Abstract
Generative artificial intelligence (AI) chatbots, powered by large language models, are emerging as transformative tools with diverse applications in healthcare. This narrative review aims to explore their unique potential for addressing significant gaps in headache education and research, with a main focus on primary headache disorders, a substantial global health burden. In headache education, chatbots can provide tailored, individual information to patients. This improved accessibility could increase the adherence to treatment, reducing the risk of chronification, resulting in a better quality of life. Similarly, clinicians, particularly non-headache specialists, can access a wealth of up-to-date information on headache disorders, including clinical training simulations, which would facilitate reaching a correct diagnosis and optimize treatment. In headache research, generative chatbots can assist by streamlining data collection and analysis, aiding complex experimental setups, and supporting clinical trials, thus accelerating the discovery pipeline. While generative chatbots have demonstrated significant promise for revolutionizing the headache field, challenges persist, with the most important being ensuring data accuracy and privacy. Future developments should focus on pre-training with headache-specific curated databases, multimodal integration, and establishing robust regulatory and ethical frameworks among users (patients, researchers, clinicians), and AI developers to address its limitations. With responsible development, generative chatbots hold the potential to bridge current gaps in headache education and meaningfully advance medical research from bench to bedside, and beyond.
This is a visual representation of the abstract.
Introduction
Primary headache disorders are among the most prevalent neurological conditions, affecting approximately 50% of the general population worldwide (1). The two most common forms, tension-type headache (TTH) and migraine, impose a considerable burden on individuals, healthcare systems, and society (2). These disorders often start at a young age, frequently during critical periods of professional and personal development, with migraine disproportionately affecting women (3,4). According to the 2021 Global Burden of Disease (GBD) study, headache disorders rank among the top three causes of years lived with disability (YLDs) with migraine alone ranked as the second leading cause overall, and the primary cause among women under 50 years (3,5).
Despite the high prevalence and significant disease burden of primary headache disorders, challenges exist in the education of patients and healthcare providers (6). Migraine remains widely underdiagnosed and undertreated. In population-based samples, less than 20% of patients with migraine had seen a general practitioner, and even fewer percentages had consulted a headache specialist (7). Specific acute and preventive treatments are prescribed only to a small percentage of patients, despite being necessary for a significant proportion, potentially leading to the chronification of these disorders (7,8). Furthermore, healthcare providers, particularly in primary care, as well as general neurologists, frequently receive limited training in headache disorders, contributing to misdiagnosis, under-treatment, and wastage of resources (6,9,10). At the same time, many patients lack adequate awareness of headache triggers, treatment strategies, the importance of early intervention, and avoidance of self-medication, often leading to delayed diagnosis, unnecessary diagnostic exams, suboptimal treatment, and progression of the disease (8,11). Therefore, gaps in the headache field include the necessity of educational programs focusing on headache disorders and providing innovative tools, biomarkers, and digital health solutions for personalized treatment approaches to secure correct diagnosis and treatment for patients from any level of care (12,13). This narrative review aims to explore the potential of generative chatbots in the headache field, particularly in education and research. Specifically, it evaluates current applications, their benefits in patient engagement and data collection, existing limitations, and future directions for integrating artificial intelligence (AI)-driven solutions into headache care.
Rise of AI in healthcare
In recent years, the application of AI in the headache field has grown, with machine learning (ML) models increasingly developed for diagnostic, prognostic, classificatory purposes, and treatment-response prediction (14).
Chatbots, or conversational agents, are AI-based computational programs or software applications that have been designed to engage in simulated conversations with users by using natural language processing (NLP). They are emerging as important tools in healthcare, driven by advancements in AI and digital technology (15). Chat Generative Pretrained Transformer (ChatGPT) is a well-known example of this type of chatbot that is optimized to produce a natural, “human-like” conversation (16). Even though ChatGPT was not initially developed for healthcare or health research use, there are a variety of chatbots currently available for patients that can be used to assist them in different health aspects (15,17). These applications include chatbots functioning as digital health assistants, offering patient support, education, healthy behavior promotion, as well as administrative assistance to healthcare providers (17). In the field of headache, the use of chatbots in clinical practice has begun to be explored, particularly for the diagnosis of migraine and suggesting potential treatment strategies, although with mixed and sometimes contradictory findings (18,19). This highlights that despite their potential benefits, it is important to continuously assess the reliability and effectiveness of AI-generated health information (18,19).
