Abstract
Background:
Balance is an important variable to consider during the rehabilitation process of individuals with trans-tibial amputation. Limited evidence exists on the balance abilities of people with trans-tibial amputation due to vascular causes.
Objective:
The purpose of this article is to review literature and determine if standing balance is diminished in people with trans-tibial amputation due to vascular causes.
Study design:
Literature review.
Methods:
Data were obtained from PubMed, Google Scholar, OandP.org, CINHAL, and Science Direct. Studies were selected only if they included standing balance assessment of people with unilateral trans-tibial amputation due to vascular causes.
Results:
The review yielded seven articles that met the inclusion criteria. The general test methodology required participants to stand still on force platforms, with feet together, while center of pressure or postural sway was recorded.
Conclusion:
According to the findings of this review, individuals with trans-tibial amputees due to vascular causes have diminished balance abilities. Limited evidence suggests their balance might be further diminished as compared to individuals with trans-tibial amputation due to trauma. Although the evidence is limited, because of the underlying pathology and presence of comorbidities in individuals with trans-tibial amputation due to vascular causes, one cannot ignore these findings, as even a minor injury from a fall may develop into a non-healing ulcer and affect their health and well-being more severely than individuals with trans-tibial amputation due to trauma.
Clinical relevance
Individuals with trans-tibial amputation due to vascular causes have diminished balance abilities compared to healthy individuals and individuals with trans-tibial amputation due to trauma. This difference should be considered when designing and fabricating prostheses. Prosthetists and rehabilitation clinicians should consider designing amputation cause-specific rehabilitation interventions, focussing on balance and other functional limitations related to comorbidities of amputation.
Keywords
Background
Successful performance of various activities of daily living largely depends on one’s capability to control balance. 1 Static/standing balance involves maintaining one’s center of mass (CoM) within the base of support while the body is at rest. 2 It differs from dynamic balance, where the individual is required to maintain their CoM within the base of support while the body is in motion. 2 Balance is controlled by the action of muscles which are in turn controlled by the brain through feedback it receives from the visual, vestibular, and somatosensory systems 3 and through feedforward strategies.4,5 Damage or reduced feedback to any of the sensory systems as a result of disease or trauma could affect balance. 6 For example, loss of sensory receptors below the knee as a result of trans-tibial amputation (TTA) will affect the feedback to the somatosensory system, disrupting balance in this population. However, the underlying cause of amputation could also affect residual limb sensation and further diminish balance in people with TTA due to vascular diseases (TTA-vascular) such as peripheral vascular disease (PVD) or diabetes.
In people with TTA-vascular, pre-existing sensory deficits such as peripheral neuropathy, on the amputated and non-amputated sides, may be present.1,7 Peripheral neuropathy can lead to a loss of peripheral cutaneous sensation and muscle spindle function, both of which may impair balance. 8 Consequently, in people with TTA-vascular with peripheral neuropathy of the non-amputated side, the loss of peripheral muscle spindle function reduces the individual’s ability to perceive ankle joint motion and reduces balance capabilities. In an effort to improve the sensory feedback from the residual limb, a person with a TTA is typically provided with a snug fitting total contact prosthetic socket, 9 wherein the cutaneous mechanoreceptors of the residual limb are in contact with the socket walls. However, the potential loss of cutaneous sensation at the residual limb in people with TTA-vascular could limit the feedback that is provided from the snug fitting socket. Additionally, the presence of peripheral circulatory complications in some individuals with TTA-vascular could prevent use of a snug fitting prosthetic socket.
In addition to the proprioceptive feedback loss in individuals with TTA, reduced leg muscle strength is also a comorbidity of the amputation and can result in reduced balance capabilities. Insufficient use of the lower limbs following amputation causes hypotrophy of the muscles 10 which leads to a deficit in their strength.10–12 Although no evidence is available on whether differences exist in the muscle strength of individuals with TTA-vascular as compared to those with TTA-trauma, evidence on individuals with diabetes (no amputation) suggests that lower limb muscle strength is significantly reduced as compared to individuals without diabetes.13–15 Diminished muscle strength has been associated with decreased balance.16,17 In individuals with TTA, the loss of a physiological ankle joint and corresponding musculature reduces their ability to utilize an ankle strategy for maintaining balance during quiet stance18,19 and they might have more reliance on a hip strategy to maintain standing balance. 19 Thus, the presence of weaker hip/thigh muscles could mean reduced balance in this population.
