Abstract
Background:
Food insecurity (FI) is an important public health issue for US veterans. For many veterans, civilian life is fraught with service-incurred health issues and socioeconomic challenges, each risk factors for FI. The FI literature on veterans is limited due to insufficient coverage of the topic’s complexity and the methods used to study it in this population. No published analysis has evaluated how FI has been examined in US veterans.
Objectives:
We assessed how FI has been examined in US military veterans by identifying (1) the major content areas, or domains, studied in association with FI and (2) the existing research gaps.
Methods:
A scoping literature review was conducted to map the main research domains of the FI literature and identify knowledge gaps. Electronic database and hand searches identified potentially relevant studies (n = 61). Data extraction, utilizing a standardized set of design parameters, was completed. Duplicate removal and application of inclusion/exclusion criteria resulted in the studies (n = 21) selected for critical review.
Results:
Eight research domains were determined: FI prevalence, health status, dietary practices, health care utilization, economic instability, homelessness/housing instability, food program participation, and community/emergency preparedness—the most dominant was health status and the least dominant were social determinants (ie, homelessness/housing instability, food program participation). Research on validity and usability of FI assessment methods in veterans was virtually absent. Military service factors, longitudinal effects, FI among women, intervention effectiveness, and other areas lacked sufficient inquiry.
Conclusion:
Research is required on lesser examined content areas and methodology to optimize surveillance and policy for veteran FI.
Introduction
Although the US food supply is varied and may provide the nutrients for maintaining health, food may not always be available in sufficient quantity or quality to meet the dietary requirements for some individuals or households. The inability for people to obtain sufficient and nutritious food at all times and in socially acceptable ways is termed food insecurity (FI), 1 -3 which has strong social and economic underpinnings and is a highly complex issue that goes well beyond food. 3,4
Various factors relate to higher FI risk in the general population 5 -15 and may even be more prevalent in the veteran population. Notably, veterans have on average poorer health and health behaviors than do civilians. 16 -19 They also represent a greater proportion of the US homeless population compared to civilians. 20 -23 Veterans are at high risk of post-traumatic stress disorder 19 , substance abuse, 17,24 and other mental health conditions, 25 which increase the risk of functional disability. Mental and physical health status affect workforce participation, 26 which impacts income and thus food affordability. Younger veterans who are transitioning from recent conflicts may be at higher risk of FI than older veterans because their entry into the workforce postservice may be limited by fewer years of employment preservice 27 or less time in receipt of military benefits. Veterans residing in rural areas or low-income urban areas may have less access to nutritious food due to a higher prevalence of food deserts (ie, areas with little availability to nutritious food) 28 in their communities or due to absent or reduced transportation that makes travel to locations where food may be more available and varied less likely.
Less support from federal food assistance programs is another factor that may increase FI risk among veterans. The US Department of Agriculture’s (USDA) Supplemental Nutrition Assistance Program (SNAP), formerly the Food Stamp Program, has been cut over time. 29,30 This is partly due to recent legislative actions that changed work requirements and consequently SNAP eligibility. 29 Barriers to participation also exist, such as the lack of knowledge about SNAP and the stigma of program participation, 31 issues that may be more evident among veterans because of beliefs about self-reliance that may have developed while in military service. 32
Because of FI’s importance as a public health issue and its limited examination in US veterans, the objective of this report was to determine how FI has been investigated in this population and to speak to research areas that may have been underaddressed to date. This was accomplished using a scoping literature review, 33,34 which helps map the broad research domains underlying the literature on topics that have not been comprehensively addressed before and to identify major knowledge gaps. 33,35,36
Methods
A scoping review was conducted using an extension of the PRISMA guidelines originally developed for systematic literature reviews. 33 -35 Systematic description and critical synthesis of the research in each of the domains was completed based on the following: (1) conduct of an initial, limited review of the literature to develop search terms from study titles and abstracts and to develop a listing of study extraction fields; (2) completion of a more exhaustive review of electronic databases using the previously compiled search terms; (3) review of reference lists of the resulting studies to identify other sources of relevant information; (4) extraction and charting of study details; (5) final selection of studies meeting search criteria and research objectives; and (6) classification of the domains of research. The dominant domain of each study was identified by the authors based on what they interpreted to be its central focus.
Study Search Methodology
An initial electronic search of MEDLINE in 2016 resulted in 14 articles that were used to develop search criteria and extraction variables for charting. This limited search was then supplemented by a series of electronic citation searches, spanning literature between 1946 and 2019 and using criteria established from the initial query. Searches were performed between January and December 2019 on the following bibliographic databases: MEDLINE (PubMed), Web of Science, Social Work Reference Center, Psychological and Behavioral Science Collection, PsychINFO, CINAHL, and Scopus. Reference lists for each of the collected articles were reviewed for additional, relevant research, and journals were hand-searched for studies not yet identified. 33 A listing of the studies found was developed and information was tabulated from each using the following extraction fields: author (last name of first author); publication year; if FI was addressed; study population; library database; major focus/theme; research design/methodology; measures of FI or other outcomes; measures of veteran status or other key variables; major results; and limitations. Further refinement of the study listing involved removal of duplicate articles (those identified in more than 1 database), written formats that did not represent original research (ie, commentaries, systematic or other literature reviews), and articles that did not explicitly address FI in US veterans.
