Abstract
Liposarcoma, rhabdomyosarcoma, and hibernoma share some overlapping histologic and immunohistochemical features. Although immunohistochemistry (IHC) is commonly used in the diagnosis of these neoplasms, expression of muscle markers has been reported in human liposarcoma and canine hibernoma in addition to rhabdomyosarcoma. Thus, these neoplasms are a diagnostic challenge but important to distinguish because of differences in prognosis and treatment. Rhabdomyosarcoma and liposarcoma are both malignant, but rhabdomyosarcoma has a higher potential for metastasis. In contrast, hibernomas are benign with low risk of recurrence. This study investigated expression of the muscle markers desmin, myogenin, and α-smooth muscle actin (α-SMA) and the brown fat marker uncoupling protein 1 (UCP1) in 25 cases of canine liposarcoma using IHC. Oil red O histochemistry was performed to confirm the presence of lipid and the diagnosis of liposarcoma in cases that were not well-differentiated. The 25 cases included 15 well-differentiated, 5 pleomorphic, 3 myxoid, and 2 dedifferentiated subtypes of liposarcoma. By IHC, 23 of 25 expressed UCP1, 7 of 25 expressed α-SMA, 7 of 25 expressed desmin, and 3 of 25 expressed myogenin with no clear relationship of antigen expression and tumor subtype. These findings clarify the immunohistochemical profile of canine liposarcoma and suggest overlap in the expression of several muscle antigens and UCP1 between liposarcoma, hibernoma, and rhabdomyosarcoma.
Keywords
Liposarcoma is a malignant neoplasm of adipose tissue that is uncommon in domestic animals. Local invasion is frequent, but metastasis—usually to the lung, liver, and/or bone—is rare. 9,26 Liposarcomas are morphologically hetereogeneous, ranging from sheets of pleomorphic adipocytes in well-differentiated liposarcomas to streams of spindloid cells and lipoblasts in myxoid liposarcomas. 9,16,24,29 Oil red O and Sudan black stains, while not specific for liposarcoma, can confirm the diagnosis for cases in which morphology is consistent with one of the liposarcoma subtypes. These stains also help to rule out liposarcoma for cases in which there is morphologic overlap, such as in myxofibrosarcoma, a neoplasm resembling myxoid liposarcoma that is composed of pseudolipoblasts (ie, vacuolated cells containing mucin instead of lipid) in a myxoid matrix. 16 Lipid stains require fresh tissue or unprocessed formalin-fixed tissue, which is not always available in diagnostic settings. 8,9 Prognosis of canine liposarcoma is assumed to correlate with grade as determined by a soft tissue sarcoma (STS) grading scheme for subcutaneous masses. 7 A retrospective study on canine liposarcoma found that the width of surgical margin was correlated with survival time. That study did not consider histologic grade but found that histologic subtype, neoplasm size, and anatomic location were not correlated with survival time. 3
While the diagnosis of canine liposarcoma is often straightforward for well-differentiated neoplasms, pleomorphism or poorly differentiated variants and/or small sample size may obscure the correct diagnosis. Conflicting data on the expression of muscle markers by canine liposarcomas have been reported. Markers of muscle differentiation are reportedly expressed in some spindle cells in certain subtypes of human liposarcomas, including well-differentiated, dedifferentiated, and pleomorphic subtypes. 14 A recent review of liposarcoma in domestic animals stated that pleomorphic liposarcomas are uniformly negative for these markers. 8 In contrast, another recent article reported that 2 poorly differentiated canine liposarcomas were immunoreactive to a muscle marker (ie, desmin), but these poorly differentiated tumors were not confirmed to be liposarcoma with lipid stains. 19
Potential misdiagnosis of liposarcoma as rhabdomyosarcoma has prognostic significance as rhabdomyosarcomas have a particularly poor prognosis. Further, liposarcoma is graded using the scheme for canine STS, whereas rhabdomyosarcoma is excluded from this grading scheme. 7,15 The histomorphology of liposarcoma subtypes overlaps with some rhabdomyosarcoma subtypes, complicating the distinction of these 2 neoplasms. For example, both myxoid liposarcoma and spindloid embryonal rhabdomyosarcoma are composed of spindle cells in a myxoid background. Similarly, pleomorphic rhabdomyosarcoma and pleomorphic liposarcoma share histologic features, especially in cases of pleomorphic liposarcoma with a small lipoblast component. 4 Additionally, findings from a recent report of canine hibernoma—a benign tumor of brown adipose tissue—are based on the expression of electron transport coupling (uncoupling protein 1 [UCP1]) in addition to neoplastic cells showing benign histomorphologic features resembling brown adipocytes. This study suggested that UCP1 expression distinguishes hibernomas from other lipomatous tumors; however, the study did not include a liposarcoma control group, and the expression of UCP1 by canine liposarcoma is unknown. 25 There is potential for misdiagnosis of benign hibernomas if the diagnosis is solely based on UCP1 expression, and this is prognostically significant as liposarcoma has potential for aggressive behavior both locally and systemically. The purpose of this study was to determine the immunohistochemical profile of canine liposarcoma in relation to markers classically associated with skeletal muscle and brown adipose differentiation.