Furthermore, individuals with TTA present with reduced balance confidence compared to individuals without amputation. 20 Reduced balance confidence is associated with a limitation or restriction of activity and participation, 21 which can be detrimental to muscle strength, endurance, and balance. 20 Interestingly, Miller et al. 22 found individuals with TTA-vascular to have lower balance confidence than individuals with TTA-trauma. In a recent review, Ku et al. 23 explored the literature on balance control in individuals with lower extremity amputation and concluded that balance control decreases with a higher level of amputation, that is, individuals with trans-femoral amputation (TFA) have more impaired balance control than those with TTA. However, the authors did not differentiate between those with TTA-vascular as compared to TTA-trauma. Balance limitations in people with diabetic neuropathy and PVDs have been established.8,24,25 It is likely that these limitations are also present in people with TTA-vascular. The presence of comorbidities like insufficient sensory feedback, reduced muscle strength, and diminished balance confidence could predispose them to have reduced balance abilities as compared to people with amputations from other causes. Although it is understood in clinical practice that individuals with TTA-vascular have performance limitations, insufficient evidence exists. A comprehensive review of literature on standing balance in individuals with TTA-vascular is needed and could improve our understanding of the balance capabilities of this population and potentially inform rehabilitation strategies. The purpose of this article is to review literature to determine the standing balance capabilities of people with TTA-vascular.
Methods
Search strategy
An electronic search of databases was performed in November 2015 and was limited to PubMed, Google Scholar, OandP.org, CINHAL, and Science Direct. A comprehensive search was performed using a combination of the following search terms: vascular, amputation, balance, postural, sway, diabetic, below knee amputation, and TTA.
Eligibility