Inclusion and exclusion search criteria
Inclusion criteria for the search were “food insecurity,” “food scarcity,” “veterans,” “military,” “food restriction,” “hunger,” “food insufficiency,” and “food availability.” The specific, FI-related terms used were those frequently cited in FI studies. Common terms reportedly related to FI or conflated with it 1 were food insufficiency (“an inadequate amount of food intake due to insufficient money or other resources”), 1,15,37 hunger (“the uneasy or painful sensation caused by a lack of food or the recurrent and involuntary lack of access to food”—the extreme end of FI), 2,38 food scarcity, 15,39 food restriction, 40 and food availability. 1,4,15,41 Focus was placed on studies of individual US veterans or veteran households. Exclusion included restriction to published peer-reviewed journal articles and only those in English.
Gray literature (ie, theses, conference proceedings, bibliographies, technical and commercial documentation, government reports and documents, and unpublished materials acquired through contact with researchers having knowledge of a specified topic) 42 was not systematically searched. However, it still represented a substantial portion of information highly central to this review that was obtained mainly through article bibliographies, Internet searches, and personal communications. 3,11,15,27– 29,31,38,43 -50 Further searching of gray literature was not performed because the emphasis here was on peer-reviewed evidence meeting quality criteria for publication by expert, external reviewers. Gray literature does not always meet such standards, and its benefits for inclusion have been deemed by some to be debatable. 51 There is no limit to the amount of gray literature that is currently available, which extends to a wide range of “gray data” and “gray information” 52 in the form of written (eg, blogs, tweets, Facebook status updates, emails, meeting notes) and unwritten materials (eg, podcasts, video clips), 52,53 making the time and other resources needed for this type of investigation indeterminable.
Study selection and classification
Sixty-one studies were initially identified and reviewed (Figure 1). Of these, 12 duplicate articles were removed because they were found in more than 1 database. An additional 28 articles were removed because they did not address FI in veterans (eg, targeted active military, facilities, nonveterans), 54 -56 were commentaries 57 or reviews of less directly related topics, such as eating disorders, 58 or focused on veterans from other countries. 59 This left 21 studies for final review and classification.
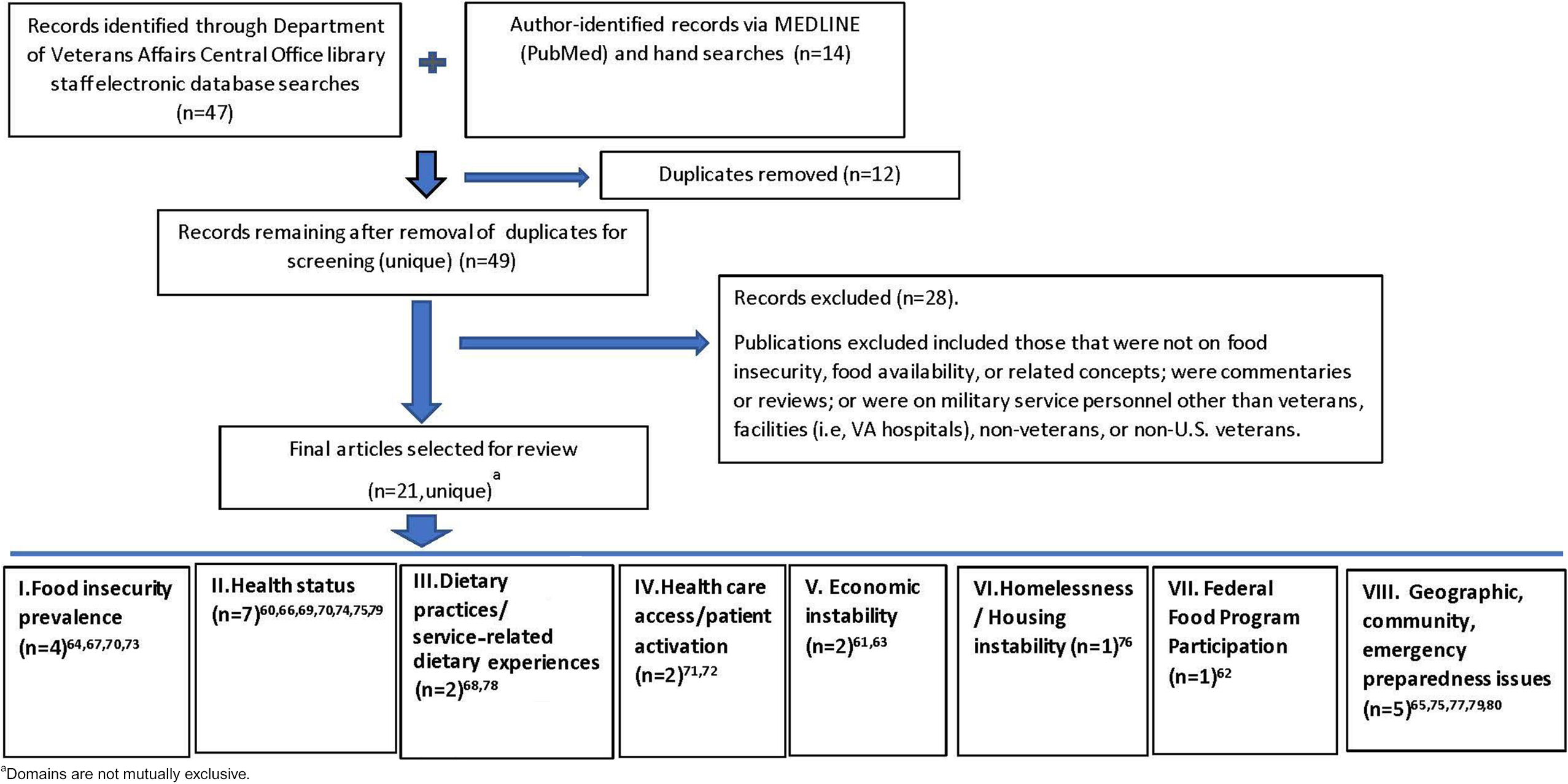
Flowchart of process for publication identification and review.