Materials/Methods
The UC Davis Veterinary Medical Teaching Hospital (Davis, CA) archives were searched for the diagnosis of liposarcoma in dogs, and potential cases were retrieved. Three additional cases diagnosed as liposarcoma were obtained from VDx (Davis, CA), a private diagnostic laboratory. All cases were reviewed for potential inclusion in this study. Based on standards for diagnosis of liposarcoma in humans, cases in which histomorphology alone was considered sufficient for the diagnosis of liposarcoma included all well-differentiated liposarcomas, pleomorphic liposarcomas in which ≥50% of the neoplasm was composed of lipid-containing neoplastic cells, and dedifferentiated liposarcomas in which ≥50% of the neoplasm was composed of well-differentiated regions. 16 Cases in which histomorphology alone was not considered definitive included all myxoid liposarcomas, pleomorphic liposarcomas in which <50% of the neoplasm was composed of lipid-containing neoplastic cells, and dedifferentiated liposarcomas in which <50% of the neoplasm was composed of well-differentiated regions. To establish a definitive diagnosis in cases in which histomorphology alone was considered inadequate, sections stained with oil red O were reviewed from archival slides or performed on wet tissues. Wet tissues were retrimmed, embedded in Optimal Cutting Temperature (OCT), snap-frozen, cryosectioned at 4 μm, and stained with oil red O to confirm the presence of intracellular lipid. Cases were included when intracytoplasmic lipid droplets were confirmed in definitively neoplastic cells.
Paraffin-embedded tissues were sectioned at 4 μm for immunohistochemistry (IHC). Heat-induced epitope retrieval was performed with Dako Target Retrieval Solution (S1699; Dako, Carpinteria, California, USA) for 30 minutes at 95°C followed by a 20-minute cool down. Primary antibodies, diluted in phosphate buffered saline (PBS), applied to each neoplasm were anti-desmin (Cell Marque, Rocklin, California, USA, 243M-16, 1:100 dilution, mouse monoclonal), anti-myogenin (NeoMarkers, Fremont, California, USA, MS-1113-P, 1:200 dilution, mouse monoclonal), anti–α-smooth muscle actin (α-SMA; BioGenex, San Ramon, California, USA, MU128-UC, 1:300 dilution, mouse monoclonal), and antibody recognizing uncoupling protein 1 (UCP1; Acris Antibodies, San Diego, California, USA, ABIN1720809, 1:100 dilution, rabbit polyclonal). The primary antibodies were detected with the 4+ Detection System (Biocare Medical, Concord, California, USA) and visualized with Vector NovaRED for peroxidase (SK-4800, Vector Laboratories, Burlingame, California, USA) according to the manufacturer’s instructions. Sections were counterstained in Mayer’s hematoxylin. Sections of canine skeletal muscle, canine smooth muscle, or canine brown fat (from tissues identified histologically as brown adipose tissue in the abdomen of an approximately 2- to 3-week-old puppy), treated in the same manner, were used as positive controls for the respective antibody against which they were targeted, while PBS replaced the primary antibody for negative controls. All antibodies were also applied to canine white adipose tissue as a negative control.
