Abstract
Background:
This review aimed at synthesizing evidence on the effectiveness of nutritional interventions that were carried out before and/or during early pregnancy versus the control groups on reducing the risk of low weight at birth in sub-Saharan Africa.
Methods:
We have searched on MEDLINE, SCOPUS, CINAHL, HINARI, and Cochrane Library of systematic review databases for published articles in English language from 2010 to 2021 years. For unpublished studies, we searched on Google scholar. Randomized controlled trial studies of nutritional interventions carried out before/or during early pregnancy in sub-Saharan Africa to improve low birth weight were considered. The data were extracted and pooled using the Joanna Briggs Institute software. The effect size was calculated using fixed-effect models. Mantel-Haenszel method was used to calculate the relative risk with their respective 95% CI. Heterogeneity was assessed using the standard chi-square and I 2 tests.
Results:
Seven studies were included in the review with a total of 5934 participants. Three types of nutritional interventions were identified: iron supplementations, lipid-based supplementations, and nutritional education and counseling. We have identified only one intervention started during preconception. The meta-analysis showed that none of the identified nutrition interventions had a statistically significant effect on low birth weight.
Conclusions:
Based on the review evidence, nutritional interventions before and/or during early pregnancy in sub-Saharan Africa had no significant effect on low birth weight. However, since our evidence was derived from a small number of trials and participants, a large-scale randomized controlled trials review might be required to elucidate the finding.
Keywords
Background
Globally, 20.5 million or 1 in 7 live birth children are low birth weight (LBW). 1,2 Almost three fourth of this LBW is from South Asia and sub-Saharan African countries with an estimated rate of 48% and 28%, respectively. 3 World Health Organization (WHO) defined LBW as weight at birth less than 2500 g regardless of the newborn gestational age. 4 Low birth weight is a major predictor of infant morbidity and mortality. 5 Accordingly, LBW infants weighing 2000 to 2499 g at birth are 4 times more likely to die within their first month of life than infants who weigh 2500 to 2999 g, and 10 times more likely to die than infants weighing 3000 to 3499 g. 6 Moreover, evidence indicated that maternal anemia during pregnancy has an impact on the risk of LBW, preterm birth, and neonatal mortality. 7 Therefore, birth weight is considered as an important measurement gauge of maternal and fetal health outcomes of pregnancy. 8,9 Furthermore, children with LBW are at a greater risk of developing noncommunicable diseases such as metabolic syndromes, diabetes mellitus, and cardiovascular diseases in their later life. 6,10 Although LBW has several identified determinant factors, poor maternal nutrition and health have a greater share. 11,12 Thus, it is clear that an effective and large-scale practical intervention to prevent LBW has a great impact on the health and productivity of individuals and societies as a whole; particularly where the prevalence rate of LBW is high. 6 The prepregnancy weight of the mother, her nutritional status, and the amount of gestational weight gain are the most useful indicators for interventions to reduce LBW. 1,6,13,14 Globally despite efforts being made by the countries, still, reports revealed that the rate of LBW persists and remains unacceptably high especially in sub-Saharan African countries. 3,15 Accordingly, evidence from the recent lancet report of LBW trends revealed that the number of LBW was estimated to have increased in sub-Saharan Africa from 4.4 million in 2000 to 5 million in 2015. 3 This indicated that to achieve the WHO global nutrition target, more than doubling the current progress in the region must be required. 1 Nutrition-specific and nutrition-sensitive interventions have been proposed as a conceptual framework to optimize fetal and child growth and development globally. 16 Accordingly, multiple micronutrient supplementations (MMNs), 17 iron supplementations, 18 and nutritional educations 19 are among the common nutrition-specific interventions carried out during pregnancy to address the immediate determinants of malnutrition and improve fetal outcomes in sub-Saharan Africa, 16 whereas malaria preventive drugs are among the common nutrition-sensitive interventions to address the underlying causes of malnutrition during pregnancy in the continent. 20
A preliminary search for systematic reviews on this topic was performed in June 2020 on PROSPERO, MEDLINE, the Cochrane Database of Systematic Reviews, and the Joanna Briggs Institute (JBI) Database of Systematic Reviews. No current or underway systematic reviews were identified in these databases that address the objective of the review and use the same inclusion criteria. Therefore, this evidence might be used by program designers and policymakers to invest in effective nutrition intervention methods that targeted the causes of LBW, according to the local context to attain the global nutrition target set of 30% reduction of LBW by the year 2025. 1,10,21 In addition to this, it might be used by researchers to generate additional evidence.
Methods
Data Sources and Searching Strategies
This review was designed to synthesize scientific evidence on the effectiveness of nutrition interventions conducted before and/or during early pregnancy on the reduction of the risk of LBW in sub-Saharan African countries. The study protocol of this review was registered in the international prospective register of a systematic review (PROSPERO) under protocol number CRD42020188236. We followed the Preferred Reporting Item for Systematic Review and Meta-analysis guideline to report our results (Figure 1). The search strategy was aimed to find both published and unpublished studies. Three-step search strategies were utilized in this review. An initial search was done on MEDLINE, SCOPUS, CINAHL, HINARI, and COCHRANE library of systematic review databases, published in English language from 2010 to 2021 followed by an analysis of the text words contained in the title and abstract. The second search was done using identified key words and index terms across all included databases. Then, finally, the reference lists of included articles were checked for articles not identified by the above-stated search. The search strategy included only terms related to the described intervention. The search terms were combined with database-specific filters for randomized controlled trial (RCT) interventions, where these were available. The searches were rerun just before the final analyses to include further studies retrieved. Two review authors were first searched independently and screened for inclusion by looking over the title and abstracts of the studies. Then, full texts were assessed for inclusion using predefined inclusion criteria again independently. Unpublished studies and conference proceedings were searched on Google scholar to identify gray literature appropriate to the review objective.