Generative chatbots: An overview
As mentioned previously, generative chatbots utilize NLP and deep learning techniques, a subset of ML that employ multi-layered neural networks to automatically learn complex patterns of data, to process and enable dynamic, near real-time conversations (16,20). These models are usually trained on extensive multimodal datasets, equipping them with key skills: contextual understanding (comprehension of background information), semantic parsing (transforming natural language to a machine-understandable representation) and coherent text-generation (16,20). Chatbots leverage self-attention mechanisms which transform the input information by dynamically weighting word importance, coupled with contextual understanding and semantic parsing to generate relevant responses. Figure 1 shows an example of how a generative chatbot (DeepSeek) handles the query of a clinician about a patient with headache.
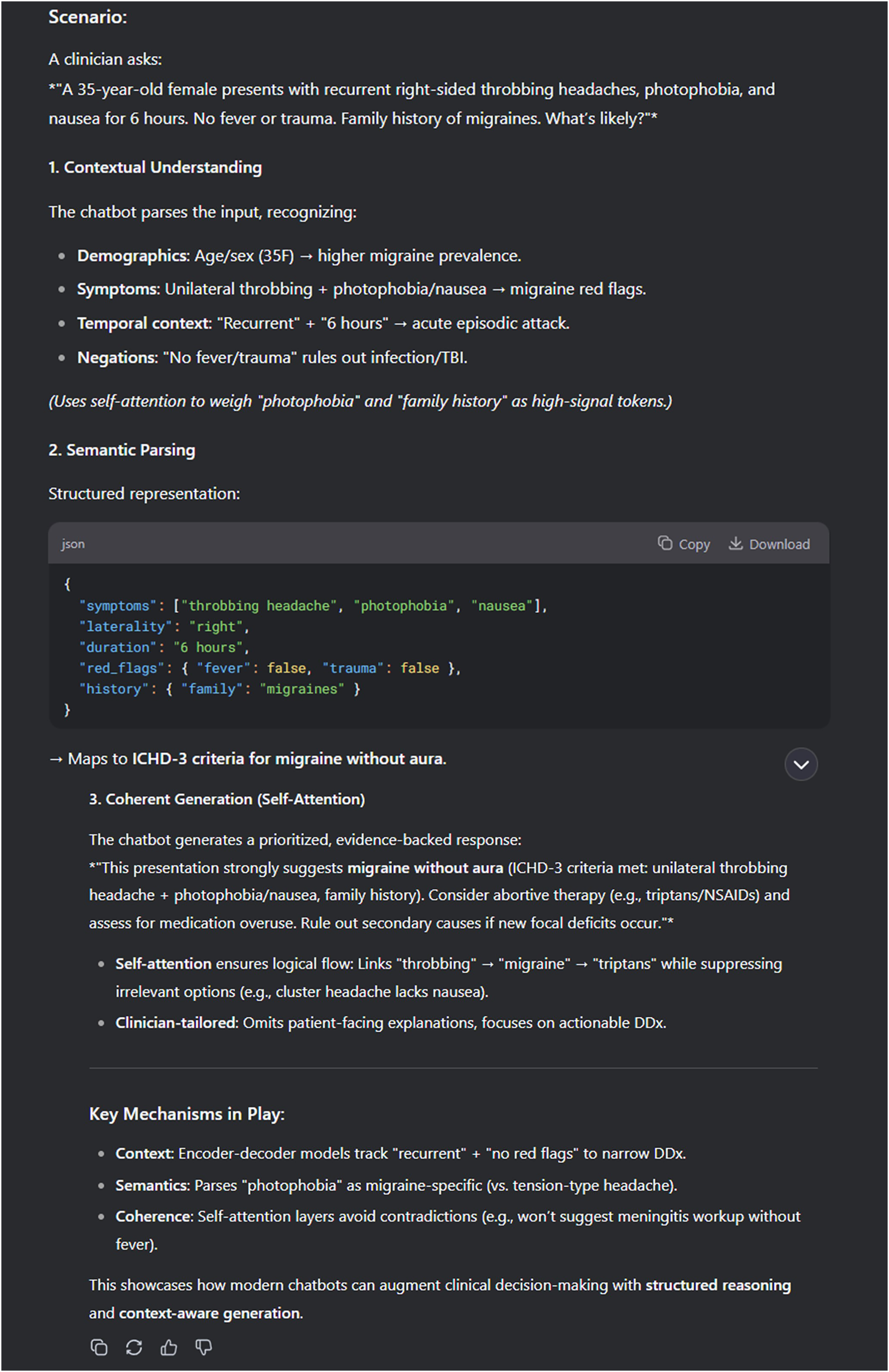
Example of how a generative chatbot (DeepSeek) handles the query of a clinician about a patient with headache, leveraging contextual understanding, semantic parsing and self-attention mechanisms.