All HE slides were evaluated by two reviewers (S.S., E.L.) to designate a liposarcoma subtype and grade; equivocal cases were evaluated by a third reviewer (C.R.) for consensus. Subtype was based on a revised classification scheme in dogs that includes the 3 established subtypes according to the World Health Organization tumor classification scheme in domestic animals (ie, well-differentiated liposarcoma, pleomorphic liposarcoma, and myxoid liposarcoma), as well as a dedifferentiated subtype (ie, dedifferentiated liposarcoma), which was recently reported in dogs and is a widely accepted subtype of human liposarcoma. 2,11,16 Grading was based on a scheme for canine STS. 7 Immunoreactivity was only counted as positive if present in neoplastic cells defined as cells that either had distinct lipid vacuoles or unequivocal evidence of malignancy (ie, cellular or nuclear atypia). Positive immunoreactivity was then semiquantitatively scored based on the distribution of immunoreactive cells within the tumor. IHC was categorized as +++ (50%–100% of neoplastic cells were immunoreactive), ++ (5%–50% of neoplastic cells were immunoreactive), + (0.25%–5% of neoplastic cells were immunoreactive), or 0 (<0.25% of neoplastic cells were immunoreactive, which was interpreted as spurious immunoreactivity). The specific cutoffs for this categorization scheme were developed by reviewing a subset of the cases to estimate the variation in immunoreactivity prior to scoring the entire set of cases. If there was a discrepancy between the reviewers’ opinions, a third reviewer (C.R.) evaluated the case to reach a consensus. Staining intensity was subjectively assessed by comparing intensity of controls to intensity of immunoreactive neoplasms.
Results
