Abstract
Uterine tumors resembling ovarian sex cord tumors (UTROSCTs) are rare uterine neoplasms that exhibit prominent sex cord-like differentiation. The authors describe 4 cases of UTROSCTs that were identified as incidental lesions in female baboons. All baboons were in good body condition. One animal had a 2-mm-diameter yellow-tan mass in the uterine body along the attachment of the left broad ligament; the other 3 did not have any gross lesions in the uterus. Histologically, the myometrium contained multifocal well-demarcated neoplasms composed of cuboidal to columnar cells arranged in variable arrangements of sheets, nests, cords, trabecular, and retiform patterns that occasionally formed Call-Exner-like bodies. In all cases, the neoplastic cells were diffusely positive for WT-1 and negative for calretinin, CD99, and desmin. One case was positive for inhibin and CD10. To the best of the authors’ knowledge, this is the first report of UTROSCTs in nonhuman primates and in the veterinary literature.
Keywords
Uterine tumors resembling ovarian sex cord tumors (UTROSCTs) are rare uterine tumors that resemble ovarian sex cord tumors and exhibit prominent sex cord-like differentiation without a component of recognizable endometrial stroma. 10,13 In humans, they were initially thought to be either endometrial stromal tumors or uterine granulosa cell tumors due to their histological resemblance to granulosa cell tumors of the ovary. 3,13 The exact histogenesis is not known; there is some immunohistochemical and cytogenetic evidence that the neoplastic cells are derived from ovarian sex cord stromal cells, but the debate is still ongoing. 5,8,15,17 UTROSCTs typically present as well-circumscribed, yellow, gray, or tan masses up to 10 centimeters in diameter, with variable cellular arrangements including anastomosing cords, trabeculae, nests, diffuse sheets, or retiform patterns. 15 UTROSCTs have been reported in humans, 16 but have not been reported in the veterinary literature. We present 4 cases of UTROSCTs identified as incidental lesions in captive baboons at Southwest National Primate Research Center.
Materials and Methods