Summary of how generative chatbots are being used in headache education and research, and possible new avenues. In the field of headache research, chatbots can accelerate the analysis of large datasets (e.g., omics, treatment response), assist in optimizing experimental setups, and support clinical trials (e.g., recruitment, patient assistance, data processing). In headache education, both healthcare providers and patients can benefit from this technology. In clinical settings, generative chatbots facilitate access to up-to-date information on diagnostic and treatment guidelines. Similarly, for patients, chatbots can offer lifestyle recommendations and address questions regarding their diagnosis and treatment.
Generative chatbots are powered by advanced AI systems called large language models (LLMs). These models learn how to communicate by analyzing extensive amounts of data in a first phase called unsupervised pre-training, allowing identification of language patterns (21). Then, the models go through a supervised fine-tune, where human trainers refine the chatbot responses by providing examples of context-dependent “high-quality” answers. Finally, reinforcement learning from human feedback is used to optimize response quality, clarity and helpfulness (16,20). Taken together, these steps ensure that generative chatbots generate coherent, relevant and safe responses tailored to the user needs/prompt.
Generative chatbots in headache education
Migraine presents unique clinical and management challenges. These include its episodic yet chronic nature, the heterogeneity of symptoms, the broad range of triggers, the influence of lifestyle factors such as sleep hygiene and physical activity, and its exacerbating factors such as medication overuse and concomitant psychiatric disorders (22,23). Moreover, given its high prevalence, meaningful impact on quality of life and lifelong course, generative chatbots have great potential in enhancing patient education by providing continuous accessible information (19). This is extremely important considering the frequently crowded consultations, with tight schedules and prolonged waiting lists, resulting in healthcare providers focusing more on the diagnosis of patients and selection of treatment, sacrificing the education and training of patients on the optimal management of the disease. Furthermore, widespread stigma and misinformation about migraine persist nowadays, such as attributing migraine to cervical arthrosis or not considering it a proper disease but a psychiatric disorder (24). These often result in unnecessary and inappropriate diagnostic procedures and lead to suboptimal management strategies (25). A chatbot designed for patients with primary headache disorders could address this by answering frequently asked questions (FAQ), personalizing content based on individual patient input, proposing potentially tailored guidance on common migraine triggers and lifestyle changes, thus enhancing patient engagement, potentially improving adherence (26,27). Patients can get personalized and interactive learning experiences. This has been shown in other disciplines, such as smoking habit cessation (28), vaccine hesitancy (29) or student motivation (30). They can easily access information on various topics or can get feedback on their performance on some aspects, such as headache frequency, acute treatment usage or presence of red flags (23). This may compensate for the high number of people living with headache, which makes a close follow-up challenging in the routine clinical setting. Nonetheless, AI may also use suboptimal references, therefore, feedback on the most accurate information, and selection of the most reliable sources is essential. Accordingly, Li et al. (27) assessed LLMs in answering patient queries on several aspects of migraine, including evaluation, diagnosis, treatment, follow-up, and prognosis. Most LLM responses were accurate and rated as “good” or “borderline” by experienced neurologists, with ChatGPT-4.0 showing the highest accuracy. However, these tools showed limited ability to discriminate between primary and secondary headache disorders, a crucial distinction for therapeutic implications and prognosis (27). These limitations are intrinsic to chatbot systems, as patients presenting with headache exhibiting atypical clinical features may require a direct medical evaluation to avoid missing secondary headaches, which can sometimes indicate life-threatening conditions (31).