The immunohistochemical profiles, histologic subtypes, and grades of all liposarcomas are summarized in Table 1. Twenty-five cases of liposarcoma were identified in dogs ranging from 8 to 14 years old including 11 females and 13 males. Mixed breed was the most common (n = 7), followed by Labrador retriever (n = 3), Shetland sheepdog (n = 2), Doberman pinscher (n = 2), and 1 case each of cocker spaniel, Alaskan malamute, Brittany spaniel, Bassett hound, beagle, Yorkshire terrier, Great Dane, toy poodle, golden retriever, daschund, and Chihuahua. Most liposarcomas were located in the subcutis (14/25, 56%), with most subcutaneous masses on the limbs (n = 8) or thorax (n = 5). Other locations included the peritoneum/omentum (n = 3), skeletal muscle (n = 2), intraorbital space (n = 2), and thoracic cavity (n = 1). Location was not specified in 3 cases. Oil red O stain revealed intracytoplasmic lipid droplets in all 15 cases in which it was examined (Table 1).
Histologic Subtype, Grade, and Immunohistochemical Profile of 25 Canine Liposarcomas.a
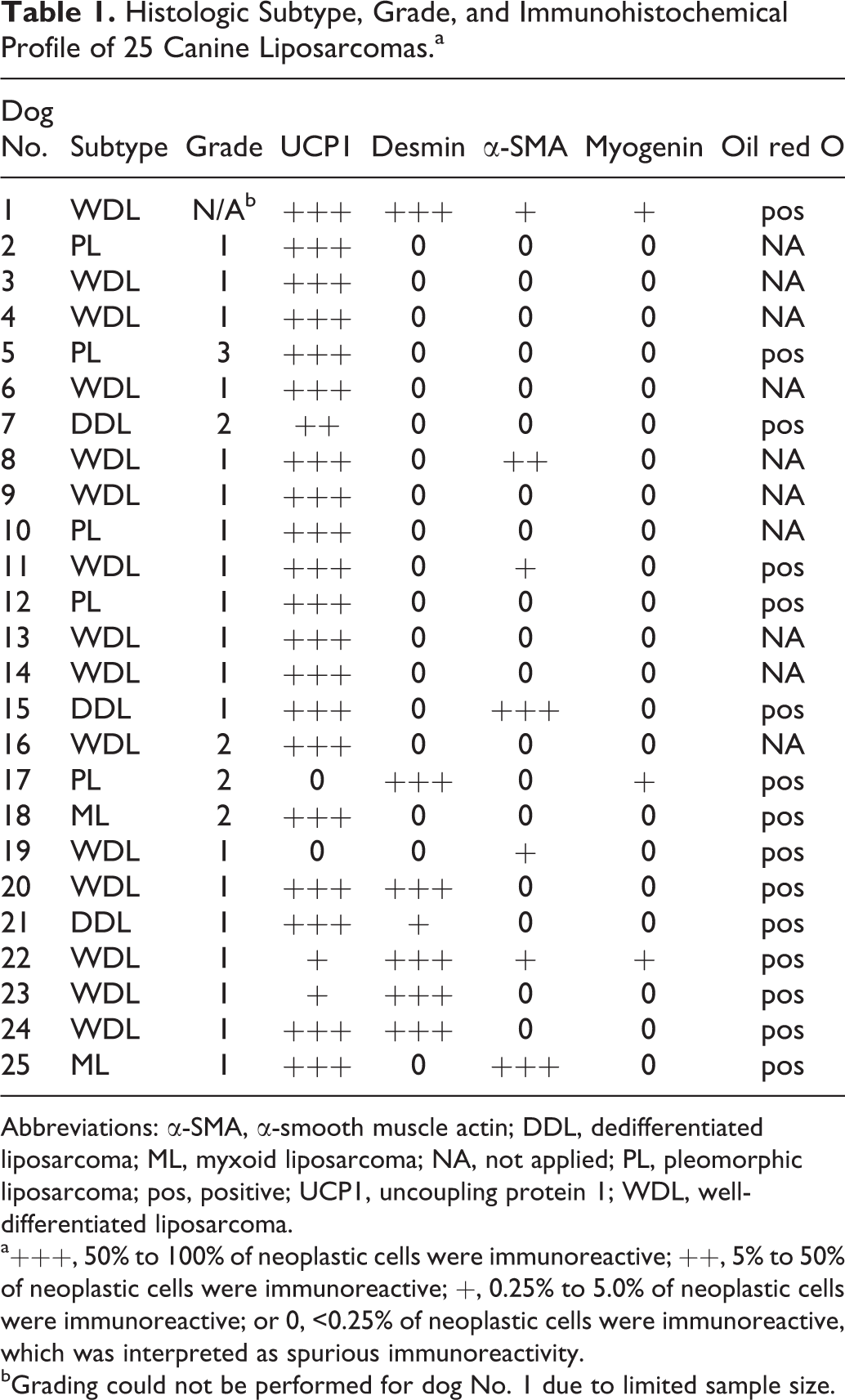
Abbreviations: α-SMA, α-smooth muscle actin; DDL, dedifferentiated liposarcoma; ML, myxoid liposarcoma; NA, not applied; PL, pleomorphic liposarcoma; pos, positive; UCP1, uncoupling protein 1; WDL, well-differentiated liposarcoma.
a+++, 50% to 100% of neoplastic cells were immunoreactive; ++, 5% to 50% of neoplastic cells were immunoreactive; +, 0.25% to 5.0% of neoplastic cells were immunoreactive; or 0, <0.25% of neoplastic cells were immunoreactive, which was interpreted as spurious immunoreactivity.
bGrading could not be performed for dog No. 1 due to limited sample size.
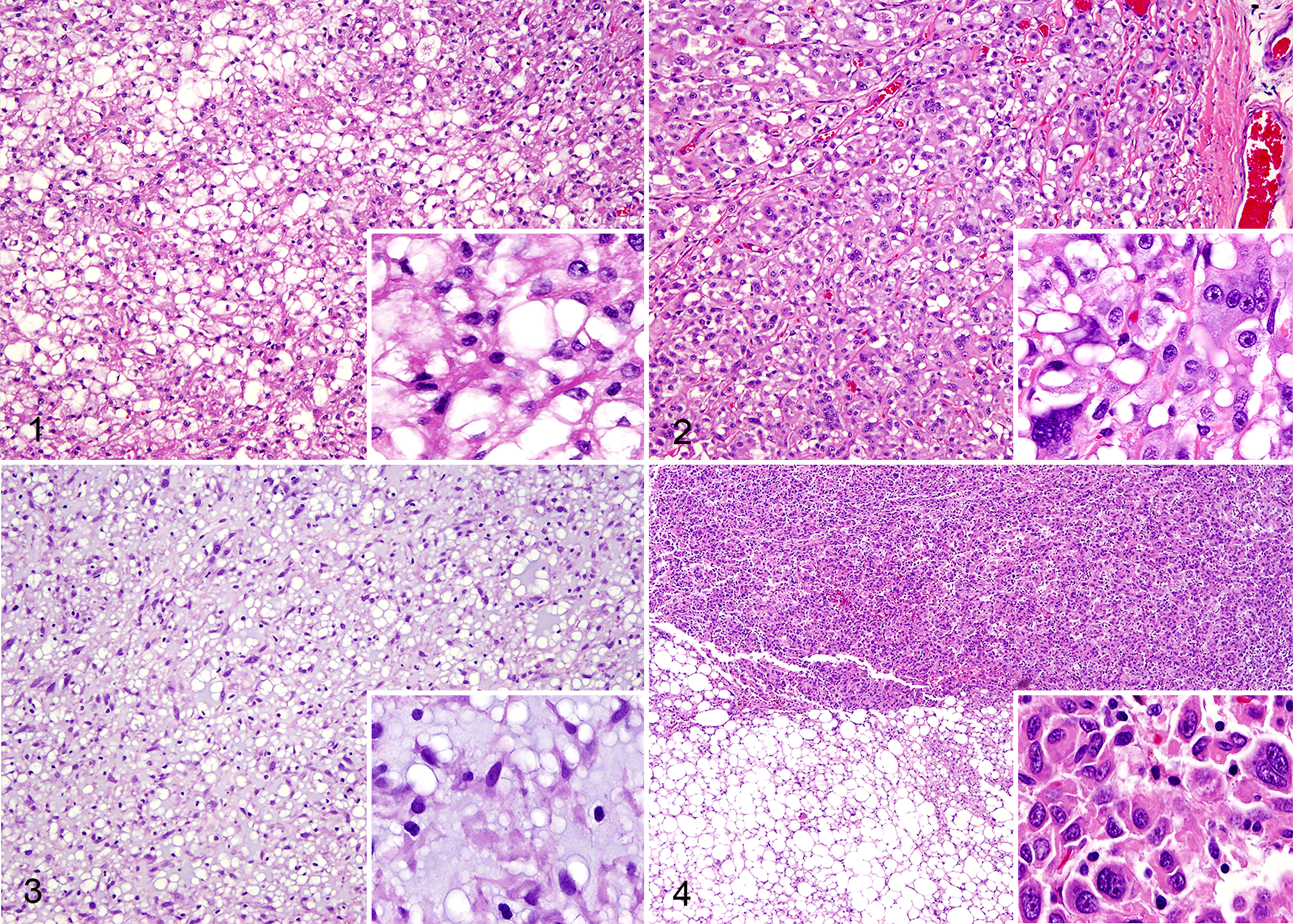
