Abstract
Background:
One in 4 children globally is stunted. Stunting is associated with reduced cognitive development, reduced productivity, and chronic disease in later life.
Objective:
To explore the association between maternal diet during pregnancy and low birth weight, which increases the risk of stunting.
Methods:
Current literature pertaining to maternal diet and low birth weight was reviewed.
Results:
Low birth weight and small for gestational age are risk factors for stunting. Dietary pattern studies show an association between moderate dairy protein intake and increased birth weight and reduced risk of low birth weight. Protein-to-carbohydrate ratios are important factors in relation to gestational weight gain and fetal programming. There is evidence suggesting that whey protein could play a role in fetal lean body mass and reduced risk of low birth weight.
Conclusions:
Maternal diet is associated with birth weight.
Introduction
One in 4 children globally under the age of 5 years is stunted. 1 Stunting is associated with reduced cognitive development, reduced productivity, and chronic disease in later life. 2 Thus, stunting has been recognized and acknowledged in the UN Sustainable Development Goal No. 2—End hunger, achieve food security and improved nutrition, and promote sustainable agriculture, where in Task 2.2, it is stated “by 2030 end, all forms of malnutrition, including achieving by 2025, the internationally agreed targets on stunting and wasting in children under 5 years of age and address the nutritional needs of adolescent girls, pregnant and lactating women, and older persons.” The impact of eradicating stunting is not restricted to individuals; it is also beneficial to countries where it has been shown to deliver reductions in gross domestic product, which can be as high as 20% because of the effect stunting has on educational and earning potential. 2,3
Low Birth Weight and Stunting
More than 25% of the first 1000 days of life are spent in utero. The association between low birth weight (LBW—babies born with a weight of less than 2500 g, regardless of gestational age) and stunting has been acknowledged by the World Health Assembly (WHA). In its Stunted Policy brief, 4 the WHA states that “reducing the rate of infants born with LBW is associated with a decreased risk of stunting” and further “that actions focused on prevention such as ensuring pregnant mothers are adequately nourished can help address both stunting and wasting.”
The association between LBW and stunting derives from multiple studies. Most recently, Aristami and colleagues reported that LBW was the most dominant predictor associated with stunting among children aged between 12 and 23 months in Indonesia. The prevalence of stunting in Indonesia is more than 40%, and in this study, the odds ratio for LBW infants to be stunted was 1.74 (95% confidence interval = 1.38-2.19) times more likely than a normal child. 5 A very recent study conducted in Zimbabwe again found that LBW was the major contributing predictor of stunting among participants aged 0 to 59 months. 6 Other measures of fetal size and development—for example, small for gestational age and also term length are associated with stunting. For example, in the study by Danaei and colleagues (2016), risk factors for stunting were grouped into 5 risk clusters including maternal nutrition and infection, teenage motherhood and short birth intervals, preterm birth and small for gestational age, child nutrition and infection, and environmental factors. It was determined that preterm birth and small for gestational age was the leading risk cluster, as it was associated with 10.8 million cases of a total of 44 million in 2010—that is, 25%. 7
Diet and Birth Weight
A review by Grieger and Clifton (2014) 8 looked at dietary patterns among pregnant women in developed countries and found that high intakes of Mediterranean diets of fish, low fat dairy, lean meat, and legumes were associated with higher birth weight and lower risk of intrauterine growth retardation. Intrauterine growth retardation refers to fetal weight being below the 10th percentile for gestational age. 9 Grieger and Clifton also found that high intakes of refined grains, processed meat, confectionary, and soft drinks was associated with increased risk of small for gestational age and LBW. 8 Brantsaeter and colleagues 10 drilled deeper into the influence of specific dietary components, focusing on maternal milk and dairy consumption and how that influenced birth weight. Again the studies were among Western mothers. Whereas 2 of the reviewed studies showed no association, 4 showed positive associations with milk and dairy consumption and birth weight. 10 The positive effect was most pronounced at low-to-moderate milk intake levels indicating that limited intake of dairy was associated with reduced risk of LBW. Since that review was published, more recent work has been reviewed, 11 and more observational studies 12 -14 have been published. The conclusions of these reports have remained consistent. In Spain, Olmeda-Requena and colleagues showed low dairy product intake was associated with higher risk of small for gestational age. Dose–response analysis indicated that increasing intake by 100 g/d in early pregnancy decreased the risk of small for gestational age by 11% (adjusted odds ratio by age = 0.89; 95% confidence interval [CI]: 0.83-0.96). 