Resultant articles were classified into major conceptual areas (domains) by the authors, and results were charted and illustrated in a flowchart (Figure 1). Basic characteristics for research falling into each of 8 domains are summarized in Table 1. Domains were not mutually exclusive; therefore, the number of studies summed across all domains does not equal the number of unique articles identified. Some domains viewed as being minimally researched and highly relevant, such as “homelessness” or “federal food program participation,” were classified separately even though they could map to other content areas like economic instability. In contrast, the mention of a particular content area for a study did not always signify that the study was included in a domain. For example, Schure et al 60 examined FI and housing insecurity and their association with poor physical and mental health status using regression, but the regression model testing FI did not include housing insecurity as a covariate. Lastly, prevalence is primarily presented for those studies with a major focus on prevalence.
Purpose, Sample, Data Source, and Food Insecurity Measure in 21 Studies of US Veterans.
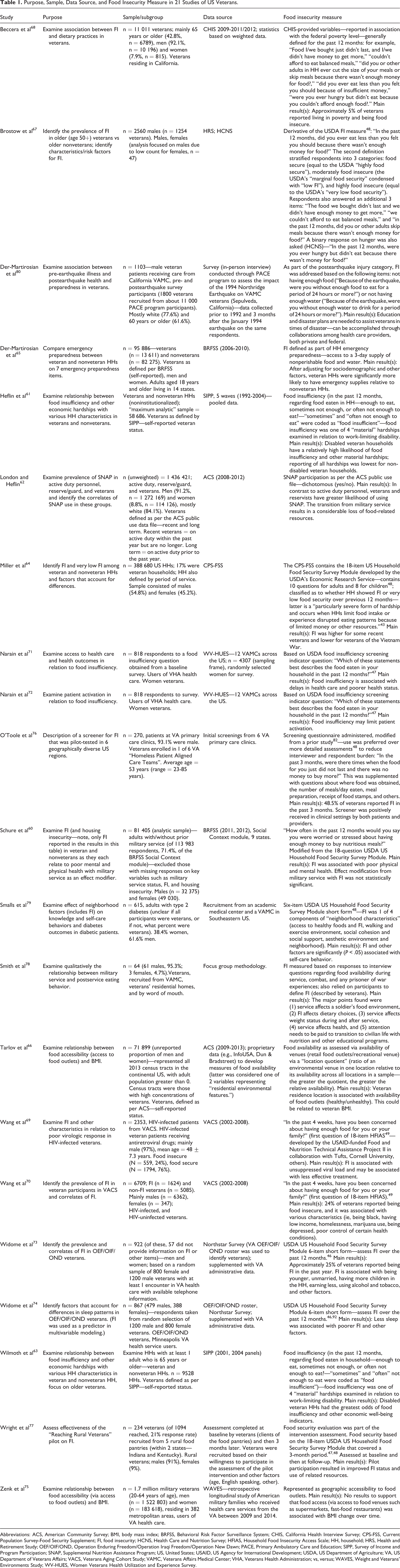
Abbreviations: ACS, American Community Survey; BMI, body mass index; BRFSS, Behavioral Risk Factor Surveillance System; CHIS, California Health Interview Survey; CPS-FSS, Current Population Survey-Food Security Supplement; FI, food insecurity; HCNS, Health Care and Nutrition Survey; HFIAS, Household Food Insecurity Access Scale; HH, household; HRS, Health and Retirement Study; OEF/OIF/OND, Operation Enduring Freedom/Operation Iraqi Freedom/Operation New Dawn; PACE, Primary Ambulatory Care and Education; SIPP, Survey of Income and Program Participation; SNAP, Supplemental Nutrition Assistance Program; US, United States; USAID, US Agency for International Development; USDA, US Department of Agriculture; VA, US Department of Veterans Affairs; VACS, Veterans Aging Cohort Study; VAMC, Veterans Affairs Medical Center; VHA, Veterans Health Administration; vs, versus; WAVES, Weight and Veterans’ Environments Study; WV-HUES, Women Veterans Health Utilization and Experience Survey.
