_associated_risk_factors - Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, Funnel_plot_showing_publication_bias_for_stuning_and_associated_risk_factors for Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, PRISMA_checklist_S1_table - Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, PRISMA_checklist_S1_table for Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, Quality_assessement_S2_table - Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, Quality_assessement_S2_table for Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, Quality_assessement_S3_table - Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis
Supplemental Material, Quality_assessement_S3_table for Prevalence and Determinants of Stunting and Thinness/Wasting Among Schoolchildren of Ethiopia: A Systematic Review and Meta-Analysis by Tamirat Hailegebriel in Food and Nutrition Bulletin
Footnotes
Author’s Note
Tamirat Hailegebriel was involved in designing; conducting the review, data analysis, interpretation of the findings; and drafting the manuscript. The author declared that this review article is his original work, and this manuscript is not submitted to other journals elsewhere. The author declared that there is no conflict of interest.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