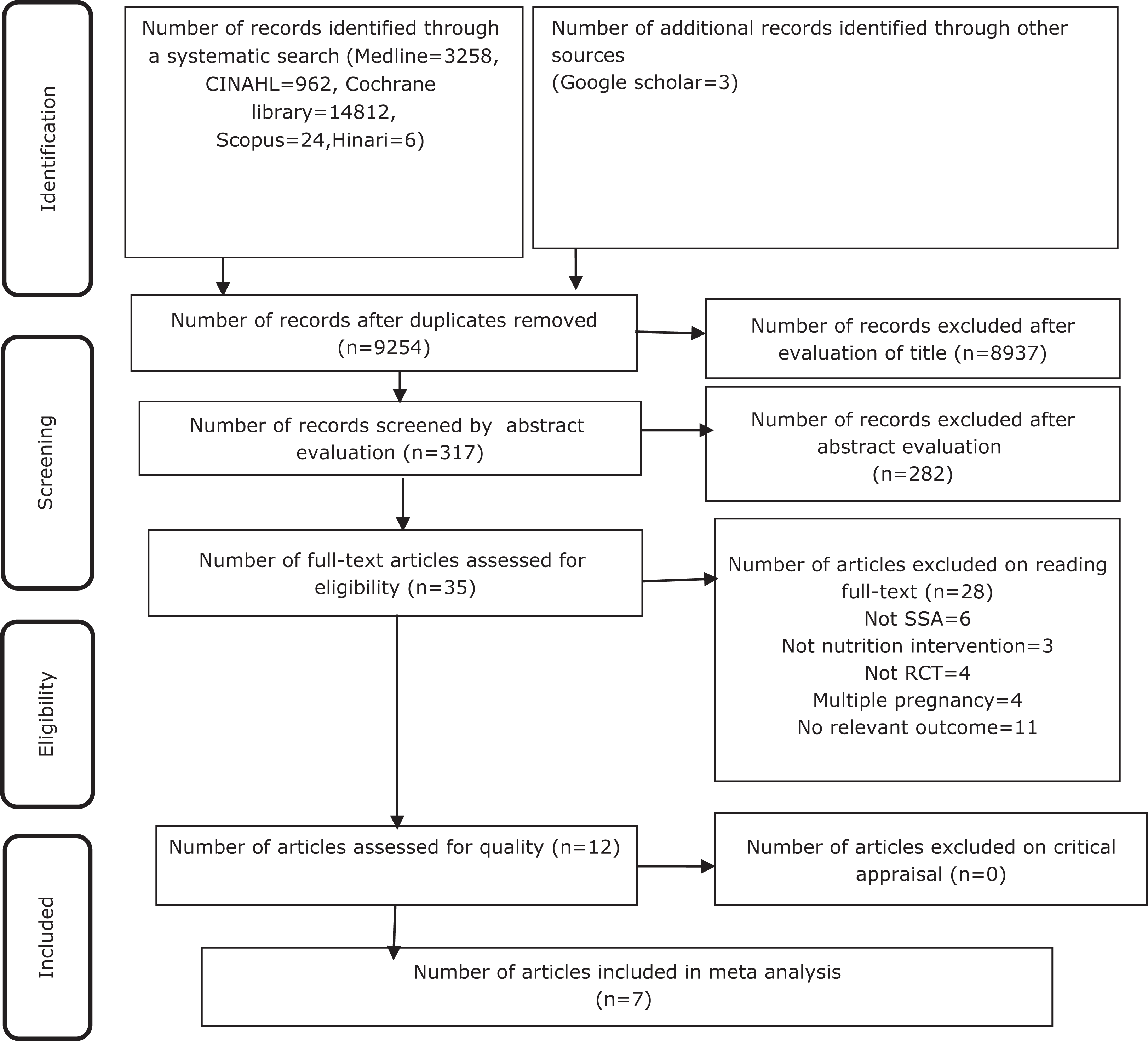
Flow diagram for the literature search (PRISMA) results and study selection process of the effect of nutrition interventions before and/during pregnancy on low birth weight in sub-Saharan Africa from 2010 to 2021. PRISMA indicates Preferred Reporting Item for Systematic Review and Meta-analysis. 22
Initial key words used were Pregnancy [MeSH Terms] OR Preconception Care [MeSH Terms] OR Prenatal Care [MeSH Terms] AND Prenatal Nutritional Physiological Phenomena [MeSH Terms], OR health education [MeSH Terms] OR micronutrients OR fortification OR multivitamin OR vitamin OR vitamins iodine OR zinc OR folic acid OR iron OR protein OR fatty acid OR marine oil OR salt reduction AND Infant, Newborn [MeSH Terms] AND low birth weight [MeSH Terms] AND Africa South of the Sahara [MeSH Terms]. The details of the search strategies for each database were provided (Additional File 1-5).