12 A cross-sectional study conducted in Indonesia by Madajian and colleagues showed that more than 50% of women of reproductive age were unable to meet national nutrient requirements, and 44% of pregnant women had an inadequate intake of energy and protein. 13 Women who were consuming or had access to dairy did increase the amount of dairy that they were taking during pregnancy, but that amount was insufficient to meet nutrient requirements. A study from Malawi by Hjertholm and colleagues found that whereas a diet rich in carbohydrate was negatively associated with birth length and abdominal circumference, a diet high in fat was positively associated with birth length and abdominal circumference, and that milk intake was positively associated with birth weight. 14 Each additional day of milk consumption within 7 measurement days was associated with a 75 g increase in birth weight (P = .02). In the context of birth weight in an undernourished population, the authors stated, “…taking into account the effect sizes of the associations between birth size and the different nutrients and food groups, it becomes apparent that milk foods are the most important food to promote.” 14
As with any nutrition guidance, particularly in women, it is important to consider a balance of calories, macro-, and micronutrients. Over or imbalanced nutrition during pregnancy may have undesirable consequences. In the case of the mother, the association of dairy intake with gestation weight gain is unclear. For example, Steube and colleagues looked at associations of diet and physical activity during pregnancy with the risk of excessive weight gain in a cohort of mothers residing in the Boston area of the United States. 15 They found a positive association between excessive gestational weight gain and dairy consumption, but the result was only just significant (odds ratio for excessive gestational weight gain = 1.09 (95% confidence interval [CI]: 1.01-1.19 ). In contrast, Abreu and colleagues reported that dairy intake during the first and second trimester of pregnancy had a positive association with neonatal head circumference, positive association with placental weight, and a negative association with gestational weight gain (unstandardized regression coefficient = −0.007, P = .020) among Portuguese women. 16 More research in this area is clearly warranted.
In fact, there is evidence that excessive gestational weight gain appears to be more influenced by protein:carbohydrate ratios. Maslova and colleagues working with data from the Danish National Birth Cohort reported that high protein to carbohydrate ratios were associated with reduced gestational weight gain, partly driven by decreasing intake of added sugar. 17 However, further analysis of protein intake by source by these authors showed that an effect was associated with meat and fish protein, but not dairy protein.
Dietary intake during pregnancy not only can impact the mother but also the fetus. In particular, fetal programming is also a topic of concern. Fetal programming relates to the hypothesis that prenatal diet defines the risk of chronic disease in later life. Research in this area is still evolving. Maslova and colleagues found, “higher BMI in offspring…(was) driven by protein from meat and meat products rather than fish or milk products.” 18 This is in contrast to findings from the same research group where meat consumption was found to display the beneficial association with reduced gestational weight gain. 17 Jihan-Mihan and colleagues in their review of fetal programming stated that both low- and high-protein maternal diets had detrimental effects on body weight and body composition of offspring, 19 although 2 of the 3 cited references supporting the comment were rat studies. A more consistent finding is that protein-to-energy ratio remains the important factor, and increasingly evidence points to dairy protein intake by the pregnant mother is associated with leanness in the neonate. Initial reports of this finding date back to Moore and colleagues who found that the amount of energy in the pregnant mother’s diet derived from carbohydrate was negatively associated with leanness in the neonate. 20 Further, they showed that the percentage energy from dairy protein in the mothers diet was more positively associated with neonate leanness than other protein sources and that every 1% increase in energy from dairy protein delivered an average 24 g increase in birth weight. 20 This observation of dairy protein–associated changes in body composition toward increased lean body mass aligns with many more recent studies of whey protein–induced changes in body composition in other study populations. 21
The dairy/whey protein impact on body composition may be of particular importance when considering certain phenotypes which appear to be more susceptible to accumulation of higher levels of body fat at lower body mass index (BMI). For example, the Asian phenotype appears to exhibit increased risk of chronic diseases, such as obesity and type 2 diabetes at lower BMIs than other phenotypes. 22 The complexity associated with accurate measurement of body composition means that studies into this field are still limited. However, one recent publication by Chen and colleagues from the Growing Up in Singapore Towards healthy Outcomes study reported that higher protein and lower carbohydrate and fat intakes during pregnancy was associated with lower neonatal abdominal internal adipose tissue. 23 Further, this association was attributed to higher maternal intake of animal protein but not plant protein.