The search for articles was performed by one person. Articles were considered only if they met the following criteria: included people with unilateral TTA due to vascular diseases (PVD, diabetes) and measured standing balance. Standing balance measurement is defined as the recording of center of pressure (CoP) or postural sway while a person maintains his or her CoM within the base of support while the body is at rest. Articles were also selected if they compared the balance of people with TTA-vascular to people with TTA-trauma. Articles were excluded if they focused on balance control after a perturbation. No restrictions were placed on age, sex, prosthetic componentry, and time since amputation.
Review process
The review process began with an identification of the duplicate files. Following this, articles were screened based on their titles and abstracts. The initial exclusion decisions were based on this. Full texts of the selected articles were read and only articles meeting the inclusion criteria were selected. References of the selected articles were also examined. Rejected articles were re-examined to avoid any confusion created as a result of the title or the abstract.
Study quality
The methodological quality of the selected articles was assessed using the Downs and Black 26 checklist which was developed for both randomized and non-randomized control trials. The checklist consists of 27 questions pertaining to the quality of reporting, internal validity, external validity, and power of the studies. The maximum possible points were 31, with higher scores representing better quality. Most questions were answered as a yes “1” or no “0.” Some questions had the option “unable to determine,” which was also marked as “0.” Question 27 was about the power of a study and was excluded from the review as the checklist 26 does not detail criteria for measuring power. Hence, the maximum possible points for a study in this review were 26.
Results
Article selection
An initial electronic database search yielded 160 articles (Figure 1). An identification of the duplicates excluded 46 articles. Screening of the title and abstract further excluded 86 articles because they were either investigating balance confidence or did not include people with TTA-vascular. Of the 28 articles meeting the inclusion criteria, 21 were removed after reviewing the full texts because they did not focus on standing balance measurement. In all, seven articles were selected for the review.
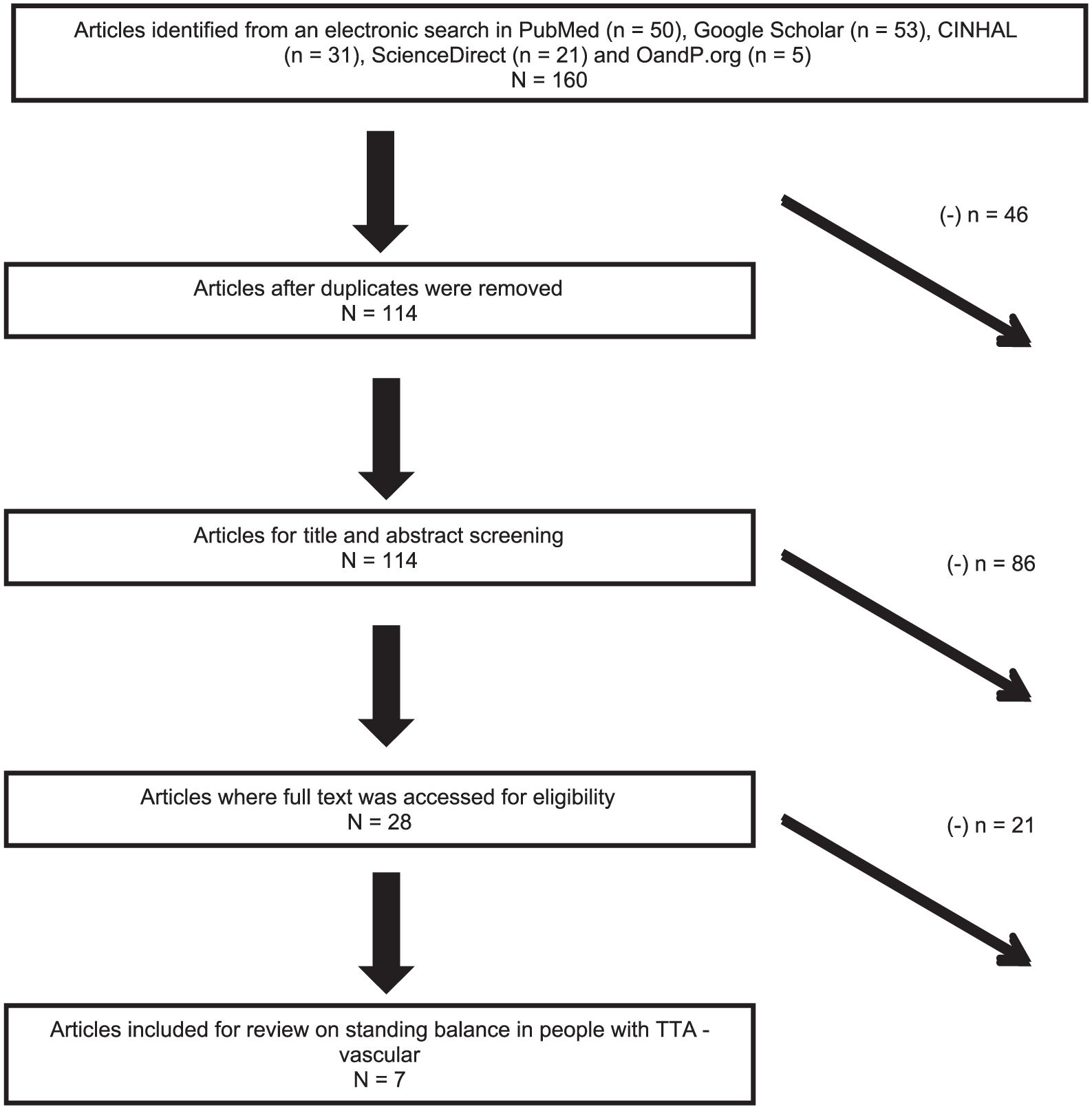
Article selection algorithm.
Participants
