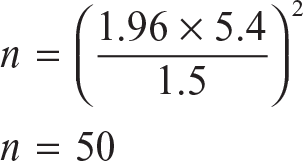Abstract
Abstract
Context: As lingual bonded retainers are required for long-term retention in the oral cavity, the wire-composite combination of choice may be the determining factor for the success of lingual bonded retainers.
Aim: We compared the shear bond strength of different wire-composite combinations used for lingual bonded retainers and identified the combination of choice for lingual retention in terms of the shear bond strength.
Materials and Methods: A total of 108 extracted human maxillary premolars in pairs were divided into 6 groups of 9 samples each. Three different types of retainer wires (namely, Respond [Ormco Corp., Orange, CA, USA], Leone Ligature Wire [Leone S.p.a., Firenze, Italy], and SRW™ Stranded Retention Wire [Ortho Classic Inc., USA]) were bonded to the teeth with the composites (G-aenial™ Universal Flo and Tetric N-Flow). The shear bond strength was measured on debonding using universal testing machine INSTRON.
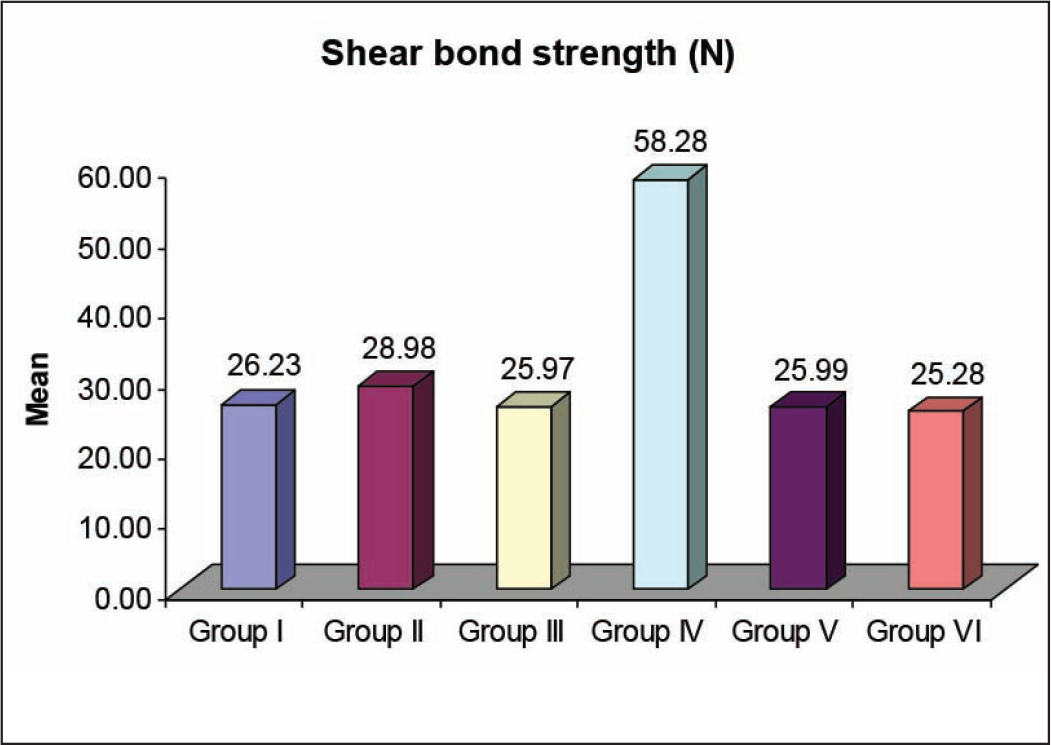
Results: The maximum shear bond strength (58.28 N) was observed in group IV (Respond wire with Tetric N-Flow), whereas the minimum (25.28 N) was observed in group VI (SRW™ Stranded Retention Wire with Tetric N-Flow). A highly significant difference was observed when the shear bond strength of group IV was compared with all the other groups.
Conclusions: The maximum shear bond strength was observed in the wire-composite combination of Respond dead-soft wire with Tetric N-Flow composite. Therefore, it could be the wire-composite combination of choice for bonded lingual retainer.