The liposarcoma subtypes were well-differentiated liposarcoma (15/25, 60%), pleomorphic liposarcoma (n = 5, 20%), myxoid liposarcoma (n = 3, 12%), and dedifferentiated liposarcoma (n = 2, 8%) (Table 1). Well-differentiated liposarcoma was characterized by proliferation of mature adipocytes with variation in cell size and nuclear atypia (Fig. 1). Pleomorphic liposarcoma was characterized by lipoblasts with marked cytologic and nuclear atypia (Fig. 2). Lipoblasts, which are defined as having 1 or multiple small cytoplasmic vacuoles and a hyperchromatic scalloped nucleus, and marked atypia are the key diagnostic features of pleomorphic liposarcoma. 16 Myxoid liposarcoma was characterized by a variably cellular mass of round to spindle cells in a myxoid background with variable numbers of lipoblasts (Fig. 3). Dedifferentiated liposarcoma was characterized by areas of nonlipogenic sarcoma with abrupt, multifocal transition to mature adipocytes with small numbers of lipoblasts. In one of the dedifferentiated liposarcomas, the dedifferentiated portion was most consistent with a myxofibrosarcoma. In the other dedifferentiated liposarcoma, the dedifferentiated portion was most consistent with an undifferentiated pleomorphic sarcoma (Fig. 4). Grade 1 was most common, followed by grade 2 and lastly grade 3 (Table 1).
Immunoreactivity to the UCP1 antibody was identified in 23 of 25 cases (92%), including 14 of 15 well-differentiated liposarcomas, 4 of 5 pleomorphic liposarcomas, 3 of 3 myxoid liposarcomas, and 2 of 2 dedifferentiated liposarcomas. Immunoreactivity in the positive control (ie, brown adipose tissue) and neoplastic cells was cytoplasmic and stippled (Fig. 5). The positive control had more intense immunoreactivity than neoplastic cells. Additional canine cell types in this study that were immunoreactive to this UCP1 antibody, with moderate cytoplasmic stippling, included skeletal myocytes, keratinocytes, and occasional cells with multiple small cytoplasmic vacuoles in white adipose tissue.
