Abstract
Background:
The introduction of the Echelon prosthetic foot with a hydraulic self-aligning ankle adds improved adaptability to varied terrains and uneven walking surfaces. However, the specific indications for prescribing such components and the potential benefits are yet to be fully established.
Case Description and Methods:
Nine amputees including three bilateral amputees evaluated their standard prostheses using the Seattle Prosthesis Evaluation Questionnaire. They were then provided with Echelon feet, and they evaluated them after 4 weeks of use.
Findings and Outcomes:
Improved satisfaction in all categories of use in relation to the Echelon foot with the greatest increase reported by bilateral amputees.
Conclusion:
The use of prosthetic feet with hydraulic self-aligning ankle improves prosthetic users’ satisfaction in general with a particular benefit in bilateral amputees.
Clinical relevance
Establish the clinical impact and user satisfaction after using Echelon feet in prosthetic users with different levels of amputations.
Background
The Echelon foot is a dynamic carbon fibre foot comprising independent toe and heel springs with a hydraulic self-aligning ankle. This combination allows the foot to adjust to uneven surfaces and slopes, while the amputee stands safely and with stability on most terrain normally encountered during the activities of daily living. Several studies have been presented reviewing the function and acceptability of this foot, including the study by Portnoy et al. 1 that looked at internal stresses in the residual limb and the study by McDougall and Wood 2 that assessed user satisfaction in unilateral amputees. Both studies however excluded bilateral amputees, which is an important group that requires improved stability and adaptability in the foot and ankle components. The aim of this study was to perform a qualitative assessment of the claims of the manufacturers of this foot and the impact on patients’ quality of life. We compared the Echelon foot to the patients’ standard prescription for all the patients who were prescribed the Echelon foot over a 4-month period.
Case Description and Methods
Nine male patients aged 42–62 years were prescribed 12 Echelon feet by the multidisciplinary team. This included three unilateral transtibial patients, three bilateral transtibial patients and three transfemoral patients. Patients were not chosen at random due to the ethical and financial issues related to prosthetic provision. Instead, the decision to provide Echelon feet was based on clinical need and level of mobility. Suitability for prescription was decided as follows:
Those who need to manage uneven surfaces or slops on regular bases;
Activity level of k2 or k3 and SIGAM (Special Interest Group in Amputee Medicine) mobility grade of D/b (able to walk 50m or more on level ground in good weather with one stick/crutch) or higher;
Unilateral amputees with musculoskeletal problems in the contralateral limb (e.g. ankle stiffness or arthrodesis).
Patients were initially asked to evaluate their current standard prosthetic foot (either the Esprit or Multiflex) using the validated Seattle Prosthesis Evaluation Questionnaire (PEQ).3–5 Patients would then re-evaluate their prosthesis 4 weeks after using the Echelon feet. The PEQ is a self-report questionnaire containing 54 questions organized into nine functional domain scales. Each of the scales may be used individually to measure only a specific domain of interest. We analysed the data in relation to six domains 3 presented in Table 1.
Data were analysed from six domains in the PEQ.