The participant demographics are presented in Table 1. All studies included people with TTA-vascular. Only three studies included participants with TTA-trauma.27–29 Two studies did not make use of a control group.30,31 The number of participants varied across all the studies with the largest including 84 participants. 1
Participants’ demographic characteristics.
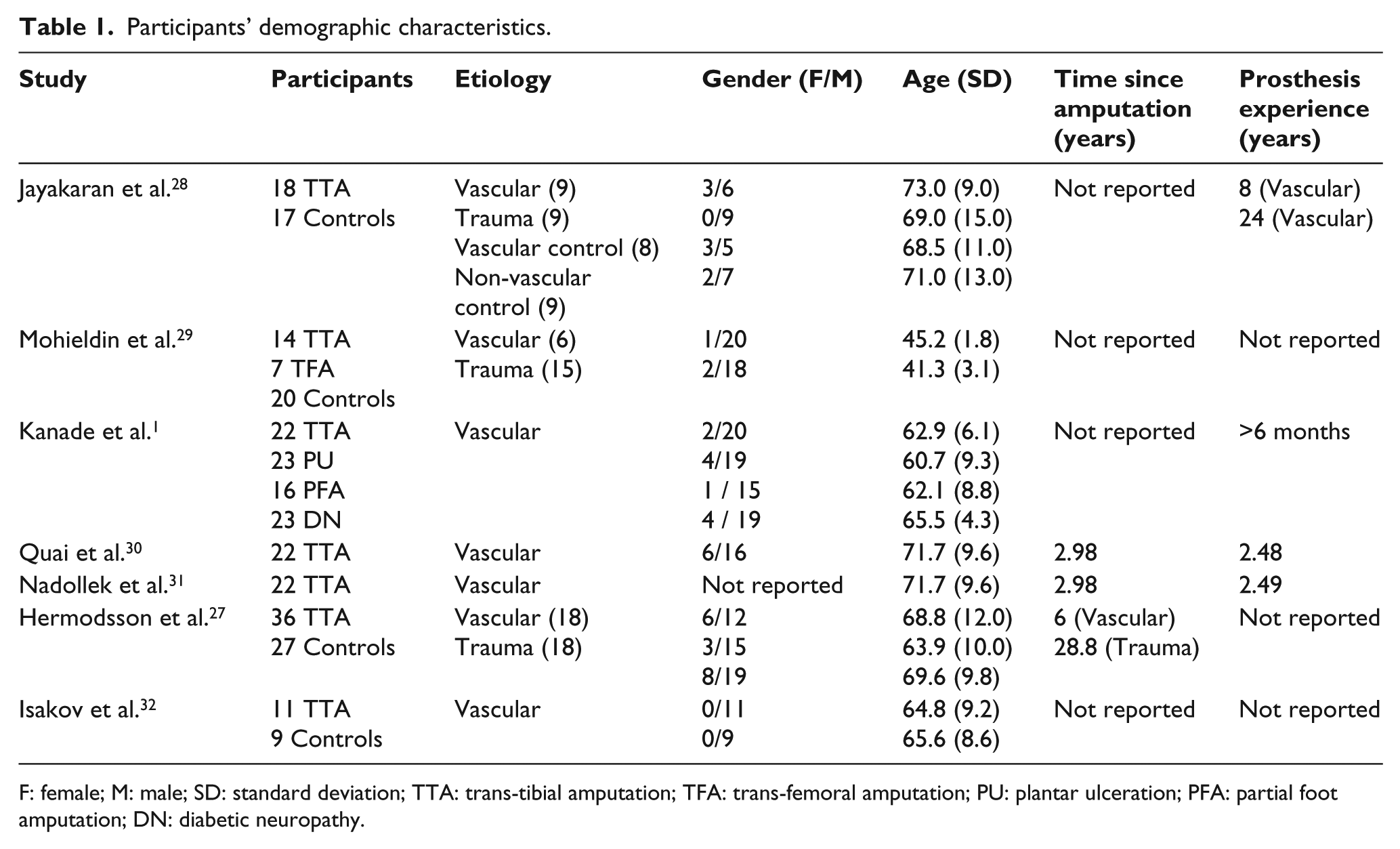
F: female; M: male; SD: standard deviation; TTA: trans-tibial amputation; TFA: trans-femoral amputation; PU: plantar ulceration; PFA: partial foot amputation; DN: diabetic neuropathy.
Study procedures
Most studies in this review were investigating standing balance measured with force platforms. Generally, the test methodology required participants to stand still on the force platforms for a period of time (varied between studies from 30 to 40 s) with feet together, while CoP or postural sway was recorded. It is generally accepted that the larger, more variable the CoP excursions are, the less balance control the person has. Most studies performed standing balance testing under eyes open (EO) and eyes closed (EC) conditions. Two studies made use of the sensory organization test (SOT) as part of computerized dynamic posturography to test the static and dynamic balance of the participants.28,29 SOT includes six testing conditions, the first three conditions involve standing on a fixed platform with EO, EC, and using sway referenced vision (static balance function). The next three conditions involve standing on a moving platform (sway referenced surface) with EO, EC, and using sway referenced vision (dynamic balance function). Sway reference is defined as movement of the platform and/or surrounding walls to directly follow the individual’s A-P sway.
Outcome measures
Load distribution or weight bearing on either limb was investigated by four of the seven studies1,30–32 (Table 2). Three studies measured CoP excursions during quiet stance.1,30,31 Two studies, although measuring balance on force platforms, did not report CoP excursions, but used postural sway to describe standing balance,27,32 which is derived as the standard deviation of CoP. Two studies used the SOT to investigate static and dynamic balance.28,29 Mohieldin et al. 29 reported composite equilibrium score (CES), while Jayakaran et al. 28 report root mean square distance (RMSD) and mean velocity (mV) of the CoP.
Data extraction from reviewed articles.