Introduction
Angle stated that “the problem involved in retention is so great as to test the utmost skill of the most competent orthodontist, often being greater than the difficulties being encountered in the treatment of the case up to this point.” 1
Lingual bonded retainers have established their popularity since the late 1970s, particularly in the mandibular incisor area. 2 However, bond failure in the retainer system is a frequently observed problem, resulting in the loss of retainer function, leading to relapse. 3
Conventional lingual bonded retainers have been made of high dimension, round/rectangular wires fixed to the canines only. Later on thin, flexible multistranded wires commonly 0.0195″ or 0.0215″ were bonded to each tooth from canine to canine. 4
The multistranded wires are recommended for lingual bonded retainers because of 2 main causes, first, having the irregular surface, which offers better mechanical retention for adhesion of composite, and second, the increased flexibility of the wire, which permits the physiologic tooth movement. 5
The failure of bonded lingual retentions may occur due to microcracks within the adhesive that form owing to the deformed interdental wire. Therefore, the wire-composite combination may be the factor for the success of bonded lingual retainers.
Therefore, this study was designed to compare different wire-composite combinations routinely used and to determine the wire-composite combination of choice for lingual retention.
Materials and Methods
A total of 108 extracted maxillary first premolars of patients undergoing orthodontic treatment were considered. The sample was decided based on the statistical power analysis. 6
Z is the value from the table of probabilities of the standard normal distribution for the desired confidence level (Z = 1.96 for 95% confidence).
E is the margin of error from the supporting studies2,7 (E = 1.5).
Therefore,
The sample should have the following criteria:
The crowns should be grossly perfect with no defect or any evidence of surface deformities. No history of chemical insult with agents like hydrogen peroxide. No structural alteration caused by mechanical procedures. Teeth with intact lingual enamel.
Teeth with any defect, surface defect, and caries were excluded.
Materials
In this study, 3 different types of wires were used as follows (Figure 1):
Respond (Ormco Corp., Orange, CA, USA), 0.0190″ dead-soft coaxial wire. Leone Ligature wire (Leone S.p.a., Firenze, Italy), 0.010″ dead-soft stainless steel ligature wire. SRW™ Stranded Retention Wire (Ortho Classic Inc., USA), 6 flattened coaxial stranded wire measuring 0.0195″.
For bonding, 2 different bonding kits (bonding agent and adhesive) were used according to the manufacturers’ recommendations to obtain the maximum bond strength (Figure 1).
G-aenial™ Bond and Universal Flo Kit (G-aenial™ Bond + G-aenial™ Universal Flo, microfilled hybrid composite, GC America Inc.)
Tetric N-Collection System Kit (Tetric N-Bond + Tetric N-Flow, microfilled hybrid composite, Ivoclar Vivadent, Ellwangen, Germany).
Study Sample
Based on the type of wire-composite combination to be used, the samples were randomly divided into 6 groups of 9 samples each as follows:
Group I—Respond wire + G-aenial™ Bond and Universal Flo Kit Group II—Leone Ligature wire + G-aenial™ Bond and Universal Flo Kit Group III—SRW™ Stranded Retention Wire + G-aenial™ Bond and Universal Flo Kit Group IV—Respond wire + Tetric N-Collection System Kit Group V—Leone Ligature wire + Tetric N-Collection System Kit Group VI—SRW™ Stranded Retention Wire + Tetric N-Collection System Kit.
Materials Used in the Study

The extracted premolars were cleaned and soft-tissue remnants removed using an ultrasonic scaler, and the teeth were stored in 10% formalin solution. Self-cure acrylic resin was poured into cylindrical polyvinyl chloride molds of 2.5 cm diameter and 2.5 cm height, and the roots of the 2 anatomically equal teeth in approximate contact were embedded in the acrylic to simulate contact point. The teeth were embedded in the acrylic so that the long axis of each tooth was perpendicular to the base (Figure 2). Fluoride-free pumice was used for polishing the lingual surfaces of each tooth, which was followed by washing with distilled water and air-drying.
