Abstract
Background
Racial disparities in migraine have been reported in the US. Migraine in African Americans (AA) is more frequent, more severe, more likely to become chronic and associated with more depression and lower quality of life compared to non-Hispanic Whites (NHW). It is possible that racial differences in prescribing practices contribute to these differences, but little is known about the quality of migraine prescribing patterns in the US or whether racial differences exist.
Objective
To determine if racial differences in quality of migraine medical prescription care exist.
Methods
We used data from the National Ambulatory Medical Care Survey to estimate differences in the use of migraine prophylactic and abortive medications by race. Quality of migraine care was defined using the American Academy of Neurology Headache Quality Measure Set (AAN-HQMS). Patients were assigned to one of four categories representing the overall quality of evidence for their abortive and prophylactic medications using the AAN-HQMS. We hypothesized that there would be suboptimal migraine treatment in minority populations. Racial comparisons were made using descriptive statistics after applying NAMCS survey weights.
Results
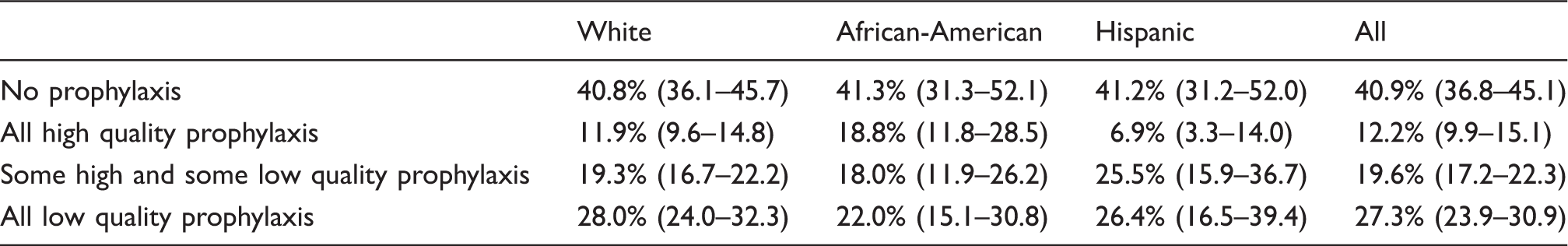
Two thousand, eight hundred and sixty visits were included in the study, representing approximately 50 million migraine visits in the US from 2006–2013. In all, 41.3% of AA, 40.8% of NHW, and 41.2% of Hispanic (HI) patients received no prophylactic treatments (p = 0.99). A total of 18.8% of AA patients, 11.9% of NHW patients, and 6.9% of HI patients received exclusively Level A prophylaxis (p = 0.30). A total of 47.1% of AA patients, 38.2% of NHW patients, and 36.3% of HI patients received no abortive treatments (p = 0.23). In total, 15.3% of AA patients, 19.4% of NHW patients, and 17.7% of HI patients received any Level A abortives (i.e. triptans or Dihydroergotamine; DHE, p = 0.64). A total of 15.2% of all patients had a prescription for opiates, but there were no racial differences.
Conclusions
Migraine may be undertreated with prophylactic medications. Level A acute analgesics may be underused and opiates overused. No major racial/ethnic differences in abortive or prophylactic treatment were identified.
Introduction
Headache is a leading reason for medical consultation, especially for neurological evaluation (1,2). Tension type headache and migraine are ranked as the second and third most common prevalent disorders, respectively, and migraine is the seventh-highest specific cause of disability worldwide (3). Several medications have been shown to effectively treat and prevent migraine, but the quality of evidence for these medications varies. The American Academy of Neurology (AAN) Headache Work Group recently defined quality measures summarizing the varying evidence and prioritizing some medications over others (4).