Results
The remaining 21 articles (Table 1) were published roughly in the past decade and most within the past 5 years. Most of the selected studies relied on surveys—8 analyzed data from nationwide, population-based federal surveys, or surveys supported by the federal government, including the Survey of Income and Program Participation (SIPP; US Census Bureau; n = 2), 61,63 the Current Population Survey (CPS; US Census Bureau; n = 1), 64 the Behavioral Risk Factor Surveillance System survey (BRFSS; US Department of Health and Human Services; n = 2), 60,65 the American Community Survey (ACS; US Census Bureau; n = 2), 62,66 and the Health and Retirement Study (HRS; University of Michigan Institute for Social Research; n = 1). 67 Findings from one study were based on data from a survey of California state residents. 68 In contrast, 7 publications reported on surveys specifically designed for veterans such as the Veterans Aging Cohort Study (VACS), 69,70 the Women Veterans Health Utilization and Experience Survey (WV-HUES), 71,72 the Northstar Survey, 73,74 and the Weight and Veterans’ Environments Study 75 —all involved users of Department of Veterans Affairs (VA) health care. Two studies piloted approaches to examining FI in veterans, 76,77 while another qualitatively examined FI and related issues using focus group methods. 78 Longitudinal survey data were cited as data sources in some reports—either a single wave of data was evaluated or pooled or multiple years of data were used. 61 -64,66,67 One study assessed changes in body mass index (BMI) and food outlet access over time. 75
Eight central themes were dominant (Figure 1): (1) FI prevalence in veterans (n = 4), 64,67,70,73 (2) health status (n = 7), 60,66,69,70,74,75,79 (3) dietary practices/service-related dietary experiences (n = 2), 68,78 (4) health care utilization (n = 2), 71,72 (5) economic instability (n = 2), 61,63 (6) homelessness/housing instability (n = 1), 76 (7) federal food program participation (n = 1), 62 and (8) community and emergency preparedness factors (n = 5). 65,75,77,79,80 Health status was the most dominant domain, while food program participation and homelessness/housing instability were the least dominant (Figure 2).
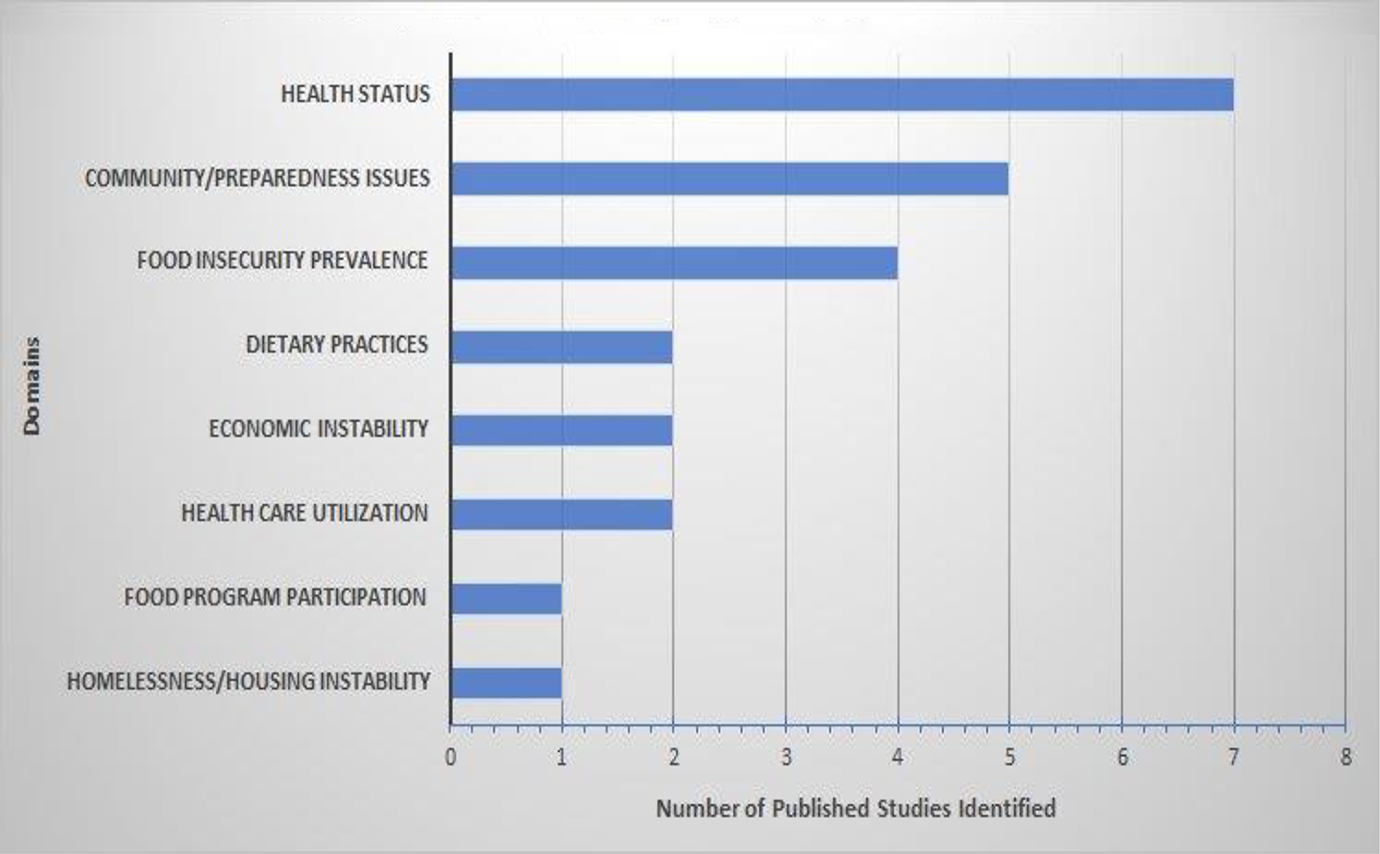
Research domains in the food insecurity literature, US veterans.