The baboons were socially housed in two 6-acre outdoor corrals, outdoor metal and concrete gang cages, and indoor-outdoor cages. For variable periods of time, baboons were housed inside buildings individually or in groups for research or other special purposes. The baboons were fed a diet of commercial monkey chow (Teklad©, PMI Nutrition International, LLC, Brentwood, MO 63144) supplemented with grains, fruits, and vegetables and provided water ad libitum. All animal care and procedures were approved by the Texas Biomedical Research Institute Institutional Animal Care and Use Committee. The lifetime records for each baboon were retrieved and reviewed for clinical and surgical history, research-use, and reproductive history.
The animals were euthanized for tissue collection. Complete necropsies were performed and appropriate tissue samples were taken for histologic evaluation. All tissues were fixed in 10% neutral buffered formalin, processed conventionally, embedded in paraffin, cut at 5 micrometers, stained with hematoxylin and eosin and evaluated by board-certified veterinary pathologists.
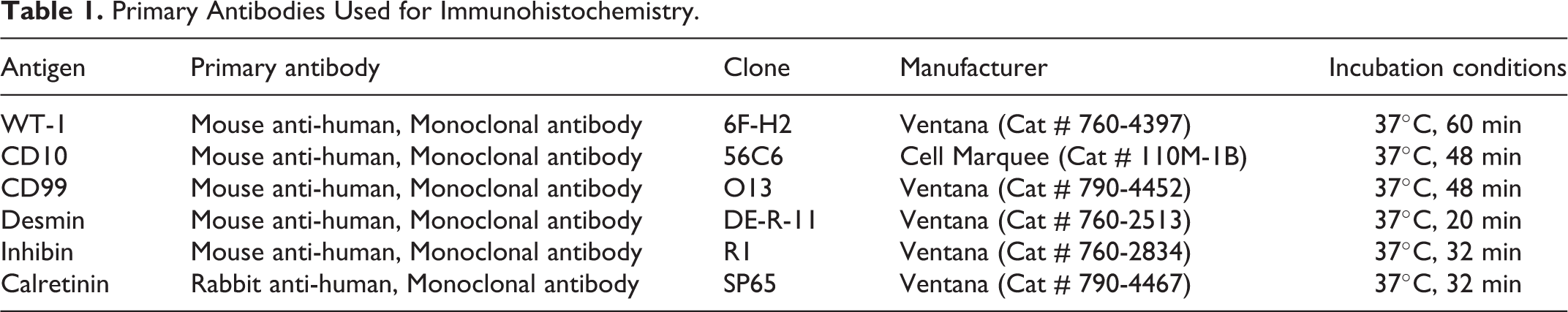
For immunohistochemical labeling, reagents were procured from Ventana Medical Systems, Tucson, AZ, USA. All stains were completed using the Ventana BenchMark Ultra automatic stainer (Ventana Medical Systems, Inc., Tucson, AZ, USA). Immunohistochemical staining was performed on formalin-fixed, paraffin-embedded, 4-micrometer-thick serial sections of uterus as well as appropriate control tissues. For all immunohistochemical labeling except desmin, slides were deparaffinized, and treated with heat-induced epitope retrieval in cell conditioning solution (CC1; Ventana Medical Systems, catalog number 950-124) at 95°C for 36 minutes. For desmin, the deparaffinized slides were treated with Protease1 for 4 minutes at room temperature and no heat treatment was performed. Subsequently, all slides were incubated with primary antibody. The specific primary antibodies used, and their respective incubation temperatures are listed in Table 1. The UltraView Universal DAB detection Kit (Ventana Medical Systems, catalog number 760-500) was applied containing a secondary multimeric antibody and 3,3-diaminobenzidine (DAB) as the chromogen, and the slides were counterstained with hematoxylin (Ventana Medical Systems, catalog number 760-2021)/Bluing (Ventana Medical Systems, catalog number 760-2037) for 4 minutes each. For negative controls, the primary antibody was replaced with a commercial antibody diluent (Ventana Medical System Inc.).
Primary Antibodies Used for Immunohistochemistry.
Results
Animal Demographics and Relevant Clinical History