Study Selection (Inclusion/Exclusion Criteria)
This review considered RCT studies only. The eligibility of the included study was determined using the participant intervention control outcome framework:
Participants: singleton pregnant mothers of 28 weeks and less gestational age at the time of enrollment or nonpregnant mothers.
Interventions: Any nutritional intervention.
Control groups: women who took standard care or usual care, placebo, or no treatment before and/or during early pregnancy to reduce the risk of LBW.
Outcomes: LBW is defined as weight at birth less than 2500 g, regardless of the gestational age of the infant. 4
Study Screening and Selection
Following the search, all identified citations were collated and uploaded into EndNote version x8.1 bibliographic software, 2001 to 2014, and duplicates were removed. Titles and abstracts were then screened by 2 independent reviewers for assessment against the inclusion criteria for the review. Potentially, relevant studies were retrieved in full and their citation details were imported into the JBI System for the Unified Management, Assessment, and Review of Information (SUMARI; https://www.jbisumari.org/). Then full text of the selected citations was assessed in detail against the inclusion criteria by 2 independent reviewers. Reasons for the exclusion of critically appraised studies were recorded and reported in the systematic review (Additional File 6).
Quality Appraisal
Eligible studies were critically appraised by 2 independent reviewers Melesse Niguse Kuma (KMN) and Girma Beressa (BG) before inclusion. For methodological quality in the review, standardized critical appraisal instrument from the JBI for experimental studies was used (Additional File 6). The results of the critical appraisal were reported in narrative form and a table (Table 1). In addition to this, we grade the quality of the study by using Grading Recommendations Assessment, Development, and Evaluation (GRADE) 3.6.1 software (Table 2).
Summary of the Critical Appraisal Results of the Included Studies of Effect of Nutrition Interventions Before and During Pregnancy on Low Birth Weight in Sub-Saharan Africa.a
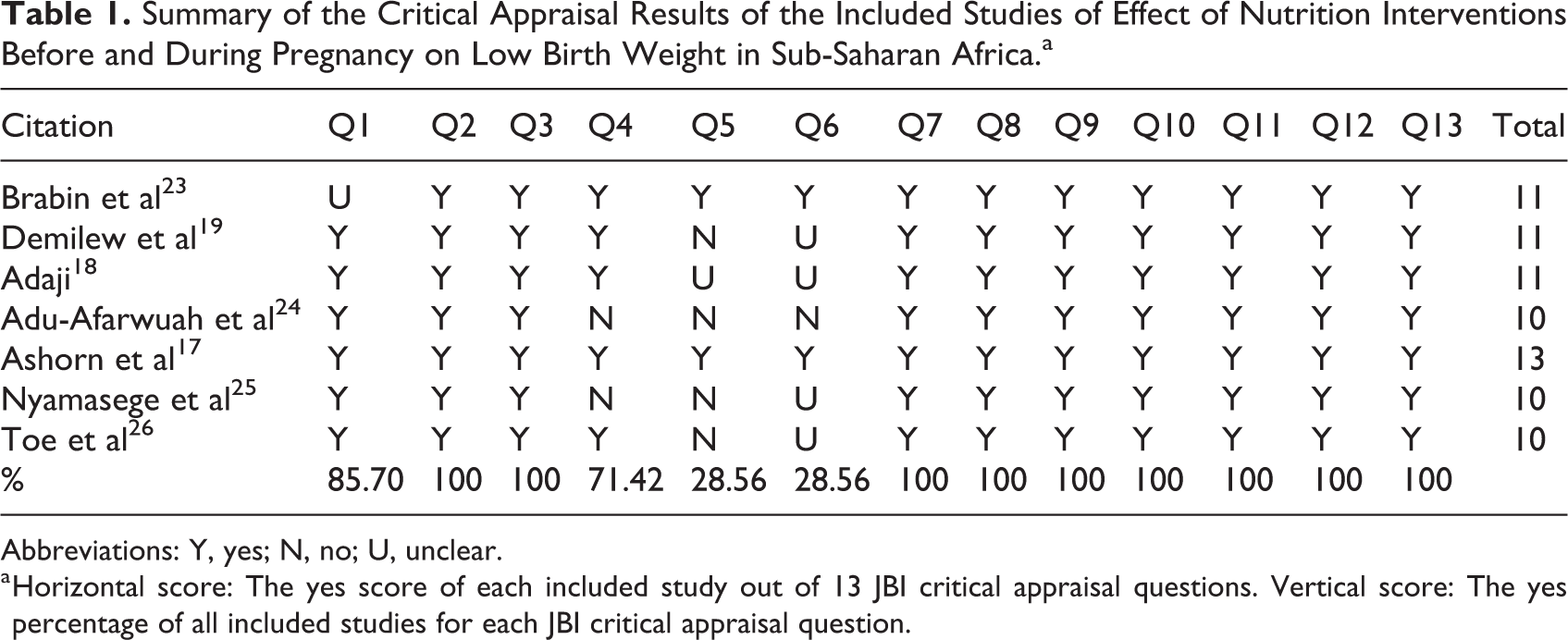
Abbreviations: Y, yes; N, no; U, unclear.
a Horizontal score: The yes score of each included study out of 13 JBI critical appraisal questions. Vertical score: The yes percentage of all included studies for each JBI critical appraisal question.