Surface Conditioning
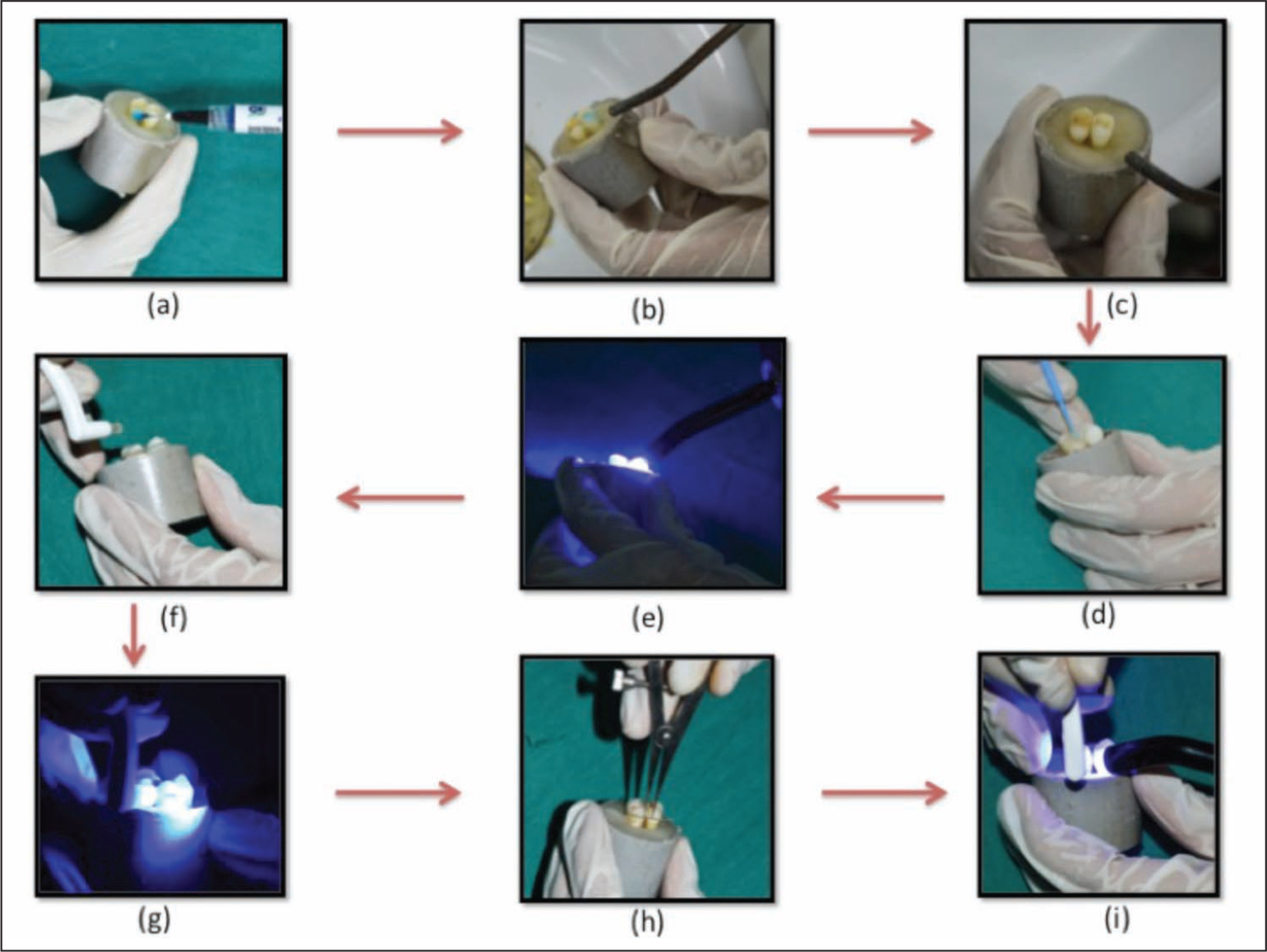
Etching was done using 37% phosphoric acid, FROST (Ammdent, Mehrauli, India) for 30 seconds. The samples were then washed with water for 10 seconds and air-dried for another 10 seconds using the 3-way syringe. The bonding kits (bonding agent and adhesive) were then applied to the samples of the respective groups according to the manufacturer’s instructions (Figures 3[a]-[e]).
Mounted Samples

Bonding Procedure
The wire was curved gently to give a passive fit to the tooth surface. A length of 15 mm was marked on the respective wire and then cut using a sharp ligature wire cutter. The center point of the wire segment was marked using a marking pen and placed on the conditioned enamel so that it was parallel to the base of the mold below the contact point of the teeth. The amount of composite used for bonding the wire segment was standardized using commercially available dome-shaped mold, Mini-Mold (Ortho Arch) (Figure 4). It has an indentation in the center that allows the wire to be placed right in the middle of the composite. To keep the wire span constant, 2 mm distance on each side of the midpoint on the wire is kept constant, and the molds were placed just distal to it. The composite was applied using wire bonder tips (Figure 3[f]).