In the US, marked racial and ethnic differences in migraine and quality migraine care exist. Data from the American Migraine Prevalence and Prevention Study suggest that probable migraine is more prevalent in African Americans (AA); however, migraine is more prevalent in non-Hispanic Whites (NHW) than AA (5,6). Yet in AA, health care services for migraine treatment are less utilized, follow-up appointments are terminated more regularly, inaccurate diagnoses are more common, acute migraine attack medications are prescribed less frequently, and mistrust and lower quality communication with physicians is reported (7). Moreover, the burden of migraine is increased in AA: Migraine is more frequent, more severe, more likely to become chronic and associated with more depression and lower quality of life compared to NHW (8,9). Given that, when treated, AA appear to respond to medications as well as NHW (9,10), high quality treatment may reduce these disparities.
One possible explanation for the greater burden of migraine in AA is that AA receive lower quality medication treatment for migraine, yet little is known about racial differences in the quality of headache medication use. This likely reflects that, prior to the AAN’s recently published headache measure set, measuring quality of headache care was a major challenge. Thus, we sought to estimate racial differences in migraine treatment. We hypothesized that racial differences in the use of high quality abortive and prophylactic medications would exist in ambulatory care settings and the quality of medical treatment for migraine disorders as defined by the AAN Headache Quality Measure Set would be suboptimal in minority populations. We tested this hypothesis using nationally representative data.
Methods
Dataset/inclusion criteria
The National Ambulatory Medical Care Survey (NAMCS) is a nationally representative survey that uses a three-stage sampling design (geographic regions, physician practices stratified within specialties, and patient visits within practices) to characterize outpatient, office-based care (11). It is a sample of all medical care delivered in an ambulatory care setting. In a typical year, NAMCS will include data on 30,000–50,000 actual visits representing upwards of 900 million outpatient visits in the US. For this study, we analyzed all headache visits for patients over 18 years of age in NAMCS from 2006 to 2013. Headache visits were identified using ICD-9-CM codes 346.xx (12). Race and ethnicity were recorded by the provider or the provider’s staff (13). Individuals were assigned to one of three race/ethnicity categories based on these assignments: a) NHW; b) AA; c) Hispanic (HI, including individuals that reported AA race and Hispanic ethnicity). Individuals that reported other race/ethnicity were excluded due to small sample size. Institutional review board exemption was obtained from the University of Michigan Health System.
Identifying and classifying medications
NAMCS records up to eight medications for each patient visit, which are then assigned a unique identifier based on the medication name (14) and then assigned to medication categories using Lexicon plus a proprietary drug database. This classifies each medication by the components in that medication, and by the category of components in a medication. As an example, Treximet is assigned the unique identifier 08197, and classified into drug categories “non-steroidal anti-inflammatory agents” and “antimigraine agents” based on its components, naproxen and sumatriptan.
For both prophylactic and abortive medications, an overall category was then assigned for whether a patient’s potentially migraine-related medications would be classified as high quality based on the American Academy of Neurology’s Headache Quality Measurement Set (AAN-HQMS) (4). These quality measures define specific medications that are recommended, based on evidence, as high quality treatments both as migraine abortives (Measure 1) and as migraine prophylactic agents (Measure 3) Plausible migraine abortive agents or prophylactic agents were identified based on a review of the literature, and each of these agents was determined to be a “high” or “low” quality medication based on the AAN-HQMS. Then, each patient was assigned overall headache quality scores for both their abortive and prophylactic regimens.
For abortive agents, subjects were assigned to one of four categories: a) No abortive agent prescribed; b) all high quality abortive agents; c) some low quality abortive agents; or d) any opiate agent. The number of patients that received some low quality and some high quality abortive agents was relatively small, thus this group was combined with the group that received all low quality abortive agents to simplify interpretation. To reduce the likelihood that patients may have been prescribed an abortive agent for a non-migraine complaint, subjects were excluded from the abortive measure if they had any of a broad set of musculoskeletal pain diagnoses assigned during their visit (ICD-9 710-739 and 338).