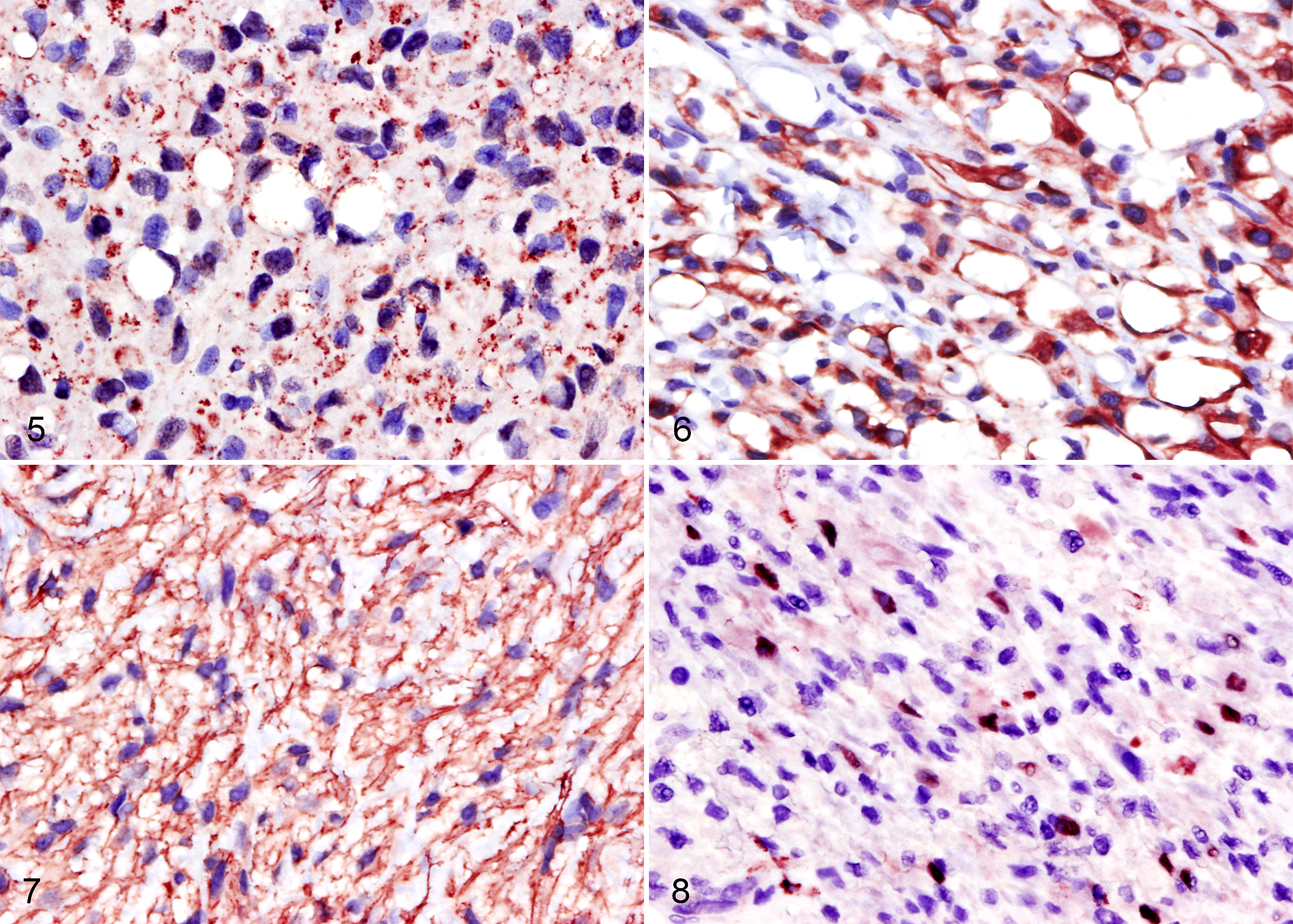
Cytoplasmic immunoreactivity to the desmin antibody was identified in 7 of 25 cases (28%), including 5 of 15 well-differentiated liposarcomas, 1 of 5 pleomorphic liposarcomas, and 1 of 2 dedifferentiated liposarcomas (Fig. 6). Immunoreactivity was graded as +++ in almost all cases (6/7) and + in 1 case (1/7). The intensity was similar in neoplasms and the positive control. Cytoplasmic immunoreactivity to the α-SMA antibody was identified in 7 of 25 cases (28%), including 5 of 15 well-differentiated liposarcomas, 1 of 5 myxoid liposarcomas, and 1 of 2 dedifferentiated liposarcomas (Fig. 7). Immunoreactivity was graded as + (4/7 cases), ++ (1/7 cases), and +++ (2/7 cases). Intensity was similar in neoplasms and the positive control. Nuclear immunoreactivity to the myogenin antibody was identified in 3 of 25 cases (12%), including 2 of 15 well-differentiated liposarcomas and 1 of 5 pleomorphic liposarcomas (Fig. 8). Immunoreactivity to myogenin was graded as + in all positive cases. Intensity was similar in neoplasms and the positive control.