Methodology. (a) application of etchant; (b) rinsing of etchant; (c) drying of etchant; (d) application of bonding agent; (e) light curing of bonding agent; (f) application of adhesive on wire using Mini-Mold wire bonder on one tooth; (g) light curing of adhesive on the first tooth; (h) measurement of space for the application of adhesive on the second tooth; (i) light curing of bonding agent on the second tooth.
Mini-Mold (Ortho-Arch) and Wire Bonder Holder
The size of the composite dome was 3 mm in diameter with a maximum depth of 1.5 mm. Hence, in total, an area of 7.65 mm2 was available for bonding on each tooth and 14.13 mm2 for each sample.
Flash was then removed from the margins of the mold before curing the composite. Composite was cured for 20 seconds using a light-cure unit (Figure 3[g]). The same procedure for bonding is repeated for the adjacent tooth in each sample (Figures 3[h] and [i]). Each specimen was stored in artificial saliva at room temperature for 24 hours.
Debonding Procedure
The debonding procedure was followed according to the method prescribed by Aldrees et al. The sample was mounted such that the long axis was parallel to the force applied, and bonded wire segment was perpendicular to the force applied for bond failure in the study. Apically directed force was applied at the midpoint of the bonded wire using a plunger with a beveled edge fixed to the universal testing machine INSTRON at a speed load of 1 mm/min until bond failure occurred (Figure 5). The load was recorded in Newton (N). 4
Measurement of Shear Bond Strength on Debonding Using Universal Testing Machine INSTRON

Statistical Analysis
Shear bond data were summarized as mean ± standard error of the mean and compared using one-way analysis of variance (ANOVA), and the significance of the mean difference between (inter) the groups was done using Tukey’s honestly significant difference post hoc test after ascertaining normality by using Shapiro-Wilk test and homogeneity of variance between groups by using Levene’s test. A p value of (<0.05) was considered significant. Analyses were performed on SPSS Statistics 17.0 (SPSS software, IBM Corp., Armonk, NY, USA).
Results
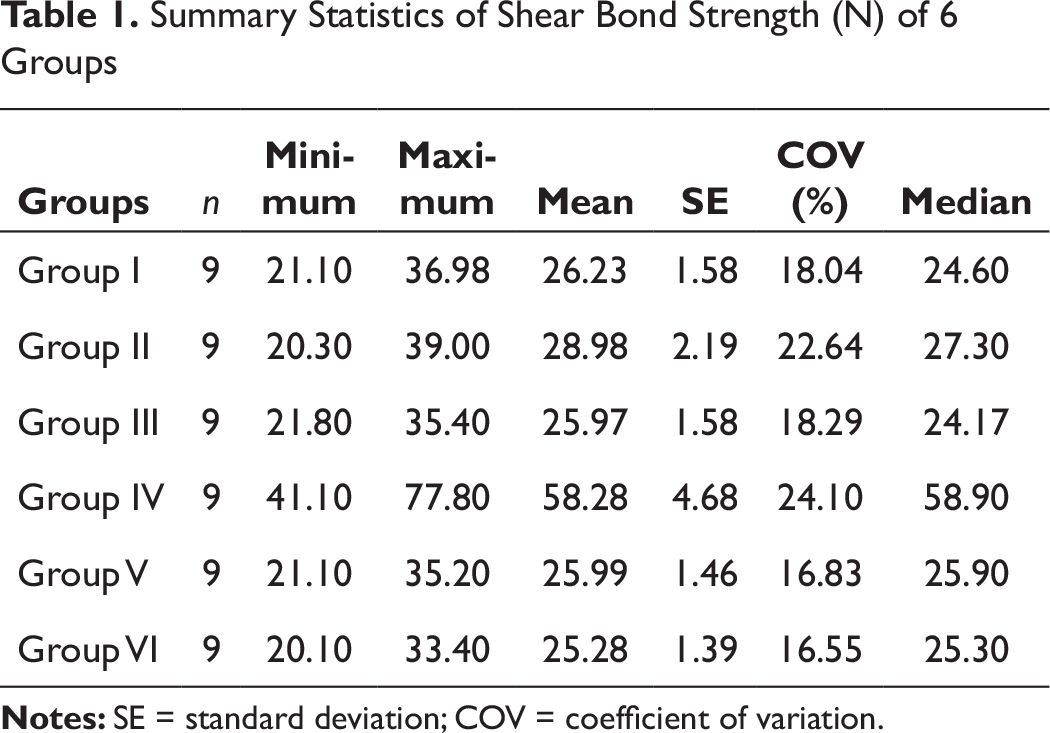
The shear bond strengths (N) of the 6 groups are summarized in Table 1 and Figure 6. Maximum shear bond strength was observed in group IV (58.28 N), whereas minimum was observed in group VI (25.28 N).