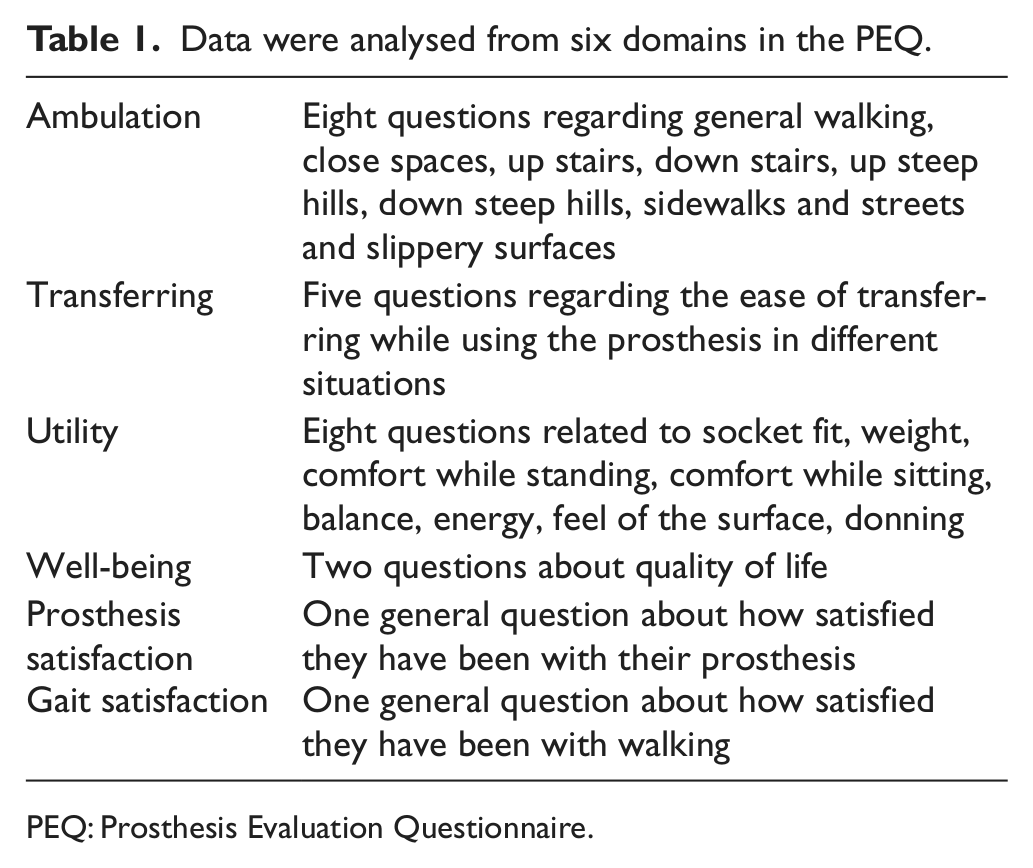
PEQ: Prosthesis Evaluation Questionnaire.
Eight of the nine patients who were supplied the Echelon foot had it fitted to their existing prosthetic limbs with no other changes; one patient – unilateral transtibial amputee – had it supplied as part of a new prosthesis as he preferred to retain his original prosthesis for other specific activities. It was felt unnecessary to add activity monitors to the prosthesis as previous studies had shown no increase or decrease in the activity when using the Echelon foot. 2
Findings and Outcomes
The results from the PEQ showed that patient satisfaction was higher with the Echelon foot in all categories compared to the previous standard foot with a statistically significant average improvement of 12.2% (p = 0.01) (see Figure 1(a) and (b)). When the results are analysed by amputation level, the patient group that showed the greatest increase in satisfaction was the bilateral transtibials with an average improvement of 22% (p = 0.01) (see Figure 2(a)). The average improvement recorded by the other patient groups was not statistically significant at 8% for the unilateral transtibials (see Figure 3(b)) and 9.2% for the transfemoral patients (see Figure 3(c)). McDougall and Wood 2 also reported transfemorals recording a greater increase in overall satisfaction in their findings.