Discussion
This report describes immunoreactivity to muscle antigens—including desmin, α-SMA, and myogenin—in canine liposarcoma. There are rare reports of immunoreactivity of liposarcoma to muscle markers in animals. 8,19 Skeletal muscle and white fat may share a common embryologic origin, and it is possible that immunoreactivity of adipocytic tumors to muscle markers reflects this common mesenchymal origin. 28 This information has relevance for veterinary pathologists because if canine liposarcoma can be immunoreactive to muscle markers, these neoplasms may be misdiagnosed as rhabdomyosarcoma, especially in poorly differentiated neoplasms. This has prognostic implications as canine rhabdomyosarcoma is typically a more malignant neoplasm and is not graded with the standard STS grading scheme. 7 While difficult to quantify in the literature, it is the authors’ experience that some cells may be vacuolated in a number of neoplasms, and this can raise the suspicion of an adipocyte neoplasm and indicate the need for IHC in diagnosis. Histomorphology alone is considered sufficient for the diagnosis of liposarcoma in well-differentiated liposarcoma, pleomorphic liposarcomas in which ≥50% of the neoplasm is composed of lipoblasts, and dedifferentiated liposarcoma in which ≥50% of the neoplasm is well differentiated. 16 For the remaining cases (ie, all myxoid liposarcomas, pleomorphic liposarcomas in which <50% of the neoplasm is composed of lipoblasts, and dedifferentiated liposarcoma in which <50% of the neoplasm is well differentiated), IHC and lipid stains may be necessary to establish a definitive diagnosis.
Desmin and α-SMA were selected in this study because they are the most commonly reported muscle markers to be immunoreactive to liposarcoma in pleomorphic liposarcomas in humans. 14 Our results indicate that this is also true in canine liposarcoma as desmin and α-SMA actin were the most commonly expressed muscle markers in this study. Desmin is frequently considered a muscle-specific antigen, but recent research has revealed its relatively low specificity. 4,14 This and previous studies have reported immunoreactivity to desmin in several human and canine nonmuscular neoplasms, including osteosarcoma, liposarcoma, lipoblastoma, lipoma, and hemangiopericytoma. 2,14,19,21,28 The literature on the specificity of α-SMA is varied, with some reports indicating it is specific and useful for differentiating neoplasms of myogenic origin and others suggesting its specificity is limited. 6,19,28 The results in this study are in agreement with previous reports of moderate specificity of α-SMA as 28% of liposarcomas were immunoreactive to this marker. Myogenin is generally considered a more specific and sensitive marker for muscle-specific neoplasia than α-SMA or desmin. 4,5 In reference to its high specificity, myogenin has been reported only rarely to have sparse immunoreactivity in nonmuscular spindle cell neoplasms in people. 5 This is supported by findings in this study, in which myogenin was the least common muscle marker to be immunoreactive to canine liposarcomas, with reactivity in only 12% of cases; in those cases, immunoreactivity was mild.
In humans, well-differentiated liposarcoma, dedifferentiated liposarcoma, and pleomorphic liposarcoma are reported to express muscle markers. 16 In this study, not only did well-differentiated liposarcoma, dedifferentiated liposarcoma, and pleomorphic liposarcoma variably express muscle markers, but also 1 myxoid liposarcoma expressed a muscle marker (ie, α-SMA); the latter is not reported in human liposarcoma to our knowledge. 14 Mouse double minute 2 homolog (MDM2) is a ubiquitin ligase whose expression has been reported in several types of canine neoplasms, including hepatoid gland tumors, mast cell tumor, and mammary gland carcinoma. The immunohistochemical expression of MDM2 has been used with increasing frequency in human liposarcoma to confirm malignancy as this marker is almost never expressed in benign tumors of fat. MDM2 is positive in only a subset of well-differentiated liposarcomas and dedifferentiated liposarcomas and should be negative in most myxoid liposarcomas and pleomorphic liposarcomas in humans. 16 A previous study reported expression of MDM2 in well-differentiated liposarcoma, dedifferentiated liposarcoma, and myxoid liposarcoma in dogs, and several liposarcomas that were originally classified as well-differentiated liposarcoma based on histomorphology were reclassified as pleomorphic liposarcoma based on a lack of MDM2 expression. 2 Although MDM2 clusters with certain liposarcoma subtypes, it is not immunoreactive in 100% of well-differentiated liposarcomas and hence is not sensitive for the diagnosis. In humans, MDM2 expression is not recommended as a confirmatory diagnosis but part of an IHC panel to determine malignancy and subtype. 16