Mean Shear Bond Strength (n) of 6 Groups
Summary Statistics of Shear Bond Strength (N) of 6 Groups
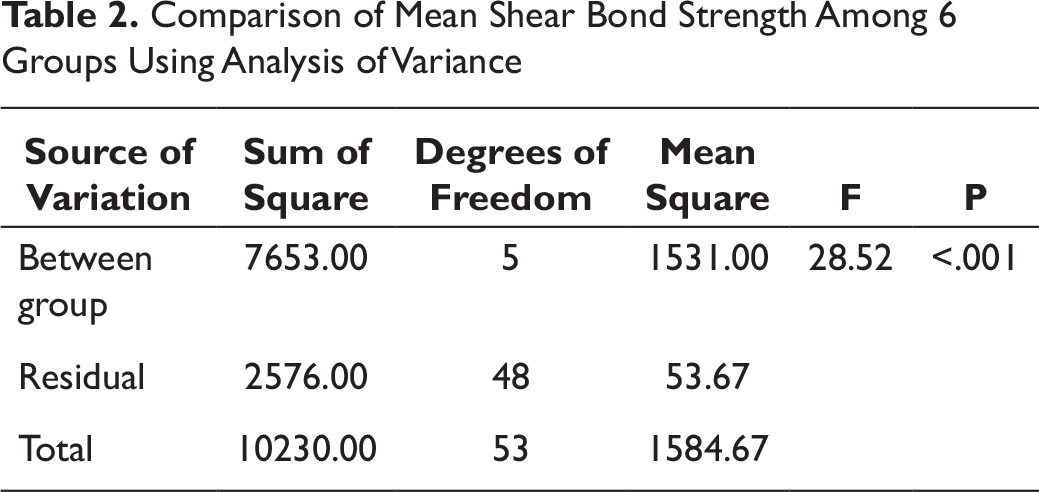
On comparison of the mean shear bond strength among 6 groups, ANOVA revealed statistically significant difference (F = 28.52, P < .001) (Table 2).
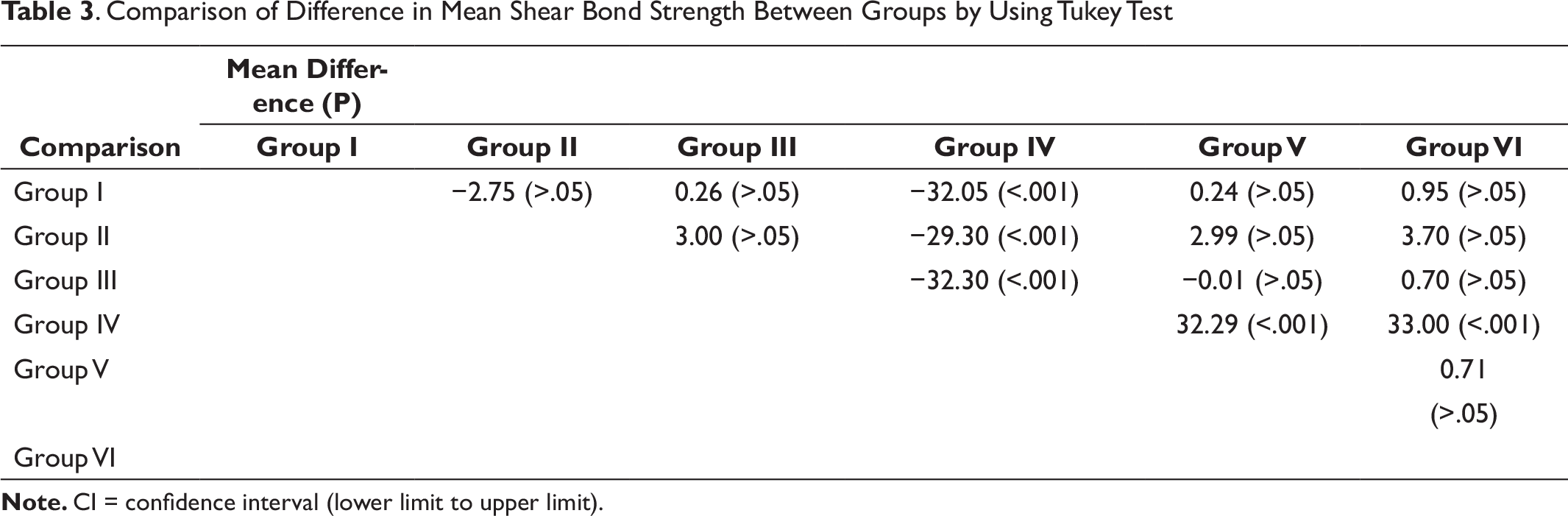
On applying the Tukey’s test, there was a highly significant difference when the shear bond strength of group IV was compared with all the other groups (groups I, II, III, V, and VI). No statistically significant difference was observed between the groups except for group IV (Table 3).