Summary of Findings of Nutrition Interventions Before and During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa.a
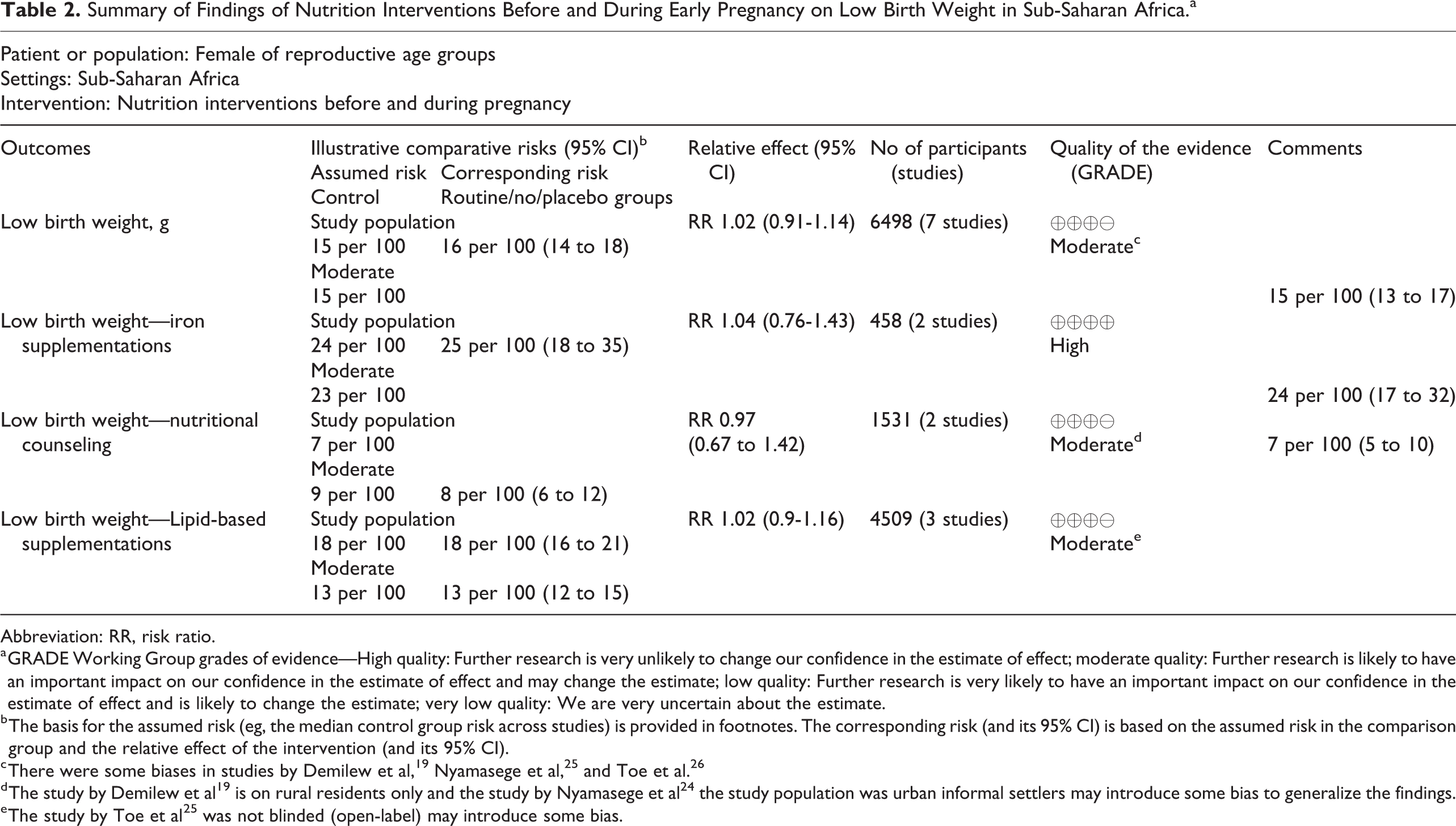
Abbreviation: RR, risk ratio.
a GRADE Working Group grades of evidence—High quality: Further research is very unlikely to change our confidence in the estimate of effect; moderate quality: Further research is likely to have an important impact on our confidence in the estimate of effect and may change the estimate; low quality: Further research is very likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate; very low quality: We are very uncertain about the estimate.
b The basis for the assumed risk (eg, the median control group risk across studies) is provided in footnotes. The corresponding risk (and its 95% CI) is based on the assumed risk in the comparison group and the relative effect of the intervention (and its 95% CI).
d The study by Demilew et al 19 is on rural residents only and the study by Nyamasege et al 24 the study population was urban informal settlers may introduce some bias to generalize the findings.
e The study by Toe et al 25 was not blinded (open-label) may introduce some bias.
Data Extraction
Data were extracted using the standardized data extraction tool from JBI SUMARI by 2 independent reviewers (Additional File 7). The data extracted were included specific details about the populations, intervention, comparator, and primary outcome of interest to the review question and specific objective. Any discrepancy that arose between the reviewers was resolved through discussion or third review author.
