Abstract
Background:
When the first carpometacarpal joint of the wrist is immobilized using an orthosis to combat the effects of osteoarthritis, atrophy of the thenar muscles may occur.
Objectives:
The aim of this study was to evaluate the thenar muscle diameter and cross-sectional area, joint function, and pain, before and after being supplied with an orthosis in patients with grades 1 and 2 carpometacarpal osteoarthritis compared to a control group.
Study design:
Randomized clinical trial.
Methods:
A total of 25 volunteer patients were randomized into two groups (an orthosis group and a control group) using a randomization table. A visual analog scale, the Michigan Hand Questionnaire, and ultrasound were used to measure pain, function, and specific muscle cross-sectional areas at baseline and after 4 weeks in both groups.
Results:
Mean visual analog scale pain scores decreased by 20% after 4 weeks of splinting, while those in the control group decreased by 3%. Changes in scores were significantly different between both groups (p = 0.001). There was no significant difference between the groups in either the Michigan Hand Questionnaire score or the muscle cross-sectional area.
Conclusion:
A large and significant effect on perceived pain in patients with first carpometacarpal joint osteoarthritis was observed after 4 weeks of splint use. Differences in treatment effects were found with regard to muscle cross-sectional areas, but these were not significant.
Clinical relevance
Custom-made splints may be recommended for the treatment of first carpometacarpal joint osteoarthritis. Moderate to large but non-significant treatment effects were found with regard to muscle cross-sectional areas.
Keywords
Background
Osteoarthritis (OA) is the most common joint disorder seen in humans. 1 The most commonly affected joints are the hands, feet, hips, and knees. Hand OA typically involves the distal interphalangeal (DIP), proximal interphalangeal (PIP), and the first carpometacarpal (CMC) joints. 2 About 75% of those affected with hand OA are women aged between 60 and 70 years. 3 A radiographic study has shown that 44%–70% of people over 55 years and 80%–85% of people over 75 years have one or more symptoms of OA. 4 Moreover, it is suggested that OA severity is related with age, 5 while the prevalence of hand OA is 54% in people aged over 55 years. 6
Pain, dysfunction, and loss of grip power are commonly reported in patients with hand OA, 7 with pain as the main presenting symptom. 8 These symptoms are often caused by writing, opening jars, using the hand for an extended period for some particular task, and especially due to repetitive pinching movements which can be difficult to perform. 1 The patients often have weakness due to the pain that may affect their ability to work, perform activities of daily living (ADLs), and to follow leisure/recreational pursuits. 7 They may also develop adduction deformity of their thumb during the later stages of the disease. 2 The early signs include tenderness over the CMC joint at the base of the thumb, thenar wasting, and reduced pinch and grip strength. 5 The conservative treatment for this type of injury involves orthoses, exercise, and physical therapy.7,9
The use of an orthosis is one conservative approach that is routinely used in case of these patients5,10,11 and is based on its ability to increase stability in the CMC joint. 12 This treatment aims to hold the thumb in an abducted position and prevent adduction and retro positioning. 7 This ensures that the metacarpal base is covered by the trapezium which provides joint stability and results in the reduction of metacarpal subluxation.1,13 The articular surface is rough and incongruous within an OA joint, which can lead to localized pressure. 14 The corrective orthosis use can provide external support for a joint, increase the joint congruency, and limit the motion that reduces the shear force and friction on the surface of joint. 7
When comparing two types of orthoses (prefabricated and custom-made) after 1 week of wear, Weiss et al. found no significant differences between them based on the parameters tested. However, a valid scoring system was not used to assess the improvement noted. Two studies have reported no agreement on the most effective splint design for the improvement of symptoms in patients with grades 1 and 2 OA of the first CMC joint7,8. In a previous study, the conservative structure and inexpensive low-temperature thermoplastic devices directly molded onto the body of the patient using a specific design template has been proposed. 15 Bani et al.12,16 demonstrated that wearing a custom-made orthoss by patients with OA of the first CMC joint reduced pain and increased grip strength, pinch strength, and hand function. In addition, in a further study, comparing the influence of prefabricated and custom-made thumb splints on pain, function, grip strength, and key pinch movements in patients with basilar joint OA showed that the custom-made orthoses produced greater pain reduction. 1
Functional performance levels and their relation to pain in patients with CMC OA have been reported by a number of authors.6,12,16 Bani and colleagues16,17 noted a reduction in pain in patients with CMC OA and a subsequent improvement in function following orthotic intervention. However, Carreira et al. 6 demonstrated no relationship between pain and improvement of function in their study. Despite a reduction in pain, an improvement in function does not correlate well in patients with CMC OA. Limited improvement in function and grip strength can be related to this point. 6 This is supported by Mckee et al., 18 who reported the use of serial casting and immobilization stating that it can often be a reason for muscle atrophy. Bulthaup investigated the effect of commonly used long and short types of commercially produced wrist extension orthoses on the activity of the proximal muscles of the shoulder, elbow, and wrist flexor, as well as extensor muscle activity. The results showed an increase in the function of muscle with the use of the splint by the patients. 19 Chinchalkar et al. analyzed the early post-operative movement of a 27-year-old female patient who had undergone a dorsal capsulodesis procedure to correct capitolunate instability. They reported that the use of splint produced early movement and activated the motor units in the muscle of the upper limb joints. 20
This study was therefore designed to investigate parameters in patients with early stage CMC OA. More specifically, the aim of this study was to evaluate the thenar muscle cross-sectional area (MCSA), hand function, and pain before and after orthotic intervention in patients with grades 1 and 2 thumb CMC joint OA compared to a control group.