Food Insecurity Prevalence in Veterans
Four studies, published between 2015 and 2017, mainly examined FI prevalence and its correlates. Two studies used data from large-scale surveys designed for the general US adult population, 64,67 while the remaining 2 studies administered surveys that specifically targeted veterans. 70,73
Methodologies and study populations differed among them—one was based on a comparison of veterans (any conflict) versus civilians using the Census Bureau’s CPS data for US households, 64 while another examined Operation Enduring Freedom/Operation Iraqi Freedom/Operation New Dawn (OEF/OIF/OND) male and female veterans between 33 and 35.5 years (mean) of age who used the Minneapolis VA Health Care System (Northstar Survey). 73 A third study surveyed veterans of any conflict who were 50 years or older and who participated in the University of Michigan’s HRS and Health Care and Nutrition Survey (HCNS). 67 The last, conducted by Wang et al, 70 investigated the prevalence of FI in participants of the VACS—veterans who have accessed VA health care and were either HIV infected or not.
All 4 studies used different FI assessments. Miller et al 64 used the “CPS - Food Security Supplement” (CPS-FSS), which contains the full 18-item USDA US Household Food Security Survey Module (HFSSM). 48 Brostow et al 67 used questions from the HCNS that were similar to but not as extensive as the HFSSM, while Widome et al 73 utilized a 6-item version 46 of the full USDA module to examine “food security,” defined as “high/marginal” (no food access problems or some anxiety over food insufficiency with little or no impact on diet), “low” (reduced diet quality with little or no reduced intake), and “very low” (multiple occasions with impacted eating and food intake). In contrast, Wang et al 70 used a broad FI measure that was derived from the first question of the 9-item US Agency for International Development–sponsored Household Food Insecurity Access Scale (HFIAS). 49
The extent of military service characteristics that was reported in relation to FI prevalence varied. Widome et al 73 provided prevalence estimates of FI by military pay grade, service-connected disability, and the number of deployments, while fewer service factors were addressed in the remaining studies. 64,67,70 Brostow et al 67 reported prevalence for military pension benefits stratified by veterans status, “food security” status, and age group. Wang et al 70 reported on FI prevalence among veterans in VACS, and Miller et al 64 reported on FI level by service period.
The prevalence estimates of FI from these studies varied from approximately 3% to over 20% depending on veteran characteristic (Table 2). Among male veterans,
67
FI was 3.7% (95% CI: 2.3, 5.1) for those 65 years or older and 11.5% (95% CI: 7.0, 16.0) for men less than 65 years (
Studies Targeting FI Prevalence.a

Abbreviations: CI, confidence interval; FI, food insecurity; HFI, high food insecurity; H/M, high/marginal; L, low; MFI, moderate food insecurity; OEF/OIF/OND, Operation Enduring Freedom/Operation Iraqi Freedom/Operation New Dawn; PHQ-9, Patient Health Questionnaire-9 (Spitzer RL et al. 1999. Validation and utility of a self-report version of the PRIME-MD. The PHQ Primary Care Study.
a FI terms refer to those reported by studies’ authors. Statistics for selected characteristics are reported.
b%(95% CI).
Miller et al 64 compared the adjusted odds of FI between veterans and nonveterans and found no difference by veteran status. Recent veterans, however, and those who served during the Vietnam War had the highest risk of FI. Brostow et al 67 found that veteran age resulted in different correlates of FI that spanned various physical and mental health conditions and behaviors. Widome et al 73 found that lower incomes, households with children, and certain health behaviors were associated with “food security level” in veterans (“food security” and FI were terms used in this study; food security was defined as the inverse of FI). Other characteristics related to FI 70 were unemployment, homelessness, and drug use.
All 4 studies included men and women, but for most studies, 64,67,70 FI prevalence estimates for women were absent or not optimal. Forty-seven women were in the sample in one study, 67 but the count of women was too low to draw any meaningful results, so major analyses focused on men. Miller et al 64 reported that 45% of the sample was women, but FI statistics did not distinguish between female veterans and nonveterans (the variable “female” was applied to the “head of households in nonveteran homes or veterans with the most recent service in veteran homes”). Wang et al 70 reported prevalence for both men and women, but the sample was restricted to users of VA health care and HIV-infected/uninfected veterans.
Health Status
Study of the relationship between FI and health status was the dominant domain resulting from this review and represented one-third of the 21 studies identified. 60,66,69,70,74,75,79 Some of the veteran samples that were studied focused on specific subpopulations of veterans, 69,70,74,79 whereas others relied on broader veteran samples. 60,66,75 Most had samples containing men and women, 60,69,70,74,75,79 but FI statistics were not reported by gender for all. 60,66,69,74,79
The relationship between FI and mental and physical health was tested using 2011 to 2012 BRFSS data in US adults who either did or did not have prior military service. 60 In that study, an FI question was derived from the 18-item USDA module. 38 Schure et al 60 found that FI was significantly associated with poor mental (adjusted odds ratio [aOR] = 3.47, 95% CI: 3.18, 3.77) and physical health (aOR = 3.21, 95% CI: 2.92, 3.53) after controlling for various socioeconomic characteristics. Wang et al 70 investigated whether FI as an outcome was associated with HIV status and other health and socioeconomic factors in VACS participants 69 using the HFIAS. 49 The question used in the VACS analysis asked how frequently an individual felt worried or stressed about having enough money to purchase nutritious meals. Poor control of HIV, in addition to poor control of comorbidities such as hypertension and diabetes, was related to FI as well as other factors such as drug use, homelessness, and income and minority status. Earlier research by the same investigator on HIV status and FI showed similar results. 69 Widome et al 74 reported on the relationship between sleep duration and various characteristics, including FI in VHA users, where high, marginal, low, and very low “food security” were evaluated using the 6-item USDA HFSSM short form. 46,48
Smalls et al
79
examined the association between diabetes care behaviors in VHA health care users (n = 615, diabetics) and neighborhood characteristics (eg, attractiveness, noise, recreational access) that included access to healthy food and FI as measured by a 6-item USDA household FI measure.