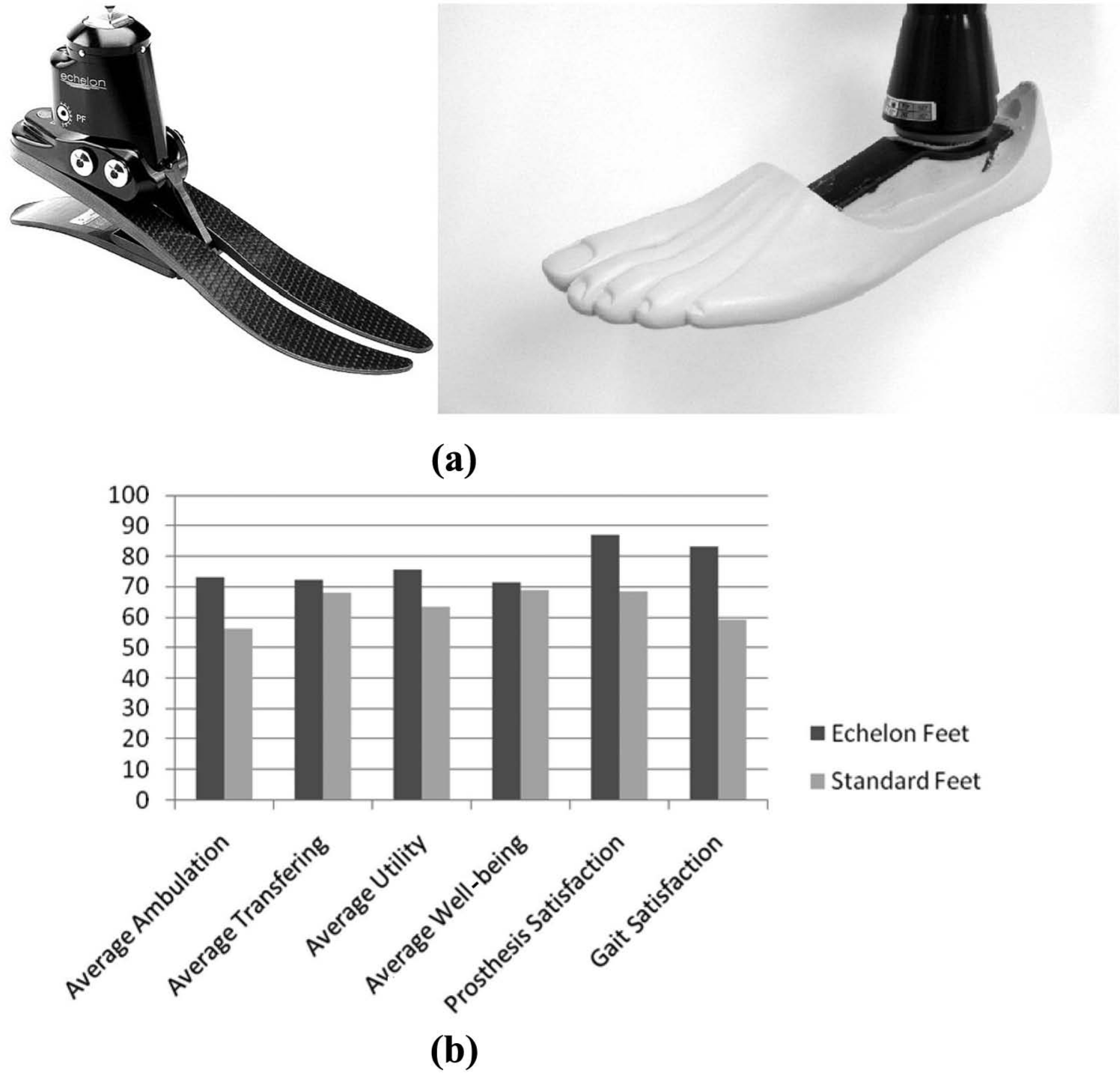
(a) An Echelon foot (left) and an example of a ‘Standard foot’, a Multiflex foot (right). (b) Average differences in PEQ domains for all patients.
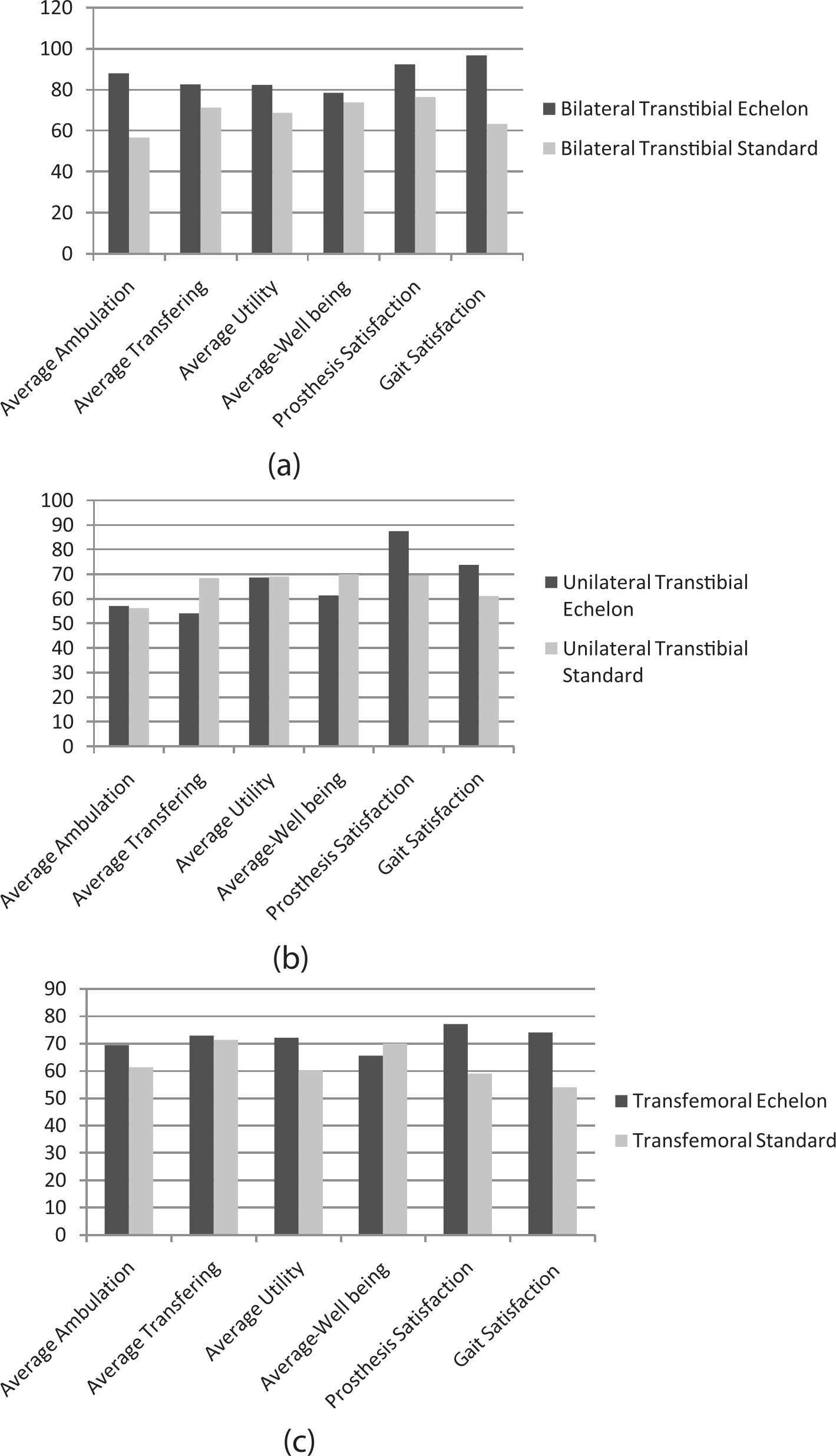
Average differences in PEQ domains for (a) bilateral transtibial amputees, (b) unilateral transtibial amputees and (c) transfemoral amputees.
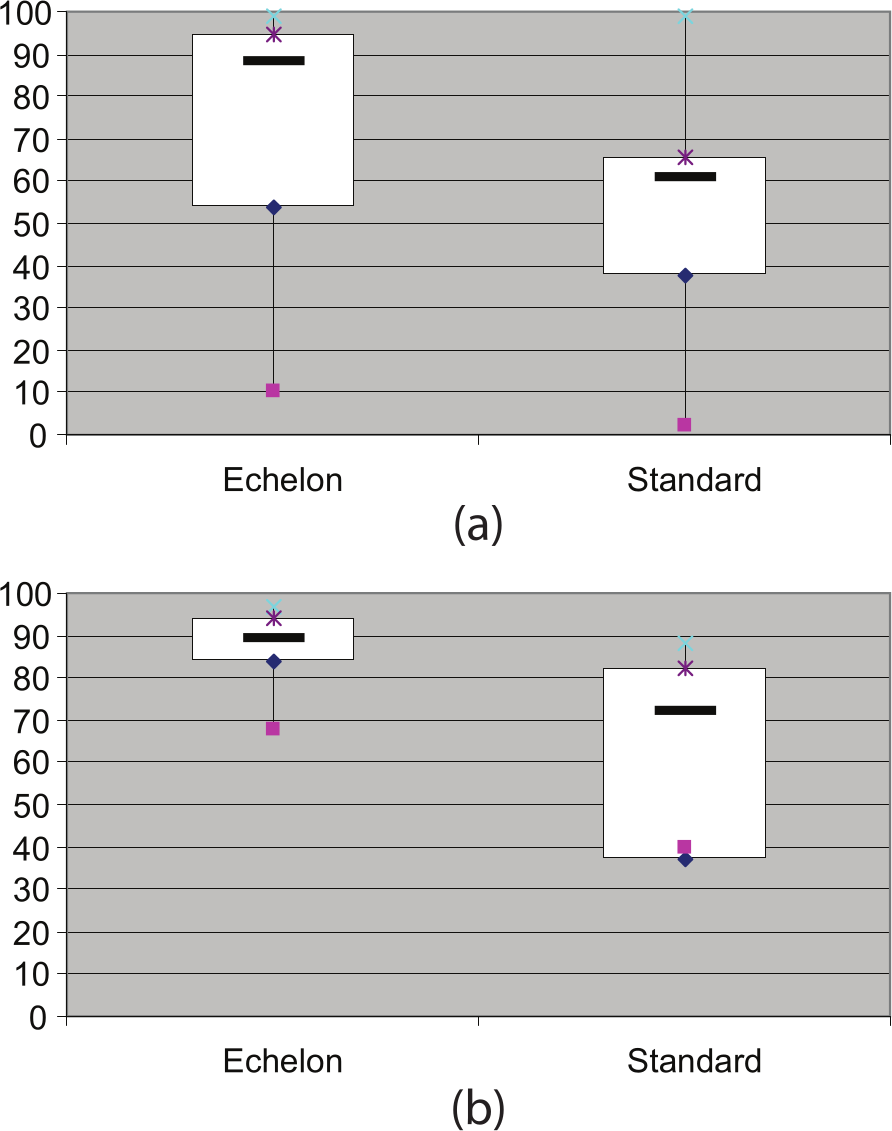
Overall reported (a) ambulation satisfaction box plot and (b) prosthesis satisfaction box plot.
When the evaluation questionnaire is further analysed by amputation level and evaluation domain, the levels of improvement show a marked variation. For instance, there was a drop in satisfaction of 14.5% in ‘transferring’ in unilateral transtibial amputees compared to 31.3% improvement in ‘ambulation’ in bilateral transtibial amputees. When the results are assessed together for all participants, however, most categories show a statistically significant increase in satisfaction. The domains where