Methods
Subjects
Patients were referred with a diagnosis of grades 1 and 2 thumb CMC joint OA by an orthopedic surgeon at the Orthotics and Prosthetics Department of University of Social Welfare and Rehabilitation Sciences. Referred patients were selected based on a specific inclusion and exclusion criteria. Patients were randomly allocated using the randomization table: splint using group or control group. A total of 25 patients (splint group = 16; control group = 9) and 20 healthy volunteer subjects participated in this study.
Inclusion/exclusion criteria
The inclusion criteria for patients included those patients with (1) a positive clinical and radiological diagnosis of thumb CMC joint OA of grade 1 or 2, of either gender; (2) pain in the base of the thumb; and (3) a cognitive ability to respond to a questionnaire and to undergo the tests. In addition, patients and healthy subjects who (1) had no deformities in the affected hand, or DIP joint of the thumb; (2) had not used a splint on the affected thumb during the previous 6 months; (3) had not undergone any surgery on the affected hand during the previous 6 months; (4) had no potential allergy to the splint material; and (5) had no evidence of injection therapy in the affected hand in the previous 6 months, or the presence of additional disease affecting the ipsilateral upper limb (e.g. carpal tunnel syndrome, De Quatrains tendonitis, Dupuytren’s contracture, arthritis, and fifth or sixth cervical vertebral disc herniation) were also included as a part of this study. Ethical approval was obtained from the Ethics Committee of the University of Social Welfare and Rehabilitation Sciences. All patients signed the consent forms to participate in this study.
Orthotic intervention
According to the existing literature,21,22 the custom-made thumb orthosis was constructed to provide first CMC joint stabilization. In addition, it was also designed to keep the pulp of the distal phalange of the index finger and thumb free to grip with the other fingers in a functional position with the wrist free from any limitation of motion.
The first step in the production of a custom-made orthosis was to obtain a pattern which matched the dimensions of the patient’s hand. Low-temperature moldable thermoplastic material with a 3.2-mm thickness (Aquafit NS Stiff: 3.2 mm (1/8″), Orfit Company, Inc., Belgium) was then used to construct a custom-made device from the template by direct molding to the patient’s wrist and hand (when wrist is in a neutral position and thumb and middle fingers’ pulp are in touch with each other) with appropriate trimming to allow thumb function. After the material had cooled, a 3-mm-low-density Plastazote lining was adhered to the shell and closed by Velcro© on the patients’ hand (Figure 1).
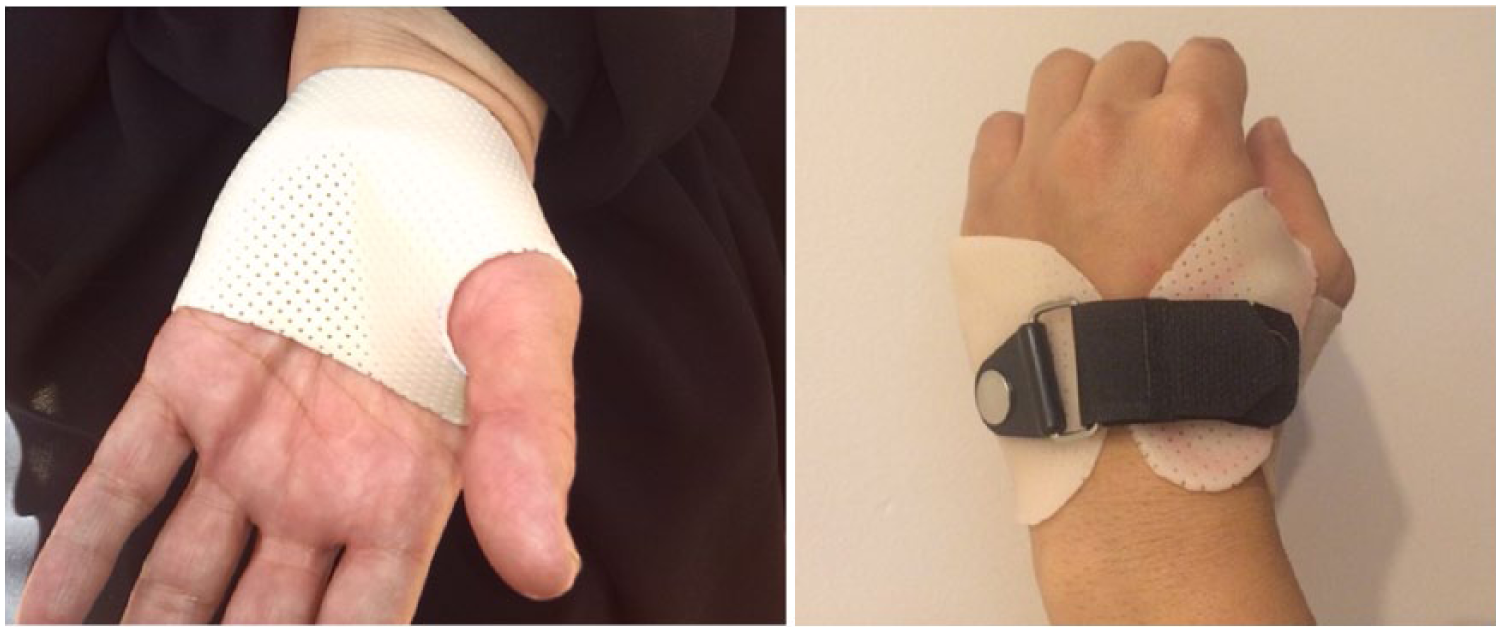
The custom-made thumb splint used in this study.