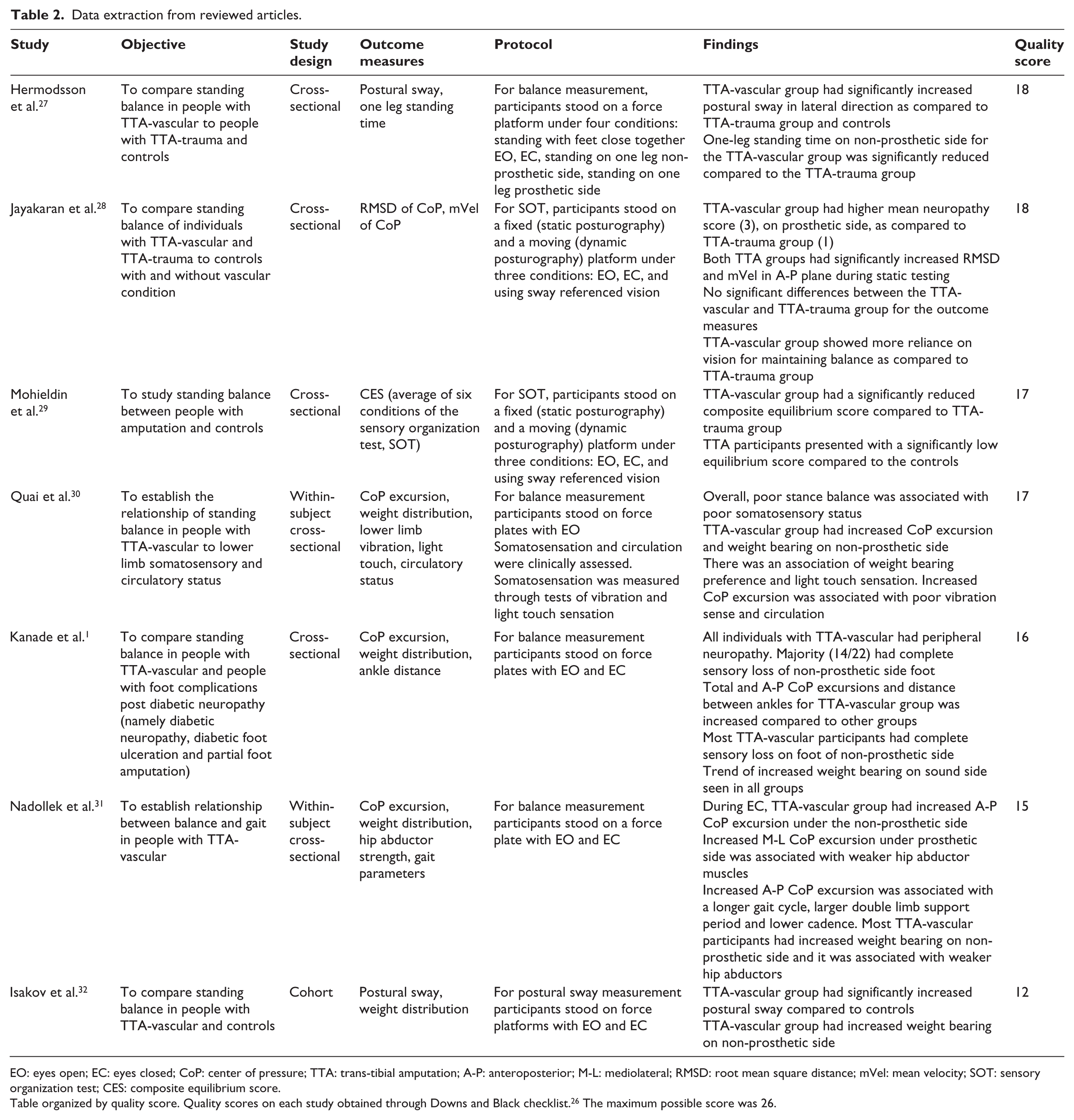
EO: eyes open; EC: eyes closed; CoP: center of pressure; TTA: trans-tibial amputation; A-P: anteroposterior; M-L: mediolateral; RMSD: root mean square distance; mVel: mean velocity; SOT: sensory organization test; CES: composite equilibrium score.
Table organized by quality score. Quality scores on each study obtained through Downs and Black checklist. 26 The maximum possible score was 26.
Weight distribution
Weight distribution on the prosthetic and non-prosthetic legs during the standing balance task was measured by four of the seven studies. Two studies compared individuals with TTA-vascular to healthy individuals,1,32 while the other two derived a relationship between weight distribution and other physiologic functions.30,31
Nadollek et al. 31 aimed to establish a relationship between weight distribution, CoP excursion, hip abductor strength, and gait parameters of individuals with TTA-vascular. They found their participants to have significantly (p = 0.003) more weight bearing on the non-prosthetic side while no significant differences were found between the EO and EC conditions. Increased weight bearing on the prosthetic side was positively correlated with stronger hip abductor muscles (r = 0.449).
Quai et al. 30 established a relationship between weight bearing preference (prosthetic or non-prosthetic side) and light touch sensation on the residual limb and intact limb. They associated weight bearing preference through the non-prosthetic side with a higher light touch sensation score on the residual limb during both EO (p = 0.012) and EC (p = 0.006). A higher score means good sensation in residual limb, however suggests a preference of weight bearing through non-prosthetic side. According to their results, majority of participants, 73%, preferred weight bearing through their non-prosthetic side during both EO and EC conditions.
