Abstract
Despite the frequency of videolaryngoscope use, to the authors’ knowledge, there are no publications exploring the role of playback video recording in real time to improve patient care. We present a patient with a difficult airway complicated by trauma during GlideScope® (Verathon Inc., Bothell, WA, USA) intubation. The injury was not recognised by any of the anaesthetic staff observing the intubation, and was only identified when playback video footage was viewed. This provided the opportunity for early ear, nose and throat surgical review prior to extubation. Airway trauma can be missed by the anaesthetist. Reviewing video playback footage at an appropriate time during the case may enable more timely recognition of airway injuries and, ultimately, improved patient care.
Introduction
Airway trauma following videolaryngoscope intubation is not uncommon, but it can be missed. Playback of recorded videolaryngoscope footage has been previously used both as a teaching aid and to identify abnormal glottic anatomy. In this case report, we describe the potential role of video playback in the early diagnosis of concealed airway injury, enabling timely and improved patient care.
Case report
A 26-year-old woman required an elective craniotomy for glioblastoma tumour excision. She had a significant past history of traumatic incomplete T8 paraplegia six years earlier, requiring a temporary tracheostomy. No documentation was available regarding previous upper airway management.
On examination, her airway was grossly normal with adequate mouth opening, thin neck and slightly reduced thyromental distance. Following induction of anaesthesia with intravenous remifentanil at 0.3 µg/kg/min, propofol target-controlled infusion at 4 µg/mL and rocuronium 50 mg, she was easy to facemask ventilate but was found to be a grade III view with standard laryngoscopy using a Macintosh 3 blade. She was successfully intubated atraumatically with a hyperangulated C-MAC® D-BLADE™ (Karl Storz, Tuttlingen, Germany) using a manually preformed hyperangulated stylet inserted into the tube to assist intubation. The case proceeded smoothly, and the patient was extubated uneventfully. Subsequently, in the recovery room, her Glasgow Coma Scale score deteriorated, and she developed new focal neurology. Computed tomography brain imaging confirmed an intracranial bleed at the operative site, requiring urgent return to theatre for evacuation.
Airway management for the reintubation was performed by the same anaesthetic Fellow as earlier in the day. Following induction of anaesthesia as before, a hyperangulated GlideScope® 3 blade (Verathon Inc., Bothwell, WA, USA) was used in accordance with the duty anaesthetist’s preference. A GlideRite® Rigid Stylet was pre-inserted into a size 7.0 mm internal diameter cuffed endotracheal tube. The intubation was additionally observed by an anaesthetic trainee, two anaesthesia consultants and three anaesthesia nurses. The four-step approach 1 was used to reduce the risk of soft tissue injury. A grade IIa view was initially observed on the screen. Intentional worsening of the view by pulling back the GlideScope® 2 whilst lifting the tube vertically upwards enabled successful intubation of the glottis, which was deemed atraumatic by all staff present. Oxygen saturation and haemodynamic parameters remained stable throughout. The afterhours anaesthetist arrived to accept handover midway through the case, and the anaesthesia Fellow exited the theatre.
Immediately after the case was handed over, for personal quality assurance, the intubation footage was played back on a computer screen by the anaesthetic Fellow. In a final snapshot of the video depicting withdrawal of the videolaryngoscope post successful re-intubation, the endotracheal tube was observed to have completely transected the anterior faucial pillar (see Figure 1).
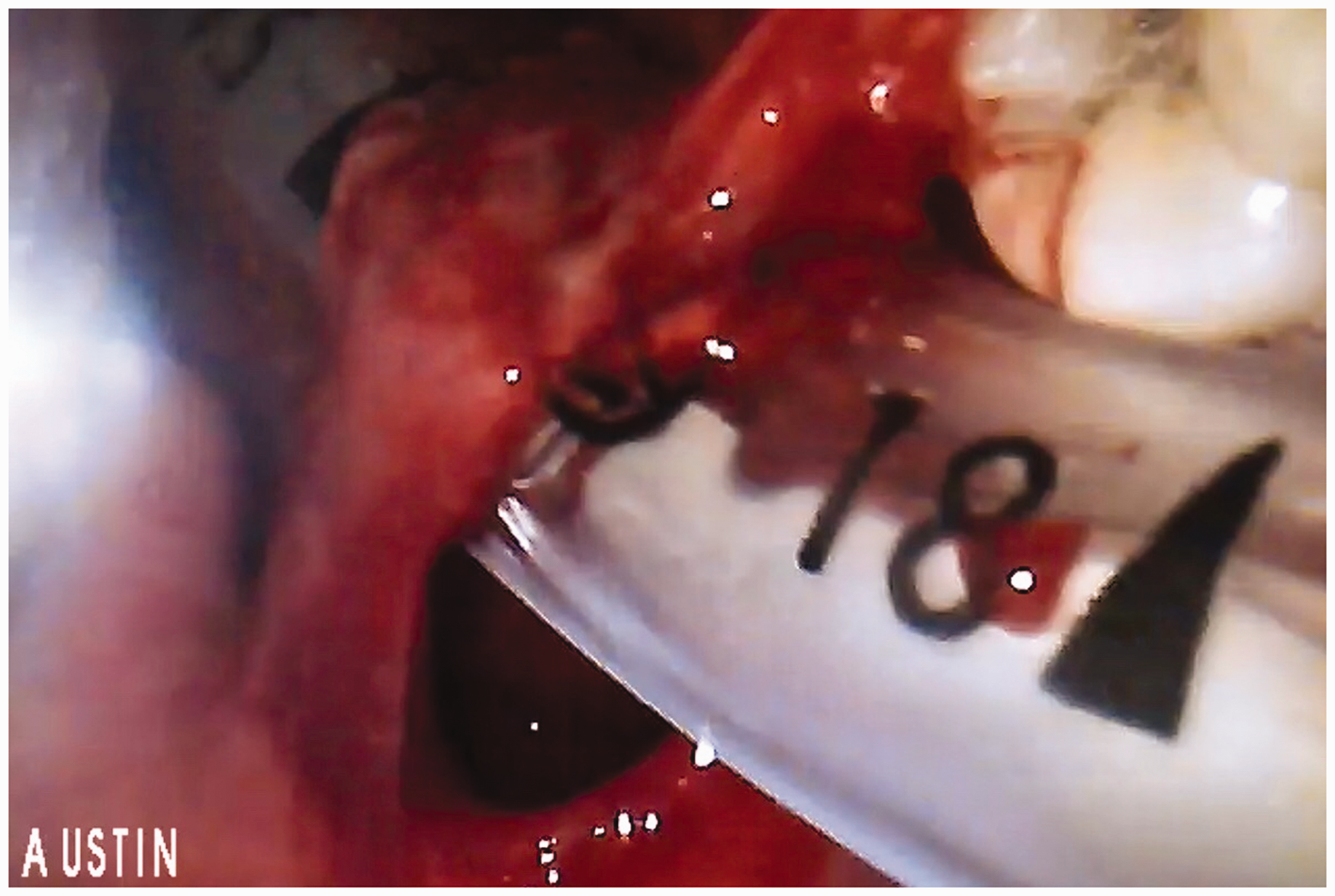
Final snapshot during playback of recorded videolaryngoscope footage depicting withdrawal of the laryngoscope and identification of soft palate injury. This injury was not recognised at the time of intubation.