The subjects were asked to wear the orthosis when performing ADLs and remove them during sleeping, bathing, and in conditions that would adversely affect the splint material (e.g. when exposed to excessive heat). Each subject was further advised to keep the splint in a clean condition. Steps to apply and remove the orthosis were also demonstrated to all the subjects. They were further instructed to contact the rehabilitation team if they felt any discomfort while wearing the orthosis.
Procedure
The retest reliability measurements
In order to determine the intra-rater reliability of measurements (within day and between days) using ultrasound (US) technique for abductor pollicis brevis (APB) and opponens pollicis (OP) muscle diameters and cross section, 20 healthy volunteer subjects were measured by the same examiner on three different occasions. The first two measurements were taken within half an hour on the first occasion and were used to assess the within-day reliability. However, the third measurement was taken within 3–5 days of the first test and was used to assess the between-day reliability. After the confirmation of US technique as an acceptable and reliable method for measuring the diameter and muscle cross section, this procedure was performed on the referred patients.
US procedures
The MCSA and diameter were measured using the US technique. The frequencies used were 120 MHz and a general probe was applied. US evaluation was carried out with the patient’s hand resting in a relaxed position on a table and the probe applied to the thenar side of hand.
For the APB and OP muscles, the probe was placed on the sesamoid radial side with a measurement angle of 20°, while the angle between the probe and the middle of the hand was 120°. For the adductor pollicis and first lumbrical, the probe was positioned parallel with the medial side of the first metacarpal bone, while the angle between the probe and the middle section of the hand was 60°–70° (Figure 2). All the measurements were performed at baseline and after 4 weeks of use of orthosis.
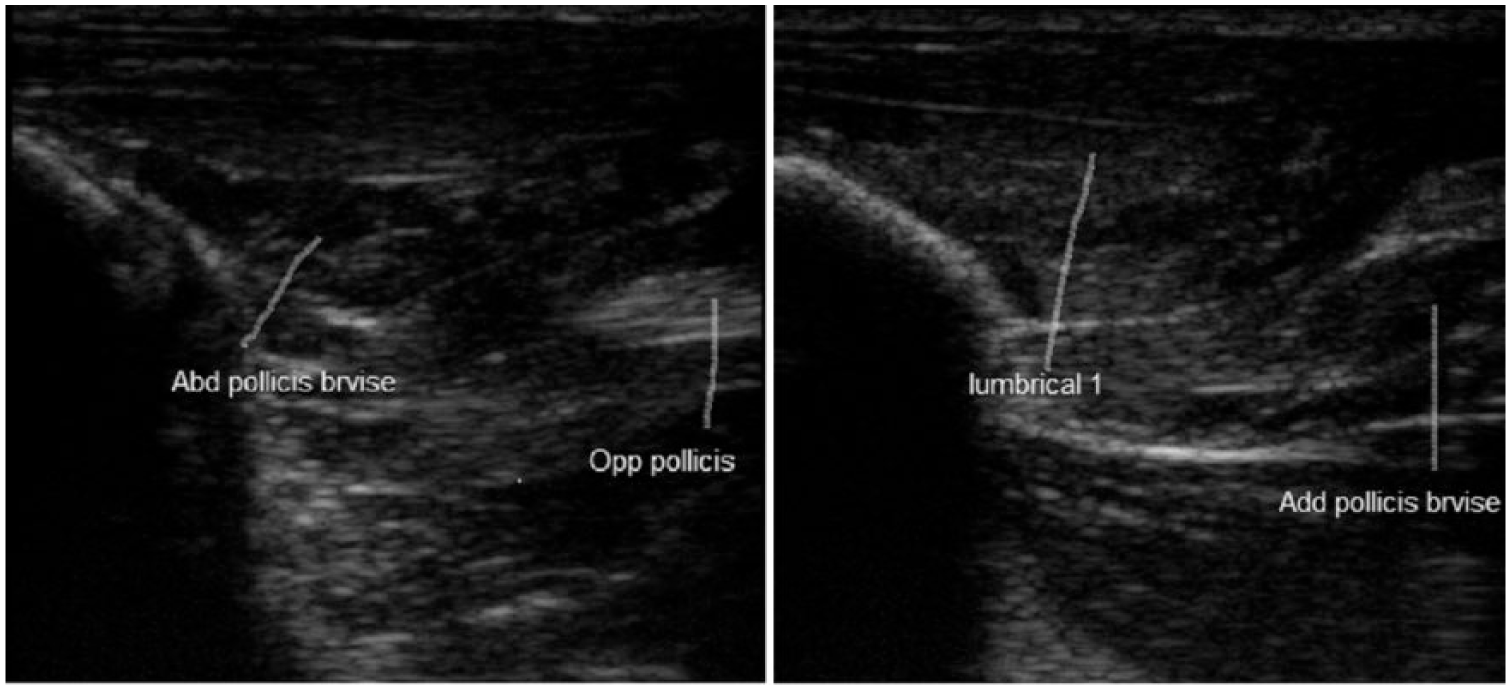
A typical ultrasonographic scan approximately parallel to the first metacarpal bone (with the angle between the transducer and the midline of the hand being approximately 120° for the abductor brevis and abductor pollicis brevis muscles and 70° for the lumbrical and adductor pollicis brevis muscles from the palmar surface).
Clinical tests
The evaluation of all the patients was performed by an experienced orthosist who had been previously educated to administer the tests at baseline and following 4 weeks of orthosis use. The primary outcome measures included pain levels, diameter and cross-sectional area (CSA) of the thenar muscles, and hand function based on Michigan Hand Questionnaire (MHQ) scores. The MHQ sub-scores of function, ADL, pain, work performance, esthetics, and satisfaction scores were also derived.