Commonly used migraine-tracking applications have evolved to incorporate additional features beyond frequency and symptom reporting, including educational resources, FAQs, and brief learning pills (32). This could also promote a better understanding of the condition for patients. A recent review of commercially available headache applications identified Migraine Buddy, Migraine Coach, and Migraine Monitor as the most promising options due to their user-friendly design, clinical accuracy, and high levels of user engagement (33). However, it is worth highlighting that some of these applications are available only in English (33). These tools typically include daily diaries and personalized analytic reports that help patients identify potential migraine triggers, ranging from environmental and dietary factors to emotional stressors. Notably, apps like Migraine Coach allow users to record symptoms, triggers, and medication use while offering a light-sensitive interface, facilitating use even during migraine attacks. Additionally, some apps feature an AI-based chat function designed to answer common headache-related questions (33). Importantly, the information collected in apps and potentially chatbots could be shared with healthcare providers, enabling remote monitoring of outcomes and providing a basis for timely feedback and therapeutic adjustments (33). Such tools could theoretically add value in terms of convenience and cost savings, particularly for individuals in rural or underserved areas.
Chatbots could represent a valuable resource in migraine care, by also supporting the education and training of physicians across different healthcare settings, from primary care to specialized clinics in both low- and high-income countries (34). Training on headache disorders is often limited for healthcare professionals and still represents a gap in this field (6,9,10). These AI-based tools can help physicians stay updated with the latest guidelines and advancements, which is essential given the continuous development of novel treatments in the last decade (35). Furthermore, chatbots can simulate a patient visit, allowing physicians to practice diagnostic reasoning and management strategies in a virtual environment with various and different clinical scenarios. Through a chatbot, trainees could receive immediate feedback on decisions or treatment choices, allowing them to learn from mistakes without patient harm and reinforcing best practices in headache management (23). Regarding the possibility of providing treatment suggestions, studies have shown that ChatGPT is not yet a reliable tool. In a study by Moskatel et al. (18), ChatGPT assessed the efficacy of 47 migraine prevention drugs and provided supporting citations. While it correctly identified FDA-approved medications with grade A/B recommendations as effective, the evaluations of the remaining drugs were inconsistent and often inaccurate, and a percentage of the suggested supporting references were false.
Overall, while generative chatbots are not without limitations, particularly in diagnostic precision and accuracy, they represent a promising tool in the evolving landscape of migraine care. By enhancing patient education, supporting lifestyle modification, and aiding clinician training, these AI-driven solutions can complement traditional care, especially in resource-limited or high-demand settings (see Figure 2).
Generative chatbots in headache research
In headache research, generative chatbots can assist both preclinical and clinical studies, with one of the most immediate applications being literature review and data extraction. However, it is important to consider that the accuracy of chatbot outputs depends heavily on contextual understanding and the quality of training data, and as such, of how recent the data is. For example, ChatGPT models have undergone iterative advancements, resulting in each model having different training cutoff dates ranging from September 2021 in the case of GPT-3.5, to June 2024 for GPT-4.1 (36). Since these cutoff dates delineate the temporal scope of the extracted data, generative chatbots rely on Deep Research (i.e., real time web search), partner-supplied data (e.g., global newspapers, libraries) and the input of previous users. Additionally, studies have previously shown a high rate of “hallucinations”, a phenomenon exhibited by LLM, in which the system generates output that is coherent and plausible but incorrect, fabricated, or ungrounded in real-world data (37–40). It is crucial that researchers are aware of these limitations, and instruct chatbots to mine specific databases like PubMed to reduce the risk of misleading outputs and the influence of any biases present in non-scientific databases, particularly in relation to underrepresented or marginalized demographic groups. For instance, training on non-diverse datasets can lead to inaccurate diagnoses for minority groups. A chatbot trained mainly on Western patient data may misinterpret symptoms in Asian populations (41–44).