Data Synthesis
Quantitative data were pooled in a statistical meta-analysis using JBI-MAStARI (Meta-Analysis of Statistics Assessment and Review Instrument). Effect sizes were expressed as relative risk along with 95% CIs around the summary estimate. The meta-analysis was computed using the fixed-effect model by review manager software, 5.3 version. Considering that, the studies included in each subgroup were very small and homogeneous enough in terms of the study participants, study design, and outcomes. Mantel-Haenszel method was used to calculate the relative risk along with its respective 95% CI. We used the Mantel-Haenszel method because it is more robust when the number of trials is very small. 27 Heterogeneity was assessed statistically using the standard chi-square test and visual inspection of meta-analysis output on a forest plot. The level of heterogeneity was defined based on I 2 (I 2 = 0% no heterogeneity, I 2 < 50% low heterogeneity, I 2 = 50%-75% medium heterogeneity, and I 2 > 75% high heterogeneity). 28 Subgroup analyses were carried out to verify the source of heterogeneity in the study trials and to give estimates of different effects for the types of nutrition interventions. Sensitivity analysis was also performed to test decisions made under different assumptions.
Results
Identification Studies
The initial search identified 9254 potentially relevant studies after removing the duplicates (Figure 1). Then, 8937 studies were excluded after reading the title. From 317 studies evaluated by reading the abstract, 282 were removed because they did not meet the inclusion criteria. Twenty-eight studies were excluded after reading the full text with a reason (Figure 1). The remaining 7 studies were critically appraised by using the JBI tool and included in the review (Additional File 6). No study was excluded based on methodological quality. Thus, the 7 studies with a total of 5934 participants were included in the final systematic review (Table 3). The included studies were one each from Ghana, 24 Kenya, 25 Malawi, 17 Ethiopia, 19 Nigeria 18 , and 2 from Burkina Faso. 23,26
The Characteristics of the Included Studies in the Meta-Analysis of the Effect of Nutrition Interventions Before and During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa. 22
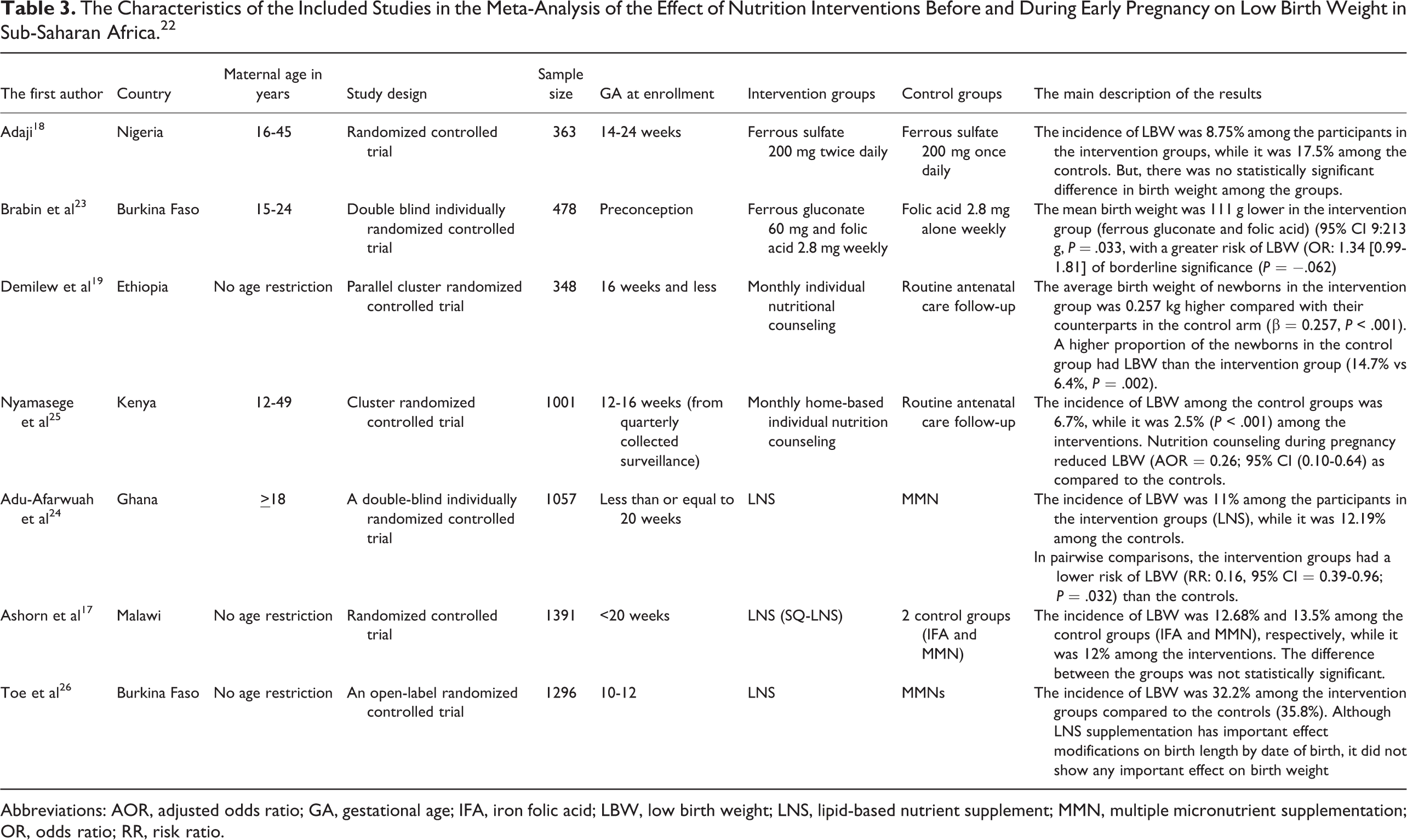
Abbreviations: AOR, adjusted odds ratio; GA, gestational age; IFA, iron folic acid; LBW, low birth weight; LNS, lipid-based nutrient supplement; MMN, multiple micronutrient supplementation; OR, odds ratio; RR, risk ratio.