Evaluation of pain via visual analog scale
A visual analog scale (VAS), which is a common approach in the assessment of pain as demonstrated in the literature in this field,20–22 was used within a range of 0 cm (“no pain”) to 10 cm (“worst pain imaginable”) for evaluating the pain in the affected part. The patient indicated his/her level of pain while using the tip of a pen based on this score. For the evaluation of pain for the control group (i.e. those who did not receive orthotic intervention), the average level of pain the patients felt they had experienced during the previous week was considered. The splints were assessed for pain based on the average pain felt by the patient using the splint during the assessment.
Evaluation of function via MHQ
MHQ is a hand-specific outcomes instrument which measures the health outcomes of patients with chronic hand conditions. The MHQ contains six distinct scales: (1) overall hand function, (2) ADLs, (3) pain, (4) work performance, (5) esthetics, and (6) level of patient satisfaction with the hand function. It also encompasses a demographic section which deals with questions about patients’ gender, ethnic background, and other pertinent enquiries.
The MHQ consists of 72 questions, is self-administered and takes approximately 15 min to complete. When administered several times (i.e. pre- and post-intervention), MHQ can be used to assess changes in the hand function. In this study, the MHQ was answered based on the patient’s experiences in the previous week. However, the patient was asked to estimate his/her most accurate answer if he/she did not perform any ADLs during the previous week. The MHQ has points ranging from 0 to 100, with higher scores demonstrating worse functional capacity.
Statistical analysis
Intraclass correlation coefficient (ICC) and standard error of mean (SEM) were used to evaluate the intra and inter session reliability in measuring diameter and CSA of related muscles. The paired t-test was used for evaluating the changes in parameters within the groups. An analysis of covariance (ANCOVA) was used to determine any significant difference between groups once the effect of time was removed. The ANCOVA test was also used to determine whether there is a main effect for treatment (orthosis, no orthosis) or time (pre, post) or an interaction effect (treatment × time) for all of the outcome measures (CSA, pain, and MHQ). Change scores were computed by subtracting the baseline scores from the scores at 4 weeks. Differences in change scores between the splinting group and the control group were analyzed using ANCOVAs with the baseline scores of the outcome variable as the covariate. Parametric assumptions for performing ANCOVA included normal distributed data, homogeneity of variance, and homogeneity of regression.