Four female baboons from the breeding colony were euthanized for tissue collection. Their demographics and clinical histories are shown in Table 2. The most recent data collected from menstrual cycle observations of these individuals, recorded based on a numerical grade point system that scores the tumescence of the perineal region (sex skin), 7 suggested that Case 3 had regular menstrual cycle measurements about 2 months prior to necropsy. For Cases 1, 2, and 4, menstrual cycle measurements were regular until monitoring was stopped approximately 2 years before necropsy because they were either retired breeders, or were used as nannies. Pedigree analysis was performed for each of the 4 cases to establish relatedness between the 4 baboons, but was not successful because of incomplete/insufficient data.
Demographic Data and Relevant Clinical History in 4 Baboons With Uterine Tumors Resembling Ovarian Sex Cord Tumors.

aStillbirth.
bCaesarian section.
Pathologic Findings
At necropsy, all animals had adequate muscle mass, hydration, and adipose tissue. Case 1 had a small, yellow-tan, 2-mm-diameter mass in the uterine body along the attachment of the left broad ligament (Fig. 1). Case 2 had a translucent, right paraovarian cyst approximately 1 millimeter in diameter. Otherwise, the reproductive tract from all baboons did not have any gross lesions.
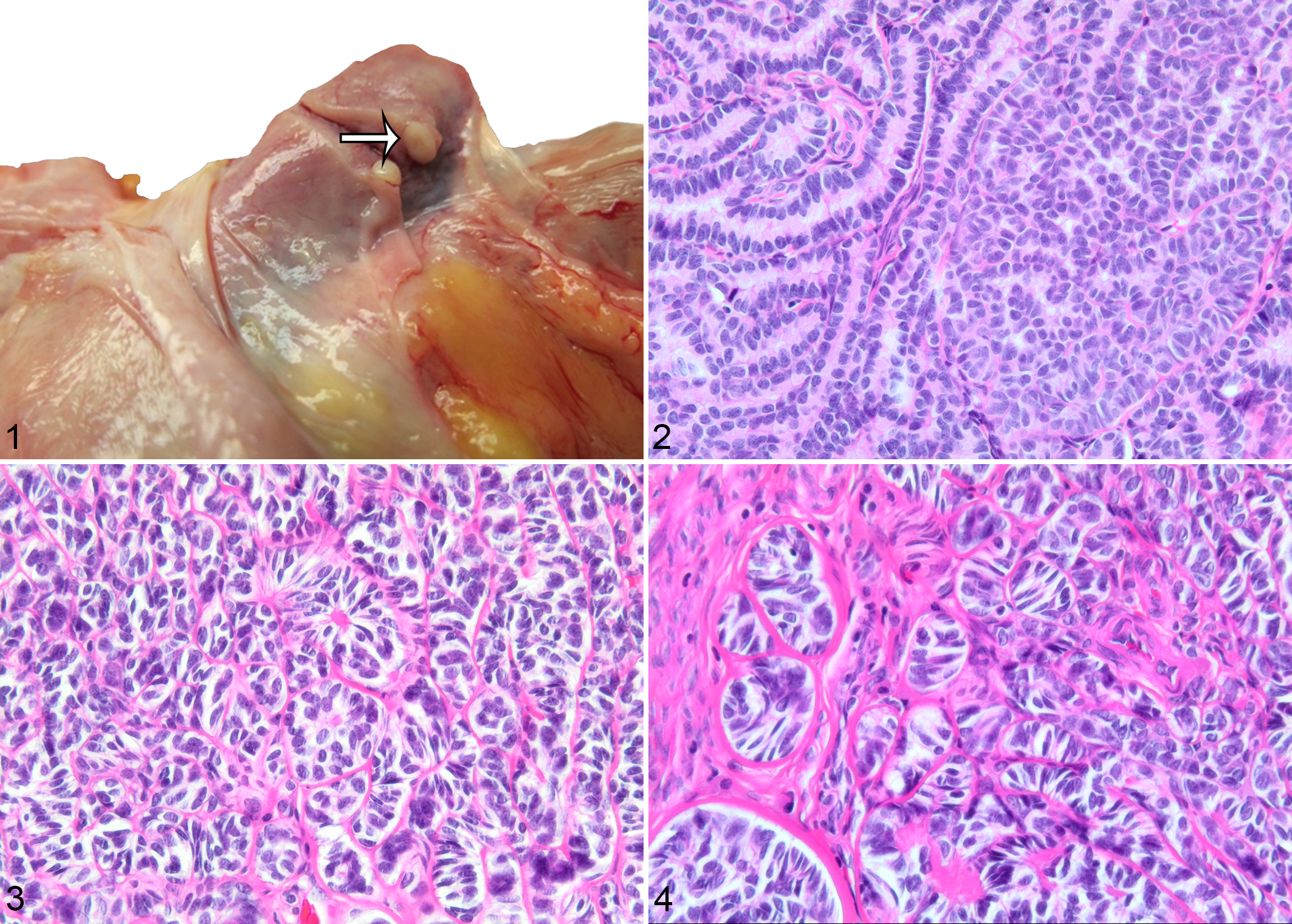
Histologically, all baboons had well-defined, expansile, nonencapsulated tumors (Figs. 2–5) located in the myometrium, near or adjacent to the serosa, composed of cuboidal to columnar cells arranged in anastomosing cords and trabeculae (Fig. 2), and small nests and packets occasionally surrounding a central space filled with eosinophilic fluid (Call-Exner-like bodies, Fig. 3). The neoplastic cells were supported by a fine fibrovascular stroma and had indistinct margins, scant, homogeneous, clear to eosinophilic cytoplasm, a round to ovoid nucleus with clumped chromatin and an indistinct nucleolus. There was minimal anisocytosis and anisokaryosis, and mitoses were not noted. Some variations were noted between the different individuals. Case 4 had multiple spindle-shaped cells within the mass forming a retiform or sertoliform pattern (Fig. 4). Cases 2 and 4 had multiple small masses grouped in 1 area in which neoplastic cells were arranged in diffuse sheets (Fig. 5a). Case 3 had more tubular formations interspersed throughout the mass.