Discussion
Lingual bonded retainers are popularly used after the active orthodontic treatment to prevent relapse. However, the failure of the bonded retainer due to wire breakage or bond failure is the only drawback. Therefore, the bond strength of the wire-composite combination becomes the important factor for the success of lingual bonded retainer. 3
Multistranded round wires are popular in lingual retention as they provide improved mechanical retention due to their intertwined nature and also allow for physiologic tooth movement.4, 8, 9 With lesser tendency for stress fracture, the multistranded wires have resulted in higher success rate when used in lingual bonded retainers.10, 11
From the large range of composites available, 2 microfilled hybrid composites (Tetric-N-Flow and G-aenial Universal Flo) were selected because they had better polishing characteristics and elasticity than macrofilled composites, thus helping them to withstand forces in the retainer system. 3
Comparison of Mean Shear Bond Strength Among 6 Groups Using Analysis of Variance
In our study, the mean shear bond strength ranged from 25.28 to 58.28 N, with group IV (Respond dead-soft wire with Tetric N-Flow) showing the highest shear bond strength. Similarly, Radlanski and Zain 3 observed the maximum shear bond strength of 64.3 N in groups bonded with Tetric-N-Flow, which was higher than groups bonded with Heliosit. According to Bryan and Sherriff, 12 clinically acceptable mean shear bond strength is found to be 71 N.
Filler content of G-aenial Universal Flo is 69 wt% when compared with Tetric N-Flow, which is 63.8 wt%. Because viscosity increases with increase in filler content, it could be assumed that Tetric N-Flow has better flowability and wettability than G-aenial Universal Flo, which contributed to increased bond strength. In terms of shear bond strength, we can conclude that group IV (Tetric N-Flow with Respond wire) showed the highest shear bond strength.
Highly significant difference was observed when group IV was compared with groups V and VI. This means that Respond wire fared better than ligature wire retainer and SRW in terms of the shear bond strength.
As both Respond and SRW are coaxial wires, the large difference between them could be attributed to the nature of the retainer material. Wires with a high degree of annealing are described in the literature as “dead soft.” 13 Heat treatment relieves the stresses retained from archwire formation and improves malleability and stability of archwire form because of increased proportional limit, strength, and range.4, 11, 14 Furthermore, dead-soft wire adapts better to vertical loads. Respond is a dead-soft wire, which means that it is passive and does not exert any active force when adapted to the tooth surface. On the other hand, SRW is a plain coaxial wire, which might have residual forces while twisting the strands during manufacturing process. These stored forces can lead to the accumulation of stresses at the points of masticatory overloads, causing fatigue and failure of the bond between wire and adhesive. 13
Therefore, from our study, it can be concluded that the most deciding factor in the shear bond strength is neither the wire nor the composite alone. It is the wire-composite combination that decides the ultimate shear bond strength. The combination of TetricNFlow and Respond wire produced clinically acceptable shear bond strength values possibly due to the greater flowability of the resin around the strands of the wire, which increases the micromechanical retention and the flexibility of the dead-soft wire, which adapted better to the tooth surface.
Comparison of Difference in Mean Shear Bond Strength Between Groups by Using Tukey Test
Conclusions
The following can be concluded from our study:
Maximum shear bond strength was observed in the wire-composite combination of Respond dead-soft wire with Tetric N-Flow composite. A highly significant difference was observed between group IV (Tetric N-Flow and Respond wire) and the other groups. All the other wire-composite combinations showed no statistically significant difference, exhibiting similar shear bond strength values. Respond dead-soft wire with Tetric-N-Flow would be the wire-composite combination of choice for bonded lingual retainer.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.