To give an indication of the magnitude of the treatment effects, effect sizes or standardized mean differences (Hedges’ g) were calculated as the difference between the mean change of the intervention group and the control group divided based on the pooled standard deviation (SD). A correction factor was applied to adjust for small and unequal sample sizes. An effect size of 0.2 was considered as a small effect, 0.5 a moderate effect, and 0.8 a large effect. 23 SPSS 16 (SPSS, Inc., Chicago, IL, USA) was used for data analysis. The significant level considered was α = 0.05.
Results
Within-day diameter and CSA measurements using US technique with good ICC values were considered to be acceptable (ICC was 0.73 and 0.69 for APB and OP, respectively, in muscle diameter and 0.81 and 0.75 for APB and OP, respectively, in CSA) (Table 1). Between-day measurements also demonstrated acceptable reliability with the good values of ICC (ICC was 0.73 and 0.64 for muscle diameter of APB and OP, respectively, and 0.68 and 0.73 for CSA of APB and OP, respectively, in healthy subjects group).
ICC and SEM of APB and OP muscles diameter and CSA.
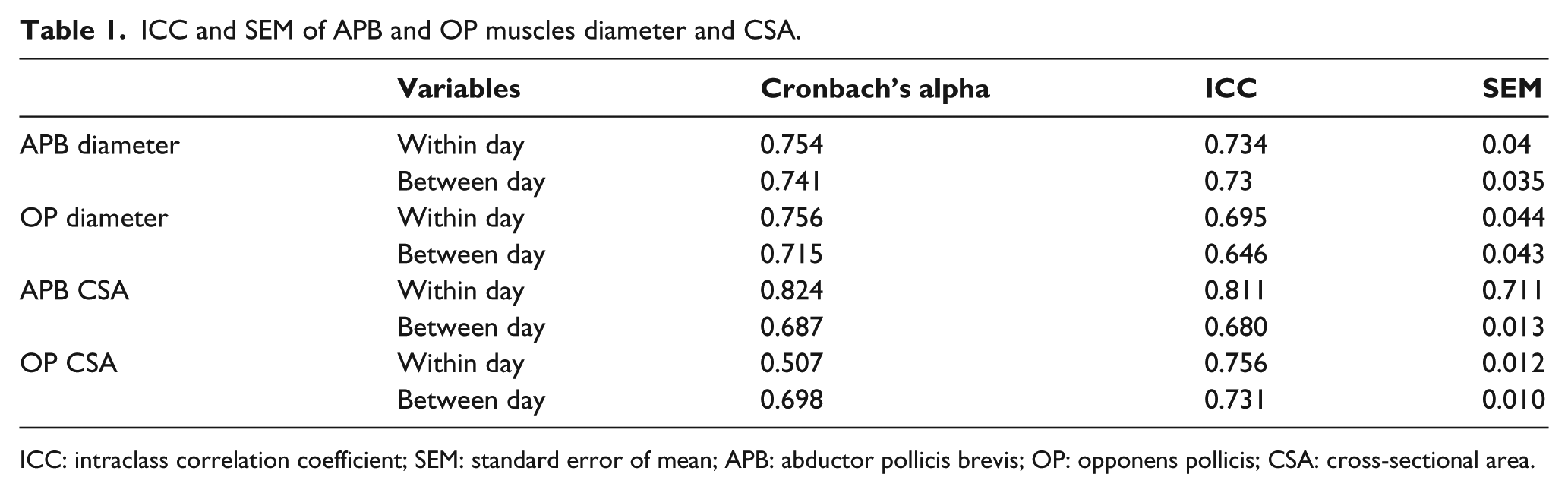
ICC: intraclass correlation coefficient; SEM: standard error of mean; APB: abductor pollicis brevis; OP: opponens pollicis; CSA: cross-sectional area.
A total of 25 patients were enrolled in this study. In all, 16 patients were allocated to the splinting group and 9 to the control group. All patients completed the study. Mean ± SD age was 50.18 ± 5.7 years in the splinting group and 52.33 ± 6.4 years in the control group. The mean ± SD symptoms durations were 12 ± 1.95 months and 15 ± 1.92 months, respectively. The majority of the patients in both groups were female (87% and 88%, respectively). Mean ± SD MHQ scores at baseline were 55.43 ± 14.7 and 64.19 ± 15.32, respectively. During the 4-week study period, the patients in the splint group wore the splint for at least 5 h, with mean ± SD duration of 7.5 ± 2.5 h/day.