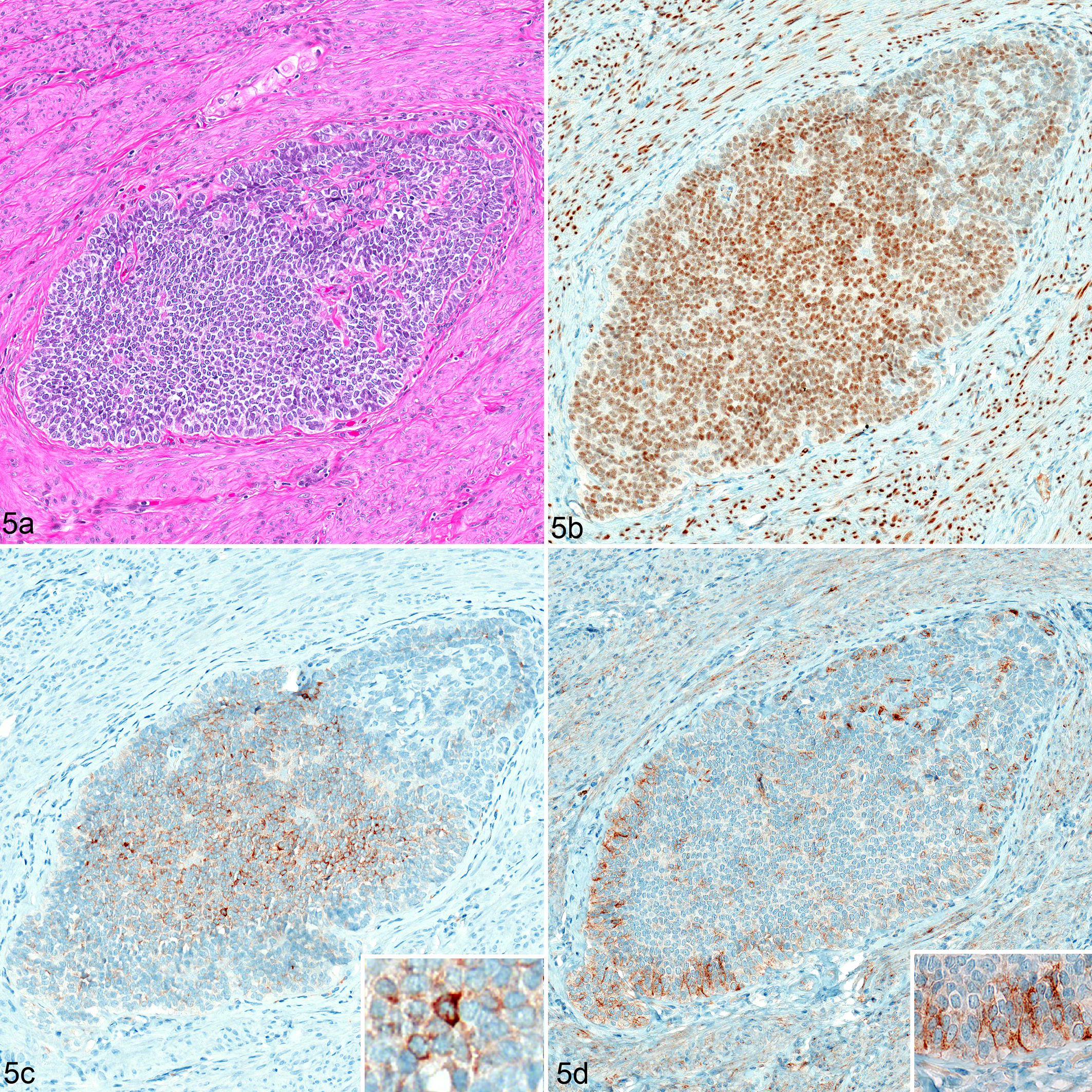
Uterine Tumor Resembling Ovarian Sex Cord Tumors, Baboon. Case 2.
For all cases, the neoplastic cells were diffusely and strongly positive for WT-1 (Fig. 5), and were diffusely negative for calretinin, CD99, and desmin. In 1 case (Case 2), neoplastic cells showed moderate cytoplasmic immunoreactivity for inhibin and weak membranous staining for CD10 (Fig. 5; Table 3).
Immunohistochemistry Findings in Uterine Tumor Resembling Ovarian Sex Cord Tumors of Baboons (UTROSCT) and Comparison to Reported Human Cases.