48
Food insecurity, which was evaluated as one of a range of covariates, was significantly (
Dietary Practices
Two studies 68,78 predominantly examined food patterns and eating behaviors. Both collected data from specific veteran subgroups—one from veterans (95.3% male) recruited from VA medical centers (VAMCs) and other sources 78 and the other from a survey administered to veterans residing in California. 68
Beccera et al 68 studied the relationship between dietary practices and FI in veterans who responded to the California Health Interview Survey (CHIS); 7.9% (weighted) of the veteran sample was women. Food insecurity was based on whether a veteran had sufficient money to buy food and a veteran’s federal poverty level status using variables provided by the CHIS. It was not clear, however, if some of the FI questions were independently developed or derived from some other source. The investigation found that veterans who were food insecure and living in poverty were more likely to consume foods of lower dietary quality. Smith et al, 78 using qualitative methods, found that military service detrimentally affected postservice food consumption patterns and behaviors among VHA health care users; recommendations were made to provide veterans, who are transitioning to civilian life, with nutrition and other educational programs. Approximately 5% (n = 3) of the 64 veterans studied were women.
Health Care Utilization
Two studies examined responses about health care access and food insufficiency in women VHA health care users as part of the WV-HUES.
71,72
“Food insufficiency” was used as an index of FI and was defined from the screener question of the USDA HFSSM: “Which of these statements best describes the food eaten in your household in the past 12 months?—enough but not always the kinds of food we want, sometimes not enough to eat, or often not enough to eat.”
47
In one study,
71
food insufficiency was significantly (
Economic Instability
Economic instability was a dominant theme in 2 studies of veteran and nonveteran households varying in disability status using US Census Bureau’s SIPP data. 61,63 Economic instability was assessed as “food insufficiency” and 3 other dependent measures (ie, home, medical, and bill-paying hardships). Food insufficiency was defined by: “Which of the following statements best describes the food eaten in your household in the past 12 months: enough to eat, sometimes not enough to eat, or often not enough to eat” (the latter 2 categories were coded as food insufficient). Wilmoth et al 63 contrasted older veteran and nonveteran households, whereas Heflin et al 61 conducted similar comparisons, but not on households containing older adults. Results from both studies demonstrated that disabled veteran households were more likely to be food insufficient and have other economic hardships compared to non-disabled veteran households. Statistics were not reported by gender in either study, although other important explanatory variables on household demographics were reported for both studies, such as race/ethnicity, education, and marital status.
Homelessness/Housing Instability
One study focused on homelessness and FI in predominantly male veterans who used VHA services. 76 The study by O’Toole et al 76 was methodological in design. Its purpose was to pilot-test a FI screener in homeless veterans who participated in the VA’s Homeless Patient Aligned Care Teams. The screener was modified from a single-question “hunger” screening tool that was used in a previous study. 82 O’Toole et al 76 modified that screener from a 1-month assessment (“In the past month, were there times when the food for you just did not last and there was no money to buy more?”) to a 3-month period and also included other FI-related questions about where food was obtained, who prepared meals, whether food stamps were received, and other topics. Of the 270 screened, 93% were male.
Federal Food Program Participation
Supplemental Nutrition Assistance Program participation in veterans and other service personnel was the main focus in a study by London and Heflin. 62 ACS 2008 to 2012 data were analyzed on active duty and reserve/guard personnel and recent and long-term veterans to estimate the prevalence of SNAP participation and its correlates by service status; 9% of the total sample (ie, veterans, active duty, reserve/guard) were women. SNAP participation was used as an index of FI. The use of SNAP among veterans was estimated at 7.1% and 6.5% for recent and long-term veterans, respectively—it was lowest for active duty personnel (2.2%) and highest for reserve/guard (9.0%). Factors contributing to greater SNAP use in veterans were being younger (≤39 years of age), minority (black, Native American, multiple race, Hispanic), unmarried, and unemployed or in poverty. Low educational attainment and having young children were also important factors related to SNAP participation in veteran households. London and Heflin 62 suggested that the transition from military service to civilian life may result in a considerable loss of food-related resources, particularly for recent veterans.
Community Characteristics/Emergency Preparedness
Five studies examined community characteristics or emergency preparedness in relation to FI.
65,75,77,79,80
Wright et al
77
examined the effect of a pilot program to improve awareness of food resources (eg, food pantries, food programs such as SNAP and Temporary Assistance to Needy Families) for veterans. Household FI was defined based on the 18-item USDA measure.