In laboratory settings, chatbots can serve as intelligent assistants by automating the retrieval of experimental protocols and standard operating procedures, facilitating real-time data entry, as well as sample tracking, contributing to data integrity and reproducibility. Moreover, coupled with molecular modelling computational tools, and omics or in silico databases, chatbots could be used to facilitate and accelerate the prediction of drug targets and drug development (43,45–47). In line with this, ChatGPT recently released an Advanced Data Analysis feature, that allows researchers to upload raw experimental datasets, and it automatically interprets the content for analysis by preprocessing the data, running statistical and basic ML models, and creating static and interactive charts, all using embedded Python code (48). Nonetheless, errors in analysis can occur, thus researcher oversight is vital to avoid misinterpretation of the data.
In clinical research, chatbots offer innovative solutions at multiple stages of the clinical trial process, from participant recruitment to engagement and monitoring. Recruiting eligible participants often involves extensive outreach and pre-screening. Chatbots can automate this process by engaging potential participants via websites or social media, asking eligibility questions, and providing study information in real time. This significantly reduces the workload of study staff and improves recruitment speed (48). Chatbots can facilitate informed consent by explaining the study protocol in accessible language, addressing questions, and guiding individuals through the documentation, thereby improving understanding and compliance (43). Previous studies exploring the responses to questions asked by patients observed that chatbots successfully provided empathetic and practical advice (49,50).
Chatbots can also support clinical trials by enhancing data collection, particularly of patient-reported outcomes. Traditional methods, such as paper diaries, phone calls or clinical visits, are prone to recall bias, low compliance, and incomplete data. In a recent cross-sectional survey, patients were asked about their willingness to interact with a chatbot and more than 80% responded that they would agree to it, particularly during clinical trials (51). In headache research, where outcomes rely heavily on natural language descriptions rather than test results, chatbots are of great promise due to their ability to parse free-text entries. Recently, an information extraction model was developed, and showed high accuracy at extracting headache frequency from free-text electronic health records (52). Patients could interact with chatbots via platforms on smartphones, tablets or computers to log headache episodes, symptoms, triggers, medication use and response to treatment, drastically reducing the time it would take to process patient data (48). Furthermore, unlike static forms, generative chatbots can adapt their questions based on previous responses, personalizing the data collection process. For example, if a patient reports a migraine with aura, the chatbot could follow up with targeted questions about visual disturbances, duration, or precipitating factors, therefore providing an intuitive, conversational interface that encourages real-time symptom tracking, improving the relevance of the data collected. Moreover, chatbots could prompt users with reminders, reducing missed entries, increasing patients’ adherence and refining longitudinal tracking, crucial aspects for understanding patterns over time, and assessing treatment effectiveness (53). Researchers could also integrate ML backends to facilitate data preprocessing and analysis, and potentially identify emerging patterns in headache presentation, triggers, and treatment efficacy. This bottom-up, data-driven approach offers a new paradigm for hypothesis generation (54,55). Furthermore, chatbots could monitor participant responses for signs of adverse events and notify clinical staff when necessary, this would not only improve safety but also ensures data integrity throughout the study. Nonetheless, it is crucial to develop tools and policies to safeguard patient data, ensuring that no identifiable data is exposed, thus compromising patient privacy (48,51).
In summary, as seen in Figure 2, generative chatbots have great potential in assisting headache research by facilitating literature review, as well as data extraction and processing, enabling the generation of novel hypothesis and the development of new therapeutic avenues. Moreover, chatbots can support clinical studies by accelerating the recruitment of patients, increasing patient adherence, refining longitudinal tracking, and potentially identify emerging patterns in disease presentation and response to treatment. Nonetheless, risks such as hallucinations, potential bias and concerns about data privacy require structured continuous evaluation frameworks, targeted model development, human oversight and safeguarding mechanisms to ensure data protection. With responsible development chatbots are poised to meaningfully advance medical research from bench to bedside, and beyond.