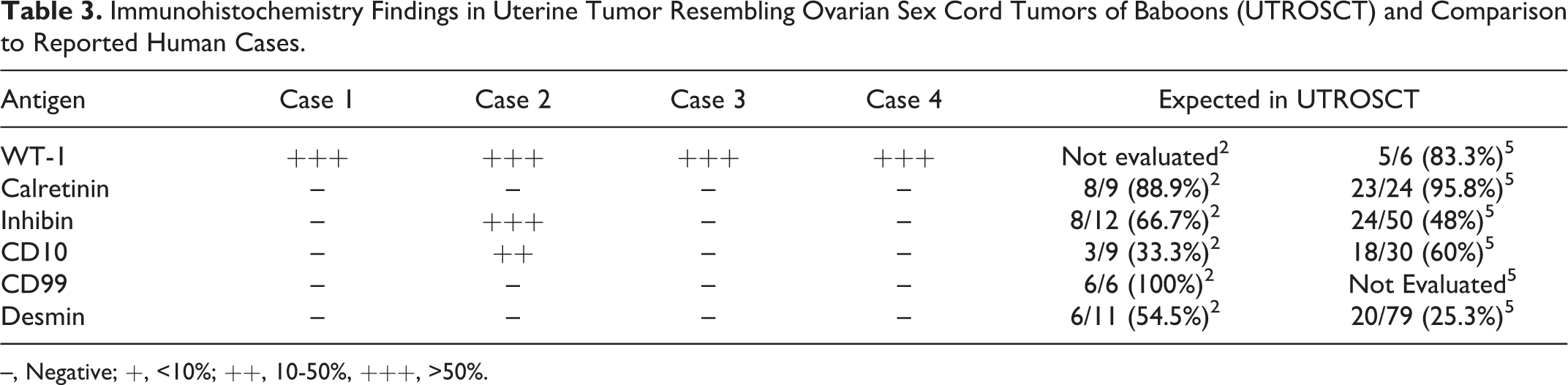
–, Negative; +, <10%; ++, 10-50%, +++, >50%.
Discussion
We present 4 cases of UTROSCTs in baboons. UTROSCTs are a subgroup of endometrial stromal tumors, which are histologically similar to ovarian sex cord stromal tumors. The overall incidence is unknown, and is likely underreported, given that they are usually diagnosed after hysterectomy. Endometrial stromal tumors were first reported by Morehead and Bowman in 1945 as heterologous mesodermal tumors of the uterus, 13 and subsequently, Clement and Scully divided them into 2 groups based on their clinical behavior and histopathologic appearance: Group I, which included endometrial stromal tumors with sex cord-like elements (ESTSCLE), where there is predominant endometrial stromal tumor differentiation with less than 50% ovarian sex cord-like areas, and Group II, UTROSCTs, where there is a predominant ovarian sex cord-like component (50–100%). 3 In the most recent WHO Classification of Tumours of Female Reproductive Organs, UTROSCTs are classified as those without a recognizable endometrial stromal component. 10 UTROSCTs are typically benign, although there have been a few reported cases of metastasis and recurrence. 14,16,18
UTROSCTs are typically seen in multiparous or nulliparous, peri-menopausal to postmenopausal women, although, they have been reported infrequently in younger women as well. 3,15 This is consistent with our case series, in which 2 baboons were multiparous older females (21 and 23 years old), a relatively younger multiparous 15-year-old female, and a 12-year-old nulliparous female with a small vaginal opening, which could have been the cause of the observed infertility. In the terms of reproductive senescence in baboons (menopause), increased cyclic variation begins around 19 years of age and cessation of cycling usually occurs at their mid-20s, which puts the animals in the present case series in peri-menopausal to postmenopausal age range. 12,19 Because of the incomplete menstrual cycle records for 3 animals (Cases 1, 2, and 4), it couldn’t be confirmed if the baboons exhibited signs of menopause or not. Human UTROSCT cases typically present with abnormal uterine bleeding, pelvic or abdominal pain, an enlarged uterus, or a palpable mass. 11,15 However, all 4 cases in this report were incidental lesions with no clinical signs.
The tumors are generally located in the intramural, submucosal, or subserosal regions in the uterine fundus with sizes ranging from 2 to 15 centimeters, with a fleshy, gray, yellow to white color. 4,15 The masses are nonencapsulated but well-circumscribed with expansile or infiltrative borders. The gross description of UTROSCTs in humans closely resembles the appearance of the tumor found in the uterus of Case No.1. In humans, the overlying endometrium may be involved and polypoid masses in the uterine cavity are common. 15 One human case of UTROSCT also had a concurrent granulosa cell tumor in the ovary. 1 No concurrent neoplasms were observed in any of the 4 baboons.