The characteristics of patients who participated in this study are shown in Table 2. No significant differences in mean of age, gender, body mass index, dominant hand, affected hand, and duration of injury were noted in the patients group and parameters in the two groups at baseline (p > 0.05). All parameters were homogeneous among the two groups. Table 3 demonstrates the mean (SD) and comparison of variables in first CMC OA patients after 4 weeks of orthosis use. Figure 3 shows the CSA of the four muscles investigated in this study.
Characteristics of the control group, intervention group, and healthy subjects at baseline.
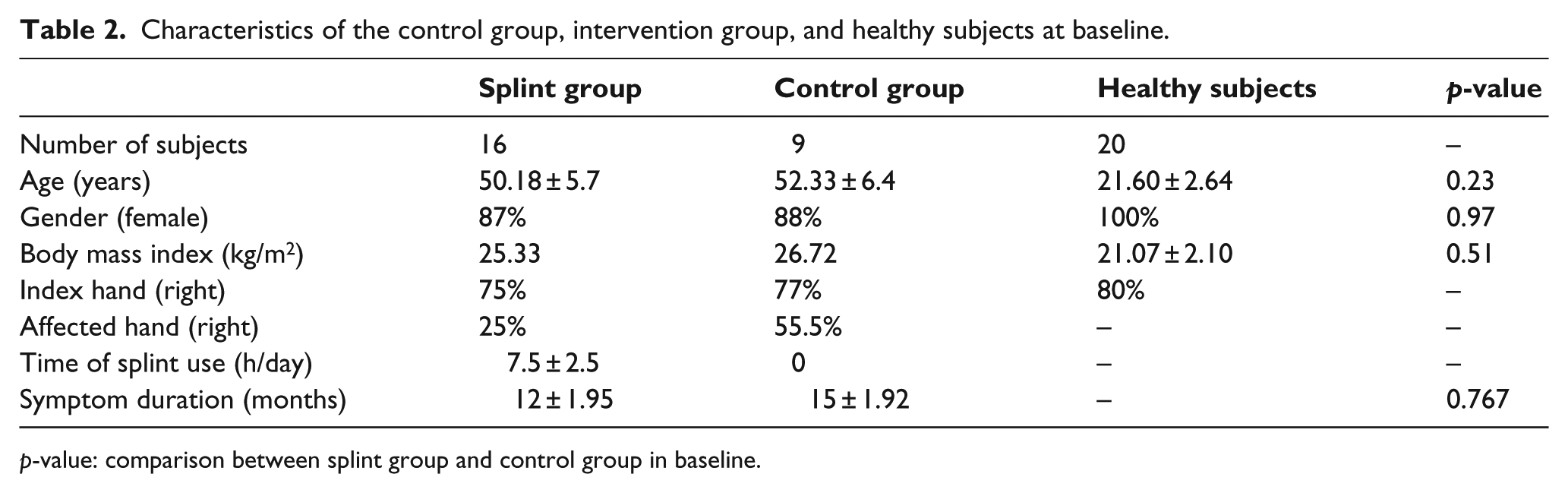
p-value: comparison between splint group and control group in baseline.
Baseline, after 4 weeks scores on outcome measures, and indices for the treatment effect.
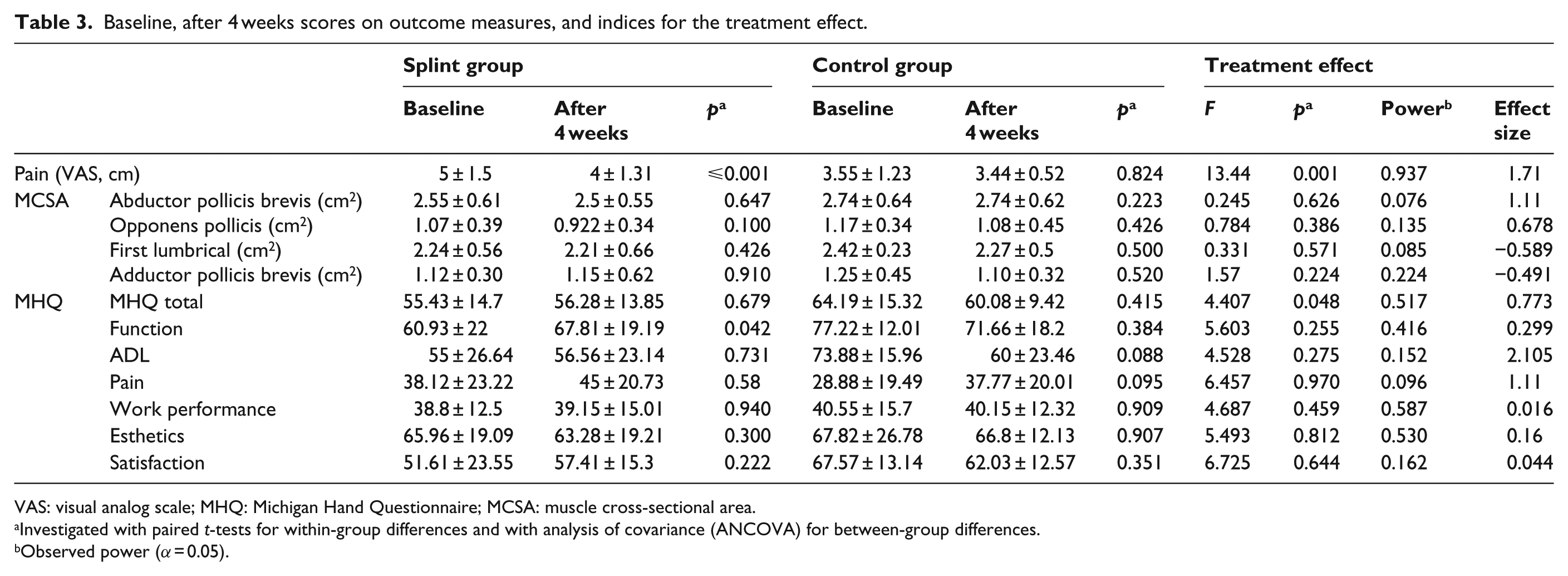
VAS: visual analog scale; MHQ: Michigan Hand Questionnaire; MCSA: muscle cross-sectional area.