For prophylactic agents, subjects were similarly assigned to one of four categories: a) No prophylactic agent; b) all high-quality prophylaxis; c) some low quality prophylaxis; d) all low quality prophylaxis. As with abortives, it is difficult to confidently determine that a medication was prescribed specifically for migraine or whether it was for another purpose. To explore this possibility, we repeated our primary analyses after excluding all patients that had a hypertension diagnosis recorded on the NAMCS survey instrument.
Statistical analysis
The study population was characterized with survey-weighted descriptive statistics on baseline factors measured in NAMCS and the number of visits by race. Pearson chi-squared tests were used to compare abortive and prophylactic medication categories across all race/ethnicity categories. Secondary analyses included separate comparisons of prophylactic and abortive medication categories for AA and HI compared to NHW and for individual medication categories by race/ethnicity. To determine if racial differences in care may be due to geography, we also repeated our primary analyses after accounting for whether the patient resided in a metropolitan statistical area (MSA) by performing logistic regression analyses adjusting for race and MSA. Analyses were performed in Stata 14. (StataCorp 2015. Stata Statistical Software: Release 14. College Station, TX: StataCorp LP).
Results
Patient/visit characteristics by race/ethnicity.

Quality of abortive and prophylactic medication use
Quality of abortive medication use by race (proportion (95% CI)).

Quality of preventive medication use by race/ethnicity (proportion (95% CI)).
Discussion
Contrary to our primary hypothesis, we did not find that lower quality abortive or prophylactic medications were prescribed to AA compared to HI or NHW. In fact, we found that AA seen in ambulatory care settings were slightly more likely to receive high quality prophylactic medications than NHW and HI. Our data also suggest that there are major opportunities to improve the quality of headache medication prescribing in the United States, as less than a quarter of migraine patients received all high quality abortive or prophylactic medications. Improving medication prescribing patterns may be a high yield strategy to reduce headache burden.
There is considerable room to improve headache abortive prescribing patterns – there are nearly as many migraine patients receiving opiates as there are patients receiving level A abortive medications. Opiate-related mortality is rapidly increasing in the United States (15). The argument against opiate use for migraine is strengthened by the observation that it is associated with more severe headache-related disability, symptomology, comorbidities (depression, anxiety, and cardiovascular disease and events), greater need to see health care providers and high risk for medication overuse headache (16,17). Moreover, most evidence suggests that opiates are, if anything, less effective than non-opiate alternatives (4,18). Given the considerable risks of opiates and the lack of evidence of increased efficacy, opiates should be used rarely, if ever, for migraine. Interventions to reduce opiate use in the migraine population are urgently needed.
Similarly, our findings reiterate prior findings that migraine prophylaxis agents are likely underutilized (19). We add to this body of work by showing that low quality agents are often used. Among patients that receive a prophylactic agent, it is almost twice as likely that they will receive exclusively agents with low-quality evidence as it is that they will receive agents with only high-quality evidence. Additional work is needed to understand the reasons underlying these prescribing patterns to inform future initiatives to improve the quality of headache treatment and ultimately to improve headache outcomes. In addition, this is an area where the AAN quality measures, if widely implemented, may help to improve care. If these suboptimal prescribing patterns contribute to the conservative estimate of more than $31 billion in headache expenditure in the United States (US) (20,21), it would add an important economic rationale to the clinical rationale for improving prescribing practices.
While overall migraine prescribing patterns are suboptimal, we did not find major differences by race. It is possible, though, that more modest racial differences in abortive prescribing exist, but that we lacked statistical power to identify those differences. For example, AA were four percentage points less likely to receive all high-quality abortive agents and HI five percentage points less likely to receive all high-quality prophylactic agents compared to NHWs, yet neither difference was statistically significant. Nevertheless, if these differences represented true differences, they would have important clinical and policy implications. While prior data have been mixed on opioid use in minority populations in the emergency department, our findings are consistent with population-based study designs of analgesics in the emergency department finding no statistical differences in opioid prescriptions by race (22).