47
Researchers concluded that this intervention was helpful in decreasing FI prevalence in rural veterans. Veterans were predominantly male (91%) and residents of rural communities in Indiana and Kentucky. Food security (or insecurity) status was used as a main outcome variable. In a second study, Smalls et al
79
found that FI, one of the 14 “neighborhood characteristics,” was significantly associated with several health care behaviors (
Der-Martirosian et al 80 examined emergency preparedness among mostly older veterans recruited from a VAMC in Los Angeles, California, where food and water availability was investigated after the occurrence of a natural disaster. The FI variable, not having enough food or water, was based on the following question: “Because of earthquake, were you without food to eat <or, without enough water to drink> for a period of 24 hours or more?.” Der-Martirosian et al 65 also compared household emergency preparedness between veteran and nonveteran households using data collected from a general preparedness module developed by the BRFSS (2006-2010). The module included questions on 3-day supplies of food, water, and other emergency items. Veteran households had greater food and water preparedness relative to nonveteran households.
Discussion
Eight research domains were identified: (1) FI prevalence, (2) health status, (3) dietary practices, (4) health care utilization, (5) economic instability, (6) homelessness/housing instability, (7) food program participation, and (8) community/emergency preparedness factors. The most dominant theme was health status, while social determinants such as food program participation and homelessness/housing instability were the least dominant. Few studies addressed FI in a representative veteran population (e.g., unclear if sample designs included veterans) and few placed sufficient attention on women veterans or households headed by them. Most survey studies provided limited information on military service characteristics even though these factors impact veterans’ postservice well-being. 16,83 -85 The measures and terminology of FI were varied, and analyses were mainly cross-sectional in nature.
Although there was wide variation in the way studies measured FI, there was no methodological research about how to assess FI in veterans. Also, no standardized methodology was used across studies. For example, the USDA HFSSM that has been deemed valid and reliable based on its use in civilian populations 4,86,87 was used in various versions (full, abbreviated) for the majority of studies. 60,64,67,71 -74,77,79 Of the 21 studies, 2 reported the use of the entire 18-item module, 64,77 while at least 7 relied on various shortened versions of the HFSSM. 60,63,67,71,72,74,79 Two studies 69,70 used the USAID-developed, 9-item assessment, the HFIAS. 49 Neither the HFIAS nor the HFSSM referred to above or its variants has ever been tested to determine their validity and usability in a veteran population. No testing of deviations of the 12-month reference period specified for the HFSSM has also been conducted. Moreover, to the best of our knowledge, there has been minimal testing in any population of how differences in positioning of FI questions may affect prevalence estimates. Basiotis 88 reported that placing a single-item question on food sufficiency either before or after questions on food program participation may bias classification of a household’s FI status.
There are limitations to the use of abbreviated FI methods that are derived from the full HFSSM. Nationwide surveys, such as the CPS or the National Health and Nutrition Examination Survey, administer the full HFSSM to provide national FI estimates. 89 But comparability between full and various abbreviated modules is questionable because the latter generally do not provide information about perceptions of food adequacy or data on food restriction for all members of an individual’s household (ie, questions 11-18 of the HFSSM are only asked if there are children less than 18 years of age in the household). 1,48 Although evidence points to the usefulness of the 1-item food sufficiency question as a surrogate FI measure, 88,90,91 some consider it to be a weaker version of the full module 48 and different versions may produce different results. 87,89 Moreover, the 6-item version of the HFSSM may be less reliable 48 and not useful for populations where disability is prevalent because it does not consider food access restrictions related to an individual’s physical state or to transportation barriers. 92 Overall, abbreviated versions vary in the extent to which they can assess FI severity, experiences, and behaviors.
Differences in terminology add to difficulty in interpreting and generalizing results across studies. “Food insufficiency” was originally used by the USDA to describe an inadequate amount of food resulting from having too little money or resources. 37 However, food insufficiency as defined in several studies 61,63,71,72 excluded economics or availability of money: “Which of these statements best describes the food eaten in your household in the past 12 months?: enough but not always the kinds of food we want, sometimes not enough to eat, or often not enough to eat.” The term “food insufficiency” was dropped by the USDA and Department of Health and Human Services once the term “food insecurity” was developed. 1 Food insecurity has also been used synonymously with “hunger,” which has been defined as undernourishment, extreme FI, 1 or physical sensation of pain or weakness. 15 Of the 21 studies examined, only Brostow and coworkers 67 provided estimates of “hunger” in male veterans, differentiating it from FI by defining it as a yes/no response to: “In the past 12 months, were you ever hungry, but didn’t eat because there wasn’t enough money for food”?
Most studies used survey data, but it is not clear to what extent recruitment of veterans was actually considered in survey design. Large-scale, population-based surveys should be developed and administered that have sampling designs inclusive of veterans, ascertain veteran status using mechanisms other than self-report, and provide for oversampling of selected subgroups of the population, namely, women and racial/ethnic minorities. Greater collaboration between the VA, the largest federally funded health care system that is specifically targeted to veterans, 93 and other federal agencies would allow for improved representation of veterans. The last nationwide survey of veterans conducted by the VA, the National Survey of Veterans, was administered in 2010, 94 but FI was not studied then and no plans currently exist to our knowledge to continue its administration or for it to be inclusive of FI-related issues. A recently fielded study conducted by the VA, the Comparative Health Assessment Interview Study, 95 includes a question on FI but asks about it in association with housing insecurity (“Have you ever not had enough money for food or a place to live?”) and targets OEF/OIF/OND veterans.