Investigated with paired t-tests for within-group differences and with analysis of covariance (ANCOVA) for between-group differences.
Observed power (α = 0.05).
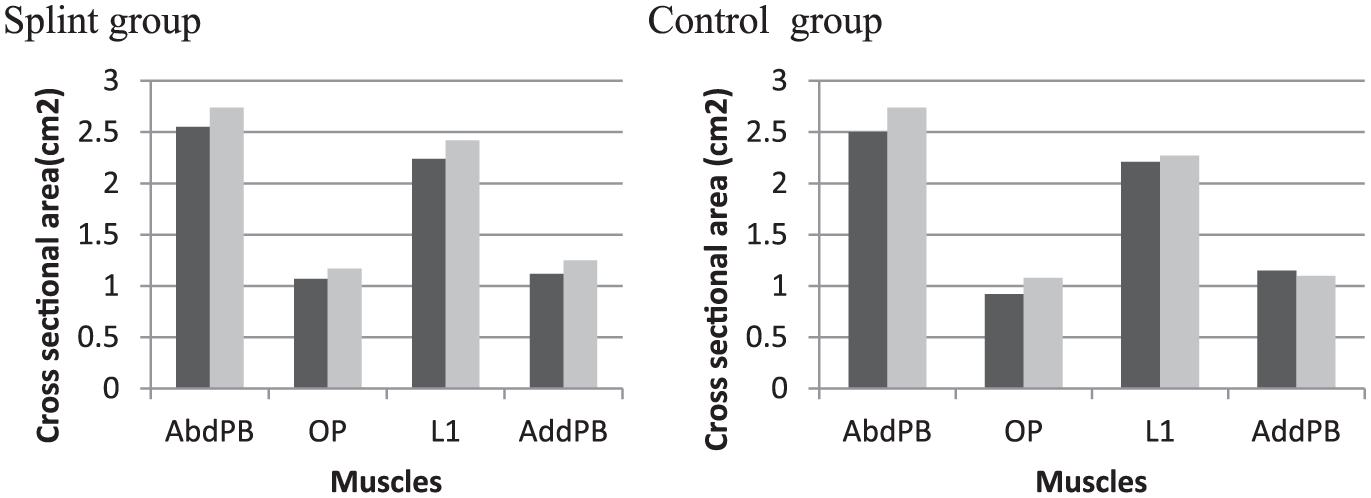
The cross-sectional area of mentioned muscles in splint and control groups in baseline (black column) and after 4 weeks (gray column) evaluation.
Pain evaluation based on VAS score
Mean ± SD of the VAS pain scores at baseline and after 4 weeks is shown in Table 3. In the splinting group, mean VAS pain scores decreased by 20% after 4 weeks of splinting. In the control group, mean VAS pain scores decreased by 3%. Change scores were significantly different between both the groups (F = 13.44, p = 0.001). The effect size was 1.71, indicating a large treatment effect of splints on VAS-measured pain.
Functional ability outcome
No significant difference between baseline and 4 weeks of splint wearing in the MHQ score was noted in the splinting group. In the control group, MHQ scores were slightly decreased after 4 weeks. Change scores were significantly different between both the groups (p = 0.048). Treatment effects were large, as denoted by the effect sizes (0.773).
MCSA outcome
Mean ± SD of the MCSA at baseline and after 4 weeks in two groups is shown in Table 3. There were no significant differences noted in MCSA of the APB, OP, first lumbrical, or adductor pollicis brevis before and after the orthosis use. These results were similar for the control group after 4 weeks of splint wearing. There was no significant difference between two groups in the MCSA. Treatment effects were moderate to large, as shown by the effect sizes (Table 3).