Beyond headache education and research
Benefits for clinical practice settings
Several tools that can be used for headache education and research can also be transferred to clinical settings. For example, chatbots could serve as a first step in the evaluation of patients. They can collect clinical information, including prior history, the headache phenotype, accompanying symptoms and the efficacy of previous treatments. Prior studies show promising results, with better accuracies in headache diagnosis when compared to other neurological disorders, which could be associated with the younger age of headache patients (56). Even though, in the present time, chatbots are not skilled enough to substitute the evaluation of a clinician (57), they can save time and optimize the consultation flow, to focus more on aspects that cannot be retrieved by a device, such as the physical examination of the patient and the clarification of some terms that may result misleading (e.g., light-headedness, unsteadiness, dizziness). The retrieved information can be supervised and corrected by the healthcare provider (58), and if directly stored, it may be highly useful for the elaboration of the consultation report and the acquisition of data for quality monitoring and research purposes. By integrating generative chatbots in headache-tracking applications with electronic health record and real-time data (e.g., physical activity, vital signs or sleep patterns), this could facilitate the detection of different patient profiles (59–61). This passive collection of large amounts of data can be a scientific revolution (62).
Challenges in clinical practice settings
AI is causing significant excitement, although in most places, in some respects, it is still more a hope than a reality. In many settings, multiple daily aspects of clinical practice are still quite archaic, such as paper reports, prescriptions or face-to-face appointments (63). The information technologies’ progress is asymmetric, and there are multiple software programs that are not always user-friendly or agile. The integration of AI-driven tools in these obsolete settings is truly challenging and may constitute a technical advancement comparable with the written post jumping to the smartphone, without passing through the conventional telephone. In addition, the number of publications addressing the usage of AI in healthcare is increasing exponentially, but in many settings, its use is still testimonial. Other important barriers are their free use, and that they are not always fully intuitive. Most headache patients are relatively young, but both elderly patients and children may require some specific adjustments or guidance in the use of chatbots, to make them fully deployable and valid (64,65). They may also increase the gap between underserved populations and high-income settings since many users from resource-constrained settings may not have the necessary devices or networks to connect to these systems, and this may worsen the inequity regarding the access and use of headache therapies (66,67). Another concern is that patients may perceive chatbots as hostile tools, if they do not capture user feedback, or require multiple questions and queries. In the middle of a headache attack, interaction with a chatbot may not be preferred, even more so if the patient is experiencing cognitive or speech difficulties(68,69).
A crucial consideration is the importance of contextual understanding. Healthcare providers frequently ask the same question multiple times with different wording, as some features may significantly change the work-up of the patients (70). For instance, the presence of orthostatic changes, even if the rest of the picture indicates a migraine-like phenotype, may suggest a cerebrospinal fluid related disorder, and worsening by standing up may be confounded by routine physical activity (71). Another common example is the response to acute treatment. Some patients may perceive as “normal” a decrease in the pain intensity, when the expected outcome is the complete pain resolution, ideally within 1–2 h (72,73). This degree of response, in the absence of adverse effects, may not be easily recognized by a chatbot, since human communication should be adapted to the target, and not all patients may have a similar background, educational level or knowledge of the disease.
As previously mentioned, one of the great challenges of chatbots is whether the retrieved information is accurate and reliable enough. As has been criticized in other domains, some answers may be inaccurate (74–76). Conversely, it has been shown that healthcare providers can also commit mistakes in the classification of headache patients (77), and AI could overcome some of these (78). Therefore, the validity of information is key, since headache disorders are still diagnosed based on clinical features and not on biomarkers (70). Most importantly, there are ethical concerns that require the development of safeguarding systems. Theoretically, most tools have been developed in accordance with the ethical guidelines that ensure safety, privacy, transparency and technical robustness (79). However, some of these AI-driven tools incorporate the feedback they receive into their “armamentarium”, so the inclusion of certain data can pose a threat in data privacy. Despite the reassurance of the companies that all the systems have the highest safety standards, both patients and healthcare providers may not be fully convinced and may be reluctant to share or provide certain data.