Description of Included Studies
All of the 7 included studies were RCT reported on LBW as their outcomes. Moreover, we have identified only one study that the nutritional intervention was started during the preconception period. 23
The included studies were categorized into 3 types of nutritional interventions. These were:
1. iron supplementations included 2 trials of 841 women study participants. 18,23
2. Nutritional education and counseling intervention comprised 2 trials on 1349 pregnant women. 19,25
3. Lipid-based supplementation nutritional interventions comprised 3 trials on 3744 pregnant women. 17,24,26 Of the included trials, 2 studies by Adu-Afarwuah et al 24 and Toe et al 26 were not blinded to the study participants. On the other hand, 3 studies by Adu-Afarwua et al, 24 Ashorn et al, 17 and Adaji 18 were not blinded to those who delivered the intervention. Similarly, it was unclear whether those who delivered the intervention and the outcome assessors were blinded or not to in other studies conducted. 18 In study trials of Adu-Afarwuah et al 24 and Ashorn et al 17 the data collectors were unblinded to the intervention (Table 3).
Methodological Qualities of the Included Studies
We have used a summary finding table created using version 3.6.1 software of the GRADE criteria to grade the included studies. The GRADE covers parameters that could measure the quality of information such as reporting bias, directness, consistency, and the precision of effect estimates. Then, we rated the certainty of the evidence for the outcome as “high,” “moderate,” “low,” and “very low.” Therefore, we have constructed a GRADE summary of finding a table for LBW (Table 2). The included studies grouped based on the intervention type were graded as moderate and high quality.
Meta-Analysis
The data on LBW from 7 studies were pooled to run a meta-analysis. The data extracted were absolute numbers, not effect measures. Besides, 2 studies have 3 arms. 17,24 We grouped the aforementioned studies into binary (2 groups) each by combining their arms according to the Cochrane guideline section 7.7.3.8 before we used it in the analysis. 29 The overall heterogeneity of this review was χ2 = 23.50, P < .001, and I 2 = 74% .This finding shows that there is significant heterogeneity among the studies (Figure 2). The overall result of the meta-analysis revealed that nutritional interventions before and/or during early pregnancy in sub-Saharan Africa had no significant effect on LBW (1.02, 95% CI = 0.91-1.40, P = .75; Figure 2).
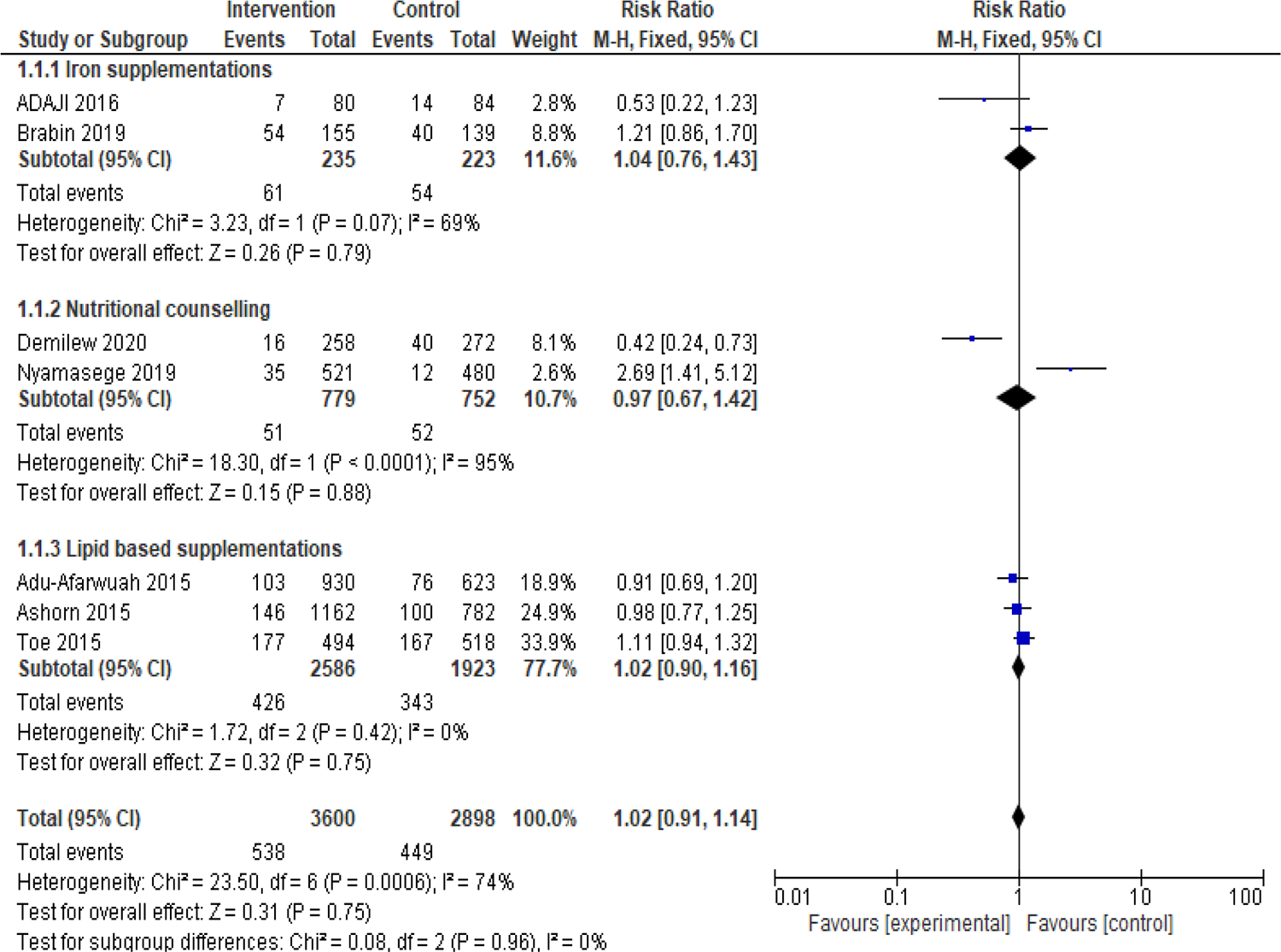
Forest plot of a meta-analysis of the effect of nutrition interventions before and during early pregnancy on low birth weight in Sub-Saharan Africa.
Low Birth Weight by the Types of Interventions
1. The effect of iron supplementations on LBW
Two trials with 841 participants were examined on the effect of iron supplementations before and/or during early pregnancy on LBW. 18,23 Thus, the results revealed that iron supplementations before and/or during pregnancy had no effect on LBW (risk ratio [RR] = 1.04, 95% CI = 0.76-1.43, P = .79), with no significant heterogeneity (χ2 = 3.23, I 2 = 69%, P = .07; Figure 2).
