Abstract
Purpose
The shear bond strength of orthodontic brackets is an important factor in imparting desired treatment as repeated breakages during treatment not only delay its completion but also affect the quality of treatment. Thus, the aim of this review is to analyze the in vitro studies related to bond strength testing and to identify experimental conditions that are not standardized while performing in vitro studies.
Materials and Method
The total of 580 studies were searched, and 84 studies were accepted for review as per inclusion criteria. The 12 experimental conditions were analyzed, and it was found that none of the studies described all the conditions listed.
Results
There is no uniformity in parameters guidelines such as storing media, temperature, crosshead speed, type of testing method, and testing machine used in studies. None of the studies considered all reviewed conditions in their study design.
Conclusion
There is a need to frame proper recommendations for the testing protocols to be followed for in vitro bond strength studies so that baseline data as a reference will allow the intercomparison of results among studies and to reach any conclusion.
Introduction
Various types of malocclusions need orthodontic treatment, which nearly takes 2 years or more to complete. Thus, debonding of brackets during the treatment delays its completion and affects the quality of treatment outcome. Therefore, enormous data pertaining to many factors affecting bond strength with different combinations are present. Although, in vivo testing in a controlled manner is considered a better method to test any bonding systems simulating clinical situations.1, 2 But, it is almost impossible in vivo settings to demarcate out the strength of any adhesive bonding material independent of other variables that can affect overall results. Thus, most studies in the literature are based on in vitro settings, which permit uniform standard procedures for bond strength testing.
Test parameters that can influence bond strength include the type of enamel, substrate storage, and enamel surface pretreatment. Bond strength testing is also affected by the test mode used, such as tensile or shear testing. Thus, different outcomes seen in vitro bond strength studies might be because of the possibility of an unidentified combination of physical and mechanical properties related to the testing surfaces. Recent studies 3 have assessed the effect of some factors on bond strength, including the location of force, type of tooth, variations in crosshead speed, and mode of loading.
Normally, the bond strength testing in laboratory cannot anticipate the clinical efficacy of adhesives as there is a need for standard bond strength testing guidelines. Hence, the studies related to bonding testing method can only be evaluated on individual basis. Thus, the aim of this review is to assess the in vitro bond strength testing methods and suggest guidelines for proper standardization for testing conditions.
Materials and Methods
Literature search was performed in the databases of Medline, Scopus, and Google Scholar from 2016 to 2020 to identify relevant studies based on inclusion criteria. Search was limited to English language only.
Prescreening was done initially to identify the studies in the form of the titles and abstracts related to the topic of this study (shear bond strength of orthodontic metal brackets). The complete text of relevant studies was assessed by authors for assessment of the testing parameters needed to conduct studies (Figure 1). Inclusion criteria for the study included: in vitro investigation, with the shear bond strengths of orthodontic metal brackets evaluated with Universal testing machine and the sound tooth enamel. Case reports and small abstracts were not included.
Algorithm of Study Selection Procedure.
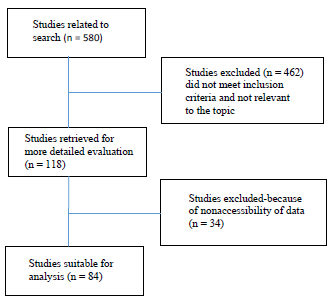
Results
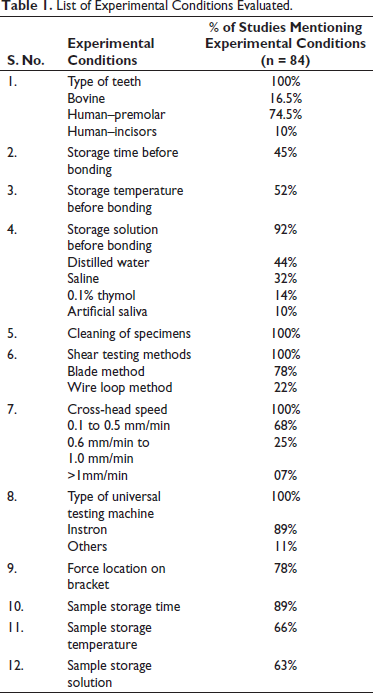
A list of parameters was used to evaluate the experimental conditions, each depicting the laboratory variables that influence the results of in vitro bond strength testing and the percentage of studies clearly mentioning the experimental conditions (Table 1). A total 580 studies were searched, and finally, 84 studies were accepted for review. The 12 experimental conditions were analyzed, and it was found that none of the studies mentioned all the conditions in the article. The type of teeth used in the study with the type of testing machine and method with its crosshead speed are the only variables that were mentioned in all reviewed articles. The type of storing media and temperature at which specimens were stored before and after bonding was mentioned in around 60% of studies.
List of Experimental Conditions Evaluated.
