Abstract
Background
It was suggested that right-to-left shunt (RLS) may be highly prevalent in chronic migraine (CM) patients, indicating that patent foramen ovale (PFO) might be an aggravating and chronifying factor of migraine. Since a high proportion of chronic migraineurs also have medication-overuse headache (MOH), one may wonder if they have a more severe form of the disorder and more frequently a PFO.
Objective
The objective of this study is to determine the prevalence and grade of RLS in patients suffering from CM and MOH.
Methods
A cross-sectional multicenter study of air-contrast transcranial Doppler was conducted in 159 patients with CM (n = 57) or MOH (n = 102) attending a tertiary headache clinic.
Results
The prevalence of RLS in CM was 37% (11% large shunts) and in MOH patients 31% (13% large shunts). There was no difference between the two groups (p = 0.49).
Conclusion
RLS prevalence in CM is within the upper range of those reported in episodic migraine without aura or in the general population, and not higher in MOH. PFO is thus unlikely to have a significant causal role in these chronic headaches.
Keywords
Introduction
A right-to-left shunt (RLS) is an abnormal communication between right (venous) circulation and the left (arterial) circulation (1). The most frequent cause of RLS is patent foramen ovale (PFO) (2). Occurrence of PFO in the general population ranges from 15% to 35% (3,4). People with PFO have an RLS that occurs either at rest or with Valsalva maneuver.
Migraine with aura (MA) has been associated with PFO in multiple studies (50%) (5–8) whereas migraine without aura has shown mixed results (5,9–11). Collectively, these studies showed only a weak association between PFO and migraine, but PFO may be relevant in highly selected subgroups of migraine patients.
Chronic migraine (CM) is the diagnosis for patients who have at least 15 days of headache per month and at least eight of these days fulfill criteria for migraine (12), while medication-overuse headache (MOH) is a chronic headache disorder associated with the overuse of acute headache drugs (13). CM and MOH are very disabling, complicate the clinical course in 2–3% of migraineurs per year in the general population (14) and form the bulk of patients seen in tertiary headache clinics. Nahas et al. (15) found that RLS was more common (66%) in CM patients, but this finding has not yet been replicated.
CM and MOH are at the most severe end of the migraine disability spectrum. An established risk factor for both is high attack frequency (16). The study by Nahas et al. (15) suggests that RLS, and thus most likely PFO, might be associated as a possible risk factor with CM. Whether this could also be the case for MOH is not known. Despite common epidemiological and pathophysiological features between CM and MOH, differences have also been reported, for instance regarding cortical excitability changes (17). About 50% of MOH patients reverse to episodic migraine after withdrawal, but the others do not (18), suggesting that they may suffer from CM. If PFO were associated with CM and not with MOH, one might expect a lower RLS prevalence in MOH patients. If PFO were rather a risk factor for high attack frequency, RLS prevalence could be similar in both conditions.
The objective of the present study was therefore twofold: to replicate the study by Nahas et al. (15) by determining the prevalence and grade of RLS in patients suffering from CM and to compare CM with MOH patients. To achieve these objectives we used air-contrast transcranial Doppler (TCD).
Methods
Study design
This was a cross-sectional multicenter study involving three European Headache Centers: the Headache Research Unit, Department of Neurology and GIGA-Neurosciences, Liège University; Danish Headache Center and Dept. of Neurology, Glostrup Hospital, University of Copenhagen; and Department of Neurology, University of Duisburg-Essen.
Study population
All patients gave a detailed clinical history including family history, disease onset, duration and comorbidity. Inclusion criteria were: patients diagnosed with CM or MOH and migraine according to the International Headache Society (IHS) criteria (12), and age between 18 to 65 years. Exclusion criteria were: subjects with a known history of cerebrovascular disease, paradoxical embolism, or decompression illnesses. We also excluded patients suffering from chronic tension-type headache, new daily persistent headache and hemicrania continua.The study was approved by the ethics committee of the Citadelle Hospital, Liège (n° 950) and the Ethics Committee of Copenhagen (H-D-2008-132). All subjects gave informed consent to participate in the study.
TCD procedure
Air-contrast transcranial Doppler (cTCD) was used for PFO detection and was performed according to international recommendations (4,19). The procedure was performed in a supine position. An intravenous catheter was placed in an antecubital vein. The right (or left) middle cerebral artery was insonated with a 2-MHz pulsed Doppler probe over a temporal window at a 40–55 mm depth. Contrast medium = 9 ml saline + 1 ml air (flushed 10 × between two syringes) was injected intravenously. This procedure was performed three times: The first time during normal breathing, the second time during a five-second Valsalva maneuver that starts five seconds after the injection, and the third time is a repetition of the second injection with exactly the same procedures. cTCD monitoring was performed up to at least 25 seconds after injection. RLS during rest and Valsalva were graded according to the international four-point scale (20): 0 = no microbubbles, 1 = 1–10 microbubbles (small shunt), 2 = ≥10 (moderate shunt), 3 = curtain, no single bubbles (large shunt). We will present the data for small and moderate RLS (grades 1 and 2) during Valsalva combined because such shunts have little clinical relevance.
Statistics
The primary outcome was the prevalence of RLS in the two studied groups (CM and MOH). Chi-square was used to calculate statistical differences. No studies have indicated that age, sex or geographic location in Europe have an influence on PFO prevalence. We therefore assumed that it was acceptable to combine the data from the three headache centers.