If prescribing patterns do not explain disparities in headache outcomes amongst AAs, what other theories exist? Our data cannot fully elucidate this question; however, some subtle trends merit consideration. Amongst the entire headache population of headache visit, AA visits account for only 10% of all NAMCS headache visits. Given their larger representation in the population and higher yet representation expected given the increased incidence of headache in AA, this may represent an inadequate number of visits. Consequently, one hypothesis is that the primary cause of disparities is that AA are not seen in the ambulatory setting for headaches – either they are not receiving any care for headaches, or they are being disproportionately seen in emergency departments where prophylactic medications are rarely prescribed. Also, we only assessed patients with a diagnosis of migraine, so if AA are less likely to receive a migraine diagnosis, that too could explain this pattern (e.g. AA receive generic headache, ICD-9 “784.0”, diagnoses more frequently, when migraine diagnoses are warranted).
Cost-related non-adherence is another plausible explanation. Many migraine medications are relatively costly, and if AA are less likely to be able to afford these medications, then the right prescription will not lead to better outcomes (23). Studies to understand racial and ethnic minorities’ beliefs, perceptions, and behaviors related to migraine and other headache disorders, and the care thereof, are needed. In addition to these access factors, other considerations such as genetics, epigenetics, social determinants, headache literacy, access to non-pharmacological modalities and other care providers may be possible explanations in caring for those with migraine (24,25). In addition, minorities are underrepresented in migraine clinical trials. Minority underrepresentation in clinical trials may be a link to understanding race-based differences in migraine expression, treatment responses and medication toxicity among different races (26). Future studies that explore other mechanisms of disparities in headache and migraine are needed.
Our study has limitations. We had no details on headache severity and duration. Also, we cannot completely ascertain the reasons why patients are given medications. However, we adjusted for hypertension due to the potential overlap of commonly prescribed anti-hypertensive medication and the recommended prophylactic medications within the anti-hypertensive class. In addition, race/ethnicity was not self-reported, which could bias our results. There was not enough power to estimate statistical significance in other racial/ethnic groups due to small sample size, which limited our ability to analyze other races/ethnicities. The study may be underpowered to detect differences in a world where only a small minority of people with migraine receive preventive medication. Another limitation is that this is a cross-sectional study. It may be that longitudinal care is a key factor contributing to positive headache outcomes, and this may differ by race. In addition, there was no controlling for socioeconomic status such as household income. Exclusion of patients who had other pain diagnoses may eliminate patients with comorbidity who have more severe illness, and if they are overrepresented in any of the groups, a difference may be less likely to be detected. However, we performed a secondary analysis including pain diagnoses. Including pain diagnosis added the use of opiates, but did not significantly change our primary findings. Again, our population database is of visits and not those with headaches per se. Nevertheless, given the data, our study provides a baseline for subsequent headache quality improvement initiatives based on the recently published headache quality measure set by the American Academy of Neurology (4).
Conclusions
We did not find evidence to support our primary hypothesis that racial differences in prescribing patterns contribute to headache disparities. More generally, we found that migraine disorders are likely undertreated with prophylactic medications. Similarly, suboptimal migraine abortive prescribing patterns exist – migraine patients receive opioids about as commonly as they receive medications with high quality evidence. There is apparent underuse of medications with high quality evidence. Understanding what drives these prescribing patterns and improving overall migraine prescribing should be a central concern for headache care practitioners, quality improvement initiatives and a target of future interventions.
Clinical implications
There is apparent underuse of medications with high quality evidence for migraine. Patients in the US with migraine receive prescriptions for opioids about as commonly as they receive prescriptions for medications with high quality evidence for migraine treatment. Migraine disorders are likely undertreated with prophylactic medications.
Footnotes
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: James F Burke has received payments from Astra Zeneca for case adjudication in the SOCRATES trial and for reviewing legal case materials. Larry Charleston IV reports no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: James F Burke is funded by NIH grants K08 NS082597 (NINDS), and R01 MD008879 (NIMHD).