Kanade et al. compared balance between people with TTA-vascular and others with foot complications post diabetic neuropathy (Table 1). They found all four groups (Table 1) with foot complications, post diabetic neuropathy, to have increased weight bearing on the non-affected side. 1 Although not statistically significant (p = 0.213), the mean weight bearing on the non-affected side was highest in the TTA-vascular group and lowest in the control group (diabetic neuropathy).
Isakov et al. 32 investigated the weight bearing imbalance of people with TTA-vascular at two time points: first test was done 2 days after receiving their first prosthesis and second test was done 3–4 weeks later, upon completion of their rehabilitation. In both the testing cycles, the authors found increased weight bearing on the non-prosthetic side during both EO (Test 1, p = 0.001; Test 2, p = 0.001) and EC (Test 1, p = 0.001; Test 2, p = 0.016) conditions. Interestingly, there was a significant improvement in weight bearing onto the prosthetic side post rehabilitation with EC (p = 0.027) for individuals with TTA-vascular.
Center of pressure excursions
Nadollek et al. 31 found that the anteroposterior (A-P) CoP excursions occurred significantly more under the non-prosthetic side during quiet stance (p = 0.000). The A-P CoP excursions were further increased when the participant’s eyes were closed (p = 0.006). Greater A-P CoP excursions under the prosthetic side were negatively correlated with time since amputation (EC, r = −0.423) and prosthesis experience (EC, r = −0.402). Greater M-L CoP under the prosthetic side was negatively correlated with hip abductor muscle strength (EC, r = −0.362), time since amputation (EO,r = −0.369; EC, r = −0.55), and prosthesis experience (EO, r = −0.365; EC, r = −0.499).
Quai et al. 30 established a relationship between A-P CoP excursions and vibration sensation. Greater A-P CoP excursions under the prosthetic side, during EO (p < 0.001) and EC (p = 0.041) conditions, were associated with a diminished vibration sensation. A majority of participants had greater A-P CoP excursions under non-prosthetic side during both EO and EC conditions.
Kanade et al. 1 found both A-P and total CoP excursions in quiet stance were significantly (p < 0.001 and p = 0.001, respectively) greater in the TTA-vascular group as compared to the other groups (Table 1). There was also a trend toward an increase in mediolateral (M-L) CoP excursions from control to TTA-vascular group. The results, however, were not statistically significant (p < 0.05). Individuals with complete sensory loss over the unaffected foot had a significantly higher mean CoP excursion (p = 0.048) compared to those that had some or intact sensation over that foot. Interestingly, majority (14/22) of individuals in the TTA-vascular group had complete sensory loss over their non-prosthetic side foot.
Postural sway
Hermodsson et al. 27 compared postural sway in people with TTA-vascular, TTA-trauma, and controls during quiet stance under EO and blindfolded conditions. When blindfolded, they found their participants with TTA-vascular to have significantly more postural sway in the M-L direction as compared to controls (p = 0.02) and A-P direction as compared to those with TTA-trauma (p = 0.03).
Isakov et al. measured total sway activity (A-P and M-L) during quiet stance under EO and EC conditions. They found people with TTA-vascular to have more postural sway than controls, especially during EC condition (p = 0.001). 32 The sway, however, decreased for the TTA-vascular group during EO condition (p = 0.01) in the second test cycle (post-rehabilitation).
SOT
Mohieldin et al. 29 used the six conditions of the SOT to measure and report the CES. CES is the weighted average of the center of gravity across six testing conditions. The authors found people with amputation from vascular causes to have significantly lower (poorer balance) overall CES (all six SOT conditions) than people with amputation due to trauma (p < 0.05). For the static balance testing (fixed platform), there were no significant differences in the CES between the vascular and trauma groups (p > 0.05). However, for all conditions, the vascular group had lower scores than the trauma group, in particular, during the EC condition and when using sway referenced vision.
Jayakaran et al. 28 used the static and dynamic testing cycles of the SOT to measure and report the RMSD and mVel of the CoP of individuals with TTA-vascular, TTA-trauma, and controls with and without vascular conditions. Greater RMSD reflected greater difficulty in maintaining a stable posture, while greater mVel indicated increased sway. In quiet stance (static testing), both amputation groups showed greater RMSD and mVel scores as compared to the control groups. The authors found no significant differences between the TTA-vascular and TTA-trauma groups for the RMSD and mVel scores for any of the SOT conditions. However, during static testing, the TTA-vascular group had higher mean scores on both legs for A-P RMSD and A-P mVel as compared to TTA-trauma group, where higher scores represent poor balance.