Turning back to birth weight, the question can be posed as to why milk consumption during pregnancy appears to be consistently associated with reduction in the risk of LBW. Could it be due to a specific component in milk? The answer to that question is still unclear. However, there are intriguing clues. Two observational studies based on the analysis of dietary intake data from the Danish National Birth Cohort and Dutch Generation R studies report shed some light on this question. 24,25 Both these studies compared to the intake of nondairy and dairy protein intake (Figure 1) and found that unlike nondairy protein intake, dairy protein consistently resulted in a modest increase in birth weight. In these studies, dairy protein intake referred to all dairy sources including milk, yogurt, cheese, and ice cream. Both studies also examined the effect of cheese intake alone, and while these data were limited, it can be seen in Figure 1 that the effect of increased levels of cheese intake have only small or no impact on birth weight when compared to total dairy protein intake. This finding is suggestive that whey protein, which is absent from cheese, could be a contributing factor to the reduction in the risk of LBW.
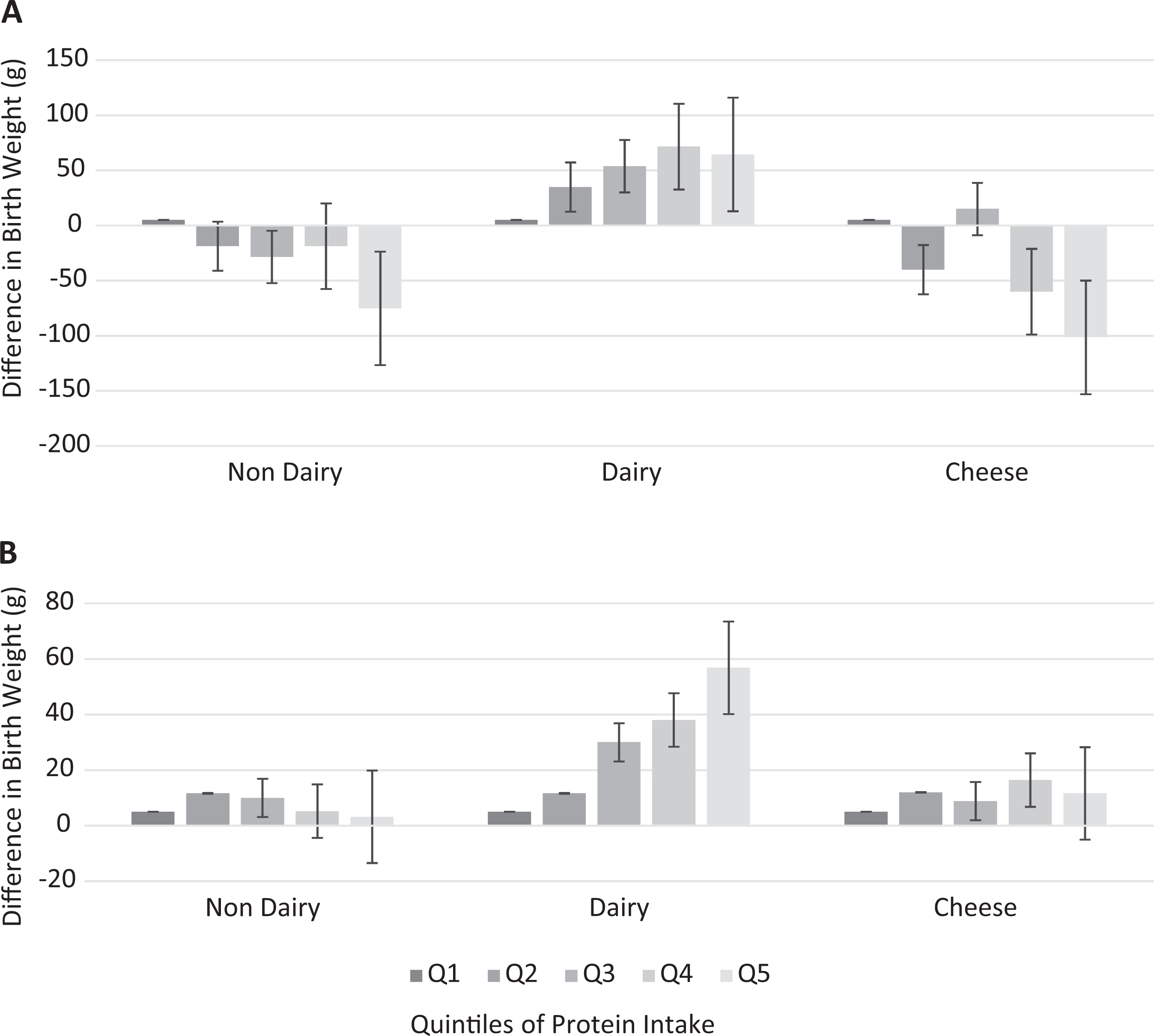
Associations of maternal protein intake with offspring birth weight. A, Heppe et al., 2011 25 Generation R Study, Rotterdam, The Netherlands—the results are based on multivariate linear regression models and reflect the difference and 95% confidence interval for each level of daily protein intake comprising nondairy protein (P = .93), dairy protein (P = .01), and protein from cheese (P = .24). Intake is expressed in terms of quintiles of consumption (Q) which are categorized as equivalent to 0, <1, 1-2, 2-3, and >3 glasses (150 mL) milk/day. B, Olsen et al., 2007 24 —Danish National Birth Cohort Study. The increment in birth weight (95% confidence interval) for each quintile compared with the lowest quintile for nondairy (P = .98), dairy (P < .0001), and cheese (P = .23) intakes. The P value for the trend refers to student t test for the regression coefficient. (Adapted from Heppe et al 25 and Olsen et al. 24 )