patients indicated the largest average improvement were ‘ambulation satisfaction’ showing a 16.7% improvement, ‘prosthesis satisfaction’ showing a 19.6% improvement and ‘gait satisfaction’ showing a 25.3% improvement (all p < 0.01; Figure 3(a) and (b)).
Discussion
The results shown are taken from a limited sample group and only indicate the patient’s subjective view of the foot after a 4-week trial period; however, they do demonstrate a marked preference towards the hydraulic ankle unit (Echelon foot). In the specific domains of ‘transferring’, ‘utility’ and ‘well-being’, there was only marginal improvement expressed by patients; however, all the patients reported a significant improvement in comparison to their previous foot in relation to walking (the ‘ambulation’ and ‘gait’ domains) and to the patients’ overall impression of the prosthesis. This coincides with similar reports in previous studies. 2
Although this improvement was felt across all the amputation levels, it was in the bilateral transtibial group where the largest improvement was recorded (including a statistically significant 33.4% improvement in gait satisfaction). This was perhaps unsurprising as both other groups had a functional ankle on the contralateral limb, and the prescription change for the bilateral amputee allowed for a more radical increase in function. Therefore, we propose that prosthetic feet with a self-aligning ankle should be considered in all bilateral amputees who are able to achieve outdoors walking.
Conclusion
There are grounds for further research into the use of hydraulic ankle units. Although this study was only carried out on a relatively small sample, all patients taking part reported an improvement in their ambulation/gait and overall satisfaction with their prosthesis/prostheses when they used the Echelon foot. It may be particularly relevant for bilateral amputees where the improved ankle function is most keenly felt.
Footnotes
Conflict of interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