Standing time
Hermodsson et al. 27 investigated the standing time on one and both legs in their participants. Overall, they found the standing time on both legs was significantly reduced for the TTA-vascular group as compared to TTA-trauma group (p = 0.02) and controls (p = 0.004), when blindfolded. Non-prosthetic side standing time was also significantly reduced for the TTA-vascular group as compared to the TTA-trauma group (p = 0.02) and the controls (p = 0.0009).
Discussion
A TTA can limit an individual’s ability to perceive the ground underneath and maintain balance. The underlying cause of amputation, however, could further affect balance in people with TTA-vascular. The studies selected for this review quantitatively measured standing balance in individuals with TTA-vascular and the outcome measures collectively provide a better understanding of the balance ability of this population. According to the findings of this review, balance ability is diminished in people with TTA-vascular. Furthermore, limited evidence suggests individuals with TTA-vascular present with diminished standing balance compared to individuals with TTA-trauma.
During normal standing, an individual with no lower limb pathology can be expected to approximate an even weight distribution between both lower limbs. 33 This, however, is not the case in people with TTA-vascular and the ability to judge weight distribution can be diminished. The loss of the anatomical ankle and potential sensory loss of the contralateral foot could be limiting factors. All four studies measuring weight distribution found individuals with TTA-vascular bear more weight on their non-prosthetic side.1,30–32 Interestingly, Kanade et al. 1 found not only individuals with TTA-vascular but all of their participants with foot complications post peripheral neuropathy to have decreased weight bearing on the affected side, suggesting the effect of peripheral neuropathy on weight distribution. The presence of sensory loss as a result of the peripheral neuropathy possibly reduces the individual’s ability to perceive the ground and affects his or her ability to judge weight distribution on each leg.
CoP excursions were measured and reported by three studies in this review.1,30,31 According to their findings,1,30,31 individuals with TTA-vascular have increased CoP excursion in the A-P direction during quiet stance, which represents a diminished balance ability in this population. Reduced cutaneous sensation1,30,31 at the residual limb coupled with insufficient feedback from the ground (as a result of TTA) possibly reduces their ability to control A-P CoP excursions during quiet stance. Interestingly, Nadollek et al. 31 and Quai et al. 30 found that A-P CoP excursion was significantly more under the non-prosthetic side as compared to the prosthetic side. This could be due to the mobile and multi-axial nature of the anatomical ankle joint. However, in the presence of peripheral neuropathy, this finding could possibly be due to the diminished anatomical ankle proprioception. On comparing individuals with TTA-vascular with other individuals who had foot complications post diabetic neuropathy (Table 1), Kanade et al. 1 found the TTA-vascular group to have significantly more A-P CoP excursion than the other groups. However, increased CoP excursions were also seen in the other groups with peripheral neuropathy 1 possibly suggesting a relationship between peripheral neuropathy and diminished standing balance.
Two studies in this review made use of postural sway to measure standing balance instead of CoP excursion.27,32 According to their findings, people with TTA-vascular have increased sway as compared to healthy individuals. Hermodsson et al. 27 found individuals with TTA-vascular to have significantly increased sway in the lateral direction as compared to healthy individuals. Isakov et al., 32 on the other hand, do not report the sway direction. With just one study reporting the sway direction between individuals with TTA-vascular and healthy individuals, it is difficult to make conclusions. Hermodsson et al. investigated postural sway between people with TTA-vascular and TTA-trauma. As compared with the TTA-trauma group, individuals in the TTA-vascular group had increased sway in the A-P direction, 27 which is consistent with the CoP excursion findings of this review. Both Hermodsson et al. 27 and Isakov et al. 32 found that sway magnitude in people with TTA-vascular was increased when they were blindfolded or asked to keep their eyes closed. This is consistent with the finding of Nadollek et al. 31 who found CoP excursion of individuals with TTA-vascular increased with eyes closed. Interestingly, Isakov et al. 32 found individuals with TTA-vascular to have decreased sway (EO) post rehabilitation. This is a very essential finding and one that points toward the importance of rehabilitation focused on improving balance.