2. The effect of nutritional education and counseling on LBW
The effect of nutritional counselling during pregnancy on LBW was assessed in 2 trials of 1349 participants. The results indicated nutritional education and counselling had no significant effect on LBW (RR = 0.97, 95% CI = 0.67-1.42, P = .88), with statistically significant heterogeneity (χ2 = 18.30, I 2 = 95%, P < .001; Figure 2).
3. The effect of lipid-based supplementations on LBW
The effect of lipid-based supplementation on LBW during pregnancy on LBW was reported in 3 trials of 3744 participants. The results indicated lipid-based supplementation had no significant effect on LBW (RR = 1.02, 95% CI = 0.90-1.16, P = .75), with no significant heterogeneity (χ2 = 1.72, I 2 = 0%, P = .42; Figure 2).
Discussions
The meta-analysis was aimed to determine the effect of a nutrition intervention during and/or pregnancy on LBW.
Summary of the Main Result
This systematic review and meta-analysis indicated that nutrition interventions during pregnancy had no effect in reducing the risk of LBW compared to the control groups.
Overall Completeness and Applicability of Evidence
Both published and unpublished RCT studies that were reported the effect of nutrition interventions before and/or during early pregnancy on LBW were included. Therefore, this review included 7 RCT studies with 5934 study participants which were conducted in sub-Saharan Africa. Accordingly, nutritional interventions before and/or during early pregnancy had no significant effect on LBW as compared to the controls (RR = 1.02, CI = 0.91-1.14, P ≤ .001). This finding was consistent across 4 of the 7 individual studies. In addition to this, subgroup analyses were carried out based on the type of nutritional interventions. Accordingly, meta-regression analyses were done based on the iron supplementations, nutritional counseling, and lipid-based supplementations subgroups. Likewise, in all the 3 subgroup analyses, we had not observed statistically significant improvement in the risk of LBW.
Agreements and Disagreements With Other Reviews
Iron supplementations during pregnancy have been a longstanding public health intervention. Systematic reviews were reported on iron supplementation during pregnancy. 30,31 However, most of these studies were comparing trials done in developed and developing countries. 10,30 -32 Our findings on the effect of iron supplementations on LBW are consistent with 10 global reviews of 61 RCTs, quasi-RCTs, and cluster-RCTs randomizing 43 274 pregnant women which assess the effect of daily iron supplementation on LBW. Thus, oral iron supplementation, iron plus folic acid or iron plus other vitamins and minerals, had no effect on LBW. Similarly, another systematic review report 33,34 shows there is no statistically significant improvement of LBW among the pregnant mothers who received iron or iron-folic acid supplementation during pregnancy compared with the controls, whereas it was against the findings of other reviews 30,32 which revealed that iron supplementations during pregnancy had a significant benefit in reducing the risk of LBW. This inconsistency might be explained by the difference in the number of study participants, time, and duration of the supplement.