Although UCP1 has traditionally been considered a marker of brown adipose tissue, UCP1 expression has been reported in murine brain; skeletal muscle; thymocytes; pancreatic islet cells; uterine smooth muscle; white adipose tissue of knockout mice with a defective vitamin D receptor; human keratinocytes, sweat glands, hair follicles, sebaceous glands, pancreatic islet cells, and “beige” adipocytes; macaque pancreatic islet cells; and rat thymocytes. 1,13,17,20,22,23 In light of the diverse cellular expression of UCP1, new roles for UCP1 have been suggested, including aiding in muscle contractility and protecting against oxidative stress. 20,23 In this study, the expression of UCP1 by neoplastic liposarcoma cells and cells with multiple small cytoplasmic vacuoles in control white adipose tissue was particularly interesting. Recent research revealed that some of the cells in white adipose tissue express UCP1 under certain conditions, such as exposure to cold. These cells that are capable of expressing UCP1 have been termed beige adipocytes to differentiate them from brown or white adipocytes. 10 Additionally, a study on human hibernoma revealed that a subpopulation of neoplastic brown adipocytes differentiate into white adipocytes and have weaker and more patchy staining to UCP1 than brown adipocytes. 18 This suggests that some transdifferentiated neoplastic white adipocytes are immunoreactive to UCP1 but have slightly weaker immunoreactivity than their brown adipocyte counterparts, which may be a cause for the weaker staining pattern seen in neoplastic cells in the current study compared to other published canine hibernoma studies. An additional reason for weaker immunoreactivity in this study compared to previous reports of canine hibernoma is that the UCP1 antibody was diluted to 1:100 in this study but was 5 times more concentrated in the other reports of canine hibernoma. 25,27 It is unknown in the present study if UCP1 expression by neoplastic cells represents transdifferentiation of white adipocytes to brown adipocytes, aberrant expression of UCP1 in white adipocytes, neoplastic transformation of beige adipocytes, or cross-reaction of the antibody against human UCP1 with a different canine protein.
In light of the increasing number of potential roles for UCP1 and increased number of cell types that may be able to express UCP1, immunoreactivity to this antigen should be interpreted with a broader lens considering cell types other than brown adipocytes, particularly in canine tissues. This is particularly relevant when differentiating between canine hibernomas and liposarcomas, both of which have now been reported to express muscle markers and UCP1. Hibernomas, however, are a benign tumor and should lack cellular atypia and other features of malignancy. A recent report diagnosed several cases of canine retrobulbar hibernomas based on UCP1 expression in all cases and abundant mitochondria identified ultrastructurally in 1 case. However, abundant mitochondria are a prominent ultrastructural feature in the epithelioid component of some human pleomorphic liposarcomas, 12 and UCP1 expression was identified in many canine liposarcomas in this study. In light of the overlap in ultrastructural features and immunohistochemical profiles of hibernomas and liposarcomas, histomorphology should be used as the primary differentiating factor between canine liposarcomas and hibernomas, and the differentiation of these 2 neoplasms should be made with caution. Histologically, hibernomas are tumors of brown adipocytes with coarse, granular cytoplasm and centrally located nuclei with a distinct lobular pattern; mitotic figures and cellular atypia are usually absent. 15 None of the neoplasms in this study had histologic features consistent with hibernoma.
The proportion of canine liposarcoma subtypes in this study is similar to that previously reported as the most common canine liposarcoma subtype was well-differentiated liposarcoma, followed in descending frequency by pleomorphic liposarcoma, myxoid liposarcoma, and dedifferentiated liposarcoma. 2 Well-differentiated liposarcoma is also the most common subtype of human liposarcoma, but in contrast to dogs, human myxoid liposarcoma and dedifferentiated liposarcoma subtypes are more common than pleomorphic liposarcoma. 16
Soft tissue sarcomas comprise between 7% and 15% of all cutaneous and subcutaneous tumors in the dog. A common hurdle in grading and in turn prognosticating these tumors is the difficulty in determining the specific histologic type. 7 Because liposarcoma has a similar immunohistochemical profile as rhabdomyosarcoma, misdiagnosis can lead to inaccurate prognostication and inappropriate treatment recommendations. This is especially important for liposarcoma subtypes that have overlapping histomorphology with rhabdomyosarcoma subtypes. Conversely, well-differentiated liposarcomas may be misdiagnosed as hibernomas if the diagnosis is solely based on UCP1 immunoreactivity, with an underestimation of risk. 25 The findings of this study clarify the immunohistochemical profile of liposarcoma and indicate that there is overlap in the expression of several muscle antigens and UCP1 between hibernoma, liposarcoma, and rhabdomyosarcoma.
Footnotes
Acknowledgments
We thank Felicia DonRussello, Kurt Takahashi, and Christopher Kwong of UC Davis Histology Laboratory for technical assistance. Special thanks is to Michael Manzer for his assistance in validating UCP1 antibody and for performing all immunohistochemical stains for this work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this project was supported by the Center for Companion Animal Health, School of Veterinary Medicine, University of California, Davis.