More than half of the studies reviewed were based on specific subsets of the veteran population—veterans using VA health care 69 -76,78,79 or those with specific health conditions, 69,74,79 residing in specific regions of the United States, 65,68,77,79,80 or predominantly male. 62,67 -70,76 -78,80 More comparisons need to be made between male and female veterans with respect to FI and military service, disability/health concerns, and psychosocial characteristics (eg, low income, social support, housing, other social determinants) in studies adequately powered for gender-based contrasts. Two of the 4 studies that targeted FI prevalence drew contrasts between men and women veterans but found no difference by gender. 70,73 These comparisons are needed because women veterans’ use of VA health care is increasing and they may be at higher FI risk than their male counterparts. 71
Individuals who are food insecure typically have poor food and nutrient intakes. 96 Therefore, the lack of dietary research among veterans is particularly problematic when evidence points to poorer adherence of federal dietary recommendations among veterans relative to nonveterans. 45 Just 2 studies targeted dietary patterns in this review, 68,78 one of which was a qualitative analysis of food eating behaviors. 78
Also, analyses of longitudinal effects were limited so that less could be concluded about the cyclical nature of FI that varies with household food budgets over time 7,97,98 and affects health by promoting excessive food intake when food is available. 7 Greater use of these research designs would enable assessments of legislative changes on SNAP and other similar types of programs over time.
Few studies targeted food program participation and emergency food resource use (eg, food banks). Use of food assistance by veterans may be related to their knowledge and attitudes about these programs, and understanding these constructs through research could uncover information about barriers to participation. Narain et al 72 addressed this to some extent by examining the association of food sufficiency with patient activation, a measure that assesses an individual’s beliefs and knowledge of their health and its management. 81
Intervention effectiveness had not been a major focus in past research. The VA has incorporated into its electronic health record clinical reminder system a single-item screener to identify veterans at risk of FI 44,50 and to connect veterans with referrals to various food support systems. Research results, however, have not been extensively published on how effective these interventions are. Only 1 of the 21 studies examined the FI status of veterans after an intervention, 77 but it was a small-scale study limited to rural veterans residing in Kentucky and Indiana. And because veteran health care can be administered through government and nongovernment providers, investigation should possibly be extended into the types of assessments and interventions that are applied in private health care facilities.
A limitation of this review was that an exhaustive search of the gray literature for unpublished materials was not performed, resulting in possible threats to the validity of our review. Publication bias may exist because studies reporting statistically significant findings are more likely to be published—therefore, the literature identified may not represent the state of the evidence on this topic. 99 Gray literature, however, is also not free from bias. Moreover, there is no comparable equivalent of a scoping review for gray literature/information 52 and no universally accepted means of systematically collecting data from gray literature. 100
Our classification of studies was subjectively determined, and therefore, our perspective on how these studies were grouped could be interpreted differently by others. For instance, Ashby and coworkers 41 classified studies identified through a systematic literature review into a predetermined set of domains consisting of “food access, availability, utilization, and stability over time.” Also, although not a “systematic literature review” or meta-analysis, the purpose of our review was to provide a broad representation of the major areas of the FI research and to identify areas where future work could be directed as per scoping review guidelines. This was a qualitative review; therefore, it did not provide information on the magnitude and direction of effects across studies of varying designs as would have been achieved through these other mechanisms. Moreover, some search terms were not used that may have increased the number of studies that could have been potentially reviewed—these included terms such as food access, food poverty, and food deserts. 41
In conclusion, this is the first review focused on FI in US veterans and provides information on what major topic areas have been examined and what gaps in the evidence exist that could provide direction for future research. Noted in this review is a need for (1) validity testing of the methods and definitions used to assess FI in veterans and underexamined veteran subgroups (eg, women, racial/ethnic minorities); (2) design and administration of veteran-centric surveys that consider dietary/FI status and associations with service characteristics (eg, the military-to-civilian transition process, 62,78 rank, military occupation), postservice physical and mental health status, and social determinants (eg, housing insecurity, neighborhood characteristics—food deserts); and (3) intervention effectiveness (eg, relationship to assistance programs and changes in federal legislation over time). Other salient but minimally investigated issues that were made more visible through this review of the published evidence in veterans include “hunger” (eg, how should this be defined and studied?) and attitude/behavior/knowledge interrelationships.
Food insecurity has been studied since the 1960s when the issue of hunger in America was foremost in the minds of many 89 and which resulted in national nutrition monitoring of the US population in the 1990s. 101 Despite this major health initiative, established associations between dietary adequacy and good health, 102 and the important contributions already made by researchers on this topic, a lasting commitment to expanding research on FI and dietary intake among veterans seems lacking. Research on FI should continue with greater attention to approaches and explanatory variables that reflect its complexity.
Footnotes
Acknowledgments
The views expressed are those of the authors and do not necessarily reflect the position or policy of the US Department of Veterans Affairs (VA) or the US government. The authors greatly appreciate the expertise of the VA Central Office Library staff (ie, Ms Janice Young, Ms Robyn Washington, Ms Ternell McCullough, Ms Faith Steele, Ms Nancy Clark) who conducted the electronic database searches and provided input on other related matters. The authors also thank Dr Victoria Davey (Office of Research and Development, US Department of VA) for her contribution related to the inception and design of the article.
Authors’ Note
Y.C. initiated the research described in this article and acquisition of the identified publications. All authors (Y.C., J.K., M.S., S.S.) contributed to the design, analysis, and interpretation of the results and drafting of the manuscript. All authors reviewed and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