Discussion
A previous study has reported that thumb splints can result in muscular atrophy. 23 After 4 weeks following the treatment in patients with first CMC joint OA, the results were at variance when compared to the previous data reported within the literature. In the study, there was no significant difference in MCSA of the muscles tested between the orthosis group and the control group after the treatment period. In addition, there were no significant differences in these parameters within the orthosis intervention group between the baseline and after 4 weeks of use. In this study, the use of orthosis improved pain after a 4-week period, while in the control group, the mean VAS pain scores remained unaltered (no reduction in pain). This observation is similar to previous studies in this field, where a custom-molded splint had a similar limited effect.12,16 According to stabilization and decreasing inflammation of joint as a consequence of the warmth created by the splint, pain may be decreased;1,12,16,17,22 however, the pain remained constant in case of the control group because a splint was not used.
Pain usually impairs the ADL. In this study, incidence of pain has been measured by two different methods, VAS score and a sub-score of MHQ questionnaire. VAS demonstrated reduction in pain in the intervention group, while there was no significant change in results of MHQ in the same group. This internal inconsistency may be due to the different methods used. The patients reported pain on a Likert scale (Always, Often, Sometimes, Rarely, and Never) by MHQ but announced a number during the previous week based on the 10-cm horizontal VAS. Hence, differences in announcement approach in MHQ and VAS might affect the result.
The reduction in pain levels associated with using the custom-made orthosis can cause an increase in function in patients with first CMC OA. In this study, MHQ was used to evaluate this function. There was no significant difference found within group evaluation in the orthotic intervention group before and after the use of splint. In addition, there was no significant difference observed within the control group between baseline and 4 weeks following time. But significant differences were also observed when comparing the two groups. Based on joint pain, the patients initially reported limitation in hand performance, and therefore, they had an inability to perform ADLs. The literature in this field demonstrates conflicting results with regard to hand function. In comparison with the present findings, Carreira et al. 6 found no increase in the function, but Bani and colleagues,12,17 Weiss et al., 7 and McKee and Eason-Klatt 22 demonstrated an increased function. The Disability of the Arm, Shoulder, and Hand (DASH) questionnaire was used in all these studies.
It has also been reported that serial casting and orthosis use can cause muscle atrophy. 18 Loss of lean muscle mass has been announced as one of the most predictable consequences of joint immobilization. The time course of changes in MCSA has been reported by a reduction following unilateral lower limb suspension, 24 immobilization, 25 bed rest 26 , and aging. 27 Short-term immobilization between 4 and 14 days demonstrated 1.1%, 1.6%, 1.8%, and 3.5% reduction in strength capacity.28–30 Since orthosis wearing time in previous studies was reported between 4 and 6 weeks, the period of intervention in this study was taken as 4 weeks.
The improvement in function was related to muscle atrophy that may be caused by splint use. 19 One limitation in this field is the lack of literature on the effect orthotic intervention on muscle atrophy in patients with first CMC joint OA. Since grip and pinch strength are produced as a consequence of forceful flexion of all finger joints around the first CMC joint and fine coordination of the joints in the thumb, 31 the atrophy of muscles and pain can cause reduction in these parameters in the patients with first CMC OA. The results of this study demonstrated that a splint had no effect on MCSA. Furthermore, the results of the effects of hand splints on pinch and grip strength in the literature seemed to be inconsistent.6,7,12,17. Carreira et al. 6 reported no change in these two parameters with a custom-made thumb splint on the first CMC joint OA patients. However, increased pinch strength using prefabricated and custom-made splints12,17 and short- and long-hand splints has been reported. 32 Furthermore, the results indicated that using US technique appears to be a reliable method for measuring muscles diameter and CSA, and can be used as a reliable tool in the assessment of function of hands muscles.
The main limitation associated with this study is the short evaluation time. In addition, grip and pinch force were not evaluated and would be useful to focus upon for further research to explore if a relationship exists with these parameters and muscle function. In this study, only the custom-made orthosis was compared to baseline and the control group. Comparisons between conventional prefabricated and custom-molded thumb orthoses are now required to give more evidence on muscle atrophy and function for OA of the first CMC joint.
Conclusion
The results of this study show that 4 weeks of splinting has a large and significant effect on perceived pain in patients with first CMC joint OA. Large and significant effects in reduction of the MHQ score were observed in 4 weeks of splint wear. Moderate to large but non-significant treatment effects were found with regard to MCSAs.
Footnotes
Acknowledgements
Essential materials and resources were provided by the Department of Orthotics and Prosthetics of University of Social Welfare and Rehabilitation Sciences.
Author contribution
All authors contributed equally in the preparation of this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