Another limitation of generative AI chatbots is that, compared to classical ML approaches, they offer greater flexibility in NLP but may lack the reproducibility and task-specific robustness that structured-data models provide, particularly for applications like treatment response prediction (14,80). While the flexibility of generative AI chatbots offers clear benefits in patient education and interactive engagement, single-purpose tools such as those designed to predict responses to preventive treatments, including newer target-specific treatments like anti-CGRP drugs or combination therapies, may be more important for clinicians in supporting clinical decision-making (14,80–82).
Despite their potential, generative AI chatbots in headache care have yet to undergo real-world validation. Key metrics to assess their effectiveness would include diagnostic accuracy aligned with ICHD-3 classification criteria, as well as improved treatment adherence among patients engaging with chatbot-based interventions (83).
Finally, a remaining threat is that AI may substitute human intelligence. This does not refer to a battle between humans and machines, but the insufficient and inadequate training of students and residents, that should use AI as an aid, and not as a replacement of their clinical abilities and critical thinking (84). With great power comes great responsibility, and AI should be used wisely by both patients and healthcare providers, especially in the beginning of this new era.
Future directions and conclusions
Future developments in AI will prioritize multimodal integration, enabling generative chatbots to understand and process diverse inputs such as speech descriptions of headache characteristics and associated symptoms, visual diagrams of pain localization and electrophysiological and neuroimaging metadata. Healthcare-focused chatbots could correlate those inputs to refine differential diagnoses. Moreover, headache-specific chatbots pre-trained on curated databases (e.g., ICHD-3 criteria, real-world electronic data, evidence-based therapeutic guidelines) would enhance patient education and clinical precision. These models will leverage hierarchical self-attention mechanisms to discern patterns in complex or rare headache disorders (e.g., distinguishing a first episode of migraine aura from seizure-related phenomena). The use of collaborative learning protocols, also known as federated learning, privacy-focused systems that allow AI models to train without exchanging sensitive data, would ensure continuous refinement of generative chatbots across multicenter sites without compromising data privacy (85,86). To further protect the private data of patients, anonymized data collections schemes (e.g., clustering-based anonymization) need to be implemented in the healthcare data collection process (87).
For headache chatbots to hold transformative potential for global health equity, particularly in underserved regions with limited access to headache specialists, they need to be easily deployed via low-bandwidth mobile interfaces (67). They could triage patients in remote settings using symptom-checking algorithms and guide local providers through evidence-based management steps. However, successful implementation will depend on structured collaborative frameworks uniting AI developers, clinicians, researchers, patient advocacy groups and other stakeholders (86); furthermore, multilingual adapted AI tools are required, since most chatbots are currently only available in English.
Robust governance must address the inherent risks of using AI in healthcare. Clinical validation guidelines remain essential for regulatory approval (e.g., FDA/EMA oversight) to achieve diagnostic accuracy and bias mitigations (88). Strict transparency protocols should require headache chatbots to disclose confidence intervals for recommendations, cite primary literature, and log decision pathways for auditor review (88,89). Additionally, accountability mechanisms must be embedded to prevent AI hallucinations, constraining outputs to verified evidence-based medical knowledge (90,91). Ethically, developers must prioritize algorithmic fairness to prevent disparities in care (e.g., ensuring models account for gender/racial variations in headache presentation) and establish clear liability structures for potential errors. Despite all the promising benefits of implementing chatbots in the headache field, excessive use could lead to diagnostic over-reliance and long-term deterioration of essential cognitive abilities such as critical thinking, analytic acumen and creativity (92).
In conclusion, generative AI chatbots present a unique opportunity to advance headache management by addressing key challenges in both education and research. Focused developments and rigorous evaluation are essential to harness their full potential in revolutionizing headache understanding and care. However, a delicate balance between benefiting from AI assistance and avoiding over-reliance risks is needed to integrate these tools effectively in headache research and clinical practice.
Article highlights
Generative AI chatbots present a unique opportunity to advance headache management by addressing key challenges in education and research.
Robust ethical frameworks and fostering strong user-developer partnerships are needed to fully harness the use of chatbots in the headache field.
Future success depends on developing specialized headache-specific chatbots, integrating multimodal capabilities, and expanding to underserved populations.
Footnotes
Declaration of conflicting interests
The authors declare that there are no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