So what might be the mechanism by which whey protein could be involved in increasing birth weight? Several authors have pointed out that human growth and specifically chondral plate growth, which is a determinant of linear growth, is regulated by the mechanistic target of rapamycin (mTOR) pathway. 26,27 The mTOR pathway represses protein and lipid synthesis when certain amino acids, specifically leucine, are deficient. Stunted children have lower serum levels of indispensable and conditionally essential amino acids. 28 Dairy and in particular whey protein are rich sources of indispensable amino acids. Indeed, there is a substantial body of evidence from both animal and human infant studies that indirectly support a role and even a mechanism that could explain the influence of maternal whey consumption during pregnancy and its positive association with increased birth weight and/or size.
Conclusion
LBW and small for gestational age are risk factors for stunting. Dietary pattern studies do show an association between moderate dairy protein intake and increased birth weight and reduced risk of LBW. Protein to carbohydrate ratios are important in relation to gestational weight gain and fetal programming, but more research is needed to establish mechanisms and whether there is really an association between maternal whey protein intake and birth weight. Evidence is accumulating that is supportive of an association between maternal whey protein consumption during pregnancy and reduced risk of LBW.
Footnotes
Author’s Note
This article reports an invited presentation by David Clark PhD at the “Dairy Nutrition: An Engine for Economic Growth” conference organized by Dairy for Global Nutrition in Boise, ID, in May 2017.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Research that provided a basis for this review was in part funded by U.S. Dairy Export Council.