Although the purpose of this study was to review the evidence of standing balance in individuals with TTA-vascular, the authors also included studies that compared balance between individuals with TTA-vascular and TTA-trauma. The presence of comorbidities like insufficient sensory feedback, 8 reduced muscle strength,10–12 and diminished balance confidence 22 could possibly limit the balance abilities of individuals with TTA-vascular. Balance between both groups was measured using force platform 27 and through SOT.28,29 All studies found standing balance of individuals with lower limb amputation to be significantly reduced compared to individuals with no amputation.27–29 A comparison between the two amputation groups (vascular and trauma) yielded significant differences only for standing time 27 and overall CES. 29 However, it is interesting to note that for most static test conditions, the vascular group performed worse than the trauma group.28,29 These differences in performances were particularly apparent during the EC condition, where individuals in the vascular group showed stronger dependence on visual input for maintaining balance.28,29 This finding is consistent with that of other studies in this review, where under the EC conditions, the TTA-vascular group did not perform as well. The SOT assesses two of the three sensory systems (somatosensory, vestibular, and vision) at a time. In the absence of input from one sensory system, an individual should be able to maintain balance using input from the other two sensory systems. Unlike the trauma group, individuals in the vascular group had diminished balance in the absence of visual input, showing limited reliance on the other sensory inputs (possibly somatosensory) to maintain balance which suggests a limitation of somatosensory information in the TTA-vascular group. Similar results were observed by Hermodsson et al. 27 when they measured standing time between individuals with TTA-vascular and TTA-trauma. With EC and no visual information present, the standing time (on both legs) of individuals with TTA-vascular was significantly reduced as compared to individuals with TTA-trauma. Although limited, the evidence does highlight the balance limitation in individuals with TTA-vascular as compared to those with TTA-trauma. Perhaps the small group sample sizes used are responsible for the lack of statistical significance. Interestingly, across all three studies both groups, vascular and trauma, had similar mean ages (Table 1), which might not have been the most appropriate comparison, and could have resulted in the limited statistical significance. Commonly amputations resulting from trauma happen at a younger age compared to those from vascular disease. 22 Hence, a comparison of the two groups (vascular vs trauma) based on time since amputation might be more appropriate and have better generalizability. Future studies would probably be able to tease out the differences in balance between both groups by controlling the time since amputation and using a larger sample size.
Majority of evidence on balance in people with TTA-vascular has focused on the sensory deficits in this population; however, other comorbidities could also affect balance outcomes. For example, Nadollek et al. 31 found an association between stronger hip abductor muscle strength and increased weight bearing on the prosthetic side. With the loss of the anatomical ankle on prosthetic side, individuals with TTA could have higher reliance on a hip strategy to initiate weight distribution between both limbs and stronger hip muscles possibly allowing them to transfer weight evenly. However, the opposite could be true for weaker hip muscles and they might be contributing to the higher weight borne on the non-prosthetic side, which might be one of the reasons why most participants took significantly more weight on their non-prosthetic side. 31 Standing balance in individuals with TTA could also be affected by individual’s confidence in the task, that is, balance confidence.20,22 However, none of the selected studies measured balance confidence. In light of previous evidence on balance confidence, it would be appropriate for future studies and rehabilitation programs to consider this variable, especially since individuals with TTA-vascular have lower balance confidence than individuals with TTA-trauma. 22
In addition to internal factors, standing balance could also be affected by external factors like prosthetic componentry and alignment. For example, the non-dynamic nature of a prosthetic foot could be responsible for the increased CoP excursions seen under the non-prosthetic side; 31 the location of the ground reaction force vector in M-L plane, as a result of the alignment, could potentially predispose the prosthesis user to bear more weight on a particular side. Although these factors can be common to all amputation causes, in light of the current evidence on individuals with TTA-vascular, prosthetic prescription and alignment strategies should take these findings into consideration.
In summary, the standing balance abilities are diminished in individuals with TTA-vascular as compared to healthy individuals. Furthermore, limited evidence suggests that their balance might be further diminished as compared to individuals with TTA-trauma. Although the limitations of individuals with TTA-vascular are well documented in research and clinical practice, balance deficits are still present in this population, which could compromise the health and well-being of the individual. For example, bearing more weight on the non-prosthetic side on a regular basis could increase the chances of secondary complications like knee pain and osteoarthritis;34,35 increased CoP excursions or postural sway, during quiet stance, produces an A-P or M-L moment thereby increasing the likelihood of a fall34,35 and due to the nature of a vascular condition, a bruise or injury from a fall may lead to further complications.
Conclusion
The presence of vascular disease like diabetes or PVD could result in the affected individual developing peripheral neuropathy. Diminished sensation as result of the peripheral neuropathy could reduce the feedback from the feet, which could possibly affect standing and walking balance. Balance could further be affected by the reduced muscle strength and lower balance confidence in people with vascular diseases. This review is based on the hypothesis that in individuals with TTA-vascular, the presence of comorbidities like diminished sensation, weaker hip muscle strength, and lower balance confidence, in addition to the amputation, could affect standing balance. According to the findings of this review, individuals with TTA-vascular have diminished balance abilities, which might be further diminished when compared to individuals with TTA-trauma. Future studies should aim to compare the balance of this population with TTA-trauma population during dynamic activities like walking or running, while also measuring potential comorbidities like muscle strength and balance confidence.
Footnotes
Author contribution
All authors contributed equally in the preparation of this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