The current review revealed that MMNs during pregnancy had no effect on the reduction of LBW risk. Similarly, 2 of the 3 included reviews 17,26 on MMN supplementations demonstrated that it had no effect on LBW. In contrast to this, several systematic reviews 10,35 -38 reported that pregnant women who received MMNs had a fewer risk of LBW. This discrepancy might be explained by the difference in the number of included studies, settings, quality, duration, and compliance of the interventions.
Although both of the included studies 19,25 reported that nutritional counseling and education during pregnancy had a positive effect on LBW, the overall pooled effect of the current review revealed no statistically significant effect on LBW. There is evidence that supports our finding, 38,39 that is, nutritional education and counseling during pregnancy had no effect on LBW. However, it is against the findings, 10 which shows that pregnant women receiving nutritional education to increase energy and protein intake were decreased LBW by 96% compared with the control groups. These observed differences might be due to the difference in the study settings, number, and quality of studies included.
Potential Biases in the Review Process
Biases were assessed during the review process. The majority of the included trials were moderate to high in methodological quality. Concerning the selection of participants and study design, it was RCT in all of the included studies. In one study, 24 the study participants and data assessors were unblinded. In the other study, 26 an open-label RCT design was employed. The validity of all the included studies was assessed based on JBI critical appraisal tool for RCTs. The heterogeneity observed in the meta-analysis might be because of the difference in the sample size of included studies. Funnel plot and quantitative publication bias analyses were not reported due to a limited number of included studies.
Quality of the Evidence
The quality of the evidence included in this study was assessed by using GRADE software. Thus, the finding of this review was graded as moderate and high-quality evidence (Table 2). Additionally, searching for unpublished research findings to reduce publication bias and the use of the JBI critical appraisal instrument to assess the methodological quality of the studies could be taken as the strength of this systematic review.
Limitations of the Review
In this review, we have restricted to articles published in English language only. Therefore, key articles possibly published in other languages in the area were not considered. We have based the search on a few main databases for published articles. Besides, the gray literature search was not systematic or complete. Thus, there might be a possibility of missing important articles. Therefore, the interpretation of this review’s findings considered these limitations.
Conclusions
In our systematic review and meta-analysis, we found that nutritional interventions before and/or during early pregnancy in Sub-Saharan Africa had no effect on LBW as compared to the controls.
Implications for Research
The studies included in this review were graded as moderate and high-quality RCTs. However, we found only a small number of studies with substantial heterogeneity in a few sub-Saharan African countries. Therefore, a large-scale RCT is required to elucidate the effect of nutrition intervention on LBW.
Implications for Practice
This systematic review included 7 RCTs that demonstrated that nutritional interventions during pregnancy had no effect on the LBW risk reduction. Thus, program managers and policymakers need to curiously evaluate the evidence of nutrition intervention used before the application.
Supplemental Material
Supplemental Material, sj-pdf-1-fnb-10.1177_03795721221078351 - Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-1-fnb-10.1177_03795721221078351 for Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis by Melesse Niguse Kuma, Dessalegn Tamiru, Girma Beressa and Tefera Belachew in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, sj-pdf-2-fnb-10.1177_03795721221078351 - Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-2-fnb-10.1177_03795721221078351 for Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis by Melesse Niguse Kuma, Dessalegn Tamiru, Girma Beressa and Tefera Belachew in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, sj-pdf-3-fnb-10.1177_03795721221078351 - Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-3-fnb-10.1177_03795721221078351 for Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis by Melesse Niguse Kuma, Dessalegn Tamiru, Girma Beressa and Tefera Belachew in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, sj-pdf-4-fnb-10.1177_03795721221078351 - Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-4-fnb-10.1177_03795721221078351 for Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis by Melesse Niguse Kuma, Dessalegn Tamiru, Girma Beressa and Tefera Belachew in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, sj-pdf-5-fnb-10.1177_03795721221078351 - Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-5-fnb-10.1177_03795721221078351 for Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis by Melesse Niguse Kuma, Dessalegn Tamiru, Girma Beressa and Tefera Belachew in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, sj-pdf-6-fnb-10.1177_03795721221078351 - Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-6-fnb-10.1177_03795721221078351 for Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis by Melesse Niguse Kuma, Dessalegn Tamiru, Girma Beressa and Tefera Belachew in Food and Nutrition Bulletin
Supplemental Material
Supplemental Material, sj-pdf-7-fnb-10.1177_03795721221078351 - Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis
Supplemental Material, sj-pdf-7-fnb-10.1177_03795721221078351 for Effect of Nutrition Interventions Before and/or During Early Pregnancy on Low Birth Weight in Sub-Saharan Africa: A Systematic Review and Meta-Analysis by Melesse Niguse Kuma, Dessalegn Tamiru, Girma Beressa and Tefera Belachew in Food and Nutrition Bulletin
Footnotes
Authors’ Note
KMN contributed to conception of the research protocol, study design, literature review, quality assessment, data extraction, data analysis, interpretation, and drafting the manuscript. BG contributed to study design, literature review, quality assessment, data analysis, review, and editing of the manuscript. TD contributed to conception of the research protocol, study design, literature review, data extraction, data analysis, review, and editing the manuscript. BT contributed to conception of the research protocol, study design, quality assessment, data extraction, data analysis, review, and editing the manuscript. All authors have read and approved the manuscript.
Acknowledgments
We thank the Joanna Briggs Institute training center of Jimma University for their excellent training course presentations, offering reading materials, and encouraging us to conduct this review.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