Diagnosis of UTROSCT is usually made after a combination of histological and immunohistochemical analyses. 15 Histological features include the presence of anastomosing cords or small nests of cells, trabeculae supported by fibrovascular stroma, and Call-Exner-like bodies, with no histological indication of malignancy. 18 The presence of spindle-shaped cells in Case 4, suggestive of a mesenchymal origin for some of the cells, and the diffuse sheets of cells in Cases 2 and 4 have previously been reported in some cases of UTROSCTs. 3,20 Some of the other morphological variations noted in the present case series including solid tubules containing vacuolated cells and sertoliform pattern have been previously reported. 5,15
Human UTROSCTs are generally reported positive for sex cord markers such as WT-1, calretinin, inhibin, CD99, and Melan-A, with variable expression of other markers. 8 Their immunophenotype is variable as they often exhibit coexpression of epithelial, myoid, sex cord markers, and hormone receptors. 1,4 –6,8,9 WT-1 has been shown to be expressed during development of the urogenital system and is detected in the mesonephros, metanephros, spleen, gonads, and mesothelium of fetuses, as well as nephroblastomas, desmoplastic round cell tumors, mesotheliomas, ovarian carcinomas, sex cord tumors of the ovary, endometrial stromal tumors, and uterine smooth muscle tumors. 5 The neoplastic cells in all 4 cases were diffusely and strongly positive for WT-1 and negative for calretinin, CD99, and desmin. One case was positive for inhibin and CD10. Inhibin, calretinin, and WT-1 are often used as markers of sex cord differentiation (and most cases of UTROSCTs are positive for 1 or more sex cord markers), 5 desmin is a smooth muscle marker, and CD10 is a stromal marker. 5,15 This immunohistochemical staining pattern is nonspecific, but broadly consistent for UTROSCTs and supports a sex cord phenotype. 5,8,9
There is some debate as to the histogenesis of UTROSCTs. Their immunohistochemical profile appears to overlap with those of ESTSCLE which have less sex cord marker expression, and ovarian sex cord stromal tumors which have high sex cord marker expression. Czernobilsky postulated that with the variable morphological and mixed epithelial-myoid immunohistochemical features, the origin of UTROSCTs as well as their similar counterpart ESTSCLE is likely to be from pluripotent mesenchymal uterine cells. 4 Ultrastructural analyses of 13 UTROSCTs found that the neoplastic cells have both epithelial and sex cord-like features with concurrent immunohistochemical reactivity for epithelial and sex cord markers. 6 This study by Gupta et al, found that the neoplastic cells did not exhibit smooth muscle features ultra-structurally, but most were positive for smooth muscle markers. 6 Their findings suggest that UTROSCTs either derive from endometrial stromal tumors, which are typically positive for smooth muscle markers, or they represent a distinct group of uterine tumors with sex cord-like differentiation. 6 A cytogenetics based study in which UTROSCTs were found to not have a gene translocation seen in over 60% of ESTSCLEs and their variants (JAZF1-JJAZ, also called JAZF1-SUZ12 translocation) further supports the latter argument. 17
In conclusion, we report 4 cases of UTROSCTs in baboons (Papio spp.), which to the best of our knowledge is the first report of these neoplasms in nonhuman primates and in the veterinary literature. The histological findings of well-demarcated, unencapsulated, expansile myometrial masses with cuboidal to columnar neoplastic cells arranged in anastomosing cords, trabeculae, small nests, and packets supported by a scant fibrovascular stroma, and the presence of Call-Exner-like bodies are consistent with a diagnosis of UTROSCT. It is noteworthy that all 4 cases reported here were incidental lesions, and 3 were not grossly apparent. Hence, such cases may be underdiagnosed.
Footnotes
Acknowledgements
The authors thank Dr Philip Branton, MD (Joint Pathology Center, Silver Spring, MD) for his assistance in diagnosing these cases. The authors thank Sarah Pennington, Jesse Martinez, Antonio “Tony” Perez, and Renee Escalona for their anatomic pathology support and the clinical support staff of the Texas Biomedical Research Institute, Mark Sharp and Deborah Newman for assistance with pedigree analysis and interpretation and Terry Hawkins and Scott Rouse for database assistance.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This investigation used resources that were supported by the Southwest National Primate Research Center Grant P51 RR013986 from the National Center for Research Resources, National Institutes of Health and are currently supported by the Office of Research Infrastructure Programs through P51 OD011133. This investigation was conducted in facilities constructed with support from the Office of Research Infrastructure Programs (ORIP) of the National Institutes of Health through Grant 1 C06 RR016228. The views expressed in this article are those of the author and do not reflect the official policy of the Department of the Army/Navy/Air Force, Department of Defense, or the US Government.