Early referral was made to an ear, nose and throat (ENT) surgeon to review the playback footage and to assess the patient at the end of the case, immediately prior to extubation, who determined that the injury did not require surgical intervention. Post-extubation ENT assessment of the soft palate revealed no further injury. On day 1 review, the patient reported a sore throat, and on examination, the wound had completely closed. The sore throat resolved by day 2.
Full open disclosure was provided by the Fellow to the patient. The intubation video was played to the patient upon her request, and she provided written consent for use of the video material for educational purposes and for publication in a medical journal. A difficult airway letter was provided to the patient in the event of any future anaesthesia. This letter was also provided to the patient's general practitioner and included in her medical record.
Discussion
Soft tissue injury following intubation with a hyperangulated videolaryngoscope is well described,3–5 most frequently following use of the GlideScope®. 6 However, despite knowledge of this potential complication and the implementation of specific strategies 1 to minimise occurrence, such as direct observation of tube tip–stylet insertion until past the view of sight, 1 airway trauma following videolaryngoscope use can still occur. The incidence of injury may be far more common than previously appreciated. A recent prospective blinded randomised study involving post-intubation airway examinations by an ENT surgeon reported an incidence of airway injury of 21% following GlideScope® use. 7 Although frequently minor in nature, this is markedly greater than the 1% incidence of airway injury reported in previous retrospective studies.6,8
Iatrogenic airway injury following videolaryngoscope intubation has the potential to be missed at the time of the intubation.9,10 In this case, experts observing the intubation did not recognise that an airway injury had occurred. Not observing signs of injury during intubation does not eliminate actual injury, nor is it a reliable method of assessing severity of injury when it does occur. We therefore recommend that in addition to preventative measures, a clear strategy should be employed to identify or exclude airway injury formally, particularly when a hyperangulated blade is used. A hyperangulated blade may be more likely to be required in an inherently difficult airway, when the consequences of a missed complication are potentially more significant. Timely review of videolaryngoscopy footage should be considered as an important component of such a strategy. In this case, playback video review enabled early identification of an airway injury that was otherwise missed, and enabled prompt ENT involvement prior to extubation, consistent with surgical recommendations. 4
Conservative management was deemed appropriate in this patient. However, serious complications have been reported from videolaryngoscope intubation, including retropharyngeal injury 11 and post-extubation airway obstruction secondary to pharyngeal wall bleeding, necessitating emergency tracheostomy and surgery for haemostatic control. 12 In this case involving repeat difficult intubation and intracranial haemorrhage, delayed recognition of airway injury could have been particularly problematic. Protracted airway compromise would have made neurological assessment difficult and could have resulted in secondary brain injury.
The recording of videolaryngoscope footage has been previously used as a tool to aid teaching novices, 13 for identification of abnormal glottic anatomy14,15 and for patient reassurance. 16 However, to the authors’ knowledge, there are no published cases of recorded GlideScope® footage unmasking a concealed injury, and allowing the opportunity for prompt assessment, management and decision-making. There are competing priorities in the theatre environment, particularly immediately following intubation. The replay of recorded intubation footage at an appropriate time during the case may provide a key strategy to identify concealed airway injury, enabling timely and improved patient care.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