Discussion
Only the recent data from 2016 to 2020 was reviewed in our present study as the aim was to evaluate current prevailing methods of testing shear bond strength ,which technically is evolved from studying the past documented literature on the subject only. Thus, we believe that analyzing the data diligently from current literature will be more useful and relevant while formulating some meaningful guidelines for future studies. However, a study by Katrina et al 4 in 2010 had evaluated testing protocols pertaining to shear bond strength without mentioning any guidelines for specific parameters needed for future investigations.
The literature revealed that experimental conditions related to bond strength testing vary, and there is no uniformity in study design, leading to comparing results on an individual basis. The analysis from the literature reveals that the testing conditions such as storage of water, type of enamel with crosshead speed with type of blade used to apply load remarkably affect the outcome of in vitro bond strength testing.5 It was noted that none of the studies mentioned all experimental conditions. The type of teeth used in the study with the type of testing machine and method with its crosshead speed are the only variables mentioned in all 84 studies evaluated (Table 1). This shows that there is a lack of required data present in literature which can allow for comparing the results in toto.
There was a reduction in bond strength by 5 MPa to 7 MPa when samples were stored in water. 1 Distilled water was commonly used to store specimens in many in vitro studies. 6 However, few studies 7 did not mention the type of medium used to store specimens. Crosshead speed significantly affects the outcome of bond strength testing as it was reported that an increase in crosshead speed by 1 mm/min led to an increase in shear bond strength by 1.5 MPa. 8 However, few studies reported contrast findings where there is decrease in bond strength with an increase in crosshead speed.9, 10 In other studies, no impact was seen on bond strength with changes in crosshead speed. 10
Shear bond strength values reported in the literature ranged from 3.2 MPa to 41.3 MPa.11, 12 An in vitro bond strength of 6 MPa to 8 MPa is considered “clinically acceptable,” and bond studies relate their findings according to recommendation by Reynolds 13 in 1975. Bond strength between 6 MPa to 8 MPa is considered as a gold standard. However, it has never been tested whether in vitro 6 MPa to 8 MPa is an adequate bond strength in clinical settings. Thus, the use of this baseline value for comparison has been questioned previously by many authors. Hence, we proposed that absolute comparison of bond strength values with so-called “clinically acceptable” baseline value must be avoided or compared cautiously.6, 13
Different blade designs were used in studies to estimate the shear bond strength of orthodontic bracket. The blade method to debond the brackets was used in many studies, whereas wire loop method was used in a few studies.7, 14 The wire loop method is not a popular method for debonding the brackets as it generates some kind of tensile stress which is not a true form of shear bond strength testing. The wire loop method usually produces less shear bond strength than the blade method as some energy is loss because of presence of tensile stress.15-17
Although bond strength obtained from in vitro studies determine the actual strength of bonding adhesive with the surface of the enamel, its direct clinical implications are still doubtful.17, 18 Simulation of the oral environment is mandatory to correlate outcomes from in vitro studies for actual clinical scenarios. However, because of many unknown situations in oral environment, it is impossible to simulate oral environment accurately. Still, in vitro bond strength testing is considered acceptable to initially screen and select the biomaterials. 11 However, it cannot be considered an alternative to in vivo testing. Therefore, orthodontic biomaterials that prove their efficacy in in vitro settings, if can be tested with in vivo clinical testing, which is still away from reality, would add tremendous value and will truly validate the results for clinical practice.
Adhesive remnant index is the most valuable way to assess the type of bond failure. 3 Low adhesive remnant index (ARI) score achieved with any bonding system is significant clinically in preventing major loss of enamel as less adhesive remains on tooth surface need minimum amount of cleaning and polishing. The scoring of adhesive remnant indices is more subjective in nature; still it provides insight into the type of bond failure which is valuable in studies of orthodontic adhesive systems. A remarkable variation between ARI scores was reported 19 when the debonded teeth surface were evaluated at different magnifications. Hence, there is a need to standardize the guidelines related to the method assessing ARI score and formulate new methods which are more objective and quantitative that can assess the adhesive remnant present on tooth surface more accurately.
This review has the possibility of some limitations, especially related to selection bias and language restrictions. Although we tried reviewing the currently available literature on shear bond strength testing, we cannot deny the possibility of some kind of addition or deletion of studies based on variables that were not included.
Conclusion
With recent advances in adhesive dentistry, as reflected by the increased number of bond strength studies, there is a need to form recommendations to standardize the parameters to conduct in vitro bond strength research. Thus, experimental conditions such as storing media, temperature, crosshead speed of testing machine, type of shear testing method, and evaluation of adhesive remnant index will help establish the baseline data allowing the comparison of results among studies and thus reach a conclusion.
Clinical Relevance
This review highlights the orthodontic materials that prove their efficacy in laboratory settings, and if tested with in vivo clinical scenarios will truly validate the results for clinical practice.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