Results
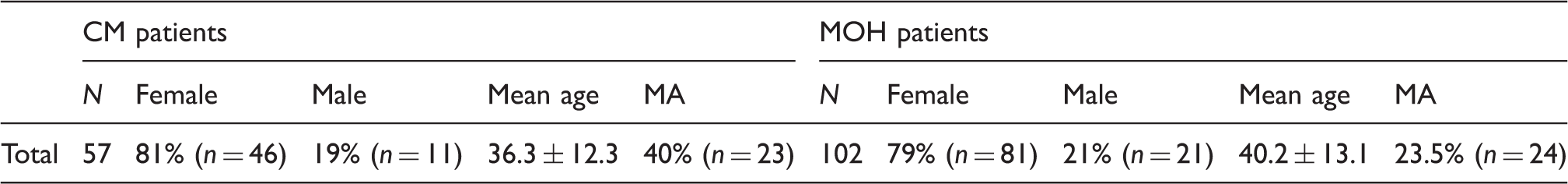
Sex, mean age and percentage of migraine with aura (MA) of the patients recruited with chronic migraine (CM) and medication-overuse headache (MOH).
Combined data from the participating centers (Liège, Essen and Copenhagen) of included patients with chronic migraine (CM) and medication-overuse headache (MOH) and detected shunts with percentage.

RLS: right-to-left shunt.
The prevalence of RLS was 37% in the CM group and 31% in the MOH group (Figure 1). Eleven percent of CM patients and 13% of MOH patients had a large RLS (grade 3). At rest 12% of CM patients and 15% of MOH patients had a small/moderate RLS (grade 1 and 2). 58% of patients who had RLS during Valsalva did not have RLS at rest, but all the patients who had RLS at rest had RLS during Valsalva (data not shown in the table).
Percentage of RLS with grading in CM patients and MOH patients during Valsalva detected by air contrast TCD.
The statistical comparison of RLS prevalence and grading between the CM and MOH groups revealed no difference (p = 0.52).
Discussion
The major outcome of the present study was that the prevalence of RLS was not different between CM (n = 57; 37% with 11% large shunts) and MOH (n = 102; 31% with 13% large shunts). There was, however, a higher proportion of migraine with aura patients in the CM group (40%) than in the MOH group (23%), which may have biased the CM prevalence data toward a higher value (5–8).
Using a similar TCD method, Nahas et al. (15) reported a 66% prevalence of RLS in chronic migraine patients (n = 131), which is clearly superior to that reported here (37%). The proportion of large shunts (grades IV and V of the Spencer logarithmic scale) was also larger (25.6%) than ours (11%). The proportion of patients with MA was similar (41%) to that of our CM group. We have no straightforward explanation for these differences, except that there might have been slight methodological differences including a different grading scale of RLS. Bias due to the inclusion of MA patients cannot account for the difference observed, as their proportion was almost equal in both CM groups (41% and 40%). Surprisingly, however, Nahas et al. (15) found no increase in RLS prevalence or grade in patients reporting an aura, which is at variance with the majority of MA studies (8,21,22).
Like in Nahas et al.’s study, a major weakness of our study is the lack of control groups of healthy volunteers and episodic migraineurs. As our major objectives were to replicate the findings of Nahas et al. (15) and to compare CM and MOH, we think that the study might nonetheless provide some interesting information and that the rather large number of patients included allows some cautious but thought-provoking comparisons with available historical data. Studies using transesophageal echocardiography (TEE) or TCD reported the prevalence of RLS in the general population to be between 15% to 35% (3,4). Using the cTCD method, a recent population-based case-control study reported a 41.5% prevalence of RLS in controls (19.5% large shunts) and 34.1% in episodic migraineurs without aura (16.3% large shunts) (23). In the latter study, number of controls (n = 41), sex ratio (female (F) = 78%/male (M) = 22%), mean age (48.9 ± 9.0 years), and range (27–69 years) were similar to our material. Taken together, available data suggest that there is most likely no major difference between the prevalence figures found by us in CM (37%) or MOH (31%) patients compared to the healthy background population. As far as large shunts are considered, their prevalence might actually be lower in our CM (11%) and MOH (13%) groups compared to controls in Küper et al.’s study (19.5%) (23).
Regarding the method, TEE has a high sensitivity (89%) and specificity (100%) for the detection of a PFO (24). TCD combined with Valsalva maneuver has a sensitivity and specificity of respectively 96.8% and 78.4% (25), suggesting that TCD is more sensitive than TEE. The slight difference between the two methods should be kept in mind but overall the method used in the present study is reliable.
Finally, it is still controversial whether PFO closure provides any benefit in migraine patients. Retrospective and prospective studies have shown positive results (6,26–28), but the only available randomized sham-controlled trial was negative (29), although methodologically criticizable. This area therefore still needs further investigations.
In conclusion, the prevalence and grade of RLS were not different between CM and MOH patients. In both groups they were within the range of those reported in episodic migraine without aura and in the general population. The present study therefore does not favor the hypothesis that PFO contributes significantly to the pathogenesis of CM or MOH.
Clinical implications
The prevalence of right-to-left shunts (RLS) is not different between chronic migraine (CM) and medication-overuse headache (MOH) and is within the upper range of those reported in the general population. PFO is unlikely to have a significant causal role in CM and MOH.
Footnotes
Funding
This study was sponsored by Coherex Medical Inc, USA.
Conflicts of interest
JS and MA were members of the advisory board for Coherex Medical Inc, USA.
